Abstract
Introduction
As a result of the SARS-CoV-2 (COVID-19) pandemic in 2020, elective surgeries, including total joint arthroplasty (TJA), were suspended nationwide. Concurrent removal of total hip arthroplasty (THA) from the Medicare inpatient-only list posed challenges to the delivery of quality patient care with low payor cost. Therefore, the objective of this study was to compare temporal trends in patient demographics, case volumes, length of stay, and complications following elective THA in the years 2019 to 2020 in the United States.
Methods
The 2019 to 2020 ACS-NSQIP database was queried for elective THA patients. Patients Pre-COVID (2019 and 2020Q1) were compared with post-COVID (2020Q2-Q4). THA utilization, demographics, 30-day complications, and length of stay (LOS) were compared between years. Linear regression evaluated changes in case volumes over time with significance threshold of P < 0.05.
Results
A total of 77,797 patients underwent elective THA in 2019 (n = 43,667) and 2020 (n = 34,130), resulting in a 24.5% decline. Outpatient THA increased in 2020 (35.6%) vs. 2019 (5.7%) (P < 0.001). There was no significant difference in the volume of cases in 2019Q1 through 2019Q4 (P = 0.984). Elective THA volumes declined by 68.8% in 2020Q2, returned to pre-pandemic baseline in 2020Q3, before leveling off at 81.5% of baseline in Q4. Average LOS was significantly shorter in 2020 (1.55 days) vs. 2019 (1.78 days) (P < 0.001) and the proportion of same day discharge (SDD) increased quarterly from 2019 to 2020. There was no significant difference in the total complication rates in 2019 (6.6%) vs. 2020 (6.6%) (P = 0.831).
Discussion
Elective THA precipitously declined during the second quarter of 2020. The combined effect of policy changes and the COVID-19 pandemic resulted in a seven-fold increase in the number of surgeries performed in the outpatient setting in 2020. Rates of SDD doubled over the study period, despite no change in complication rates.
Similar content being viewed by others
Introduction
The SARS-CoV-2 (COVID-19) pandemic was first reported in the United States on January 30th, 2020 [1]. In order to contain the spread of disease and allocate healthcare workers and resources appropriately, elective surgery including total joint arthroplasty (TJA) was suspended nationwide [2]. On March 10, 2020, the World Health Organization (WHO) declared COVID-19 a worldwide pandemic [3]. Subsequently, the Surgeon General and the Centers for Medicare & Medicaid Services (CMS) declared the cancellation of all elective surgery in the United States in March 2020 [2].
The ramifications of cancelling elective joint arthroplasty have been felt by both patients and orthopedic joint replacement surgeons in the United States [4,5,6,7,8,9,10,11,12,13]. From a surgeon’s perspective, the projected backlog of cases was estimated to take between 9 to 35 months to recover [14]. Equally as concerning, the number of patients defined to be in a health quality of life state "worse than death" (WTD) due to waiting for a total joint replacement doubled during the pandemic [5]. Current total joint arthroplasty studies evaluating the decline in case volume due to COVID-19 are limited by lack of sample size and annual trend analysis. The few studies on this topic are either from countries outside the United States, review articles, single institutional evaluations, small multicenter collaborations, or simple projections based on historical data [4, 14,15,16,17,18,19]. Lowry Barnes et al. analyzed Medicare Claims limited to the first quarter of 2020. They reported a steep decline in TKA and THA volumes in mid-March of 94% and 92% [4]. More importantly, the clinical outcomes and complications for patients undergoing THA during the pandemic have not been reported.
In light of the worldwide suspension of elective total joint arthroplasty and the lack of nationwide reporting on an adequate representative sample, the primary purpose of the current study was to compare temporal trends in case volume of elective total hip arthroplasty (THA) from 2019 (pre-pandemic) to 2020 in the United States using a nationwide database. Secondarily, we sought to compare patient demographics, length of stay, and postoperative outcomes of those undergoing surgery before and after the pandemic origin. We hypothesized that not only would case volumes precipitously decline in 2020, but patient demographics and postoperative outcomes may be different.
Materials and methods
Database and patient selection
This study is a retrospective analysis of prospectively collected data from the 2019 to 2020 American College of Surgeons National Surgery Quality Improvement Program (ACS-NSQIP) database [20,21,22,23,24]. The NSQIP database includes detailed patient demographics in addition to preoperative and 30-day postoperative outcomes on patients undergoing major surgery. As of 2019, the database contained over 1 million cases from 719 participating institutions in the United States. The database is a source of accurate data, directly recording in-hospital morbidity and mortality as well as 30-day complications.
