Abstract
Background
We aimed to synthesise data on issues related to stakeholder perceptions of consent for the use of secondary data. To better understand the current literature available, we conducted a systematic literature review of healthcare consumer attitudes towards the secondary use and sharing of health administrative and clinical trial data.
Methods
EMBASE/MEDLINE, Cochrane Library, PubMed, CINAHL, Informit Health Collection, PROSPERO Database of Systematic Reviews, PsycINFO and ProQuest databases were searched. Eligible articles included those reporting qualitative or quantitative original research and published in English. No restrictions were placed on publication dates, study design or disease setting. One author screened articles for eligibility and two authors were involved in the full-text review process. Conflicts were resolved by consensus. Quality and bias were assessed using the QualSyst criteria for qualitative studies.
Results
This paper focuses on a subset of 47 articles identified from the wider search and focuses on the issue of consent. Issues related to privacy, trust and transparency, and attitudes of healthcare professionals and researchers to secondary use and sharing of data have been dealt with in previous publications. Studies included a total of 216,149 respondents. Results indicate that respondents are generally supportive of using health data for research, particularly if the data is de-identified or anonymised. The requirement by participants to obtain consent prior to the use of health data for research was not universal, nor is the requirement for this always supported by legislation. Many respondents believed that either no consent or being informed of the research, but not providing additional consent, were sufficient.
Conclusions
These results indicate that individuals should be provided with information and choice about how their health data is used and, where feasible, a mechanism to opt-out should be provided. To increase the acceptability of using health data for research, health organisations and data custodians must provide individuals with concise information about data protection mechanisms and under what circumstances their data may be used and by whom.
Systematic review registration
PROSPERO CRD42018110559 (update June 2020).
Similar content being viewed by others
Explore related subjects
Find the latest articles, discoveries, and news in related topics.Background
As healthcare moves to an increasingly digitised environment, new opportunities for researchers emerge. The use of health data traditionally collected for administrative purposes can be combined (linked) with other datasets to allow better insights into real-world clinical practice and patient outcomes. Further, this data can be used to inform health system design and responsiveness. In addition, data obtained during a clinical trial is also a key source of information; the secondary analysis of this data can confirm new findings and encourages transparency in research [1,2,3,4].
While the benefits of secondary data analysis have been widely discussed over the last decade, questions about how this data is accessed, by whom, and under what circumstances continue to attract debate. The principles of the International Conference on Harmonisation-Good Clinical Practice (ICH-GCP) and the requirement for obtaining informed consent prior to participating in research [5] are well known. However, the requirement for consent to use both administrative and clinical trial health data for secondary purposes is less clear to both patients and researchers. The use of this data, particularly health administrative data, is regulated by privacy laws of the country in which the data was collected. In Australia, the Commonwealth Privacy Act (1988) (the Act) [6] promotes and protects the privacy of individuals. Given the sensitive nature of health data, the Act provides extra protection around its collection and handling [7]. In certain circumstances, this data can be accessed for health and medical research, and where individual consent is impractical, two legally binding guidelines issued by the National Health and Medical Research Council (NHMRC) [7] add additional protections. The first stipulates data handling procedures for human research and ethics committees (HRECs) and researchers when using personal information disclosed from a Commonwealth agency for medical research (Guidelines under Section 95 of the Act) [7]. The second provides a framework for HRECs to assess proposals which use health information without an individuals’ consent (Guidelines under Section 95A of the Act) [7].
While there is a large amount of literature on the attitudes of healthcare consumers towards secondary data usage, it is fundamental that researchers develop a better understanding of the views of healthcare consumers towards consent for its use. Therefore, this paper presents a synthesis of health consumers’ attitudes towards consent and the use of administrative data and clinical trial data for research purposes.
Methods
This systematic literature review presents the results of a subset of articles identified in a larger review of articles addressing data sharing which was undertaken in accordance with the PRISMA statement for systematic reviews and meta-analysis [8]. The protocol was prospectively registered on PROSPERO (www.crd.york.ac.uk/PROSPERO, CRD42018110559, updated June 2020). Given the substantial number of articles identified in our larger search, we have focused on specific issues over three articles; results relating to the attitudes of health researchers and issues relating to privacy, trust and transparency have been reported in other publications [9, 10].
The following databases were searched: EMBASE/MEDLINE, Cochrane Library, PubMed, CINAHL, Informit Health Collection, PROSPERO Database of Systematic Reviews, PsycINFO and ProQuest. The search was conducted on 24 June 2020. No date restrictions were placed on the search; key search terms are listed in Table 1.
Our original goal was to focus on attitudes towards data reuse by breast cancer patients. However, due to a paucity of studies targeting this group, we re-ran the search without this limitation and present the results of all disease settings. Breast cancer is a disease that impacts older individuals, therefore respondents under the age of 18 years were excluded from this analysis, as were attitudes towards biobanking and genetic research.
We note that increasingly the delineation between data collected for administrative purposes and other forms of electronic documentation such as electronic health records (EHR) (or other terms for these) becomes less clear. These records can contain both administrative and clinical data. Where possible, EHRs have been excluded from this literature review; however, we acknowledge that the lack of separation has made this a grey area.
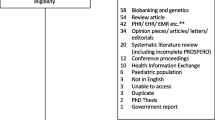
Papers were considered eligible if they were published in English in a peer-reviewed journal; reported original research, were either qualitative or quantitative with any study design, related to data sharing in any disease setting; and included participants over 18 years of age. Reference list and hand searching were undertaken to identify additional papers. Systematic literature reviews were included in the wider search, but were not included in the results. Papers were considered ineligible if they focused on: electronic health records (including other terms for these); health information exchanges; biobanking and genetics; or were review articles; opinion pieces, articles, letters, editorials or non-peer-reviewed theses from masters or doctoral research. Duplicates were removed and title and abstract and full-text screening were undertaken using the Cochrane systematic literature review programme ‘Covidence’ [11]. One author screened articles for eligibility and two authors were involved in the full-text review process; conflicts were resolved by consensus.
Quality and bias were assessed at a study level using the validated QualSyst system for quantitative and qualitative studies as described by Kmet et al. [12]; the assessment was undertaken using the criteria for qualitative studies. No modifications were made to the QualSyst criteria prior to use. Quality and bias assessment was undertaken independently by two authors; conflicts were resolved by consensus. A maximum score of 20 is assigned to articles of high quality and low bias; the final QualSyst score is a proportion of the total with a possible score ranging from 0.0 to 1.0 [12].
