Abstract
Background
Advances in understanding of cancer biology, genomics, epigenomics, and immunology have resulted in development of several therapeutic options that expand cancer care beyond traditional chemotherapy or radiotherapy, including individualized treatment strategies, novel treatments based on monotherapies or combination therapy to reduce toxicities, and implementation of strategies for overcoming resistance to anticancer therapy.
Results
This review covers the latest applications of epigenetic therapies for treatment of B cell, T cell, and Hodgkin lymphomas, highlighting key clinical trial results with monotherapies and combination therapies from the main classes of epigenetic therapies, including inhibitors of DNA methyltransferases, protein arginine methyltransferases, enhancer of zeste homolog 2, histone deacetylases, and the bromodomain and extraterminal domain.
Conclusion
Epigenetic therapies are emerging as an attractive add-on to traditional chemotherapy and immunotherapy regimens. New classes of epigenetic therapies promise low toxicity and may work synergistically with other cancer treatments to overcome drug resistance mechanisms.
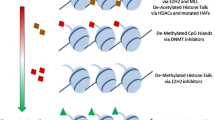
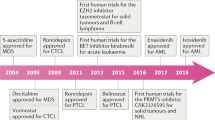
Graphical Abstract

Similar content being viewed by others
Background
Non-Hodgkin lymphoma (NHL) is the seventh-most prevalent cancer and has the sixth-highest mortality rate among cancers in the USA [1]. Hodgkin lymphoma (HL) is the other main subtype of lymphoma. An estimated 8830 individuals in the USA will have been diagnosed with HL in 2021 [2]. Other subtypes of NHL include B cell, T cell, and natural killer cell lymphomas, with the most common B cell lymphoma subtypes being diffuse large B cell lymphoma (DLBCL; 31% of diagnosed lymphomas), follicular lymphoma (FL; 22%), and marginal zone lymphoma (8%) [1]. The prognoses for patients with HL and NHL are dependent on a variety of factors, such as age at diagnosis, cancer stage, lymphatic involvement, how well the patient performs normal daily activities (performance status), and levels of lactate dehydrogenase in the blood [3]. Although survival rates are dependent on these factors, the overall 5-year survival rate is 89% for patients with HL [2] and 73% for patients with NHL [2, 3]. Survival rates are globally increasing; however, the prognosis for people with relapsed lymphoma remains poor.
In patients with NHL or HL, common treatment options include chemotherapy, immunotherapy, and radiotherapy, used alone or in combination, and have high curative potential for many patients but come with significant challenges for a small subset of patients. Although chemotherapy is a well-established, effective method of treating lymphoma, many adverse events (AEs) are associated with chemotherapeutic agents due to their cytotoxic and nonselective mechanisms of action [4]. Some of the short-term impacts of chemotherapy, such as fatigue, nausea, hair loss, and loss of appetite, resolve quickly with lifestyle modifications and/or supportive therapy [5]. Supportive therapy or other approaches used to reduce the impact of chemotherapy-induced AEs are not effective in reducing the long-term impact of chemotherapy and may be associated with additional AEs. Some of the long-term impacts of chemotherapy that may or may not be controlled by supportive medicine include loss of fertility, secondary cancer development, and lung damage. In aggressive forms of lymphoma, such as DLBCL, most patients are older than 60 years when diagnosed and some are too frail for standard chemotherapies [6].
