Abstract
Background
Race and gender disparities in outcomes have been documented in many cancers. Our study evaluated the role of race, gender, and tumor primary site in predicting in-hospital mortality, discharge disposition, and complications among patients with brain metastases.
Methods
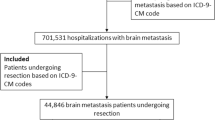
Using Nationwide Inpatient Sample (NIS) data from 1998 to 2007, we evaluated in-patient outcomes of brain metastases patients who underwent a craniotomy in U.S. hospitals. Univariate and multivariate analyses were used to assess the effect of patient/tumor characteristics in predicting the proposed outcomes.
Results
NIS estimated 78,170 patients with metastatic brain tumors underwent craniotomy between 1998 and 2007 in the United States. Median age was 59.2 years, 52.1 % were women, and 6.4 % were black. In-hospital mortality rate was 2.2 % with an average length of stay of 7.6 days. Black patients had significantly higher morbidity and nonroutine discharges than whites/others (p < .0001). Black women had almost twice the mortality (3.4 vs 1.8 %, p < .0001), a higher complication rate (24.6 vs 18.8 %, p < .0001), longer hospital stays (10.0 vs 7.3 days, p < .0001), and more nonroutine discharges (45.1 vs 36.8 %, p < .0001), compared with white/other women. Tumor histology was a significant predictor of outcomes, with female lung cancer patients having the highest odds of mortality and primary gastrointestinal tumors having the highest number of complications.
Conclusions
Evidence of race and gender disparities in outcomes were found in black patients, especially in black females who underwent surgical resection for brain metastases. These findings highlight an opportunity to reduce the gap of outcome disparities in brain metastasis patients.

Similar content being viewed by others
References
American Cancer Society 2011. Available from URL http://www.cancer.org/Research/CancerFactsFigures/index [Accessed November, 2011].
Linskey ME, Andrews DW, Asher AL, Burri SH, Kondziolka D, Robinson PD, et al. The role of stereotactic radiosurgery in the management of patients with newly diagnosed brain metastases: a systematic review and evidence-based clinical practice guideline. J Neurooncol. 2010;96:45–68.
JS N, A cD, Petersen I JR-C. Metastatic tumors of the CNS. 2000.
Da Silva AN, Nagayama K, Schlesinger DJ, Sheehan JP. Gamma Knife surgery for brain metastases from gastrointestinal cancer. J Neurosurg. 2009;111:423–30.
Go PH, Klaassen Z, Meadows MC, Chamberlain RS. Gastrointestinal cancer and brain metastasis: a rare and ominous sign. Cancer. 2011;117:3630–40.
Sampson JH, Carter JH, Friedman AH, Seigler HF. Demographics, prognosis, and therapy in 702 patients with brain metastases from malignant melanoma. J Neurosurg 1998;88:11–20.
Patchell RA, Regine WF, Loeffler JS, Sawaya R, Andrews DW, Chin LS. Radiosurgery plus whole-brain radiation therapy for brain metastases. JAMA. 2006;296:2089–90; author reply 2090–1.
Ammirati M, Cobbs CS, Linskey ME, Paleologos NA, Ryken TC, Burri SH, et al. The role of retreatment in the management of recurrent/progressive brain metastases: a systematic review and evidence-based clinical practice guideline. J Neurooncol. 2010;96:85–96.
Andrews DW, Scott CB, Sperduto PW, Flanders AE, Gaspar LE, Schell MC, et al. Whole brain radiation therapy with or without stereotactic radiosurgery boost for patients with one to three brain metastases: phase III results of the RTOG 9508 randomised trial. Lancet. 2004;363:1665–72.
Grossman R, Mukherjee D, Chang DC, Purtell M, Lim M, Brem H, et al. Predictors of inpatient death and complications among postoperative elderly patients with metastatic brain tumors. Ann Surg Oncol. 2011;18:521–8.
