Abstract
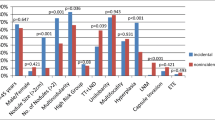
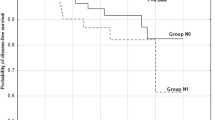
We previously demonstrated that (1) most papillary microcarcinomas can be followed without surgical treatment and (2) when surgery is performed, patients with lateral lymph node metastasis detected on preoperative ultrasonography (US) are more likely to develop recurrence. In this study, we further investigated the application of these strategies. To date, we have observed 211 patients (average follow-up 47.9 months). In more than 70% of these patients the tumor size did not increase during the follow-up period. There were no clinicopathologic features linked to tumor enlargement except in tumors ≥ 7 mm, which tended to enlarge in patients followed for 4 years. To evaluate not only whether observation can continue but also how to dissect the lymph nodes optimally at surgery, US diagnosis for lateral node metastasis is essential because the presence of US-diagnosed lateral metastasis is an even stronger predictive marker for recurrence than the presence of pathologically confirmed node metastasis. The positive predictive value (PPV) was 80.6% for US but reached 100% if fine-needle aspiration biopsy (FNAB) of nodes or FNAB-thyroglobulin measurement is added. Furthermore, carcinomas occupying the upper region of the thyroid more frequently showed US-diagnosed and pathologically confirmed lateral metastasis, and those measuring ≥ 7 mm were more likely to show pathologically confirmed lateral metastasis. These findings suggest that, for papillary microcarcinoma: (1) US-diagnosed lateral metastasis is a strong marker predicting a worse relapse-free survival; (2) FNAB of nodes and FNAB-thyroglobulin measurement are useful tools for evaluating lymph node metastasis; and (3) careful US evaluation for lateral metastasis is necessary in patients with a tumor measuring ≥ 7 mm or that is located in the upper region of the thyroid both during observation and preoperatively.


Similar content being viewed by others
References
T Yokozawa A Miyauchi K Kuma et al. (1995) ArticleTitleAccurate and simple method of diagnosing thyroid nodules by the modified technique of ultrasound-guided fine needle aspiration biopsy Thyroid 5 141–145 Occurrence Handle1:STN:280:ByqA2srlsFU%3D Occurrence Handle7647575
MD Bramley BJ Harrison (1996) ArticleTitlePapillary microcarcinoma of the thyroid gland Br. J. Surg. 83 1674–1683 Occurrence Handle1:STN:280:ByiC1M%2FlvVQ%3D Occurrence Handle9038540
F Iida A Sugenoya A Muramatsu (1991) ArticleTitleClinical and pathologic properties of small differentiated carcinomas of the thyroid gland World J. Surg. 15 511–515 Occurrence Handle1:STN:280:By6A28flsVQ%3D Occurrence Handle1891937
JM Rodriguez MP Parrilla J Sola et al. (1997) ArticleTitlePapillary thyroid microcarcinoma: clinical study and prognosis Eur. J. Surg. 163 255–259 Occurrence Handle1:STN:280:ByiA3crls1A%3D Occurrence Handle9161822
H Rassael LDR Thompson CS Heffess (1998) ArticleTitleA rationale for conservative management of microscopic papillary carcinoma of the thyroid gland: a clinicopathological correlation of 90 cases Eur. Arch. Otorhinolaryngol. 255 462–467 Occurrence Handle10.1007/s004050050100 Occurrence Handle1:STN:280:DyaK1M%2FltVCjuw%3D%3D Occurrence Handle9833215
K Sugino K Ito SuffixJr O Ozaki et al. (1998) ArticleTitlePapillary microcarcinoma of the thyroid J. Endocrinol. Invest. 21 445–448 Occurrence Handle1:STN:280:DyaK1cvjvFeqtA%3D%3D Occurrence Handle9766259
ID Hay CS Grant JS Heerden Particlevan et al. (1992) ArticleTitlePapillary thyroid microcarcinoma: a study of 535 cases observed in a 50-year period Surgery 112 1139–1147 Occurrence Handle1:STN:280:ByyD1cfhs1M%3D Occurrence Handle1455316
FH Fukunaga R Yatani (1975) ArticleTitleGeographic pathology of occult thyroid carcinomas Cancer 36 1095–1099 Occurrence Handle1:STN:280:CSmD2c7kvVQ%3D Occurrence Handle1182663
Y Yamamoto T Maeda K Izumi et al. (1990) ArticleTitleOccult papillary carcinoma of the thyroid Cancer 65 1173–1179 Occurrence Handle1:STN:280:By%2BC2M%2Fgtlc%3D Occurrence Handle2302665
HR Harach KO Franssila VM Wasenius (1985) ArticleTitleOccult papillary carcinoma of the thyroid: a “normal” finding in Finland; a systematic autopsy study Cancer 56 531–538 Occurrence Handle1:STN:280:BiqB38jptFQ%3D Occurrence Handle2408737
K Takebe M Date Y Yamamoto et al. (1994) ArticleTitleMass screening for thyroid cancer with ultrasonography Karkinos 7 309–317
Y Ito R Uruno K Nakano et al. (2003) ArticleTitleAn observation trial without surgical treatment in patients with papillary microcarcinoma of the thyroid Thyroid 13 381–388 Occurrence Handle10.1089/105072503321669875 Occurrence Handle12804106
Ito Y, Tomoda C, Uruno T, et al. Preoperative ultrasonographic examination for lymph node metastasis is useful when designing lymph node dissection for papillary microcarcinoma. World J. Surg. in press
A Antonelli P Miccoli P Fallahi et al. (2003) ArticleTitleRole of neck ultrasonography in the follow-up of children operated on for thyroid papillary cancer Thyroid 13 479–484 Occurrence Handle10.1089/105072503322021142 Occurrence Handle12855015
A Frasoldati E Toschi M Zini et al. (1999) ArticleTitleRole of thyroglobulin measurement in fine-needle aspiration biopsies of cervical lymph nodes in patients with differentiated thyroid cancer Thyroid 9 105–111 Occurrence Handle1:STN:280:DyaK1M7ovVKqtg%3D%3D Occurrence Handle10090308
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ito, Y., Tomoda, C., Uruno, T. et al. Papillary Microcarcinoma of the Thyroid: How Should It Be Treated?. World J. Surg. 28, 1115–1121 (2004). https://doi.org/10.1007/s00268-004-7644-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-004-7644-5