Abstract
Background
In robot-assisted laparoscopic prostatectomy (RALP), concerns include the formation of atelectasis and reduced functional residual capacity. The present study aimed to examine the feasibility of positive end-expiratory pressure (PEEP) setting based on transpulmonary pressure (Ptp) as well as the effects of incremental PEEP on respiratory mechanics, blood gases, cerebral oxygenation (rSO2), and hemodynamics.
Methods
Fourteen male patients who were scheduled to receive RALP were recruited. Patients received mechanical ventilation (tidal volume of 6 mL kg−1) and were placed in Trendelenburg position with positive-pressure capnoperitoneum. PEEP levels were increased from 0 to 15 cmH2O (5 cmH2O per increase) every 30 min. PEEP levels were assessed where end-expiratory Ptp levels of ≥0 cmH2O were achieved (PtpEEP0). Airway pressure, esophageal pressure, cardiac index, and blood gas and rSO2 values were measured after 30 min at each PEEP step and respiratory mechanics were calculated.
Results
With increasing PEEP levels from 0 to 15 cmH2O or PtpEEP0, the values of PaO2 and respiratory system compliance increased, and the values of driving pressure decreased. The median PEEP level associated with PtpEEP0 was 15 cmH2O. Respiratory system compliance values were higher at PtpEEP0 than those at PEEP5 (P = 0.02). Driving pressure was significantly lower at PtpEEP0 than at PEEP5 (P = 0.0036). The cardiac index remained unchanged, and the values of rSO2 were higher at PtpEEP0 than at PEEP0 (right; P = 0.0019, left; P = 0.036).
Conclusions
PEEP setting determined by transpulmonary pressure can help achieve higher respiratory system compliance values and lower driving pressure without disturbing hemodynamic parameters.
Similar content being viewed by others
Explore related subjects
Find the latest articles, discoveries, and news in related topics.Background
Robotic surgery may enhance laparoscopic procedures in various contexts. However, respiratory management during robot-assisted laparoscopic prostatectomy (RALP) requires caution, as the procedure requires positive-pressure capnoperitoneum and steep Trendelenburg position. The dependent lungs may be compressed by positive pleural pressure, and their alveoli may collapse at end-expiration if positive end-expiratory pressure (PEEP) levels are inadequate. PEEP helps to prevent the formation of atelectasis and reduction of functional residual capacity; however, high airway pressure may result in overdistension or nonuniform ventilation distribution, or hemodynamic depression.
To reduce the risk of ventilator-induced lung injury and avoid barotrauma, evaluating the stress on the alveolar wall is recommended, while keeping the alveolus open [1]. Transpulmonary pressure (Ptp: airway pressure–intrathoracic pressure) has been previously used to determine PEEP levels in the respiratory management of acute respiratory distress syndrome [2, 3]. If the Ptp values at end-expiration are of <0 cmH2O, then the alveoli may collapse. Intrathoracic pressure can be substituted with esophageal pressure (Peso), measured with an esophageal balloon catheter. Intrathoracic pressure may be elevated during RALP; however, few studies to date have observed the changes in Ptp values at end-expiration with increasing PEEP levels. While low tidal volumes may benefit patients receiving general anesthesia using positive-pressure ventilation [4,5,6,7,8], the method for determining the optimum PEEP level during RALP remains unclear. Low PEEP may induce negative Ptp on end-expiration and promote atelectasis.
The present study aimed to clarify the changes in intrapleural and transpulmonary end-expiratory pressure (PtpEEP) values associated with increasing PEEP, given the positive-pressure capnoperitoneum combined with the Trendelenburg position, to determine the PEEP level where the Ptp exceeds 0 cmH2O. This study also aimed to examine the effects of those PEEP levels on cardiac output and cerebral oxygenation.
Methods
This single-center, prospective, observational interventional study was approved by the Ethics Committee of Tokyo Medical University Hospital (T2018-0065). The study protocol adhered to the principles of the Declaration of Helsinki; written informed consent was obtained from all patients. This registered clinical trial (UMIN000036376) included consecutive patients undergoing the RARP procedure at the Tokyo Medical University Hospital from April to August in 2019.
