Abstract
Objective
Critically ill patients admitted in ICU because of COVID-19 infection display severe hypoxemic respiratory failure. The Surviving Sepsis Campaign recommends oxygenation through high-flow nasal cannula over non-invasive ventilation. The primary outcome of our study was to evaluate the effect of the addition of a surgical mask on a high-flow nasal cannula system on oxygenation parameters in hypoxemic COVID-19 patients admitted in ICU who do not require urgent intubation. The secondary outcomes were relevant changes in PaCO2 associated with clinical modifications and patient’s feelings.
Design
We prospectively assessed 21 patients admitted in our mixed Intensive Care Unit of the Cliniques Universitaires Saint Luc.
Main results
While FiO2 was unchanged, we demonstrate a significant increase of PaO2 (from 59 (± 6), to 79 mmHg (± 16), p < 0.001), PaO2/FiO2 from 83 (± 22), to 111 (± 38), p < 0.001) and SaO2 (from 91% (± 1.5), to 94% (± 1.6), p < 0.001), while the patients were under the surgical mask. The SpO2 returned to pre-treatment values when the surgical mask was removed confirming the effect of the device rather than a spontaneous positive evolution.
Conclusion
A surgical mask placed on patient’s face already treated by a High-flow nasal cannula device improves COVID-19 patient’s oxygenation admitted in Intensive Care Unit for severe hypoxemic respiratory failure without any clinically relevant side.
Similar content being viewed by others
Background
A novel coronavirus named severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) is responsible for an acute and a rapidly evolving illness that the World Health Organization termed Coronavirus Disease 2019 (COVID-19) [1]. This disease spread around the entire globe because of its great contagiousness and led to a severe public health problem. While most patients present with mild respiratory symptoms, some present with severe pneumonia requiring hospitalization and in the most severe cases Intensive Care Unit (ICU) admission.
This situation induced an increased pressure on ICUs that are stretched beyond their capacity to provide specific care for the most severely ill patients including the need of specific materials for mechanical ventilation such as ventilators [2].
Actually, hypoxic respiratory failure is observed in 14% of patients that will require hospitalisation with supplemental oxygen administration. Furthermore, a severe acute respiratory failure is observed in 5% of these patients despite conventional oxygen therapy, requiring hospitalisation in ICU [3]. This COVID-19 associated pneumonia is well characterized by a bilateral infiltrates on chest X-ray and by bilateral ground-glass opacifications with occasional consolidation in multi-lobe lesions on chest CT [4].
In this critical pandemic situation, where the incidence of COVID-19 severe patients requiring specific intensive treatment continues to rise with limited resources such as ventilators, we tried to improve oxygenation parameters of our patients with easy-to-perform procedures. Our ICU used high-flow nasal cannula (HFNC), as recommended by the guidelines for acute hypoxemic respiratory failure in COVID-19 adults patients that do not require urgent endotracheal intubation [5]. In our hospital, to decrease the risk of viral transmission from exhaled air, a surgical mask is actually recommended on patient’s face during HFNC treatment when healthcare workers are in the room. Indeed, recent data suggest a variable increase in the mean distance of droplet dispersion from coughing with the use of HFNC devices, especially when the flow rate is increased [6, 7].
The primary outcome of our study was to evaluate the effect of the addition of a surgical mask on an HFNC system on oxygenation parameters (PaO2) in hypoxemic COVID-19 patients admitted in ICU who do not require urgent intubation. The secondary outcomes were relevant changes in PaCO2 associated with clinical modifications and patient’s feelings.
Materials and methods
This study is a prospective monocenter study performed in a 22-bed mixed ICU at the Cliniques Universitaires Saint Luc. We enrolled all consecutive COVID-19-infected patients admitted in ICU who did not require urgent intubation. This study was performed only when the investigators were present at the time of admission. All patients were connected to a HFNC device (Optiflow TM RT202, Fisher & Paykel, Auckland, New Zealand) upon ICU admission and were monitored through our usual system (Intellivue Patient Monitor MP70, Philips Medizin Systeme Boeblingen GmbH, Boeblingen, Germany).
