Abstract
Background
The glossopharyngeal nerve is both a sensitive and motor entity that emerges from the posterior lateral sulcus of the bulb and exits the skull through the jugular foramen. Schwannomas arising from glossopharyngeal nerves are extremely rare, and the clinical and imaging features of glossopharyngeal schwannomas closely resemble that of acoustic schwannomas.
Case presentation
We report a case of a 65-year-old female patient with glossopharyngeal neurinoma of incidental finding on brain CT scan requested after she sustained a minor traumatic brain injury. She was taken to the operating room, and the tumor was excised endoscopically via a retrosigmoid approach and the postoperative course was simple and uneventful. Histopathology of the sample showed short spindle-shaped cells with poor atypia proliferated in fascicles, and shelf-like arrangement of nuclei was seen partially, which was in keeping with a neurinoma.
Conclusions
Glossopharyngeal neurinoma may not present with obvious symptoms and signs related to its compression and may also be found incidentally compared to its counterpart vestibular schwannoma.
Similar content being viewed by others
Explore related subjects
Find the latest articles, discoveries, and news in related topics.Background
Neurinomas or schwannomas (neurilemmomas) are encapsulated and generally benign tumors that result from the abnormal proliferation of Schwann cells, which are responsible for generating myelin [1]. Schwannomas of the glossopharyngeal nerve are extremely rare tumors of the posterior fossa. In a 100-year review, a total of 42 cases were found between 1908 and 2008; in this review, most common clinical data were associated with its location, the most common being cochlear vestibular symptoms and symptoms of glossopharyngeal nerve function [2].
Intracranial schwannomas comprise around 7–10% of primary intracranial tumors. They are divided into vestibular schwannomas, which are the majority, and non-vestibular schwannomas. Non-vestibular schwannomas make up around 0.8–8% of all intracranial schwannomas. Among non-vestibular schwannomas the 5th, 7th, and 12th cranial nerves are the most common sites, in decreasing frequency. Glossopharyngeal schwannomas are relatively uncommon and are often lumped with jugular foramen schwannomas [3].
Despite its accuracy, magnetic resonance imaging is not diagnostic of a ninth nerve schwannoma. This is because the schwannoma may be primarily localized to the cerebellopontine angle and may not cause enlargement of the jugular foramen. The diagnosis is possible only at surgery, once attachment to the ninth cranial nerve is seen [4].
The glossopharyngeal nerve is visualized through the choroid plexus of the lateral recess of the fourth ventricle and the dural entrance porus at the jugular foramen in the subarachnoid space. Removal of lesions involving the jugular foramen region requires detailed knowledge of the anatomy and anatomical landmarks of the related area, especially the lower cranial nerves. The glossopharyngeal nerve courses along the uppermost part of the jugular foramen and is well hidden in the deep layers of the neck, making this nerve the most difficult one to identify during surgery [5]. Endoscopic surgery allows for a smaller craniotomy, less dissection and minimal retraction, without compromising the goals of the operation [6].
The aim of reporting this case is that sometimes glossopharyngeal neurinoma can be discovered incidentally during routine check-up or during imaging for other reasons.
Case presentation
We report a case of a 65-year-old female patient who presented to us with a history of headaches after she slipped and fell and landed by hitting her head on a rock. She lost consciousness for few minutes. Her past history was unremarkable. On arrival at our emergency room, she was fully conscious and vital signs were in the normal limits; neurological examination revealed no deficit.
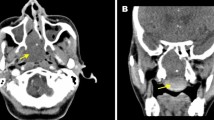
A brain CT scan was requested which showed nothing related to the trauma but showed an isodense mass lesion in the left cerebellopontine angle which enhanced in postcontrast scan (Fig. 1A, B); following this, an MRI scan was requested which showed the same lesion which was hyperintense on T1W1 and iso to hypointense on T2W1 (Fig. 2) and CT angio (Fig. 3A) and DSA (Fig. 3B) were done and showed that the lesion was poorly vascularized. A diagnosis of vestibular schwannoma was made at that moment.
