Abstract
Background
Transfers from one intensive care unit (ICU) to another ICU are associated with increased length of intensive care and hospital stay. Inter-hospital ICU transfers are carried out for three main reasons: clinical transfers, capacity transfers and repatriations. The aim of the study was to show that different ICU transfers differ in risk-adjusted mortality rate with repatriations having the least risk.
Results
Observational cohort study of adult patients transferred between Swedish ICUs during 3 years (2016–2018) with follow-up ending September 2019. Primary and secondary end-points were survival to 30 days and 180 days after discharge from the first ICU. Data from 75 ICUs in the Swedish Intensive Care Register, a nationwide intensive care register, were used for analysis (89% of all Swedish ICUs), covering local community hospitals, district general hospitals and tertiary care hospitals. We included adult patients (16 years or older) admitted to ICU and subsequently discharged by transfer to another ICU. Only the first admission was used. Exposure was discharge to any other ICU (ICU-to-ICU transfer), whether in the same or in another hospital. Transfers were grouped into three predefined categories: clinical transfer, capacity transfer, and repatriation. We identified 15,588 transfers among 112,860 admissions (14.8%) and analysed 11,176 after excluding 4112 repeat transfer of the same individual and 300 with missing risk adjustment. The majority were clinical transfers (62.7%), followed by repatriations (21.5%) and capacity transfers (15.8%). Unadjusted 30-day mortality was 25.0% among capacity transfers compared to 14.5% and 16.2% for clinical transfers and repatriations, respectively. Adjusted odds ratio (OR) for 30-day mortality were 1.25 (95% CI 1.06–1.49 p = 0.01) for capacity transfers and 1.17 (95% CI 1.02–1.36 p = 0.03) for clinical transfers using repatriation as reference. The differences remained 180 days post-discharge.
Conclusions
There was a large proportion of ICU-to-ICU transfers and an increased odds of dying for those transferred due to other reasons than repatriation.
Similar content being viewed by others
Background
Intensive care beds are expensive and limited. The need for beds varies over time, and sometimes all beds are occupied, particularly on intensive care units (ICUs) where a high proportion of admissions are acute. When a critically ill patient needs admitting to a full ICU, the usual procedure is to either delay admission or create a temporary bedspace for a short period, while trying to free an intensive care bed by discharging another patient urgently to a general ward or to another ICU. This strategy comes at a cost since, firstly, premature discharge to a general ward may be associated with increased mortality [1] and, secondly, transfer to another ICU (ICU-to-ICU transfer) appears to be associated with increased total duration of intensive care and hospital stay, although unclear whether this is associated with increased mortality [2, 3].
Studies on ICU-to-ICU transfer are problematic since transfers are carried out for three main reasons that must be considered separately in the analyses. First, patients are transferred when there is need for specialised care that is not available in the admitting hospital (clinical transfer). Second, ICU patients are transferred to their home ICU after having undergone initial treatment at another unit (repatriation). Third, patients are transferred to make room for patients with more urgent need for intensive care when all ICU beds are occupied (capacity transfer). Furthermore, follow-up of transferred patients should preferably be carried out after discharge from ICU or hospital to capture important long-term effects on survival.
The present study is based on data from a large nationwide intensive care register, the Swedish Intensive Care Register (SIR), which registers the three principal reasons for transfer as well as long-term follow-up data. Our aim was to compare mortality between the three classes of ICU-to-ICU transfers with the assumption that mortality was lowest among repatriations.
Methods
This was an observational cohort study on patients admitted to Swedish intensive care units (ICUs) from Jan 1st, 2016 to Dec 31st, 2018. Follow-up ended Sept 30th, 2019.
Setting and participants
We used the Swedish Intensive Care Register (SIR) to identify eligible patients (see below). SIR is a national quality register which collects data from intensive care admissions in Sweden. Admissions to a few non-affiliated and paediatric ICUs were not included, leaving data from 75 ICUs for analysis (89% of all Swedish ICUs). The ICUs were located in local community hospitals (25 ICUs), district general hospitals (24 ICUs) and tertiary care hospitals (26 ICUs).
