Abstract
Background
Childhood pneumonia is the commonest cause of suffering worldwide. Among under-five children where it accounts for more than one out of seven under-five death globally. It is the single leading cause of death in Ethiopia, accounting for 18% of all under-five mortality burdens. These deaths are easily preventable and treatable through simple and cost-effective interventions. The study aims to assess the prevalence and associated factors of pneumonia among under-five children at Angolela Tera district, North Shoa, Ethiopia, 2021. A community-based cross-sectional study was conducted on a simple random sample with a sample size of 414 registered mothers with 6–59 months of children. Semi-structured questionnaires were used to collect data. The data were entered using the EpiData version 3.1, and analysis was done by SPSS version 24. Bivariable and multivariable logistic regression analysis was used.
Results
The prevalence of pneumonia in children under five was 5.8% (95% CI 3.6–8.2%). Based on the multivariable logistic regression analysis of this study, child male sex, have no family toilet, children having fever in the last 2 weeks, lack of maternal ANC follow-up and children with stunted were associated with pneumonia.
Conclusions
The study shows that the prevalence of under-five pneumonia was low as compared to recent EDHS 2016. Therefore, by making interventions on potential determinates such as by improving family latrine utilization, improving the nutritional status of children, and early control of respiratory tract infection and fever, we can reduce under-five pneumonia.
Similar content being viewed by others
Background
Pneumonia is a lower respiratory tract infection that exclusively affects the lung. While it attacks every person, Children under the age of five years are particularly prone to pneumonia (Mulholland 2007).
Bacteria are the most common cause of community-acquired pneumonia (CAP), with Streptococcus pneumonia isolated in nearly 50% of cases. The clinical picture of pneumonia differs depending on the microorganism causing the disease and the age of a child (Eddy et al. 2005). The presence of cough and fast breathing and or difficulty of breathing for specific age clenches the classification of suspected pneumonia in children older than 2 months and yet less than 60 months of age (Child WHODo, Health A, Organization WH, UNICEF 2005; Bazie et al. 2020).
The World Health Organization (WHO) estimates there are 156 million cases of pneumonia each year in children younger than five years, with as many as 20 million cases severe enough to require hospital admission and 1.2 million deaths annually, making up 18% of all deaths of this age group and mainly affecting children in developing countries. In developing countries, respiratory tract infections are not only more prevalent but more severe, accounting for more than 2 million deaths annually; pneumonia is the number one killer of children in these societies.
More than 60% of such incidence of pneumonia is reportedly concentrated in just two regions, namely Southeast Asia and Africa, each bears 35 and 61 million new infections in a year, respectively (Harris et al. 2011; Walker et al. 2013). In Ethiopia, pneumonia is a leading single disease killing under-five children. It is estimated that in Ethiopia, 3,370,000 children encounter pneumonia annually which contributes to 18 percent of all causes of death killing over 40,000 under-five children every year (Rudan et al. 2013; Rashid et al. 2017).
These deaths are easily preventable by cost-effective interventions like immunization, good nutrition, exclusive breastfeeding, appropriate complementary feeding hand washing (Chopra et al. 2013).
According to a study conducted at Wondo Genet district, Sidama zone, Ethiopia, the prevalence of pneumonia among under-five children who visit health centers was 33.5% (Abuka 2017).
It is therefore important that to look at a combination of strategies for reducing the morbidity and mortality from pneumonia. These include preventive strategies such as routine immunizations, zinc, and vitamin A supplementation, control of environmental factors, promotion of breastfeeding, good nutrition, safe drinking water, and good sanitation. So, addressing current gaps for the prevention of under-five pneumonia is critical to achieving Sustainable Development Goal (SDG 3) (Bawankule et al. 2017).
The widespread nature of the problem in Ethiopia has already killed thousands of children which need to look for a lasting solution to end the problem. Despite the sustained effort to stop the problem, pneumonia continues to common mortality of children which calls for innovative strategies that will come about only through systematic research works. Data on the prevalence of pneumonia and its risk factors are important in planning child health services but are not available in our countries. There is no study done on the pneumonia prevalence and associated factors in our research area, Therefore, this study aimed to assess the prevalence and associated factors of pneumonia among under-five children in Angolela Tera district, North Shoa, Ethiopia, and 2021.
Methods
Study design, setting, and period
A community-based cross-sectional study was conducted from November 30 to December 30, 2021. The study was conducted in the Angolela Tera area of North Shewa. The wereda is 112 km far away from Addis Ababa, the capital of Ethiopia.
Populations
Source population
The source populations were all mothers with children pair from 6 to 59 months of age who live in the households of Angolalla Tera district North Shoa, Amhara region.
