Abstract
Background
Heart failure (HF) in pediatric populations is a major public health concern. It is associated with high rates of hospital admissions, disability, and mortality in high-income countries (HIC), but its burden is poorly documented in low- and middle-income countries (LMICs). We present a protocol for a systematic review and meta-analysis to summarize available data on the prevalence, incidence, etiologies, treatment, and outcomes including hospital admission and mortality and economic burden of HF in neonates, infants, children, and adolescents in LMICs.
Methods
A comprehensive search of articles published between January 01, 2000, and December 31, 2017, will be performed in PubMed/MEDLINE, EMBASE, Global Index Medicus, and Web of Science. All cross-sectional, cohort studies and case-control studies reporting on the prevalence, incidence, etiologies, treatment, prognosis, admission rates, mortality, and economic burden of HF in pediatric populations in LMICs will be included in the review. The methodological quality of included studies will be appraised accordingly. For prognosis data, the Quality in Prognosis Studies (QUIPS) tool will be used. The symmetry of funnel plot and Egger’s test will be used to identify publication bias. An overall summary estimate of prevalence/incidence of pediatric HF across studies will be obtained from study-specific estimates pooled through a random-effect model. Heterogeneity of studies will be assessed by the χ2 test on Cochrane’s Q statistic. A p value less than 0.05 will be considered significant for factors that predict mortality. This systematic review and meta-analysis will be reported following the PRISMA guidelines.
Discussion
This study will report and summarize epidemiology data, as well as the economic burden of HF in neonates, infants, children, and adolescents of LMICs. Limitations will mainly arise from the heterogeneity in the diagnostic of HF.
Systematic review registration
PROSPERO CRD42017070189.
Similar content being viewed by others
Background
Heart failure (HF) is a major threat to global public health, affecting about 26 million people worldwide [1]. Over the past decades, several cohort studies have improved our knowledge on the epidemiology of heart failure in adults. Furthermore, major advances have been done in the diagnosis and management of HF in adults, especially in developed countries. On the other hand, the global epidemiology of HF in pediatric populations remained largely unknown [2, 3]. However, it is estimated in the US that more than 14,000 hospitalizations related to pediatric HF occur annually [4], caused mainly by cardiomyopathies and congenital heart diseases (CHD). Although early operative management has improved the prognosis of CHD and prevalence of symptomatic HF to as low as 10% in some series [5], almost half of patients with cardiomyopathies develop severe and life-threatening forms of HF, necessitating cardiac transplantation [6]. Therefore, the mortality related to pediatric HF is significantly higher (more than 20 times) than in other children, reaching 7% in some studies [4]. Pediatric HF is also associated to a very high cost of care, evaluated to almost $1 billion yearly in the US, for inpatient charges only [7].
In low- and middle-income countries (LMICs), HF in adults is mainly due to hypertensive heart disease and cardiomyopathies and to a lesser degree to ischemic heart disease and valvular heart disease [8]. Available data in these countries suggest that pediatric HF is predominated by acquired and preventable causes, namely, rheumatic heart diseases (RHD), endomyocardial fibrosis, nutritional deficiencies, and other tropical diseases [9], with RHD as the first cause of cardiovascular mortality in children and young adults [10]. The main treatment option for this poverty-linked disease is surgery, especially in severe cases. Despite major advances in cardiac surgery and cardiology, most children with heart disease in LMICs are still unable to access these services, due to severely limited financial, human, and infrastructural resources [11,12,13]. Children of LMICs are therefore faced with a double burden of HF etiologies, added to a limited availability of resources for their management.
LMICs are characterized by a higher burden of infectious diseases, a situation that can modify etiological profile compared to other regions. Hence, streptococcal infections, the main etiology of RHD, are mainly found in Africa, Asia, Latin America, Middle East, and in the Pacific region [14]. In addition, health systems in LMICs are weak with limited access to quality health care. Cardiac surgery is almost inaccessible and not routinely performed in most of these countries.
Consequently, it is crucial to synthesize data on the magnitude of pediatric HF in order to adequately identify the challenges and gaps in the diagnosis and the management of this condition and then provide the adequate resources to curb the impact of HF on neonates, infants, children, and adolescents of LMICs. This systematic review and meta-analysis aims to summarize epidemiologic data on HF in neonates, infants, children, and adolescents in LMICs, including
-
The prevalence and incidence of HF
-
The etiologies of HF
-
The treatment of HF and outcomes including hospital admission and mortality
-
The economic burden of treatment of HF.
