Abstract
Objective
Stroke is a significant cause of disability, rendering patients with inability to perform activities of daily living due to lack of functional recovery. Precise prognosis in the early stage after stroke could enable realistic goal-setting and efficient resource allocation. Prediction algorithms have been tested and validated in the past, but they were using neurological biomarkers; thus, they were time-consuming, difficult to apply, expensive, and potentially harmful. The aim of this study was to create a new prediction algorithm that would not utilize any biomarkers.
Methods
A total of 127 stroke patients prospectively enrolled at day 3 after their stroke (mean age: 71, males n: 84, females n: 43). First, a sum of shoulder abduction and finger extension (SAFE) Medical Research Council (MRC) score was graded at day 3. Secondly, a binarized response was marked by the Mobilization and Simulation of Neuromuscular Tissue (MaSoNT) concept’s basic application on the upper limb. Third, the National Institutes of Health Stroke Scale (NIHSS) score was assessed. All data from the patients were included in a Classification and Regression Tree analysis to predict upper limb function 3 months post-stroke according to the Action Research Arm Test score at week 12.
Results
The Classification And Regression Tree (CART) analysis was performed that combines three different scores in order to predict upper-limb recovery: the SAFE score, MaSoNT’s application response, and the NIHSS. The overall correct prediction of the new algorithm is 69% which is lower than previous algorithms, though not significantly.
Conclusion
This study offers basic data to support the validity of the APRAHL algorithm. The new algorithm is faster and easier, but less accurate. Future studies are needed to create new algorithms that do not involve neurological biomarkers so that they will cost less and be easily applicable by health professionals.
Similar content being viewed by others
Introduction
Stroke is the second commonest death cause worldwide and the third commonest reason for long-term disability in adults in developed countries [1]. A main issue that stroke patients present is upper-limb motor impairment that severely affects their activities of daily living [2] and renders difficulties to live independently [3].
There are significant variables among individuals that affect a prediction on the time course of rehabilitation post-stroke [4], such as genetics, like the brain-derived neurotrophic factor gene and its key role to induce synaptic plasticity in the cortex [5], as well as the extent of motor impairment where severe motor impairment strongly lowers the chances of acquiring higher levels of recovery [6]. Low degree of sensorimotor deficits as well as the absence of spasticity early after stroke indicates that the patient will probably not be seriously affected by spasticity [7,8,9] which has a positive effect on post-stroke recovery [10]. Furthermore, early recovery of synergism [11] along with finger and wrist extension [12] is a good predictor of upper-limb recovery. Generally, an estimation of motor recovery is important as it affects the type and duration of rehabilitation, enables the correct allocation of rehabilitation resources [13], offers realistic goal-setting, allows optimal designing of future clinical trials in stroke recovery, and provides correct information to patients and relatives [14] which, in turn, assists in expectation management [13].
The need to achieve a distinction among stroke patients with non-favorable and favorable recovery prognosis led to the creation of a few computational prediction models (CPMs) [4, 15]. CPMs aim to provide an estimation of a probable outcome which is objective and supplements professional expertise, guidelines, and clinical intuition [16]. However, the vast majority of the CPMs are rarely met in everyday clinical practice as they lack usability and generalizability [16]. To be more specific, some prognostic indicators that have been tested with regard to upper-limb recovery after stroke are as follows: voluntary shoulder abduction and finger extension (SAFE) score [17], neuroimaging through magnetic resonance imaging (MRI) in two studies with low number of participants [18, 19], and neurophysiological assessments through transcranial magnetic stimulation (TMS) [20]. All of the aforementioned had limitations which rendered their predictive value to be low per se and highlighted the necessity for a new prognostic tool in the area of interest [4].