Inclusion criteria included hypoxemic and awake patients requiring HFNC who were relatively stable under this treatment and without a presumed intubation or anticipated changes to respiratory clinical management within the next 2 h. Exclusion criteria of this study assimilate exclusion criteria for classical HFNC including an altered consciousness, confusion, persistent hypoxemia or hypoventilation, respiratory acidosis, exacerbation of asthma or chronic respiratory failure, cardiogenic pulmonary oedema, circulatory failure with use of vasopressor, the need for non-invasive or invasive mechanical ventilation [8]. During the study, the patient’s feeling was evaluate by asking questions about eventual sensation of suffocation or the onset of dyspnoea and by analysing the behaviour’s patient by the investigators that monitored the experiment.
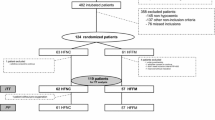
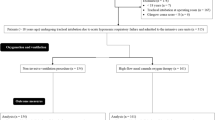
The enrollment process allowed us to include 21 patients between 27/03/2020 and 22/04/2020. All the patients agreed to participate in the study and had supplementary arterial blood gas drawn through the arterial line since the surgical mask on the HFNC device was a special request of our hospital (hospital hygiene department) for all patients admitted in ICU. Written informed consent was obtained from all participants before inclusion. We excluded three patients that required immediate intubation upon their arrival in ICU and one patient admitted during the night required HFNC but with a very rapid clinical improvement in the next morning that no longer justified administration of an HFNC device.
Statistical analysis
Because no preliminary data were available for sample size determination, we made some hypotheses, based on our clinical knowledge. Assuming a standard deviation of 15 mmHg in the response of matched PaO2 measurements, a sample size of at least 20 patients allows having a power of 80% to detect a mean increase of at least 10 mmHg in PaO2, at the statistical significance level of 0.05. Such assumption corresponds to a Cohen’s effect size of 0.67; the larger the effect size the lower the sample size.
All results are expressed as mean ± SD. Data with and without surgical mask were compared using paired t tests, after checking with Q–Q plots if differences were normally distributed. Values with repeated measures like the SpO2 were analysed using a within-factor ANOVA with F test and a Bonferroni correction was used for multiple comparisons. All tests were two sided and a p < 0.05 was considered as statistically significant. Analyses were performed with Graph Pad Prism version 8.1.2.
Protocol
Subjects were enrolled a few hours after admission in our ICU, while lying in a calm environment in a single room. Placement of an inline arterial catheter was performed as usual upon ICU admission. Oxygenation through the HFNC device was started and adapted in all patients with a SpO2 target above 90%. The flow was fixed at 60 L/min. The temperature was set at 31–37 °C. These parameters were then fixed without any modification during the ongoing experiment unless deleterious evolution was observed. In particular, we did not change the FiO2 parameters during the experiment. Patients were placed in a semi-recumbent position, with the HFNC already in place.
A first blood gas measurement after a minimum of 30 min of HFNC was performed. Then, a surgical mask was set on the patient’s face, encompassing the nose to the chin. The mask was placed by the study investigator to avoid any misplacement and to assure the absence of leak. Correct placement of the mask was assessed all along the procedure. A second blood gas measurement after a minimum of 30 min of HFNC with the surgical mask was performed. This blood gas measurement was performed as standard of care to verify the absence of secondary side effects including hypercapnia. The surgical mask was then removed and SpO2 was registered after another 30 min of HFNC only.
Recorded haemodynamic and respiratory parameters on each study phase included heart rate, blood pressure, SpO2 and respiratory rate.
Results
Our patient population consisted of 21 patients (18 males and 3 females). The mean age was 60 years (± 12.3) and the mean body mass index was 28 kg/m2 (± 4). The mean FiO2 administration through HFNC at the beginning of the study protocol was 75% (± 18%) and they all were receiving oxygen at a flow rate of 60 L/min. The maximum SOFA score of our patient population was 5 with a range of 3–6, mainly due to the severe hypoxemia. All our patients presented a normal neurologic evaluation (Glasgow Coma Scale of 15/15). The characteristics of the patients are detailed in Table 1.
