Abstract
Objective
The present study characterizes patients with the mildest of mild traumatic brain injury (TBI), as defined by a Glasgow coma score (GCS) of 15.
Methods
This is an IRB approved observational cohort study of adult patients who presented to the emergency department of a Level-1 trauma center, with the primary diagnosis of TBI and a GCS score of 15 on arrival. Data collected included demographic variables such as age, gender, race, mechanisms of injury, signs and symptoms including associated vomiting, seizures, loss of consciousness (LOC), alteration of consciousness (AOC), and post-traumatic amnesia (PTA).Pre- hospital GCS, Emergency Department (ED) GCS, and results of brain CT scans were also collected as well as patient centered outcomes including hospital or intensive care unit (ICU) admission, neurosurgical intervention, and in hospital death. Data were stored in REDCap (Research Electronic Data Capture), a secure, web- based application. Descriptive and inferential analysis was done using JMP 14.0 for the Mac.
Results
Univariate predictors of hospital admission included LOC, AOC, and PTA, all p < 0.0001. Patients admitted to ICU were significantly more likely to be on an antiplatelet or anticoagulant (P < 0.0001), have experienced PTA (p = 0.0025), LOC (p < 0.0001), or have an abnormal brain CT (p < 0.0001). Patients who died in the hospital were significantly more likely to be on an antiplatelet or anticoagulant (P = 0.0005. All who died in the hospital had intracranial hemorrhage on ED head CT, despite having presented to the ED with GCS of 15. Patients were also significantly more likely to have had vomiting (p < 0.0001). Patients who underwent neurosurgical intervention were significantly more likely to be male (P = 0.0203), to be on an antiplatelet or anticoagulant (P = < 0.0001) likely to have suffered their TBI from a fall (P = 0.0349), and experienced vomiting afterwards (P = 0.0193).
Conclusions
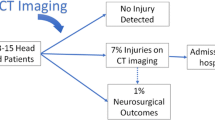
This study underscores: 1) the importance of neuroimaging in all patients with TBI, including those with a GCS 15. Fully 10% of our cohort was not imaged. Extrapolating, these would represent 2.5% bleeds, and 1.47% fractures. 2) The limitations of GCS in classifying TBI, as patients with even the mildest of mild TBI have a high frequency of gross CT abnormalities.
Similar content being viewed by others
Introduction
Traumatic brain injury (TBI) accounts for over 1 million US emergency department visits annually [1], 275,000 civilian hospitalizations [2] and 21,000 military [3] injuries. Traumatic brain injury can have lasting consequences with neurocognitive deficits [4,5,6,7], post concussive symptoms [8,9,10], and repeat return visits to the emergency department [11].
Traumatic brain injury has traditionally been classified as mild, moderate and severe based on the Glasgow Coma Scale (GCS), a scoring system never intended to classify brain injury per se but rather level of consciousness. Developed originally in 1974 [12] then modified in 1976 [13], the GCS consists of eye opening, motor, and verbal components, for a total of 15 points. A TBI consensus workgroup points out that while the GCS can be useful in the clinical management and prognosis of TBI, it “does not provide specific information about the pathophysiologic mechanisms which are responsible for the neurologic deficits and targeted by interventions [14].”
Nonetheless, this score is still widely used today. While a GCS of 13 to 15 is considered mild traumatic brain injury (mTBI) per the American College of Rehabilitation Medicine [15], studies have shown that an mTBI with GCS 13 is not the same as one with GCS 15 [16]. Indeed, even in patients who have a GCS of 15, the mTBI is not always benign. This study characterizes those patients with the mildest of mTBI, as defined by a GCS of 15, and describes the acute injury features, as well as clinical outcomes.
