Abstract
Background
To compare clinical outcomes and technical success when direct versus indirect revascularization was achieved after endovascular technique for critical limb ischemia patients with isolated below-the-knee lesions. Fifty patients were included, 34 male and 16 female, their age from 49 to 77 years (mean 63 ±16). All patients were subjected to infra-genicular angioplasty and divided into direct 28 (31 limbs) and indirect groups 22 (24 limbs). Antegrade approach through ipsilateral CFA was used in 48 patients, while retrograde approach through tibiopedal access was used in 2 patients. Diagnostic angiography was done for all cases and duplex ultrasound was used for follow-up.
Results
One hundred thirty-two lesions were encountered, 46 in the ATA, 43 in PTA, 29 in peroneal artery, and 19 in dorsalis pedis artery. Transluminal approach was done in 47 limbs while subintimal cross was used in 8 limbs. After 1 year follow-up, AFS was 75% in the direct group and 67% in the indirect group. Freedom from MALE was 65% in the direct group and 55% in the indirect group. Freedom from MA was 86% in the direct group and 75% in the indirect group.
Conclusion
When there is a choice of target artery for revascularization, preference should be given to the artery directly feeding the wound’s angiosome.
Similar content being viewed by others
Background
The main task of revascularization in critical limb ischemia patient is limb salvage, improving quality of life, and survival prolongation [1, 2]. In clinical practice, two modalities of revascularization exists, either surgical bypass or through endovascular technology [3], and an achievement of revascularization in surgically high-risk patients has led many to predilect endovascular therapy (EVT) as the treatment of choice [4].
Successful revascularization does not ensure freedom from major amputation and wound healing [5, 6]. This failure may be due to inefficient local revascularization as no adequate vascular connections exist between the revascularized artery and the local ischemic area [7], inadequate wound treatment, systemic factors associated with delayed wound healing, and characteristics of the lesions [8].
There is also increasing evidence that treatment of chronic limb ischemia (CLI) patients either by bypass surgery or EVT mostly could provide best results if based on angiosome concept [9, 10], which was introduced by Palmer and Taylor in 1987. Angiosome concept refers to the three-dimensional block of tissue that is supplied by a specific artery and has a specific vein to drain it [11].
There are six angiosomes on the foot according to the regions supplied by the posterior tibial artery (PTA), anterior tibial artery (ATA), and peroneal artery (PeA). The calcaneal branch of the PTA supplies the medial ankle and plantar heel. The medial plantar branch of PTA supplies the medial plantar foot and the lateral plantar branch of PTA that supplies the lateral forefoot, plantar midfoot, and entire plantar forefoot. On the dorsum of the foot, the ATA continues as the dorsalis pedis artery. The calcaneal branch of the PeA supplies the plantar heel and lateral ankle while the anterior branch of PeA feeds the anterior upper ankle [12].
Evidence-based angiosome concept in managing patients with CLI gives rise to wound healing and limb salvage as well as avoid major amputation [13].
The aim of this study was to study the outcome after EVT for CLI patients with isolated below-the-knee (BTK) lesions and compare results of the direct and indirect revascularization.
Methods
The study protocol was developed in accordance with the Declaration of Helsinki and was approved by the local ethical committee.
We conducted a case series of 50 consecutive patients (55 limbs) who presented with either life-threatening non-healing ulceration, gangrene, or both (Rutherford 5 or 6), due to isolated BTK lesions. They subjected to infragenicular angioplasty presented to our hospitals from September 2015 to January 2017.
Our enrolled patients were divided into direct and indirect groups. Twenty-eight patients (31 limbs) were included in the direct group when the feeding artery flow to the site of ulceration/gangrene was successfully achieved by EVT according to the angiosome concept (Fig. 1) . Twenty-two patients (24 limbs) were included in the indirect group in whom the feeding artery flow to the site of ulceration/gangrene could not be achieved by EVT. Success was achieved if the flow was obtained through at least one vessel to the pedal arch without bypass surgery.
Procedures
-
The antegrade approach from the ipsilateral CFA was preferred using 6F sheath. The retrograde tibiopedal access in addition to the antegrade access is used when antegrade crossing fails.
-
Diagnostic angiography was done to all cases (using Philips BV Pulsera C-Arm, Germany), with fluoroscopic capability and automatic injector to exclude any supragenicular arterial lesions, confirm infrapopliteal arterial disease, and determine the TransAtlantic Inter-Society Consensus (TASC) group and the target revascularization vessel.