Data extraction was by one author undertaken using a pre-piloted form in Microsoft Office Excel; a second author confirmed the data extraction. Conflicts were resolved by consensus. Data points included: author, country and year of study, study design and methodology, health setting and key themes and results. Where available, detailed information on research participants was extracted including age, sex, employment status, highest level of education and health status.
Quantitative data were summarised using descriptive statistics. Synthesis of qualitative findings used a meta-aggregative approach, in accordance with guidelines from Lockwood et al. [13]. The main themes of each qualitative study were first identified and then combined, if relevant, into categories of commonality. Using a constant comparative approach, higher order themes and subthemes were developed. Quantitative data relevant to each theme were then incorporated. Using a framework analysis approach as described by Gale et al. [14], the perspectives of different groups towards data sharing were identified. Where differences occurred, they are highlighted in the results. Similarly, where systematic differences according to other characteristics (such as age or sex) occurred, these are highlighted.
Results
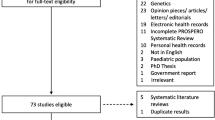
This search identified 10,500 articles, of which 323 underwent full-text screening; 75 articles met the inclusion criteria for the larger review. The PRISMA diagram is presented in Fig. 1. This article presents a subset of the results of the wider search and focuses on issues of consent.
A subset of 47 [15,16,17,18,19,20,21,22,23,24,25,26,27,28,29,30,31,32,33,34,35,36,37,38,39,40,41,42,43,44,45,46,47,48,49,50,51,52,53,54,55,56,57,58,59,60,61] of the 75 articles addressed issues relating to consent in the context of sharing health data and were included in this analysis (Fig. 1 and Table 2). A total of 216,149 respondents were included in the studies.
Study design, location, clinical focus and study populations
Qualitative research methodologies included interviews (face-to-face or via telephone) [16, 19, 22, 45] and focus groups [31, 33, 36, 38], a combination of both [49] or surveys and focus groups [57]. Other methodologies included questionnaire-based interviews [50], surveys [15, 17, 18, 20, 21, 25, 26, 28,29,30, 32, 34, 37, 39, 40, 42, 44, 46, 48, 53,54,55, 58, 59] and combinations of deliberative sessions/interviews and surveys [23,24,25, 27, 56, 57]. Two studies used a citizens’ jury model [43, 51], one study was a randomised controlled trial [47], one was a nested cohort within a randomised controlled study [41], three studies requested consent to access data by letter [35, 52, 61] and one requested consent directly from the participant [60]. Studies were conducted in several countries; a breakdown by country is presented in Table 3.
Most articles focused on the attitudes of the general public towards the access to and secondary use of digital health data in different settings, particularly general medicine [16, 18, 20, 21, 26, 30, 31, 34,35,36,37,38, 40, 41, 44,45,46,47,48, 50,51,52,53,54,55,56, 58,59,60,61], but also National Cancer databases [19, 39], and pharmacoepidemiological [43] and epidemiological [29, 33, 49] research. Other studies focused on the attitudes of health consumers to secondary data analysis and sharing of health data in individuals: attending US Veterans Affairs (VA) facilities [27], retirees [45], recently discharged from tertiary care [23], patients attending a hospital with a cancer diagnosis [32], cardiology patients [15] and patients with asthma and stable angina [17]. Other articles focused on responses from those with acquired immune deficiency syndrome (AIDS) or multiple sclerosis (MS) or mental health concerns [42], rare diseases [25, 28], clinical trial data [22], fertility [24] and respondents with potentially stigmatising conditions (DM, hypertension, chronic depression, human immunodeficiency virus [HIV], breast cancer or lung cancer) [57].
Articles considered general attitudes towards health data use [15,16,17,18, 20, 21, 25, 26, 37, 38, 41, 45,46,47,48, 50, 57,58,59, 61], linking health administrative data to clinical trial data [32] and reuse of clinical trial data [22], access to medical records [23, 27, 29, 31, 33, 35, 40, 42,43,44, 48, 51, 52, 54,55,56,57,58, 60], statistical databases [36], registries [19, 24, 28, 30, 39], health data for epidemiological research [49] and the linking of health insurance data with survey data [34]. Commercial access to health data [53] was considered in one article. Five studies included data from respondents both over and under the age of 18 years of age [16, 19, 26, 37, 60]; where this has happened, only data from respondents over 18 years of age have been included in this analysis.
Mechanisms of consent
Several mechanisms of consent were discussed in the articles; a description of each of the consent mechanisms, by study, is included in Table 4.
Study quality
Results of the quality assessment are provided in Table 2. QualSyst [12] scores ranged from 0.35 to 1.0 (possible range 0.0 to 1.0). While no studies were blinded, most provided clear information on respondent selection and data analysis methods and used justifiable study designs and methodologies. No key themes stood out for studies which were deemed to be of lower quality. No data were from randomised studies; the highest level of evidence was from a nested cohort, with other data obtained from studies which used surveys and interviews.
Consent preferences
The included studies described several consent models including opt-in, opt-out, passive, broad (blanket), none, assumed and dynamic models (see Table 4). Key observations from the included studies are presented below and in Table 2.
Studies from Continental Europe
Five studies described the issues of data usage and consent preferences of Continental European respondents [22, 25, 28, 30, 50] representing a total of 6790 respondents. Consent preferences for accessing data held in registries were not universal, and a willingness to share health data was not precluded by a wish to control access to it [25]. In the setting of registry-based research, respondents to a quantitative study were divided between believing that a single informed consent was acceptable, that no consent was necessary, that consent should be sought in some cases or sought every time [30]. Some respondents believed that their data should not be used at all for research, while others believed that everyone’s medical records should be available for research [30]. Where there is a potential for the data to be used for research, respondents wanted to be informed at the time of hospital admission, and over half of respondents wanted specific details about the type of research for which it could be used [30]. In the setting of a leukodystrophy registry, respondents in a qualitative study believed that a combination of initial broad consent, supported by ongoing information about the use of data, research results and new partnerships (academic and/or pharmaceutical companies) was acceptable [28]. The use of an interactive consent tool, where individuals could specify their consent preferences and exercise more control over their data, was supported [22].