We included patients (16 years or older) admitted to ICU and subsequently discharged by transfer to another ICU. For patients with multiple admissions during the study period, we included the first admission only using the Swedish personal identity number for identification [4]. We excluded patients missing to follow-up (i.e. non-Swedes and a few individuals with concealed identity number, n = 714) or missing SAPS3 risk-adjustment data (n = 300 in 4 ICUs).
Variables and definitions
The primary end-point, survival 30 days after discharge from the first ICU, and the secondary end-point, survival 180 days after discharge from the first ICU, were both determined by linking SIR to the Swedish Population Register.
Exposure was discharge to any other ICU (ICU-to-ICU transfer), whether in the same or in another hospital. Transfers are grouped by participating ICUs in three categories according to SIR guidelines: clinical transfer, capacity transfer, and repatriation. Clinical transfer is when the patient is transferred for specialised treatment or investigations not provided in the referring ICU. Capacity transfer is when a patient is transferred to make room for another patient with more urgent need for intensive care when all ICU beds are occupied. Repatriation is when a patient is transferred from the referring ICU to another ICU closer to the patient’s home.
Patient age, gender and admission and discharge times were retrieved from SIR which was the principal data source. The duration of ICU stay was calculated, as well as identification of discharges at night and during weekends. Night-time was defined as 10.00 PM to 6.59 AM and weekend as Saturday 0.00 AM to Sunday 23.59 PM [5]. We used the Simplified Acute Physiology Score (SAPS) 3 model to score chronic comorbidities and circumstances prior to admission, and reasons for admission and physiologic derangements on admission to ICU [6]. The score was subdivided into the original three boxes where Box 1 included comorbidities and time in hospital before ICU (age was deducted from Box1), Box 2 included circumstances on admission, and Box 3 included reasons for admission and physiological derangements on admission. Organ failure at discharge was calculated according to the Sequential Organ Failure Assessment (SOFA) score [7]. The score was based on clinical examination before discharge and blood samples obtained on the day of discharge. Missing individual organ scores were presumed normal (0 points). One primary and multiple secondary disease diagnoses were recorded by the attending physician at discharge from ICU according to SIR guidelines. In our analyses we used the primary diagnosis only. The International Classification of Diseases version 10 (ICD-10) was used to group patients into six principal disease groups (see Additional file 1: Table S1).
Data were recorded in raw format by each ICU and after local validation transferred to SIR for central validation (required data were present, entries were within prespecified limits, and inconsistencies and illogical entries were identified). If necessary, data were returned for correction and revalidation before being accepted and entered into the master database. In addition to a required comprehensive data set, SIR has a number of optional data sets, including SAPS3 and SOFA, which were used in the present study. While the SAPS3 set was used in all but a few ICUs (300 admissions in 4 ICUs had missing SAPS3 data), SOFA was used in 22 ICUs only. We used admissions from 75 ICUs with SAPS3 data and 22 ICUs with SAPS3 data and SOFA scores at discharge in our risk-adjusted analyses.
Calculations and statistical methods
Descriptive data are presented as mean (95% confidence intervals, CI) or median (interquartile range, IQR) values and proportions (95% CI) as appropriate. Differences in crude survival were examined using the Kaplan–Meier estimate and the log-rank test.
The association between category of transfer and survival was analysed using univariable and two-level multivariable logistic regression models. The two-level approach was used to model intra-cluster correlation with ICUs treated as a random factor. The primary multivariable model was adjusted for age, gender, comorbidity, reasons for admission, circumstances and physiological derangements on admission as recorded in the SAPS3 model, duration of ICU stay and whether ICU discharge was during the night or weekend. All variables determined by expert opinion, prior experience and common use in critical care literature as relevant predictors of mortality. Additional candidate variables, not used, were completely decomposed SAPS3 score (instead of the partially broken-down score in this study), hospital category, admission time, day of the week and season of the year. All variables in our analyses were related to admission and treatment in the referring ICU, no variables were collected during transport or in the receiving ICU.