The anti-CD monoclonal antibody rituximab revolutionized the treatment and prognosis for CD20+ B cell malignancies and established immunotherapy as a valid treatment option for B cell malignancies [7]. Despite the success of rituximab, resistance to first-line rituximab in indolent B cell NHL and in relapsed or refractory (R/R) disease can occur [8]. Rituximab is indicated for treatment of patients with previously untreated or R/R B cell NHL [9]as monotherapy for patients with R/R FL, in combination with chemotherapy regimens containing cyclophosphamide, doxorubicin, vincristine, and prednisone (CHOP) for patients with untreated DLBCL, and with cyclophosphamide, vincristine, and prednisolone (CVP) for patients with untreated FL [9, 10]. For advanced-stage FL, common treatment regimens include rituximab alone or in combination with chemotherapy, such as CVP or CHOP [11], or a targeted therapy, such as rituximab plus lenalidomide (R2), as first-line therapy [12]. R2 is also used as a treatment option for multiple NHL subtypes [9, 10, 13]. Combination rituximab and bendamustine is also indicated for patients with indolent NHL [14]. Rituximab is a component in 58% of second-line FL combination therapies, and the majority of patients with R/R FL will receive rituximab again in subsequent lines of therapy [15]. For example, one study showed that 40% of patients with relapsed FL or low-grade NHL responded to re-treatment with rituximab after having received prior rituximab therapy [16]. However, rituximab rechallenge in patients with R/R NHL is associated with a shorter progression-free survival rate than patients naive to rituximab [10]. Therefore, alternatives to existing treatments are being sought, particularly with regard to targeted therapies [17]. More recently, glycoengineered type II anti-CD20 monoclonal antibodies, such as obinutuzumab, have shown superior response rates to rituximab, whether as monotherapy or in combination for R/R indolent lymphoma [18]. Unfortunately, this therapy is associated with increased side effects compared with rituximab monotherapy and may be better suited in combination with therapies with low risk of AEs [17, 18].
Subsequent advances in our understanding of the biology, genetics, and immunology of cancer led to development of targeted therapies and immunomodulatory drugs, including small molecule kinase inhibitors and monoclonal antibodies targeting proteins involved in cancer cell growth and mitogenic signaling. Although these therapies are more selective than chemotherapy and thus designed to generate fewer off-target effects [4], their use is associated with unique AEs related to their targets, such as cutaneous toxicity observed with epidermal growth factor receptor inhibitors [19], and hepatotoxicity, diarrhea, glucose regulation abnormalities (e.g., hyperglycemia) [20], as well as pneumonitis associated with phosphatidylinositol 3-kinase inhibitor use [21]. Emerging anticancer immunotherapeutic agents (e.g., immune checkpoint inhibitors, T cell therapies) are associated with immune-related AEs that can affect their safety and tolerability profiles [22, 23]. Issues of cytotoxicity, treatment resistance, and tolerability with the aforementioned therapies indicate additional need for new classes of therapeutics.
Epigenetic therapies are a selective way to treat cancer that avoid the cytotoxic AEs associated with chemotherapy and targeted therapies [24]. They are also a means of overcoming drug resistance pathways, making them an important complementary tool in the treatment of R/R lymphomas. Epigenetic modulators control gene expression and are involved in several cellular processes that depend on modification of nucleic acids and histones, including cellular growth and proliferation [25]. Epigenetic modifications include DNA methylation and histone acetylation/methylation, all of which regulate the accessibility of chromatin to transcription factors and other DNA-binding proteins (Fig. 1) [25]. Many epigenetic processes are linked to oncogenesis and cancer proliferation [25]. Several epigenetic therapies are approved for treatment of lymphomas [26,27,28,29,30].
This review provides an in-depth summary of key clinical advances of epigenetic therapies for treatment of lymphoma in the last 5 years and the potentially synergistic benefits they provide when administered with other therapeutic agents. Classes of therapeutic agents covered include inhibitors of DNA N-methyltransferases (DNMTs), histone methyltransferases (HMTs), protein arginine methyltransferases (PRMTs), histone deacetylases (HDACs), bromodomain (BRD), and BRD/extraterminal domain (BET; Table 1) [31,32,33,34,35,36,37,38,39,40,41,42,43]. This review covers the safety profiles of key agents from these classes (Table 2).