Studies from the UK and Ireland
Sixteen studies [16, 19, 23, 24, 26, 29, 31, 33, 37, 39, 44, 46, 47, 51,52,53] from the UK and Ireland discussed health data usage and consent preferences representing a total of 108,824 respondents. The proportion of respondents who would give permission to access information in their medical notes was high, but varied based on the type of information to be used [23]. Most respondents wanted to be asked when data relating to side effects and medical history were taken from medical records, while few wanted to be informed when data on sex and age were sought (5% and 7% respectively) [23]. Signing a consent form to allow future data use during the patient’s hospitalisation was a preferred method but respondents were also happy to be informed, but not required to provide consent, each time the data was to be used [23]. Variation in views on the need for consent was seen in other studies; while some respondents acknowledged that re-consent is difficult and has the potential for low response rates, they still saw it as best practice to ask [33]. For some, an opt-out consent process was seen as acceptable as it allows the individual the right to refuse participation while informing them of the types of research being undertaken [33, 51, 52]. Higher rates of support were shown for the current data collection methods used for the UK cancer registry in people living with cancer (PLWC) (65%) compared with general public respondents (52%); however, 9% (PLWC) and 12% (general public) were opposed [39]. Of those who were opposed, 6% (PLWC) and 17% (general public) believed that it should be an ‘opt-in’ process rather than ‘opt-out’ [39]. While there are opt-out and data withdrawal options for the UK cancer registry, few were aware of these options [39]. Two studies noted the complexity of retrospectively opting out of data collection processes [24, 31]. A citizens’ jury process found that respondents preferred opt-out consent over opt-in (70.6% vs 17.6%); a small percentage (8.8%) believed that all records should be available for use for the public benefit [51]. In one study, younger respondents equated an ‘opt-in’ process with being asked if their data could be used [16].
Studies from North America
Ten studies from the USA [17, 18, 20, 27, 35, 38, 40, 45, 58, 60] and six from Canada [15, 32, 42, 55,56,57] discussed secondary data use and consent preferences representing a total of 42,620 respondents. Studies from Canada showed variability in consent preferences and included the use of consent each time, broad consent, and notification with opt-out consent [55]. Many respondents believed that no consent or notification was required in some circumstances [42, 55]. Where general consent was provided, 80% wanted to periodically review this decision, while others wanted either no or minimal involvement (36%) or notification with an opt-out option (24%) [55]. Various consent processes were proposed across the studies and included opt-out [27], opt-in [56], opt-in/one-off consent with blanket authorisation [27, 42], consent to be sought each time [27, 42, 56], assumed consent [56] or no requirement for consent but with individuals being informed about data usage [42]. Respondents liked different aspects of each consent process [56]. For some, where consent was not sought, respondents considered it to be a violation of privacy [38]. In the setting of potentially stigmatising health conditions, respondents to a mixed-methods study had a range of views about consent ranging from ‘just use it’ to ‘the information should not be shared at all’ [57]. Respondents felt that where data were to be used for quality improvement, no consent was needed; however, where data were to be linked or used in profit-based activities, consent was required before each use [57].
Studies from Australia and New Zealand
Six studies from Australia [21, 36, 48, 49, 59, 61] and two from New Zealand [43, 54] discussed consent preferences and represented a total of 42,104 respondents. While seeking consent to use data should be the ‘cornerstone’ of contemporary research practice [49], views on consent about the use of health data for research ranged from not important to the need to provide detailed information [36]. Respondents to a qualitative study believed that while people had the right to refuse access to health data for research, most believed that data linkage research could be undertaken without consent [59]. Reasons for not requiring consent included a perceived benefit from research, large datasets serving as protection, practical considerations, that the use of de-identified data does not breach privacy, and that audit activities do not require consent [59]. Where data was to be used for epidemiological research, respondents in a mixed-methods study were divided about the requirement for consent [49]. Opt-out consent was considered acceptable to 54% of the respondents in one study, but nearly one-third (28%) preferred an opt-in method and a fifth had no preference (19%) [21]. The use of a hybrid consent model was proposed in a quantitative study from New Zealand [54]. This method proposed a mix of general consent processes including specific criteria for use in the context of accessing data in the clinical setting and the requirement for specific consent when data is accessed for other purposes [54].
Several other themes were addressed in the included papers and are presented below by theme.
Support for medical research and permission to access data
Several studies noted broad support for medical research [15, 19, 28, 30,31,32,33, 36, 42,43,44, 49, 51, 55, 58, 59] using both identifiable [42] and de-identified or anonymous [31, 36, 43] data. Reasons for support included the potential to develop/improve medical care and reduce medical errors [42], develop new treatments [25], and an increased understanding of disease and diagnosis [25]. Other reasons included a sense of obligation to make data collected when using government health services available [49], and to benefit society more generally [44, 59]. A small percentage (approximately 4%) of respondents were not supportive of using medical data for research [28, 30, 55]. In an Australian study, 46% of respondents assumed that their health data was already used for medical research, without explicit consent [21], and in a second study, respondents believed that health data was a similar resource to tissue samples [22]. Several articles discussed preferences in relation to the levels of permission required to access data and varied by the type of data to be accessed. Support for secondary data usage was high, in one study, 97.4% of respondents (N = 590) would allow researchers to access their data for the purposes of conducting a clinical trial [15] or for health services research (67%; N = 1,106) [58]. However, a significant number of participants did not provide consent, between 10% (N = 3,429) [17] and 25% [58]. Respondents wanted to be asked permission when their data was to be used for reasons other than treatment [36], but permission was least required when age or sex was extracted [23]. Even in the setting of using anonymous data, respondents wanted to or preferred to be asked permission [23]. Some respondents believed no consent was required prior to use when their health data were anonymous [36, 42]. Where consent was not feasible, but required to conduct the research, over 50% of respondents believed that it was essential, even if it meant not conducting the research [42]. Nearly half of the respondents (50% PLWC, 43% general public) were concerned about a lack of permission being sought prior to their data being included in the UK cancer registry [39].
Record linkage
Agreement with record linkage was generally high [18, 20, 26, 34, 37, 50] ranging between 96.3% (N = 2,271) [18] and 86.2% (N = 1,574) [20]; however, agreement for data linkage was significantly lower in other studies [61], with rates between 41% (N = 6,433 and N = 13,454) [37, 46] and 67.8% (N = 6384) [45]. There was some misunderstanding about what data linking is, with some believing that it relates to information sharing within the health system [59]. A lack of consensus on the requirement for consent for data linkage is evident. Some respondents wanted to provide consent [16, 44], broad consent [56], consent in specific circumstances [30], or notification with opt-out options [56]. Some respondents believed that there was no requirement for consent [16, 44, 56, 59], while others believed that everyone’s data should be available for research [30]. In one study, if consent was not obtained, 31% of respondents (N = 1,202) believed that the research should be abandoned; however, an equal number believed that while consent should be sought, the research should not be abandoned if it was not possible (34%) [44].