In a secondary model, in addition to the other variables, the SOFA score was used at discharge using observations from the 22 ICUs using SOFA scores. We also performed three sensitivity analyses in different subsets of the study cohort using the primary multivariable model. In the first subset, we included only admissions of six principal disease groups (see Additional file 1: Table S1). In the second subset, only admissions with no life-sustaining treatment limitations before transfer were included and, in the third subset, we excluded ICU-to-ICU transfers within the same hospital.
The regression results are reported as odds ratios (ORs) with 95% CI. We used STATA/SE 16 (StataCorp, College Station, TX, USA) for data analysis. A p-value < 0.05 was considered significant. This manuscript is conducted in accordance with the Equator network STROBE-statement [8].
Results
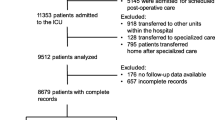
From 1st Jan, 2016 to 31st Dec, 2018 there were 112,860 adult admissions to Swedish ICUs, 15,588 (14.8%) of which ended with discharge by transfer to another ICU (see patient flow diagram Fig. 1). The majority were transferred for specialised care that was not available at the admitting hospital or ICU (clinical transfers, 62.8% of the study cohort). Capacity transfers were 15.8% of all transfers accounting for roughly 2.0% of ICU survivors.
Table 1 provides an overview of baseline patient data and characteristics of the referring ICUs. Clinical transfers differed from non-clinical transfers; they were slightly younger and less often male. Repatriation and capacity transfers were usually from tertiary care hospital ICUs where the median stay on the referring ICU was about 48 h before transfer. Most repatriations occurred during the day while almost one in five capacity transfers were at night. Capacity transfers had greater SOFA scores on discharge from the referring ICU, mainly due to cardiovascular and/or respiratory failure. Clinical transfers were more likely to have central nervous system injury while capacity transfers had acute lung injury and sepsis as primary diagnoses (see Additional file 1: Tables S2 and S3).
Unadjusted mortality within 30 days after discharge from the referring ICU was greater among capacity transfers where 25.0% died within 1 month of discharge (Table 1). Mortality in the capacity transfer group remained significantly higher for at least 180 days after discharge from the referring ICU, as seen in the unadjusted Kaplan–Meier diagram (Fig. 2).
Table 2 displays the uni- and multivariable associations between category of transfer and the primary end-point. In the primary multivariable analysis, an increased risk of death within 30 days of discharge was seen if the transfer was due to any other reason than repatriation. Adjusted results were similar when 180-day survival was analysed, with an OR of 1.19 (95% CI 1.02–1.39) p = 0.029 (see Additional file 1: Table S4).
The results remained when adjusting for persistent organ failure at ICU discharge using SOFA scores. The 30-day mortality rate after ICU discharge was roughly 50% greater among those transferred for clinical or capacity reasons compared to repatriation (see Table 3). The increased risk associated with capacity transfer was slightly less pronounced when 180-day survival was analysed among admissions with SOFA score (adjusted OR 1.53, 95% CI 1.13–2.06, p = 0.006; see Additional file 1: Table S5).
We also applied our primary multivariable model in three subsets of the study cohort: patients belonging to any of six principal disease groups, patients with no life-sustaining treatment limitations before transfer and patients who were transferred to an ICU located in another hospital. The results were comparable to the analyses of the main study cohort as shown in Additional file 1: Tables S6, S7 and S8.
Discussion
There were two principal findings in this study. First, non-clinical transfers due to resource constraints in the transferring ICU (capacity transfers) were associated with increased 30-day mortality compared to other non-clinical transfers (repatriations). Second, the proportion of ICU-to-ICU transfers in Sweden was greater than generally reported from comparable healthcare systems abroad. Before considering the implications of these findings, we need to discuss some methodological issues.
