Abstract
Background
More than two million early care and education (ECE) providers care for young children in the USA each day. These providers tend to earn low wages and many are enrolled in public assistance programs. Nearly all ECE providers are female and they are disproportionately women of color. Despite the fact that these attributes place the ECE workforce at greater risk of chronic disease, the health status of the workforce is not established and the availability and effectiveness of interventions to improve their health status is also not known.
Methods
We conducted a scoping review of both the published literature and current practice to identify all articles and interventions targeting the health status of the ECE workforce. Our search strategy identified scientific articles published in English within the past 10 years as well as any interventions targeting the ECE workforce that have been implemented within the past 3 years. Data from both scientific articles and practice were extracted using systematic methods and summarized.
Results
Thirteen studies described some component of physical health including diet quality (11 studies), physical activity (8 studies), and height/weight/body mass index (7 studies), and 21 studies assessed component(s) of mental health including depression (15 studies), stress (8 studies), and mindfulness (3 studies). ECE providers reported a high prevalence of overweight, obesity, and chronic disease diagnoses and spend significant time being sedentary, and some report low diet quality. Mental health concerns in this population include depression and high stress. Eleven interventions targeting ECE workforce wellness were also identified; most focused on nutrition, physical activity and/or stress.
Conclusion
The limited evidence available for review describes a workforce in need of health promotion interventions to address high levels of mental and physical health challenges, some above and beyond peers with comparable demographic characteristics. Several promising interventions were identified from both the published and unpublished literature; these interventions should be further implemented and evaluated to assess their impact on the workforce.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Background
In the United States (USA), more than two million early care and education (ECE) providers care for approximately ten million young children every day [1]. The ECE system in the USA serves children from birth through 6 years of age and includes several program types: child care centers that can be for-profit or non-profit, Early Head Start and Head Start Programs that are funded through grants from the federal government to serve children from low-income households, pre-kindergarten programs available in some jurisdictions for children age 3–4 years and family child care programs where a small number of children receive care from one or more adults in a home setting [2]. The ECE workforce that supports this system is comprised of populations that are considered higher risk for chronic disease. ECE providers tend to earn low wages ($11.17/h versus $18.50/h for all occupations), and more than half of all ECE providers are enrolled in at least one public support program, such as Medicaid or Supplemental Nutrition Assistance. Nearly all ECE providers are female and they are disproportionately women of color [3] (see Table 1 for more demographic characteristics of the ECE workforce in the USA).
Just 15% of the ECE workforce receives employer-sponsored health insurance, compared to 49.9% of workers in other occupations [3]. According to the Early Childhood Workforce Index, in 2012, prior to the full implementation of the Affordable Care Act (ACA), nearly 25% of center-based staff, and 21–28% of home-based providers were uninsured. A few studies conducted after Medicaid (publicly funded health insurance) expansion have shown that more ECE providers are enrolling in Medicaid as it is made available in their states [1]. However, given that only 33 states have expanded Medicaid coverage and lack of publicly available data, it is difficult to get the full picture of health insurance coverage for this population [1]. Health disparities and increased chronic disease risk among people with low socioeconomic status, racial minorities and the uninsured is well-documented [4,5,6]. Despite a potentially elevated risk for chronic disease, little research has been done on the health of the ECE workforce or on the effectiveness of non-clinical health interventions that may reduce chronic disease risk within this population.
Worksite wellness programs are growing in popularity as a way to improve employee productivity, retention, and job satisfaction and lower healthcare costs [7]. These programs typically focus on modifiable health behaviors such as smoking, diet, physical activity, and receiving cardiovascular disease screenings. However, worksite wellness programs are not widely available to the ECE workforce [8, 9]. Most ECE settings operate independently or within small organizations that may not have the resources to offer worksite wellness programs. One exception is ECE settings that are embedded within larger organizations (e.g., large companies, universities, government settings) where the ECE workforce has access to wellness programs offered organization-wide.