Epigenetic mechanisms targeted in cancer therapy
Epigenetic writers
DNA hypermethylation in cancer cells is associated with silencing of tumor suppressor genes and activation of oncogenes, and it is one of the most characterized epigenetic mechanisms in cancer [44]. Targeting epigenetic writers, such as DNMTs, PRMTs, and HMTs, are an attractive strategy to restore the epigenomic regulation of cellular proliferation and halt cancer cell growth (Fig. 1) [25]. DNA methyltransferases transfer a methyl group from S-adenosylmethionine to the cytosine ring in a cytosine–phosphate–guanine dinucleotide pair in the C5 position to create 5-methylcytosine, a molecule that regulates gene transcription [44]. Studies show that DNMT inhibitors induce hypomethylation and upregulation of genes involved in DNA transcription, RNA processing, and ribosomal function as their primary therapeutic effect, although it is unclear if the modest increase in the rate of hypomethylation caused by an inhibitor is enough to affect cellular functions [45, 46]. DNMT mutations are common in many kinds of cancer cells, including lymphomas, and studies have shown that a higher baseline level of methylation exists in cancerous cells compared with noncancerous cells, even when cells stop dividing [47, 48].
Histone methyltransferases play a similar role to that of DNMTs in cancer cell biology, catalyzing the transfer of 1 or more methyl groups to lysine and arginine residues on histone proteins [49]. Depending on the site of methylation, histones can promote or repress gene transcription [50]. The HMT EZH2 has emerged as an attractive therapeutic strategy for various malignancies because of its noncytotoxic mechanism of action and hypothesized role in overcoming mechanisms of chemoresistance [51,52,53]. Enhancer of zeste homolog 2 is the enzymatic subunit of polycomb repressive complex 2 that catalyzes 1 to 3 methylations of Lys27 on histone H3, which serves to repress gene transcription [54, 55]. The gain-of-function EZH2 mutation at tyrosine 641 within the catalytic SET domain increases H3K27 trimethylation and decreases H3K27 monomethylation [54, 56]. However, wild-type germinal center-derived lymphomas also retain dependency on EZH2 to proliferate and repress plasma cell differentiation [57]. EZH2 plays a role in many processes within the tumor microenvironment, including CD4+, natural killer, and CD8 T cell differentiations and functions [58].
Other potential epigenetic writer targets are protein arginine methyltransferase 5 (PRMT5) and lysine methyltransferase 2 (KMT2). PRMT5 is a subtype of PRMT that catalyzes the methylation of mono- and symmetric dimethylarginine, which can repress or promote gene transcription. PRMT5 is one of the most overexpressed PRMT types in cancer cells, regulating B cell proliferation and survival, and germinal cell formation and expansion, hence its emergence as a possible therapeutic target [59, 60]. KMT2, a lysine methyltransferase, is considered to be the main lysine 4 of the core histone H3 (H3K4) methyltransferase [61]. KMT2 positively regulates gene expression and mutations, in particular subsets of the KMT2 family, and has been implicated in hematologic malignancies owing to induction of H3K4me3 to the promoter of genes associated with hematopoietic cell development and differentiation [62].
Epigenetic erasers
Epigenetic erasers are proteins that remove DNA and histone protein modifications produced by epigenetic writers to regulate gene expression (Fig. 1) [25]. Histone and nonhistone protein acetylation is regulated through opposing functions of histone acetyltransferases and HDACs [25, 42, 63]. Histone acetylation promotes cancer cell growth by increasing the rate of gene expression of oncogenes, such as B cell lymphoma 6 (BCL6), which regulates oncogenes implicated in FL, DLBCL, and B cell lymphoproliferative disorders [25, 42, 63, 64]. Histone deacetylases are made up of 4 classes that are all potential anticancer targets, although some are zinc dependent (classes 1, 2a/b, and 4) or nicotinamide–adenine–dinucleotide dependent (class 3) [42]. Studies show HDAC inhibitors reactivate tumor suppressor genes and promote an immune response [65].
Another epigenetic eraser, histone demethylases (KDM), removes the arginine and lysine residues added by HMTs [66]. A particular subfamily of KDMs, KDM5, can remove tri- and dimethyl marks from H3K4. KDM5 can either activate or suppress transcription depending on the methylation site and has been shown to be involved in the regulation of oncogenes [66].