We enrolled male patients with the American Society of Anesthesiologists (ASA) Physical Status Classification score of 1 or 2 points, scheduled for RARP using a robotic operating system (da Vinci™ Surgical System, Intuitive Surgical, Inc., Sunnyvale, CA, USA). Patients with a history of chronic obstructive pulmonary disease, renal or heart failure, esophageal diseases, or body mass index (BMI) of ≥35 kg m−2 were excluded from this study.
No premedication was administered. Upon arriving in the operating theater, patients were monitored by electrocardiography; non-invasive automated blood pressure measurement and pulse oximetry were performed. SedLine® Brain Function Monitoring for patient state index (PSi) and O3® Regional Oximetry sensors for bilateral forebrain oxygenation (rSO2) monitoring were attached to the forehead and connected to Root Monitor® (Masimo, Irvine, CA, USA). A pulse oximetry probe was placed on the forefinger; body temperature was measured, using a 3M™ BearHugger™ deep temperature monitoring system. The patients were breathing a fraction of inspired oxygen (FIO2) of 1.0 for 3 min before the induction of general anesthesia with intravenous remifentanil at a rate of 0.3 μg kg−1 min−1 and propofol via target-controlled infusion to a plasma concentration of 4–4.5 μg mL−1. The lungs were ventilated manually, using a Jackson Rees breathing system via a face mask with an FIO2 of 1.0. Muscle relaxation was achieved with rocuronium of 1 mg kg−1 to facilitate orotracheal intubation. The patients were intubated with a cuffed reinforced tracheal tube with an internal diameter of 7.5 mm, using a McGrath MAC® video laryngoscope (Medtronic Co., USA). After confirming tracheal intubation, the lungs were ventilated using a mechanical ventilator (AVEA™ Ventilator Systems; CareFusion Inc., San Diego, CA, USA) with volume-controlled ventilation. The inspiratory-to-expiratory time ratio was 1:2.5 with an end-inspiratory pause of 20% and tidal volume (VT) of 6 mL kg−1 of the predicted body weight. The predicted body weight was calculated as 49.9 + 0.91 × (height [cm] − 152.4).
The respiratory rate was initially set at 12 breaths/min and changed to maintain normocapnia (end-tidal carbon dioxide partial pressure [EtCO2] of 35–45 mmHg). Patients were ventilated using oxygen and air, with an FIO2 of 0.5. After the recruitment maneuver (35 cmH2O CPAP for 30 s), 3 cmH2O PEEP was added. A 22-G arterial cannula was inserted percutaneously into the radial artery after the induction of anesthesia for continuous monitoring of arterial pressure and blood gas sampling; it was also connected to a Flo Trach™ sensor with a Vigileo monitor system (Edwards Lifesciences, Irvine, CA, USA) for continuous monitoring of arterial pressure wave form, based on cardiac index (CI) and stroke volume variation (SVV). Arterial blood gas analysis was performed within 1 min of sampling, using a blood gas analyzer (The epoc® Blood Analysis System, Co. Siemens Healthineers, PA, USA). To measure esophageal pressure and gastric suctioning, a 16-Fr SmartCath™ adult nasogastric tube with an esophageal balloon (Vyaire Medical Inc., Mettawa, IL, USA) was inserted transorally and advanced into the stomach. By pulling back the tube, the positioning of the balloon was confirmed in the presence of a cardiac oscillation reflective of cardiac activity and esophageal pressure wave fluctuation during a ventilation cycle. Furthermore, the balloon location was confirmed using an occlusion technique; the airway was occluded at end-expiration and esophageal pressure and airway pressure were simultaneously compared for similarity. The position of the catheter was also checked on routine postoperative chest radiography.
After the induction of anesthesia, patients were placed in a horizontal lithotomy position. Anesthesia was maintained with a continuous infusion of propofol, remifentanil, and rocuronium throughout the surgery. The infusion rate of propofol was adjusted to maintain the PSi in the range of 25–50, with the administration of remifentanil at the rate of 0.3 μg kg−1 min−1. The neuromuscular block was maintained by continuous intravenous administration of rocuronium at the rate of 0.3 mg kg−1 h−1. Hemodynamic stability (arterial systolic pressure and heart rate of 80–100% of the preanesthetic value) was maintained by fluid management or vasopressors. Specifically, standardized fluid management was performed using acetated Ringer’s solution. In cases of intraoperative hypotension (mean arterial pressure of <65 mmHg or a decrease in mean arterial pressure by >20% from baseline), 6% hydroxyethyl starch in 0.9% sodium chloride solution was given, provided the SVV was >13%; otherwise, it was managed with phenylephrine or ephedrine, as required.