This led to the development of the predicting recovery potential (PREP) algorithm for the hemiparetic upper-limb [13] which is a sequence of measurements conducted in different periods of time post-stroke, starting off with the SAFE score (less than 72 h post-stroke) and then moving on to TMS if the SAFE score was less than 8 and from then to MRI if motor evoked potentials (MEPs) were not present. PREP algorithm managed to alter therapy content and improved therapist confidence and it was combined with a decrease in length of stay for 1 week, along with no negative effects on patient’s outcomes [21]. PREP algorithm drove to innovation out of necessity because, given that no clinical measure or neurological biomarker could accurately predict motor recovery alone, the researchers had to combine [22]. However, the demand for use of the aforementioned biomarkers made it difficult for the algorithm to be used in clinical settings as it was time-consuming and facility-specific, there were economic burdens to its use, and it was tiresome for the patients [22].
As a result, there was a need to modify PREP and this happened a couple of years later with PREP2 algorithm [23] where the clinicians replaced the MRI with the National Institutes of Health Stroke Scale (NIHSS) and, also, considered the age parameter of the patient. The new algorithm was more accurate as it correctly predicted 3 out of 4 stroke patients in contrast to 2 out of 3 actual correct predictions from the PREP algorithm [23]. Moreover, PREP2 was more accessible and efficient, given that the MRI was not necessary and that the TMS was used for only one third of the patients. However, there was still a need for the neurological biomarker of TMS.
With regard to the use of TMS for assessment purposes, it is both very expensive and time-consuming [24]. Moreover, TMS is considered a comparatively safe neurological biomarker with caution being advised when applied in patients with epilepsy or heart diseases (which is a common trigger of ischemic stroke [25]) and contraindicated in those with skull implants [26]. As to epilepsy, it is reported that the number of patients to present seizure after TMS is fewer than 10 in a period of 20 years [27] and another 4 subjects in 10 years where TMS was applied according to safety guidelines [28]. Furthermore, evidence shows that TMS potentially augments the risk of seizures in patients with chronic stroke [29]. Lastly, there is a consensus on other potential side effects of TMS which include syncope, burns from scalp electrodes, paresthesia, transient neuropsychological/cognitive changes, histotoxicity, and structural brain changes [28].
Apart from the TMS application, the PREP2 algorithm presents some other disadvantages. First of all, in the study of the PREP2 algorithm, patients with cognitive or communication impairments were excluded [23]. However, the taxonomy between limited and poor outcome was granted by the National Institutes of Health Stroke Scale (NIHSS). Hence, if the patients had cognitive or communication impairments, the NIHSS would have been useless, given that the NIHSS has a high consideration for cognition [30]. This, also, implies that many more than a third of the patients would have gone through TMS, which does not essentially fix the problem generated from the original PREP algorithm, and that patients would have showed poor outcome more frequently.
Furthermore, both PREP and PREP2 algorithms divide the recovery prognosis into four categories: complete, notable, limited, and none [13, 23]. First of all, it must be noted that the formed neural circuits after stroke are always weaker than before stroke [31]. Generally, there is no evidence to support that a stroke patient can reach complete recovery after stroke. Explaining the complete category, authors mentioned it as normal or near-normal [13] and complete or near-complete [23]. This taxonomy, however, underlies some ambiguity because it raises a question about how far away to normal is notable and ends being near-normal or how close to near-normal becomes considered as normal, seizing to be notable. This renders the classification unsuccinct.
These limitations created the necessity for a new prognosis tool that does not make use of any biomarker, has succinct classification, and could be used for patients with cognitive or communication impairments. Hence, the Alternative Prognosis of Recovery Assessment for the Hemiparetic Limb (APRAHL) was envisioned. The initial goal of the tool was to preclude the time-consuming expensive biomarkers and offer a fast approach to assess upper-limb prognosis. The APRAHL tool was originally mentioned in a premature stage [32], though no research was conducted on a holistic systematic approach in a form of an algorithm.
As originally mentioned, APRAHL would eliminate biomarkers in general, by using the basic facilitatory technique of Mobilization and Stimulation of Neuromuscular Tissue (MaSoNT) that is applied on the extensors’ muscle group of the upper limb [32]. The rationale was not to substitute TMS with MaSoNT, but to create a new algorithm with no need of biomarkers.