Consent for record linkage was influenced by health status [20], socio-economic variables [26], demographics [20, 26], and what datasets were to be linked [56]. Where data was linked to education or economic data [46, 55] or a government identification number (ID) [41] agreement for record linkage decreased. Respondents who provided no information on income were less likely to give consent to data linkage, if they did consent it was more likely for administrative data [50]. Linking health data to education, income or occupation records, resulted in respondents wanting more control over consent mechanisms. Interestingly, respondents were more willing to link health data to biological samples, compared with this data, although consent was required [57].
Organisations and individuals conducting the research and proposed use of data
Consent to share data was influenced by the organisations or individuals conducting the research and the nature of the data to be shared [23, 36, 54]. In the setting of health registries, there was support for the information to be used for aetiological studies, disease monitoring, and assessing the effectiveness of healthcare; many believed that the information should be used for any research purpose [30]. In one quantitative study, there was strong support for using data when used for rare disease research (90%); however, when the data was used for research into other diseases, the rate of consent was lower [28]. The intended use of data made little impact on support for data reuse, with many having no consent preferences or preferring not to be asked [23]. Respondents preferred to have their data extracted by either a doctor’s nurse [55] or by the NHS [44], although in both studies, some respondents believed both options to be unacceptable. Respondents were less willing to share data with government agencies [42, 54], employers [42], health insurers [54], pharmaceutical companies [42], or with commercial organisations [53]. In these settings, respondents wanted to provide consent [42, 53, 56], even if this means that a lack of consent would stop the research proceeding [53]. Where profit was involved, respondents moved to consent processes with greater control, and where data was to be linked for market research or with leftover tissue specimens, high rates of either ‘should not be used’ or ‘permission required each use’ were seen [56]. For others, the use of data for marketing and/or profit was not seen as appropriate [57]. Where data were to be shared with an outside organisation, the need for re-consent was higher, however this was due to issues of trust and data security more than an objection to data sharing [22]. In the setting of a rare disease, 60% of respondents (n = 149 relatives, n = 46 patients) were willing to have registry data used for research undertaken in partnership with pharmaceutical organisations; about 10% were opposed to this [28].
Identifiable versus non-identifiable/de-identifiable data
Differences in acceptability of the use of health data varied by its identifiability and individual preference. Respondents believed that where data is to be used in an identifiable manner, this needs to be clearly stated at the consent stage, and where data were non-identifiable, respondents were more willing to allow access without consent [24, 42]. Studies from Australia [59] and New Zealand [43, 54] found that respondents were more willing to share de-identified data compared with identifiable data. Respondents believed that identifiable data should only be accessible to researchers in specific circumstances such as to ensure medicine safety [43]. Some respondents believed that once patient identifiers had been removed, it becomes detached from the individual and is just information which should be available to researchers [59]. Even when anonymous data are to be used, some voice concern about sharing this data with non-healthcare professionals [54]. Some respondents believed that the process of anonymisation did not remove the need for consent; this was due to concerns about the effectiveness of data anonymisation processes [16] and the belief that data could not ever be fully anonymised [31]. Some respondents believed that the process of anonymisation and data encryption were safeguards, and therefore, no consent was required to use the data [33].
Influences on consent
Age
Several studies found differences in attitudes towards consent by respondent age [17, 30, 52]. Across the studies, older respondents were more willing to share or link data than younger participants [20, 32, 46] and those with younger respondents were more willing to consent to health data use [25, 35, 37, 58, 61] and/or record linkage [26, 34]. One study found that while patterns of consent were similar across responders, consent decreased with age (over 50 years of age) in both males and females [29].
Sex
Differences were seen in support for data reuse and methods of appropriate consent processes by sex; however, these were not always significant [26, 30, 46, 52]. Where it was a factor, males were more likely to consent to medical record review [29] and believed that informed consent was not required for registry-based research more than women [30]. Women believed that consent should be required in some cases more than males (44% compared with 31%) [30], were less likely to give authorisation [35], and consented less [58] suggesting a greater desire for control over their data [25] compared with males.
Location
By location, respondents from Northern Ireland (adjusted OR 50.56; 95% CI, 0.50–0.63) had lower levels of support for data access compared with respondents from other parts of the UK (adjusted OR 51.17; 95% CI, 1.06–1.29) (N = 50,994) [26], and respondents from the former West Germany were less likely to consent to data linkage compared with those from Berlin or East Germany [50]. Respondents living closer to a study centre (5.8% and 2.1%) had higher rates of refusal compared with those living further away [35].
Education and socio-economics
Levels of education influenced attitudes towards consent. Respondents with a secondary education were more likely to provide consent compared with those with lower levels of education [25, 26, 37, 45, 46, 50, 58, 61]. Education level also impacted a respondent’s willingness to share health data without consent. Those with no academic qualifications were less likely to agree to research on health data being conducted without consent compared with those with higher levels of education (38%, no qualification; 26%, graduate level), with this decreasing with as the respondents’ level of education increased [44]. Those with lower levels of education and who had lower incomes were less likely to be non-responders to requests for consent compared with respondents who actively declined consent [58]. In one study, respondents who were married, illiterate, who lived in a suburban area (compared with urban/rural) or those with a lower monthly income were less likely to consent to data linkage [34]. Three studies noted the impact of socio-economic variables on consent; however, all reported different outcomes. While one study found that socio-economics did not influence consent [37], other studies found that low income did influence consent patterns [34] and that respondents in the higher socio-economic group were less likely to provide consent when compared with those in lower socio-economic groups [24]. Respondents who declined to answer questions about income from investments had lower levels of consent for data linkage, however other socio-economic variables did not appear to influence consent [46]. Those who provide consent were more likely to have health insurance [61]. Other influences on providing consent for data use included undertaking voluntary work or previous data record linkage by a family member [46].