Study population
The population of the study was randomly selected children aged 6–59 month who lived with their mothers in administrative sampling kebeles in the Angolela Tera region at the time of the study.
Inclusion and exclusion criteria
Inclusion criteria
Children 6–59 months of age, who were living with their mothers, and whose mothers were available in the selected households were included.
Exclusion criteria
Children, who were seriously ill and the child’s mother critically ill, during data collection, were excluded.
Sample size determination and sampling techniques
The sample size was determined using a single population proportion formula assuming 50% of prevalence as there was no previous study in the study area. Also 5% error rate with 95% confidence level expected 10% non-response rate.
A simple random sampling method was used to select children in the houses. Of the 21 cables, six Kebele were selected by random samples (lottery method).
Variables
Dependent variable
Pneumonia of 6–59-month-old children.
Independent variable
-
Socio-demographic characteristics.
-
Environmental characteristics.
-
Nutritional factors.
-
Health-related factors.
Data collection procedures
The questionnaire was first developed in English and translated into the local Amharic language and then translated back into English by the third person to check the consistency. Five data collectors and one supervisor were recruited. Mothers who had 6–59-month-old children were interviewed on the presence or absence and duration of cough and history of measles and diarrhea. The respiratory rate of each of the children who had been reported to have cough was measured then by counting the number of times the child’s body moves up and down for one full minute. Mothers in the household with 6–59-month-old children who were absent during the first day of data collection were interviewed in the subsequent days (visited three times a day) until the final day of data collection.
Data quality control and assurance management
Both data collectors and a supervisor were trained for one day on such issues as the techniques of data collection and or face-to-face interview skills.
Data collectors used certain unforgettable events such as the time of death and wedding of family members or another person, and the season of the year, to help mothers relate, and remember the exact age of their child. Besides, mothers requested to report the age of the child in month/s and or in month/s and year/s whenever the child had not yet celebrated his/her next birthday. Mechanisms of maintaining the confidentiality of the participants throughout the whole process of data collection and the study were discussed and ascertained during the two-day long training. A supervisor was followed on how to check the completeness and consistencies of questionnaires filled by the data collectors to ensure the quality of the data.
Data analysis procedures
The data were entered by EpiData 3.1 version. The analysis was performed with the IBM SPSS 20 version after exporting the modified data. Descriptive statistics such as frequency distribution, cross-tabulation classification, and other measurements of medium and variance trends (mean deviations and norms) were computerized to describe the major variables of the study. Odds measurement and p value were computerized to determine the relationship between exposure and outcome variability. A p value less than 0.05 is considered statistically significant. Binary logistic regression was done to see the effect of each of the independent variables on the outcome variable by simultaneously suppressing the effect of extraneous variables.
Operational definitions
Respiratory rate = the number of respirations in one full minute (also called breathing rate).
Respiratory distress = respiratory difficulty manifested by nasal flaring, grunting, supraclavicular or intercostal retractions and lower chest in drawing.
Pneumonia = child having cough with fast breathing.
Results
Demographic and socioeconomic characteristics
Atotal of 414 participated in the study with a response rate of 98.1%. The mean age (± 1SD) of participant children was 24.93 (± 15.57) months for both sexes. More than half, 212 (51.2%) of the children were male, and nearly one-third, 142 (34.3%) of the children were found in the age group 12–23 months. Among the total respondents, 389 (94.0%) were Amhara, and 362 (87.4%) were orthodox religion followers. From the total participant, the first birth order children were 118 (28.5%), and 137 (33.1%) of the children were born in less than 24 months spacing from the preceding siblings. From the total number of mothers, 362 (87.4%) were married, 363 (87.7%) were housewives and 258 (62.3%) of mothers had no formal education (Table 1).
Health care and environmental characteristics
As it is depicted in Table 2, 185 (44.7%) of children had a normal birth weight of 2.5–4.0 kg and 50 (12.1%) were < 2.5 kg. Of the total of 414children, 183 (46.3%) were fully vaccinated, whereas 166 (42%) of them are not fully vaccinated. Among the total children, 288 (69.6%) had got diarrhea during the 2 weeks of the period before data collection and 245 (59.2%) children were affected by recurrent diarrhea. Out of the total mothers, 251 (60.6%) mothers were delivered at health institutions, whereas 163 (39.4%) were delivered at home. The majority 336 (81.2%) of the mothers had no postnatal care (PNC), visits. Concerning the source of drinking water, 178 (43%) of the households used protected as well as the main source of drinking water (Table 2).