Methods
This study is derived from a subset of data from a previously published cohort study [17] which included adult patients who presented to the emergency department (ED) of a Level-1 trauma center, over an 18-month period with the primary complaint of TBI (ascertained using ICD-9 codes of 800–804.9, 850–854, and 959.01). For the current study, the patients had to have a GCS of 15 upon ED arrival, and the injury had to have occurred within 24 h prior to presentation. Demographic variables such as age, gender, past medical history, and medications were abstracted, in addition to the mechanism of injury, and associated signs and symptoms such as vomiting, seizures, loss of consciousness (LOC), alteration of consciousness (AOC), and post- traumatic amnesia (PTA). The patient was considered to have AOC if the neurologic exam revealed a decreased mental status, or if the patient reported feeling dazed or confused or having difficulty thinking. Varibales collected are summarized in the Table 6 in Appendix.
The prehospital and emergency department (ED) GCS were also recorded, as well as vital signs and computed tomography (CT) scan results. This study was approved by our Institutional Review Board. Data were stored in Research Electronic Data Capture (REDCap), a secure web-based application. Descriptive and inferential data analysis was done using JMP 14.0 for Mac.
Results
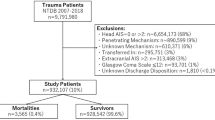
The cohort (n = 2211) was 57% male. The marital status was 61% single, 27% married, 7% divorced or separated, and 6% unknown. The median age was 37 years (IQR = 23–57), with a range of 18–101 years. Cohort demographics are summarized in Table 1.
The most common symptomatology associated with a GCS of 15 was LOC followed by PTA and AOC. The most common mechanism of injury was fall at 48%, followed by motor vehicle collision at 34%, and assault or being struck in the head at 30%. The most common location of injury reported was on the road (39%), followed by inside a home (21%). The frequency of symptoms is summarized in Fig. 1, and clinical outcomes are summarized in Fig. 2.
More than half the cohort (55%) reported no alcohol in the 12 h preceding the head injury, while 17% admitted to drinking, and another 27% were “unknown”. Alcohol levels were obtained in only 233 patients, or 10% of the cohort. The range was from 0 to 441, with a median of 153, and an IQR of 37–241. Interestingly, a higher alcohol level was significantly associated with not being admitted to the hospital (P < 0.0001), and did not result in any higher association with having an abnormal head CT either.
The prehospital GCS was obtained for all 946 patients transported via ambulance. It ranged from 3 to 15, with a median of 15 and an interquartile range of 15–15. Thus, the majority of the patients had a prehospital GCS of 15. However, 3% had a prehospital GCS of 13, and 17% had a 14. A total of 838 patients were brought in by ambulance, while 86 were brought in by helicopter. More people brought in by helicopter (48%) vs ambulance (21%) had a prehospital GCS < 15 (P < 0.0001). Regardless, having a prehospital GCS < 15 was significantly associated with being admitted to the hospital (P < 0.001) and having an abnormal CT scan (P < 0.001).
A third of the cohort (30%) were admitted to the hospital, of which 192 (29%) were admitted to the Intensive Care Unit (ICU). Univariate predictors of hospital admission included LOC, AOC, and PTA, all p < 0.0001. In multivariate analysis, only LOC and PTA retained statistical significance. Having a lower prehospital GCS was also significantly associated with being admitted to the hospital (p < 0.0001, 95% CI -0.0677 to − 0.1523). However, none of the symptoms or prehospital GCS were significantly associated with ICU admission.
Compared to the general population, patients admitted to the ICU (Table 2) were significantly older, with a median age of 62 (IQR = 41–78). Patients admitted to the ICU were significantly more likely to be on an antiplatelet or anticoagulant agent (p < 0.0001, 95%CI -0.3153 to − 0.4047) with warfarin, aspirin and clopidogrel retaining independent statistical significance. Patients admitted to the ICU were also significantly more likely to have experienced PTA (p = 0.0025, 95% CI -0.0352 to − 0.1648), LOC (p < 0.0001, 95% CI -0.3282 to − 0.4318) or have an abnormal brain CT (p < 0.0001, 95% CI -0.6584 to − 0.7816).