Methods
Design
This review will be conducted and reported according to the guidelines of the Centre for Reviews and Dissemination [15] and the guidelines for the Preferred Reporting Items for Systematic review and Meta-Analysis (PRISMA) [16], respectively. The present protocol conforms to the Preferred Reporting Items for Systematic review and Meta-Analysis for Protocol (PRISMA-P) [16]. An additional file shows the PRISMA for protocol checklist [see Additional file 1]. This review protocol is registered in the PROSPERO International Prospective Register of systematic reviews, registration number CRD42017070189. We do not intend to make any amendments to the protocol, to avoid the possibility of outcome reporting bias. However, amendments during the review process will be reported transparently.
Criteria for considering studies for the review
Types of studies
The types of studies included are cross-sectional, case-control, or cohort studies reporting the prevalence, incidence, factors associated with, economic burden or etiologies of HF among children in LMICs, and cohort studies reporting on incidence or predictors of mortality in this population.
Types of participants
Studies including patients aged from 0 to 20 years will be included. If it is impossible to extract data from this age group in studies with both children and adults, these studies will be excluded.
Other criteria
Our search will be focused on studies published and unpublished from January 01, 2000, to December 31, 2017. We have chosen this period because the epidemiology of a disease such as HF can markedly change over time. It is therefore important to present contemporaneous data, which can be used to inform current policies and help for contemporaneous efficient strategies. Only participants from LMICs will be included as classified by the World Bank. For the 2017 fiscal year, low-income economies are defined as those with a gross national income (GNI) per capita, calculated using the World Bank Atlas method, of $1005 or less in 2016; lower-middle-income economies are those with a GNI per capita between $1026 and $3955; and upper-middle-income economies are those with a GNI per capita between $3956 and $12,2354 [17].
Search strategy used to identify relevant studies
Databases searching
An expert librarian will perform a comprehensive and exhaustive search of Medline through PubMed, Excerpta Medica Database (EMBASE), Global Index Medicus (including the Literature in the Health Sciences in Latin America and the Caribbean–LILACS, Western Pacific Region Index Medicus–WPRIM, Index Medicus for the South-East Asian Region–IMSEAR, Index Medicus for the Eastern Mediterranean Region–IMEMR, Africa Index Medicus–AIM, WHO library database–WHOLIS), and Web of Science to identify all relevant articles published from January 01, 2000, to December 31, 2017, without any language restriction. A search strategy based on the combination of medical subheadings and keywords will be applied, after which the name of all LMICs will be included in the search strategy. The main search strategy for PubMed/Medline is shown in Table 1. This search strategy will be adapted to fit other considered databases.
Searching for other sources
Reference lists of eligible articles and relevant reviews will be manually searched to identify other potential sources of data.
Selection of included studies
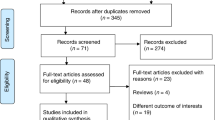
Two review authors will independently identify articles and sequentially screen their titles and abstracts for eligibility. The full texts of potentially eligible studies will be retrieved. These review authors will further independently assess the full text of each study for eligibility and consensually retain studies to be included. Disagreements, there be any, will be solved by a third review author. A screening guide will be used to ensure that all review authors reliably apply the selection criteria. Study selection will be managed using Rayyan application for systematic reviews [18]. Studies published in English and French will be included, and eligible studies in other languages will be translated using Google Translate and considered for inclusion. Otherwise, they will be listed in the Appendix. A flowchart will be used to report the study selection process.
Appraisal of the quality of included studies
Two review authors will independently assess study quality, with disagreements resolved by consensus or arbitration of a third review author. The methodological quality of included studies for prevalence/incidence estimate will be assessed using an adapted version of the risk of bias tool for prevalence studies developed by Hoy and colleagues [see Additional file 2] [19]. A score of 0–4, 5–7, and 8–10 will rate the risk of bias as high, moderate, and low, respectively.
The methodological quality of included studies for prognosis will be assessed using the Quality In Prognosis Studies (QUIPS) tool, designed for systematic reviews of prognostic studies through an international expert consensus [see Additional file 3] [20]. The QUIPS contains six domains assessing bias due to patient selection, attrition, measurement of prognostic factors, outcome measurement, confounding on statistical analysis and reporting results, and confounding on presentation. Hence, each included article will be scored with the algorithm developed by de Jonge and colleagues [21]. The items included in each of the six categories will be scored to evaluate the methodological quality of included studies. In case of low, moderate, or high risk of bias of individual studies, the risk of bias will be evaluated as of high (+), moderate (+/−), or low (−) quality. Each category will have a maximum score of 15 points, equally divided between all the items of each domain. The sum of each domain will give a total score, not exceeding 90 points. A score of < 54 and 54–71 (between 60 and 80% of maximum attainable score), and 72–90 (≥ 80% of maximum attainable score) will rate the risk of bias as high, moderate, and low, respectively.
Data extraction and management
Data extraction will be conducted by two review authors, and discrepancies will be resolved through discussion and consensus or the arbitration of a third review author. The data of interest are listed in Table 2 including the outcomes. In case of missing data, the corresponding authors will be contacted to request for the missing information. We will exclude the articles from which no relevant data will be available even after contacting the authors.