Epigenetic readers
Epigenetic readers are composed of domains that recognize and bind to specific post-translational DNA or histone modifications. These modifications include BRD-containing proteins that recognize acetylated histone residues, methyl cytosine–phosphate–guanine-binding domains that recognize methylated cytosine–phosphate–guanine, and chromodomains that recognize methylated lysine (Fig. 1) [25]. The BET family of epigenetic readers plays a critical role in cancer development by activating and potentiating expression of key oncogenes [25, 63]. The BET family comprises 4 members, including BRD-containing proteins 2 (BRD2), 3 (BRD3), 4 (BRD4), and t (BRDt) [25], although targeting BRD4 is thought to be the primary cause of the anti-oncogenic effects of BET inhibitors [67].
Epigenetic therapies for lymphomas
B cell non-Hodgkin lymphomas
DNA methyltransferase inhibitors
Two DNMT inhibitors, azacitidine and decitabine, are approved by the US Food and Drug Administration (FDA) and the European Medicines Agency for treatment of acute myeloid leukemia and myelodysplastic syndrome [27, 68, 69], but studies thus far have shown no evidence that decitabine promoted hypomethylation in individuals with DLBCL [31].
Although decitabine is ineffective as a monotherapy [31], a phase 1/2 study combined decitabine with chemotherapy in 6 patients with DLBCL, NHL, and HL who previously experienced progressive disease (PD) on chemotherapy. Two participants maintained stable disease (SD), and the remainder experienced PD after several months [70]. In phase 1 studies, DNMT inhibitors CC-486 (oral azacitidine) and azacitidine rendered chemotherapy-resistant DLBCLs sensitive to CHOP [71, 72]. In 26 participants with R/R DLBCL eligible for high-dose therapy, azacitidine followed by vorinostat in combination with gemcitabine, busulfan, and melphalan as second-line therapy yielded an objective response rate (ORR) of 78% and a complete response (CR) rate of 55% [32]. Common AEs reported with this regimen include mucositis, dermatitis, and transient hyperbilirubinemia, which resolved after 1 week on treatment [32,33,34,35, 38, 39, 73,74,75,76,77,78,79,80].
Enhancer of zeste homolog 2 inhibitors
In early clinical trials, tazemetostat, an EZH2 inhibitor that also reduces methyltransferase activity in EZH2 mutant and wild-type FL [81], produced CR rates of 38% in participants with NHL [82] and 33% in participants with R/R DLBCL [83]. In a phase 2 trial in 99 participants with R/R FL, those with wild-type EZH2 FL (n = 54) had an ORR of 35% and participants with mutant EZH2 FL (n = 45) had an ORR of 69%. Durations of response in wild-type EZH2 FL were 13.0 months and 10.9 months in the mutant EZH2 FL group [33]. In 2020, tazemetostat received accelerated regulatory approval from the FDA for treatment of R/R FL. Grade ≥ 3 AEs associated with tazemetostat were low and included thrombocytopenia (3%), neutropenia (3%), and anemia (2%) [33]. By contrast, grade 3–4 AE rates of > 30% for thrombocytopenia were reported with other classes of epigenetic agents [79, 80, 84]. Following its approval as monotherapy, tazemetostat is undergoing evaluation in combination with rituximab (NCT04762160), in combination with lenalidomide and rituximab (NCT04224493) for treatment of R/R FL, and in combination with prednisolone for treatment of R/R DLBCL (NCT01897571).
Another EZH2 inhibitor with reported clinical data is valemetostat, an oral dual inhibitor of EZH2 and enhancer of zeste homolog 1 (another methyltransferase) [85]. An ORR of 53% was achieved in the first-in-human clinical trial of 15 participants with B or T cell lymphoma [38, 63]. Several other EZH2 inhibitors are in ongoing clinical studies for treatment of NHL and include CPI-0209 (NCT04104776), HH2853 (NCT04390737), and PF-06821497 (NCT03460977; Table 3) [86, 87].
