Abstract
Introduction
Studies regarding coronavirus disease 2019 (COVID-19) were mainly performed in the initial wave, but some small-scale data points to prognostic differences for patients in successive waves. We therefore aimed to study the impact of time on prognosis of ICU-admitted COVID-19 patients.
Method
We performed a national retrospective cohort study, including all adult patients hospitalized in French ICUs from March 1, 2020 to June 30, 2021, and identified three surge periods. Primary and secondary outcomes were in-hospital mortality and need for invasive mechanical ventilation, respectively.
Results
105,979 critically ill ICU-admitted COVID-19 patients were allocated to the relevant three surge periods. In-hospital mortality for surges 1, 2, and 3 was, respectively, 24%, 27%, and 24%. Invasive mechanical ventilation was the highest level of respiratory support for 42%, 32%, and 31% (p < 0.001) over the whole period, with a decline in the use of vasopressors over time. Adjusted for age, sex, comorbidities, and modified Simplified Acute Physiology Score II at ICU admission, time period was associated with less invasive mechanical ventilation and a high risk of in-hospital death. Vaccination against COVID-19 was associated with a lower likelihood of invasive mechanical ventilation (adjusted sub-hazard ratio [aSHR] = 0.64 [0.53–0.76]) and intra-hospital death (aSHR = 0.80, [0.68–0.95]).
Conclusion
In this large database of ICU patients admitted for COVID-19, we observed a decline in invasive mechanical ventilation, vasopressors, and RRT use over time but a high risk of in-hospital death. Vaccination was identified as protective against the risk of invasive mechanical ventilation and in-hospital death.
Similar content being viewed by others
Introduction
In December 2019, a widespread outbreak of acute respiratory illness—which was due to SARS-CoV-2, a novel coronavirus—emerged from China [1, 2]. The disease, named coronavirus disease 2019 (COVID-19), rapidly spread to over 200 countries worldwide and was officially declared a pandemic by the World Health Organization (WHO) in March 2020 [3]. As of February 2022, more than 130,000 deaths related to COVID-19 have been reported in France [4]. The outbreak caused an unprecedented number of severe cases and intense demand for hospital admissions, especially in intensive care units (ICUs) [3, 5].
The overall pattern of the disease so far has been a series of COVID-19 surges [6]. Although several studies have described the characteristics and the management of COVID-19 patients admitted to an ICU during the first surge of the pandemic [7,8,9], information regarding the evolution of patients’ characteristics and management over time (i.e., during subsequent surges) is still limited [6, 10]. A decline in the rate of invasive mechanical ventilation use, as well as a rise in in-hospital mortality, was reported in USA between March 2020 and January 2021 [6]. Further studies are still needed to describe trends in ICU care and mortality related to COVID-19.
Using the large French administrative health care database, we aimed to describe the characteristics and the outcomes over time of COVID-19 related critically ill patients. Our primary goal was to compare the characteristics, management, and outcome of patients in French ICUs between the different surges of the pandemic. In addition, we evaluated whether a surge was associated with invasive ventilation and mortality in this population. Finally, we sought to evaluate to what extent vaccination against SARS-CoV-2 could be linked to a decrease in invasive mechanical ventilation and mortality rate.
Patients and methods
Study design and participants
This retrospective cohort study used information from the French administrative health care database (Système National des Données de Santé [SNDS]). The SNDS contains data on outpatient care (medical consultation, paramedical interventions, and reimbursed drug dispensation) as well as data from the French hospital discharge database [programme de médicalisation des systems d’informations (PMSI)] collected during hospital stay (admission date, duration, ICD-10 codes for main and associated diagnosis, and medical interventions) [11]. All these data are linked through a unique personal identification number.
We included all adult patients (≥ 18 years old) hospitalized in French ICUs from March 1, 2020 to June 30, 2021, for whom a complete hospital course was available and who had at least one ICD-10 diagnosis code for COVID-19. The complete list of ICD-10 diagnosis codes used to identify patients is provided in Additional file 2: Appendix S1.