Data synthesis including assessment of heterogeneity
Data will be analyzed using R software version 3.3.3. Unadjusted prevalence and unadjusted incidence of HF and its etiologies will be recalculated based on the information of crude numerators and denominators provided by individual studies. To keep the effect of studies with extremely small or extremely large prevalence estimates on the overall estimate to a minimum, the variance of the study-specific prevalence/incidence will be stabilized with the Freeman-Tukey single arc-sine transformation before pooling the data with the random-effects meta-analysis model [22]. Heterogeneity will be evaluated by the chi-squared test on Cochrane’s Q statistic [23], which will be quantified by I2 values, assuming that I2 values of 25, 50, and 75% being the representative of low, medium, and high heterogeneity, respectively. When substantial heterogeneity will be detected (I2 > 50%), meta-regression and subgroup analyses will be performed to investigate the possible sources of heterogeneity using study characteristics, participants’ characteristics, and study methodological quality. The following subgroups will be considered: age groups (children versus adolescents), sex (female versus male), WHO regions (Africa, Americas, South-East Asia, Europe, Eastern Mediterranean, Western Pacific), and level of income (low, lower-middle, upper-middle income). Only variables significantly associated (p < 0.20) with the outcome of interest in univariable meta-regression analysis will be included in the multivariable model. Multivariable meta-regression analysis will be conducted if there are least ten studies per variable eligible for the model. We hypothesized that prevalence or incidence would increase when the level of income decreases. Sensitivity analysis including only studies with low risk of bias in their methodological quality will be performed. The symmetry of funnel plots and Egger’s test will be done to assess the presence of publication and selective reporting bias [24]. A p value < 0.10 will be considered indicative of statistically significant publication bias. The inter-rater agreement between the review authors for study inclusion and methodological quality assessment will be evaluated using Kappa Cohen’s coefficient [25]. We presume that the reporting of factors associated with HF and predictors of mortality, hospital admission, and readmission will present high reporting clinical and methodological heterogeneity. This will also be possible for other outcomes. If it is the case, we will summarize the findings in a narrative format.
Discussion
Clinicians, researchers, and policymakers need to be informed on the situation of children presenting HF in LMICs. In order to achieve this goal, this review aims at providing estimates of the prevalence, incidence of HF, and its etiologies and prognosis, as well as the cost of care of HF among the pediatric population of LMICs. To the best of our knowledge, this will be the first systematic review and meta-analysis on the topic. The main limitation would be the ascertainment of some etiologies such as idiopathic dilated cardiomyopathy or myocarditis, which requires endomyocardial biopsy rarely done in developing countries. In addition, the limited data with a predominance of hospital-based studies could alter the generalizability of the findings. Data would also be limited with high heterogeneity on diagnostic criteria for HF, especially among children.
The current study is based on data already collected from primary studies and approved by the ethics committee, and as such, requires no ethical approval. The final report of the systematic review in the form of a scientific paper will be published in a peer-reviewed journal. Findings will further be presented at conferences and submitted to relevant health authorities. We also plan to update the review in the future to monitor changes and guide health service and policy solutions.
Abbreviations
- CHD:
-
Congenital heart diseases
- HF:
-
Heart failure
- HIC:
-
High-income countries
- LMICs:
-
Low- and middle-income countries
- MOOSE:
-
Meta-Analyses and Systematic Reviews of Observational Studies
- PRISMA:
-
Preferred Reporting Items for Systematic Review and Meta-Analysis
- UK:
-
United Kingdom
- US:
-
United States
References
Ambrosy AP, Fonarow GC, Butler J, Chioncel O, Greene SJ, Vaduganathan M, et al. The global health and economic burden of hospitalizations for heart failure: lessons learned from hospitalized heart failure registries. J Am Coll Cardiol. 2014;63(12):1123–33.
Andrews RE, Fenton MJ, Ridout DA, Burch M. British congenital cardiac association. New-onset heart failure due to heart muscle disease in childhood: a prospective study in the United Kingdom and Ireland. Circulation. 2008;117(1):79–84.
Webster G, Zhang J, Rosenthal D. Comparison of the epidemiology and co-morbidities of heart failure in the pediatric and adult populations: a retrospective, cross-sectional study. BMC Cardiovasc Disord. 2006;6:23.
Rossano JW, Kim JJ, Decker JA, Price JF, Zafar F, Graves DE, et al. Prevalence, morbidity, and mortality of heart failure–related hospitalizations in children in the United States: a population-based study. J Card Fail. 2012;18(6):459–70.
Massin MM, Astadicko I, Dessy H. Epidemiology of heart failure in a tertiary pediatric center. Clin Cardiol. 2008;31(8):388–91.
Lipshultz null. Ventricular dysfunction clinical research in infants, children and adolescents. Prog Pediatr Cardiol. 2000;12(1):1–28.