The purpose of this project was to establish the current state of the science with regards to ECE workforce health status as well as begin to understand the current state of practice.
Methods
We used a scoping review approach to collect and describe this emerging field [10, 11]. This approach allows for a more flexible integration of different types of evidence, as is appropriate for a new field. We compiled both published, peer-reviewed evidence, and information on unpublished interventions and programs in an effort to identify what is currently known about the health status of the ECE workforce and examples of interventions currently being implemented to improve health status.
Data sources
We used two different procedures to gather data for this scoping review, one focused on the published literature and another on practice. For the published literature, we first searched both PubMed and Google Scholar. Search terms encapsulated the environment (child care or daycare or early care and education or preschool or head start), the target population (workforce or employee or worksite or teacher or provider) and at least one component of health (health or wellness or stress or well-being). We also conducted hand searches of the reference sections of relevant papers and forward citation searches.
For practice, we disseminated a call for interventions via several different professional channels focused on the ECE workforce in the USA (e.g., Child Care Aware of America, the CDC’s Division of Nutrition, Physical Activity and Obesity’s Early Care and Education News Blast, Nemours Children’s Health System). In addition, the authors reached out directly to individuals and organizations to inquire about any relevant programs.
Study selection
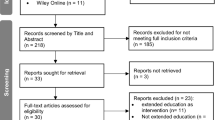
Following the searches, a multi-step review process was used to select publications to include in the review. For the published literature, inclusion criteria consisted of both descriptive and intervention studies focusing on the target population (ECE workforce in the USA), published in English within the past 10 years. We did not limit the types of study designs that were included in this review and so we did not assess the quality of the resulting evidence. Given the relatively small size of the evidence base in this area, we included otherwise unpublished dissertations, Master’s theses and organizational reports (e.g., government, non-profit). To assess whether articles met these criteria, titles and abstracts were first reviewed by the first author for relevance and duplicates were deleted. Next, full-text of remaining papers (n = 43) were reviewed to confirm that each paper met the inclusion criteria. Lastly, discussion with the whole author team was used if there was ambiguity about a particular paper. During this process, six articles were excluded because they were conducted outside of the USA and two were excluded because they were commentary pieces and did not contain primary data.
For programs, we included any program targeting some component of ECE workforce health that has been offered in the USA at least one time within the past 3 years. We excluded studies and programs that focused on only acute health topics (e.g., infectious disease or injuries). Both published intervention studies and unpublished programs were included.
Data extraction
For publications, data on target population/sample, methods, and results were gathered from the full-text of the articles. One author (MM) did an initial extraction of each article which was reviewed and confirmed by the lead author to confirm the accuracy of the extraction and summarization. Following extraction, we summarized the resulting evidence qualitatively and present themes across the evidence base. Only quantitative data on health status or behaviors was included (e.g., attitudinal or knowledge data were excluded from extraction).
For practice, organizations and individuals were asked to complete a form providing information about the intervention design (e.g., target behaviors/outcomes; activities or program components) and any evaluation data or results. We followed up with individuals as needed to obtain complete information.
Results
In total, 26 articles met the inclusion criteria for health status (Table 2). Two articles were excluded from the health status analysis because they involved qualitative methods and did not present prevalence estimates [36, 37]. The themes from these papers were, however, integrated within the results section.
Physical health
Thirteen studies described some component of physical health including diet quality (11 studies), physical activity (8 studies), and height/weight/BMI (7 studies). Five studies each measured sleep and smoking and four studies measured chronic disease status.
Diet quality
Ten studies measured fruit and/or vegetable consumption. The proportion of providers meeting recommendations for fruit and vegetable consumption (3.5 cups or 5 servings per day) varied from 22.5% of Head Start staff [17] to 50% of family child care (FCC) providers [32]. Mean fruit and vegetable consumption exceeded recommendations in one study of Head Start teachers [16] but were below recommendations in one study of child care center (CCC) directors and staff [9].