Ethnicity
Differences in consent preferences were noted by respondent ethnicity. Research from a study in the UK found that consent for data linkage was significantly lower (58.9%) in respondents (N = 50,994) who identified as non-white compared with those who identified as white (72%) [26]. This was similar to two other studies from the UK and the USA where those who reported their ethnicity to be British/Irish white had higher consent compared with other groups [37], and those who identified as being of African-American heritage were less likely to consent to data usage [58]. Language and the need for an interpreter were also seen to influence consent. In an Australian study, opt-out consent was preferred by respondents who were illiterate in their primary language or who were refugees [21] while an English study found language to be a barrier to discussing/seeking consent [24].
Health status
Consent preferences were found to be influenced by the respondent’s health status. Respondents with lower physical and mental functioning scores, measured using the 36 Item short form (SF-36) questionnaire, were shown to have lower levels of consent for data usage [34]; however, in a second study, respondents with lower SF-36 physical and mental health scores were more likely to consent [58]. In one quantitative study, respondents with lower Charlson Comorbidity Index (CCI) scores were less likely to allow survey and health data linkage compared with respondents with higher scores [20]. Experience of a major personal illness and hospitalisation in the last year [61] and severity of illness [58] did not impact the frequency of consent; however, respondents with more severe rare diseases were more likely to support data sharing compared with those with less severe diseases [25]. Consent was higher in respondents with life-limiting and lifelong illness [26], those with health conditions under investigation [29], those with two or more medical diseases [50], those in good health (compared with those in poorer health) [30], and those with diabetes or who were obese [37]. In contrast, in one quantitative study respondents with long-term health conditions were more likely to be against health data sharing compared with those with no long-term health conditions (~ 25% vs 20%) [44]. Respondents (N = 15,997) who presented for mental health concerns, trauma, and eye care had higher rates of refusal for providing access to medical records for research [60].
Sensitive topics
Several health topics were considered more sensitive than others and influenced consent preferences [48]; the need for ethical oversight when research is undertaken on a sensitive topic [30] was noted. Respondents were less likely to provide consent to access medical records for research which included sensitive topics [35]. Requesting data on sexual orientation [23], sexual or sexually transmissible diseases [42], infectious diseases [35], reproductive issues [35], contraception or female genital disorders [58], urinary disorders [58], mental health [25, 35, 42], disability [25] and genetics [25] were all reasons for increased need to ask permission or provide consent to access data or were associated with lower levels of consent. Interestingly, in one study non-consent rates were higher in respondents seeking care for uncomplicated diabetes and or headache [58], conditions which may not be considered sensitive by healthcare consumers. Women receiving pregnancy care had the highest response of ‘undecided’ about providing consent [60]. In the setting of potentially stigmatising conditions (HIV, chronic depression, HT, alcoholism, DM, breast or lung cancer), provision of consent was similar between diseases [57]. The diagnosis of stable angina or asthma was not considered particularly sensitive [17]; however, for others, information about symptoms and the name of their disease [25] was. Consent was lower in respondents who did not answer questions on smoking status, income, or functional status [58], however, questions relating to income did not always decrease consent [47]. Respondents to a study from New Zealand were less willing to share data of a sensitive nature with those not involved in their care [54]. In one study, respondents with HIV, MS or mental health presentations believed that only physicians involved in their care should be able to access medical records without consent [42]. Where data was to be linked, respondents in one study were unable to reach a consensus on consent when medical data were to be linked with data on teenage pregnancy and state benefits, birthweight and future health outcomes, mental health and criminal records, and asthma diagnosis and postcodes [16]. In other studies, some respondents identified the need for consent where health, employment and WorkCover (workers compensation insurance) data [59] were linked. Consent was not required when health data were linked to cancer registry and death data, and if de-identified health data and criminal records [59].
Other
Several articles discuss the relationship between trust, transparency, privacy and consent, and quality, and these issues are explored at length in a subsequent publication [9]. Other influences on consent included health literacy and government insurance status [18], or requesting a national identity number [41]. Other negative influences on consent included a fear of discrimination, fraud, threat to personal safety and use of data without their knowledge or in a context they do not approve of [25]. Further, perceived benefits and harms, trust, anxiety or feelings of being overwhelmed, and understanding of processes and research more generally influenced consent [24]. Where data were to be used in a for-profit setting or where individuals were more concerned about privacy [57] and where information was to be shared with a third party [25] respondents required more conditions and more restrictive consent processes. Interestingly, in a Canadian study, there was a difference in consent rates for the use of paper-based versus electronic records, with 27% percent of respondents (N = 1,235) believing that electronic data can be used without permission compared with 12% for paper records [55]. Respondents who responded to the request for consent via a website were younger compared with those who responded by letter (38.7 years compared with 53.5 years) [52].
Ethics committees and institutional review boards
The role of human research ethics committees (HREC) and institutional review boards (IRBs) in influencing the need for consent was noted in one study [40]. In one article, the requirements of the IRB were shown to have significantly impacted the overall rates of study consent and completion [40]. Three studies [25, 27, 42] described respondents’ views about the role of HRECs in deciding if researchers should be allowed to access existing health data for research (secondary data analysis). Even in the setting of HREC approval and where the research was deemed low harm, 67.7% of respondents (N = 235) wanted to be asked to consent to the use of their data for medical research [42]. This was similar to a European study, where near equal numbers of respondents (N = 2,013) were for (49%) and against (43%) allowing an HREC to decide about access to data [25]. Finally, one study found that a third of respondents believed that the decision of the HREC regarding consent was sufficient, although two-thirds of respondents wanted to be able to tell the HREC how they wanted their data shared [27].
Activities to improve acceptance of data use
Several studies noted inconsistencies in respondent expectations about secondary data use and local requirements (laws, policies, procedures), with some not requiring individual patient consent to use data [32]. In the UK, the legal framework allows for the use of data for medical research without consent [19]; however, there is also a requirement for individual consent when individual-level administrative data is to be linked to research such as survey data [46]. Inconsistencies between UK legislation and institutional policies and procedures can cause confusion [19]. In one Finnish study, a similar proportion of respondents argued for both a tightening of legislation and an increased liberalisation of laws relating to health data (35% versus 25%) [30]. The inconsistent application of consent generally in society, with both opt-in and opt-out being used, can be confusing to participants [53].