Patients with COVID-19 were classified into three groups according to the surges during which they were admitted to the ICU (Additional file 1: Fig. S1) [12]. The first surge occurred between March 1 and June 30, 2020, the second between July 1 and December 31, 2020, and the third from January 1 to June 30, 2021.
Variables
Age, sex, and Simplified Acute Physiology Score (SAPS) II score [13] at admission were collected for each in-patient stay. We recomposed the Charlson Comorbidity Index [14] based on all ICD-10 diagnoses collected. A number of comorbidities were also collected, namely, arterial hypertension, diabetes mellitus, heart disease, chronic lung disease, cirrhosis, cancer, hematological malignancies, chronic kidney disease, and immunocompromised status. Immunocompromised patients were defined as patients with agranulocytosis, medullar aplasia, immunodeficiency, cancer treated by chemotherapy, or solid organ transplants (ICD-10 diagnosis codes are available in Additional file 2: Appendix S1).
We identified oxygenation and ventilation procedures recorded during hospitalization (according to the French Common Classification of Medical Procedures [CCAM] [15]): invasive mechanical ventilation, non-invasive mechanical ventilation, and high-flow nasal cannula (HFNC) therapy. Patients were classified according to their maximal level of ventilation which was invasive mechanical ventilation followed by non-invasive mechanical ventilation and HFNC therapy. We also identified patients who required prone positioning as well as those who were placed on extracorporeal membrane oxygenation. The list of CCAM codes is available in Additional file 2: Appendix S2. For those requiring invasive mechanical ventilation, time between ICU admission and tracheal intubation was collected.
We used ICD-10 diagnoses to identify complications that occurred during the hospital stay, such as shock-requiring vasopressors, renal replacement therapy (RRT), venous thrombosis events including pulmonary embolism, acute liver failure, and disseminated intravascular coagulation.
Patient outcomes included mechanical ventilation duration, ICU, hospital length of stay (LOS), and vital status at hospital discharge.
For patients admitted after January 1, 2021, we collected vaccination status. A full vaccination scheme was defined as more than 28 days after a single dose of Ad26.COV2-S vaccine (COVID-19 Vaccine Janssen®) or more than 7 days after the second dose of vaccine other than Ad26.COV2-S vaccine. A partial vaccination was defined as fewer than 28 days after a single dose of Ad26.COV2-S vaccine or fewer than 7 days after the second and/or after the first dose of vaccine other than Ad26.COV2-S. Patients were considered non-vaccinated if they did not receive any dose of any vaccine against COVID-19.
Ethics consideration
The SNDS database was created by French law no. 2016-41 dated 26 January 2016 [16]. The purpose of the database is researched through the reuse of claim data gathered after names and social security numbers have been removed. Condition of use and security applying to the database is defined by French government regulation dated 22 March 2017 [17]. As part of its public statistics missions, the Department for Research, Studies, Assessment, and Statistics (DREES) of the French Ministry of Health has permanent access to the SNDS database. An Internet page informs the public about the reuse of the database and their rights according to the European General Data Protection Regulation no. UE 2016/679 dated 27 April 2016 [18].
Statistical analysis
Characteristics of patients were described as frequencies and percentages for categorical variables and as medians and interquartile ranges (IQRs) for continuous variables. Chi-square test, analysis of variance univariate regression, and logistic univariate regression were used, as appropriate, to compare characteristics of different outbreaks among COVID-19 patients. In all patients of our study, we found 13% of missing values on SAPS II score. We decided not to impute missing data, because we assume that missing data were not at random, and complete case analysis, considering the large number of patients, did not involve a significant change in the confidence intervals of our estimations.
