Abstract
Background
Repetitive transcranial magnetic stimulation (rTMS) is a promising treatment option for people with severe, enduring anorexia nervosa (SE-AN). As depression is often comorbid with AN, antidepressant medication is commonly prescribed to this patient group. Concurrent antidepressant medications may affect the rTMS treatment response. Therefore, in a secondary analysis of data from a feasibility trial, we explored the effect of antidepressant medication on responses to rTMS in people with SE-AN.
Methods
Twenty-six participants with SE-AN received 20 sessions (over 4 weeks) of neuronavigated high-frequency real rTMS to the left dorsolateral prefrontal cortex. Eating disorder (ED) and general psychopathology symptoms were assessed at baseline, post-treatment and at a 4-month follow-up.
Results
Participants taking antidepressants (n = 16) for the duration of the rTMS treatment had a greater reduction in ED symptoms at the 4-month follow-up, compared to those not taking antidepressants (n = 10). Antidepressant status was not however associated with significant changes in mood outcomes.
Conclusions
In people with SE-AN receiving rTMS treatment, preliminary findings suggest a potential synergistic effect of antidepressant medication in reducing ED symptomatology. There was however no associated reduction in affective symptoms i.e., the effect does not seem to be related to changes in mood. The sample in this exploratory study was small and heterogenous. However, the preliminary results provide a basis for hypothesis generation for future studies.
Similar content being viewed by others
Plain English summary
Approximately 20–30% of patients with anorexia nervosa have a severe and enduring form of the illness. Therefore, new treatment approaches are needed. Repetitive transcranial magnetic stimulation (rTMS) is a promising treatment option for people with severe, enduring anorexia nervosa. Research in people with depression suggests that taking antidepressants may affect a person’s response to rTMS treatment. People with anorexia nervosa often experience depression and antidepressants are commonly prescribed to this patient group. This study explored the effect of antidepressants on responses to rTMS in people with severe, enduring anorexia nervosa. Participants received 20 sessions (over 4 weeks) of rTMS. We found that those taking antidepressants during rTMS treatment showed a greater reduction in eating disorder symptoms at follow-up, compared to those not taking antidepressants. Participants not taking antidepressants and those taking antidepressants showed similar improvements in depression and anxiety symptoms. This suggests that the improvement in eating disorder symptoms associated with the combination of rTMS and antidepressants was not related to changes in mood. The study sample was small, and we were unable to explore the effect of other medications on response to rTMS treatment. Further research is needed to investigate the effect of antidepressant medication on response to rTMS treatment in this patient group.
Background
Repetitive transcranial magnetic stimulation (rTMS) is a promising treatment option for severe, enduring anorexia nervosa (SE-AN; [1]). In a recent feasibility clinical trial (the TIARA study; [2]), we found small effects of rTMS on body mass index (BMI) and eating disorder (ED) symptoms, together with moderate to large positive effects on mood outcomes at follow-up (Cohen's d = 0.61 to 1.0; 4-months post-randomisation), favouring real rTMS over sham, in people with SE-AN [3]. It has been proposed that concurrent antidepressant medication use may influence rTMS treatment outcomes in major depressive disorder (MDD; [4]). A higher proportion of participants (61.7%) in the original TIARA trial were taking antidepressant medication, compared to those in other treatment trials in AN (e.g., [5, 6]). Therefore, using data from the TIARA trial (and the subsequent open trial), we explored whether rTMS treatment response was affected by concurrent antidepressant medication.
Methods
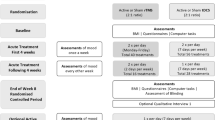
Full methods of the TIARA trial are described elsewhere ([2, 3]; trial registration number: ISRCTN14329415, pre-results). The study was a double-blind, randomised sham-controlled feasibility trial in adult women with SE-AN. Participants were randomly allocated to 20 sessions of real or sham neuro-navigated high-frequency rTMS delivered to the left dorsolateral prefrontal cortex (DLPFC). Participants in the real group received rTMS at the following parameters: 110% resting motor threshold; 10 Hz frequency consisting of twenty 5-s trains with 55-s inter-train intervals (1000 pulses/session) with a total duration of 20 min (see Supplementary S1 for further details). Sham stimulation was administered at the same parameters as real rTMS; however, a sham coil was used. Ethical approval was given by the London – City Road & Hampstead Research Ethics Committee (Reference: 15/LO/0196).
