Abstract
Background
A low burden of disease represents an independent favorable prognostic factor of response to peptide receptor radionuclide therapy (PRRT) in patients affected by gastro-entero-pancreatic neuroendocrine tumors. However, it is not clear whether this is due to a lower diffusion of the disease or thanks to debulking surgery.
Methods
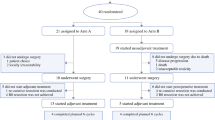
From 1996 to 2013 those patients diagnosed with G1–G2 pancreatic neuroendocrine tumor (PNET) and synchronous liver metastases who were not deemed eligible for liver radical surgery but were eligible to receive upfront PRRT were prospectively included in the study. Two groups of comparison were identified: those submitted for primary tumor resection before PRRT and those who were not. The outcome was evaluated as: objective response to PRRT (OR), progression-free survival (PFS), and overall survival (OS).
Results
Of the 94 subjects, 31 were previously submitted for primary tumor resection. After propensity score adjustments, patients who underwent surgery before PRRT showed higher stabilization or objective responses after PRRT (p = .006), and this translated into a better median PFS (70 vs. 30 months; p = .002) and OS (112 vs. 65 months; p = .011), for operated versus nonoperated patients, respectively. At multivariate analysis, operated patients showed a statistically significantly improved PFS: HR, 5.11 (95 % CI 1.43–18.3); p = .012, whereas Ki-67 in continuous fashion was correlated significantly with OS: 1.13 (95 % CI 1–1.27); p = .048.
Conclusions
Primary tumor resection prior to PRRT can be safely proposed in G1–G2 PNETs with diffuse liver metastases because it seems to enhance response to PRRT and to improve significantly PFS.


Similar content being viewed by others
References
Modlin IM, Lye KD, Kidd M. A 5-decade analysis of 13 715 carcinoid tumors. Cancer. 2003;97:934–59.
Yao JC, Hassan M, Phan A, et al. One hundred years after “carcinoid”: epidemiology of and prognostic factors for neuroendocrine tumors in 35,825 cases in the United States. J Clin Oncol. 2008;26:3063–72.
Chamberlain RS, Canes D, Brown KT, et al. Hepatic neuroendocrine metastases: does intervention alter outcomes? J Am Coll Surg. 2000;190:432–45.
Hockwald SN, Conlon KC, Brennan MF. Nonfunctional pancreatic islet cell tumors. In: Doherty G, Skogseid B, editors. Surgical endocrinology. 1st ed. Philadelphia: Lippincott Williams & Wilkins; 2001. pp. 361–73.
Panzuto F, Boninsegna L, Fazio N, et al. Metastatic and locally advanced pancreatic endocrine carcinomas: analysis of factors associated with disease progression. J Clin Oncol. 2011;29:2372–7.
Evans DB, Skibber JM, Lee JE, et al. Nonfunctioning islet cell carcinoma of the pancreas. Surgery. 1993;114:1175–81.
Solorzano CC, Lee JE, Pisters PW, et al. Nonfunctioning islet cell carcinoma of the pancreas: survival results in a contemporary series of 163 patients. Surgery. 2001;130:1078–85.
van der Zwan WA, Bodei L, Mueller-Brand J, de Herder WW, Kvols LK, Kwekkeboom DJ. GEPNETs update: Radionuclide therapy in neuroendocrine tumors. Eur J Endocrinol. 2015;172:R1–8. doi: 10.1530/EJE-14-0488.
Kwekkeboom DJ, Teunissen JJ, Bakker WH, et al. Radiolabeled somatostatin analog [177Lu-DOTA0,Tyr3] octreotate in patients with endocrine gastroenteropancreatic tumors. J Clin Oncol. 2005;23:2754–62.
Kwekkeboom DJ, de Herder WW, Kam BL, et al. Treatment with the radiolabeled somatostatin analog [177 Lu-DOTA0,Tyr3]octreotate: toxicity, efficacy, and survival. J Clin Oncol. 2008;26:2124–30.
Bertani E, Fazio N, Botteri E, et al. Resection of the primary pancreatic neuroendocrine tumor in patients with unresectable liver metastases: possible indications for a multimodal approach. Surgery. 2014;155:607–14.
Capurso G, Bettini R, Rinzivillo M, Boninsegna L, Delle Fave G, Falconi M. Role of resection of the primary pancreatic neuroendocrine tumour only inpatients with unresectable metastatic liver disease: a systematic review. Neuroendocrinology. 2011;93:223–9.
Bodei L, Cremonesi M, Grana CM, et al. Peptide receptor radionuclide therapy with 177Lu-DOTATATE: the IEO phase I-II study. Eur J Nucl Med Mol Imaging. 2011;38:2125–35.
Rindi G, Arnold R, Bosman FT. Nomenclature and classification of neuroendocrine neoplasm of the digestive system. In: Bosman FT, Carneiro F, Hruban RH, et al., editors. WHO classification of tumor of the digestive system. Lyon: International Agency for Research on Cancer (IRAC), 2010. pp. 13–14.
Falconi M, Eriksson B, Kaltsas G, et al. ENETS consensus guidelines update for the management of patients with functional pancreatic neuroendocrine tumors and non-functional pancreatic neuroendocrine tumors. Neuroendocrinology. 2016;103:153–71.
Kulke MH, Anthony LB, Bushnell DL, et al. NANETS treatment guidelines: well-differentiated neuroendocrine tumors of the stomach and pancreas. Pancreas. 2010;39:735–52.
Kulke MH, Shah MH, Benson AB 3rd, et al. Neuroendocrine tumors, version 1 2015. J Natl Compr Cancer Netw. 2015;13:78–108.
Bettini R, Mantovani W, Boninsegna L, et al. Primary tumour resection in metastatic nonfunctioning pancreatic endocrine carcinomas. Dig Liver Dis. 2009;41:49–55.
Nguyen SQ, Angel LP, Divino CM, Schluender S, Warner RR. Surgery in malignant pancreatic neuroendocrine tumors. J Surg Oncol. 2007;96:397–403.
Frilling A, Modlin IM, Kidd M, et al. Recommendations for management of patients with neuroendocrine liver metastases. Lancet Oncol. 2014;15:8–21.
Campana D, Capurso G, Partelli S, et al. Radiolabelled somatostatin analogue treatment in gastroenteropancreatic neuroendocrine tumours: factors associated with response and suggestions for therapeutic sequence. Eur J Nucl Med Mol Imaging. 2013;40:1197–205.
Ezziddin S, Opitz M, Attassi M, et al. Impact of the Ki-67 proliferation index on response to peptide receptor radionuclide therapy. Eur J Nucl Med Mol Imaging. 2011;38:459–66.
Metz DC, Choi J, Strosberg J, Heaney AP, Howden CW, Klimstra D, Yao JC. A rationale for multidisciplinary care in treating neuroendocrine tumours. Curr Opin Endocrinol Diabetes Obes. 2012;19:306–13.
Acknowledgment
We thank William Russell-Edu for his assistance in reviewing the English of this text. This work was supported by the Italian Association for Neuroendocrine Tumors (It.A.Net).
Disclosure
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bertani, E., Fazio, N., Radice, D. et al. Resection of the Primary Tumor Followed by Peptide Receptor Radionuclide Therapy as Upfront Strategy for the Treatment of G1–G2 Pancreatic Neuroendocrine Tumors with Unresectable Liver Metastases. Ann Surg Oncol 23 (Suppl 5), 981–989 (2016). https://doi.org/10.1245/s10434-016-5550-3
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-016-5550-3