Dietary characteristics
In terms of breastfeeding, the majority of 380 mothers (91.8%) were breastfeeding their babies. one hundred and seventy-six children (46.3%) started breastfeeding, within the first hour. Of the 380 infants’ total breastfeeding, 294 (77.3%) were colostrum. Of the 414 babies in total, 134 (32.4%) received prenatal diet.
Babies who were breastfed for less than 12 months were 167 (43.9%), 12–24 months were 157 (41.3%), and over 24 months were 56 (14.8%). The majority of the 281 respondents (67.9%) were initiated on parallel feeds at 6 months. In terms of nutrition, the mothers who used the cup to feed their babies were 140 (33.8%) and 138 (33.3%) used the hand to feed their babies (Table 3).
Prevalence of pneumonia among children
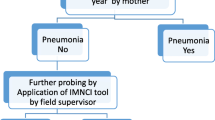
Of 414 children’s participated in the study, 231 (55.8%) of them had a history of cough during the time of the study, 125 (30.2%) of children had difficulty of breathing and 102 (24.6%) had fast breathing at the time of the study. Among a total of 414 children, 259 (62.6%) had a fever, the overall prevalence of under-five children’s pneumonia during the study was 24 (5.8%) (Fig. 1).
Multivariate logistic regression
Data were analyzed using binary logistic regression analysis. Statistical associations were checked by 95% CI and odds ratio. Those variables which had a p value less than 0.2 in the binary logistical regression analysis were eligible for multivariable logistic regressions. Finally, the adjusted odds ratio was checked, and the significant variables p value < 0.05 were considered as associated factors for pneumonia.
Based on the multivariable logistic regression analysis of this study, child male sex, having a family toilet, children having fever in the last 2 weeks, maternal ANC follows up and children with stunted were associated with pneumonia. Male children were 4.1 times (AOR = 4.1, 95% CI 1.49–11.8) more likely to develop pneumonia.
This finding suggests that children who had stunting were 2.9 times (AOR = 2.9, 95% CI 1.16–7.60) more likely to develop pneumonia as compared to children who had no stunting. Also, this finding indicates that children who had a fever in the last 2 weeks were three times (AOR = 3.02, 95% CI 1.23–7.40) more likely to develop pneumonia as compared to children who had no fever in the last 2 weeks. Similarly mothers who had no ANC follow-up were two times (AOR = 2.07, 95% CI 1.16–7.6) more likely to develop pneumonia as compared to children who had no ANC follow-up. The family who has not to used latrine were three times (AOR = 3.12, 95% CI 1.09–8.94) more likely to develop pneumonia than those who have used latrine (Table 4).
Discussion
The finding of the study revealed that the prevalence of pneumonia was 5.8% (95% CI 3.6–8.2), this is lower than the national prevalence of pneumonia 7%, according to EDHS 2011 (Amsalu et al. 2019). This discrepancy might be because of differences in sample size, sampling method. Also, this finding was lower than the findings from a cross-sectional survey in Este town which found the prevalence of under-five pneumonia to be significantly higher, 16.1% (Fekadu et al. 2014). The possible reason for this difference could be that the ascertainment of pneumonia was based on mothers' reports like with EDHS report. The other reason could be attributed to the difference in the skills of data collectors and methodology. Similarly, this finding is also lower than the findings from the retrospective study in UNHCR refugee camps where pneumonia accounted for 17% of child morbidity (Abuka 2017). Besides the difference in methodology, the study setting, i.e., the refugee camps are the area where there is overcrowding and a hence a higher chance of transmission of the disease, may have accounted for the difference in the prevalence of pneumonia in children. Furthermore, the relatively low prevalence of pneumonia in the study area may reflect improved access to water and sanitation. On the other hand, this figure is in line with the prevalence of under-five pneumonia (6.4%) in the Amhara region (Amsalu et al. 2019).
The prevalence of pneumonia in children in this study setting is not consistent with the findings from a cross-sectional survey in Uganda where pneumonia prevalence was found to be significantly higher (53.7%). The discrepancy in the difference in the prevalence of pneumonia could be due to the difference in the setting in which these two studies were conducted, the latter being done in the National referral hospital of Uganda. The cross-sectional survey in Kuhati, Bangladesh showed the prevalence of under-five pneumonia was estimated to be 53% (Rahman et al. 2014).
In this study, the occurrence of pneumonia was not affected by the residence. This is comparable to the findings from the cross-sectional survey in Este town where pneumonia prevalence was not different between urban and rural dwellers (Gedefaw and Berhe 2015).