Study protocol
The patient was placed in the 30° Trendelenburg lithotomy position with a positive-pressure capnoperitoneum and CO2 insufflation, when the respiratory rate increased to 15 breaths/min. Capnoperitoneum was kept at the pressure of 12 mmHg; however, pressure levels were occasionally changed at the surgeon’s discretion. PEEP level was initially maintained at 0 cmH2O for 30 min; thereafter, while the intraabdominal pressure was kept at 12 mmHg, blood gas levels and hemodynamic and ventilatory parameters were recorded. Esophageal and airway pressure values were simultaneously read on a monitor screen at end-inspiration and end-expiration. Ptp estimates for both phases were calculated, as the difference between airway and esophageal pressure values. The respiratory rate was changed, such that the ETCO2 levels were between 40 and 50 mmHg during surgery.
PEEP levels were increased by 5 cmH2O in a stepwise manner at 30-min intervals; measurements were performed before each increase. Recruitment maneuver was performed before each PEEP trial. Once the PEEP levels reached 15 cmH2O and the measurements were completed, PEEP levels were changed, such that the Ptp was 0 cmH2O (PtpEEP0).
Data collection
Patient characteristics of interest included height, weight, body mass index, ASA physical status, and respiratory function test findings. The values of the following parameters of respiratory mechanics were recorded: inspiratory peak pressure, inspiratory plateau pressure (Pplat), end-inspiratory esophageal pressure (PesoEIP), end-expiratory esophageal pressure (PesoEEP), and ETCO2.
Hemodynamic parameters of interest included heart rate, mean arterial pressure, arterial pressure wave form base CI, and SVV values. The following arterial blood gases were examined: pH, PO2, PCO2, and SaO2. Cerebral oxygenation was measured as bilateral rSO2 levels.
The following parameters were calculated as follows: respiratory system driving pressure (DP) = Pplat − PEEP; end-inspiratory transpulmonary pressure (PtpEIP) = Pplat − PesoEIP; end-expiratory transpulmonary pressure (PtpEEP) = PEEP − PesoEEP; transpulmonary driving pressure (PtpDP) = PtpEIP − PtpEEP; respiratory system compliance = VT/(Pplat − PEEP); chest wall compliance = VT/(PesoEIP − PesoEEP); and pulmonary compliance = VT/ PtpDP.
Data were collected (1) after the induction of anesthesia (baseline), (2) 30 min after capnoperitoneum and Trendelenburg position (PEEP0 cmH2O: PEEP0) were achieved, (3) 30 min after PEEP of 5 cmH2O (PEEP5) was achieved, (4) 30 min after PEEP of 10 cmH2O was achieved (PEEP10), (5) 30 min after PEEP15 cmH2O (PEEP15) was achieved, (6) 30 min after PEEP level corresponding to PtpEEP of 0 (PtpEEP0) was achieved, and (7) at the end of surgery. After the RALP procedure was completed, the patients were returned to the supine position and PEEP levels were set at 5 cmH2O.
Statistical analysis
The present study aimed to determine the PEEP levels, where the PtpEEP values exceeded 0 cmH2O during the RALP surgery, and to observe whether such PEEP levels were beneficial for oxygenation or respiratory mechanics parameters. A formal power analysis was not performed because this was an observational study; however, sample size calculation was performed based on the preliminary findings obtained from the first seven patients in the first 2 months. Since PtpDP from PEEP 0 to PtpEEP0 values were 9.3±5.8 cmH2O and 6.0±2.8 cmH2O, we calculated that 11 patients were required to test the null hypothesis at a significance level of 0.05 and power of 0.90. Accounting for possible study dropouts, we aimed to include 16 participants. Categorical variables were reported as counts and percentages. Continuous data were examined for normal distribution, using the Shapiro–Wilk test, and were presented as mean±standard deviation or median and interquartile range, as appropriate. The Friedman non-parametric test with Scheffe’s multiple comparison procedure was used to test for differences between each PEEP level. All analyses were performed using the statistical software package BellCurve for Excel for Windows® (Social Survey Research Information C., Ltd. Tokyo, Japan). P-values of <0.05 were considered statistically significant.
