Abstract
Background
Myeloproliferative neoplasms (MPNs) describe a group of diseases involving the bone marrow (BM). Classical MPNs are classified into chronic myelogenous leukemia (CML), polycythemia vera (PV), essential thrombocythemia (ET), and primary myelofibrosis (PMF). This classification is based on the presence of Philadelphia (Ph) chromosome (BCR/ABL1). CML is BCR/ABL1-positive while PV, ET, and PMF are negative. JAK2 p. Val617Phe pathological variant is the most associated mutation in BCR/ABL1-negative MPNs. The frequency of JAK2 p. Val617Phe is 90–95% in PV patients, 50–60% in ET, and 40–50% in patients with PMF. Studies on MPL gene led to the revelation of a gain of function pathological variants in JAK2 p. Val617Phe-negative myeloproliferative neoplasms (MPNs). MPL p. W515 L/K pathological variants are the most common across all mutations in MPL gene. The prevalence of these pathological variants over the Egyptian population is not clear enough. In the present study, we aimed to investigate the prevalence of MPL p. W515 L/K pathological variants in the Philadelphia (Ph)-negative MPNs over the Egyptian population.
Results
We have tested 60 patients with Ph-negative MPNs for MPL p. W515 L/K pathological variants. Median age was 51 (22–73) years. No MPL p. W515 L/K pathological variants were detected among our patients. JAK2 p. Val617Phe in PV and PMF patients showed significantly lower frequency than other studies. Splenomegaly was significantly higher in ET patients compared to other studies.
Conclusion
MPL p. W515 L/K pathological variants are rare across the Egyptian Ph-negative MPNs, and further studies on a large number are recommended. MPN patients in Egypt are younger compared to different ethnic groups.
Similar content being viewed by others
Background
Myeloproliferative neoplasms (MPNs) describe a group of diseases involving the bone marrow where there is a myeloid cell lineage proliferation that leads to an increase in the numbers of erythrocytes, megakaryocytes, or granulocytes in the bloodstream [1] Classical MPNs include chronic myelogenous leukemia (CML), polycythemia vera (PV), essential thrombocythemia (ET), and primary myelofibrosis (PMF) according to the World Health Organization (WHO) 2008 classification and the 2016 revision [2, 3]. Classical MPNs are classified according to the presence of Ph-chromosome (BCR/ABL1), CML is BCR/ABL1-positive while BCR/ABL1-negative MPNs include PV, ET, and PMF [4].
Somatic pathological variant in exon 14 of the JAK2 gene p. Val617Phe is the most associated mutation in BCR/ABL1-negative MPNs. The frequency of JAK2 p. Val617Phe is 90–95% of patients meeting the clinical criteria for PV, 50–60% for ET, and 40–50% for PMF [5]. While JAK2 exon 14 mutation is the most frequent mutation in MPN, about 10% of patients with clinical characteristics of PV, ET, and PMF lack this mutation [5]. Somatic variants in exon 12 of JAK2 gene are found exclusively in PV patients and are detected in one third of PV patients who are p. Val617Phe negative [6].
Pathological variants causing gain of function in the MPL gene (thrombopoietin receptor) are detected in JAK2-negative ET and PMF patients. The most prominent MPL pathological variants are located at the transmembrane region of the thrombopoietin receptor (TPO) [7,8,9,10].
The most frequent variants are found at codon 515 of the MPL gene being either p. Trp515Lys or p.Trp515Leu which is commonly referred to as MPL p. W515 L/K. The tryptophan residue (W) at position 515 in the MPL gene is responsible for the inhibition of the MPL transmembrane helix dimerization thus preventing the thrombopoietin-independent activation. The substitution of this residue with another amino acid such as leucine or lysine constitutively activates the JAK-STAT signaling and causes the thrombopoietin receptor to have uncontrolled self-activity leading to MPN [1, 10,11,12,13]. MPL p. W515 L/K variants are not found in PV patients but restricted to 3–5% in ET and 5–10% in PMF [14].
The prevalence of these mutations over the Egyptian population still is not clear enough. In the present study, we aimed to investigate the frequency of MPL p. W515 L/K pathological variants in Philadelphia (Ph)-negative MPNs over the Egyptian population.