We did not observe any significant change in haemodynamic parameters during all the process, while we noticed a small decrease of the respiratory rate with the surgical mask set on the HFNC device (from a rate to 27.8/min (± 5.5) to 26.2/min (± 5.6), p < 0.05). We observed a significant improvement of the PaO2 from (59 mmHg (± 6), to 79 mmHg (± 16), p < 0.001) (Fig. 1a), the SaO2 (from 91% (± 1.5), to 94% (± 1.6), p < 0.001) (Fig. 1b), the PaO2/FiO2 (from 83 (± 22) to 111 (± 38), p < 0.001) (Fig. 1c). We also observed a change in the mean PaCO2 (from 31 mmHg (± 3) to 32 mmHg (± 4), p < 0.002) (Fig. 1d). All these parameters are detailed in Table 2 for each patient.
We then removed the surgical mask and observed that SpO2 fell back to its initial value with a mean SpO2 of 91% (± 1) (Fig. 2). No patients revealed any complaints of discomfort and our observation confirmed that everyone accepted the surgical mask on the HFNC device very well.
Repeated SpO2 performed with high flow nasal cannula before the test alone (HFNC before test), in presence of the surgical mask (HFNC/surgical mask) and finally again with high flow nasal cannula alone (HFNC after test). *p < 0.05 in a within-factor ANOVA with Bonferroni correction for multiple comparisons. HNCF before compared to HFNC after the test showed no statistical difference in paired t tests
Discussion
All patients exhibited a hypoxemic acute respiratory failure related to Coronavirus Disease 2019 and presented refractory hypoxemia under classical nasal supplemental oxygen. As recommended, they benefited from a HFNC device to obtain a SpO2 above 90% [5]. As recommended, benefited of an HFNC device to obtain a SpO2 above 90% [5]. In this study, we demonstrated that the simple addition of a surgical mask on the patient’s face increased significantly the oxygenation of these hypoxemic COVID-19 patients admitted in ICU.
All started with the observation that these hypoxemic patients increased their SpO2 directly after receiving the surgical mask over the HFNC, a request of our hospital hygiene department. Adding this mask on the patient’s face while receiving HFNC oxygenation increases all the oxygenation parameters compared to classical HFNC therapy, without clinically significant change of PaCO2. All the settings of the HFNC devices were kept constant during the experiment.
We did not give to our patients any specific recommendation concerning mouth opening or closing during the experimentation, but we observed often an opened mouth with an increased room intake. The observed improvement in oxygenation parameters could be explained not only by an increased oxygen concentration in front of the mask but also by a decrease of room air entrainment that is known to dilute the gas mixture with less inspired O2 concentration [9]. The mask would then play a filter role by increasing the positive effect of the HFNC device and by decreasing the negative effect of entrainment of room air. We confirmed the additional effect of surgical mask to HFNC device rather than a favorable spontaneous evolution as its removal directly induced a return to previous oxygenation parameters as measured by the SpO2. Interestingly, none of our patients presented subjective complaints of discomfort by adding this surgical mask on top of HFNC.
The HFNC oxygen therapy is a well-known technique allowing heated and humidified gas with a maximum flow rate of 70 L/min and an adjustable oxygen fraction (FiO2) from 21 to 100% [10]. A recent meta-analysis showed that patients admitted with an acute hypoxemic respiratory failure from diverse aetiologies could improve oxygenation with HFNC compared to conventional oxygen therapy evolving towards a reduced need for tracheal intubation [11]. Likewise, it was recently demonstrated that the addition of a double-trunk mask on HFNC improves oxygenation in acute respiratory failure patients [12]. Non-invasive respiratory support plays an essential role in the treatment of COVID-19 patient with acute respiratory failure without the need of an urgent endotracheal intubation even if HFNC has not been assessed much yet. However, in adult patients admitted in ICU for an acute hypoxemic respiratory failure despite conventional oxygen therapy, as mentioned above, the Surviving Sepsis Campaign COVID-19 suggests the use of HFNC over Non-invasive positive-pressure ventilation (NIPPV) [5]. Recent study even observed an HFNC-positive response in moderate hypoxemic patients while failure rate increased as long as the PaO2/FiO2 decreased [13].
Importantly, this study was designed to assess the efficacy of adding a surgical mask on HFNC device and not to prevent endotracheal intubation.
