Abstract
Background
Abnormalities of the cardiovascular system are the most common congenital diseases in the fetus and the first cause of infant mortality. Echocardiography is still the method of choice to visualize the fetal cardiac cardiovascular abnormalities, yet cardiovascular magnetic resonance (CMR) is relatively unaffected by maternal and fetal conditions such as maternal obesity, uterine myoma, twins, oligohydramnios, fetal position and rib calcification, which particularly impair sonographic visualization of the fetal heart. Fetal cardiac MR imaging is a novel MRI technique which can provide valuable information that could add to the prenatal diagnosis and evaluation of cardiac and most of extra-cardiac anomalies. In this work, we aimed to highlight the advantage of FCMRI over fetal echocardiography in assessment of fetal congenital cardiac anomalies.
Results
Fifty-Two fetuses with suspected or diagnosed congenital cardiac anomalies. All cases underwent detailed history taking, underwent fetal echocardiography using suitable curvilinear probe and performed according to standard protocol, then fetal cardiac MR was done with Balanced fast field echo, Black blood single shot, white blood Cine, Real-time 3D dynamic sequences, images were acquired in the transverse, four-chamber, short-axis, coronal and oblique sagittal views. Findings of fetal echocardiography were compared with that of cardiac MRI and with standard post-natal echocardiography. Prenatal Echo and fetal cardiac MRI showed significant moderate agreement between the two modalities in the detection of different congenital cardiac anomalies, Kappa test: 0.500; p value 0.021. Fetal MRI had a significant role in detection of extra cardiac anomalies in most cases. Comparing to gold standard post-natal echo. Accuracy of fetal CMRI is 95.5% and of fetal Echo is 86.4% regarding overall cardiac anomalies:
Conclusion
Fetal cardiac MR imaging as an adjunct to fetal echocardiography may provide valuable information that could add to the prenatal diagnosis and evaluation of cardiac and most of extra cardiac anomalies.
Similar content being viewed by others
Introduction
Abnormalities of the cardiovascular system are the most common congenital diseases in the fetus and the first cause of infant mortality [1].
Although fetal echocardiography has been used successfully for many years in the diagnosis of fetal congenital cardiovascular abnormalities, there is a need at times for additional information without limitation to the acoustic windows [2].
The role of fetal cardiovascular magnetic resonance (FCMR) as a tool additional to ultrasound has grown exponentially. Unlike fetal echocardiography imaging, cardiovascular magnetic resonance (CMR) is relatively unaffected by maternal and fetal conditions such as maternal obesity, uterine myoma, twins, oligohydramnios, fetal position and rib calcification, which particularly impair sonographic visualization of the fetal heart and great vessels [3].
Without a doubt, Echocardiography is the method of choice to visualize the fetal cardiovascular abnormalities, FCMR imaging has the potential to complement ultrasound in detecting cardiovascular malformations and extra cardiac anomalies [3, 4]. It has been reported that echo cannot be replaced by MRI but, it really can provide some additional important information in fetal CHD [5].
Aim of the work
To highlight the advantage of FCMRI over fetal echocardiography in assessment of fetal congenital cardiac anomalies.
Methods
A diagnostic prospective study is approved by The Ethical Committee of the Department of diagnostic radiology, Faculty of Medicine and the review board of University Hospital. All patients provided informed consent for the MR imaging examinations and for inclusion of their data in this analysis.
From November 2019 to April 2021, Fifty-Two cases were included in our study, their age ranged from 20 to 39 years. The study included all pregnant females suspected or diagnosed with fetal congenital cardiac anomalies by routine obstetrics or fetal echocardiography, high-risk pregnant females with gestational diabetes mellites (GDM), hypertension(HTN), consanguinity, and history of previously baby with CHD all are included. Subject refuses to participate in the research and subject with contraindication to MRI as having any non-compatible metallic implants like pacemaker, aneurysm clips, joint replacement or any other electronic or magnetically activated implants as well as claustrophobic are excluded from the study.
Written consent was taken from all participates before recruitment in the study after explanation of the purpose and procedures of the study.