Patients who died in the hospital (Table 3) were significantly more likely to be on an antiplatelet or anticoagulant agent: warfarin (P = 0.0051, 95% CI -0.042 to − 0.238), aspirin (p = 0.0005, 95% CI -0.1139 to − 0.4061), or clopidogrel (p < 0.0001, 95% CI -0.1214 to − 0.3186). All patients in the hospital death group had intracranial hemorrhage on ED head CT, despite having presented to the ED with a GCS of 15, and all but one patient also having a pre-hospital GCS of 15. Patients were also significantly more likely to have presented with vomiting (p < 0.0001, 95% CI -0.5514 to − 0.8286) and were older with a median age of 81, compared to the survivor cohort median age of 37.
Patients who underwent neurosurgical intervention (Table 4) were significantly more likely to be male (P = 0.0203), to be on an antiplatelet or anticoagulant agent: warfarin (P = < 0.0001), aspirin (P < 0.0001), or clopidogrel (P = .0003). They were also more likely to have suffered their TBI from a fall (P = 0.0349), and experienced vomiting afterwards (P = 0.0193). Fourteen patients had their anticoagulant status reversed. 11 received IV vitamin K, 7 received both IV vitamin K and fresh frozen plasma (FFP), 2 received FFP only, and 1 received SC vitamin K.
A total of 1996 or 90% of patients had a brain CT scan. Of these, 485 or 24% had a CT abnormality (Table 5). The frequency of specific CT abnormalities is summarized in Fig. 3. The most common CT lesions noted on CT were extra-calvarial soft tissue swelling (41%), parenchymal or hemorrhagic contusion (26%), subdural hematoma (25%), and subarachnoid hemorrhage (22%). Patients who had an abnormal CT scan were significantly more likely to be older, on an anticoagulant, and have suffered a fall as their TBI mechanism (all P < 0.001).
Discussion
In this observational study of emergency department presentations for patients with a GCS of 15 upon arrival, a number of findings emerge that suggest that the simple characterization of head injury by GCS score may not be sufficient.
The cohort is somewhat unique in the proportion of patients who received a brain CT as part of their evaluation. Indeed, there are several rules that specifically seek to limit the use of head CT for head injury, within certain parameters. The Canadian head CT [18] rule excludes people on blood thinners, and those who had a seizure after the head injury. Also, a number of high-risk criteria have been noted with the rule, including use of blood thinners, any suspicion of skull fracture, age > 65, and a change in GCS level. Medium risk criteria including a “dangerous mechanism” is also noted as a caveat. The New Orleans head CT criteria [19] actually targets only the GCS 15 head injury population, and “suggests patients with GCS 15 and head trauma are unlikely to need a head CT as long as they do not have headache, vomiting alcohol or drug intoxication, persistent anterograde amnesia, seizure, visible trauma above the clavicles.”
Clearly, neither of these rules are optimal for the mild TBI cohort in this emergency department study. Studies published years after these rules concur, suggesting that “Patients with GCS 15 and risk factors or neurological symptoms should be evaluated with CT scan, [as] the outcome of mild TBI depends on the combination of preinjury, injury and postinjury factors” [20]. CT abnormalities are in fact not uncommon in mild TBI. A study of 2766 patients with mild TBI imaged in ED found that every sixth patient (16.1%) with mild TBI had an intracranial lesion [21]. The most common lesions were subdural hematomas, subarachnoid hemorrhages, and contusions. Similar to the current study, the authors noted that a lower Glasgow Coma Scale score, male sex, older age, falls, and chronic alcohol abuse were associated with higher risk of acute intracranial lesion in patients with mild TBI. These findings underscore the heterogeneity of neuropathology associated with the mild TBI classification.
Even in cases of mTBI, patients sometimes require neurosurgical intervention (NSI), as noted in the current study. In their study of mTBI patients, Tierney et al. [22] also noted that 8.2% had some form of NSI performed (including placement of an intracranial pressure monitor and other measuring devices). The in-hospital death rate for the NSI group was 13%, significantly higher than general figures for mTBI ranging from 0.3–1.8%. The use of anticoagulants as well as age being over 60 predicted a bad neurological outcome.