-
Crossing the lesion: Our policy is that in long tibial occlusions, we try to cross by stiff 0.018 wire, as this gives us the opportunity to use low profile balloons and if it fails, we try using the 0.035 wire.
-
Ballooning dilatation: In our institute, we try to cross occlusive lesions transluminally, and if failed, subintimal technique is tried. Our policy is that when the lesion is crossed by the wire, we use balloons with diameters ranging from 2.5 to 3 mm, lengths slightly longer than the lesion to do the PTA with the least number of inflations as we believe that this reduces complications. Inflation pressure ranges between nominal and burst pressure dedicated to each balloon type. Inflation time ranged between 1 and 3 min.
-
Stent deployment: It is our policy not to put stents except in complicated cases.
-
Following deflation of the balloon, the catheter was withdrawn to the mid-superficial femoral artery. One hundred to two hundred micrograms of intra-arterial nitroglycerin was used routinely if not contraindicated. A check angiogram was performed with a wire across the lesion for access. Redilatation was done whenever required.
-
The procedure is considered to be successful depending on the following:
-
Clinical success, i.e., regain of pulse, revascularization warmness, edema, and disappearance of rest pain if present pre-procedure.
-
Angiographic success defined as less than 30% residual stenosis measured at the narrowest point of vascular lumen.
-
In the case of isolated PTA or the peroneal artery, a successful procedure was defined as good distal collateralization to the foot circle.
Post-procedural management
The arterial sheath was routinely removed immediately after the procedure. Digital compression was held over the puncture site for 15–20 min and mobilization was delayed for 12–24 h.
Most patients were discharged on the second day following the procedure after receiving instructions on risk factor control and treatment including low molecular weight heparin subcutaneously for 2 days, aspirin 81 mg/day for life, clopidogrel 75 mg/day for at least 3 months, and antihyperlipidemic drugs according to the presence or absence of dyslipidemia.
The patients received foot care consisting of wound dressing, minor debridement, limited amputations, infection control, and appropriate footwear before discharge.
Follow-up
The patients were followed up at 1 month intervals. Clinical follow-up consisted of pulse examination, evaluation of the ulcer or amputation site healing, resolution of infection, and study outcome assessment. Using duplex surveillance program (Logiq P5, GE Medical Systems, Korea) with linear (5–12 MHz), 2 months interval was dedicated as strong guidance for the condition progress. The patients were examined in the supine or sitting position, as clinically appropriate. Gray-scale ultrasound was used first to localize the affected arterial segment then a color Doppler examination was performed and estimated the length of affected segment, degree of patency of stenosis, and the distal runoff (Fig. 2).
Study outcomes
Healing of the ulcer of any wounds was assessed as well as the amputation-free survival (AFS). Freedom from major amputation (MA) also assessed and compared between the two groups of patients. These outcomes suggested by the international Society of Vascular Surgery as objective performance goals for evaluating catheter-based therapies in CLI (Fig. 3).
Statistical analysis
Comparisons between the two groups were tested using chi-squared test for categorical data. For quantitative data, comparison between two groups was done using t test. A P value less than 0.05 was considered statistically significant.
Results
Fifty-five limbs from 50 consecutive CLI patients were included in this study complaining from life-threatening non-healing ulceration, gangrene, or both (Rutherford 5 or 6), due to isolated BTK lesions (Fig. 4).
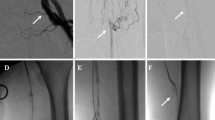
A 67-year-old male patient comes with large unhealed Rt. foot ulcer at the dorsum extending to the big toe as well as second toe: a Pre-procedure below-knee arterial angiogram where the vertical arrows refer to the radio-opaque landmark and the horizontal arrow indicates the markedly stenosed segment of PTA. b Post-procedure angiogram where the horizontal arrow refers to the recanalized segment of the PTA. c The foot before intervention. d The foot few months after revascularization. e, f Post-procedure foot angiogram with average foot vasculatures
Our inclusion criteria were considered in the enrollment of the patients in the study. The patients were divided into direct group, 28 patients (31 limbs), and indirect group, 22 patients (24 limbs) (Figs. 5 and 6).