Physical activity
Five studies explored the proportion of providers meeting national physical activity requirements (e.g., 150 min per week of moderate to vigorous physical activity); the results included 27% of CCC employees [23], 29.4% of CCC directors and staff [9], and 55% of Head Start teachers [22] met these recommendations. Approximately 40–50% of FCC providers in two studies reported meeting guidelines [24, 32]. Providers across four studies reported large quantities of sedentary time; one study of Head Start (HS) teachers found they spent 291.69 min (4.9 h) per weekday sitting [22]; two studies of CCC employees found a mean of 481 and 513.6 min (8–8.6 h) of sedentary time per day, respectively [9, 23]. One study of FCC providers found that nearly one third (32.8%) reported nine or more hours of sedentary time per day [24].
Weight status
Seven studies assessed height and weight and converted to BMI; high levels of overweight and obesity (defined as BMI > 25) were reported. Rates of overweight and obesity included between 73.5 and 80.1% for HS staff [22, 28, 30], 71% and 89.9% for FCC providers, and 88.5% and 87.2% of CCC staff [9, 23]. Nationally, 71.6% of adults are overweight or obese [38].
Sleep
Three studies explored whether FCC providers were meeting sleep recommendations (7 or more hours of sleep per night); between 43.4 and 56.7% were regularly meeting these goals [24, 32].
Smoking
A small proportion of providers reported being current smokers; from 15.6% of CCC staff [23] to just 7.5% of FCC providers [24].
Chronic disease status
Three studies assessed diabetes prevalence and found similar rates (10.6% for FCC, 10.4% for FCC, 11.9% for HS) [24, 33] compared to just 7.8% of a comparable national sample [33]. Rates of diagnosed high blood pressure included 22.3% of HS staff and 36% of FCC providers [24, 33]. One study of HS staff found higher rates of four additional chronic diseases and conditions (severe headache/migraine, lower back pain, obesity and asthma) as compared to a similar national sample [33].
Mental health
In total, we found 21 studies that included measurement of mental health including depression (15 studies), stress (8 studies), and mindfulness (3 studies).
Depression
Fifteen studies explored depression levels of ECE providers; from two samples of FCC, approximately 23% reported a depressive disorder or diagnosis [24]. Among the five analyses of HS staff, one study found an average Center for Epidemiologic Studies—Depression (Scale) (CES-D) of 10.8 (at or above 16 is considered screening positive for depression) [12]; another found 35% of respondents with at least moderate depression at two time points during the year [18]; and Ling found that 31% of HS teachers were experiencing depressive symptoms [22]. In two analyses from the Pennsylvania Head Start Survey [33, 34], approximately 24% of respondents had a CES-D score at or above 16. This contrasts with only 17.6% of a national comparison sample with similar demographics. The eight studies that included CCC staff generally found lower rates of depressive symptoms; fewer than 19% of respondents in one study of CCC staff scored above 16 on the CES-D [35] and only 8.9% of respondents in another study had clinically significant depression [26]. Two analyses of data from CCC providers in North Carolina found higher rates of depression (34.9–36% with a CES-D at or above 16), compared to the national average of 12.3% of women ages 40–59 [9, 23].
Stress
While only one of the eight studies that explored stress levels of providers included prevalence data on high stress, several explored the impact that stress levels have on performance. One study of 39 providers (CCC staff and FCC providers) found that higher levels of provider stress were associated with lower child engagement in the classroom [25]. Another study found that stress levels were associated with a greater intention for teachers to leave rather than stay in their positions [15]. In a survey of FCC providers conducted by Tovar and colleagues (2017), 62% of respondents had a high stress score on the Perceived Stress Scale [32].
Mindfulness
Three studies measured mindfulness traits among ECE providers, each with a different measure (CAMS-R, FFMQ, MAAS), which makes comparisons across samples difficult.
Interventions
Following the literature and practice searches, seven published and four unpublished programs were identified. Details on the audience, target behaviors/outcomes, activities/components, and evaluation results (if available) are included in Table 3.