Risk factors of mechanical ventilation were identified through a competing risk framework (i.e., the Fine-Gray model) with ICU discharge alive or death in the ICU without intubation as competing events [19, 20]. The strength of the association between a specific risk factor and the event of interest in the Fine and Gray model is reflected by the sub-hazard ratio (SHR), which is the ratio of hazards associated with the cumulative incidence function in the presence and absence of the risk factor. We first computed SHR for invasive mechanical ventilation and 95% confidence intervals (CIs) associated with each of the risk factors in univariate analysis. Then, we performed a multivariate analysis to adjust for the following predefined potential confounding factors: age, sex, arterial hypertension, diabetes mellitus, heart disease, chronic lung disease, cirrhosis, cancer, hematological malignancies, chronic kidney disease, immunosuppression, and modified SAPS II score. The modified SAPS II score corresponds to SAPS II score without the points related to age. This modification allow us to include both modified SAPS II score and age in the model. Modified SAPS II score was divided into four categories corresponding to the quartiles. No selection covariate procedure was used, because the high number of events limited the risk of overfitting. Proportional hazard assumption was verified with test based on the scaled Schoenfeld residuals.
In the same way, we assessed the association between surge and in-hospital mortality (considering that being discharged alive is a competing risk). To assess the effect of vaccine status, sensitivity analyses were performed in the subgroups of patients admitted after January 1, 2021.
A P value < 0.05 was considered significant. Analyses were computed using the SAS 2017 software (SAS Institute, Cary, NC, USA).
Results
Patients’ characteristics
During the study period, 105,979 patients critically ill with COVID-19 were admitted to the ICU of 662 hospitals in France: 25,150 (24%), 32,689 (31%), and 48,140 (45%) during the first, second, and third surges, respectively. The majority (n = 67,951, 64%) were men and 30% (n = 32,044) were younger than 60 years of age. The median SAPS II score was 32 (24–41) (Table 1). Compared with the first surge, patients from the second surge were older (70 [60–78] vs 66 [56–76] years old, p < 0.001). Patients from the second and third surges had fewer comorbidities, resulting in a lower Charlson comorbidity index (62% and 73% vs 58% of Charlson comorbidity index equal to 0, p < 0.001).
ICU management and complications according to surge
Invasive mechanical ventilation, non-invasive mechanical ventilation, and HFNC therapy were the maximal level of respiratory support for 34% (n = 36,185), 6% (n = 6749), and 18% (n = 19,024) of these COVID-19 patients, respectively (Table 1). The median (IQR) duration of invasive mechanical ventilation was 13 [6–26] days for survivors and 14 [6–26] days for non-survivors.
Prone position and extracorporeal membrane oxygenation were used in 20,231 (19%) and 1125 (1%) patients, corresponding to 56% and 3% of all patients treated with invasive mechanical ventilation, respectively.
Vasopressors were administrated to 27% (n = 28,943) of patients (Table 1). RRT was used in 7% (n = 7358) of patients. Pulmonary embolism was diagnosed in 8% (n = 7981) of patients: 9% during the first surge vs 7% during the second and third surges. During the first surge, vasopressor use, as well as acute kidney injury requiring RRT, were more frequent than during the second and third surges (Table 1).
During the first surge, invasive mechanical ventilation was more frequent than during the second and third surges (42% vs 32% vs 31%, respectively, p < 0.001). The third surge was marked by a three-times highest use of HFNC therapy compared to the first surge (7%, vs 19% vs 23%, p < 0.001) (Table 1). Among patients with invasive mechanical ventilation, prone position was more frequent during the third surge (58% vs 54% during the first and second surges, p < 0.001).
Among patients with COVID-19, the median ICU LOS was 7 [3–16] days and the median hospital LOS was 14 [8–24] days. Of those with invasive mechanical ventilation, ICU LOS was 20 [11–36] days for survivors and 17 [8–36] days for those who did not survive. Of those without invasive mechanical ventilation, ICU LOS was 5 [2–9] and 4 [2–9] days for survivors and non-survivors, respectively.
Risk factors of invasive mechanical ventilation
A Fine-Gray model revealed that second (adjusted SHR (aSHR) = 0.64 [0.62–0.66]) and third (aSHR = 0.62 [0.61–0.64]) surges were associated with lower risk of invasive mechanical ventilation. The other risk factors of invasive mechanical ventilation were male sex, arterial hypertension, and increased modified SAPS II. Increased age, heart disease, cirrhosis, cancer, hematological malignancies, chronic kidney disease, and immunosuppression were associated with lower risk of invasive mechanical ventilation. Conversely, these covariates were strongly associated with the competing event of death without invasive mechanical ventilation. Table 2 shows the results of this analysis.