Understanding the impact of ICU-to-ICU transfer on patient outcome is complex and must consider a couple of important aspects. First, ICU-to-ICU transfers can be analysed from two different perspectives: the perspective of the referring ICU or the perspective of the receiving ICU. Second, whether a patient is transferred due to a clinical need or non-clinical reason must be known. Clinical transfers occur when there is a need for specialised care not available at the referring hospital. These transfers are usually associated with specific and sometimes lifesaving treatments, such as acute neurosurgical or cardiac interventions, which makes it difficult to find suitable non-transferred control patients. Hence, the first step must be to examine clinical and non-clinical transfers separately. Furthermore, non-clinical transfers need to be grouped into repatriations or capacity transfers, which usually have different urgencies. While the above categorisation facilitates an overall analysis, relevant control patients must still be identified for comparison of outcomes of non-clinical transfers. Studies from the referral’s perspective usually compare outcome of transferred patients with those staying in the ICU [3, 9], while studies from the receiver’s point-of-view usually compare outcomes of received referrals with those of admissions from the hospital’s own ward or emergency department [2, 10, 11]. Identifying appropriate control patients is challenging since non-clinical transfers are rarely undertaken when caregivers believe that discharge is imminent, either due to presumed recovery or death. Thus, comparing outcomes of patients transferred for non-clinical reasons with non-transferred patients may lead to biased results depending on the choice of control population.
In the present study, we examined transfers from the perspective of the referring hospital, and tried to circumvent the problem of identifying a proper control population by comparing outcomes within the cohort of transferred patients. This study design was based on the notion that, within the group of transferred patients, repatriations should be associated with the smallest adjusted risk of death due to ICU-to-ICU transfer. Repatriation was therefore used as our reference. Ideally, capacity transfers should also be associated with no or minimal risk increase compared to repatriations, while it is reasonable to believe that clinical transfers are associated with a higher risk.
Somewhat surprisingly, we found that 30-day mortality after capacity transfer was greater than after clinical transfer and repatriation in the unadjusted analyses. The difference in outcome between clinical and capacity transfers disappeared in the adjusted analyses but remained for repatriation. The adjusted risk relationships also remained after limiting analysis to admissions with information on organ failure (SOFA-score) at discharge in the multivariable analyses. While SOFA-score at discharge from the referring ICU was independently associated with poor outcome, it only partly explained the increased risk associated with clinical and capacity transfers compared to repatriation. Hence, other explanations not apparent from the results of the present study, must be considered.
It has been well established that transfer of critically ill patients is associated with more adverse outcomes partly due to transportation and poor communication of vital information [12,13,14,15]. In up to 50% of adverse events en route, pretransport recommendations provided by the referring intensivist were ignored [16]. Several studies have addressed the need for structured informative handover of the critically ill patient [17, 18]. However, further studies are needed to see if inadequacy of communication has less impact on the outcome of repatriation cases compared to clinical and capacity transfers. A more obvious explanation is that patients transferred for clinical and capacity reasons are more likely to endure an extra transfer compared to repatriations. A complete understanding of the care trajectory of patients undergoing ICU-to-ICU transfer is of great importance if we are to improve the chance of survival, particularly since such transports are likely to increase in the future [19].
The second notable result was that almost 15% of discharges from ICU were transfers to another ICU. Moreover, roughly 2% of all discharges were referred to another ICU due to lack of resources (capacity transfers). These numbers appear high compared to the literature [3, 20, 21], although most studies typically report transfers as a proportion of admissions to, rather than discharges from ICU. The overall high numbers of transfers may partly be explained by centralisation of specialised care to the few highly populated centres in our otherwise sparsely populated country. However, we believe that the large numbers of ICU-to-ICU capacity transfers also reflects the low overall number of available ICU beds in Sweden; one of the lowest in Europe [22, 23]. The high rate of capacity transfers suggest that ICUs regularly deliver care close to their surge capacity and prefer to transfer already admitted patients instead of refusing new patients with urgent needs. While refusal rates would enrich our analysis, such data were not available in the registry.