The patient was prepared after written consent and taken to the operating theater a month later. Under the monitoring of brainstem auditory evoked potentials (BAEP), a retrosigmoid approach (Fig. 4) was performed and intraoperatively the tumor was noted to be attached to the glossopharyngeal nerve instead. Excision was done endoscopically using an ultrasonic aspirator and working between the glossopharyngeal nerve and the vagus nerve (Fig. 5A, B). The glossopharyngeal nerve and the lower cranial nerves were preserved. Removal rate was near total by leaving the part of the tumor on the perineurium to avoid the nerve damage. The dura was closed in a watertight fashion; the bone flap was placed back and fixed by titanium plates and screws, and the wound was reapproximated in layers. The sample of the tumor was taken and sent for histopathology examination, and the results came back and showed short spindle-shaped cells with poor atypia proliferate in fascicles. A shelf-like arrangement of nuclei was seen partially (Fig. 6A–D), which was in keeping with a neurinoma. Patient was discharged on day 4 postoperative, and currently, she is doing well with no complications.
Discussion
Glossopharyngeal (that is, cranial nerve IX) schwannomas are extremely rare nerve sheath tumors that frequently mimic the more common vestibular schwannoma in their clinical as well as radiographic presentation [7].
They most commonly affect men and, as with other intracranial schwannomas, the age of presentation ranges between the third and the fifth decade of life with the youngest patient reported of four-year-old male [7]. Two major classifications for glossopharyngeal schwannomas have been proposed. Both are based on the extent of the tumor in the cerebellopontine angle, jugular foramen and extracranial space. Type A tumors, involving the cerebellopontine angle with minimum enlargement of jugular foramen, are the most common in the literature. They typically present with vestibulocochlear dysfunction. Type B which is foraminal and Type C (extracranial and/or foraminal) are the least common; they present with CN IX and XII deficits, mainly hoarseness and decreased gag reflex [3, 7].
Glossopharyngeal nerve schwannoma is an infrequent tumor which may not always produce lower cranial nerve deficit, and clinical presentation may mimic an acoustic neurinoma. Hence, it is usually not recognized preoperatively [8].
Clinical presentation of intracranial schwannoma is usually characterized by local cranial nerve dysfunction. However, since the posterior fossa is a small compartment, multiple cranial nerves may be affected simultaneously. Palsies of the ninth cranial nerve are unusual, and symptoms of ninth nerve dysfunction may not become apparent until there is bilateral involvement like our patient who had no symptoms until it was discovered incidentally though the tumor was quite big; this so important clinical feature should be further studied in comparison with the acoustic neurinoma which hearing symptoms seem to appear earlier in the course of disease. Furthermore, this neurinoma usually grows toward the cerebellopontine angle (CPA) and initially affects the facial–acoustic nerve complex. Therefore, hearing loss is the most common symptom in 90–93% of cases like in acoustic neurinoma, hoarseness and decreased gag reflex ranked next in the review of the literature [9, 10].
Radiologically, compared to vestibular schwannomas, lower cranial nerve schwannomas originating from CN IX, X, XI tend to be centered in the jugular foramen. Schwannomas originating from CN IX and X may extend to the deep neck parapharyngeal space, while schwannomas from CN XII may enlarge the hypoglossal foramen [11].
Our patient underwent a part from CT scan, MRI scan, CTA and DSA in preoperatively for differential diagnosis and to check the blood supply; occasionally schwannomas can mimic paragangliomas on conventional cross-sectional imaging. Digital subtraction angiography (DSA) remains the gold standard technique to differentiate between the two entities [12].
The ideal primary treatment of these tumors is total surgical removal. The management of these lesions is particularly challenging as a result of the complex anatomic location and potential postoperative complications [13]. A purely endoscopic retrosigmoid approach was performed for excision of the lesion in park bench position under guidance of neuronavigation; this went well and she woke up from general anesthesia without neurological deficit. The endoscope allowed us easy access to the root entry zone (REZ) of lower cranial nerves through the keyhole and easy access to the jugular foramen by using a 30°. Our tumor removal rate was near total; we did not remove the small part of the tumor attached to the perineurium to avoid the nerve damage (Fig. 7).
The endoscope offers a highly illuminated and extremely detailed view of the tumor and the anatomic structures within the surgical field, adding greatly to the safety of surgery. Furthermore, the panoramic view and large depth of focus of the endoscope result in greater ease of orientation within the surgical field with significant reduction of the number of times the viewing angle needs to be changed during the procedure [14].