The database was queried for all patients undergoing elective THA (Current Procedural Terminology code 27130) in 2019 and 2020. Non-elective cases were excluded. Patients undergoing revision THA or conversion THA were also excluded from the study. Cases involving polytrauma, malignancies, or infections were excluded by using International Classification of Diseases, 9 or 10 Revision codes. Patients with missing demographic data were omitted from the study. As the data were derived from a de-identified national surgical database, the study was therefore exempt from Institutional Review Board (IRB) approval.
Variables and outcomes studied
The change in national case volume from 2019 to 2020 was investigated. Secondarily, we directly compared admission quarters to evaluate the true influence of the COVID-19 pandemic on THA utilization over time. As admission quarter 1 (Q1) ends March 31, a comparison in the year prior to (2019) and during (2020) the COVID-19 pandemic was performed.
Patient demographics, included as part of the study, were age, gender, race, body mass index (BMI), and comorbidities (diabetes mellitus, smoking history, chronic obstructive pulmonary disease, congestive heart failure, hypertension, dialysis-dependent, disseminated cancer, chronic steroid use, bleeding disorder, ascites, dyspnea, and functional health status). The 5-item modified frailty index (mFI-5) was calculated for each patient by assigning one point for each comorbidity present: diabetes mellitus, hypertension, congestive heart failure, chronic obstructive pulmonary disease, and functionally dependent health status [25,26,27,28]. Operative and postoperative data included American Society of Anesthesiologists (ASA) grade, anesthesia administered, total operative time and length of stay (LOS) [29].
Postoperative complications
Short-term postoperative complications (medical and surgical) were recorded and grouped into major and minor complications. Major complications included deep infections, organ infections, unplanned intubations, pulmonary emboli, ventilator use > 48 h, strokes, cardiac arrests, deep vein thromboses, sepsis, acute renal failures, blood transfusions, return to the operating room, and death. Complications were further broken down into the following broad categories: infection (superficial or deep surgical site infection), wound (wound dehiscence or other complications, not including surgical site infection), cardiac (cardiac arrest or myocardial infarction), pulmonary (pneumonia, pulmonary embolism, unplanned reintubation), hematological (deep vein thromboembolism, need for transfusion), renal (progressive renal insufficiency, acute kidney failure) issues, and adverse hospital discharge (discharge to other than home). Clavien Dindo IV complications (life-threatening complications including cardiac arrest, myocardial infarction, septic shock, pulmonary embolism, and renal failure) were collected and analyzed separately [30]. Rates of 30-day complications, reoperations, and readmissions were evaluated annually.
Statistical analyses
Bivariate analysis using Pearson chi-squared tests, student’s t test, and analysis of variance (ANOVA) were used to assess the differences in patient demographics between years and admission quarters. Linear regression was used to evaluate for changes in the case volume over the study period. A statistical significance threshold of P < 0.05 was used. Statistical analysis was performed using SPSS version 24 [International Business Machine (IBM), Armonk, NY, USA)].
Results
Patient demographics
A total of 77,797 patients underwent elective THA in 2019 (n = 43,667) and 2020 (n = 34,130) (Table 1). The majority of patients were white, female, with an ASA class 2 comorbidity burden. Patient demographics of 2019 vs. 2020 cohorts were similar with respect to age, gender, BMI, and the presence of the following comorbidities (diabetes mellitus, tobacco use, chronic obstructive pulmonary disease, heart failure, hypertension). A significant increase was noted in the number of patients who underwent outpatient THA in 2020 vs. 2019 (35.6% vs. 5.7%; P < 0.001). Further breakdown comparing 2019 and 2020Q1 vs. 2020Q2-Q4 demonstrated that patients undergoing elective surgery during the COVID pandemic (after 2020Q2) were younger (65.5 years vs. 65.8 years; P = 0.003) and stayed in the hospital shorter (1.50 days vs. 1.76 days; P < 0.001) (Table 2). BMI was similar between cohorts (30.4 vs. 30.5; P = 0.127).
Quarterly trends in THA utilization
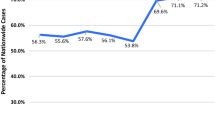
Overall, there was a 24.5% decline in elective THA from 2019 to 2020. There was no significant difference in the volume of cases in 2019Q1 through 2019Q4 (P = 0.984) (Fig. 1). However, compared to 2019, elective THA volumes minimally dropped by 14.4% in 2020Q1, and drastically decreased by 68.8% in 2020Q2 (Fig. 1). Elective THA case volumes returned to pre-pandemic baseline in 2020Q3 before eventually leveling off at 81.5% of baseline (Fig. 1).
