Abstract
Background
No agreement has been made about the optimal extent of thyroidectomy or lymph node dissection in papillary thyroid microcarcinoma (PTMC). Our aim was to find out the factors associated with the presence of lymph node metastases in the patients with PTMC and to discuss the extent of thyroidectomy and lymphadenectomy.
Methods
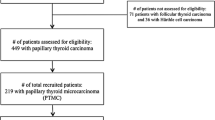
A total of 254 patients with PTMC (212 women, 42 men; age 14 to 85 years, median 47 years) were treated at our institute between 1975 and 2007. Lymph node metastases were confirmed in 59 patients (23%) by histopathology. The median observation time was 56 (range, 1–397) months, and the recurrence was diagnosed in seven patients. Modified radical neck dissection and central neck dissection were performed in 55 and 30 patients, respectively. The data on the clinicopathological characteristics of patients and treatment were collected.
Results
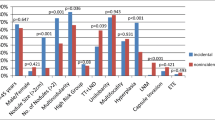
An incidental PTMC was diagnosed in 107 patients postoperatively. In none of them was a lymph node metastasis or tumor recurrence detected. Preoperatively, an overt PTMC was diagnosed in 147 patients. Clinically manifest metastases were diagnosed in 59 (40%) of them: in 51 preoperatively, and in 8 during the surgical procedure. In 147 patients who had preoperative diagnosis of PTMC, the factors that correlated (P < 0.05) with the presence of lymph node metastases were sex, age, and tumor type.
Conclusions
The patients with high-risk PTMC with preoperatively confirmed lymph node metastases had a higher recurrence rate than those with low-risk PTMC without preoperatively detectable lymph node metastases; therefore, careful therapeutic node dissection is necessary in high-risk patients.
Similar content being viewed by others
References
Hedinger CW, Sobin LH. Histologic typing of thyroid tumours. In: Hedinger CW, Sobin LH, editors. International Histological Classification of Tumours No. 11. Geneva: World Health Organization, 1988. p.1–18.
Gomez Segovia I, Gallowitsch HJ, Kresnik E, et al. Descriptive epidemiology of thyroid carcinoma in Carinthia, Austria: 1984–2001. Histopathologic features and tumor classification of 734 cases under elevated general iodination of table salt since 1990: population-based age-stratified analysis on thyroid carcinoma incidence. Thyroid. 2004;14:277–86.
Appetecchia M, Scarcello G, Pucci E, Procaccini A. Outcome after treatment of papillary thyroid microcarcinoma. J Exp Clin Cancer Res. 2002;21:159–64.
Pelizzo MR, Boschin IM, Toniato A, et al. Papillary thyroid microcarcinoma (PTMC): prognostic factors, management and outcome in 403 patients. Eur J Surg Oncol. 2006;32:1144–8.
Roti E, Rossi R, Trasforini G, et al. Clinical and histological characteristics of papillary thyroid microcarcinoma: results of a retrospective study in 243 patients. J Clin Endocrinol Metab. 2006;91:2171–8.
Cheema Y, Olson S, Elson D, Chen H. What is the biology and optimal treatment for papillary microcarcinoma of the thyroid? J Surg Res. 2006;134:160–2.
Lim DJ, Baek KH, Lee YS, et al. Clinical, histopathological, and molecular characteristics of papillary thyroid microcarcinoma. Thyroid. 2007;17:883–8.
Besic N, Pilko G, Petric R, Hocevar M, Zgajnar J. Papillary thyroid microcarcinoma: prognostic factors and treatment. J Surg Oncol. 2008;97:221–5.
Wada N, Duh QY, Sugino K, et al. Lymph node metastasis from 259 papillary thyroid microcarcinomas: frequency, pattern of occurrence and recurrence, and optimal strategy for neck dissection. Ann Surg. 2003;237:399–407.
Sakorafas GH, Giotakis J, Stafyla V. Papillary thyroid microcarcinoma: a surgical perspective. Cancer Treat Rev. 2005;31:423–38.
Ito Y, Miyauchi A. Lateral lymph node dissection guided by preoperative and intraoperative findings in differentiated thyroid carcinoma. World J Surg. 2008;32:729–39.
Hay ID, Grant CS, van Heerden JA, et al. Papillary thyroid microcarcinoma: a study of 535 cases observed in a 50-year period. Surgery. 1992;112:1139–46.
