Abstract
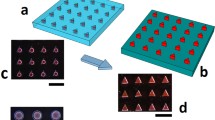
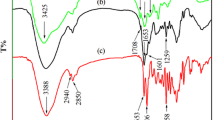
This study optimized conditions for preparing and characterizing gelatin surface modified poly (lactic-co-glycolic acid) (PLGA) copolymer microspheres and determined this systems interaction with fibronectin. Some gelatin microspheres have an affinity for fibronectin-bearing surfaces; these miscrospheres exploit the interaction between gelatin and fibronectin. PLGA copolymer microspheres were selected because they have reproducible and slowrelease characteristics in vivo. The PLGA microspheres were surface modified with gelatin to impart fibronectin recognition. Dexamethasone was incorporated into these microspheres because dexamethasone is beneficial in chronic human diseases associated with extra fibronectin expression (eg, cardiovascular disease, inflammatory disorders, rheumatoid arthritis). The gelatin surface modified PLGA microspheres (prepared by adsorption, conjugation, and spray coating) were investigated and characterized by encapsulation efficiency, particle size, in vitro release, and affinity for fibronectin. The gelatincoated PLGA microspheres had higher interaction with fibronectin compared with the other gelatin surface modified PLGA microspheres (adsorption and conjugation). Dexamethasone was released slowly (over 21 days) from gelatin surface modified PLGA microspheres.
Similar content being viewed by others
References
Perrin DA, English JP. Polyglycolide and polylactide. In Domb AJ, Kost J, Wiseman DM, eds. Handbook of Biodegradable Polymers. Amsterdam: Harwood Academic Publishers, 1997:3–25.
Watts PJ, Davies MC, Melia CD. Microencapsulation using emulsification solvent evaporation: an overview of techniques and applications. Crit Rev Ther Drug Carrier Syst. 1990;7:235–259.
Anderson JM, Shive MS. Biodegradation and biocompatibility of PLA and PLGA microspheres. Adv Drug Deliv Rev. 1997;28:5–24.
Leach KJ. Cancer, drug delivery to treat-local & systemic. In Mathiowitz E. ed Encyclopedia of Controlled Drug Delivery. Vol 1. New York: John Wiley & Sons, 1999:119–142.
Scholes PD, Coombes AGA, Davies MC, Illum I, Davis SS. Particle engineering of biodegradable colloids for site-specific drug delivery. In: Park K, ed. Controlled Drug Delivery. Challenges and Strategies. Washington, DC: American Chemical Society, 1997:73–106
Stolnik S, Dunn SE, Garnett MC, et al. Surface modification of poly(lactide-coglycolide) nanospheres by biodegradable poly(lactide)-poly(ethylene glycol) copolymers. Phann Res. 1994;11:1800–1808.
Groves MJ. Parenteral drug delivery systems. In Mathiowitz E, ed. Encyclopedia of Controlled Drug Delivery: Vol 1. New York: John Wiley & Sons, 1999;743–777
Lou Y, Olson WP, Tian XX, Klegeman ME, Groves MJ. Interaction between fibronectin-bearing surfaces and Bacillus Calmette-Guerm (BCG) or gelatin microparticles. J Pharm Phaumacol, 1995;47:177–181.
Colvin RB. Fibronectin in wound healing. In: Mosher DF, ed. Fibronectin, San Diego: Academic Press, 1989:201–218.
Carsons S, Lavietes BB, Diamond HS. Role of fibronectin in rheumatic diseases. In: Mosher DF, ed. Fibronectin. San Diego: Academic Press. 1990:218–145
Hynes RO. Fibronectins. New York: Springer-Verlag; 1990:113–145.
Thompson PN, Cho E, Blumenstock FA, Shah DM, Saba TM. Rebound elevation of fibronectin after tissue injury and ischemia: role of fibronectin synthesis. Am J Physiol. 1992;263 (4 Pt 1);G437-G445.
Tsung M, Burgess DJ, Preparation and characterization of heparin/gelatin microspheres. Submitted to J Pharm Pharmacol. 2001.
Dev V, Eigler N, Fishbein MC, et al. Sustained local drug delivery to the arterial wall via biodegradable microspheres. Cathet Cardiovasc Diagn. 1997;41:324–332.
Labhasetwar V, Song C, Levy RJ. Nanoparticle drug delivery system for restenosis. Adv Drug Deliv Reviews. 1997;24:63–85.
Humphreya WR, Ericksona LA, Simmonsa CA, et al. The effect of intramural delivery of polyneric nanoparticles loaded with the antiproliferative 2-aminochromone U-86983 on neointimal hyperplasia development in balloon-injured porcine coronary arteries. Adv Drug Deliv Rev. 1997;24:87–108.
Bodmeier R, McGinity JW. Solvent selection in the preparation of poly(DL-lactide) microspheres prepared by the solvent evaporation method. Int J Pharm 1988;43:179–186.
Cohen EM. Dexamethasone [9□-fluoro-11 □. 17□. 21-trihydroxy-16□-methyl pregna-1, 4-diene-3, 20-dione]. Anal Profiles Drug Subst. 1973;2:163–197.
Tsung M, Burgess DJ. Preparation and stabilization of heparin/gelatin complex coacervate microcapsules. J Pharm Sci. 1997;86:603–607.
Lamiable D, Vistelle R, Millart H, et al. High-performance liquid chromatographic determination of dexamethasone in human plasma. J Chromatogr. 1986;378:486–491.
Calis S, Jeyanthi R, Tsai T, Mehta RC, DeLuca PP. Adsoption of salmon calcitoninto PLGA microspheres. Pharm Res. 1995;12:1072–1076.
Rouzes C, Gref R, Leonard M, Delgado AD, Dellacherie E. Surface modification of poly(lactic acid) nanospheres using hydrophobically modified dextrans as stabilizers in an o/w emulsion/evaporation technique. J Biomed Materials Res. 2000;50:557–565.
Nam YS, Song SH, Choi JY, Park TA. Lysozyme microencapsulation within biodegradable PLGA microspheres: urea effect on protein release and stability. Biotechnol Bioengineering. 2000;70:270–277.
Kim TA, Burgess DJ. Formulation and release characteristics of poly(lactic-co-glycolic acid) microspheres containing chemically modified protein. J Pharm Pharmacol. 2001;53:23–31.
Author information
Authors and Affiliations
Corresponding author
Additional information
Published: May 1, 2001.
Rights and permissions
About this article
Cite this article
Jamie Tsung, M., Burgess, D.J. Preparation and characterization of gelatin surface modified PLGA microspheres. AAPS PharmSci 3, 11 (2001). https://doi.org/10.1208/ps030211
Received:
Accepted:
Published:
DOI: https://doi.org/10.1208/ps030211