Methods
Patients
A total of 60 patients with MPNs were recruited for this study. All patients were referred to the outpatient clinic of Nasser institute hospital Cairo, Egypt. The study was carried out between February 2016 and January 2018. The diagnosis of MPN was based on the World Health Organization criteria (2016 revision) [3]. All patients were subjected to full clinical examination and laboratory studies. Patients with positive BCR/ABL were excluded. All patients gave informed consent, and the study was carried out per The Code of Ethics of the World Medical Association (Declaration of Helsinki) for experiments in humans.
Treatment
Low-dose aspirin was given to all PV and ET patients. For PV patients, repeated venesection was done to maintain hematocrit level below 45. Patients with PV/ET, older than 60 years, and/or with previous history of thrombosis were considered as high risk and were given cytoreductive therapy with hydroxyurea. PMF patients with anemia were treated with repeated blood transfusion, danazol, erythropoietin, and corticosteroids whereas patients with huge splenomegaly were managed by hydroxyurea.
Methods
-
1.
DNA isolation
Peripheral blood samples were collected at the time of diagnosis on EDTA anticoagulant tubes. Genomic DNA was extracted using QIAamp DNA Blood Mini Kit (Qiagen, Germany) (Cat: 51104) according to the manufacturer’s instructions. DNA quality and quantity were assessed using Nanodrop.
- 2.
MPL p. W515 L/K pathological variants analysis
Amplification refractory mutation system (ARMS) PCR technique was used for the screening of MPL W515K/L pathological variants NM_005373.2: (p.Trp515Lys)/(p. Trp515Leu). ARMS PCR assay contains four primers (Table 1) in a single PCR tube, two forward and two reverse that are used in different combinations to amplify three probabilities, the internal control, wild allele, and the mutant allele bands. PCR was performed in 25 μl reaction volume using one unit hot start Taq DNA (Cat:154013297) as previously described by Zhuge et al. 2010 [15]. PCR products were evaluated on 1.5% agarose gel (Fig. 1).
- 3.
JAK2 p. Val617Phe mutation analysis
Electrophoresis of amplified PCR products to detect MPL p. W515 L/K pathological variants by ARMS technique. Left to right: lane 1 is 100-base pair (bp) DNA ladder and lanes 2, 3, 4, 5, 6, 7, 8, 9, 10, and 11 are wild type cases showing only internal control band of 246 bp and wild type band of 98 bp
JAK2 p. Val617Phe mutation (NM_004972.3) c.1849G>T (p. Val617Phe) was screened using ARMS technique. Two forward primers and two reverse primers were used (Table 2) in a single PCR tube to amplify three amplicons, an internal control, a wild allele, and mutant allele bands. PCR reaction contained one unit of Hot start Taq DNA polymerase (Cat: 154013297) as previously described by Chen et al. 2007 [16]. PCR products were analyzed on 2% agarose gel (Fig. 2).
Electrophoresis of amplified PCR products to detect JAK2 p. Val617Phe pathological variant in MPNs by ARMS technique. ARMS PCR shows an internal control band at 463 bp; the 229-bp band indicates the presence of the wild allele and the 279-bp band indicates the presence of the JAK2 p. Val617Phe mutant allele. Left to right: lane 1 is 100-base pair (bp) DNA ladder and lanes 2, 3, 5, and 6 are JAK2 p. Val617Phe positive while lanes 4 and 7 are wild type cases
Statistical analysis
Data were analyzed using SPSS windows statistical package, version 22.
Numeric data were presented as mean and standard deviation or median and range as appropriate. Categorical variables were presented as frequency and percentage. Comparison between the different results regarding categorical data was done using chi-square test (Fisher’s exact test). P value less than 0.05 was considered significant, and all tests were two-tailed.
Results
The present study included 60 MPN patients: 14 (23.3%) were diagnosed as PV, 26 (43.3%) as ET, and 20 (33.3%) as PMF. The median age was 51 (22–73) years. No significant difference was detected between the three groups in age or sex, Table 1
Laboratory characteristics
Median WBC was 7.7 (1.08–69) × 109/L, Median hemoglobin was 12.9 (3.1–26.3) g/dL and median platelet count was 497.5 (13–2433) × 109/L. Patients diagnosed with PV had significantly higher hemoglobin levels compared to ET and PMF (17.4 ± 2.39 vs. 13 ± 3 .49; 8.7 ± 2.8, p < 0.001) g/dl, respectively. Patients diagnosed with ET had a significantly higher level of platelet count compared to PV and PMF (1099 ± 470 vs. 294 ± 165, 268.45 ± 351.8, p < 0.001) × 109/L, Table 3.