ICU death outcomes
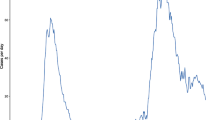
Overall, in-hospital mortality of COVID-19 patients was 25% (n = 26,407): 24% (n = 6055), 27% (n = 8698), and 24% (n = 11,654) during the first, second, and third surges, respectively. Among subgroups of patients who required invasive mechanical ventilation, in-hospital mortality was 40% (n = 14,516): 35% (n = 3789), 44% (n = 4576), and 41% (n = 6151) during the first, second, and third surges, respectively. The age-specific mortality rate for each COVID-19 surge is shown in Fig. 1. For patients younger than 70, mortality rates were higher during the first surge than in the second and third surges, whereas for those older than 70, the mortality rate during the third surge was higher.
In-hospital mortality by age during each surge of COVID-19. Blue, orange, and gray lines represent age-related mortality rate during the first, second, and third surges, respectively. The mortality rate was higher in people under 70 in the first wave than in the second and third waves. Conversely, the mortality rate increased from wave to wave in patients aged 70 and over
Competing risk survival analysis revealed that the third surge was associated with a higher risk of in-hospital mortality (Fig. 2A). Other independent risk factors were increasing age, male sex, diabetes mellitus, chronic lung disease, cirrhosis, cancer, hematological malignancies, immunocompromised status, and increasing modified SAPS II score. Conversely, arterial hypertension was associated with a lower risk of in-hospital mortality (Fig. 2A, Additional file 1: Table S1).
Association between vaccination status and mechanical ventilation and outcome
Of the 48,140 patients of the third surge, 670 (1%) and 4301 (8%) had received a complete or partial vaccination. Characteristics of patients of the third surge, according to their vaccination status, are reported in Additional file 1: Table S2. Invasive mechanical ventilation was less frequent in patients who had completed vaccination programs (19%, n = 124) compared to those who had been partially (29%, n = 1041) or not vaccinated (32%, n = 13,975 (p < 0.001). Among patients treated with invasive mechanical ventilation, the duration of mechanical ventilation was shorter in patients with complete vaccination programs (9 [3–14] days) than in those who had only been partially vaccinated (12 [5–23] days) or who were not vaccinated (13 [6–25] days) (p < 0.001).
Notably, the Fine–Gray model revealed that full vaccination against SARS-CoV-2 was associated with a lower risk of invasive mechanical ventilation (aSHR = 0.64 [0.53–0.76]), lower risk of in-hospital death (aSHR = 0.80 [0.68–0.95]), and higher risk of discharge alive from the ICU without invasive ventilation (aSHR = 1.32 [1.17–1.49]) (Fig. 2B, Additional file 1: Table S3). Even though incomplete vaccination was not associated with in-hospital death, we observed a significant association with the use of invasive mechanical ventilation (aSHR = 0.93 [0.87–0.99]) and being discharged alive without ventilation (aSHR = 1.08 [1.03–1.14]) (Additional file 1: Table S4).
Discussion
Of the 105,979 COVID-19 patients admitted to an ICU in France between March 2020 and June 2021, we found a reduction in invasive mechanical ventilation, vasopressors, and RRT use over time. However, after adjustment for confounders such as age, sex, comorbidities, and modified SAPS II, the likelihood of in-hospital death was higher during the third surge compared with the first one. Finally, we confirmed that vaccination was associated with a lower risk of invasive mechanical ventilation treatment and in-hospital death.