Audience
The majority of the programs were delivered to center-based teachers and staff, with only one developed specifically for family child care providers [44, 46]. Others focused on Head Start staff [39, 42] or a broader audience of providers including FCC (33, Building Well-Being Resilient).
Target behaviors and program components
All but one program included nutrition/healthy eating components; most included physical activity and five included stress or other mental health-related targets. The majority of the published interventions were larger, multi-component interventions that included some staff wellness component (as opposed to a stand-alone staff intervention). Most were also conducted over a long period of time ranging from 6 to 12 months with multiple pedagogical techniques (e.g., workshops, print materials, individual or group coaching). Only one identified program (YMCA child care) described ongoing efforts that are always available to employees. All others represented one-time interventions, with the majority sponsored by outside organizations and/or researchers working in conjunction with providers.
Evaluation result
Limited evidence on the effectiveness of these interventions is available. Among the published interventions, only four included participant-level impact data. The CARE Intervention has shown preliminary evidence of impact; a pilot study showed positive impact on BMI, physical activity, fruit and vegetable intake, and smoking [8]. Another intervention, offered over 9 months as part of a larger intervention targeting center-based providers in California, showed positive impact on only sugar sweetened beverage consumption [41]. The Eat Healthy, Stay Active! program has been shown to positively impact provider BMI, diet, physical activity, and health-related knowledge [42]. A one-time mindfulness workshop did not show significant impact on provider mindfulness or workplace stress [43]. Among the unpublished programs, only one has evaluation results available. The Create Healthy Futures program, a 4-hour online program, showed improvements in nutrition knowledge and perceived barriers to promoting wellness in the classroom [45].
Discussion
This scoping review provides a well-rounded picture of the health status of the ECE workforce in the USA along with description of interventions recently implemented to improve health in this population. From the health status literature, it is clear that many ECE providers struggle with chronic disease risk behaviors (e.g., healthy eating, sedentary time) and mental health challenges (e.g., stress and depression). These challenges persisted across setting (e.g., HS versus CCC; teachers versus directors). This is likely exacerbated by the low socioeconomic status among a majority of ECE providers, as well as lack of access to health insurance through their employers [1]. Given that many child care centers and homes cannot afford to provide health insurance, introducing workforce wellness programs may be an affordable work-around to addressing chronic disease risk behaviors and mental health challenges. Specific recommendations on health behavior targets likely vary depending on the ECE type (e.g., FCC versus HS) and the local context; however, it is clear that there is room for improvement across the board for physical activity and diet. Many providers in the included studies were overweight or obese, raising their chronic disease risk.
For physical activity, three studies found that ECE providers spend between 4 and 8.6 h/day in sedentary activity levels, which have been shown to be associated with obesity and certain cancers, independent of physical activity levels [47, 48]. Thus, interventions targeting sedentary time may be especially warranted in this population.
Insight can also be drawn from research done on ECE providers in other countries, as well, as workplace stress is a common factor for child care providers in many countries. For example, Corr et al. looked into the relationship between Australian family child care educators’ mental health and working conditions, finding that social support was associated with higher mental well-being [49]. Similarly, Nislin et al. found that teamwork was critical to supporting the well-being of ECE providers in Finland [50]. Both of these studies were conducted in countries where there is significantly more government financial support for ECE providers (in Australia, for example, over 70% of ECE providers said their income was “enough” or “more than enough” to meet needs) [49], as well as nearly universal health care access, which eliminates some of the socioeconomic stresses that American ECE providers face.
The interventions and programs included in our review provide a wide range of options for future efforts. Many were embedded in larger, facility-wide programs targeting obesity prevention in adults and children. Research shows that Whole Systems Approaches are most likely to have a significant impact on complex public health challenges including obesity [51]. Most were conducted over 6 months or more, illustrating that impact on chronic disease and mental health outcomes requires a significant investment of time and support. Given the diversity within the ECE workforce, it is also likely that different intervention approaches will need to be used for different audiences. For example, interventions originally developed for center-based staff may not be appropriate for family child care providers who have different access to colleagues (e.g., social support) and administrative supports to facilitate wellness programming.