Nationwide comparison of elective THA volume by quarter. There was no significant difference in the volume of cases in 2019Q1 through 2019Q4 (p = 0.984). However, compared to 2019, elective THA volumes minimally declined by 14.4% in 2020Q1, and drastically declined by 68.8% in 2020Q2. Elective THA case volumes returned to pre-pandemic baseline in 2020Q3 before eventually leveling off at 81.5% of baseline
Postoperative outcomes and complications
The average length of stay was significantly shorter in 2020 vs. 2019 (1.55 days vs. 1.78 days; P < 0.001). The proportion of same day discharge increased quarterly from 2019 to 2020 (Fig. 2). The overall 30-day complication rate was 6.6% (5,112/77,797). There was no significant difference in the total complication rates in 2019 (6.6%) vs. 2020 (6.6%) (P = 0.831). When comparing 2019 to 2020, rates of major complications (5.2% vs. 5.1%; P = 0.944), infection (1.3% vs. 1.4%; P = 0.415), wound complications (0.16% vs. 0.17%; P = 0.669), cardiac (0.24% vs. 0.29%; P = 0.205), pulmonary (0.56% vs. 0.53%; P = 0.584), hematological (3.0% vs. 3.0%; P = 0.801), renal complications (0.09% vs. 0.12%; P = 0.183), and Clavien Dindo IV complications (0.55% vs. 0.54%; P = 0.965) were similar. The overall 30-day mortality was significantly higher in 2020 (0.15%) vs. 2019 (0.09%); P = 0.011. Thirty-day reoperation (1.75% vs. 1.62%; P = 0.175) and readmission rates (3.16% vs 2.93%; p = 0.066) were no different between calendar years.
Discussion
Total hip arthroplasty (THA) and total knee arthroplasty (TKA) are some of the highest-volume procedures performed in hospitals on an elective basis in the United States. The effects of the COVID-19 pandemic on elective total hip arthroplasty case volumes in the United States are still being investigated [31]. To date, an adequate nationwide representation of joint arthroplasty decline in the calendar year 2020 has yet to be reported. Here we presented the first temporal trends analysis of elective total hip arthroplasty in the year prior to and during the COVID-19 pandemic. In this study, we found a 24.5% decline in annual elective THA from 2019 to 2020. The volume of cases in 2019Q1 through 2019Q4 remained constant, with a significant 68.8% decline in 2020Q2. These results confirmed our hypothesis that in quarter 2 of 2020, the effects of the pandemic-related restrictions on elective surgery would be apparent. Unknown to the orthopedic arthroplasty community was whether case volumes would recover or remain lower than the prior year. The combined effect of policy changes and the COVID-19 pandemic resulted in a seven-fold increase in the number of surgeries performed in the outpatient setting in 2020, with no change in complication rates.
TJA is responsible for a significant amount of revenue for the health care system but is also viewed as a non-essential procedure during the COVID-19 pandemic. Comparing annual elective THA, we found a 24.5% decline from 2019 to 2020. From 2019Q1 through 2019Q4 there was no significant difference in the volume of elective THA cases (P = 0.984). However, compared to 2019, elective THA volumes declined by 14.4% in 2020Q1, and drastically dropped by 68.8% in 2020Q2. Elective THA case volumes returned to pre-pandemic baseline in 2020Q3 before eventually plateauing at 81.5% of baseline. The results of our study mirror survey responses by American Association of Hip and Knee Surgeons (AAHKS) members related to their clinical practice during this time. The proportion of AAHKS members who reported a dramatic reduction of performing inpatient arthroplasty included 82% in late March 2020, peaking to 92% early April 2020, and then correcting to a 23% reduction by mid-June 2020 [11]. The consequences of this included a projected backlog of cases estimated to take 9 to 35 months to recover [14].
To date, no studies have evaluated the temporal trends in patient demographics of those undergoing elective surgery in the year prior to and during COVID-19. It was hypothesized that, nationwide, patients would be younger and healthier in order to promote minimal risk. Despite these predictions, we did not find any appreciable difference in annual cohorts with respect to age, BMI, and comorbidity burden. Groups have queried patients about their perceptions and feelings about delaying total joint arthroplasties during the pandemic [7, 8, 10, 13]. Patients have generally felt an increase in anxiety and decline in quality of life [5]. Although 85% of patients understood and agreed with the public health measures to curb infections, almost 90% of patients planned to reschedule their joint replacement as soon as possible [7].