Clinical outcomes were assessed in all participants at baseline (pre-randomisation), within 1 week of completing rTMS treatment (post-treatment; 1-month post-randomisation) and at a follow-up (4-months post-randomisation). Outcomes used in the present analyses were related to ED symptoms, assessed by BMI and the Eating Disorder Examination – Questionnaire (EDE-Q; [7]), and mood, as measured by the Depression Anxiety Stress Scales – Version 21 (DASS-21; [8]). Medication status was recorded at screening and confirmed at start of rTMS treatment.
Participants were unblinded following completion of data collection at the follow-up assessment. If they remained eligible, those who completed sham treatment were given the opportunity to receive real rTMS treatment (using the identical protocol and rTMS parameters to that used in the main trial, described above). Participants who took this opportunity were re-screened and completed baseline, post-treatment, and follow-up assessments at the same schedule as described above as part of an open study. For the present study, only participants who received real rTMS, either in the initial trial (originally allocated to real rTMS) or the associated open study (originally allocated to sham rTMS but completed real rTMS), were included.
Data analyses were performed in Stata 15 [9]. Depending on the distribution of the data, between-subjects t-tests or Mann-Whitney U tests were used to assess group differences in baseline demographic and clinical characteristics. A chi-squared test was used to examine group differences in AN-type. The post-treatment and follow-up group means and SDs for the clinical outcomes were adjusted for baseline (post-treatment/follow-up scores minus baseline scores) and have been presented with between-group effect sizes (Cohen’s d) alongside 95% confidence intervals.
Results
Twenty-six participants received real rTMS and were included in this study (n = 16 initially randomised to real rTMS treatment, n = 10 completed real rTMS treatment as part of the open study after initially being randomised to sham rTMS). Sixteen participants were taking a stable dose of antidepressant medication for the duration of rTMS treatment (data from one participant is missing at follow-up) and ten were not taking antidepressants. In the antidepressant group, ten were taking only a selective serotonin reuptake inhibitor (n = 1 Fluvoxamine, n = 2 Fluoxetine, n = 7 Sertraline), two were taking both a norepinephrine–dopamine reuptake inhibitor and a selective serotonin reuptake inhibitor (n = 1 Bupropion and Sertraline, n = 1 Bupropion and Fluoxetine), two were taking a selective serotonin and norepinephrine reuptake inhibitor (Duloxetine), one was taking a monoamine oxidase inhibitor (Phenelzine), and one was taking a tetracyclic antidepressant (Mirtazapine).
Full medication details and other concurrent treatments are detailed in Supplementary S2. Baseline demographics for both groups are shown in Table 1. Groups did not significantly differ in demographic or clinical characteristics at baseline (p > 0.05), although the antidepressant group reported more severe ED, depression and anxiety symptoms. Clinical characteristics at post-treatment and follow-up are presented in Supplementary S3.
The means, standard deviations and between-group treatment effect sizes (with confidence intervals) for change scores (baseline to post-treatment and baseline to follow-up) of the clinical outcomes are shown in Table 2. Post-treatment group differences in clinical outcomes were of small effect: ED symptom outcomes favoured rTMS with concurrent antidepressant medication whereas BMI and mood outcomes favoured rTMS alone (i.e., no concurrent antidepressant medication). At follow-up however, there were large between-group effect sizes in measures of ED symptoms and small to medium effect sizes for BMI and mood outcomes. These all favoured rTMS treatment with concurrent antidepressant medication.
We further explored the association between antidepressant use and changes in ED symptoms by calculating ED symptom recovery rates (EDE-Q Global Score < 2.77, i.e., < 1 SD above community mean; [10]) for each group. In the antidepressant group at baseline, no participants were classed as recovered in terms of ED symptoms. ED symptom recovery was reported in 3/16 (18.75%) participants at post-treatment and 6/15 (40%) participants (including the n = 3 recovered at post-treatment) at follow-up. In the no antidepressant group, of those who did not report ED symptom recovery prior to rTMS treatment (n = 7, 70%), one additional participant reported ED symptom recovery at post-treatment only (1/7, 14.29%) and one further participant at follow-up only (1/7, 14.29%).