To be more descriptive on the application procedure, for MaSoNT’s basic application on the upper limb, the therapist initially brings the thumb over the extensor’s muscle belly and grips the lower surface of the forearm with the other hand, keeping the patient’s hand in a relaxed position and giving it clearance to move (Fig. 1). Afterwards, the therapist turns the thumb across the attached muscle belly, offering a bit of compression along the way (Fig. 2) [32]. When applying the basic technique of MaSoNT for the extensor’s muscle group of the hand, the response should be a muscular jerk [32]. This aspect of MASONT has never been further explored.
The aim of this study was to create a new biomarker-free prognosis tool in terms of the function of the upper limb and check its algorithm with regard to accuracy by comparing the patient stratification predicted by a newly formed APRAHL’s algorithm with the stratification produced by an unbiased cluster analysis of upper limb function.
Methodology
Procedures
SAFE score was assessed by grading shoulder abduction and finger extension of the hemiplegic upper limb using the Medical Rating Council (MRC) grades at day 3 after stroke symptom onset. MRC scores for both the aforementioned movements were summed in order to obtain a score range out of 10. The Fugl-Meyer assessment for the upper extremity (FMA-UE) [33] scores were obtained at day 3 and month 3. The Action Research Arm Test (ARAT) [34] assessments provided the primary outcome and its score was obtained at day 3 and month 3 after stroke. All assessments were conducted by an experienced clinical assessor who was a physiotherapist, blinded towards the algorithm of the prognosis tool and uninvolved in patient care. All patients received standard upper-limb rehabilitation care. Therapy dose was standardized and recorded for every session by both the physical and occupational therapist, meaning that each profession offered the same standard upper-limb treatment in the same time duration and no patient was favored in terms of treatment.
Analysis
A hypothesis-free cluster analysis of ARAT scores at 3 months post-stroke was performed, to re-assess the limits between the four outcome categories of Very Good, Good, Limited, and Poor upper limb outcome, which replaced the previous category labels [13, 23]. Classification of each subject was conducted into one of the four aforementioned outcomes based on their ARAT score at 3 months. A Classification and Regression Tree (CART) analysis was performed by using the IBM SPSS (version 24) to decide which factors best predict the outcome category. A decision tree is generated by the CART analysis and the variables to include, or their order, in the tree, is not determined by the user. This method offers some rigor to the study given that there were no a priori assumptions made about the likely sequence or type of predictors that were included in the resulting decision tree.
The clinical variables and demographic for the CART analysis were the SAFE score [17], hemisphere affected (left, right), upper limb impairment (FMA-UE score), hand affected (dominant, nondominant), intravenous thrombolysis (yes, no), sex, basic MaSoNT’s applications for the hemiplegic upper-limb (response, poor or no response), stroke classification (lacunar infarct, partial anterior circulation infarct, total anterior circulation infarct, posterior circulation infarct, intracerebral hemorrhage), stroke severity (NIHSS score), and upper limb therapy dose (minutes).
Maximum tree depth of the CART analysis was predetermined to be 3, following the rationale of the PREP2 algorithm. The CART analysis, also, had a minimum terminal node size of 10 cases, as well as, an automated pruning in order to prevent over-fitting which had a maximum difference in risk of 1 standard error. Homogeneity within the terminal nodes was enhanced by using “Gini”. CART analyses’ results were recomposed and integrated in order to generate the APRAHL algorithm.
Results
Subjects
The subjects of this study were patients with ischemic stroke that were prospectively enrolled at day 1 after the CVA from a single rehabilitation clinic. Inclusion criteria for the patients were to be aged over 18 years old, their stroke to be their first-ever and to have upper-limb hemiplegia or hemiparesis within 72 h after stroke. Patients were excluded if they were diagnosed with hemianopia as MaSoNT’s application offers an advantage to those without hemianopia. Furthermore, patients were excluded if they resided outside the clinic which precluded a follow-up and if they were aged above 80 years old as that is the main age point where age significantly interferes with upper-limb recovery prediction in stroke patients [23]. Other exclusion criteria were recurrent stroke, pregnancy, history of seizures for safety reasons, and pre-existing conditions that preclude compliance or informed consent.