Perhaps the most clinically important finding of our study was the notable shift of cases from the inpatient to outpatient setting before and during the pandemic. We found a seven-fold increase in outpatient THA cases. Furthermore, length of stay declined over each quarter of the study period, with frequencies of same day discharge doubling during the COVID-19 pandemic. The coinciding events including the onset of the COVID-19 pandemic and Centers for Medicare & Medicaid Services (CMS) removal of total hip arthroplasty from the “inpatient-only” list are responsible for this change [32,33,34,35]. In the present study, the overall 30-day complication rate was 6.6% (5,112/77,797). We found no significant differences in the major complications, infection, wound complications, cardiac, pulmonary, hematological, renal complications, and Clavien Dindo IV complications from 2019 to 2020. The 30-day reoperation (1.75% vs. 1.62%) and readmission (3.16% vs. 2.93%) rates following elective THA were low in our study and not impacted by the COVID-19 pandemic. However, the overall 30-day mortality was significantly higher in 2020 (0.15%) vs. 2019 (0.09%). While our data provided no direct cause of this mortality increase, it is probable that this was secondary to sequalae of the COVID-19 pandemic.
There are a few limitations to the study that warrant discussion with any national database evaluation of retrospectively collected data. The database used for this study is one of the largest nationwide representative samples, however, does not capture every hospital or surgery in the United States. Therefore, the case volume trends reported in this study should be taken in the appropriate context. Our inclusion criteria were narrowed to include only elective arthroplasty cases as this would ensure a homogeneous sample when comparing 2019 to 2020. The present study trends may be a result of other confounding factors, including changes in clinical practice instead of directly the COVID-19 pandemic. Data accuracy is potentially a concern, however, NSQIP undergoes auditing for inter-rater reliability to ensure the validity of the data [36]. All dependent variables of interest, including complications, reoperations, and readmissions, were limited to 30 days postoperatively, which do not capture patients who presented to the hospital after that time. The use of the ACS-NSQIP database prevented the ability to report on more granular postoperative outcomes such as the cause of mortality, the cause of reoperation, and exact cause of readmission. Despite these limitations, this is the first nationwide sample using this data to compare temporal trends in elective THA utilization prior to and during suspension of non-emergent surgery.
Conclusion
In the United States, there was a 24.5% decline in elective THA in 2020. Case volumes precipitously declined by 68.8% during the second quarter of 2020, before returning to pre-pandemic baseline in 2020Q3 and eventually leveling off at 81.5% of baseline. Patient demographics of those undergoing elective THA in 2020 were similar in comorbidity burden. The combined effect of policy changes and the COVID-19 pandemic resulted in a seven-fold increase in the number of surgeries performed in the outpatient setting in 2020, with rates of same day discharge doubling over the study period.
Availability of data and materials
All data are publicly available to participating institutions. The ACS-NSQIP from which the data are derived have not verified and are not responsible for the statistical validity of the data analysis or the conclusions derived by the authors.
Abbreviations
- ACS-NSQIP:
-
American College of Surgeons National Surgical Quality Improvement Program
- ASA:
-
American Society of Anesthesia
- CMS:
-
Centers for Medicare & Medicaid Services
- COVID-19:
-
Coronavirus Disease 2019
- mFI:
-
Modified Frailty Index
- SDD:
-
Same Day Discharge
- THA:
-
Total Hip Arthroplasty
- TJA:
-
Total Joint Arthroplasty
- WHO:
-
World Health Organization
References
Centers for Disease Control and Prevention. CDC Confirms Person-to-Person Spread of New Coronavirus in the United States | CDC Online Newsroom | CDC. CDC Media Releases. 2020. https://www.cdc.gov/media/releases/2020/p0130-coronavirus-spread.html. Accessed 20 Dec 2021.
Centers for Medicare and Medicaid Services. Non-Emergent, Elective Medical Services, and Treatment Recommendations. 2020. https://www.cms.gov/Files/Document/31820-Cms-Adult-Elective-Surgery-and-Procedures-Recommendations.Pdf. Accessed 20 Dec 2021.
Cucinotta D, Vanelli M. WHO Declares COVID-19 a Pandemic. Acta Bio Medica Atenei Parm. 2020;91:157.
Barnes CL, Zhang X, Stronach BM, et al. The Initial Impact of COVID-19 on Total Hip and Knee Arthroplasty. J Arthroplasty. 2021;36:S56.