Education and the provision of more information about data use and research practices were cited in several articles. Researchers need to clearly communicate how an individual’s data is to be used and at the conclusion of the study provide feedback and the study results to the participant [25]. Other activities, such as providing increased information about their disease, the capacity to withdraw consent, and being informed of any data breaches if they occur, also promote acceptance of secondary data use in health [25]. Where respondents were provided with information on research processes, they became more accepting of the use of medical data without consent [33, 53]. The requirement for consent was connected to an individual’s desire to control access to data [56], and where obtaining consent is not practical, for transparency researchers should clearly communicate to participants why this is so [53]. Further, individuals should be clearly informed of current data sharing practices [54, 59] when receiving health services; one study noted that implied consent is not always well-informed consent [54]. Increasing the awareness of health research using routine data will increase the acceptability of this type of research and may increase rates of consent [24]. Requesting consent when individuals are under stress or anxious can result in fewer individuals who consent [24]; an Australian study found a delay in seeking approval to link health and survey data did not compromise authorisation rates [48]. In a citizens’ jury process, 50% of respondents (N = 34) became more willing to share their health data for public benefit, a small percentage (5.9%) opted for more control over their data after receiving education and information on research using health data [51]. Clear rules about data not being accessible to third parties and knowledge of these safeguards can increase the acceptability of data sharing [53, 56].
Discussion
This systematic literature review highlights the ongoing complexity associated with secondary data analysis and linking of health data. While respondents believed that the principles of data sharing were sound, agreement on the type and need for consent was not universal. In many circumstances, individuals may not be aware of the current national laws and regulations which govern health data sharing and linking in their countries, and these may be inconsistent with their personal beliefs on the need for consent. The variation in responses about the type of consent that individuals prefer suggests two things. First, that the use of a single type of consent process for all research projects may not be appropriate and that mechanisms such as dynamic or hybrid models should be considered. Second, that even in the setting of seeking consent to use data, not all individuals will agree with consent processes used, or potentially with the use of secondary use of health data more generally.
Differences in the need for consent are complicated by the identifiability and subject of health data to be used. While respondents were generally happy to consider sharing their health data for research, de-identified or anonymous data appeared to be more acceptable to many respondents. Differences in consent preferences require researchers to be conscious of variations by age, sex, ethnicity, location, and education levels of their potential research participants, as this may affect the level of consent preferred. Further, the type and subject matter of the data used may also impact attitudes towards consent, and researchers should be conscious that topics of a sensitive nature may attract less consent. The role of ethics committees in determining the need for consent in studies using secondary data analysis should consistently reflect the requirements of national and local laws and regulations. Researchers need to be better informed about the requirements for consent when undertaking research using health data. Finally, education and information should be provided to the health consumer about data protection mechanisms, how an individual’s health data can and will be used and by whom, and the laws and policies governing secondary use of health information.
Limitations
The papers included in this study were limited to those indexed on major databases, some literature on this topic may have been excluded if it was not identified during the grey literature and hand searching phases. As the search was restricted to English language publications, some relevant literature may have been excluded from the search. We note that health systems and health funding models may be different in non-English speaking countries and that Western ideals of autonomy may not be universally held.
Implications
Results of this systematic literature review indicate that respondents recognised the advantages of health research using existing health data and are generally supportive of these initiatives. The provision of increased information to individuals about data protection and data usage is central to the use of health data for research. Therefore, health organisations and those who act as data custodians should work towards increasing the awareness of current data sharing practices and data protections in their patient populations.
Conclusion
The literature confirms that individuals are generally supportive of using health data for research, particularly in a de-identified or anonymous format. By increasing the awareness of current data sharing practices and data protections in individuals who interact with the health system, the use of medical records for health research may become more widely accepted as a regular function of medical care.
Availability of data and materials
All data generated or analysed during this study are included in this published article.
References
Goldacre B. Are clinical trial data shared sufficiently today? No. Br Med J. 2013;347(1):f1880. https://doi.org/10.1136/bmj.f1880.
Goldacre B, Gray J. OpenTrials: towards a collaborative open database of all available information on all clinical trials. Trials. 2016;17(1):164. https://doi.org/10.1186/s13063-016-1290-8.
Kostkova P, Brewer H, de Lusignan S, Fottrell E, Goldacre B, Hart G, et al. Who owns the data? Open data for healthcare. Front Public Health. 2016;4. https://doi.org/10.3389/fpubh.2016.00007.
Elliott M. Seeing through the lies: innovation and the need for transparency. London: Gresham College Lecture Series; Museum of London; 2016.
Good Clinical Practice Network. International Conference on Harmonisation Good Clinincal Practice (ICH GCP): Good Clinical Practice Network; 2020. Available from: https://ichgcp.net/
Australian Government. Privacy Act (1988) (Cth). Amended 2018. Cited: 28 May 2020. Available from: https://www.legislation.gov.au/Details/C2018C00292.
Office of the Information Commissioner. Health and medical research Canberra: Australian Govenment; 2020. Available from: https://www.oaic.gov.au/privacy/the-privacy-act/health-and-medical-research/. Accessed 26 May 2020.
Moher D, Liberati A, Tetzlaff J, Altman DG, Group P. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Plos Med. 2009;6(7):e1000097-e.
Hutchings E, Loomes M, Butow P, Boyle FM. A systematic literature review of health consumer attitudes towards secondary use and sharing of health administrative and clinical trial data: a focus on privacy, trust, and transparency. Syst Rev. 2020;9(1):235. https://doi.org/10.1186/s13643-020-01481-9.
Hutchings E, Loomes M, Butow P, Boyle FM. A systematic literature review of researchers’ and healthcare professionals’ attitudes towards the secondary use and sharing of health administrative and clinical trial data. Syst Rev. 2020;9(1):240. https://doi.org/10.1186/s13643-020-01485-5.
Veritas Health Innovation. Covidence systematic review software. Melbourne: Cochrane Collaboration; 2018.
Kmet LM, Cook LS, Lee RC. Standard quality assessment criteria for evaluating primary research papers from a variety of fields. Edmonton: Alberta Heritage Foundation for Medical Research (AHFMR); 2004.
Lockwood C, Munn Z, Porritt K. Qualitative research synthesis: methodological guidance for systematic reviewers utilizing meta-aggregation. Int J Evid Based Healthcare. 2015;13(3):179–87. https://doi.org/10.1097/XEB.0000000000000062.
Gale NK, Heath G, Cameron E, Rashid S, Redwood S. Using the framework method for the analysis of qualitative data in multi-disciplinary health research. BMC Med Res Methodol. 2013;13(1):117. https://doi.org/10.1186/1471-2288-13-117.