Conclusion
Glossopharyngeal neurinoma may not present with obvious symptoms and signs related to its compression and may also be found incidentally compared to its counterpart vestibular schwannoma. Radiologically, it is usually not recognized preoperatively, and usually the diagnosis is possible only at surgery when attachment to the ninth cranial nerve is especially better seen while using endoscopic keyhole approaches.
Availability of data and materials
Not applicable.
Abbreviations
- BAEP:
-
Brainstem auditory evoked potential
- CN:
-
Cranial nerve
- CPA:
-
Cerebellopontine angle
- CT:
-
Computed tomography
- CTA:
-
Computed tomography angiography
- DSA:
-
Digital subtraction angiography
- MRI:
-
Magnetic resonance imaging
- T1WI:
-
T1 weighted imaging
- T2WI:
-
T2 weighted imaging
- REZ:
-
Root entry zone
References
Asadi M, Mohseni M, Jahanshahi F, Esmaeili A, Mohsenifar Z. Schwannoma (neurilemmoma) of tongue: a rare case presentation and review of literature. Clin Case Rep. 2023;11(4):e7235.
Vorasubin N, Sang UH, Mafee M, Nguyen QT. Glossopharyngeal schwannomas: a 100 year review. Laryngoscope. 2009;119(1):26–35.
Darwish H, Adada B. A small glossopharyngeal schwannoma presenting with intractable vomiting: case presentation and literature review. World Neurosurg. 2018;115:101–4.
Agrawal A, Pandit L, Bhandary S, Makannavar JH, Srikrishna U. Glossopharyngeal schwannoma: diagnostic and therapeutic aspects. Singap Med J. 2007;48(7):e181-185.
Ozveren MF, Türe U. The microsurgical anatomy of the glossopharyngeal nerve with respect to the jugular foramen lesions. Neurosurg Focus. 2004;17(2):E3.
Shahinian HK, Eby JB, Ocon M. Fully endoscopic excision of vestibular schwannomas. Minim Invasive Neurosurg MIN. 2004;47(6):329–32.
Thomas JA, Bank WO, Myseros JS. Glossopharyngeal schwannoma in childhood. J Neurosurg Pediatr. 2008;2(2):130–2.
Gupta V. Glossopharyngeal schwannoma: a case report and review of literature. Neurol India. 2002;50(2):190.
Rapanà A, Lamaida E, Bracale C, Lepore P, Pizza V, Graziussi G. Glossopharyngeal schwannoma, an uncommon posterior fossa tumor: diagnostical and therapeutical aspects: a case report. Clin Neurol Neurosurg. 1997;99(3):196–8.
Zhao H, Li X, Lv Q, Yuan Y, Yu H. A large dumbbell glossopharyngeal schwannoma involving the vagus nerve: a case report and review of the literature. J Med Case Rep. 2008;2(1):334.
Khoo WX, Yuen HW, Chen MW, Tan TY, Hui NJ. Glossopharyngeal schwannoma as a differential for a cerebellopontine angle mass. Otolaryngol Case Rep. 2022;1(23):100405.
Suthiphosuwan S, Bai HD, Yu E, Bharatha A. Computed tomography angiography lightbulb sign: characteristic enhancement pattern on neck computed tomography angiography in differentiating paraganglioma from schwannoma of the carotid space. Neuroradiol J. 2020;33(5):437–42.
Sanna M, Bacciu A, Falcioni M, Taibah A. Surgical management of jugular foramen schwannomas with hearing and facial nerve function preservation: a series of 23 cases and review of the literature. Laryngoscope. 2006;116(12):2191–204.
Azab WA. Purely endoscopic retrosigmoid approach for excision of a large multicystic hypoglossal schwannoma. World Neurosurg. 2022;168:133.
Acknowledgements
Not applicable
Funding
Nil.
Author information
Authors and Affiliations
Contributions
KDMK helped in conceptualization, methodology and writing; AS, YY were involved in collection of imaging and arrangement, visualization, investigation; KT, KKNK, YK contributed to supervision, validation, reviewing and editing.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Ethical approval and consent to participate were obtained.
Consent for publication
Consent for publication was obtained from the patient.
Competing interests
Authors declare no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Kabulo, K.D.M., Takeuchi, K., Yamada, Y. et al. Glossopharyngeal neurinoma of incidental finding in a 65-year-old female patient: case report. Egypt J Neurosurg 38, 53 (2023). https://doi.org/10.1186/s41984-023-00226-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s41984-023-00226-9