There have been calls in the literature for an increase in practice-based evidence (PBE) or studies that combine the rigor of the scientific process with the realities of implementation in the real world [52]. Researchers interested in this approach can use the list of interventions provided here as a jumping off point to develop collaborative research projects to assess the implementation and impact of these interventions on the ECE workforce. Additional research should be done to determine the extent to which these programs align with best practices in worksite health promotion developed by the CDC [53].
Limitations
Many of the descriptive studies did not include a comparison group of individuals with similar demographics but different occupations. Such a group would improve understanding of whether the health status of the ECE workforce is different from others with similar demographic characteristics, especially age, education level, and income. Our programs only included one facility-level wellness intervention (YMCA child care), though ECE professionals connected to larger employers, such as corporations or universities, are likely have access to employee wellness programs. A recent national survey found that nearly 50% of workplaces in the USA with at least 10 employees offer some sort of employee wellness programming [54]. While none of those programs responded to our call for programs, the authors are aware that these initiatives exist across the country despite their relative absence from our review.
Conclusions
The results of this scoping review suggest that additional research into the health status of the ECE workforce is needed to properly categorize chronic disease risk across the diversity of the workforce. The limited body of evidence available for review paints a picture of a workforce in need of health promotion intervention to address high levels of mental and physical health challenges, some above and beyond peers with comparable demographic characteristics. Several promising interventions were identified from both the published and unpublished literature; these interventions should be further implemented and evaluated to assess their impact on the workforce.
Availability of data and materials
Data sharing is not applicable to this article as no datasets were generated or analyzed during the current study.
Abbreviations
- BMI:
-
Body mass index
- CCC:
-
Child care center
- CDC:
-
Centers for Disease Control and Prevention
- CES-D:
-
Center for Epidemiologic Studies—Depression (Scale)
- ECE:
-
Early care and education
- FCC:
-
Family child care
- HS:
-
Head Start
- PBE:
-
Practice-based evidence
- YMCA:
-
Young Men’s Christian Association
References
Whitebook M, McLean C, Austin LJE, Edwards B. Early childhood workforce index – 2018, vol. 4. Berkeley: Center for the Study of Child Care Employment, University of California, Berkeley; 2018.
Scott K, Looby AA, Hipp JS, Frost N. Applying an equity lens to the child care setting. J Law Med Ethics. 2017;45(1_suppl):77–81.
Gould E. Child care workers aren’t paid enough to make ends meet. Washington: Economic Policy Institute; 2015.
Adler NE, Stewart J. Health disparities across the lifespan: meaning, methods, and mechanisms. Ann N Y Acad Sci. 2010;1186(1):5–23.
Adler N, Stewart J, Cohen S, et al. Reaching for a healthier life: facts on socioeconomic status and health in the United States. San Francisco: The John D. and Catherine T MacArthur Foundation Research Network on Socioeconomic Status and Health; 2007. Available at http://www.macses.ucsf.edu.
Centers for Disease Control and Prevention. CDC Health Disparities and Inequalities Report – United States, 2013. MMWR. 2013;62(Suppl3):1–2.
Stiehl E, Shivaprakash N, Thatcher E. Worksite health promotion for low-wage workers: a scoping literature review. Am J Health Promot. 2017;32(2):359–73. https://doi.org/10.1177/0890117117728607.
Arandia G, Vaughn AE, Bateman LA, Ward DS, Linnan LA. Development of a workplace intervention for child care staff: Caring and Reaching for Health’s (CARE) healthy lifestyles intervention. Health Promot Pract. 2018. https://doi.org/10.1177/1524839918786214.