Clement ND, Scott CEH, Murray JRD, et al. The number of patients “worse than death” while waiting for a hip or knee arthroplasty has nearly doubled during the COVID-19 pandemic. Bone Joint J. 2021;103-B:672–80.
Abdel MP, Meneghini RM, Berry DJ. Current Practice Trends in Primary Hip and Knee Arthroplasties Among Members of the American Association of Hip and Knee Surgeons: An Update During the COVID-19 Pandemic. J Arthroplasty. 2021;36:S40-S44.e3.
Brown TS, Bedard NA, Rojas EO, et al. The Effect of the COVID-19 Pandemic on Electively Scheduled Hip and Knee Arthroplasty Patients in the United States. J Arthroplasty. 2020;35:S49-55.
Wilson JM, Schwartz AM, Grissom HE, et al. Patient Perceptions of COVID-19-Related Surgical Delay: An Analysis of Patients Awaiting Total Hip and Knee Arthroplasty. HSS J. 2021;16:45–51. https://doi.org/10.1007/s11420-020-09799-9.
Athey AG, Cao L, Okazaki K, et al. Survey of AAHKS International Members on the Impact of COVID-19 on Hip and Knee Arthroplasty Practices. J Arthroplasty. 2020;35:S89-94.
Sequeira SB, Novicoff WM, McVey ED, et al. Patient Perspectives on the Cancellation of Elective Primary Hip and Knee Arthroplasty During the COVID-19 Pandemic. J Am Acad Orthop Surg. 2021;29:e1321–7.
Stambough JB, Deen JT, Walton SL, et al. Arthroplasty During COVID-19: Surveillance of AAHKS Members in the First Year of the Pandemic. Arthroplast Today. 2021;7:209–15.
Chen AZ, Shen TS, Bovonratwet P, et al. Total Joint Arthroplasty During the COVID-19 Pandemic: A Scoping Review with Implications for Future Practice. Arthroplast Today. 2021;8:15–23.
Brown TS, Bedard NA, Rojas EO, et al. The Effect of the COVID-19 Pandemic on Hip and Knee Arthroplasty Patients in the United States: A Multicenter Update to the Previous Survey. Arthroplast Today. 2021;7:268–72.
Wilson JM, Schwartz AM, Farley KX, et al. Quantifying the Backlog of Total Hip and Knee Arthroplasty Cases: Predicting the Impact of COVID-19. HSS J. 2020;16(Suppl 1):85–91.
Bedard NA, Elkins JM, Brown TS. Effect of COVID-19 on Hip and Knee Arthroplasty Surgical Volume in the United States. J Arthroplasty. 2020;35:S45–8.
Czubak-Wrzosek M, Czubak J, Grzelecki D, et al. The Effect of the COVID-19 Pandemic on Total Hip and Knee Arthroplasty Surgical Volume in 2020 in Poland. Int J Environ Res Public Health. 2021;18(16):8830.
Yapp LZ, Clarke JV, Moran M, et al. National operating volume for primary hip and knee arthroplasty in the COVID-19 era: a study utilizing the Scottish arthroplasty project dataset. Bone Jt open. 2021;2:203–10.
Jain A, Jain P, Aggarwal S. SARS-CoV-2 Impact on Elective Orthopaedic Surgery: Implications for Post-Pandemic Recovery. J Bone Joint Surg Am. 2020;102:e68.
O’Connor CM, Anoushiravani AA, DiCaprio MR, et al. Economic Recovery After the COVID-19 Pandemic: Resuming Elective Orthopedic Surgery and Total Joint Arthroplasty. J Arthroplasty. 2020;35:S32–6.
Ng MK, Vakharia RM, Bozic KJ, et al. Clinical and Administrative Databases Used in Lower Extremity Arthroplasty Research. J Arthroplasty. 2021;36:3608–15.
Bedard NA, Pugely AJ, McHugh MA, et al. Big Data and Total Hip Arthroplasty: How Do Large Databases Compare? J Arthroplasty. 2018;33:41-45.e3.
Pugely AJ, Callaghan JJ, Martin CT, et al. Incidence of and risk factors for 30-day readmission following elective primary total joint arthroplasty: analysis from the ACS-NSQIP. J Arthroplasty. 2013;28:1499–504.