MPL p. W515 L/K pathological variants
All patients were negative for both pathological variants of the MPL W515 L and W515K
JAK2 p. Val617Phe pathological variant
JAK2 p. Val617Phe mutation was detected in 28 (46.7%) patients with no significant difference between the three groups, p = 0.143. JAK2 p. Val617Phe pathological variant tended to be associated with the level of hemoglobin in patients with PV compared to ET and PMF (16.689 ± 2.4927 vs. 12.838 ± 2.4808, 8.783 ± 3.6581, p = 0.062).
Symptoms
Fatigue was significantly higher in patients with PMF compared to those with PV and ET (12 (60%), 5 (35.7%), and 6 (23.1%), p = 0.04), respectively. Headache and dizziness were not significantly different between groups.
Signs
Splenomegaly was in 27/60, (45%) of patients. No significant difference was detected between groups regarding hepatomegaly or splenomegaly, Table 1.
Complications
Eleven (18.3%) MPN patients had bleeding events; bleeding and thrombotic events did not show any significant difference between the three groups, Table 1.
Discussion
In this study, we investigated the frequency of the pathological variant MPL p. W515 L/K in 60 patients with Ph-negative MPNs. No MPL p. W515 L/K pathological variants were detected in our patients. Our results are consistent with previous studies performed among both Taiwanese and Iranian populations [17, 18]. They screened 88 Taiwanese and 60 Iranian Ph-negative MPNs and did not detect any MPL mutations. In contrast, ElNahass et al. screened 93 classical Egyptian MPN patients for the detection of different MPL pathological variants and detected a frequency of 3% among ET and PMF patients [19]. The authors screened all the MPL mutations by using a high-resolution melting analysis (HRM) [19]. Also, Lieu et al. [17] detected higher frequency of MPL p. W515 L/K among ET and PMF compared to that among PV. In this study, 14/60 (23%) of our patients were with PV. Furthermore, the frequency of MPL p. W515 L/K is higher in JAK2-negative MPN [20]. About 50% of our patients were positive for JAK2 p. Val617Phe pathological variant. Screening for MPL p. W515 L/K is recommended for the JAK2 p. Val617Phe-negative MPN [21, 22].
The prevalence of MPL mutations in MPN patients varies across different ethnic groups. In China, Lin et al. [13] studied 929 Chinese patients and detected MPL mutations in 1.2% in ET and 2.7% in PMF. Xu et al. [23] screened 190 MPN patients and found that MPL p. W15 L/K pathological variants were detected in 1% of ET patients, and none was found in PMF patients. In Europe, Usseglio et al. (2016) found only 3% of ET and 1% of PMF patients positive for MPL p. W515 L/K pathological variants among 164 MPN patients from France [24] while Rumi et al. screened 617 PMF patients from Italy & Spain and detected 4.1% of patients are positive for MPL p. W15 L/K pathological variants [25]. In Poland, Wojtaszewska et al. screened 184 Polish patients who were JAk2 p. Val617Phe pathological variant-negative MPNs and only 1% of ET patients had MPL mutation while none of the PMF was positive for the pathological variant [26]. Going to the Middle East, Akpinar et al. screened Turkish MPN patients and found MPL p. W515 L/K pathological variants with a frequency of 2.6% across PMF patients while they did not find any in ET patients [27]. In Iran, Shams et al. screened 105 MPN patients and the frequency was 4.76% [28].
In this study, our MPN patients showed a much lower median age at diagnosis of 49.5, 45, and 56.5 in PV, ET, and PMF, respectively, compared with other studies which had a higher median age of 59, 55, and 65 in PV, ET, and PMF, respectively [29,30,31]. This study revealed lower frequency of Jak2 p. Val617Phe pathological variant across PV and PMF represented in 64.3 and 30%, respectively, when compared to other data worldwide for the incidence of Jak2 p. Val617Phe pathological variant which was represented in 85 and 65.8% [13], 81.4 and 46.1% [32], 87.2 and 50% [2], 100% and 68% [33], and 90 and 62% [19] of PV and PMF, respectively.