Ward DS, Vaughn AE, Hales D, et al. Workplace health and safety intervention for child care staff: rationale, design, and baseline results from the CARE cluster randomized control trial. Contemp Clin Trials. 2018;68:116–26. https://doi.org/10.1016/j.cct.2018.02.018.
Rumrill PD, Fitzgerald SM, Merchant WR. Using scoping literature reviews as a means of understanding and interpreting existing literature. Work. 2010;35(3):399–404. https://doi.org/10.3233/WOR-2010-0998.
Arksey H, O'Malley L. Scoping studies: towards a methodological framework. Int J Soc Res Methodol. 2005;8(1):19–32. https://doi.org/10.1080/1364557032000119616.
Becker BD, Gallagher KC, Whitaker RC. Teachers’ dispositional mindfulness and the quality of their relationships with children in Head Start classrooms. J Sch Psych. 2017;65:40–53. https://doi.org/10.1016/j.jsp.2017.06.004.
Denham SA, Bassett HH, Miller SL. Early childhood teachers’ socialization of emotion: contextual and individual contributors. Child Youth Care Forum. 2017;46(6):805–24.
Figueroa R, Wiley A. Factors associated with time provided to children for physical activity in family child care: a cross-sectional study. SpringerPlus. 2016;5(1):1730.
Grant AA, Jeon L, Buettner CK. Relating early childhood teachers’ working conditions and well-being to their turnover intentions. Educ Psychol. 2016. https://doi.org/10.1080/01443410.2018.1543856.
Halloran KM, Gorman K, Fallon M, Tovar A. Nutrition knowledge, attitudes, and fruit and vegetable intake as predictors of Head Start teachers’ classroom mealtime behaviors. J Nutr Educ Behav. 2018;50:340–8. https://doi.org/10.1016/j.jneb.2017.10.015.
Hibbs-Ship SK, Milholland M, Bellows L. Barriers and facilitators to healthy eating and activity in head start staff: an opportunity for worksite wellness. Am J Health Educ. 2015;46(6):347–50. https://doi.org/10.1080/19325037.2015.1077488.
Hindman AH, Bustamante AS. Teacher depression as a dynamic variable: exploring the nature and predictors of change over the head start year. J Appl Dev Psychol. 2019;61:43–55. https://doi.org/10.1016/j.appdev.2018.09.004.
Jennings PA. Early childhood teachers’ well-being, mindfulness, and self-compassion in relation to classroom quality and attitudes towards challenging students. Mindfulness. 2015;6(4):732–43. https://doi.org/10.1007/s12671-014-0312-4.
Jeon L, Buettner CK, Grant AA. Early childhood teachers’ psychological well-being: exploring potential predictors of depression, stress, and emotional exhaustion. Early Educ Dev. 2018;29(1):53–69.
Jeon HJ, Kwon KA, Walsh B, Burnham MM, Choi YJ. Relations of early childhood education teachers’ depressive symptoms, job-related stress, and professional motivation to beliefs about children and teaching practices. Early Educ Dev. 2019;30(1):131–44.
Ling J. Behavioral and psychosocial characteristics among Head Start childcare providers. J Sch Nurs. 2018;34(6):435–41. https://doi.org/10.1177/1059840517725791.
Linnan L, Arandia G, Bateman LA, Vaughn A, Smith N, Ward D. The health and working conditions of women employed in child care. Int J of Environ Res Public Health. 2017;14:283. https://doi.org/10.3390/ijerph14030283.
Magerko KA. Healthy hearts in family child care: what is the current state of provider health? [dissertation]: University of Illinois; 2016.
Ota CL, Baumgartner JL, Berghout Austin AM. Provider stress and children’s active engagement. J Res Child Ed. 2013;27(1):61–73. https://doi.org/10.1080/02568543.2012.739588.
Roberts AM, Gallagher KC, Daro AM, Iruka IU, Sarver SL. Workforce well-being: personal and workplace contributions to early educators’ depression across settings. J Appl Dev Psychol. 2017. https://doi.org/10.1016/j.appdev.2017.09.007.