ICU admission for mTBI, while seemingly counterintuitive, is not all that uncommon. A retrospective study of 595,171 mTBI patients in the National Trauma Data Bank found that 44.7% were admitted to an ICU, While 17.3% of these met the criteria for overtriage, as defined by: ICU stay ≤ 1 day; hospital stay ≤ 2 days; no intubation; no neurosurgery; and discharged to home [23], that still leaves 27.4% of mTBI patients who were deemed appropriate for ICU admission. Interestingly, the study noted that a common “risk factor” for overtriage included isolated subarachnoid hemorrhage.
Conclusion
This study underscores: 1) the importance of considering neuroimaging in all patients with TBI, including those with a GCS 15. In the current study, a total of 10% of the cohort was not imaged. If the CT data is extrapolated to the non-imaged group, the proportion of bleeds and fractures would be increased by 2.5 and 1.5 percentage points, respectively. 2) recognizing the limitations of GCS in classifying TBI, as patients with even the mildest of mild TBI have a high frequency of gross CT abnormalities, and non-benign outcomes including ICU admission, neurosurgical interventions and even in-hospital death.
Abbreviations
- AOC:
-
Alteration of consciousness
- CT:
-
Computer tomography
- ED:
-
Emergency department
- GCS:
-
Glasgow coma score
- ICU:
-
Intensive care unit
- LOC:
-
Loss of consciousness
- PTA:
-
Post-traumatic amnesia
- RedCap:
-
Research Electronic Data Capture
- TBI:
-
Traumatic brain injury
References
Faul M, Xu L, Wald MM, et al. Traumatic brain in the United States: Emergency department visits, hospitalizations and deaths, 2002–2006. Atlanta, GA: Centers for Disease Control and Prevention, National Center for Injury Control and Prevention; 2010.
Centers for disease control, prevention. Report to congress on mild traumatic brain injury in the United States: steps to prevent a serious health problem. Atlanta, GA: Centers for Disease Control and Prevention, National Center for Injury Prevention and Control; 2003.
DoD Worldwide Numbers for TBI. https://www.brainline.org/article/how-many-servicemembers-have-sustained-tbi#annualdiagnoses. Accessed 25 Jan 2019.
Dean, P. J., & Sterr, A. (2013). Long-term effects of mild traumatic brain injury on cognitive performance. Frontiers in Human Neuroscience, 7, 30.T.
Ganti, L., Daneshvar, Y., Ayala, S., Bodhit, A. N., & Peters, K. R. (2016). The value of neurocognitive testing for acute outcomes after mild traumatic brain injury. Military Medical Research, 3, 23. https://doi.org/10.1186/s40779-016-0091-4.
Middelboe, T., Anderson, H. S., Birket-Smith, M., & Friis, M. L. (1992). Minor head injury: Impact on general health after 1 year. A prospective follow-up study. Acta Neurologica Scandinavica, 5, 5–9.
Ganti, L., Daneshvar, Y., Bodhit, A., Ayala, S., Patel, P. S., Lottenberg, L. L., York, D., Counsell, C., & Peters, K. R. (2015). TBI ADAPTER: Traumatic brain injury assessment diagnosis advocacy prevention and treatment from the emergency room-a prospective observational study. Military Medicine, 180(4), 380–386. https://doi.org/10.7205/MILMED-D-14-00316.
De Kruijk, J. R., Leffers, P., Menheere, P. P., Meerhoff, S., Rutten, J., & Twijnstra, A. (2002). Prediction of post-traumatic complaints after mild traumatic brain injury: Early symptoms and biochemical markers. Journal of Neurology, Neurosurgery, and Psychiatry, 73(6), 727–732.
Ganti, L., Khalid, H., Patel, P. S., Daneshvar, Y., Bohdit, A. N., & Peters, K. R. (2014). Who gets post-concussion syndrome? An emergency department-based prospective analysis. International Journal of Emergency Medicine, 7, 31. https://doi.org/10.1186/s12245-014-0031-6.
Auxéméry, Y. (2012). Mild traumatic brain injury and postconcussive syndrome: A re-emergent questioning. Encéphale, 38(4), 329–335.