Results
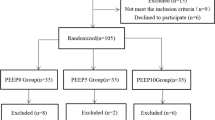
Written informed consent was obtained from 16 patients enrolled in the study. Two patients were excluded due to esophageal balloon catheter failure; a total of 14 patients were included (Table 1). No patient showed a deterioration in circulatory dynamics or received vasopressors during robot-assisted procedures. All robot-assisted procedures were successfully performed, and all patients completed this protocol without any episodes of clinical problems. No patient developed any perioperative complications related to positive-pressure capnoperitoneum, positioning, or anesthesia during and after surgery.
Effects of PEEP on respiratory pressures and ventilatory mechanics
Ventilation pressure and respiratory mechanics parameter values at each PEEP level are presented in Table 2. The value of PesoEEP during the Trendelenburg position with positive-pressure capnoperitoneum at PEEP0 was 10 (6.8–14) cmH2O; it increased with the increases in PEEP levels. However, increasing PEEP from 0 to 15 cmH2O reduced the gap between PesoEEP and PEEP levels. PtpEEP of 0 was associated with the PEEP level of 15 (range 12–20) cmH2O.
The values of DP decreased with the increase in PEEP. The values of DP at PEEP10 (P = 0.012), PEEP15 (P = 0.001), and PtpEEP0 (P < 0.001) were significantly lower than those at PEEP0; those at PtpEEP0 (P = 0.036) were also lower than those at PEEP5 (Fig. 1A). PtpDP decreased with the increase in PEEP from PEEP0 to PtpEEP0; however, this change was not significant except for the values between PEEP0 and PEEP10 (Fig. 1B). Respiratory system compliance values were higher at PEEP10, PEEP15, and PtpEEP0 than at PEEP0 (P < 0.001); in addition, the corresponding values at PtpEEP0 were higher than those at PEEP5 (P = 0.02) (Fig. 1C). The values of lung compliance at PEEP10 (P = 0.0118), PEEP15 (P = 0.0284), and PtpEEP0 (P = 0.0169) were significantly higher than those at PEEP0 (Fig. 1D). Chest wall compliance values were similar at all PEEP levels.
Effects of increasing PEEP on driving pressure (A), transpulmonary driving pressure (B), respiratory system compliance (C), and lung compliance (D) during robot assisted laparoscopic prostatectomy. PtpEEP0 PEEP levels corresponding to the end-expiratory transpulmonary pressure levels of ≥0 cmH2O were achieved. *P < 0.05, ⁑P < 0.01
Arterial blood gas analysis
Blood gas data are shown in Table 3. The values of PaO2 at PEEP of ≥10 cmH2O were significantly higher than those at PEEP0 (P < 0.0024 at PEEP10, P < 0.001 at PEEP15, and P < 0.001 at PtpEEP0, respectively). The values of PaCO2 were higher at PEEP 15 cmH2O than at PEEP0 (P = 0.0034) and PEEP5 (P = 0.0324). The values of pH decreased with the increase in PEEP; those at PtpEEP0 were significantly lower than those at PEEP0 (P < 0.001) and PEEP5 (P = 0.0324).
Circulatory parameters and cerebral oxygen saturation
Hemodynamic and cerebral oxygenation parameters during anesthesia are presented in Table 4. Heart rate, mean blood pressure, and CI values did not change during anesthesia, except that the values of mean blood pressure at PEEP15 were significantly lower than those at PEEP0 (P = 0.0324). The levels of lactate were significantly lower at PEEP15 than at PEEP5 (P = 0.032). The values of rSO2 at PtpEEP0 were significantly higher than those at PEEP0 (right: P = 0.0019, left: P = 0.036). There were no differences in the circulatory parameters or rSO2 between PEEP5 and PtpEEP0.
Discussion
This observational interventional study showed that PesoEEP, suggesting intrathoracic pressure, at end-expiration during capnoperitoneum with Trendelenburg position reached 10 cmH2O, and the PEEP levels, where PtpEEP exceeding 0 cmH2O, were variable among the patients. Theoretically, PtpEEP should exceed 0 cmH2O to open alveolus and minimize the risk of atelectasis. We assumed that PEEP levels to achieve a transpulmonary pressure of 0 cmH2O at end-expiration might be enough to prevent atelectasis. The present findings suggest that adding PEEP based on transpulmonary pressure during the RALP procedure may be feasible, as respiratory system compliance and driving pressure at such levels were improved compared to those observed at PEEP5 without disturbing circulatory or cerebral oxygenation parameters.