Sandilos LE, Cycyk LM, Scheffner Hammer C, Sawyer BE, López L, Blair C. Depression, control, and climate: an examination of factors impacting teaching quality in preschool classrooms. Early Educ Dev. 2015;26(8):1111–27. https://doi.org/10.1080/10409289.2015.1027624.
Sharma S, Dortch KS, Byrd-Williams C, Truxillio JB, Rahman GA, Bonsu P, Hoelscher D. Nutrition-related knowledge, attitudes, and dietary behaviors among head start teachers in Texas: a cross-sectional study. J Acad Nutr Diet. 2013;113(4):558–62.
Snyder K, Hill M. Wellbeing begins with employees: exploring associations of physical health in a Head Start organization [Master’s thesis]: Wright State University; 2018.
Song WO, Song S, Nieves V, Gonzalez A, Crockett ET. Nutritional health attitudes and behaviors and their associations with the risk of overweight/obesity among child care providers in Michigan Migrant and Seasonal Head Start centers. BMC Public Health. 2016;16(1):648.
Swindle TM, Ward WL, Bokony P, Whiteside-Mansell L. A cross-sectional study of early childhood educators’ childhood and current food insecurity and dietary intake. J Hunger Environ Nutr. 2018;13(1):40–54.
Tovar A, Vaughn AE, Grummon A, et al. Family child care home providers as role models for children: cause for concern? Prev Med Rep. 2017;5:308–13. https://doi.org/10.1016/j.pmedr.2016.11.010.
Whitaker RC, Becker BD, Herman AN, Gooze RA. The physical and mental health of Head Start staff: The Pennsylvania Head Start Staff Wellness Survey, 2012. Prev Chronic Dis. 2013;10:130171. https://doi.org/10.5888/pcd10.130171.
Whitaker RC, Dearth-Wesley T, Gooze RA. Workplace stress and the quality of teacher-children relationships in Head Start. Early Child Res Q. 2015;30:57–69. https://doi.org/10.1016/j.ecresq.2014.08.008.
Witherell SL. Work-related stress and mental health of child care center workers [dissertation]. Detroit: Wayne State University; 2013.
Faulkner M, Gerstenblatt P, Lee A, et al. Childcare providers: work stress and personal well-being. J Early Child Res. 2016;14(3):280–93. https://doi.org/10.1177/1476718X14552871.
Lindsay AC, Greaney ML, Wallington SF, et al. Easier said than done: a qualitative study conducted in the USA exploring Latino family child care home providers as role models for healthy eating and physical activity behaviours. BMJ Open. 2017;7:1–7. https://doi.org/10.1136/bmjopen-2017-018219.
Centers for Disease Control and Prevention. Selected health conditions and risk factors, by age: United States, selected years 1988–1994 through 2015–2016. 2017. https://www.cdc.gov/nchs/data/hus/2017/053.pdf. Accessed 30 May 2019.
Esquivel MK, Nigg CR, Fialkowski MK, Braun KL, Li F, Novotny R. Influence of teachers’ personal health behaviors on operationalizing obesity prevention policy in head start preschools: a project of the Children’s Healthy Living Program (CHL). J Nutr Educ Behav. 2016;48:318–25. https://doi.org/10.1016/j.jneb.2016.02.007.
Messiah SE, Lebron C, Moise R, Mathew MS, Sardinas K, Chang C, Palenzuela J, Walsh J, Shelnutt KP, Spector R, Altare F. Healthy caregivers-healthy children (HC2) phase 2: integrating culturally sensitive childhood obesity prevention strategies into childcare center policies. Contemp Clin Trials. 2017;53:60–7.
Gosliner WA, James P, Yancey AK, Ritchie L, Studer N, Crawford PB. Impact of a worksite wellness program on the nutrition and physical activity environment of child care centers. Am J Health Promot. 2010;24(3):186–9. https://doi.org/10.4278/ajhp.08022719.