All included patients were subjected to careful full history taking including age, consanguinity, previous history of anomalies, or any systemic disease. Followed by obstetric sonography performed between 22 and 28 weeks of gestation by Radiologist for all cases using suitable curvilinear probe of logic GE P9, S8 machine (GE Medical System, Austria), Full basic obstetric biometry was taken included biparietal diameter (BPD), head circumference (HC), abdominal circumference (AC), femur length (FL), estimated fetal weight (EFW), amniotic fluid index (AFI) with middle cerebral artery (MCA) and umbilical artery (UMA) Doppler parameter. Fetal echocardiography by which basic obstetrics measures and detailed cardiac examination was done by more than 20 years experienced Pediatric Cardiologist and more than 7 years experienced Radiologist for around 30–45 min scan time per case. With assessment of standard and extended cardiac views for diagnosis of various congenital heart malformation according to standard protocol starting with cardiothoracic ratio and cardiac axis, systematic evaluation of the following views: four chambers, left ventricular outflow tract, right ventricular outflow tract, three-vessel trachea, short axis views, long axis view, aortic arch, ductal arch, superior and inferior vena cava. After that scheduled FCMRI was performed using 1.5 Tesla Philips machine (ingenia medical system Eindhoven, Netherland) with no specific preparation of the patients except for preferring early morning scan time. The following MRI pulse sequences were included: SURVEY-BFFE. Coronal, axial and sagittal uterus BTFE. SSh-cine-SA-M2D (4 chamber and short axis views). Black blood -SSH-BH (4 chamber and short axis views). White blood Cine (Coronal, axial and sagittal) Detailed sequences parameters are presented in Table 1.
Post-acquisition images evaluation done by same radiologist who did obstetric US and shared in prenatal echo examination using PACS viewing system and interpretation by post processing software Philips workstation and compared to resulted findings of fetal echocardiography and correlated with gold standard post-natal echocardiography done by same pediatric cardiologist who was share in prenatal echocardiography and was blinded of FCMR finding. Cases with IUFD were recorded for prenatal comparative results only.
Throughout the study, we faced that fetal CMR has been limited due to technical challenges mainly the lack of a fetal ECG for gating. As a consequence of unavailable direct fetal cardiac gating so far, dynamic fetal CMR sequences analysis was dependent on complicated post-processing techniques. Also, maternal exhaustion, as well as unexpected fetal movement, were the main obstacles to obtaining aimed view with satisfactory resolution.
Statistical analysis
Recorded data were analyzed using the statistical package for social sciences, version 20.0 (SPSS Inc., Chicago, Illinois, USA). Quantitative data were expressed as mean ± standard deviation (SD). Qualitative data were expressed as frequency and percentage. The confidence interval was set to 95% and the margin of error accepted was set to 5%. So, the p value was considered significant as the following: P > 0.05: Non-significant, P < 0.05: Significant, P < 0.01: Highly significant.
Results
The study included 52 pregnant females, their age ranged from 20 to 39 years with (30.46 ± 6.81) years mean ± SD, Gestational age ranged from 24 to 39 weeks with (30.81 ± 4.30) weeks mean ± SD, demographic data distribution of basic obstetric and fetal parameters is viewed in Tables 2, 3.
The percentage of first and second degree of consanguinity was high (42.3%), previous history of anomaly (30.8%), and percentage of high-risk disease (GDM, HTN) was (11.5%).
Regarding the diagnostic performance of prenatal Echo and fetal cardiac MRI showed significant moderate agreement between the two modalities in the detection of different congenital cardiac anomalies, Kappa test: 0.500; p value 0.021*, Fig. 1.
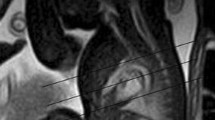
38-years-old pregnant female with 29wks fetus, a, b fetal echo finding; Complete unbalanced AVSD, dilated main pulmonary artery, pulmonary regurge, (c-f) FCMRI finding: Cardiomegaly with large common atrium (white arrow in c), hypoplastic left ventricle with atretic mitral valve and large membranous VSD (green arrow in c), hypoplastic aortic arch (short arrow in d), thickened tricuspid valve(green arow in e),and normal pulmonary venous drainage to small left atrium (two arrows in f). c, e Axial BTFE (110 flip angle) four chambers and outlet views, d, f Black blood sequence
All cardiac structures were delineable by both echocardiography and cardiac MRI. There was full agreement (κ = 1) between fetal echocardiography and cardiac MRI in evaluating the cardiac situs (48 normal, 2 levocardia, 2 ectopia cordis), aorta (40 normal, 6 hypoplastic aorta, 2 aortic stenosis, 2 right-sided aortic arch and 2 small-sized aorta), transverse cardiac diameter (44 normal, 8 cardiomegaly), foramen oval (50 normal, 2 large single atrium), good agreement was found for the position of the cardiac apex (48 normal, 4 abnormal). After exclusion of 18 IUFD cases, percentage agreement of fetal MRI and fetal echo with post-natal echo regarding individual congenital anomaly is presented in Table 4, There was statistically significant higher sensitivity of fetal MRI (95.5%) compared to fetal echo (86.4%) regarding overall anomalies, with p value < 0.001 HS. For detailed sensitivity, positive predictive value, negative predictive value, and accuracy of fetal MRI and fetal echo regarding to individual and overall cardiac anomalies refer to Table 5.