During the first surge, invasive mechanical ventilation was more frequent (42%) than during the second (32%) and third surges (31%), where HFNC therapy was more than three times more frequent. This decline in invasive mechanical ventilation use was consistent with findings from a previous study [6]. These differences might be explained by increased experience of COVID-19 management and the evolution of the characteristics of patients admitted to the ICU (especially, an older age during the second surge). In addition, at the beginning of the pandemic, the use of invasive mechanical ventilation was quickly adopted, because non-invasive ventilation or HFNC therapy was considered to put caregivers at a heightened risk of aerosolization [21, 22]. These concerns were assuaged by recent findings showing the clinical benefits of HFNC, as well as its relative safety for caregivers [23, 24]. However, the usefulness of non-invasive ventilation is still a matter of debate [24]. Thus, between the first and the second surge in France, French recommendations regarding the management of COVID-19 patients were modified by advocating corticosteroids and non-invasive ventilation support [25].
Using the first surge as a reference and after adjusting for age, comorbidities, and severity at ICU admission, the Fine and Gray model confirmed that the third surge was still strongly associated with a poorer outcome. In France, during the third surge, alpha (lineage B.1.1.7) was the predominant variant of concern. This has been associated with higher mortality in other countries [26, 27]. The other hypothesis possibly incriminated in the poorer outcome of the third surge related to the excess of strain in ICUs [28]. Although no statistic was available concerning the excess of work observed in ICUs, the peak of patients hospitalized in ICU in France were 17.893, 17.800, and 18.474, respectively, during surge 1, 2, and 3. If these peaks were not different according the first two surges, the higher number of patients admitted in ICU during the third surge may have been accompanied by a higher strain in these units. Consistent with the literature [29,30,31,32,33], we identified that age, male sex, comorbidities, and high SAPS II score at ICU admission are risk factors for poor outcomes. However, besides vital status signs, competing risk analysis highlighted that older age and several comorbidities, such as cirrhosis, cancer, chronic kidney disease, and immunosuppression, were associated with a lower risk of mechanical ventilation. However, caution is required so as not to misinterpret these results, since they are directly associated with the decision to withhold life-sustaining therapy in the frailest patients, as illustrated by the strong association of these same comorbidities with death without mechanical ventilation.
Because an active vaccination campaign began in France in December 2020, we could observe the impact of vaccination on outcomes during the third surge. Compared to non-vaccinated patients, vaccination against SARS-Cov-2 was associated with a lower likelihood of invasive mechanical ventilation, in-hospital death, and a higher risk of being discharged alive without ventilation. These results are consistent with another study [34] including 1197 patients hospitalized for COVID-19, which reported that death or invasive mechanical ventilation by day 28 was associated with a decreased likelihood of vaccination (12.0% vs 24.7%; aOR, 0.33; 95% CI 0.19–0.58). Our results reinforce the positive impact of vaccination on severity, even when vaccinated patients have been infected.
To the best of our knowledge, this study is the largest focus on critically ill patients in this context. Moreover, we were able to analyze patients admitted after the beginning of the vaccine campaign which allowed us to assess the effect of vaccination on ICU outcomes. However, our study has some limitations. First, due to the retrospective design, we could not confirm the causality of the associations we observed. However, the high number of patients included in our study limit the bias of overfitting. Second, biological information during the ICU stay is not collected in the SNDS, in which case, arterial blood gas could have been used as a surrogate for respiratory failure severity, whereas SAPS II expressed overall severity, including the respiratory component. Third, information concerning the treatment used in the ICU (such as corticosteroids, anticoagulants, and antivirals or the withholding of life-sustaining therapy) was not collected in the SNDS. Indeed, between the first surge and the others, expert recommendations were published advocating the use of corticosteroids and anticoagulants in critically ill patients with COVID-19 [25]. Unfortunately, the information was not available in our study and we therefore cannot assess the impact of these treatments on the prognosis of patients. Fourth, information about the variant of concern identified for each COVID case was not routinely recorded at the time of the pandemic. Finally, if the peak of ICU hospitalization was available, these data are too limited to be approach as a reliable proxy of excess of strain in ICU for two major reasons. First, COVID-19 pandemic has particularly involved medical and paramedical staff, accompanied by an excess of professional burnout and a possible decrease in the medical and nursing professional workforce [35]. Unfortunately, statistics describing available caregivers over time are not available. Second, the peak of ICU hospitalization is a national level information, and the intensity of the COVID-19 pandemic was not homogeneous in the whole territory.