Herman A, Nelson BB, Teutsch C, Chung PJ. “Eat Healthy, Stay Active!”: A coordinated intervention to improve nutrition and physical activity among Head Start parents, staff, and children. Am J Health Promot. 2012;27(1):27–36. https://doi.org/10.4278/ajhp.110412-QUAN-157.
Jones KJ. Promoting stress reduction using mindfulness for educators in a military based child development center [master’s thesis]: San Diego State University; 2018.
Ostbye T, Mann CM, Vaughn AE, et al. The keys to healthy family child care homes intervention: study design and rationale. Contemp Clin Trials. 2015;40:81–9. https://doi.org/10.1016/j.cct.2014.11.003.
UTHealth School of Public Health, Michael & Susan Dell Center for Healthy Living, Penn State Extension Better Kid Care Program. Create Healthy Futures: an online wellness program for ECE Professionals. 2018.
Mann CM, Ward DS, Vaughn, et al. Application of the intervention mapping protocol to develop keys, a family child care home intervention to prevent early childhood obesity. BMC Public Health 2015;15:1–13. https://doi.org/10.1186/s12889-015-2573-9.
Shen D, Mao W, Liu T, et al. Sedentary behavior and incident cancer: a meta-analysis of prospective studies. PLoS One. 2014;9(8):e105709. https://doi.org/10.1371/journal.pone.0105709.
Thorp AA, Owen N, Neuhaus M, Dunstan DW. Sedentary behaviors and subsequent health outcomes in adults: a systematic review of longitudinal studies, 1996–2011. Am J Prev Med. 2011;41(2):207–15. https://doi.org/10.1016/j.amepre.2011.05.004.
Corr L, Lamontagne AD, Cook K, Waters E, Davis E. Associations between Australian early childhood educators’ mental health and working conditions: a cross-sectional study. Australas J Early Childhood. 2015;40(3):69–78.
Nislin MA, Sajaniemi NK, Sims M, Suhonen E, Maldonado EF, Montero AH, Hyttinen S. Pedagogical work, stress regulation and work-related well-being among early childhood professionals in integrated special day-care groups, European Journal of Special Needs Education; 2015.
Bagnall AM, Radley D, Jones R, et al. Whole systems approaches to obesity and other complex public health challenges: a systematic review. BMC Public Health. 2019;19(1):8. https://doi.org/10.1186/s12889-018-6274-z.
Ammerman A, Smith TW, Calancie L. Practice-based evidence in public health: improving reach, relevance, and results. Annu Rev Public Health. 2014;35:47–63. https://doi.org/10.1146/annurev-publhealth-032013-182458.
Gutermuth LK, Hager ER, Pollack PK. Using the CDC’s worksite health scorecard as a framework to examine worksite health promotion and physical activity. Prev Chronic Dis. 2018;15:E84. https://doi.org/10.5888/pcd15.170463.
Linnan LA, Cluff L, Lang JE, Penne M, Leff MS. Results of the Workplace Health in America Survey. Am J Health Promot. 2019. https://doi.org/10.1177/0890117119842047.
Acknowledgements
Not applicable
Funding
This project did not receive any external funding.
Author information
Authors and Affiliations
Contributions
LL conceived of the study, analyzed the data, drafted portions of the manuscript, and reviewed and approved the final version. KW drafted portions of the manuscript and reviewed and approved the final version. JRM drafted portions of the manuscript and reviewed and approved the final version. MCM conducted literature searches, analyzed the data, and reviewed and approved the final version.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Not applicable. This project did not include human subjects research and was not subject to Institutional Review Board review.
Consent for publication
Not applicable
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated.
About this article
Cite this article
Lessard, L.M., Wilkins, K., Rose-Malm, J. et al. The health status of the early care and education workforce in the USA: a scoping review of the evidence and current practice. Public Health Rev 41, 2 (2020). https://doi.org/10.1186/s40985-019-0117-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s40985-019-0117-z