As shown previously [8,9,10], our study proved that capnoperitoneum in the Trendelenburg position did not significantly affect cardiac output. In addition, cardiac output was maintained at all PEEP levels. This could be partly accomplished by fluid loading according to the SVV values. On the other hand, positive-pressure capnoperitoneum combined with the Trendelenburg position has been associated with intracranial pressure (ICP) elevation [11]; an increase in thoracic pressure is partially transmitted to central venous pressure (CVP) and may thus increase venous downstream pressure of the brain. The effect of PEEP on ICP yielded conflicting results [12, 13]. Caricato et al. showed that for patients with low respiratory system compliance especially for less compliant lung, cerebral hemodynamics and ICP were not influenced by administration of higher PEEP [12]. On the other hand, Boone et al. reported that a statistically significant relationship between PEEP and ICP or PEEP and CPP was not found in normal lungs or mild to moderate lung injury, but only in severe lung injury [13]. The complex interaction between mechanical ventilation and cerebral hemodynamics appears to be influenced by multiple patient-specific factors. The transmission of PEEP into the thoracic cavity is variable and dependent on the properties of the chest wall and lungs. We did not measure CVP or jugular vein pressure, so it is beyond the scope of the present study. The results of the present study showed that cerebral oxygenation was maintained during incremental PEEP levels. Hypercapnia due to capnoperitoneum in combination with low tidal volume ventilation might contribute to maintain cerebral blood flow and rSO2.
Recently, several clinical studies have reported on using an esophageal catheter during anesthetic management of laparoscopic surgery [14,15,16]. Tharp et al. examined the optimal positive end-expiratory pressure settings needed to achieve positive end-expiratory transpulmonary pressures during robotic laparoscopic surgery, and they showed that body habitus, pneumoperitoneum, and Trendelenburg positioning may each independently impair lung mechanics [14]. Therefore, it seems important that PEEP settings should be individually adjusted based on the variability in surgical conditions and patient’s physique. Piriyapatsom examined the optimal PEEP levels during laparoscopic gynecological surgery, using an esophageal balloon catheter [15]. In this study, the titrated PEEP levels exceeded pleural pressure values. Compared with those at the conventional PEEP level (5 cmH2O), respiratory system compliance was higher and driving pressure was lower in the intervention group than in the control group. Those findings were almost identical to ours.
Using an esophageal catheter for measuring esophageal pressure can separate the respiratory mechanics between that of the chest wall and that of the lung, and it provides information about individual lung mechanics, including lung compliance or transpulmonary driving pressure values. Contrary to our expectations, the decrease in transpulmonary driving pressure and the increase in lung compliance by PtpEEP0 were not significant compared to those obtained at PEEP5. We assumed that those higher PEEP levels might not necessarily lead to uniform ventilation. These findings suggest that transpulmonary pressure, estimated by using the esophageal pressure values in the present study, reflects the levels in the dependent lung. Thus, those PEEP values may not be suitable for the entire lung, specifically, for the non-dependent lung, as the distribution of pleural pressure is not homogeneous [17]. Pleural pressure is overestimated in the non-dependent pleural space and underestimated in the dependent regions. Experimental studies have shown the presence of a vertical gradient of pleural pressure from top to bottom [18], which may be related to gravity, the weight of the lungs, and pressure from mediastinal and abdominal contents. In the present study, high PEEP increased PaCO2 levels despite increasing minute ventilation while maintaining ETCO2 constant, suggesting that the dead space-to-tidal volume ratio might increase. While tidal volume was small and kept constant throughout the surgical procedures, the more compliant lung may be ventilated at a higher PEEP level.
Shono et al. compared PEEP of 15 cmH2O with PEEP of 5 cmH2O during RALP and demonstrated that PEEP of 15 cmH2O might maintain ventilation in the dorsal region and improve lung mechanics using transpulmonary pressure and electrical impedance tomography imaging [16]. These authors concluded that PEEP of 15 cmH2O resulted in more homogeneous ventilation and favorable physiologic effects during RALP. This study did not show optimal PEEP levels during RALP; however, the PEEP level of 15 cmH2O presented with results comparable to those obtained in the present study.