A 56-year-old male patient presented with unhealed Rt. foot ulcer affecting mainly the big toe: a Pre-procedure angiogram, lateral view where the two arrows indicate the markedly stenosed segment of peroneal artery. b During procedure and the balloon is noted inflated inside the stenosed arterial segment. c Post-procedure angiogram with accepted recanalization of the previously stenosed arterial segment. d, e The foot at pre- and post-intervention
A 60-year-old male patient presented by unhealed Rt. foot ulcer: a Pre-procedure foot with large lateral aspect ulcer overlying the lateral malleolus. b Post-procedure follow-up with evident healing of the ulcer in few weeks. c Pre-procedure angiogram antero-posterior view for the distal leg and foot revealed attenuated terminal part of the peroneal artery. d Post-procedure angiogram showed recanalized peroneal artery as well as the ATA
Patient characteristics (demographics and co-morbidity)
The patient’s age ranged from 49 to 77 years with a mean age of 63, and they included 34 males (68%) and 16 females (32%).
The mean duration of diabetes mellitus was 15 years and 54% of the patients were receiving insulin. Mean glycated hemoglobin (HbA1c) was 7.6% ± 1.8%. Thirty-eight patients (76%) had arterial hypertension; 16 patients (32%) had a history of coronary artery disease, 25 patients (50%) were smoker, 27 patients (54%) were hyperlipidemic, only 3 patients (6%) had end-stage renal disease (ESRD) and on regular hemodialysis, and 9 patients (18%) had previous cerebrovascular events (Table 1).
Lower limb and lesion characteristics
Trans-Atlantic Inter-Society Consensus (TASC) classification was assessed for the individual limb that underwent intervention, 16 patients (18 limbs) TASC-C and 34 patients (37 limbs) TASC-D.
The lesions were found in 137 below-the-knee (BTK) vessels: 46 anterior tibial, 43 posterior tibial, 29 peroneal, and 19 dorsalis pedis arteries, determined by diagnostic angiography done during the procedure. The distribution of diseased vessels is shown in (Table 2).
According to the location of lesions either (ulcer or gangrene): 33 toes lesions, 13 heel lesions, 5 dorsal foot lesions, 8 plantar foot lesions, and 3 ankle lesions present. Seven limbs had more than sole lesion.
During procedure
In this study, five patients underwent treatment in more than one limb. The ipsilateral femoral approach was used in 52 (94.5%) of cases and the contralateral (crossover) approach was used in 3 (5.5%) of the cases. In two cases, the retrograde distal approach was used in addition to the antegrade approach due to failure to cross a lesion in infragenicular vessels from above.
PTA was considered successful in 50 patients (55 limbs). No stents were implanted at all cases. Transluminal cross was used in 47 lesions, while the subintimal cross was used in 8 lesions. The procedure was successful in all patients, as we control patient enrollment to the research.
Groin hematomas occurred in only two cases and did not require any special treatment, wire perforation occurred in three cases during targeting the direct vessel, and there were no other choices than attempting to dilate the non-target vessel and therefore the overall complication rate was four cases (7% of cases) (Table 3).
Study outcomes
The follow-up after intervention was every month. All the patients’ examination was completed at the 12th month. Nine patients (18%) were lost during follow-up. AFS, freedom from MALE and MA, was estimated and compared between the groups using Kaplan-Meier curves.
All major endpoints in patients with CLI due to an isolated BTK lesion had higher estimated percentage values in the direct group than in the indirect group. After 1 year follow-up, AFS percentage was 75% in the direct group vs 67% in the indirect group. Regarding the freedom from MALE, percentage was 65% in the direct group vs 55%in the indirect group. Also, the freedom from MA percentage was 86% in the direct group vs 75% in the indirect group (Table 3).
Discussion
Attractive theory of angiosome-directed revascularization is a widely accepted concept, helping interventionist to plan their infrapopliteal angioplasty; this theory was developed as an effort of plastic surgeon (Ian Taylor since 1987) [11] It provides not only the guidelines for choice of the target artery, but also influence the indications for endovascular or open repair according to which target artery is accessible by which method.
In this study, EVT was the primary choice for the management of all CLI patients due to BTK lesions even young patients those are generally fit for anesthesia.
A study done by Iida et al. [10] suggested that achieving direct flow based on the angiosome concept gives better results in freedom from MA, AFS, and MALE. Clinically, successfully achieving arterial perfusion to an ulcer by angioplasty was limited in comparison to the surgical bypass; therefore, the angiosome concept is considered relatively important for both modalities of revascularization, especially the EVT.