Ganti, L., Conroy, L., Bodhit, A., et al. (2015). Understanding why patients return to the emergency department after mild traumatic brain injury within 72 hours. WestJem. https://doi.org/10.5811/westjem.2015.2.23546.
Teasdale, G., & Jennett, B. (1974). Assessment if coma and impaired consciousness. A practical scale. Lancet, 2, 81–84.
Teasdale, G., & Jennett, B. (1976). Assessment and prognosis of coma after head injury. Acta Neurochirgica, 34, 45–55.
Saatman, K. E., Duhaime, A.-C., Bullock, R., Maas, A. I. R., Valadka, A., & Manley, G. T. (2008). Classification of traumatic brain injury for targeted therapies. Journal of Neurotrauma, 25(7), 719–738. https://doi.org/10.1089/neu.2008.0586.
Kay, T., Harrington, D. E., Adams, R., et al. (1993). Definition of mild traumatic brain injury. The Journal of Head Trauma Rehabilitation, 8(3), 86–87.
Si, B., Dumkrieger, G., Wu, T., Zafonte, R., Valadka, A. B., Okonkwo, D. O., et al. (2018). Sub-classifying patients with mild traumatic brain injury: A clustering approach based on baseline clinical characteristics and 90-day and 180-day outcomes. PLoS One, 13(7), e0198741 https://doi.org/10.1371/journal.pone.019874116.
Stead, L. G., Bodhit, A. N., Patel, P. S., et al. (2013). TBI surveillance using the common data elements for traumatic brain injury: A population study. International Journal of Emergency Medicine., 6, 5. https://doi.org/10.1186/1865-1380-6-5.
Stiell, I. G., et al. The Canadian CT Head Rule for patients with minor head injury. The Lancet, 357(9266), 1391–1396.
Haydel, M. J., Preston, C. A., Mills, T. J., Luber, S., Blaudeau, E., & DeBlieux, P. M. C. (2000). Indications for computed tomography in patients with minor head injury. The New England Journal of Medicine, 343, 100–105.
Shukla, D., & Devi, B. I. (2010). Mild traumatic brain injuries in adults. Journal of Neurosciences in Rural Practice., 1(2), 82–88. https://doi.org/10.4103/0976-3147.71723.
Isokuortti, H., Iverson, G. L., Silverberg, N. D., Kataja, A., Brander, A., Öhman, J., & Luoto, T. M. (2018 Jan). Characterizing the type and location of intracranial abnormalities in mild traumatic brain injury. Journal of Neurosurgery, 12, 1–10. https://doi.org/10.3171/2017.7.JNS17615.
Tierney, K. J., Nayak, N. V., Prestigiacomo, C. J., & Sifri, Z. C. (2016). Neurosurgical intervention in patients with mild traumatic brain injury and its effect on neurological outcomes. Journal of Neurosurgery, 124(2), 538–545. https://doi.org/10.3171/2015.4.JNS142440 Epub 2015 Sep 25.
Bonow, R. H., & Quistberg, A. (2018). Rivara. Neurocrit Care: F.P. et al https://doi.org/10.1007/s12028-018-0590-0.
Acknowledgements
None.
Funding
n/a
Availability of data and materials
n/a (retrospective chart review).
Author information
Authors and Affiliations
Contributions
LG, ANB and YD conceived the study. LG, YD, ANB, SA, and CP collected the data. LG, and ANB performed the statistical analyses and cross checked the data. TS and LG drafted the manuscript, and all authors contributed substantially to its revision. KP supervised the conduct of the research and data collection. LG takes responsibility for the paper as a whole. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
This retrospective chart review study was approved by the Institutional Review Board at the University of Florida, study#188–2011.
Consent for publication
Waiver of informed consent was approved by the IRB for this retrospective chart review.
Competing interests
None of the authors have any completing interests.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendix
Appendix
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated.
About this article
Cite this article
Ganti, L., Stead, T., Daneshvar, Y. et al. GCS 15: when mild TBI isn’t so mild. Neurol. Res. Pract. 1, 6 (2019). https://doi.org/10.1186/s42466-018-0001-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s42466-018-0001-1