Hofmann MA, Coll SH, Küchler I, Kiecker F, Wurm R, Sterry W, et al. Prognostic factors and impact of treatment in melanoma brain metastases: better prognosis for women? Dermatology. 2007;215:10–6.
Lagerwaard FJ, Levendag PC, Nowak PJ, Eijkenboom WM, Hanssens PE, Schmitz PI. Identification of prognostic factors in patients with brain metastases: a review of 1292 patients. Int J Radiat Oncol Biol Phys. 1999;43:795–803.
World Health Organization. International Classification of Diseases and Related Health Problems. Geneva, 1993.
Elixhauser A, Steiner C, Harris DR, Coffey RM. Comorbidity measures for use with administrative data. Med Care. 1998;36:8–27.
Berz JP, Johnston K, Backus B, Doros G, Rose AJ, Pierre S, et al. The influence of black race on treatment and mortality for early-stage breast cancer. Med Care. 2009;47:986–92.
Adams SA, Butler WM, Fulton J, Heiney SP, Williams EM, Delage AF et al. Racial disparities in breast cancer mortality in a multiethnic cohort in the Southeast. Cancer. 2011. doi:10.1002/cncr.26570 [Epub ahead of print].
Curry WT, Carter BS, Barker FG. Racial, ethnic, and socioeconomic disparities in patient outcomes after craniotomy for tumor in adult patients in the United States, 1988–2004. Neurosurgery 2010;66:427–37; discussion 437–8.
Yothers G, Sargent DJ, Wolmark N, Goldberg RM, O’Connell MJ, Benedetti JK, et al. Outcomes among black patients with stage II and III colon cancer receiving chemotherapy: an analysis of ACCENT adjuvant trials. J Natl Cancer Inst. 2011;103:1498–506.
Rades D, Hornung D, Veninga T, Schild SE, Gliemroth J. Single brain metastasis: Radiosurgery alone compared with radiosurgery plus up-front whole-brain radiotherapy. Cancer. 2011. doi:10.1002/cncr.26612 [Epub ahead of print].
Clarke JW, Register S, McGregor JM, Grecula JC, Mayr NA, Wang JZ, et al. Stereotactic radiosurgery with or without whole brain radiotherapy for patients with a single radioresistant brain metastasis. Am J Clin Oncol. 2010;33:70–4.
Lo SS, Clarke JW, Grecula JC, McGregor JM, Mayr NA, Cavaliere R, et al. Stereotactic radiosurgery alone for patients with 1–4 radioresistant brain metastases. Med Oncol. 2011 28 Suppl 1:S439–44.
U.S. Census Bureau. Population Profile of the United States. 2012.
Curry WT, McDermott MW, Carter BS, Barker FG. Craniotomy for meningioma in the United States between 1988 and 2000: decreasing rate of mortality and the effect of provider caseload. J Neurosurg. 2005;102:977–86.
Liu JH, Zingmond DS, McGory ML, SooHoo NF, Ettner SL, Brook RH, et al. Disparities in the utilization of high-volume hospitals for complex surgery. JAMA. 2006;296:1973–80.
Mukherjee D, Zaidi HA, Kosztowski T, Chaichana KL, Salvatori R, Chang DC, et al. Predictors of access to pituitary tumor resection in the United States, 1988–2005. Eur J Endocrinol. 2009;161:259–65.
Author information
Authors and Affiliations
Corresponding author
Additional information
M. Nuño and D. Mukherjee are co-first-authors.
Appendix
Appendix
See Table 6
Rights and permissions
About this article
Cite this article
Nuño, M., Mukherjee, D., Elramsisy, A. et al. Racial and Gender Disparities and the Role of Primary Tumor Type on Inpatient Outcomes Following Craniotomy for Brain Metastases. Ann Surg Oncol 19, 2657–2663 (2012). https://doi.org/10.1245/s10434-012-2353-z
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-012-2353-z