Azuma et al. [14] concluded that all previous studies to compare the results of direct vs indirect revascularization were retrospective and thus, liable for heterogeneity in patient selection. Also, the angiosome-specific artery will also be the most diseased artery while we most probably select the least atherosclerotic patients to the “direct revascularization” group.
Azuma et al. [14] also suggested that we should attempt the direct revascularization firstly and only go to the indirect revascularization option when this attempt failed. He stated that the preoperative variability in disease extent reflects the differences in healing rate and limb salvage between groups.
Some authors do infrapopliteal intervention in claudicants as Melki et al. and Soder et al. [15, 16] usually in association with proximal disease intervention as true lifestyle limiting claudications from isolated infrapopliteal disease is rare. Indications of intervention in this study were gangrene in 23 limbs (43.9%) and non-healing ulcers in 32 limbs (56.1%) with or without rest pain. The complication rate from infrapopliteal PTA procedures was minimal, only five cases during the procedures, and may make us offer infrapopliteal PTA in our claudicant patients.
As regards methods of crossing the lesions, Wang et al. [17] stated that 0.014-in. hydrophilic-coated can cross the stenosis and penetrate occlusive lesions. However, it is not possible to provide enough support to cross extremely long occlusions, and it cannot replace the 0.035-in. hydrophilic-coated guide wire (Wang et al.) [17]. In our study, we used 0.014 in five cases and 0.018 in 35 cases of total occlusions and 0.035 in 15 cases of total occlusions. Crossing stenosis with 0.014 is usually straightforward but crossing the occlusions is very challenging, so if we have long occlusions that are uncrossable with 0.014 wire, we usually cross with 0.018 or 0.035 and then we exchange the larger wire through an exchange catheter, continue the PTA on 0.014 with a long low profile balloons to minimize the number of inflations, and reduce complications.
The lesions in our study were TASC-B in 11 patients (12 limbs), TASC-C in 16 patients (18 limbs), and TASC-D in 23 patients (25 limbs). This means that a high technical success rate can be achieved even in situations traditionally considered unfavorable for angioplasty.
Fusaro et al. [18] restored the continuity between plantar and dorsalis pedis arteries using subintimal angioplasty (SIA) in an 84-year-old lady who presented with ischemic foot ulcer. We have used this technique in eight cases when transluminal crossing of the lesions is impossible, and in two cases, we failed to cross by either technique (20% failure rate of SIA). We have not found this technique easy as it appears in Bolia publications [19] that is why we reserved it to cases of failed transluminal crossing.
Scheinert et al. [20] presented the follow-up data of 112 patients treated with either PTA or PTA+ stent in the infrapopliteal vessels in 2004 concluding that 1-year patency rates were significantly superior with 83% in the stented group. A study done by Graziani et al. [21] showed that PTA alone is successful in salvaging 90% of the limbs. In our study, PTA only was done in all cases, as we believed that the late occlusion of the PTA did not affect the limb salvage rate and recanalization temporarily increases blood flow to the foot and has a positive effect in eradicating infection and healing ulcers and surgical wounds. As foot tissue healing reduces oxygen demand, less blood flow is generally required to maintain tissue integrity and keep the limb asymptomatic.
We tried the retrograde approach in only two cases (we punctured the dorsalis pedis artery and successfully recanalized its proximal portion; also, we punctured posterior tibial artery and successfully recanalized its mid-portion). It has been clearly shown that the retrograde approach is a highly successful option in patients with no antegrade access as has been shown by Montero-Baker et al. [22].
One puncture site hematoma occurred and managed conservatively while three perforations of the target vessel was managed by sustained balloon inflation across the perforation for 3 min, and all of them did not affect the outcome. So, the overall procedural complications were only four cases (7% of cases).
The follow-up after intervention was every month. All the patients’ examination was completed at the 12th month. Nine patients (18%) were lost during follow-up. AFS and MALE are defined as MA or any re-intervention and MA compared between the groups using Kaplan-Meier curves.
Iida et al. [10], on a study done during 4 years follow-up on 203 limbs in 177 consecutive patients with CLI treated by endovascular approaches. The results were significantly higher limb salvage rate in patients with direct revascularization than the indirectly revascularized wounds. Also, they postulated that it is not important how much blood can be provided to the foot but rather whether it reaches the ischemic area.