Localization and type of stroke were determined using CT or MRI scans earlier before commencing the study. The study was conducted in Evexia Rehabilitation Clinic, Thessaloniki, Greece. Regional ethics committee approved the study. All participants signed written informed consent according to the Declaration of Helsinki. Patients’ baseline characteristics are provided in Table 1.
Cluster analysis
The cluster analysis recognized four outcome groups that did not overlap with each other (Table 2). The cluster limits relate to those found in previous studies [13, 23].
CART analysis
A decision tree was determined by the CART analysis with the SAFE score being the first decision point and then the MaSoNT’s application response and the NIHSS (Table 2). Overall prediction accuracy was 69%. For patients with SAFE score of 8 and more, the overall prediction accuracy was 76%, while for those with less than 8, the overall prediction accuracy was 66% (Table 3). Given that the prediction accuracy among FMA-UE and SAFE score was the same, and the SAFE score is quicker and more easily implemented in clinical practice, a decision was made via vote by the researchers to keep the SAFE score in the algorithm. Alternate CART analyses were performed for patients who scored above or equal 8 and for those who scored under 8 (Fig. 3).
CART analysis for patients who had SAFE score under 8 at day 3 after stroke. + MaSoNT response stands for the vivid contraction in a full range of motion that is elicited by applying the basic upper-limb technique. − MaSoNT response stands for poor or no response elicited. The CART analysis selected the NIHSS in order to differentiate between the − MaSoNT response patients who will present limited against those with poor recovery outcome
CART analysis found that if MaSoNT’s application produced a vivid response, the patient might have a good recovery, though with medium positive predictive value (PPV) (63%) as well as negative predictive value (56%). However, if there was no response to MaSoNT’s application, the patient will have limited or poor recovery. The CART analysis selected the NIHSS for those patients who scored under 8 in the SAFE score and did not produce a vivid response upon the application of MaSoNT’s basic technique. For these patients, the CART analysis found that patients with NIHSS under 8 might have some limited recovery, whereas patients with NIHSS of 8 and above will almost definitely have poor recovery (PPV = 98%, NPV = 99%).
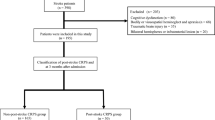
The potential predictors that the CART analysis did not select were previous stroke, sex, hand dominance, hand affected, intravenous thrombolysis, hemisphere affected, and stroke Bamford classification. A CONSORT [35] flowchart of the study was narrowly created (Fig. 4). Used for prediction model development specifically, the Tripod Checklist is also provided in Additional file 1.
The decision tree produced by the CART analyses was recomposed and the APRAHL algorithm was generated, an algorithm without any neurological biomarkers, which is time-saving and easy-to-use by the clinicians in order to make predictions upon the recovery of each patient (Fig. 5). The description as well as the rehabilitation focus resembles the ones from previous algorithms [13, 23] (Table. 4).
The APRAHL algorithm for the hemiplegic upper-limb prognosis. SAFE, sum of the shoulder abduction and finger extension Medical Rating Council muscle grades at day 3 after stroke; MaSoNT, Mobilization and Stimulation of Neuromuscular Tissue; NIHSS, National Institutes of Health Stroke Scale. The test starts at day 3 after stroke. The patient is categorized according to the SAFE score to very good recovery if the score is above or equal to 8. If the SAFE score is lower than 8, the basic technique of MaSoNT is applied on the extensors’ muscle group of the upper limb at day 3. The therapist, then, assesses the elicited brisk muscular contraction which is triggered as a response to that stimulation. If the response is a vivid muscular contraction in a large range of motion, the prognosis is good. If there is no response or if the response is narrow or subtle or takes more than three applications to elicit, the prognosis is limited if the NIHSS is under 8 and poor if the NIHSS is over 8
Discussion
The APRAHL prognosis algorithm appears to be accurate, easily accessible, and efficient. Even though its overall prognosis accuracy is slightly lower than the PREP2 algorithm [23], the complete lack of a neurological biomarker offers an important advantage. Noteworthy, the overall prognosis accuracy is lower than the PREP2 algorithm but this difference is only statistically important and it does not reflect negatively on clinical practice. To binarize the response of MaSoNT’s basic application in order to replace the biomarker is a new predictor identified by the CART analyses.