Gordon AM, Sheth B, Conway C, et al. The Resiliency of Elective Total Shoulder Arthroplasty Case Volumes in the United States During the COVID-19 Pandemic: A Nationwide Temporal Trends Analysis. J shoulder Elb Surg. 2022. https://doi.org/10.1016/J.JSE.2022.02.045.
Bovonratwet P, Ondeck NT, Nelson SJ, et al. Comparison of Outpatient vs Inpatient Total Knee Arthroplasty: An ACS-NSQIP Analysis. J Arthroplasty. 2017;32:1773–8.
Subramaniam S, Aalberg JJ, Soriano RP, et al. New 5-Factor Modified Frailty Index Using American College of Surgeons NSQIP Data. J Am Coll Surg. 2018;226:173-181.e8.
Bellamy JL, Runner RP, Vu CPCL, et al. Modified Frailty Index Is an Effective Risk Assessment Tool in Primary Total Hip Arthroplasty. J Arthroplasty. 2017;32:2963–8.
Runner RP, Bellamy JL, Vu CPCL, et al. Modified Frailty Index Is an Effective Risk Assessment Tool in Primary Total Knee Arthroplasty. J Arthroplasty. 2017;32:S177–82.
Gordon AM, Conway CA, Sheth BK, et al. The 5-Item Modified Frailty Index for Risk Stratification of Patients Undergoing Total Elbow Arthroplasty. Hand (N Y). 2022. https://doi.org/10.1177/15589447221093728.
Schaeffer JF, Scott DJ, Godin JA, et al. The Association of ASA Class on Total Knee and Total Hip Arthroplasty Readmission Rates in an Academic Hospital. J Arthroplasty. 2015;30:723–7.
Dindo D, Demartines N, Clavien PA. Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg. 2004;240:205–13.
Mattingly AS, Rose L, Eddington HS, et al. Trends in US Surgical Procedures and Health Care System Response to Policies Curtailing Elective Surgical Operations During the COVID-19 Pandemic. JAMA Netw Open. 2021;4:e2138038–e2138038.
Gold PA, Krueger CA, Barnes CL. The Changing Total Hip and Knee Arthroplasty Practice: Identifying and Creating Value for Employed Arthroplasty Surgeons in an Era of Decreasing Reimbursement. J Arthroplasty. 2022. https://doi.org/10.1016/J.ARTH.2022.02.058
Arshi A, Wellens B, Krueger CA. The Changing Economic Value and Leverage of Arthroplasty Surgeons: How the Shift in Arthroplasty Surgery Location Impacts the Relationship of Private Surgeons, Hospitals, and Ambulatory Surgery Centers. J Arthroplasty. 2021. https://doi.org/10.1016/J.ARTH.2021.12.016
Zangrilli J, Hameed D, Chisari E, et al. Low Incidence of Asymptomatic Positive Patients Detected During Preoperative Testing for Total Joint Arthroplasty During the COVID-19 Pandemic. J Am Acad Orthop Surg. 2021;29:e1217–24.
Lynch JC, Yayac M, Krueger CA, et al. Amount of CMS Reduction in Facility Reimbursement Following Removal of Total Hip Arthroplasty From the Inpatient-Only List Far Exceeds Reduction in Actual Care Cost. J Arthroplasty. 2021;36:2276–80.
American College of Surgeons NSQIP. User Guide for the 2012 ACS NSQIP Participant Use Data File. 2013. https://www.facs.org/~/media/files/qualityprograms/nsqip/ug12.ashx. Accessed 10 May 2021.
Acknowledgements
N/A
Disclosure
The authors received no funding for this study and report no conflicts of interest.
Ethical committee statement
This study was determined to be exempt from the Institutional Review Board (IRB) of Maimonides Medical Center.
Funding
The research presented has not received any grant funding.
Author information
Authors and Affiliations
Contributions
AMG, BS, CC, MKN, MM all made substantial contribution to design, analysis, interpretation of data, and were major contributors to the writing of the initial and revised manuscript. AMG contributed to the acquisition and interpretation of data. CHJW substantially contributed to the writing and editing of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
No IRB approval is required for the study because the data were deidentified.
Consent for publication
All authors consented to the publication of this manuscript.
Competing interests
The authors declare that they have no competing interests and they were not involved in the journal’s review of or decisions related to, this manuscript.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Gordon, A.M., Magruder, M.L., Ng, M.K. et al. The combined effect of policy changes and the covid-19 pandemic on the same day discharge and complications following total hip arthroplasty: a nationwide analysis. Arthroplasty 4, 28 (2022). https://doi.org/10.1186/s42836-022-00131-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s42836-022-00131-w