Strengths and limitations
An important strength in this large nationwide study is that transfers were identified and categorised on discharge by ICU staff according to specific SIR guidelines. The validity of this categorisation is supported by the fact that the direction of clinical transfers was mainly from local and district general hospitals to tertiary care hospitals while non-clinical transfers were in the opposite direction. Clinical transfers were, as expected, younger with shorter length of stay in hospital and in ICU before transfer, also supporting that clinical and non-clinical transfers were grouped accurately. Within the non-clinical transfer group, the proper separation of repatriations and capacity transfers is supported by greater SOFA scores and more frequent night-time discharges among capacity transfers compared to repatriations. Another important strength was that the results remained largely the same when we limited our analysis to three specific subsets of our study cohort. Capacity transfers were associated with increased 30-day mortality whether analysed in six defined diagnostic groups, in admissions with no life-sustaining treatment limitations or after exclusion of transfers within the same hospital.
A significant limitation is the lack of data collected during transport and after arrival to the receiving ICU. Although we have information on 180-day survival, we need to know more if we are to understand how transfer influences outcome. An important next step must be to analyse and compare complete care trajectories of transferred and non-transferred patients. Linking ICU care episodes are needed to identify factors that are associated with survival, i.e. duration and mode of transport, organ support during transport, interventions or treatment limitations in the receiving ICU.
Conclusion
This study identified an increased mortality rate associated with ICU-to-ICU transfers during periods of demand–supply mismatch. While prior studies have suggested that the only disadvantage of capacity transfers is longer intensive care periods [2, 3], this study shows that such transfers are also associated with greater mortality compared to repatriations. Avoiding the need for capacity transfers by increasing the number of ICU beds and staff is an obvious remedy. However, transfers due to demand–supply mismatch will continue to be necessary since it is impossible to meet all peaks in intensive care requirements. Future studies are needed to examine whether it is possible to minimise risk by careful patient selection, proper organisation of handover and transport and subsequent care in the receiving ICU.
Availability of data and materials
All data underlying this article were, after ethical approval, extracted and used unmodified from the Swedish Intensive Care Registry (SIR). The database cannot be shared publicly due to regulations under the Swedish law. Requests regarding the data may be made to the corresponding author.
Change history
13 April 2022
The unedited version of the Supplementary file was originally published with this article; it has now been replaced with the correct file.
References
Goldfrad C, Rowan K. Consequences of discharges from intensive care at night. Lancet. 2000;355(9210):1138–42.
Hill AD, Vingilis E, Martin CM, Hartford K, Speechley KN. Interhospital transfer of critically ill patients: demographic and outcomes comparison with nontransferred intensive care unit patients. J Crit Care. 2007;22(4):290–5.
Barratt H, Harrison DA, Rowan KM, Raine R. Effect of non-clinical inter-hospital critical care unit to unit transfer of critically ill patients: a propensity-matched cohort analysis. Crit Care. 2012;16(5):R179.
Ludvigsson JF, Otterblad-Olausson P, Pettersson BU, Ekbom A. The Swedish personal identity number: possibilities and pitfalls in healthcare and medical research. Eur J Epidemiol. 2009;24(11):659–67.
Parenmark F, Karlstrom G, Nolin T, Fredrikson M, Walther SM. Reducing night-time discharge from intensive care. A nationwide improvement project with public display of ICU outcomes. J Crit Care. 2018;49:7–13.
Moreno RP, Metnitz PGH, Almeida E, et al. SAPS 3—From evaluation of the patient to evaluation of the intensive care unit. Part 2: Development of a prognostic model for hospital mortality at ICU admission. Intensive Care Med. 2005;31(10):1345–55.
Vincent J-L, Moreno R, Takala J, et al. The SOFA (Sepsis-related Organ Failure Assessment) score to describe organ dysfunction/failure. Intensive Care Med. 1996;22(7):707–10.
von Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. Lancet. 2007;370(9596):1453–7.
Duke GJ, Green JV. Outcome of critically ill patients undergoing interhospital transfer. Med J Aust. 2001;174(3):122–5.
Maclure PT, Gluck S, Pearce A, Finnis ME. Patients retrieved to intensive care via a dedicated retrieval service do not have increased hospital mortality compared with propensity-matched controls. Anaesth Intensive Care. 2018;46(2):202–6.