The percentage of ET patients who had splenomegaly at diagnosis was 50% which is considered to be higher than the percentage of other ET patients worldwide (5–20%) [34]. This deviation may be related to endemic parasitic infections like schistosomiasis in Egyptian patients. Also, our ET patients were considered relatively young and the incidence of splenomegaly we reported was high in young patients which is consistent with the results reported by Montanaro et al. [34].
Conclusion
The current study did not detect any MPL p. W515 L/K pathological variants in the Egyptian population. The frequency of JAK2 p. Val617Phe pathological variant in PV and PMF patients was lower than other studies. MPNs affect Egyptians at a younger age compared to different ethnic groups. There is a high frequency of splenomegaly among Egyptian ET patients compared to other studies over different populations. We recommend further studies on a larger number of patients with MPNs in Egypt.
Availability of data and materials
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- MPNs:
-
Myeloproliferative neoplasms
Ph-negative
Philadelphia-negative
ARMS
Amplification refractory mutation system
PV
Polycythemia vera
ET
Essential thrombocythemia
PMF
Primary myelofibrosis
CML
Chronic myelogenous leukemia
WHO
World Health Organization
TPO
Thrombopoietin receptor
WBC
White blood cells
SD
Standard deviation
HRM
High-resolution melting analysis
References
Skoda RC, Duek A, Grisouard J (2015) Pathogenesis of myeloproliferative neoplasms. Exp Hematol. 43(8):599–608. https://doi.org/10.1016/j.exphem.2015.06.007
Azevedo AP, Silva S, Reichert A, Lima F, Junior E, Rueff J (2017) Prevalence of the Janus kinase 2 V617F mutation in Philadelphia-negative myeloproliferative neoplasms in a Portuguese population. Biomed Reports.:370–376. https://doi.org/10.3892/br.2017.977
Arber DA, Orazi A, Hasserjian R, Thiele J, Borowitz MJ, Le Beau MM et al (2016) The 2016 revision to the World Health Organization classification of myeloid neoplasms and acute leukemia. Blood. 127(20):2391–2406. https://doi.org/10.1182/blood-2016-03-643544
Boddu P, Chihara D, Masarova L, Pemmaraju N, Patel KP, Verstovsek S (2018) The co-occurrence of driver mutations in chronic myeloproliferative neoplasms. Ann Hematol. https://doi.org/10.1007/s00277-018-3402-x
Xia J, Lu MZ, Jiang YQ, Yang GH, Zhuang Y, Sun HL et al (2012) JAK2 V617F, MPL W515 L and JAK2 exon 12 mutations in Chinese patients with primary myelofibrosis. Chinese J Cancer Res. 24(1):72–76. https://doi.org/10.1007/s11670-012-0072-4
Leszczynska A, Grzenkowicz-Wydra J, Chmielewska-Gorycka L, Bieniaszewska M, Hellmann A (2016) Detection of JAK2 Exon 12 mutations in JAK2 V617F-negative polycythemia vera. Acta Haematol (exon 14):123–128. https://doi.org/10.1159/000446798
Tefferi A, Lasho T, Finke C, Knudson RA, Ketterling R, Hanson CH et al (2014) CALR vs JAK2 vs MPL-mutated or triple-negative myelofibrosis: clinical, cytogenetic and molecular comparisons. Leukemia. 28(7):1472–1477. https://doi.org/10.1038/leu.2014.3
Ji L, Qian M, Wu N, Wu J (2017) Significance of combined detection of JAK2V617F, MPL and CALR gene mutations in patients with essential thrombocythemia. Exp Ther Med. 13(3):947–951. https://doi.org/10.3892/etm.2017.4077
O’Sullivan JM, Harrison CN (2017) JAK-STAT signaling in the therapeutic landscape of myeloproliferative neoplasms. Mol Cell Endocrinol. 451:71–79. https://doi.org/10.1016/j.mce.2017.01.050
Arunachalam AK, Suresh H, Mathews V, Balasubramanian P (2018) Allele specific PCR : a cost effective screening method for MPL mutations in myeloproliferative neoplasms. Indian J Hematol Blood Transfus.:1543–1545. https://doi.org/10.1007/s12288-018-0982-5