Discussion
This small exploratory study examined the potential effects of antidepressant medication on responsiveness to rTMS treatment in people with SE-AN. These preliminary findings show that concurrent antidepressant medication is not associated with ED outcomes immediately post-rTMS treatment nor with mood-related outcomes at post-treatment or follow-up. In fact, at follow-up, in the antidepressant group, depression scores remained in the severe range (according to clinical cut-off scores on the DASS-21; [8]). However, in relation to ED symptoms, there were large between-group effect sizes on change scores from pre-treatment to follow-up: these favoured the group with real rTMS and concurrent antidepressant medication. Furthermore, following rTMS treatment, a greater number of participants in the antidepressant group reported ED symptom recovery compared to those who were not on concurrent antidepressant medication. This is of particular relevance given the somewhat limited treatment success usually seen in SE-AN.
Antidepressants are commonly prescribed to adults with AN [11]. There is some evidence that they improve symptoms of comorbid depression in AN [12], but limited data for them being effective in improving ED symptoms [13]. In the TIARA trial, ~ 60% of our participants were taking antidepressants and in fact, the total group had somewhat higher depression scores compared to other treatment studies of AN (e.g., [5]). In the present analyses, those taking antidepressants reported more severe ED, depression and anxiety symptoms at baseline i.e., they appeared to be more psychologically unwell (though none of the differences were statistically significant). In this context, it is of note that none of the participants in the antidepressant group, but 3/10 (30%) of the participants in the no antidepressant group, reported ED symptom recovery prior to rTMS treatment.
In MDD, rTMS is typically administered as an augmentation therapy to antidepressant medication (e.g., [14]). However, little is known about the potential impact of antidepressants on the clinical efficacy of rTMS (and vice versa). Data on the effects of concurrent antidepressant medication during rTMS treatment for MDD is mixed, reporting either an enhancement of the rTMS response [4, 15] or no effect [16]. In terms of potential synergistic mechanisms, it is of note that both rTMS and antidepressant medication (including those with rapid onset effects) have been reported to alter neuronal plasticity and cortical excitability [17,18,19,20]. To an extent, this is suggested by our data. It is unclear however, why antidepressant status was associated with improvements in ED outcomes, but not with significant changes in mood following the rTMS treatment, especially as symptoms of depression are the typical target of antidepressants and these medications are reported to have little efficacy in treating ED symptoms [13].
Our study has some limitations: our sample size was small and it is an exploratory analysis of pre-existing data, i.e., concurrent antidepressant medication and dose were not standardised across participants and a proportion in both groups were also taking other psychotropic medications. It was not possible to explore whether other concurrent medications (e.g., benzodiazepines) were associated with rTMS response in SE-AN due to the small number of participants taking these. Recent research suggests that in response to rTMS treatment in MDD, benzodiazepine use is associated with less improvement and psychostimulants with greater improvement [16, 21]. For these exploratory analyses, we combined participants who received real rTMS from the original randomised controlled trial (i.e., participants were blinded) with those who received real rTMS as part of the open label follow-up (i.e., participants were unblinded). However, there was approximately equal distribution of these across the no antidepressant and antidepressant groups (e.g., 60–62.5% in both groups received real rTMS in the original randomised controlled trial). In addition, we identified a possible floor effect in the no antidepressant group in terms of ED symptom recovery, where a limited potential for further symptom reductions in these participants may have contributed to the findings. Furthermore, we did not systematically assess comorbid psychiatric diagnoses (e.g., depression). Given the relatively short follow-up period, longer term follow-ups are needed to examine whether the observed effects persist and/or extend to other clinical features. There is likely also value in exploring the combination of rTMS with other treatment approaches, aside from medication in SE-AN, such as psychotherapy or cognitive training [22].
Conclusions
In people with SE-AN, who received 20 sessions of high-frequency rTMS to the left DLPFC, we have obtained preliminary findings that at follow-up, antidepressant medication appears to enhance the response to rTMS with respect to ED symptoms but not to affective symptoms. The impact of concurrent medication on rTMS efficacy needs to be more rigorously tested in larger samples of people with SE-AN and these preliminary results provide the basis for hypothesis generation for these future studies.