Another important point, judging by the PPV and NPV (Table 3), is that in case the basic MaSoNT’s application showed no response at day 3, combined with an NIHSS score equal or over 8, the patient’s recovery is almost certainly poor. This was fathomed when the idea to implement MaSoNT in prognosis was arbitrarily conceived in the beginning [32]. That is, if the application does not elicit a response on the upper limb at day 3, this must be due to spasticity development or contracture. Spasticity may appear as early as 2 weeks after stroke in a patient’s life [7] and its prevalence increases at 3 [36] and 6 [37] weeks after stroke. However, if there is low degree of motor and sensory deficit as well as absence of spasticity at the early stage, the patient probably will not be seriously affected by spasticity [7, 37, 38]. Hypothetically, the binarized MaSoNT’s basic application response could be a prognosis tool for spasticity at any time after stroke, but this remains to be researched in future studies.
Apart from the aforementioned, it is very important to highlight the value of the SAFE score. A simple bedside strength test of shoulder abduction and finger extension discriminated 80% accuracy between patients with Very Good and Good recovery at 3 months post-stroke. Its significance lies on the capability of the SAFE score in correlation with its simplicity and time-saving proprieties.
Several other studies have used clinical assessments alone in order to predict outcomes for the hemiplegic upper limb [14, 15, 39]. Another study performed the Fugl-Meyer scale and Motricity Index on day 2 after stroke predicting 6 months post-stroke [17]. Additionally, there was a study that used two items from the ARAT on day 3 in order to predict the Fugl-Meyer scale score in 12 months after stroke [40]. However, their predictions were dichotomized, vague, unexplored in clinical practice, and not offering enough details with regard to specific treatment planning. Additionally, both 6 months and a year after stroke is too long a time period to be able to predict every possible factor that could affect or restrict rehabilitation perspectives such as pain or spasticity. In contrary, APRAHL prognosis algorithm predicts with 69% accuracy for every stroke patient in 3 months after stroke, without any need for neurological biomarkers.
APRAHL was designed based on previous studies [23] which showed that their implementation could be useful in clinical practice. Previous algorithms [13] were validated and proved to be able to augment rehabilitation efficiency. Similarly to the previous algorithms [13, 23], APRAHL could be used for the stratification and selection of randomized clinical trials for early treatment approaches on the hemiplegic upper limb, assuring homogeneity within the groups, avoiding possible mismatch between the treatment groups and/or the control group and improving a trial’s sensitivity upon possible treatment effects.
Implementing APRAHL is free of cost and is not time-consuming, and it can be used at any clinical environment without difficulties as it is simple and easy to be used by health care professionals. It classifies the patient’s prognosis level at four different categories, which is similar to PREP [13] and PREP2 algorithm [23]. Additionally, it could be used on patients with more severe cognitive or mental impairments, highlighting that, in case the patient cannot perform the SAFE score, the patient moves to the below 8 SAFE score category of the algorithm.
Following the suggestion of PREP [13] and PREP2 algorithm [23], APRAHL helps practically as it directs patients’ and therapists’ expectations, aids correct goal setting, adequately organizes a treatment plan, and also, better guides the team allocation in clinical trials with stroke survivors in the future in order to accomplish homogeneity.