Lasho TL, Pardanani A, McClure RF, Mesa RA, Levine RL, Gilliland DG et al (2006) Concurrent MPL515 and JAK2V617F mutations in myelofibrosis: chronology of clonal emergence and changes in mutant allele burden over time. Br J Haematol. 135(5):683–687. https://doi.org/10.1111/j.1365-2141.2006.06348.x
Staerk J, Defour JP, Pecquet C, Leroy E, Antoine-Poirel H, Brett I et al (2011) Orientation-specific signalling by thrombopoietin receptor dimers. EMBO J. 30(21):4398–4413. https://doi.org/10.1038/emboj.2011.315
Lin Y, Liu E, Sun Q, Ma J, Li Q, Cao Z et al (2015 Jul) The Prevalence of JAK2, MPL, and CALR mutations in Chinese patients with BCR-ABL1–negative myeloproliferative neoplasms. Am J Clin Pathol. 144(1):165–171. https://doi.org/10.1309/AJCPALP51XDIXDDV
Langabeer SE, Andrikovics H, Asp J, Bellosillo B, Carillo S, Haslam K et al (2015) Molecular diagnostics of myeloproliferative neoplasms. Eur J Haematol. 95(4):270–279. https://doi.org/10.1111/ejh.12578
Zhuge J, Zhang W, Xu M, Hoffman R, Zhang W (2010) Sensitive detection of MPLW515 L/K mutations by amplification refractory mutation system (ARMS)-PCR. Clin Chim Acta. 411(1-2):122–123. https://doi.org/10.1016/j.cca.2009.10.012
Chen Q, Lu F, Jones AV, Cross NC, Silver RT, Wang YL (2007) Amplification refractory mutation system, a highly sensitive and simple polymerase chain reaction assay, for the detection of JAK2 V617F mutation in chronic myeloproliferative disorders. J Mol Diagn. 9(2):272–276. https://doi.org/10.2353/jmoldx.2007.060133
Lieu CH, Shen YJ, Lai WC, Tsai WH, Hsu HC (2010) Prevalence of MPL W515 L/K Mutations in Taiwanese patients with Philadelphia-negative chronic myeloproliferative neoplasms. J Chinese Med Assoc. 73(10):530–532. https://doi.org/10.1016/S1726-4901(10)70115-5
Ghotaslou A, Nadali F, Chahardouli B, Alizad Ghandforosh N, Rostami SH, Alimoghaddam K et al (2015) Low frequency of c-MPL gene mutations in Iranian patients with Philadelphia-negative myeloproliferative disorders. Iran J Ped Hematol Oncol. 5(1):43–49
ElNahass YH, Mahmoud HK, Mattar MM, Fahmy OA, Samra MA, Abdelfattah RM et al (2018) MPN10 score and survival of molecularly annotated myeloproliferative neoplasm patients. Leuk Lymphoma. 59(4):844–854. https://doi.org/10.1080/10428194.2017.1365852
Guglielmelli P, Pancrazzi A, Bergamaschi G, Rosti V, Villani L, Antonioli E et al (2007) Anaemia characterises patients with myelofibrosis harbouring MplW515 L/Kmutation. Br J Haematol. 137(3):244–247. https://doi.org/10.1111/j.1365-2141.2007.06565.x
Ruan G-R, Jiang B, Li L-D, Niu J-H, Li J-L, Xie M et al (2009) MPL W515 L/K mutations in 343 Chinese adults with JAK2V617F mutation-negative chronic myeloproliferative disorders detected by a newly developed. Hematol Oncol. 25(3):127–131. https://doi.org/10.1002/hon
Furtado LV, Weigelin HC, Elenitoba-Johnson KS, Betz BL (2013) Detection of MPL mutations by a novel allele-specific PCR-based strategy. J Mol Diagnostics. 15(6):810–818. https://doi.org/10.1016/j.jmoldx.2013.07.006
Xu W, Li JY, Xia J, Zhang SJ, Fan L, Qiao C (2008) MPL W515 L mutation in Chinese patients with myeloproliferative diseases. Leuk Lymphoma. 49(May):955–958. https://doi.org/10.1080/10428190802035966
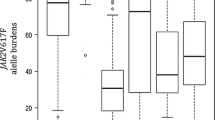
Usseglio F, Beaufils N, Calleja A, Raynaud S, Gabert J (2017) Detection of CALR and MPL mutations in low allelic burden JAK2 V617F essential thrombocythemia. J Mol Diagnostics. 19(1):92–98. https://doi.org/10.1016/j.jmoldx.2016.08.006