The present study has several limitations. First, the esophageal pressure can reflect pleural pressure in the regions where the esophageal balloon is located, i.e., mid-lung only if the calibration of the esophageal balloon is performed correctly with minimal non-stress volume. Esophageal pressure can overestimate (too large balloon volume) or underestimate (too small balloon volume) pleural pressure, depending on the volume of the balloon [19]. The inflated volume was automatically adjusted in the present ventilator, and calibration was carried out every 30 min. We ensured that the estimates were based on tidal changes in esophageal pressure. Second, the present study was observational. Randomized controlled studies of the standard PEEP and PEEP at a level above PtpEEP0 are required to validate the present findings. In addition, our findings on the effects of short-term interval PEEP increment may not be suitable for routine clinical practice. Third, esophageal pressure monitoring requires esophageal balloon catheter placement, and it is not practical in the anesthetic management of RALP surgery. The PEEP settings based on transpulmonary pressure measurements are cumbersome and may be unsuitable. Fourth, the present study did not examine the effectiveness of PEEP at a level beyond PtpEEP0. The objective of the present study was to observe the changes in esophageal pressure and PtpEEP during the RALP procedure, depending on the increase in PEEP; this study has achieved its objective.
Conclusions
Individualized level of PEEP should be determined in patients undergoing the RALP procedure to account for patient and surgical condition heterogeneity. Transpulmonary pressure measurement may help determine optimal PEEP level; however, this approach is not practical and whether thus derived PEEP levels are optimal remains unclear.
Availability of data and materials
The data that support the findings of this study are available from the corresponding author, KN, upon reasonable request.
Abbreviations
- ASA:
-
American Society of Anesthesiologists
- BMI:
-
Body mass index
- CI:
-
Cardiac index
- CVP:
-
Central venous pressure
- FIO2 :
-
Fraction of inspired oxygen
- ICP:
-
Intracranial pressure
- PEEP:
-
Positive end-expiratory pressure
- PEEP0:
-
PEEP of 0 cmH2O
- PEEP5:
-
PEEP of 5 cmH2O
- PEEP10:
-
PEEP of 10 cmH2O
- PesoEEP:
-
End-expiratory esophageal pressure
- PesoEIP:
-
End-inspiratory esophageal pressure
- Pplat:
-
Inspiratory plateau pressure
- PSi:
-
Patient state index
- PtpEEP:
-
End-expiratory transpulmonary pressure
- PtpEEP0:
-
PEEP levels corresponding to PtpEEP of 0 cmH2O
- RALP:
-
Robot-assisted laparoscopic prostatectomy
- rSO2 :
-
Forebrain oxygenation
- SVV:
-
Stroke volume variation
- VT:
-
Tidal volume
References
Chiumello D, Carlesso E, Cadringher P, Caironi P, Valenza F, Polli F, et al. Lung stress and strain during mechanical ventilation for acute respiratory distress syndrome. Am J Respir Crit Care Med. 2008;178:346–55.
Talmor D, Sarge T, Malhotra A, O’Donnell CR, Ritz R, Lisbon A, et al. Mechanical ventilation guided by esophageal pressure in acute lung injury. N Engl J Med. 2008;359:2095–104.
Beitler JR, Sarge T, Banner-Goodspeed VM, Gong MN, Cook D, Novack V, et al. Vent-2 study group. Effect of titrating positive end-expiratory pressure (PEEP) with an esophageal pressure-guided strategy vs an empirical high PEEP-FIO2 strategy on death and days free from mechanical ventilation among patients with acute respiratory distress syndrome. JAMA. 2019;321:846–57.
Wolthuis EK, Choi G, Dessing MC, Bresser P, Lutter R, Dzoljic M, et al. Mechanical ventilation with lower tidal volumes and positive end-expiratory pressure prevents pulmonary inflammation in patients without preexisting lung injury. Anesthesiology. 2008;108:46–54.
Futier E, Constantin JM, Paugam-Burtz C, Pascal J, Eurin M, Neuschwander A, et al. A trial of intraoperative low-tidal-volume ventilation in abdominal surgery. N Engl J Med. 2013;369:428–37.