Avram R, Marquis-Gravel G, Simard F, Pacheco C, Couture E, Tremblay-Gravel M, et al. Understanding the patient perspective on research access to national health records databases for conduct of randomized registry trials. Int J Cardiol. 2018;262:110–6. https://doi.org/10.1016/j.ijcard.2017.12.074.
Audrey S, Brown L, Campbell R, Boyd A, Macleod J. Young peopleʼs views about consenting to data linkage: findings from the PEARL qualitative study. BMC Med Res Methodol. 2016;16(1):34. https://doi.org/10.1186/s12874-016-0132-4.
Baker R, Shiels C, Stevenson K, Fraser R, Stone M. What proportion of patients refuse consent to data collection from their records for research purposes? Br J Gen Pract. 2000;50(457):655–6.
Bakken S, Yoon S, Suero-Tejeda N. Factors Influencing Consent for Electronic Data Linkage in Urban Latinos. Stud Health Technol Inform. 2015;216:984.
Barrett G, Cassell JA, Peacock JL, Coleman MP. National survey of British publicʼs views on use of identifiable medical data by the National Cancer Registry. BMJ. 2006;332(7549):1068–72. https://doi.org/10.1136/bmj.38805.473738.7C.
Beebe TJ, Ziegenfuss JY, Jenkins SM, Haas LR, Davern ME. Who doesn’t authorize the linking of survey and administrative health data? A general population-based investigation. Ann Epidemiol. 2011;21(9):706–9. https://doi.org/10.1016/j.annepidem.2011.03.007.
Boulos D, Morand E, Foo M, Trivedi JD, Lai R, Huntersmith R, et al. Acceptability of opt-out consent in a hospital patient population. Intern Med J. 2018;48(1):84–7. https://doi.org/10.1111/imj.13666.
Broes S, Verbaanderd C, Casteels M, Lacombe D, Huys I. Sharing of clinical trial data and samples: the cancer patient perspective. Front Med. 2020;7:33. https://doi.org/10.3389/fmed.2020.00033.
Campbell B, Thomson H, Slater J, Coward C, Wyatt K, Sweeney K. Extracting information from hospital records: what patients think about consent. BMJ Qual Saf. 2007;16(6):404–8. https://doi.org/10.1136/qshc.2006.020313.
Carson C, Hinton L, Kurinczuk J, Quigley M. ʻI havenʼt met them, I donʼt have any trust in them. It just feels like a big unknownʼ: A qualitative study exploring the determinants of consent to use Human Fertilisation and Embryology Authority registry data in research. BMJ Open. 2019;9(5):e026469.
Courbier S, Dimond R, Bros-Facer V. Share and protect our health data: an evidence based approach to rare disease patients’ perspectives on data sharing and data protection-quantitative survey and recommendations. Orphanet J Rare Dis. 2019;14(1):175. https://doi.org/10.1186/s13023-019-1123-4.
Cruise SM, Patterson L, Cardwell CR, O'Reilly D. Large panel-survey data demonstrated country-level and ethnic minority variation in consent for health record linkage. J Clin Epidemiol. 2015;68(6):684–92. https://doi.org/10.1016/j.jclinepi.2015.01.011.
Damschroder LJ, Pritts JL, Neblo MA, Kalarickal RJ, Creswell JW, Hayward RA. Patients, privacy and trust: patients’ willingness to allow researchers to access their medical records. Soc Sci Med. 2007;64(1):223–35. https://doi.org/10.1016/j.socscimed.2006.08.045.
Darquy S, Moutel G, Lapointe A-S, DʼAudiffret D, Champagnat J, Guerroui S, et al. Patient/family views on data sharing in rare diseases: study in the European LeukoTreat project. Eur J Hum Genet. 2016;24(3):338–43. https://doi.org/10.1038/ejhg.2015.115.
Dunn KM, Jordan K, Lacey RJ, Shapley M, Jinks C. Patterns of consent in epidemiologic research: evidence from over 25,000 responders. Am J Epidemiol. 2004;159(11):1087–94. https://doi.org/10.1093/aje/kwh141.
Eloranta K, Auvinen A. Population attitudes towards research use of health care registries: a population-based survey in Finland. BMC Med Ethics. 2015;16:48.
Haddow G, Bruce A, Sathanandam S, Wyatt JC. ‘Nothing is really safe’: a focus group study on the processes of anonymizing and sharing of health data for research purposes. J Eval Clin Pract. 2011;17(6):1140–6. https://doi.org/10.1111/j.1365-2753.2010.01488.x.
Hay AE, Leung YW, Pater JL, Brown MC, Bell E, Howell D, et al. Linkage of clinical trial and administrative data: a survey of cancer patient preferences. Curr Oncol. 2017;24(3):161–7. https://doi.org/10.3747/co.24.3400.
Hill EM, Turner EL, Martin RM, Donovan JL. “Let’s get the best quality research we can”: public awareness and acceptance of consent to use existing data in health research: a systematic review and qualitative study. BMC Med Res Methodol. 2013;13(1):72.
Huang N, Shih SF, Chang HY, Chou YJ. Record linkage research and informed consent: who consents? BMC Health Serv Res. 2007;7(1):18. https://doi.org/10.1186/1472-6963-7-18.
Jacobsen SJ, Xia Z, Campion ME, Darby CH, Plevak MF, Seltman KD, et al. Potential effect of authorization bias on medical record research. Mayo Clin Proc. 1999;74(4):330-8.
King T, Brankovic L, Gillard P. Perspectives of Australian adults about protecting the privacy of their health information in statistical databases. Int J Med Inform. 2012;81(4):279–89. https://doi.org/10.1016/j.ijmedinf.2012.01.005.
Knies G, Burton J, Sala E. Consenting to health record linkage: evidence from a multi-purpose longitudinal survey of a general population. BMC Health Serv Res. 2012;12(1):52. https://doi.org/10.1186/1472-6963-12-52.
Lucero RJ, Kearney J, Cortes Y, Arcia A, Appelbaum P, Fernandez RL, et al. Benefits and risks in secondary use of digitized clinical data: views of community members living in a predominantly ethnic minority urban neighborhood. AJOB Empir Bioethics. 2015;6(2):12–22. https://doi.org/10.1080/23294515.2014.949906.
Macmillan Cancer S, Cancer Research UK, Ipsos M. Perceptions of the cancer registry: attitudes towards and awareness of cancer data collection. London: Cancer Research UK; 2016.