Conclusion
From a population-based study involving 105,979 COVID-19 patients admitted to an ICU between March 2020 and July 2021, we reported a decline in invasive mechanical ventilation, vasopressors, and RRT use over time. We also found a rise in the risk of in-hospital mortality during the third compared with the first surge. Finally, vaccination was associated with a lower risk of invasive mechanical ventilation and in-hospital death.
Availability of data and materials
The data that support the findings of this study are available from the Department for Research, Studies, Assessment, and Statistics (DREES) of the French Ministry of Health, but restrictions apply to the availability of these data and so are not publicly available.
Change history
19 March 2023
A Correction to this paper has been published: https://doi.org/10.1186/s13613-023-01111-2
References
Lei Z, Cao H, Jie Y, Huang Z, Guo X, Chen J, et al. A cross-sectional comparison of epidemiological and clinical features of patients with coronavirus disease (COVID-19) in Wuhan and outside Wuhan. China Travel Med Infect Dis. 2020;35: 101664.
Zhu N, Zhang D, Wang W, Li X, Yang B, Song J, et al. A novel coronavirus from patients with pneumonia in China, 2019. N Engl J Med. 2020;382(8):727–33.
Aziz S, Arabi YM, Alhazzani W, Evans L, Citerio G, Fischkoff K, et al. Managing ICU surge during the COVID-19 crisis: rapid guidelines. Intensive Care Med. 2020;46(7):1303–25.
Coronavirus : chiffres clés et évolution de la COVID-19 en France et dans le Monde. https://www.santepubliquefrance.fr/dossiers/coronavirus-covid-19/coronavirus-chiffres-cles-et-evolution-de-la-covid-19-en-france-et-dans-le-monde. Accessed 23 Feb 2022.
Arabi YM, Murthy S, Webb S. COVID-19: a novel coronavirus and a novel challenge for critical care. Intensive Care Med. 2020;46(5):833–6.
Auld SC, Harrington KRV, Adelman MW, Robichaux CJ, Overton EC, Caridi-Scheible M, et al. Trends in ICU mortality from coronavirus disease 2019: a tale of three surges. Crit Care Med. 2022;50(2):245–55.
COVID-ICU Group on behalf of the REVA Network and the COVID-ICU Investigators. Clinical characteristics and day-90 outcomes of 4244 critically ill adults with COVID-19: a prospective cohort study. Intensive Care Med. 2021;47(1):60–73.
Grasselli G, Zangrillo A, Zanella A, Antonelli M, Cabrini L, Castelli A, et al. Baseline characteristics and outcomes of 1591 patients infected with SARS-CoV-2 admitted to ICUs of the Lombardy region, Italy. JAMA. 2020;323(16):1574–81.
Cummings MJ, Baldwin MR, Abrams D, Jacobson SD, Meyer BJ, Balough EM, et al. Epidemiology, clinical course, and outcomes of critically ill adults with COVID-19 in New York City: a prospective cohort study. Lancet Lond Engl. 2020;395(10239):1763–70.
Auld SC, Caridi-Scheible M, Robichaux C, Coopersmith CM, Murphy DJ. Declines in mortality over time for critically ill adults with COVID-19. Crit Care Med. 2020;48(12):e1382–4.
Scailteux LM, Droitcourt C, Balusson F, Nowak E, Kerbrat S, Dupuy A, et al. French administrative health care database (SNDS): the value of its enrichment. Therapie. 2019;74(2):215–23.
Costemalle V, Gaini M, Hazo JB, Naouri D. En quatre vagues, l’épidémie de COVID-19 a causé 116 000 décès et lourdement affecté le système de soins. 2021. https://www.insee.fr/fr/statistiques/5432509?sommaire=5435421. Accessed 10 Jan 2023.
