Abstract
Background
Rapid sequence induction is a well-established anesthetic procedure used in patients with a high risk of gastric aspiration. Suxamethonium has been the drug of choice; however, it carries potential risks and sometimes fatal outcomes. The aim of our study was to compare rocuronium after pretreatment with dexmedetomidine, to suxamethonium in providing excellent intubating conditions in rapid sequence induction in adults. Patients were randomly allocated to one of two groups, of 120 each. Control group (SS), patients received pretreatment with 10 ml 0.9% saline over 10 min and suxamethonium 1mg/kg. Experimental group (DR), received pretreatment with dexmedetomidine 1 μg/kg in 10 ml 0.9% saline over 10 min and rocuronium 0.6 mg/kg. Our primary endpoint was the number of patients who scored “excellent” on intubation conditions score, while secondary outcomes were hemodynamics and adverse events.
Results
The rate of excellent intubating conditions in the DR group 46% was insignificantly less (P value = 0.548) than that of the SS group 49% (relative risk (RR) of DR compared to SS = 1.04, with a confidence interval (CI) of 0.91–1.48. The percentage of patients with adverse events in the SS group was (30%) nearly more than twofold higher than that of the DR group (11%). A significant difference (P value = 0.016) in the incidence of excellent intubating conditions was higher in the female gender 59% compared to the male gender 38% (adjusted RR = 0.98, with a confidence interval of 0.79–1.1).
Conclusion
A combination of dexmedetomidine 1μg/kg and standard intubating dose of rocuronium 0.6 mg/kg provided comparable endotracheal intubation conditions to suxamethonium 1 mg/kg during RSI and might be used as an alternative to suxamethonium in situations where suxamethonium is contraindicated.
Trial registration
ClinicalTrials.gov Identifier: NCT04709315
Similar content being viewed by others
Background
Rapid sequence induction (RSI) is a well-established anesthetic procedure routinely used in emergency and trauma settings, as well as in elective situations when there is a high risk of regurgitation/aspiration (Sinclair & Luxton, 2005).
RSI technique briefly involves a rapid successive administration of an anesthesia-inducing agent, muscle relaxant followed by tracheal intubation not further than 1 min after giving muscle relaxant (Kwon et al., 2013).
The ideal neuromuscular relaxant agent used for RSI should have a quick onset, in addition to a short duration of action, which is a major advantage in a trauma setting, as it mitigates the risk of aspiration and desaturation when endotracheal intubation should be performed as early as possible. It also should have a quick offset to ensure that if trials at endotracheal intubation were unsuccessful, there would be quick neuromuscular recovery, with a return to spontaneous breathing before the patient starts desaturation. Moreover, it should have minimal cardiovascular or systemic side effects (Morris & Cook, 2001).
Unfavorable intubation conditions that should be avoided include resisting the insertion of the laryngoscope, inability to visualize the cords, and patient reaction to the intubation and cuff inflation, e.g., coughing and diaphragmatic contraction (Morris & Cook, 2001).
Typically, suxamethonium (succinylcholine) has been the neuromuscular agent of choice for RSI as it has the quickest onset and offset of action compared to other muscle relaxants. However, it has potentially risky—sometimes fatal—side effects that makes it far from being an ideal neuromuscular blocking agent in RSI (Eti et al., 2000).
Of the currently available non-depolarizing neuromuscular blocking agent, rocuronium got the fastest onset of action and thus has been suggested as a possible alternative to succinylcholine in RSI. Various studies have shown that rocuronium in a dose of 1 mg/kg provides acceptable intubating conditions within 60 s in the majority of patients, while its duration of action is up to 40 min rendering it an intermediate-acting muscle blocker (Mazurek et al., 1998; Tran et al., 2017). However, higher doses (1–1.2 mg/kg) are commonly administered during RSI because the time onset with these doses has been observed to almost parallel those of succinylcholine. As with other agents, the duration of action increases when larger doses are administered so that 60–90 min of neuromuscular blockade occurs following a dose of 1.0 mg/kg (Tran et al., 2017). Nevertheless, higher doses have a long duration of action and may pose a risk in patients with unpredictable difficult intubation (Hiestand et al., 2011).