Fetal MRI had a significant role in detection of extra cardiac anomalies in most of cases; congenital diaphragmatic hernia and its contents in 2 cases, anterior abdominal wall defects as omphalocele and its contents in 3 cases, microphthalmia and syndromic correlation in 2 cases. Excluding arteriovenous malformation (AVM) that may cause cardiac overload and right-side dilatation in 1 case, measurement of skull bony defect and differentiate contents of sac either encephalo-meningocele or encephalo-myelomeningocele with corpus callosum hypoplasia in 2 cases. Grading of congenital hydronephrosis and post urethral valve obstruction in 2 cases, confirmation of suspected talipes in1case. Anterior chest wall defect, liver herniation through omphalocele, positional ectopia cordis of the left ventricular (LV) apex, and diaphragmatic hernia in 1 case.
Discussion
Although fetal echocardiography has been used successfully for many years in the diagnosis of fetal congenital cardiovascular abnormalities, there is a need at times for additional information without limitation to the acoustic windows [2]. FCMR avoids exposure to ionizing radiation and no clinical or experimental evidence has indicated that CMR has any adverse effects on the human fetus [3].
The mean gestational age in our studied cases was 30.81 ± 4.30 ranged from 24 to 39 contrary to the results of the study of Tavares de Sousa et al. [6] who mentioned that the mean gestational age at MRI was 34 weeks (range 28 to 36 weeks). Zhu [5] stated that the mean gestational age in their study group was 27 weeks (range 17 to 39 weeks).
Zhu [5] found that 280 cases of CHD including ventricular septal defect (VSD), coarctation of aorta (CoA), interrupted aortic arch (IAA), double aortic arch, tetralogy of fallot (TOF), D type transposition of great arteries (D-TGA), L-TGA, pulmonary atresia (PA)/VSD, double outlet right ventricle (DORV), hypoplastic left ventricle syndrome (HLVS), tricuspid atresia (TA) and others, MRI provided additional important information to fetal echocardiography at 51(18%) cases while in our present study the 52 cases of CHD included VSD, atrial septal defect (ASD), right-sided dilatation, atrioventricular (AV) – ventriculoarterial (VA) discordance, right hypoplastic, HLVS, TGA, right side aortic arch (RAA), and others. MRI provided additional information at 32 cases (61%). Four chamber view still is the most important view. The fetal MR imaging of the transverse view of aortic arch just like the “three vessels view” in fetal echo also is very important [5].
In the present study, there was statistically significant agreement between FCMRI and fetal echo regarding VSD, right hypoplastic ventricle (RHV) & double inlet left ventricle (DILV), (ASD), apparent cardiomegaly, Pericardial effusion, right side dilatation & thick tricuspid valve (TV), AV&VA discordance, TGA & RAA and Ebstien anomaly that agrees with the study done by Tavares de Sousa et al. [6] who stated that There was full agreement (κ = 1) between fetal echocardiography and cardiac MRI in evaluating the cardiac situs, descending aorta, transverse cardiac diameter, foramen ovale, relationship between tricuspid and mitral valve planes and ventricular contraction patterns.
Gorincour et al. [7] added the assessment of ventricular looping by MRI as being possible in all fetuses as well which agreed with our study in a case of positional mesocardia, anterior chest wall defect causing ectopia cordis and small liver herniation with omphalocele Fig. 2. In particular, all the morpho-volumetric abnormalities of the heart and the cardiac chambers as well as the abnormalities of rotation were visualized by direct signs: cardiomegaly through the measurement of a cardio/thorax ratio (C/T ratio) over 1/3; hypoplastic left heart syndrome through the reduction in size of the left chambers; pericardial effusion through the detection of a high signal intensity fluid which agrees with 6 cases of our study.
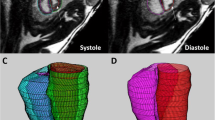
FCMR of 33wks male fetus shows, A sagittal fetal body BTFE (110 flip angle) shows anterior abdominal wall bulge with small omphalocele containing liver tissue (green arrow in A), B cardiac Black blood axial view shows positional mesocardia, C, D axial BTFE show anterior chest wall defect measuring 2.5 cm causing ectopia cordis of cardiac apex (green arrow in D). IUFD was occurred two weeks later
In Manganaro et al. [8] as regards extra cardiac abnormalities, MRI detected a CNS pathology in 6 fetuses, a non-CNS pathology in 13 fetuses which agree with our study which detect extra cardiac anomalies in 15 fetuses (CNS in 4 fetuses, non-CNS in 11 fetuses) Fig. 3.