A limitation of the study is that there was no consideration with regard to the patients of 80 years old and above as well as younger than 52. The entire algorithm could be different in that case. Future studies could further investigate on that matter. Another important factor that neither APRAHL nor PREP2 considered is the factor of pain. Pain is highly prevalent for stroke patients at least 6 months after stroke [41]. Pain could affect recovery and alter treatment goals. The same applies to spasticity as well [7, 36,37,38]. Additionally, further subjects in many different clinical settings could offer a more generalizable conclusion and validate APRAHL. Lastly, a disadvantage of APRAHL is that the description of the response from MaSoNT’s application may be somewhat confusing for the unexperienced therapist. Even though MaSoNT’s basic application for the upper limb is simple, the therapist must conduct some research to comprehend the correct application procedure. Apart from that, APRAHL seems to be a very easy-to-use prognosis tool.
Future studies could focus on APRAHL, considering other factors as well, such as pain, spasticity, visual ability, and sensation. The hemiparetic foot could, also, lack proper sensation and a new possible algorithm could implement several other factors apart from sensation in order to offer specific predictions and—consequently—specific treatment goals and planning.
Conclusion
The newly designed algorithm of APRAHL seems to offer accurate prediction of recovery after stroke in a fast and easy approach. This major advantage is granted by the fact that APRAHL does not implement any neurological biomarkers. Limitations arose in the study and new studies on larger population in multi-site clinical settings are mandatory to validate the APRAHL algorithm. Future studies could rearrange the algorithm in order to consider other factors that could affect the prediction and were omitted in this study.
Abbreviations
- APRAHL:
-
Alternative Prognosis of Recovery Assessment for the Hemiparetic Limb
- ARAT:
-
Action Research Arm Test
- CART:
-
Classification and regression tree
- MaSoNT:
-
Mobilization and Stimulation of Neuromuscular Tissue
- MEP:
-
Motor evoked potentials
- MRC:
-
Medical Rating Council
- MRI:
-
Magnetic resonance imaging
- NIHSS:
-
National Institutes of Health Stroke Scale
- PREP:
-
Predicting recovery potential
- SAFE:
-
Shoulder abduction and finger extension
- TMS:
-
Transcranial magnetic stimulation
- FMA-UE:
-
Fugl-Meyer assessment for the upper extremity
References
World Health Report. Geneva. Switzerland: World Health Organization; 2003.
Dromerick AW, Lang CE, Birkenmeier R, Hahn MG, Sahrmann SA, Edwards DF. Relationships between upper-limb functional limitation and self-reported disability 3 months after stroke. J Rehabil Res Dev. 2006;43(3):401–8.
Schiemanck SK, Kwakkel G, Post MWM, Kappelle LJ, Prevo AJH. Predicting long-term independency in activities of daily living after middle cerebral artery stroke: does information from MRI have added predictive value compared with clinical information?: Does information from MRI have added predictive value compared with clinical information? Stroke. 2006;37(4):1050–4.
Stinear C. Prediction of recovery of motor function after stroke. Lancet Neurol. 2010;9(12):1228–32.
Antal A, Chaieb L, Moliadze V, Monte-Silva K, Poreisz C, Thirugnanasambandam N, et al. Brain-derived neurotrophic factor (BDNF) gene polymorphisms shape cortical plasticity in humans. Brain Stimul. 2010;3(4):230–7.
Patel AT, Duncan PW, Lai SM, Studenski S. The relation between impairments and functional outcomes poststroke. Arch Phys Med Rehabil. 2000;81(10):1357–63.
Wissel J, Schelosky LD, Scott J, Christe W, Faiss JH, Mueller J. Early development of spasticity following stroke: a prospective, observational trial. J Neurol. 2010;257(7):1067–72.
Urban PP, Wolf T, Uebele M, Marx JJ, Vogt T, Stoeter P, et al. Occurence and clinical predictors of spasticity after ischemic stroke. Stroke. 2010;41(9):2016–20.
Sommerfeld DK, Gripenstedt U, Welmer A-K. Spasticity after stroke: An overview of prevalence, test instruments, and treatments. Am J Phys Med Rehabil. 2012;91(9):814–20.