Dexmedetomidine (DEX) is a selective centrally acting α2 adrenergic receptor agonist that has been used successfully as a procedural adjuvant, e.g., to minimize the stress response to laryngoscopy during endotracheal intubation and has gained popularity in the peri-operative period (Schultz et al., 2001a), due to its unique action as anxiolytic, sedative with no respiratory depression, analgesic, opioid-sparing effect, and its ability to decrease overall anesthetic requirements (David & Mostafa, 2001).
The aim of our study was to compare a combination of DEX (1 μg/kg) and standard intubating dose of rocuronium (0.6 mg/kg) to suxamethonium (1 mg/kg) as regard endotracheal intubation conditions during RSI in adults.
Methods
This controlled, randomized, double-blinded study was commenced after approval by the Faculty of Medicine, South Valley University. Registration code: AIP029/124. Written consent was obtained from all participants and the trial was conducted in South Valley University Hospital, between January 2020 and December 2020. It was registered with ClinicalTrials.gov Identifier: NCT04709315. This clinical research was carried out in accordance with the Helsinki Declaration 2013.
Eligibility criteria were assessed in the pre-anesthetic consultation by a member of the anesthesia team and included patients from both genders aged between 18 to 60 years with an American Society of Anesthesiologists (ASA) physical status I or II and booked for elective surgery of more than 60-min duration. Exclusion criteria entailed those with a Mallampati score of III or IV, neuromuscular disease, a history of allergy to the studied drugs, malignant hyperthermia, patients taking anticonvulsants or aminoglycoside antibiotic, hepatic dysfunction, renal dysfunction, cardiovascular dysfunction, electrolyte imbalance, morbidly obese with a body mass index (BMI) more than 30 kg/m2, and pregnant or nursing mothers. Patients were randomly allocated to one of two groups, of 120 each. The saline pretreatment/suxamethonium group (SS group) and Dex pretreatment/rocuronium group (DR group). In the SS group, patients received pretreatment with 10 ml 0.9% saline over 10 min, and succinylcholine 1mg/kg was the intubating muscle relaxant, while in the DR group, patients received pretreatment with Dex 0.1 μg/kg in 10 ml 0.9% saline over 10 min and rocuronium 0.6 mg/kg was the intubating muscle relaxant. Pretreatments were given over 10 min using an infusion pump (Sapphire plus, ICU Medical, Inc. San Clemente, CA, USA). All patients were premedicated with midazolam 0.05 mg/kg orally, or intramuscularly, half an hour and an hour, respectively, before pretreatment was administered.
As soon as the pretreatment was completed, intravenous (IV) fentanyl 1 μg/kg and preoxygenation for 3 min with a facemask, after which anesthesia was induced with IV propofol 2 mg/kg. The standardized intubating procedure was carried out that on the loss of consciousness, the neuromuscular relaxant drug was given per protocol, and, 45 s later, the intubating anesthetist was called in the operating room; at 50 s, laryngoscopy was introduced, and at 60 s, the trachea would be expectedly successfully intubated. No ventilation was carried out before orotracheal intubation. No cricoid pressure was performed because evidence does not any more support the use of cricoid pressure in rapid sequence (Priebe, 2016). Standard anesthetic monitoring included a 5-lead electrocardiogram (ECG), peripheral nerve stimulator, capnography, pulse oximetry, and temperature.
Using website software, enrolled patients were randomized, in a 1:1 ratio for gender, to one of two groups. Treatment allocation was assigned using a randomized block design. All drugs administered in the control group (saline 0.9% suxamethonium; 1mg/kg) and experimental group (Dex; 1 μg/kg rocuronium; 0.6mg/kg), were prepared in 10 ml syringe and were given via an infusion pump. Saline and Dex were given over 10 min immediately prior to induction. It is known that suxamethonium administration is associated with skeletal muscle fasciculations, and thus, satisfactory blinding would be a challenge. Multiple precautions were undertaken to mitigate observer bias: First, we designed our protocol that the persons who prepared the experimented drugs was different from the anesthetist who was responsible for the administration of all medications during pretreatment, induction, and maintenance, and he also was responsible for the patient throughout the surgical procedure till the patient was ready to transfer to the postanesthesia care unit (PACU). An independent second anesthetist blinded to the research protocol carried out the intubation and scored the intubating conditions. This independent anesthetist was summoned to enter the operating room 45 s after neuromuscular relaxant was administered and succinylcholine-associated fasciculations had waned away, and the patient was ready for intubation. To minimize performer and interobserver bias, all intubations were conducted by only two designated senior consultants.