Golestanian E, Scruggs JE, Gangnon RE, Mak RP, Wood KE. Effect of interhospital transfer on resource utilization and outcomes at a tertiary care referral center. Crit Care Med. 2007;35(6):1470–6.
Droogh JM, Smit M, Hut J, de Vos R, M Ligtenberg JJ, Zijlstra JG. Inter-hospital transport of critically ill patients; expect surprises. Crit Care. 2012;16(1):R26.
Fanara B, Manzon C, Barbot O, Desmettre T, Capellier G. Recommendations for the intra-hospital transport of critically ill patients. Crit Care. 2010;14(3):10.
Fried MJ, Bruce J, Colquhoun R, Smith G. Inter-hospital transfers of acutely ill adults in Scotland. Anaesthesia. 2010;65(2):136–44.
Beckmann U, Gillies DM, Berenholtz SM, Wu AW, Pronovost P. Incidents relating to the intra-hospital transfer of critically ill patients—an analysis of the reports submitted to the Australian Incident Monitoring Study in Intensive Care. Intensive Care Med. 2004;30(8):1579–85.
Ligtenberg JJM, Arnold LG, Stienstra Y, et al. Quality of interhospital transport of critically ill patients: a prospective audit. Crit Care. 2005;9(4):R446.
Dutra M, Monteiro MV, Ribeiro KB, Schettino GP, Kajdacsy-Balla Amaral AC. Handovers Among Staff Intensivists: A Study of Information Loss and Clinical Accuracy to Anticipate Events. Crit Care Med. 2018;46(11):1717–21.
Pickering BW, Hurley K, Marsh B. Identification of patient information corruption in the intensive care unit: using a scoring tool to direct quality improvements in handover. Crit Care Med. 2009;37(11):2905–12.
Droogh JM, Smit M, Absalom AR, Ligtenberg JJM, Zijlstra JG. Transferring the critically ill patient: are we there yet? Crit Care. 2015;19(1):7.
Grier S, Brant G, Gould TH, von Vopelius-Feldt J, Thompson J. Critical care transfer in an English critical care network: analysis of 1124 transfers delivered by an ad-hoc system. J Intensive Care Soc. 2019;9(1):33–9.
Patel JJ, Kurman J, Al-Ghandour E, et al. Predictors of 24-h mortality after inter-hospital transfer to a tertiary medical intensive care unit. J Intensive Care Soc. 2018;19(4):319–25.
Rhodes A, Ferdinande P, Flaatten H, Guidet B, Metnitz PG, Moreno RP. The variability of critical care bed numbers in Europe. Intensive Care Med. 2012;38(10):1647–53.
Bauer J, Brüggmann D, Klingelhöfer D, et al. Access to intensive care in 14 European countries: a spatial analysis of intensive care need and capacity in the light of COVID-19. Intensive Care Med. 2020;46(11):2026–34.
Acknowledgements
Not applicable
Funding
Open access funding provided by Linköping University. This study was supported by institutional grants from Centre for Research and Development Region Gävleborg and Region Östergötland, Sweden.
Author information
Authors and Affiliations
Contributions
Both authors contributed equally to the manuscript including design, acquisition and analysis/interpretation of the data as well as drafting of the final paper. Both authors have approved the submitted version. Part of this study was presented by FP at the “hot topic session” at ESICM Lives Berlin 2019. Both authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
The Swedish Intensive Care Register operates within the legal framework of the Swedish National Quality Registers. This framework does not require written informed consent from the patients, but patients may withdraw their data from the register. The study was approved by the Regional Ethics Review Board of Linköping University (2016/312-31) as well as by the Board of the Swedish Intensive Care Register.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Additional file 1.
Additional Tables.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Parenmark, F., Walther, S.M. Intensive care unit to unit capacity transfers are associated with increased mortality: an observational cohort study on patient transfers in the Swedish Intensive Care Register. Ann. Intensive Care 12, 31 (2022). https://doi.org/10.1186/s13613-022-01003-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s13613-022-01003-x