K Monaghan F Horgan C Blake C Cornall PPM Hickey BE Lyons Physical treatment interventions for managing spasticity after stroke. The Cochrane Database of Systematic Reviews [Internet]. et al 2017 [cited 2022 Jul 29];2017(2) Available from: https://doi.org/10.1002/14651858.CD009188.pub2
Kwakkel G, Kollen BJ, van der Grond J, Prevo AJH. Probability of regaining dexterity in the flaccid upper limb: impact of severity of paresis and time since onset in acute stroke: Impact of severity of paresis and time since onset in acute stroke. Stroke. 2003;34(9):2181–6.
Kwakkel G, Kollen B. Predicting improvement in the upper paretic limb after stroke: a longitudinal prospective study. Restor Neurol Neurosci. 2007;25(5–6):453–60.
Stinear CM, Barber PA, Petoe M, Anwar S, Byblow WD. The PREP algorithm predicts potential for upper limb recovery after stroke. Brain. 2012;135(Pt 8):2527–35.
Veerbeek JM, Kwakkel G, van Wegen EEH, Ket JCF, Heymans MW. Early prediction of outcome of activities of daily living after stroke: a systematic review: a systematic review. Stroke. 2011;42(5):1482–8.
Coupar F, Pollock A, Rowe P, Weir C, Langhorne P. Predictors of upper limb recovery after stroke: a systematic review and meta-analysis. Clin Rehabil. 2012;26(4):291–313.
Nijland RHM, van Wegen EEH, Harmeling-van der Wel BC, Kwakkel G. Prediction of Functional Outcome After Stroke Investigators. Accuracy of physical therapists’ early predictions of upper-limb function in hospital stroke units: the EPOS Study. Phys Ther. 2013;93(4):460–9.
Nijland RHM, van Wegen EEH, Harmeling-van der Wel BC, Kwakkel G. EPOS Investigators. Presence of finger extension and shoulder abduction within 72 hours after stroke predicts functional recovery: early prediction of functional outcome after stroke: the EPOS cohort study: Early prediction of functional outcome after stroke: The EPOS cohort study. Stroke. 2010;41(4):745–50.
DeVetten G, Coutts SB, Hill MD, Goyal M, Eesa M, O’Brien B, et al. Acute corticospinal tract Wallerian degeneration is associated with stroke outcome. Stroke. 2010;41(4):751–6.
Marshall RS, Zarahn E, Alon L, Minzer B, Lazar RM, Krakauer JW. Early imaging correlates of subsequent motor recovery after stroke. Ann Neurol. 2009;65(5):596–602.
Di Lazzaro V, Profice P, Pilato F, Capone F, Ranieri F, Pasqualetti P, et al. Motor cortex plasticity predicts recovery in acute stroke. Cereb Cortex. 2010;20(7):1523–8.
Stinear CM, Byblow WD, Ackerley SJ, Barber PA, Smith M-C. Predicting recovery potential for individual stroke patients increases rehabilitation efficiency. Stroke. 2017;48(4):1011–9.
Kim B, Winstein C. Can neurological biomarkers of brain impairment be used to predict poststroke motor recovery? A systematic review. Neurorehabil Neural Repair. 2017;31(1):3–24.
Stinear CM, Byblow WD, Ackerley SJ, Smith M-C, Borges VM, Barber PA. PREP2: A biomarker-based algorithm for predicting upper limb function after stroke. Ann Clin Transl Neurol. 2017;4(11):811–20.
Beam W, Borckardt JJ, Reeves ST, George MS. An efficient and accurate new method for locating the F3 position for prefrontal TMS applications. Brain Stimul. 2009;2(1):50–4.
Bartels MN, Duffy CA, Beland HE. Pathophysiology, medical management, and acute rehabilitation of stroke survivors. In: Stroke Rehabilitation. Elsevier; 2016. p. 2–45.
Pearce-Hughes S, Trout R. Transcranial magnetic stimulation and navigated brain thereapy. Br J Neurosci Nurs. 2017;13(1):44–5.
Rossini PM, Rossi S. Transcranial magnetic stimulation: diagnostic, therapeutic, and research potential. Neurology. 2007;68(7):484–8.