Protein arginine methyltransferase inhibitors
Three PRMT5 inhibitors—GSK3326595, JNJ-64619178, and PRT811—are in clinical development. GSK3326595 is being evaluated in a dose-escalation study of patients with solid tumors and NHL (NCT02783300). JNJ-64619178 is being studied in an ongoing phase 1 trial (NCT03573310) in which it induced partial responses and SD in participants with NHL and solid tumors [73]. PRT811 is being studied in a phase 1 trial for treatment of approximately 75 participants with either central nervous system lymphomas, advanced solid tumors, or recurrent high-grade gliomas (NCT04089449). Of the 54 patients enrolled in the JNJ-64619178 trial, preliminary clinical results indicate that 20% experienced grade ≥ 3 thrombocytopenia, 17% experienced grade ≥ 3 anemia, and 6% experienced grade ≥ 3 neutropenia [73].
Histone deacetylase inhibitors
First-generation HDAC inhibitors such as vorinostat are nonselective toward the 4 classes of HDAC enzymes, but selective HDAC inhibitors are being developed as a promising treatment class that may result in fewer off-target effects than pan-HDAC inhibitors [88].
Monotherapy with HDAC inhibitors has demonstrated modest clinical activity in several studies [34, 35, 74, 76, 79]. Vorinostat, an inhibitor of class 1/2 HDAC enzymes, was tested as a monotherapy in a phase 2 study of patients with relapsed DLBCL, but 16 of 18 enrolled patients experienced PD [74]. By contrast, vorinostat monotherapy produced an ORR of 47% to 49% in participants with FL and an ORR of 22% in participants with marginal zone lymphoma (n = 9) [34, 35]. None of the participants with mantle cell lymphoma in either study (n = 4 and n = 9) achieved a clinical response with vorinostat monotherapy. The most common grade 3/4 AE associated with vorinostat was thrombocytopenia [34, 35, 74]. Another HDAC inhibitor, mocetinostat, was tested in a phase 2 study of patients with R/R DLBCL and FL, but the drug failed to reach the threshold for clinical efficacy (> 20% ORR) [89]. Abexinostat, a pan-HDAC inhibitor, was clinically active as monotherapy in a phase 2 study of patients with FL (ORR, 56%) or DLBCL (ORR, 31%) [76]. Similar to vorinostat, the most common grade 3/4 AEs were thrombocytopenia (80%) and neutropenia (27%) [76].
Fimepinostat, a first-in-class, dual-target inhibitor of phosphatidylinositol 3-kinase (PI3K) class I and pan-HDAC enzymes, achieved an ORR of 37% when administered as monotherapy in 25 participants with R/R DLBCL [79]. Of these participants, 36% experienced grade ≥ 3 thrombocytopenia and 16% experienced grade ≥ 3 neutropenia, resulting in a safety profile comparable with other HDAC inhibitors [79]. The FDA granted fimepinostat fast-track status in 2018 for treatment of R/R DLBCL [29].
Most HDAC inhibitors have low responses in B cell lymphomas when used as monotherapy, but they demonstrate synergy with other drugs; however, this synergy is tempered by poor safety profiles. Vorinostat in combination with rituximab or rituximab plus cyclophosphamide, etoposide, and prednisone achieved an ORR of 41% to 57% in participants with R/R B cell NHL, including those with DLBCL. The most frequent grade ≥ 3 AEs included lymphopenia (25–90%), fatigue (14–32%), and lowered platelet (18–41%) and neutrophil (11–52%) counts [36, 37]. In another phase 1/2 study, vorinostat in combination with rituximab plus CHOP (R-CHOP) achieved an ORR of 81% in participants with R/R DLBCL (n = 63), but participants assigned to the study combination had a high incidence of grade ≥ 3 neutropenia (63%), thrombocytopenia (36%), and sepsis (19%) that led investigators to recommend against general clinical use of vorinostat with R-CHOP [90]. Vorinostat in combination with rituximab, ifosfamide, carboplatin, and etoposide for treatment of R/R NHL demonstrated efficacy in DLBCL (ORR, 67%; n/N = 4/6), mantle cell lymphoma (ORR, 60%; n/N = 3/5), and FL (ORR, 100%; n/N = 3/3). The most common grade ≥ 3 AEs at the maximum tolerated dose included hypophosphatemia (27%), febrile neutropenia (27%), and infection (27%) [91]. Abexinostat is being studied in combination with ibrutinib in a phase 1 trial of patients with DLBCL or mantle cell lymphoma (NCT03939182). Key AEs associated with HDAC inhibitors in patients with B cell lymphomas include grade ≥ 3 fatigue, neutropenia, and thrombocytopenia (which can affect ≥ 30% of patients), and gastrointestinal issues (e.g., diarrhea, dehydration, anorexia) [88, 92].