Nelson K, Garcia RE, Brown J, Mangione CM, Louis TA, Keeler E, et al. Do patient consent procedures affect participation rates in health services research? Med Care. 2002;40(4):283–8. https://doi.org/10.1097/00005650-200204000-00004.
Ni MY, Li TK, Hui RWH, McDowell I, Leung GM. Requesting a unique personal identifier or providing a souvenir incentive did not affect overall consent to health record linkage: evidence from an RCT nested within a cohort. J Clin Epidemiol. 2017;84:142–9. https://doi.org/10.1016/j.jclinepi.2017.01.003.
Page SA, Mitchell I. Patients’ opinions on privacy, consent and the disclosure of health information for medical research. Chronic Dis Can. 2006;27(2):60–7.
Parkin L, Paul C. Public good, personal privacy: a citizensʼ deliberation about using medical information for pharmacoepidemiological research. J Epidemiol Commun Health. 2011;65(2):150–6. https://doi.org/10.1136/jech.2009.097436.
Robinson G, Dolk H, Given J, Karnell K, Gorman EN. Public attitudes to data sharing in Northern Ireland. Northern Ireland: Administrative Data Research Centre; 2016.
Sakshaug JW, Couper MP, Ofstedal MB, Weir DR. Linking survey and administrative records: mechanisms of consent. Sociol Methods Res. 2012;41(4):535–69. https://doi.org/10.1177/0049124112460381.
Sala E, Burton J, Knies G. Correlates of obtaining informed consent to data linkage: respondent, interview, and interviewer characteristics. Sociol Methods Res. 2012;41(3):414–39. https://doi.org/10.1177/0049124112457330.
Shah S, Harris TJ, Rink E, DeWilde S, Victor CR, Cook DG. Do income questions and seeking consent to link medical records reduce survey response rates? A randomised controlled trial among older people. Br J Gen Pract. 2001;51(464):223.
Silva MS, Smith WT, Bammer G. The effect of timing when seeking permission to access personal health services utilization records. Ann Epidemiol. 2002;12(5):326–30. https://doi.org/10.1016/S1047-2797(01)00261-7.
Slegers C, Zion D, Glass D, Kelsall H, Fritschi L, Brown N, et al. Why Do People Participate in Epidemiological Research? J Bioethical Inq. 2015;12(2):227–37. https://doi.org/10.1007/s11673-015-9611-2.
Stallmann C, Swart E, Robra BP, March S. Linking primary study data with administrative and claims data in a German cohort study on work, age, health and work participation: is there a consent bias? Public Health. 2017;150:9–16. https://doi.org/10.1016/j.puhe.2017.05.001.
Tully MP, Bozentko K, Clement S, Hunn A, Hassan L, Norris R, et al. Investigating the extent to which patients should control access to patient records for research: a deliberative process using citizensʼ juries. J Med Internet Res. 2018;20(3):e112 (page 1-15).
Vellinga A, Cormican M, Hanahoe B, Bennett K, Murphy AW. Opt-out as an acceptable method of obtaining consent in medical research: a short report. BMC Med Res Methodol. 2011;11(1):40. https://doi.org/10.1186/1471-2288-11-40.
Wellcome Trust, Mori I. The one-way mirror: public attitudes to commercial access to health data. London: Wellcome Trust; 2016.
Whiddett R, Hunter I, Engelbrecht J, Handy J. Patients’ attitudes towards sharing their health information. Int J Med Inform. 2006;75(7):530–41. https://doi.org/10.1016/j.ijmedinf.2005.08.009.
Willison DJ, Schwartz L, Abelson J, Charles C, Swinton M, Northrup D, et al. Alternatives to project-specific consent for access to personal information for health research: what is the opinion of the Canadian public? J Am Med Inform Assoc. 2007;14(6):706–12. https://doi.org/10.1197/jamia.M2457.
Willison DJ, Swinton M, Schwartz L, Abelson J, Charles C, Northrup D, et al. Alternatives to project-specific consent for access to personal information for health research: insights from a public dialogue. BMC Med Ethics. 2008;9(1):18. https://doi.org/10.1186/1472-6939-9-18.
Willison DJ, Steeves V, Charles C, Schwartz L, Ranford J, Agarwal G, et al. Consent for use of personal information for health research: do people with potentially stigmatizing health conditions and the general public differ in their opinions? BMC Med Ethics. 2009;10:10.
Woolf SH, Rothemich SF, Johnson RE, Marsland DW. Selection bias from requiring patients to give consent to examine data for health services research. Arch Fam Med. 2000;9(10):1111–8. https://doi.org/10.1001/archfami.9.10.1111.
Xafis V. The acceptability of conducting data linkage research without obtaining consent: lay people’s views and justifications. BMC Med Ethics. 2015;16(1):79. https://doi.org/10.1186/s12910-015-0070-4.
Yawn BP, Yawn RA, Geier GR, Xia Z, Jacobsen SJ. The impact of requiring patient authorization for use of data in medical records research. J Fam Pract. 1998;47(5):361–2.
Young AF, Dobson AJ, Byles JE. Health services research using linked records: who consents and what is the gain? Aust N Z J Public Health. 2001;25(5):417–20. https://doi.org/10.1111/j.1467-842X.2001.tb00284.x.
Acknowledgements
The authors would like to thank Ms. Ngaire Pettit-Young, Information First, Sydney, NSW, Australia, for her assistance in developing the search strategy.
Funding
This project was supported by the Sydney Vital, Translational Cancer Research, through a Cancer Institute NSW competitive grant. The views expressed herein are those of the authors and are not necessarily those of the Cancer Institute NSW. FB is supported in her academic role by the Friends of the Mater Foundation.
Author information
Authors and Affiliations
Contributions
EH, PB and FB were responsible for developing the study concept and the development of the protocol. EH and ML were responsible for the data extraction and data analysis. FB and PB supervised this research. All authors participated in interpreting the findings and contributed to the intellectual content of the manuscript. All authors have read and approved the manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Competing interests
EH, ML, PB and FB declare that they have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Hutchings, E., Loomes, M., Butow, P. et al. A systematic literature review of attitudes towards secondary use and sharing of health administrative and clinical trial data: a focus on consent. Syst Rev 10, 132 (2021). https://doi.org/10.1186/s13643-021-01663-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s13643-021-01663-z