Le Gall JR, Lemeshow S, Saulnier F. A new simplified acute physiology score (SAPS II) based on a European/North American multicenter study. JAMA. 1993;270(24):2957–63.
Quan H, Sundararajan V, Halfon P, Fong A, Burnand B, Luthi JC, et al. Coding algorithms for defining comorbidities in ICD-9-CM and ICD-10 administrative data. Med Care. 2005;43(11):1130–9.
Bousquet C, Trombert B, Souvignet J, Sadou E, Rodrigues JM. Evaluation of the CCAM hierarchy and semi structured code for retrieving relevant procedures in a hospital case mix database. AMIA Annu Symp Proc. 2010;2010:61–5.
LOI no. 2016–41 du 26 janvier 2016 de modernisation de notre système de santé (1). 2016–41 janv 26, 2016.
Arrêté du 22 mars 2017 relatif au référentiel de sécurité applicable au Système national des données de santé.
Le règlement général sur la protection des données—RGPD | CNIL. https://www.cnil.fr/fr/reglement-europeen-protection-donnees. Accessed 14 Mar 2022.
Andersen PK, Abildstrom SZ, Rosthøj S. Competing risks as a multi-state model. Stat Methods Med Res. 2002;11(2):203–15.
Pepe MS, Mori M. Kaplan–Meier, marginal or conditional probability curves in summarizing competing risks failure time data? Stat Med. 1993;12(8):737–51.
Schünemann HJ, Khabsa J, Solo K, Khamis AM, Brignardello-Petersen R, El-Harakeh A, et al. Ventilation techniques and risk for transmission of coronavirus disease, including COVID-19. Ann Intern Med. 2020. https://doi.org/10.7326/M20-2306.
Raoof S, Nava S, Carpati C, Hill NS. High-flow, noninvasive ventilation and awake (nonintubation) proning in patients with coronavirus disease 2019 with respiratory failure. Chest. 2020;158(5):1992–2002.
Agarwal A, Basmaji J, Muttalib F, Granton D, Chaudhuri D, Chetan D, et al. High-flow nasal cannula for acute hypoxemic respiratory failure in patients with COVID-19: systematic reviews of effectiveness and its risks of aerosolization, dispersion, and infection transmission. Can J Anaesth. 2020. https://doi.org/10.1007/s12630-020-01740-2.
COVID-ICU group, for the REVA network, COVID-ICU investigators. Benefits and risks of noninvasive oxygenation strategy in COVID-19: a multicenter, prospective cohort study (COVID-ICU) in 137 hospitals. Crit Care Lond Engl. 2021;25(1):421.
SRLF-SFAR-GFRUP-SPILF-SPLF-SFMU. Recommandations d’experts portant sur la prise en charge en réanimation des patients infectés à SARS-CoV2. 2020. https://www.srlf.org/wp-content/uploads/2020/11/RFE-COVID_V5_VDef.pdf. Accessed 10 Jan 2023.
Patone M, Thomas K, Hatch R, Tan PS, Coupland C, Liao W, et al. Mortality and critical care unit admission associated with the SARS-CoV-2 lineage B.1.1.7 in England: an observational cohort study. Lancet Infect Dis. 2021;21(11):1518–28.
Challen R, Brooks-Pollock E, Read JM, Dyson L, Tsaneva-Atanasova K, Danon L. Risk of mortality in patients infected with SARS-CoV-2 variant of concern 202012/1: matched cohort study. BMJ. 2021;372: n579.
Wilcox ME, Rowan KM, Harrison DA, Doidge JC. Does unprecedented ICU capacity strain, as experienced during the COVID-19 pandemic, impact patient outcome? Crit Care Med. 2022;50(6):e548–56.
Pijls BG, Jolani S, Atherley A, Derckx RT, Dijkstra JIR, Franssen GHL, et al. Demographic risk factors for COVID-19 infection, severity, ICU admission and death: a meta-analysis of 59 studies. BMJ Open. 2021;11(1): e044640.