The prevalence of pneumonia in under-fives was not affected by the educational status and occupation of parents. This finding is consistent with the findings from a case–control study in Pakistan where there was no statistically significant difference in the prevalence of pneumonia between educated and non-educated parents (Hershey et al. 2011). The case–control study, however, reported that maternal occupation was significantly associated with pneumonia, which is contrary to the finding in this study. This difference could be explained by the difference in the methodology and skills of data collectors. Similarly, this finding is supported by the report from the cross-sectional survey in Este town where the educational status and occupation of the parent did not illustrate significant association with pneumonia in children (Gedefaw and Berhe 2015). Another case–control study from India reported that the literacy status of the father did not show any association with pneumonia in under-fives (Pore et al. 2010).
Among factors associated with under-five pneumonia, male children were about four times more likely to develop pneumonia as compared to female children. The result is similar to studies conducted in Omdurman Pediatric Hospital; Khartoum, Sudan (Organization 2014). It is also in line with a report from lancet 2013 which showed a higher occurrence of pneumonia in boys than in girls (Lema et al. 2018), a report from lancet 2013, which showed a higher occurrence of pneumonia in boys than in girls (Walker et al. 2013). The parents’ attitudinal change toward gender equality in the current study area might be the other reason for such difference.
In this study, there was also no difference in the occurrence of pneumonia with the age of the child. This finding is not in line with the report from lancet 2013 which revealed a higher occurrence of pneumonia in children younger than 2 years of age (Walker et al. 2013).
However, types of latrine were associated with pneumonia in 6–59-month-old children in this study. This is consistent with the WHO/UNICEF report which revealed that improved latrine can for the most part prevent pneumonia in children (Abuka 2017).
Breastfeeding the child exclusively during the first 6 months of the child's life was not found to factor in pneumonia in children. This is not consistent with findings from a systematic review and meta-analysis done in USA,2013, 2011 UNICEF report and the integrated action plan for prevention and control of pneumonia and diarrhea of 2013 of the WHO and UNICEF where exclusive breastfeeding was one of the factors that could determine the incidence and prevalence of and mortality from pneumonia in children (Hiko and Kebeta 2017; Child 2011). This difference could be explained by the fact that mothers who might know that breastfeeding children exclusively to the first 6 months of children's life is socially acceptable may falsely report that their children had been breastfed exclusively during their first 6 months of age. However, these same findings support the finding in this study that breastfeeding children up to 2 or more years can reduce pneumonia morbidity (from Pneumonia EPCD 2013).
Since there is a lack of sufficient source of data on the prevalence of pneumonia among 6–59-month-old children, almost all of the reviewed literature includes studies on pneumonia among 0–59-month-old children which impairs the comparison between the current and other studies. Therefore, the difference in the study population could be another big reason for the discrepancy that has occurred between the current study and other studies which were used in the discussion.
Conclusions
This study revealed a low prevalence of pneumonia among children aged six to fifty-nine months in the study area as compared to national EDHS 2016 prevalence. The finding of our study showed that male sex, have no improved family toilet, children having fever in the last 2 weeks, lack of maternal ANC follow-up and children with stunted were associated with pneumonia were found to be significant predictors of childhood pneumonia. Based on the finding, the government and the federal and wereda health office need to enhance awareness and resource mobilization for health care providers toward ANC follow-up, diarrhea prevention, educating mothers, and exclusive breastfeeding.
Availability of data and materials
Data will be available on request from the corresponding author.