Our primary outcome was the number of patients who scored “excellent” on intubation condition score. Intubating conditions were scaled as excellent, good, or poor in accordance with the guidelines set by Good Clinical Research Practice in Neuromuscular Research (Fuchs-Buder et al., 2007). This score is based on a triad of variables: how easy to insert the laryngoscope, the anatomical position of the vocal cords, and how patients react to the introduction of the endotracheal tube and cuff inflation (Table 1) (Fuchs-Buder et al., 2007). Unsuccessful intubation was defined as the inability to intubate the trachea within 30 s after laryngoscopy or within 80 s after the muscle relaxant has been given. In such circumstances, the “can-ventilate, cannot intubate” guideline was followed.
Our secondary outcomes were hemodynamics and adverse events, if any. Hemodynamics (heart rate and mean blood pressure) were checked at the following time intervals: before induction, before intubation, a minute, and 5 min after intubation. Hypotension was defined as mean arterial pressure of > 40%, Less than baseline reading. Unfavorable incidents associated with pretreatment, administration of muscle relaxant, and during 24 h post-operative were monitored and included nausea/vomiting, pain on injection, skin rash, bronchospasm, edema, erythema, awareness, muscle aches, or otherwise.
Sample size was based on a prior published study in which 110 patients were needed in each group, setting a level of statistical significance as α = .05 (2-sided) and β = .1 (Czarnetzki et al., 2020). We randomized 120 patients in each group to compensate for dropouts. The total number of patients available for randomization was therefore 240. Qualitative demographic data as well as intubating conditions were expressed as numbers of patients and percentages, while quantitative demographic data and hemodynamic values were presented as means and standard deviations. Chi-square test was used for comparisons among intubating condition variables as well as the rate of excellent intubating conditions between groups. Two-sided P < .05 was taken as significant. To counteract the problem of multiple comparisons, Bonferroni’s corrected P value was applied (P < 0.05/number of comparisons). Intraoperative and post-operative adverse events were analyzed using a chi-square test. Statistical analyses were calculated using the SPSS software, version 23.
Results
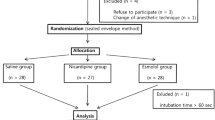
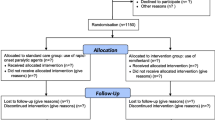
Figure 1, a flow chart of our experiment, exhibits that a total of 320 patients were enrolled to assess for eligibility for the study. Eighty patients were excluded. Initially, a total of 240 patients were equally randomized between SS and DR groups of 120 patients each. Then, data of 12 patients (7 in the SS group and 5 in the DR group) were not included in the primary outcome analysis for different reasons. Eventually, we ended up analyzing a total data of 228 patients (113 in the SS group and 115 patients in the DR group). The demographic traits of the sample population showed no significant difference between the control and experimental groups (Table 2).
The percentage of excellent intubating conditions was insignificantly (P value = 0.548) higher in the SS group 49% than that in the DR group 46% (Table 3). Moreover, the percentage of excellent ease of insertion of laryngoscopy was insignificantly (P value= 0.44) less in the SS group of 89% compared to the DR group 94%. Table 3 also shows that, the incidence of excellent vocal cord position and excellent patient reaction to intubation were 92% and 52%, respectively, in the SS group, insignificantly higher compared to 89% and 50%, respectively, in the DR group.
Table 4 demonstrates that, after multivariate data analysis was adjusted for gender and the unequal number of patients between the two tested groups, the observed incidence of excellent intubating conditions in DR group 46% was insignificantly less (P value = 0.548) than SS group 49% (RR of DR compared to SS = 1.04, with confidence interval (CI) of 0.91–1.48. Nevertheless, a significant difference (P value = 0.016) in the incidence of excellent intubating conditions was higher in female gender 59% compared to male gender 38% (adjusted RR = 0.98, with a confidence interval of 0.79–1.1).