Rumi E, Pietra D, Pascutto C, Guglielmelli P, Martínez-Trillos A, Casetti I et al (2014) Clinical effect of driver mutations of JAK2 , CALR or MPL in primary myelofibrosis key points. Blood. https://doi.org/10.1182/blood-2014-05-578435
Wojtaszewska M, Małgorzata I, Lewandowski K (2015) Frequency and molecular characteristics of Calreticulin Gene (CALR) mutations in patients with JAK2-negative myeloproliferative neoplasms. Acta Haematol. 133(2):193–198. https://doi.org/10.1159/000366263
Akpınar TS, Hançer VS, Nalçacı M (2013) Diz- Küçükkaya R. MPL W515 L/K mutations in chronic myeloproliferative neoplasms. Turkish J Hematol. 30(1):8–12. https://doi.org/10.4274/tjh.65807
Shams SF, Ayatollahi H, Sadeghian MH, Afzalaghaee M, Shakeri S, Yazdandoust E et al (2018) Prevalence of MPL (W515K/L) mutations in patients with negative-JAK2 (V617F) myeloproliferative neoplasm in North-East of Iran. Iran J Pathol. 13(4):397–402
Passamonti F, Rumi E, Pungolino E, Malabarba L, Bertazzoni P, Valentini M et al (2004) Life expectancy and prognostic factors for survival in patients with polycythemia vera and essential thrombocythemia. Am J Med 117(10):755–761. https://doi.org/10.1016/j.amjmed.2004.06.032
Cervantes F, Dupriez B, Pereira A, Passamonti F, Reilly JT, Morra E et al (2009) New prognostic scoring system for primary myelofibrosis based on a study of the International Working Group for Myelofibrosis Research and Treatment. Blood. 113(13):2895–2901. https://doi.org/10.1182/blood-2008-07-170449
Song MK, Park BB, Uhm JE (2018) Understanding splenomegaly in myelofibrosis: association with molecular pathogenesis. Int J Mol Sci 19(3). https://doi.org/10.3390/ijms19030898
Ayad MW, Nafea D (2011) Acquired mutation of the tyrosine kinase JAK2V617F in Egyptian patients with myeloid disorders. 15(1):17–21. https://doi.org/10.1089/gtmb.2010.0093
Cacemiro MDC, Cominal JG, Tognon R, Nunes NS, Simões BP, Figueiredo-Pontes LL et al (2018) Philadelphia-negative myeloproliferative neoplasms as disorders marked by cytokine modulation. Hematol Transfus Cell Ther. 40(2):120–131. https://doi.org/10.1016/j.htct.2017.12.003
Andriani A, Latagliata R, Anaclerico B, Spadea A, Rago A, Di Veroli A et al (2016) Spleen enlargement is a risk factor for thrombosis in essential thrombocythemia: evaluation on 1,297 patients. Am J Hematol. 91(3):318–321. https://doi.org/10.1002/ajh.24269
Acknowledgements
Not applicable.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
GE conceived and planned the experiments. SE carried out the experiments. GE, HI, and MS helped supervise the project. SE wrote the manuscript with support from GE, HI, and MS. SE, GE, HI, and MS have contributed in the data analysis and interpretation. SE, GE, HI, and MS have agreed both to be personally accountable for the author’s own contributions and to ensure that questions related to the accuracy or integrity of any part of the work, even ones in which the author was not personally involved, are appropriately investigated, resolved, and the resolution documented in the literature. All authors have read and approved the submitted manuscript version.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
The collected data is de-identified for a retrospective study, and the ethics approval is unnecessary according to the Research ethics Committee—MoHP.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Eldeweny, S., Ibrahim, H., Elsayed, G. et al. MPL W515 L/K mutations in myeloproliferative neoplasms. Egypt J Med Hum Genet 20, 31 (2019). https://doi.org/10.1186/s43042-019-0039-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s43042-019-0039-9