Reducing the breath dispersion distance and aerosol generation during high-flow nasal ventilation to prevent SARS-CoV-2 transmission is a major issue. However, in vitro data using lung model with smoke generator or manikin are rather reassuring on this point. By using the same study method and similar breathing patterns, in vitro studies suggested that droplet dispersal during HFNC therapy was limited to the proximal space of the face and the cannula with even less dispersal distance of exhaled smoke compared to traditional high-flow oxygen therapy systems including non-rebreathing or Venturi masks that are traditionally used in acute hypoxemic respiratory failure [14, 15]. By studying different manikin models, in vitro and clinical studies, a recent review reported scientific evidences that use of HFNC during this pandemia has probably not increased either dispersion or microbiological contamination into the environment than other oxygen devices [16]. Furthermore, clinical studies evaluating bacterial environmental contamination of patients admitted in ICU for bacterial pneumonia and treated either by HFNC device or by conventional oxygen mask did not find any significant difference in bacterial counts in air or contact surface [17]. These data support the fact that there is actually no scientific proof of an increased bio-aerosols dispersion through an HFNC device compared to conventional high-flow oxygen therapy. Moreover, computational fluid dynamic simulations reported that wearing a surgical mask over HFNC might reduce aerosol droplets dispersion [18].
Our study presents several limitations. We enrolled a limited number of patients as we only included them in the presence of the investigators. We focused essentially in improving the oxygenation parameters. In this regard, specific measurements, such as minute ventilation, were not performed. Also, we did not enroll severe COPD patients and these data might not be generalizable to this population. However, PaCO2 measurement did not show any clinically significant increase, and it is worth noting that HFNC is proposed to treat those patients at home [19]. We further believe that targeting an SpO2 of 90% would limit the risk of oxygen-induced hypercapnia. Finally, the exact FiO2 delivered by the system while using the face mask was not measured, as already proposed by other authors [8].
Conclusion
Our study suggests that a surgical mask placed on patient’s face already treated by a High-flow nasal cannula device would offer an advantage in terms of oxygenation in COVID-19 patients admitted in ICU with severe hypoxemic respiratory failure. Moreover, this oxygenation improvement is associated with neither a clinically significant change in the PaCO2 nor subjective patient complaints.
Availability of data and materials
All data generated or analysed during this study are included in this published article.
Abbreviations
- SARS-CoV-2:
-
Severe acute respiratory syndrome coronavirus 2
- COVID-19:
-
Coronavirus disease 2019
- ICU:
-
Intensive care unit
- HFNC:
-
High-flow nasal cannula
- NIPPV:
-
Non-invasive positive-pressure ventilation
References
Sohrabi C, Alsafi Z, O'Neill N, Khan M, Kerwan A, Al-Jabir A, et al. World Health Organization declares global emergency: a review of the 2019 novel coronavirus (COVID-19). Int J Surg. 2020;76:71–6. https://doi.org/10.1016/j.ijsu.2020.02.034
Truog RD, Mitchell C, Daley GQ. The toughest triage—allocating ventilators in a pandemic. N Engl J Med. 2020. https://doi.org/10.1056/NEJMp2005689.
Wu Z, McGoogan JM. Characteristics of and important lessons from the coronavirus disease 2019 (COVID-19) outbreak in China: summary of a report of 72 314 cases from the Chinese Center for Disease Control and Prevention. JAMA. 2020;323(13):1239–42. https://doi.org/10.1001/jama.2020.2648
Wang K, Kang S, Tian R, Zhang X, Zhang X, Wang Y. Imaging manifestations and diagnostic value of chest CT of coronavirus disease 2019 (COVID-19) in the Xiaogan area. Clin Radiol. 2020. https://doi.org/10.1016/j.crad.2020.03.004.
Alhazzani W, Møller MH, Arabi YM, Loeb M, Gong MN, Fan E, et al. Surviving sepsis campaign: guidelines on the management of critically ill adults with coronavirus disease 2019 (COVID-19). Crit Care Med. 2020. https://doi.org/10.1007/s00134-020-06022-5.
Hui DS, Chow BK, Lo T, Tsang OTY, Ko FW, Ng SS, et al. Exhaled air dispersion during high-flow nasal cannula therapy versus CPAP via different masks. Eur Respir J. 2019;53(4):1802339.