Out of 240 patients who received the study protocol, 50 patients (21%) suffered from at least one adverse episode (Table 5). The percentage of patients with an adverse event in the SS group was 36 patients out of 120 (30%), nearly more than twofold higher than the DR group: 14 patients out of 120 (11%). During pretreatment with dexmedetomidine, 5 patients (4%) in the DR complained of local pain at the infusion line (2 patients and they withdrew from the study); nausea (1 patient), and skin erythema (1 patient). Table 5 also demonstrates that no patient in the SS group reported any symptoms during this pretreatment phase. A total of 16 patients (7%) presented with symptoms that might be due to administration of the neuromuscular blocking drug: 11 of 119 patients (9%) in the SS group and 5 out of 118 patients (6%) in the DR group. In the SS group, the most common adverse event was skin erythema, 10 cases, with one episode of mild bronchospasm that did not need intervention. No patient manifested mucous membrane edema, due to histamine release. Nevertheless, in the DR group, 3 patients manifested skin erythema which was self-limiting and 2 patients suffered from mild hypotension which was easily managed by adjusting the inhalational anesthetic concentration. At 24 h post-operative visit, no patient reported awareness during induction or anesthesia. However, the most common reported complaint was body muscle aches mainly among the SS group patients: 24 patients of 113 (21%). Only 3 patients out of 115 (2%) in the DR group reported muscle aches. None of the patients required medication for their muscle aches when offered. No life-threatening incidents were recognized throughout the study duration.
Table 6 indicates that there was an insignificant difference between the two groups as regard systolic and diastolic blood pressure at any point of time. However, the mean heart rate was significantly lower in the DR group patients compared to the SS group, at each point of time (at induction, before intubation, 1 min, and 5 min after intubation with P values of 0.041, 0.001, 0.014, 0.020, respectively).
Discussion
Our study showed no significant difference between a combination of dexmedetomidine 1μg/kg and rocuronium 0.6 mg/kg and suxamethonium 1 mg/kg in respect of the effect on the rate of excellent intubating conditions during RSI in adult patients.
Although this study is the first one to use Dex pretreatment with rocuronium in RSI, multiple studies have experimented with the outcome of different doses of rocuronium either as a sole agent or with adjuvants, on the intubating conditions in RSI, with conflicting results (Alanoğlu et al., 2006; Tran et al., 2015). Contrary to our results, Kown et al. compared suxamethonium with a standard rocuronium dose of 0.6 mg/kg. They reported better intubation conditions in the succinyl group.(Sluga et al., 2005) This could be explained as they used a high dose of suxamethonium 1.5 mg/kg and a relatively low dose of rocuronium and they did not use adjuvants in either group. Similar to our results, higher doses of rocuronium (1–1.2 mg/kg) provided comparable intubating conditions to that of suxamethonium (Kwon et al., 2013; Patanwala et al., 2011; Schreiber et al., 2005a).
Combining DEX with a standard dose of rocuronium 0.6 mg/kg, instead of administering high dose rocuronium (1.2 mg/kg) alone, might be regarded as a suitable choice for RSI, as this high dose results in almost doubled recovery time (Schultz et al., 2001b). Moreover, avoiding high doses of rocuronium may permit spontaneous recovery and mitigate the need to antagonize rocuronium with sugammadex, which is expensive and not usually available in many countries (Murphy, 2018). Indeed, if reversal of rocuronium is required, the efficacy of standard reversal doses of sugammadex is not altered in those with Dex pretreatment (Memiş et al., 2008).