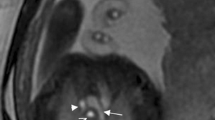
20-years-old pregnant female with 25wks fetus, a, c fetal echo finding; cardiomegaly, VSD, severe tricuspid regurge and abnormal venous drainage between Umbilical vein and azygous vein noted in doppler image (c). d–f FCMRI finding 2 weeks later: SBFFE- 3D short dynamic axial, sagittal and coronal view shows single large inlet VSD thick white arrow in (d), prominent posterior azygous vein (white arrow) with compressed sub diaphragmatic umbilical vein (green arrow) draining into it in (e) hypoplastic pulmonary artery (green arrow in (f). Fetus developed sever hydrops and IUFD was occurred
Saleem [9] study including 20 fetuses concluded that cardiac MRI can be used to determine the cardiac parameters outlined by Gorincour et al. [7], Manganaro et al. [8] which include visceroatrial situs, cardiac position, cardiac size, cardiac axis, cardiac chambers, ventricular looping, inflow veins, outflow vessels, ventriculoarterial concordance, side of the aortic arch and all cardiac anatomic components were classified into one of two categories: well visualized or poorly or non-visualized. In our study there was statistically fair agreement comparing post-natal gold standard echo & fetal echo and fetal MRI in diagnosis of right-side dilatation & TV thickening, right hypoplastic &DILV, AV&AV discordance and Ebstien anomaly.
Strength of our study, that there was statistically significant higher accuracy of diagnostic agreement with Fetal MRI (95.5%) compared to Fetal Echo (86.4%), with p value < 0.001 which agrees with the results of Dong et al. [3] study which found that Fetal MRI diagnostic accuracy rate was (79%) is significantly higher than the routine obstetric US (46%) in their study.
Finally, it should also be noted that the MRI studies provided several important complementary imaging that could directly or indirectly impact the cardiac prognosis, for example describing the devastating extent of pulmonary compression from a very large diaphragmatic hernia in a fetus that did not survive to term [10]. Fetal MRI can also be used to assess lung parenchymal lesions and airway compromise in CHD and demonstrate the presence of pulmonary lymphangiectasia in a fetus with hypoplastic left heart syndrome [11]. Limperopoulos et al. [12], Brossard-Racine et al. [13] studies agreed with our conclusion and stated that MRI of the fetal brain may provide crucial information to clinicians and parents regarding medium-term and long-term prognoses, which may have a profound effect on both prenatal and postnatal management independent of the underlying cardiac diagnosis. Our study is unique in describing extracardiac anomalies with follow up confirmation postnatally.
Limitation
Throughout our small sample size study, FCMR has been limited due to technical challenges mainly the lack of a fetal cardiac gating, maternal exhaustion, and unexpecting fetal movements.
Conclusions
Fetal cardiac MR is a complementary imaging modality that uses nonionizing radiation, good tissue contrast and large field of view, not limited by maternal obesity or overlying bone and ability of scanning the fetus in different planes, whatever the fetal lie. In our study, standard post-natal evaluation by echocardiography shows higher statistically significant sensitivity in agreement with Fetal MRI (95.5%) compared to Fetal Echo (86.4%) of overall anomalies, with p value < 0.001 HS. FCMRI also played a great role in diagnosis of extra cardiac malformation in post-nataly confirmed 15 cases. In conclusion, MR imaging as an adjuvant to fetal echocardiography may provide valuable information that could add to the prenatal diagnosis and evaluation of cardiac and most of extra cardiac anomalies, and provides additional information that improves post-natal follow-up and management.