Loh NW, Tan Y, Taculod J, Gorospe B, Teope AS, Somani J, et al. The impact of high-flow nasal cannula (HFNC) on coughing distance: implications on its use during the novel coronavirus disease outbreak. Can J Anaesth. 2020. https://doi.org/10.1007/s12630-020-01634-3.
Frat JP, Thille AW, Mercat A, Girault C, Ragot S, Perbet S, et al. High-flow oxygen through nasal cannula in acute hypoxemic respiratory failure. N Engl J Med. 2015;372(23):2185–96.
Lee CC, Mankodi D, Shaharyar S, Ravindranathan S, Danckers M, Herscovici P, et al. High flow nasal cannula versus conventional oxygen therapy and non-invasive ventilation in adults with acute hypoxemic respiratory failure: a systematic review. Respir Med. 2016;121:100–8.
Nishimura M. High-flow nasal cannula oxygen therapy in adults: physiological benefits, indication, clinical benefits, and adverse effects. Respir Care. 2016;61(4):529–34.
Rochwerg B, Granton D, Wang DX, Helviz Y, Einav S, Frat JP, et al. High flow nasal cannula compared with conventional oxygen therapy for acute hypoxemic respiratory failure: a systematic review and meta-analysis. Intensive Care Med. 2019;45(5):563–72.
Duprez F, Bruyneel A, Machayekhi S, Droguet M, Bouckaert Y, Brimioulle S, et al. The double-trunk mask improves oxygenation during high-flow nasal cannula therapy for acute hypoxemic respiratory failure. Respir Care. 2019;64(8):908–14.
Wang K, Zhao W, Li J, Shu W, Duan J. The experience of high-flow nasal cannula in hospitalized patients with 2019 novel coronavirus-infected pneumonia in two hospitals of Chongqing, China. Ann Intensive Care. 2020;10(1):37.
Kotoda M, Hishiyama S, Mitsui K, Tanikawa T, Morikawa S, Takamino A, et al. Assessment of the potential for pathogen dispersal during high-flow nasal therapy. J Hosp Infect. 2020;104(4):534–7.
Ip M, Tang JW, Hui DSC, Wong ALN, Chan MTV, Joynt GM, et al. Airflow and droplet spreading around oxygen masks: a simulation model for infection control research. Am J Infect Control. 2007;35(10):684–9.
Li J, Fink JB, Ehrman S. High-flow nasal cannula for COVID-19 patients: low risk of bio-aerosol dispersion. Eur Respir J. 2020;55(5):2000892.
Leung CCH, Joynt GM, Gomersall CD, Wong WT, Lee A, Ling L, et al. Comparison of high-flow nasal cannula versus oxygen face mask for environmental bacterial contamination in critically ill pneumonia patients: a randomized controlled crossover trial. J Hosp Infect. 2019;101:84–7.
Leonard S, Atwood CW Jr, Walsh BK, DeBellis RJ, Dungan GC, Strasser W, et al. Preliminary findings on control of dispersion of aerosols and droplets during high-velocity nasal insufflation therapy using a simple surgical mask—implications for the high-flow nasal cannula. Chest. 2020;S0012–3692(20):30579–81.
Elshof J, Duiverman ML. Clinical evidence of nasal high-flow therapy in chronic obstructive pulmonary disease patients. Respiration. 2020;99(2):140–53.
Acknowledgements
We thank all the staff who participated in the data collection.
Funding
No funding was received for this work and publication.
Author information
Authors and Affiliations
Contributions
VM conceived the study, performed the data collection, analysed the data and written the manuscript. MT and AN participated in data collection. AR (Arnaud Robert) participated in data collection and revised the manuscript. AR (Annie Robert) analysed and reviewed the data, PFL revised the manuscript. XW conceived the study and revised the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethical approval and consent to participate
We asked our Hospital and Faculty Ethics Committee (Cliniques Universitaires Saint Luc – Université Catholique de Louvain) which approved our study without ethical problem according to clinical common sense and good practises. Written informed consent was obtained from all participants before inclusion.
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Montiel, V., Robert, A., Robert, A. et al. Surgical mask on top of high-flow nasal cannula improves oxygenation in critically ill COVID-19 patients with hypoxemic respiratory failure. Ann. Intensive Care 10, 125 (2020). https://doi.org/10.1186/s13613-020-00744-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s13613-020-00744-x