Compared with other studies, that reported as high as 80% of their patients had excellent intubation conditions (Fuchs-Buder et al., 2007; Kim et al., 2015; Naguib et al., 2006), substantial low rates of excellent intubating conditions (less than 50%) were observed among our patients in both control and experimental groups. We cannot offer a clear explanation for this observation, although we have undertaken rigorous measures. Standardized protocol was applied to all patients including random allocation of patients, matching of tested drugs, and concealing labels, and participants (patients, personnel who administered tested drugs and who collected data) were blinded to the identity of the tested medications. In order to avoid observer bias two independent anesthetists were in charge of each patient; one administered all medications and was in charge of the patient throughout the whole surgery, and a second anesthetist was responsible for intubation and collecting intubation condition data. Performance bias was mitigated as only two designated senior consultants were in charge of intubation and collecting intubation conditions. Moreover, our sample size was larger than other studies (Czarnetzki et al., 2020; Alanoğlu et al., 2006; Tran et al., 2015; Sluga et al., 2005; Patanwala et al., 2011; Schreiber et al., 2005a; Schultz et al., 2001b; Murphy, 2018; Memiş et al., 2008; Kim et al., 2015; Naguib et al., 2006; El-Kobbia et al., 2015; Park et al., 2013). However, a possible explanation of the observed lower rates of excellent intubation conditions is “omitted data.” Initially, we randomly allocated 240 patients between the control and experimental groups, 120 each. However, we had to omit data and analyzed only data from 228 patients. The number of withdrawn data was higher in the control group (7 patients) than in the experimental group (5 patients). The reasons for deleting those data, in order of frequency, were as follows: Cormack and Lehan grade 3 or 4 (5 patients), taking more than 80 s for intubation (3 patients), patients asked to terminate the study because they felt pain at the infusion site (2 patients), one patient asked to withdraw from the study with no reason, and one patient that needed supplemental propofol. We might hypothesize that if the deleted data were included in the final analysis, the rate of excellent intubation conditions would have been different.
Our experiment also showed that incidence of excellent intubating conditions was notably higher in females than males. This outcome, although not the principal interest of our research, was not unpredicted as gender has its role on the pharmacodynamics of neuromuscular blocking agents and females are more susceptible to the effects of amino-steroid muscle relaxant, e.g., rocuronium than males (Adamus et al., 2007; Adamus et al., 2008; Adamus et al., 2011). Further clinical trials in the future may explore the assumption that Dex-rocuronium combination has more efficacy in females than males.
The all in all incidence of adverse effects among our study population was 21 %. Most of the adverse effects happened with the control group, 73%. The most frequent suxamethonium associated adverse outcome was muscle aches, at 24 h post-operatively. Indeed, suxamethonium associated muscle ache is well documented self- limiting complaint, and respond to simple analgesics, with no long-term consequences (Schreiber et al., 2005b).
Pretreatment associated complications occurred only with Dex pretreated group (4%), none with saline pretreated control group. The side effects were pain at the injection site (two patients and they asked to withdraw from the study due to pain and they were excluded from the final analysis), erythema, and nausea which responded well to reassurance. Also, unfavorable outcomes on administering the neuromuscular relaxant, mainly erythema, have been observed more often with the suxamethonium group. However, they were mild and did not warrant treatment.
No statistically notable difference between groups was observed as regard systolic and diastolic blood pressure at baseline (before induction), and at induction and after intubation. However, there was significant lower heart rate values in the Dex-pretreated rocuronium group than in the suxamethonium group. This was expected as bradycardia is a well-known association with Dex (Fujii & Tanaka-Mizuno, 2018; Bloor et al., 1992). However, it was self-limiting and did not require intervention.
One limitation of this study was that all our patients were premedicated with midazolam an hour before conducting our research protocol, this might have affected the values of our results as midazolam has got muscle relaxant properties through α2 γ-aminobutyric acid A (GABAA) receptors.(Park et al., 2019)
Conclusion
A combination of DEX 1μg/kg and standard intubating dose of rocuronium 0.6 mg/kg provided comparable endotracheal intubation conditions to suxamethonium 1 mg/kg during RSI and might be used an alternative to suxamethonium in situations where it is contraindicated.