Availability of data and materials
The datasets generated and/or analysed during the current study are not publicly available but are available from the corresponding author on reasonable request.
Abbreviations
- AN:
-
Anorexia nervosa
- BMI:
-
Body mass index
- DASS-21:
-
Depression Anxiety and Stress Scales – Version 21
- ED:
-
Eating disorder
- EDE-Q:
-
Eating Disorder Examination Questionnaire
- MDD:
-
Major depressive disorder
- rTMS:
-
Repetitive transcranial magnetic stimulation
- SE-AN:
-
Severe enduring anorexia nervosa
References
Dalton B, Bartholdy S, Campbell IC, Schmidt U. Neurostimulation in clinical and sub-clinical eating disorders: a systematic update of the literature. Curr Neuropharmacol. 2018;16(8):1174–92. https://doi.org/10.2174/1570159X16666180108111532.
Bartholdy S, McClelland J, Kekic M, O’Daly OG, Campbell IC, Werthmann J, et al. Clinical outcomes and neural correlates of 20 sessions of repetitive transcranial magnetic stimulation in severe and enduring anorexia nervosa (the TIARA study): study protocol for a randomised controlled feasibility trial. Trials. 2015;16:548. https://doi.org/10.1186/s13063-015-1069-3.
Dalton B, Bartholdy S, McClelland J, Kekic M, Rennalls SJ, Werthmann J, et al. Randomised controlled feasibility trial of real versus sham repetitive transcranial magnetic stimulation treatment in adults with severe and enduring anorexia nervosa: the TIARA study. BMJ Open. 2018;8(7):e021531. https://doi.org/10.1136/bmjopen-2018-021531.
Berlim MT, Van den Eynde F, Daskalakis ZJ. High-frequency repetitive transcranial magnetic stimulation accelerates and enhances the clinical response to antidepressants in major depression: a meta-analysis of randomized, double-blind, and sham-controlled trials. J Clin Psychiatry. 2013;74(2):e122–9. https://doi.org/10.4088/JCP.12r07996.
Byrne S, Wade T, Hay P, Touyz S, Fairburn CG, Treasure J, et al. A randomised controlled trial of three psychological treatments for anorexia nervosa. Psychol Med. 2017;47(16):2823–33. https://doi.org/10.1017/S0033291717001349.
Schmidt U, Magill N, Renwick B, Keyes A, Kenyon M, Dejong H, et al. The Maudsley Outpatient Study of Treatments for Anorexia Nervosa and Related Conditions (MOSAIC): comparison of the Maudsley Model of Anorexia Nervosa Treatment for Adults (MANTRA) with specialist supportive clinical management (SSCM) in outpatients with broadly defined anorexia nervosa: a randomized controlled trial. J Consult Clin Psychol. 2015;83(4):796–807. https://doi.org/10.1037/ccp0000019.
Fairburn CG, Beglin SJ. Appendix: eating disorder examination questionnaire (EDE-Q version 6.0). In: Fairburn CG, editor. Cognitive behaviour therapy and eating disorders. New York: Guilford Press; 2008.
Lovibond SH, Lovibond PF. Manual for the depression anxiety stress scales. 2nd ed. Sydney: Psychology Foundation; 1995.
StataCorp. Stata statistical software: release 15. College Station: StataCorp LLC; 2017.
Mond JM, Hay PJ, Rodgers B, Owen C. Eating disorder examination questionnaire (EDE-Q): norms for young adult women. Behav Res Ther. 2006;44(1):53–62. https://doi.org/10.1016/j.brat.2004.12.003.
Garner DM, Anderson ML, Keiper CD, Whynott R, Parker L. Psychotropic medications in adult and adolescent eating disorders: clinical practice versus evidence-based recommendations. Eat Weight Disord. 2016;21(3):395–402. https://doi.org/10.1007/s40519-016-0253-0.
Marvanova M, Gramith K. Role of antidepressants in the treatment of adults with anorexia nervosa. Ment Health Clin. 2018;8(3):127–37. https://doi.org/10.9740/mhc.2018.05.127.
Crow SJ. Pharmacologic treatment of eating disorders. Psychiatr Clin North Am. 2019;42(2):253–62. https://doi.org/10.1016/j.psc.2019.01.007.