Availability of data and materials
The datasets used and/or analysed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- FCMRI:
-
Fetal cardiac magnetic resonance imaging
- CHD:
-
Congenital heart disease
- BPD:
-
Biparietal diameter
- HC:
-
Head circumference
- AC:
-
Abdominal circumference
- FL:
-
Femur length
- EFW:
-
Estimated fetal weight
- AFI:
-
Amniotic Fluid Index
- MCA:
-
Middle Cerebral Artery
- UMA:
-
Umbilical artery
- AV:
-
Atrioventricular
- GDM:
-
Gestational Diabetes Mellitus
- HTN:
-
Hypertension
- IUFD:
-
Intrauterine Fetal Death
- AVSD:
-
Atrioventricular septal defect
- TOF:
-
Tetralogy of Fallot
- ASD:
-
Atrial septal defect
- VSD:
-
Ventricular septal defect
References
Johnson LC, Lieberman E, O’Leary E, Geggel RL (2014) Prenatal and newborn screening for critical congenital heart disease: findings from a nursery. J Pediatrics 34:916–922
Sklansky M (2004) Advances in fetal cardiac imaging. Pediatr Cardiol 25:307–321
Dong SZ, Zhu M, Li F (2013) Preliminary experience with cardiovascular magnetic resonance in evaluation of fetal cardiovascular anomalies. J Cardiovascu Magn Resonance 15:40
Manganaro L, Vinci V, Bernardo S et al (2014) Magnetic resonance imaging of fetal heart: anatomical and pathological findings. J Matern Fetal Neonatal Med 27:1213–1219
Zhu M (2015) Fetal cardiac MRI. J Cardiovasc Magn Reson 17(Suppl 1):P220
Tavares De Sousa M, Hecher K, Yamamura J et al (2019) Dynamic fetal cardiac magnetic resonance imaging in four-chamber view using Doppler ultrasound gating in normal fetal heart and in congenital heart disease: comparison with fetal echocardiography. Ultrasound Obstet Gynecol 53:669–675
Gorincour G, Bourlière-Najean B, Bonello B et al (2007) Feasibility of fetal cardiac magnetic resonance imaging: preliminary experience. Ultrasound Obstet Gynecol 29:105–108
Manganaro L, Savelli S, Di Maurizio M et al (2009) Assessment of congenital heart disease (CHD): is there a role for fetal magnetic resonance imaging (MRI)? Eur J Radiol 72:172–180
Saleem SN (2008) Feasibility of MRI of the fetal heart with balanced steady state free procession along fetal body and cardiac planes. AJR Am J Roentgenol 191:1208–1215
Sun HY, Boe J, Rubesova E et al (2014) Fetal MRI correlates with postnatal CT angiogram assessment of pulmonary anatomy in Tetralogy of Fallot with absent pulmonary valve. Congenit Heart Dis 9:E105–E109
Seed M, Bradley T, Bourgeois J et al (2009) Antenatal MR imaging of pulmonary lymphangiectasia secondary to hypoplastic left heart syndrome. Pediatr Radiol 39:747–749
Limperopoulos C, Tworetzky W, McElhinney DB et al (2010) Brain volume and metabolism in fetuses with congenital heart disease: evaluation with quantitative magnetic resonance imaging and spectroscopy. Circulation 121:26–33
Brossard-Racine M, du Plessis A, Vezina G et al (2016) Brain injury in neonates with complex congenital heart disease: what is the predictive value of MRI in the fetal period? AJNR Am J Neuroradiol
Acknowledgements
The authors thank all the study participants for their patience and support, as well as great appreciation to talented technician (Ahmed Mahfouz) who worked hardly throughout the study duration to get best quality in fastest time with no repetition or patients delay, and lastly thanks to Fetal care unite in Ain Shams university and Cairo university for being a partial source of the cases.
Funding
This study had Funded by Ain Shams university under the Research Project Plan of year 2020–2021.
Author information
Authors and Affiliations
Contributions
HGE: Suggest and develop the research idea as principal author. Data collection in the form of performing prenatal MR for all cases. Share in performance of prenatal diagnostic Fetal echo examinations. Manuscript writing, revising, and editing. Agreed to be personally accountable for the author's own contributions. NMMH: Responsible for performance of prenatal diagnostic Fetal echo examination. Responsible of post-natal diagnosis of all cases. Sharing in Reviewing literature and verified manuscript editing. ASE, ShRM: Reviewing literature and manuscript editing. Sharing in preparing figures and tables. AY: Responsible of statistical analysis and result writing. Sharing in Reviewing literature and manuscript editing. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
This study had an approval by the Research Ethics Committee (REC) of the Faculty of Medicine (FWA 000017585). at Ain shams University in Egypt on 27 October 2019. Reference Number of approval: FMASU MS 387/ 2019. The whole procedures and any possible risks that may happen are explained in detail to all participants included in this study and they gave written informed consent in this research. If any patient was unconscious at the study time, written consent for their participation was given by their own legal guardian.
Consent for publication
All participants included in this research gave written informed consent to publish all the data contained within this study. If the patient was unconscious when consent for publication was requested, written informed consent for the publication of all this data was given by their own legal guardian.
Competing interests
The authors declare that they have no competing interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Hassan, H.G.E.M.A., Habeeb, N.M.M., Ibrahim, A.S. et al. Feasibility study in assessment of congenital cardiovascular malformation by recent technique of fetal cardiac MR imaging. Egypt J Radiol Nucl Med 53, 98 (2022). https://doi.org/10.1186/s43055-022-00771-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s43055-022-00771-7