Bromodomain and extraterminal domain inhibitors
Bromodomain and extraterminal domain inhibitors that target BRD2, BRD3, and BRD4 have been studied in the clinical setting. A phase 1 study of birabresib, a BRD2/BRD3/BRD4 inhibitor, reported responses in 3 of 22 patients with DLBCL whose disease progressed on other treatments. However, because of toxicities (e.g., thrombocytopenia) associated with the chosen study drug dose, a lower dose was selected for additional studies [84].
Responses with other BET inhibitors were also disappointing. In a phase 1/2 study, INCB057643 generated an ORR of 33% in patients with R/R FL (n/N = 1/3) [93]. BAY 1238097 was ineffective against refractory malignancies of any type, and its trial was halted due to toxicity issues and lack of efficacy [94]. Interim results from a phase 1 study of molibresib, another BET inhibitor tested in patients with NHL [63, 80], found that 70% of participants (n/N = 19/27) experienced grade ≥ 3 thrombocytopenia [80]. In addition to thrombocytopenia, gastrointestinal toxicity and diarrhea are commonly reported nonhematologic AEs in patients receiving BET inhibitors [80, 84, 95,96,97].
Interim results from a phase 1 study of 44 participants showed that treatment with CPI-0610 achieved CRs in 3 of 24 participants with R/R DLBCL and 1 partial response in 8 participants with R/R FL. Eleven participants with R/R lymphomas showed ongoing partial responses (n = 5) or SD (n = 6) [97]. One participant developed grade 4 thrombocytopenia, and another developed grade 3 diarrhea.
Hodgkin lymphoma
DNA methyltransferase inhibitors
A small clinical study that included 8 patients with HL examined the efficacy of azacitidine followed by vorinostat with chemotherapy (gemcitabine, busulfan, and melphalan) as second-line therapy [32]. This combination yielded CRs in 7 of 8 participants with HL [32]. Furthermore, event-free and overall survival rates were high (76% and 95%, respectively) after a median follow-up period of 15 months. However, all participants developed neutropenic fever [32]. In addition, an ongoing phase 1 study is evaluating azacitidine followed by tumor assisted antigen-specific cytotoxic T cell lymphocytes in patients with HL and NHL (NCT01333046).
Histone deacetylase inhibitors
Several HDAC inhibitors have been tested as monotherapies in patients with R/R HL in clinical trials, including panobinostat [98], vorinostat (NCT00132028), givinostat (NCT00496431), resminostat (NCT01037478), mocetinostat (NCT00358982 [trial terminated]), abexinostat (NCT00724984, NCT01149668), ricolinostat (NCT02091063), entinostat (NCT00866333), and tinostamustine (NCT02576496). Panobinostat produced an ORR of 27% in 129 participants with R/R HL [98]. However, in the other completed or terminated clinical trials, HDAC inhibitors generated relatively low ORRs and comparable progression-free survival versus other targeted therapies or immunomodulatory antibodies that target immune checkpoint pathways such as programmed cell death 1 (PD-1) or its ligand (PD-L1) [42].