Abbreviations
- ANC:
-
Ante natal care
- CI:
-
Confidence interval
- EBF:
-
Exclusive breast feeding
- ETB:
-
Ethiopian total birr
- SPSS:
-
Statistical Package for Social Science
- UNICEF:
-
United Nations Children's Fund
- WHO:
-
World Health Organization
References
Abuka T (2017) Prevalence of pneumonia and factors associated among children 2–59 months old in Wondo Genet district, Sidama zone, SNNPR, Ethiopia. Current pediatric research
Amsalu ET, Akalu TY, Gelaye KA (2019) Spatial distribution and determinants of acute respiratory infection among under-five children in Ethiopia: Ethiopian Demographic Health Survey 2016. PLoS ONE 14(4):e0215572
Bawankule R, Singh A, Kumar K, Shetye S (2017) Does measles vaccination reduce the risk of acute respiratory infection (ARI) and diarrhea in children: a multi-country study? PLoS ONE 12(1):e0169713
Bazie GW, Seid N, Admassu B (2020) Determinants of community-acquired pneumonia among 2 to 59 months of age children in Northeast Ethiopia: a case-control study. Pneumonia 12(1):1–10
Child Y (2011) Infant and young child feeding. Nutrition 11–13
Child WHODo, Health A, Organization WH, UNICEF (2005) Handbook IMCI: integrated management of childhood illness. World Health Organization, Geneva
Chopra M, Mason E, Borrazzo J, Campbell H, Rudan I, Liu L et al (2013) Ending of preventable deaths from pneumonia and diarrhea: an achievable goal. Lancet 381(9876):1499–1506
Eddy O, Lukens T, Nazarian D, Howell J (2005) Community-acquired pneumonia: from common pathogens to emerging resistance. Emerg Med Pract + Em Pract Guidel Update. 7(12):1–22
Fekadu GA, Terefe MW, Alemie GA (2014) Prevalence of pneumonia among under-five children in Este Town and the surrounding rural Kebeles, Northwest Ethiopia: a community-based cross-sectional study. Sci J Public Health 2(3):150–155
Gedefaw M, Berhe R (2015) Determinates of childhood pneumonia and diarrhea with special emphasis to exclusive breastfeeding in north Achefer district, northwest Ethiopia: a case–control study. Open J Epidemiol 5(02):107
Harris M, Clark J, Coote N, Fletcher P, Harnden A, McKean M et al (2011) British Thoracic Society guidelines for the management of community-acquired pneumonia in children: update 2011. Thorax 66(Suppl 2):ii1–ii23
Hershey CL, Doocy S, Anderson J, Haskew C, Spiegel P, Moss WJ (2011) Incidence and risk factors for malaria, pneumonia, and diarrhea in children under 5 in UNHCR refugee camps: a retrospective study. Confl Health 5(1):1–11
Hiko D, Kebeta T (2017) Prevalence and associated factors of Pneumonia among children 2–59 months of age in Gumay district, South-west of Ethiopia, 2017
Lema K, Murugan R, Tachbele E (2018) Prevalence and associated factors of pneumonia among under-five children at public hospitals in Jimma zone, South West of Ethiopia, 2018. J Pulmonol Clin Res 2(1): 25–31. J Pulmonol Clin Res 2018 Volume 2 Issue. 2018;1.
Mulholland K (2007) Childhood pneumonia mortality—a permanent global emergency. Lancet 370(9583):285–289
Organization WH (2014) Revised WHO classification and treatment of pneumonia in children at health facilities: quick reference guide. World Health Organization, Geneva
Pneumonia EPCD (2013) Diarrhea by 2025. The integrated Global Action Plan for Pneumonia and Diarrhea (GAPPD). World Health Organization, United Nations Children’s Fund
Pore PD, Ghattargi CH, Rayate MV (2010) Study of risk factors of Acute Respiratory Infection (ARI) in under-fives in Solapur. Nat J Community Med 1(2):64–67
Rahman SS, Khatun A, Azhar BS, Rahman H, Hossain S (2014) A study on the relationship between nutritional status and prevalence of pneumonia and diarrhea among preschool children in Kushtia. Pediatr Res Int J 2014:i1-10
Rashid MM, Chisti MJ, Akter D, Sarkar M, Chowdhury F (2017) Antibiotic use for pneumonia among children under-five at a pediatric hospital in Dhaka city. Bangladesh Patient Prefer Adherence 11:1335
Rudan I, Nair H, Marušić A, Campbell H (2013) Reducing mortality from childhood pneumonia and diarrhea: the leading priority is also the greatest opportunity. J Glob Health. https://doi.org/10.7189/jogh.03.010101
Walker CLF, Rudan I, Liu L, Nair H, Theodoratou E, Bhutta ZA et al (2013) Global burden of childhood pneumonia and diarrhea. Lancet 381(9875):1405–1416
Acknowledgements
I would like to thank the study participants, data collectors, and supervisors who were involved in this study and spent their valuable time responding to my study.
Limitation of study
Since the study was conducted at community based, some variables like radiological finding, iv fluid, antibiotics and hospital admission data were not included, so I recommend future researcher to include those variables.
Funding
No funding was obtained for this study.
Author information
Authors and Affiliations
Contributions
LAM contributed to generating topics, writing proposals, data collection, analyses, development of the manuscript, processed publication. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethical approval and consent to participation
Ethical clearance was obtained from the Institutional Review Board (IRB) of Debre berhan University, and a support letter was issued from Debre Berhan University and then delivered to the Angolela Tera district Health office and finally to the respective health institution. In addition, informed consent was obtained from the parents to confirm their willingness to participate after explaining the objective of the study.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Mengstie, L.A. Prevalence of pneumonia and associated factors among children aged 6–59 months in Angolela Tera district, North Shoa, Ethiopia, 2021, community-based cross-sectional study. Bull Natl Res Cent 46, 231 (2022). https://doi.org/10.1186/s42269-022-00921-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s42269-022-00921-x