Grasselli G, Greco M, Zanella A, Albano G, Antonelli M, Bellani G, et al. Risk factors associated with mortality among patients with COVID-19 in intensive care units in Lombardy, Italy. JAMA Intern Med. 2020;180(10):1345–55.
Kim L, Garg S, O’Halloran A, Whitaker M, Pham H, Anderson EJ, et al. Risk Factors for intensive care unit admission and in-hospital mortality among hospitalized adults identified through the US coronavirus disease 2019 (COVID-19)-associated hospitalization surveillance network (COVID-NET). Clin Infect Dis Off Publ Infect Dis Soc Am. 2021;72(9):e206–14.
Haase N, Plovsing R, Christensen S, Poulsen LM, Brøchner AC, Rasmussen BS, et al. Characteristics, interventions, and longer term outcomes of COVID-19 ICU patients in Denmark—a nationwide, observational study. Acta Anaesthesiol Scand. 2021;65(1):68–75.
Karagiannidis C, Mostert C, Hentschker C, Voshaar T, Malzahn J, Schillinger G, et al. Case characteristics, resource use, and outcomes of 10 021 patients with COVID-19 admitted to 920 German hospitals: an observational study. Lancet Respir Med. 2020;8(9):853–62.
Tenforde MW, Self WH, Adams K, Gaglani M, Ginde AA, McNeal T, et al. Association between mRNA vaccination and COVID-19 hospitalization and disease severity. JAMA. 2021;326(20):2043–54.
Azoulay E, Cariou A, Bruneel F, Demoule A, Kouatchet A, Reuter D, et al. Symptoms of anxiety, depression, and peritraumatic dissociation in critical care clinicians managing patients with COVID-19. A cross-sectional study. Am J Respir Crit Care Med. 2020;202(10):1388–98.
Acknowledgements
We would like to thank Vianney Costemalle, Philippe Raynaud, and Benoit Ourliac for their proofreading.
Funding
There was no funding for this study.
Author information
Authors and Affiliations
Contributions
DN designed the study, collected the data, performed statistical analysis, interpreted the results, and wrote the manuscript. MJ designed the study and wrote the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
The SNDS database was created by French law no. 2016-41 dated 26 January 2016 [16]. The purpose of the database is research through the reuse of claim data gathered after names and social security numbers have been removed. Condition of use and security applying to the database is defined by French government regulation dated 22 March 2017 [17]. As part of its public statistics missions, the Department for Research, Studies, Assessment, and Statistics (DREES) of the French Ministry of Health has permanent access to the SNDS database.
Consent for publication
According to French law, written informed consent was not required for this type of study. An Internet page informs the public about the reuse of the database and their rights according to the European General Data Protection Regulation no. UE 2016/679 dated 27 April 2016 [18].
Competing interests
Matthieu Schmidt reports lecture fees from Getinge, Drager, and Xenios outside the submitted work. Alain Combes reports grants from Getinge, and personal fees from Getinge, Baxter, and Xenios outside the submitted work. All other authors report no competing interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this article was revised: The figure 2 which was incorrectly published in the original article has been corrected.
Supplementary Information
Additional file 1: Table S1.
Association between surge and in-hospital death. Table S2. Characteristics of patients of the third surge according to their vaccination status. Table S3. Association between vaccination status and the use of invasive mechanical ventilation. Table S4. Association between vaccination and in-hospital mortality. Figure S1. Admission of patients with COVID-19 in ICU between March 2020 and July 2021. Figure S2. Cumulative incidence curve of invasive mechanical ventilation (A) and discharge alive without invasive mechanical ventilation (B) according to vaccine status.
Additional file 2: Appendix S1.
List of ICD-10 diagnosis codes used. Appendix S2. List of CCAM codes used.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Naouri, D., Vuagnat, A., Beduneau, G. et al. Trends in clinical characteristics and outcomes of all critically ill COVID-19 adult patients hospitalized in France between March 2020 and June 2021: a national database study. Ann. Intensive Care 13, 2 (2023). https://doi.org/10.1186/s13613-022-01097-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s13613-022-01097-3