Nandi D, Rossano JW. Epidemiology and cost of heart failure in children. Cardiol Young. 2015;25(8):1460–8.
Callender T, Woodward M, Roth G, Farzadfar F, Lemarie J-C, Gicquel S, et al. Heart failure care in low- and middle-income countries: a systematic review and meta-analysis. PLoS Med [Internet]. 2014 Aug 12 [cited 2017 May 28];11(8). Available from: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4130667/
Rohit M, Gupta A, Talwar KK. Heart failure in children in tropical regions. Curr Heart Fail Rep. 2013;10(4):277–84.
Carapetis JR, Steer AC, Mulholland EK, Weber M. The global burden of group A streptococcal diseases. Lancet Infect Dis. 2005;5(11):685–94.
Tchervenkov CI, Jacobs JP, Bernier P-L, Stellin G, Kurosawa H, Mavroudis C, et al. The improvement of care for paediatric and congenital cardiac disease across the world: a challenge for the World Society for Pediatric and Congenital Heart Surgery. Cardiol Young. 2008;18(Suppl 2):63–9.
Neirotti R. Paediatric cardiac surgery in less privileged parts of the world. Cardiol Young. 2004;14(3):341–6.
Pezzella AT. International cardiac surgery: a global perspective. Semin Thorac Cardiovasc Surg. 2002;14(4):298–320.
Zühlke LJ, Beaton A, Engel ME, Hugo-Hamman CT, Karthikeyan G, Katzenellenbogen JM, et al. Group A streptococcus, acute rheumatic fever and rheumatic heart disease: epidemiology and clinical considerations. Curr Treat Options Cardiovasc Med. 2017;19(2):15.
Centre for Reviews and Dissemination. CRD’s guidance for undertaking reviews in health care. 2009.
Moher D, Shamseer L, Clarke M, Ghersi D, Liberati A, Petticrew M, et al. Preferred Reporting Items for Systematic Review and Meta-Analysis Protocols (PRISMA-P) 2015 statement. Syst Rev. 2015;4:1.
WDI 2017 Maps | Data [Internet]. [cited 2017 Dec 19]. Available from: https://data.worldbank.org/products/wdi-maps
Ouzzani M, Hammady H, Fedorowicz Z, Elmagarmid A. Rayyan-a web and mobile app for systematic reviews. Syst Rev. 2016;5(1):210.
Hoy D, Brooks P, Woolf A, Blyth F, March L, Bain C, et al. Assessing risk of bias in prevalence studies: modification of an existing tool and evidence of interrater agreement. J Clin Epidemiol. 2012;65(9):934–9.
Hayden JA, van der Windt DA, Cartwright JL, Côté P, Bombardier C. Assessing bias in studies of prognostic factors. Ann Intern Med. 2013;158(4):280.
de Jonge RCJ, van Furth AM, Wassenaar M, Gemke RJBJ, Terwee CB. Predicting sequelae and death after bacterial meningitis in childhood: a systematic review of prognostic studies. BMC Infect Dis. 2010;10:232.
Barendregt JJ, Doi SA, Lee YY, Norman RE, Vos T. Meta-analysis of prevalence. J Epidemiol Community Health. 2013;67(11):974–8.
Cochran WG. The combination of estimates from different experiments. Biometrics. 1954;10(1):101–29.
Egger M, Davey Smith G, Schneider M, Minder C. Bias in meta-analysis detected by a simple, graphical test. BMJ. 1997;315(7109):629–34.
Viera AJ, Garrett JM. Understanding interobserver agreement: the kappa statistic. Fam Med. 2005;37(5):360–3.
Acknowledgements
None.
Review status
Preliminary searches
Funding
This review received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Availability of data and materials
Not applicable.
Author information
Authors and Affiliations
Contributions
ATS, JJB, and JJN contributed to the conception and design of the protocol. ATS and JJB contributed to the first draft. ATS, JJB, VNA, UFN, and JJN contributed to the critical revision of the manuscript for methodological and intellectual content. JJN is the guarantor of the review. All authors approved the final version of the manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Additional files
Additional file 1:
PRISMA-P. (DOCX 56 kb)
Additional file 2:
Risk of bias assessment tool for prevalence, incidence, and etiologies outcomes. (DOCX 13 kb)
Additional file 3:
Adapted Quality in Prognosis Studies (QUIPS) list for scoring methodological quality of prognosis studies. (DOCX 14 kb)
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated.
About this article
Cite this article
Sibetcheu, A.T., Agbor, V.N., Nyaga, U.F. et al. Epidemiology of heart failure in pediatric populations in low- and middle-income countries: a protocol for a systematic review. Syst Rev 7, 52 (2018). https://doi.org/10.1186/s13643-018-0717-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s13643-018-0717-6