Abstract
Background
Truncal melanoma involving metastases to multiple lymph node basins has a much worse prognosis than tumor involvement of a single lymph node basin. Recent results also suggest that, independently of the status of lymph node involvement, patients with multiple lymphatic basin drainage (MLBD) on lymphoscintigraphy have an increased risk of lymph node metastasis and a worse prognosis than those with a single lymphatic drainage basin. Because published reports have conflicting results, the authors compared their experience at the University of Michigan Comprehensive Cancer Center with recently published findings.
Methods
The authors searched a prospectively maintained melanoma database at the University of Michigan for patients with primary truncal melanoma who underwent lymphoscintigraphy and sentinel lymph node biopsy between 1997 and 2004. The association of MLBD with the clinical and pathologic characteristics collected and the presence of regional metastases was tested by using contingency tables and the χ2 test statistic and by using the Fisher’s exact test statistic when cell frequencies were small. The product-limit method of Kaplan and Meier was used to estimate disease-free and overall survival probabilities.
Results
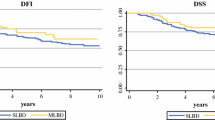
Of 423 patients with primary truncal melanoma who underwent sentinel lymph node biopsy, 123 (29%) had a positive result, and 98 patients (23.2%) had MLBD. Patients with tumors located in the middle of the trunk and tumor ulceration were more likely to have MLBD (P < .0001 and P = .045, respectively). Patients with a single lymphatic drainage basin and MLBD had a similar risk of lymph node metastasis and similar disease-free and overall survival.
Conclusions
Patients with truncal melanomas tend to have MLBD when the tumor is located in the middle of the trunk or when ulceration is present. In our experience, drainage to multiple lymphatic basins was not an independent risk factor for sentinel lymph node metastasis and has no independent prognostic significance.


Similar content being viewed by others
References
Gershenwald JE, Thompson W, Mansfield PF, et al. Multi-institutional melanoma lymphatic mapping experience: the prognostic value of sentinel lymph node status in 612 stage I or II melanoma patients. J Clin Oncol 1999;17:1–8
Johnson TM, Sondak VK, Bichakjian CK, Sabel MS. The role of sentinel lymph node biopsy for melanoma: evidence assessment 2005. J Am Acad Dermatol 2006;54(1):19–27
Balch CM, Soong S, Ross MI, et al. Long-term results of a multi-institutional randomized trial comparing prognostic factors and surgical results for intermediate thickness melanomas (1.0 to 4.0 mm). Ann Surg Oncol 2000;7:87–97
Barth RJ, Venzon DJ, Baker AR. The prognosis of melanoma patients with metastases to two or more lymph node areas. Ann Surg 1991;214:125–30
Coit DG, Rogatko A, Brennan MF. Prognostic factors in patients with melanoma metastatic to axillary or inguinal lymph nodes. Ann Surg 1991;214:627–36
Porter GA, Ross MI, Berman RS, et al. Significance of multiple nodal basin drainage in truncal melanoma patients undergoing sentinel lymph node biopsy. Ann Surg Oncol 2000;7:256–61
Jimenez RE, Panageas K, Busam KJ, et al. Prognostic implications of multiple lymphatic basin drainage in patients with truncal melanoma. J Clin Oncol 2005;23:518–24
Thompson JF, Uren RF. Teaching points on lymphatic mapping for melanoma from the Sydney Melanoma Unit. Semin Oncol 2004;31:349–56
McMasters KM, Chao C, Wong SL, et al. Interval sentinel lymph nodes in melanoma. Arch Surg 2002;137:543–7
Uren RF, Howman-Giles R, Thompson JF, et al. Interval nodes: the forgotten sentinel nodes in patients with melanoma. Arch Surg 2000;135:1168–72
Sappey MPC. Anatomie, Physiologie, des Vaisseaux Lymphtiques Consideres Chez l’Homme et les Vertebras. Paris: De Lahaye Publishing 1874
Lock-Anderson J, Rossing N, Drzewiecki KT. Preoperative cutaneous lymphoscintigraphy in malignant melanoma. Cancer 1989;63:77–82
Jacobs IA, Chang CK, Salti GI. Significance of dual-basin drainage in patients with truncal melanoma undergoing sentinel lymph node biopsy. J Am Acad Dermatol 2003;49:615–9
Sondak VK, Taylor JM, Sabel MS, et al. Mitotic rate and younger age are predictors of sentinel lymph node positivity: lessons learned from the generation of a probabilistic model. Ann Surg Oncol 2004;11:247–58
Norman J, Wells K, Kearney R, et al. Identification of lymphatic drainage basins in patients with cutaneous melanoma. Semin Surg Oncol 1993;9:224–7
Berger DH, Feig BW, Podoloff D, et al. Lymphoscintigraphy as a predictor of lymphatic drainage from cutaneous melanoma. Ann Surg Oncol 1997;4:13–8
Morton DL, Thompson JF, Essner R, et al. Validation of the accuracy of intraoperative lymphatic mapping and sentinel lymphadenectomy for early-stage melanoma: a multicenter trial. Multicenter selective lymphadenectomy trial group. Ann Surg 1999;230:453–63
Cascinelli N, Morabito A, Santinami M, et al. Immediate or delayed dissection of regional nodes in patients with melanoma of the trunk: a randomized trial. Lancet 1998;351:793–6
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
McHugh, J.B., Su, L., Griffith, K.A. et al. Significance of Multiple Lymphatic Basin Drainage in Truncal Melanoma Patients Undergoing Sentinel Lymph Node Biopsy. Ann Surg Oncol 13, 1216–1223 (2006). https://doi.org/10.1245/s10434-006-9014-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-006-9014-z