As regards, AFS between the two cohorts, after 1 year follow-up, was 75% in the direct group vs 67% in the indirect group. This percentage on a study done by Iida et al. [10] found to be 71 ± 4% in the direct group vs 50 ± 5% in the indirect group at 1 year and 49% ±8% vs 29 ± 6% at 4 years, respectively (P = .0002(.
In the study done by Iida et al. [23], the estimated freedom from MALE percentage was 61 ± 5% in the direct group vs 53 ± 5% in the indirect group at 1 year follow-up, and after 4 years follow-up, the percentage was 51 ± 8% vs 28 ± 8%, respectively (P = .008(. Also, the percentage of freedom from MA was 85 ± 4% in the direct group vs 74 ± 5% in the indirect group at 1 year, and after 4 years, it was 82 ± 5% vs 68% ± 5%, respectively (P = .01).
Open bypass surgery should be restricted to lesions technically unsuitable for EVT or patients who did not benefit from angioplasty. This was concluded by Ryer et al. [24] who considered the PTA as the first line of treatment for high-risk patients or those lacking an autogenous conduit. Other authors support the fact that PTA and surgical revascularization can be used sequentially and do not exclude each other [25]; for all these reasons, PTA is currently considered as the procedure of the first choice in diabetic subjects with ischemic foot ulcer and is not limited to those patients who cannot undergo an operation while surgery is considered a second-line procedure after PTA.
There are many limitations for this study. Firstly, it was a non-randomized analysis and the characteristic baselines were similar on the studied groups. Secondly, healing time and the details of the ulcer regarding size and depth were not evaluated and not compared in both groups. Thirdly, the angiographic follow-up was not obtained. It is promising to do a multicenter prospective cohort study model to combat these issues.
Conclusion
In CLI patients with a choice of target artery for revascularization, preference should be given to the artery directly feeding the wound’s angiosome.
Availability of data and materials
The datasets generated and/or analyzed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- AFS:
-
Amputation-free survival
- ATA:
-
Anterior tibial artery
- BTK:
-
Below-the-knee
- CFA:
-
Common femoral artery
- CLI:
-
Chronic limb ischemia
- ESRD:
-
End-stage renal disease
- EVT:
-
Endovascular therapy
- MA:
-
Major amputation
- PeA:
-
Peroneal artery
- PTA:
-
Posterior tibial artery
- TASC group:
-
TransAtlantic Inter-Society Consensus
References
Norgren L, Hiatt WR, Dormandy JA et al (2007) TASC II working group. Inter-Society consensus for the management of peripheral arterial disease (TASC II). J Vasc Surg 43:S1–S67
Dormandy JA, Rutherford RB (2007) Management of peripheral arterial disease (PAD). TASC working group. TransAtlantic inter-society consensus (TASC). J Vasc Surg. 31:1–296
Brosi P, Dick F, Do DD et al (2007) Revascularization for chronic critical lower limb ischemia in octogenarians is worthwhile. J Vasc Surg. 46:1198–1207
Kudo T, Chandra FA, Ahn SS (2005) The effectiveness of percutaneous transluminal angioplasty for the treatment of critical limb ischemia: a 10-year experience. J Vasc Surg 41:423–435
Conrad MF, Crawford RS, Hackney LA et al (2011) Endovascular management of patients with critical limb ischemia: long-term results. J Vasc Surg 53:1020–1025
Romitti M, Albers M, Cardoso Brochado-Neto F et al (2008) Meta-analysis of infrapopliteal angioplasty for chronic critical limb ischemia. J Vasc Surg. 47(5):975–981
Baldwin Z, Pearce B, Curi M et al (2004) Limb salvage following infrainguinal bypass graft failure. J Vasc Surg 39(5):951–957
Söderström M, Arvela E, Albäck A et al (2008) Healing of ischaemic tissue lesions after infrainguinal bypass surgery for critical leg ischaemia. Eur J Vasc Endovasc Surg. 36(1):90–95
Neville RF, Attinger CE, Bulan EJ et al (2009) Revascularization of a specific angiosome for limb salvage: does the target artery matter? Ann Vasc Surg. 23:367–373
Iida O, Nanto S, Uematsu M et al (2010) Importance of the angiosome concept for endovascular therapy in patients with critical limb ischemia. Catheter Cardiovasc Interv 75:830–836