Sobin LH WC. Thyroid gland. In: Sobin LH WC, editor. TNM Classification of Malignant Tumours. New York: Wiley-Liss, 2002:52–6.
Hay ID, Bergstralh EJ, Goellner JR, et al. Predicting outcome in papillary thyroid carcinoma: development of a reliable prognostic scoring system in a cohort of 1779 patients surgically treated at one institution during 1940 through 1989. Surgery. 1993;114:1050–7.
Passler C, Scheuba C, Prager G, et al. Prognostic factors of papillary and follicular thyroid cancer: differences in an iodine-replete endemic goiter region. Endocr Relat Cancer. 2004;11:131–9.
Sugitani I, Fujimoto Y. Symptomatic versus asymptomatic papillary thyroid microcarcinoma: a retrospective analysis of surgical outcome and prognostic factors. Endocr J. 1999;46:209–16.
Chow SM, Law SC, Chan JK, et al. Papillary microcarcinoma of the thyroid-Prognostic significance of lymph node metastasis and multifocality. Cancer. 2003;98:31–40.
Pellegriti G, Scollo C, Lumera G, et al. Clinical behavior and outcome of papillary thyroid cancers smaller than 1.5 cm in diameter: study of 299 cases. J Clin Endocrinol Metab. 2004;89:3713–20.
Ito Y, Tomoda C, Uruno T, et al. Papillary microcarcinoma of the thyroid: how should it be treated? World J Surg. 2004;28:1115–21.
Stoeckli SJ, Pfaltz M, Steinert H, Schmid S. Sentinel lymph node biopsy in thyroid tumors: a pilot study. Eur Arch Otorhinolaryngol. 2003;260:364–8.
Baudin E, Travagli JP, Ropers J, et al. Microcarcinoma of the thyroid gland: the Gustave-Roussy Institute experience. Cancer. 1998;83:553–9.
Ito Y, Tomoda C, Uruno T, et al. Clinical significance of metastasis to the central compartment from papillary microcarcinoma of the thyroid. World J Surg. 2006;30:91–9.
Ito Y, Tomoda C, Uruno T, et al. Preoperative ultrasonographic examination for lymph node metastasis: usefulness when designing lymph node dissection for papillary microcarcinoma of the thyroid. World J Surg. 2004;28:498–501.
Shaha AR, Tuttle RM, Shah JP. Papillary microcarcinoma of the thyroid. J Surg Oncol. 2007;95:532–3.
Son YI, Jeong HS, Baek CH, et al. Extent of prophylactic lymph node dissection in the central neck area of the patients with papillary thyroid carcinoma: comparison of limited versus comprehensive lymph node dissection in a 2-year safety study. Ann Surg Oncol. 2008;15:2020–6.
Sugitani I, Yanagisawa A, Shimizu A, Kato M, Fujimoto Y. Clinicopathologic and immunohistochemical studies of papillary thyroid microcarcinoma presenting with cervical lymphadenopathy. World J Surg. 1998;22:731–7.
Chow SM, Law SC, Mendenhall WM, et al. Papillary thyroid carcinoma: prognostic factors and the role of radioiodine and external radiotherapy. Int J Radiat Oncol Biol Phys. 2002;52:784–95.
Lo CY, Chan WF, Lang BH, et al. Papillary microcarcinoma: is there any difference between clinically overt and occult tumors? World J Surg. 2006;30:759–66.
Lin JD, Chen ST, Chao TC, Hsueh C, Weng HF. Diagnosis and therapeutic strategy for papillary thyroid microcarcinoma. Arch Surg. 2005;140:940–5.
Lin JD, Kuo SF, Chao TC, Hsueh C. Incidental and nonincidental papillary thyroid microcarcinoma. Ann Surg Oncol. 2008;15:2287–92.
Elio R, Degli Uberti E, Braverman L, Bondanelli M. Thyroid papillary microcarcinoma. A descriptive and meta-analysis study. Eur J Endocrinol. 2008;159:659–73.
Acknowledgment
This article is a part of the research studies series (J3-0570) supported by the Ministry of Education, Science, and Sport of Slovenia.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Besic, N., Zgajnar, J., Hocevar, M. et al. Extent of Thyroidectomy and Lymphadenectomy in 254 Patients With Papillary Thyroid Microcarcinoma: A Single-Institution Experience. Ann Surg Oncol 16, 920–928 (2009). https://doi.org/10.1245/s10434-009-0332-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-009-0332-9