Availability of data and materials
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- RR:
-
Relative risk for intervention and gender
- SS group:
-
The saline pretreatment/suxamethonium group: control group
- DR group:
-
Dexmedetomidine pretreatment/ rocuronium group: experimental group
- RSI:
-
Rapid sequence induction
- DEX:
-
Dexmedetomidine
- BMI:
-
Body mass index
- IV:
-
Intravenous
- μg:
-
Microgram
- kg:
-
Kilogram
- PACU:
-
Postanesthesia care unit
References
Adamus M, Gabrhelik T, Marek O (2008) Influence of gender on the course of neuromuscular block following a single bolus dose of cisatracurium or rocuronium. Eur J Anesthesiol 25(7):589–595. https://doi.org/10.1017/S026502150800402X
Adamus M, Hrabalek L, Wanek T, Gabrhelik T, Zapletalova J (2011) Influence of age and gender on the pharmacodynamic parameters of rocuronium during total intravenous anesthesia. Biomed Pap Med Fac Univ Palacky Olomouc Czech Repub 155(4):347–353. https://doi.org/10.5507/bp.2011.050
Adamus M, Koutna J, Gabrhelik T, Hubackova M, Janaskova E (2007) Influence of gender on the onset and duration of rocuronium-induced neuromuscular block. Biomed Pap Med Fac Univ Palacky Olomouc Czech Repub 151(2):301–305. https://doi.org/10.5507/bp.2007.051
Alanoğlu Z, Ateş Y, Yilmaz AA, Tüzüner F (2006) Is there an ideal approach for rapid-sequence induction in hypertensive patients. J Clin Anesth 18(1):34–40. https://doi.org/10.1016/j.jclinane.2005.06.006
Bloor BC, Ward DS, Belleville JP, Maze M (1992) Effects of intravenous dexmedetomidine in humans. II Hemodynamic changes Anesthesiol 77(6):1134–1142. https://doi.org/10.1097/00000542-199212000-00014
Czarnetzki C, Albrecht E, Masouyé P, Baeriswyl M, Poncet A, Robin M et al (2020) Rapid sequence induction with a standard intubation dose of rocuronium after magnesium pretreatment compared with succinylcholine: a randomized clinical trial. Anesth Analg 2020. https://doi.org/10.1213/ANE.0000000000005324 Epub ahead of print. PMID: 33337797.
David R, Mostafa SM (2001) Drugs and the eye. BJA CEPD Rev 1(6):161–165. https://doi.org/10.1093/bjacepd/1.6.161
El-Kobbia N, Doghaim M, Moustafa M, Deifallah A (2015) Comparative study between succinylcholine, rocuronium and magnesium sulphate with rocuronium in rapid sequence induction. Res Opin Anesth Intensive Care 2:57–61
Eti Z, Yayci A, Umuroglu T, Gogus FY, Bozkurt N (2000) The effect of propofol and alfentanil on the increase in intraocular pressure due to suxamethonium and intubation. Eur J Ophthalmol 10(2):105–107. https://doi.org/10.1177/112067210001000202
Fuchs-Buder T, Claudius C, Skovgaard LT, Eriksson LI, Mirakhur RK, Viby-Mogensen J (2007) 8th International Neuromuscular Meeting. Good clinical research practice in pharmacodynamic studies of neuromuscular blocking agents II: the Stockholm revision. Acta Anaesthesiol Scand 51(7):789–808. https://doi.org/10.1111/j.1399-6576.2007.01352.x
Fujii E, Tanaka-Mizuno S, Fujino FM, Furono M, Sugimoto Y, Takabuchi S et al (2018) Dexmedetomidine attenuates the positive chronotropic effects of intravenous atropine in patients with bradycardia during spinal anesthesia: a retrospective study JA. Clin Rep 4(1):70–76. https://doi.org/10.1186/s40981-018-0207-9
Hiestand B, Cudnik MT, Thomson D, Werman HA (2011) Rocuronium versus succinylcholine in air medical rapid-sequence intubation. Prehosp Emerg Care 15(4):457–463. https://doi.org/10.3109/10903127.2011.569853
Kim MH, Oh AY, Han SH, Kim JH, Hwang JW, Jeon YT (2015) The effect of magnesium sulphate on intubating condition for rapid-sequence intubation: a randomized controlled trial. J Clin Anesth 27(7):595–601. https://doi.org/10.1016/j.jclinane.2015.07.002
Kwon MA, Song J, Kim JR (2013) Tracheal intubation with rocuronium using a “modified timing principle”. Korean J Anesthesiol 64(3):218–222. https://doi.org/10.4097/kjae.2013.64.3.218
Mazurek AJ, Rae B, Hann S, Kim JI, Castro B, Coté CJ (1998) Rocuronium versus succinylcholine: are they equally effective during rapid-sequence induction of anesthesia. Anesth Analg 87(6):1259–1262