Rossi S, Hallett M, Rossini PM, Pascual-Leone A. Safety, ethical considerations, and application guidelines for the use of transcranial magnetic stimulation in clinical practice and research. Clin Neurophysiol. 2009;120(12):2008–39.
Lomarev MP, Kim DY, Richardson SP, Voller B, Hallett M. Safety study of high-frequency transcranial magnetic stimulation in patients with chronic stroke. Clin Neurophysiol. 2007;118(9):2072–5.
Kelly-Hayes M, Robertson JT, Broderick JP, Duncan PW, Hershey LA, Roth EJ, et al. The American Heart Association Stroke Outcome Classification: executive summary. Circulation. 1998;97(24):2474–8.
Robertson IH, Murre JMJ. Rehabilitation of brain damage: brain plasticity and principles of guided recovery. Psychol Bull. 1999;125(5):544–75.
Athanasiadis D, Dionyssiotis Y, Papathanasiou J, Stefas E. Mobilization and Stimulation of Neuromuscular Tissue (MASONT) for stroke survivors. Folia Med (Plovdiv) [Internet]. 2018 [cited 2022 Jul 29];60(1):158–63. Available from: https://pubmed.ncbi.nlm.nih.gov/29668461/
Kasner SE. Clinical interpretation and use of stroke scales. Lancet Neurol. 2006;5(7):603–12.
Van der Lee JH, De Groot V, Beckerman H, Wagenaar RC, Lankhorst GJ, Bouter LM. The intra- and interrater reliability of the action research arm test: a practical test of upper extremity function in patients with stroke. Arch Phys Med Rehabil. 2001;82(1):14–9.
Schulz KF, Altman DG, Moher D, Consort Group. CONSORT 2010 Statement: updated guidelines for reporting parallel group randomised trials (Chinese version). Zhong Xi Yi Jie He Xue Bao [Internet]. 2010;8(7):604–12. Available from: https://europepmc.org/article/med/20619135
Sommerfeld DK, Eek EU-B, Svensson A-K, Holmqvist LW, von Arbin MH. Spasticity after stroke: Its occurrence and association with motor impairments and activity limitations. Stroke. 2004;35(1):134–9.
Urban PP, Wolf T, Uebele M, Marx JJ, Vogt T, Stoeter P, et al. Occurence and clinical predictors of spasticity after ischemic stroke. Stroke. 2010;41(9):2016–20.
Sommerfeld DK, Gripenstedt U, Welmer A-K. Spasticity after stroke: an overview of prevalence, test instruments, and treatments. Am J Phys Med Rehabil. 2012;91(9):814–20.
Nijland RHM, van Wegen EEH, Harmeling-van der Wel BC, Kwakkel G, Early Prediction of Functional Outcome After Stroke Investigators. Accuracy of physical therapists’ early predictions of upper-limb function in hospital stroke units: the EPOS Study. Phys Ther [Internet]. 2013 [cited 2022 Jul 29];93(4):460–9. Available from: https://academic.oup.com/ptj/article/93/4/460/2735324
Persson HC, Alt Murphy M, Danielsson A, Lundgren-Nilsson Å, Sunnerhagen KS. A cohort study investigating a simple, early assessment to predict upper extremity function after stroke - a part of the SALGOT study. BMC Neurol. 2015;15(1):92.
Hansen AP, Marcussen NS, Klit H, Andersen G, Finnerup NB, Jensen TS. Pain following stroke: a prospective study: Post-stroke pain. Eur J Pain. 2012;16(8):1128–36.
Author information
Authors and Affiliations
Contributions
The authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Athanasiadis, D., Stefas, E. & Protopsaltis, S. Alternative prognosis of recovery assessment for the hemiparetic limb (APRAHL): a biomarker-free algorithm that predicts recovery potential for stroke patients. Bull Fac Phys Ther 27, 47 (2022). https://doi.org/10.1186/s43161-022-00106-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s43161-022-00106-7