Taylor GI, Palmer JH (1987) The vascular territories (angiosomes) of the body: experimental study and clinical applications. Br J Plast Surg. 40(2):133–141
Varela C, Acin N, Haro J et al (2010) The role of foot collateral vessels on ulcer healing and limb salvage after successful endovascular and surgical distal procedures according to an angiosome model. Vasc Endovasc Surg. 44:654–660
Iida O, Soga Y, Hirano K et al (2012) Long term results of direct and indirect endovascular revascularization based on the angiosome concept in patients with critical limb ischemia presenting with isolated below-the knee lesions. J Vasc Surg. 55:363–370
Azuma N, Uchida H, Kokubo T et al (2012) Factors influencing wound healing of critical ischemic foot after bypass surgery: is the angiosome important in selecting bypass target artery. Eur J Vascular Endovasc Surg 43:322–328
Melki J, Fermand M, Riche M et al (1993) Treatment of diabetic arteriopathy. Importance of trans-luminal angioplasty. J Mal Vasc 18:37–41
Soder H, Manninen H, Jaakkola P et al (2000) Prospective trial of infrapopliteal artery balloon angioplasty for critical limb ischemia: angiographic and clinical results. J Vasc Interv Radiol. 11:1021–1031
Wang J, Zhu Y-Q, Zhao J-G et al (2009) Infrapopliteal angioplasty with a long over-the-wire (OTW) balloon in the treatment of severe limb ischemia in diabetic patients: a retrospective study. Acta Radiol 27:189–199
Fusaro M, Paola L, Brigato C et al (2007) Plantar to dorsalis pedis artery subintimal angioplasty in a patient with critical foot ischemia: a novel technique in the armamentarium of the peripheral interventionist. J Cardiovasc Med 8(11):977–980
Bolia A, London N, Nydahl S (1996) Technical report: recanalisation of all three infrapopliteal arteries by subintimal angioplasty. Clin Radiol 51(5):366–367
Scheinert D, Krakenberg H, Schmidt A et al (2004) Endoluminal stebt graft placement for acute rupture of the descending thoracic aorta. Eur Heart J 8:694–700
Graziani L, Silvestro A, Bertone V et al (2007) Vascular involvement in diabetic subjectswith ischemic foot ulcer, a new morphologic categorization of disease severity. Eur J Vasc Endovasc Surg. 33(4):453–460
Montero-Baker M, Schmidt A, Bräunlich S et al (2008) Retrograde approach for complex popliteal and tibioperoneal occlusions. J Endovasc Ther. 15(5):594–604
Iida O, Yokoi H, Soga Y, et al (2013). Cilostazol reduces angiographic restenosis after endovascular therapy for femoropopliteal lesions in the Sufficient Treatment of Peripheral Intervention by Cilostazol study. Circulation is available at http://circ.ahajournals.org DOI., 27(23):2307-15
Ryer EJ, Trocciola SM, De Rubertis B et al (2006) Analysis of outcomes following failed endovascular treatmnent of chronic limb ischemia. Ann Vasc Surg 20:440–446
Faglia E, Mantero M, Caminiti M et al (2002) Extensive use of peripheral angioplasty, particularly infrapopliteal, in the treatment of ischemic diabetic foot ulcers: clinical results of a multicentric study of 221 consecutive diabetic subjects. J Intern Med 252(3):225–232
Acknowledgements
Not applicable
Funding
No disclosure of funding was received for this work from any organization.
Author information
Authors and Affiliations
Contributions
All authors have appraised the article and actively contributed to the work. KH and MAF contributed to the idea, clinical data, and interventional techniques. OAOI ad OI contributed to the clinical data and intervention technique. MGE contributed to the intervention technique and image revision. MAK contributed to the duplex study, image revision, and editing. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
This study was approved by the Ethics Committee of El Minia University. An informed oral consent from each patient was taken before enrollment into the study (committee reference number is not settled).
Consent for publication
A written informed consent was obtained from all individuals relevant to this research.
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Hendawy, K., Fatah, M.A., Ismail, O.A.O. et al. Revascularization of a specific angiosome for limb salvage: does the target artery matter?. Egypt J Radiol Nucl Med 50, 84 (2019). https://doi.org/10.1186/s43055-019-0106-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s43055-019-0106-8