Memiş D, Turan A, Karamanlıoğlu B, Şeker Ş, Pamukçu Z (2008) Dexmedetomidine reduces recuronium dose requirement in sevoflrane anaesthesia. Curr Anaesth Crit Care 19(3):169–174. https://doi.org/10.1016/j.cacc.2007.07.001
Morris J, Cook TM (2001) Rapid sequence induction: a national survey of practice. Anaesthesia 56(11):1090–1115
Murphy GS (2018) Neuromuscular monitoring in the perioperative period. Anesth Analg 126(2):464–468. https://doi.org/10.1213/ANE.0000000000002387
Naguib M, Samarkandi AH, El-Din ME, Abdullah K, Khaled M, Alharby SW (2006) The dose of succinylcholine required for excellent endotracheal intubating conditions. Anesth Analg 102(1):151–155. https://doi.org/10.1213/01.ANE.0000181320.88283.BE
Park JW, Min BH, Park SJ, Kim BY, Bae SI, Han SH, Hwang JW, Kim JH (2019) Midazolam premedication facilitates mask ventilation during induction of general anesthesia: a randomized clinical trial. Anesth Analg 129(2):500–506. https://doi.org/10.1213/ANE.0000000000003707
Park SJ, Cho YJ, Oh JH, Hwang JW, Do SH, Na HS (2013) Pretreatment of magnesium sulphate improves intubating conditions of rapid sequence tracheal intubation using alfentanil, propofol, and rocuronium: a randomized trial. Korean J Anesthesiol 65(3):221–227. https://doi.org/10.4097/kjae.2013.65.3.221
Patanwala AE, Stahle SA, Sakles JC, Erstad BL (2011) Comparison of succinylcholine and rocuronium for first-attempt intubation success in the emergency department. Acad Emerg Med 18(1):10–14
Priebe H-J (2016) Evidence no longer supports use of cricoid pressure. BJA Bri J Anaesth 117(4):537–538. https://doi.org/10.1093/bja/aew290
Schreiber JU, Lysakowski C, Fuchs-Buder T, Tramèr MR (2005a) Prevention of succinylcholine-induced fasciculation and myalgia: a meta-analysis of randomized trials. Anesthesiology 103(4):877–884. https://doi.org/10.1097/00000542-200510000-00027
Schultz P, Ibsen M, Østergaard D, Skovgaard LT (2001a) Onset and duration of action of rocuronium–from tracheal intubation, through intense block to complete recovery. Acta Anaesthesiol Scand 45(5):612–617. https://doi.org/10.1034/j.1399-6576.2001.045005612.x
Sinclair RC, Luxton MC (2005) Rapid sequence induction. Contin Educ Anaesth Crit Care Pain 5(2):45–48. https://doi.org/10.1093/bjaceaccp/mki016
Sluga M, Ummenhofer W, Studer W, Siegemund M, Marsch SC (2005) Rocuronium versus succinylcholine for rapid sequence induction of anesthesia and endotracheal intubation: a prospective, randomized trial in emergent cases. Anesth Analg 101(5):1356–1361. https://doi.org/10.1213/01.ANE.0000180196.58567.FE
Tran DTT, Newton EK, Mount VAH, Lee JS, Mansour C, Wells GA, Perry JJ (2017) Rocuronium vs. succinylcholine for rapid sequence intubation: a Cochrane systematic review. Anaesthesia 72(6):765–777. https://doi.org/10.1111/anae.13903
Tran DTT, Newton EK, Mount VAH, Lee JS, Wells GA, Perry JJ (2015) Rocuronium versus succinylcholine for rapid sequence induction intubation. Cochrane Database Syst Rev 10:CD002788. https://doi.org/10.1002/14651858.CD002788.pub3
Acknowledgements
Not applicable
Funding
No other source of funding rather than South Valley University.
Author information
Authors and Affiliations
Contributions
The author read and approved the manuscript. OHS has contributed to designing, recruiting, and writing the manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Approval by Faculty of Medicine, South Valley University. Registration code: AIP029/124. Written consent was obtained from all participants. It was retrospectively registered with ClinicalTrials.gov Identifier: NCT04709315.
Consent for publication
Not applicable
Competing interests
The author declares that there are no competing interests
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Salman, O.H. Comparison between single-dose suxamethonium and rocuronium after pretreatment with dexmedetomidine in rapid sequence induction. Ain-Shams J Anesthesiol 14, 1 (2022). https://doi.org/10.1186/s42077-021-00200-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s42077-021-00200-3