Mutz J, Vipulananthan V, Carter B, Hurlemann R, Fu CHY, Young AH. Comparative efficacy and acceptability of non-surgical brain stimulation for the acute treatment of major depressive episodes in adults: systematic review and network meta-analysis. BMJ. 2019;364:l1079. https://doi.org/10.1136/bmj.l1079.
Sehatzadeh S, Daskalakis ZJ, Yap B, Tu H, Palimaka S, Bowen JM, et al. Unilateral and bilateral repetitive transcranial magnetic stimulation for treatment-resistant depression: a meta-analysis of randomized controlled trials over 2 decades. J Psychiatry Neurosci. 2019;44(3):151–63. https://doi.org/10.1503/jpn.180056.
Hunter AM, Minzenberg MJ, Cook IA, Krantz DE, Levitt JG, Rotstein NM, et al. Concomitant medication use and clinical outcome of repetitive transcranial magnetic stimulation (rTMS) treatment of major depressive disorder. Brain Behav. 2019;9(5):e01275. https://doi.org/10.1002/brb3.1275.
Duman RS, Aghajanian GK, Sanacora G, Krystal JH. Synaptic plasticity and depression: new insights from stress and rapid-acting antidepressants. Nat Med. 2016;22(3):238–49. https://doi.org/10.1038/nm.4050.
Duman RS, Shinohara R, Fogaca MV, Hare B. Neurobiology of rapid-acting antidepressants: convergent effects on GluA1-synaptic function. Mol Psychiatry. 2019;24(12):1816–32. https://doi.org/10.1038/s41380-019-0400-x.
Zanos P, Thompson SM, Duman RS, Zarate CA Jr, Gould TD. Convergent mechanisms underlying rapid antidepressant action. CNS Drugs. 2018;32(3):197–227. https://doi.org/10.1007/s40263-018-0492-x.
Minzenberg MJ, Leuchter AF. The effect of psychotropic drugs on cortical excitability and plasticity measured with transcranial magnetic stimulation: implications for psychiatric treatment. J Affect Disord. 2019;253:126–40. https://doi.org/10.1016/j.jad.2019.04.067.
Deppe M, Abdelnaim M, Hebel T, Kreuzer P, Poeppl T, Langguth B, et al. Concomitant lorazepam use and antidepressive efficacy of repetitive transcranial magnetic stimulation in a naturalistic setting. Eur Arch Psychiatry Clin Neurosci. 2020. https://doi.org/10.1007/s00406-020-01160-9.
Sathappan AV, Luber BM, Lisanby SH. The dynamic duo: combining noninvasive brain stimulation with cognitive interventions. Prog Neuro-Psychopharmacol Biol Psychiatry. 2019;89:347–60. https://doi.org/10.1016/j.pnpbp.2018.10.006.
Acknowledgements
We would like to thank the individuals who participated in this study for their time and commitment.
Funding
This work was supported by a National Institute for Health Research (NIHR) Research for Patient Benefit (RfPB) grant (RB-PG-1013-32049) and Infrastructure Support for Pilot studies from the NIHR Biomedical Research Centre (BRC) at South London and Maudsley NHS Foundation Trust (SLaM) and King’s College London (KCL). Ulrike Schmidt is supported by an NIHR Senior Investigator Award. Ulrike Schmidt and Iain Campbell receive salary support from the NIHR Mental Health BRC at SLaM NHS Foundation Trust and KCL. The views expressed are those of the author(s) and not necessarily those of the NHS, the NIHR or the Department of Health.
Author information
Authors and Affiliations
Contributions
US conceived the study. Data collection was performed by BD, JM, SB, and MK. BD analysed and interpreted the data and drafted and prepared the manuscript. ICC assisted with drafting the manuscript and data interpretation. All authors critically reviewed and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Ethical approval was given by the London – City Road & Hampstead Research Ethics Committee (Reference: 15/LO/0196).
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Dalton, B., McClelland, J., Bartholdy, S. et al. A preliminary exploration of the effect of concurrent antidepressant medication on responses to high-frequency repetitive transcranial magnetic stimulation (rTMS) in severe, enduring anorexia nervosa. J Eat Disord 9, 16 (2021). https://doi.org/10.1186/s40337-021-00370-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s40337-021-00370-3