Severgnini P, Selmo G, Lanza C, Chiesa A, Frigerio A, Bacuzzi A, et al. Protective mechanical ventilation during general anesthesia for open abdominal surgery improves postoperative pulmonary function. Anesthesiology. 2013;118:1307–21.
Deng QW, Tan WC, Zhao BC, Wen SH, Shen JT, Xu M. Intraoperative ventilation strategies to prevent postoperative pulmonary complications: a network meta-analysis of randomised controlled trials. Br J Anaesth. 2020;124:324–35.
Meininger D, Westphal K, Bremerich DH, Runkel H, Probst M, Zwissler B, et al. Effects of posture and prolonged pneumoperitoneum on hemodynamic parameters during laparoscopy. World J Surg. 2008;32:1400–5.
Lestar M, Gunnarsson L, Lagerstrand L, Wiklund P, Odeberg-Wernerman S. Hemodynamic perturbations during robot-assisted laparoscopic radical prostatectomy in 45° Trendelenburg position. Anesth Analg. 2011;113:1069–75.
Falabella A, Moore-Jeffries E, Sullivan MJ, Nelson R, Lew M. Cardiac function during steep Trendelenburg position and CO2 pneumoperitoneum for robotic-assisted prostatectomy: a trans-esophageal Doppler probe study. Int J Med Robotics Comput Assist Surg. 2007;3:312–5.
Robba C, Cardim D, Donnelly J, Bertuccio A, Bacigaluppi S, Bragazzi N, et al. Effects of pneumoperitoneum and Trendelenburg position on intracranial pressure assessed using different non-invasive methods. Br J Anaesth. 2016;117:783–91.
Caricato A, Conti G, Della Corte F, Mancino A, Santilli F, Sandroni C, et al. Effects of PEEP on the intracranial system of patients with head injury and subarachnoid hemorrhage: the role of respiratory system compliance. J Trauma. 2005;58:571–6.
Boone MD, Jinadasa SP, Mueller A, Shaefi S, Kasper EM, Hanafy KA, et al. The effect of positive end-expiratory pressure on intracranial pressure and cerebral hemodynamics. Neurocrit Care. 2017;26(2):174–81.
Tharp WG, Murphy S, Breidenstein MW, Love C, Booms A, Rafferty MN, et al. Body habitus and dynamic surgical conditions independently impair pulmonary mechanics during robotic-assisted laparoscopic surgery. Anesthesiology. 2020;133:750–63.
Piriyapatsom A, Phetkampang S. Effects of intra-operative positive end-expiratory pressure setting guided by esophageal pressure measurement on oxygenation and respiratory mechanics during laparoscopic gynaecological surgery: a randomised controlled trial. Eur J Anaesthesiol. 2020;37:1032–9.
Shono A, Katayama N, Fujihara T, Böhm SH, Waldmann AD, Ugata K, et al. Positive end-expiratory pressure and distribution of ventilation in pneumoperitoneum combined with steep Trendelenburg position. Anesthesiology. 2020;132:476–90.
Silva PL, Gama de Abreu M. Regional distribution of transpulmonary pressure. Ann Transl Med. 2018;6:385.
Pelosi P, Goldner M, McKibben A, Adams A, Eccher G, Caironi P, et al. Recruitment and derecruitment during acute respiratory failure: an experimental study. Am J Respir Crit Care Med. 2001;164:122–30.
Mojoli F, Iotti GA, Torriglia F, Pozzi M, Volta CA, Bianzina S, et al. In vivo calibration of esophageal pressure in the mechanically ventilated patient makes measurements reliable. Crit Care. 2016;20:98.
Funding
Not applicable
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation was performed by KN, AK, RY, and HU. Data collection was performed by KN, RM, TM, and YI. Data analysis was performed by KN and AK. The first draft of the manuscript was written by KN and AK. The authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
The study was approved by the Ethics Committee of Tokyo Medical University Hospital (T2018-0065). All patients provided written informed consent to participate in the study and publication of the study results.
Consent for publication
All patients provided written informed consent for the publication of the study results.
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Nakazawa, K., Kodaira, A., Matsumoto, R. et al. Positive end-expiratory pressure setting based on transpulmonary pressure during robot-assisted laparoscopic prostatectomy: an observational intervention study. JA Clin Rep 8, 10 (2022). https://doi.org/10.1186/s40981-022-00501-y
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1186/s40981-022-00501-y