Vorinostat is also being evaluated as part of a combination therapy regimen in patients with R/R HL. When combined with the mechanistic target of rapamycin inhibitors everolimus or sirolimus, vorinostat produced moderate ORRs (55% and 33%, respectively) in a dose-escalation study of patients with R/R HL [43]. Key AEs included grade ≥ 3 thrombocytopenia in 67% of participants treated with vorinostat plus everolimus and in 55% of participants treated with vorinostat plus sirolimus [43]. Vorinostat in combination with rituximab plus ifosfamide, carboplatin, and etoposide also demonstrated effectiveness for treatment of patients with R/R HL (ORR, 88%; n/N = 7/8) [91].
T cell lymphomas
DNA methyltransferase inhibitors
The study described earlier [32] with azacitidine followed by vorinostat with chemotherapy as second-line therapy also included 8 patients with R/R peripheral T cell lymphoma (PTCL; n = 3; anaplastic large-cell lymphoma; n = 2 natural killer T cell lymphoma, n = 2; angioimmunoblastic T cell lymphoma, n = 1). The regimen yielded a CR rate of 100% in participants with T cell lymphoma and measurable disease (n/N = 2/2) [32]. A small retrospective series of 12 patients with angioimmunoblastic T cell lymphoma, 11 of whom had R/R disease and 1 who was treatment naive, were treated with azacitidine and experienced a 75% ORR, median progression-free survival of 15 months, and a median overall survival rate of 21 months [99]. Several studies looking at DMNT inhibitors in combination with other treatments are planned or recruiting patients.
Enhancer of zeste homolog 2 inhibitors
Valemetostat achieved an ORR of 80% in early clinical trials among 15 patients with T and B cell lymphoma; however, the study examined 2 patients with adult T cell lymphoma, 2 with angioimmunoblastic T cell lymphoma, and 1 with PTCL not otherwise specified [38]. Key AEs included decreased platelet count (73%), anemia (47%), decreased lymphocyte count (40%), dysgeusia (47%), and diarrhea (27%) [38].
Histone deacetylase inhibitors
Several nonselective HDAC inhibitors have been studied as monotherapies for treatment of T cell lymphomas. Abexinostat produced an ORR of 40% in a phase 2 study of 15 participants with T cell lymphomas [76]. Oral vorinostat yielded an ORR of 24% to 30% in phase 2 studies in participants with refractory and progressive cutaneous T cell lymphoma (CTCL) and was approved for treatment of CTCL by the FDA in 2006 [39, 75]. Panobinostat, a pan-HDAC inhibitor, produced an ORR of 67% in participants with advanced CTCL (n/N = 6/10) when administered as oral monotherapy [78]; however, in a larger phase 2 cohort of 139 participants with refractory CTCL, the ORR was 17% [77]. Romidepsin, an intravenously administered selective HDAC class 1 inhibitor, produced an ORR of 33% to 41% in patients with CTCL [100,101,102]. In patients with CTCL, the most common grade 3/4 toxicities associated with panobinostat with or without abexinostat were thrombocytopenia (20–80%) and neutropenia (9–27%) [76,77,78]. However, grade 3/4 AE rates were lower with vorinostat: thrombocytopenia (5–19%), anemia (1–8%), and fatigue (5%) [39, 75].
Histone deacetylase inhibitors have also been tested as monotherapies for treatment of R/R PTCL, although the reported response rates were modest. Belinostat, a pan-HDAC inhibitor, demonstrated an ORR of 26% in participants with R/R PTCL (n/N = 31/120) [103] and an ORR of 46% in participants with R/R angioimmunoblastic T cell lymphoma (n/N = 10/22) [104]. Romidepsin produced an ORR of 25% in patients with R/R PTCL (n = 130) [40, 105]. After demonstrating clinical efficacy in phase 2 studies [102, 106], romidepsin was approved for treatment of R/R CTCL by the FDA in 2009 and for R/R PTCL in 2011, although the company withdrew the PTCL indication in 2021 owing to lack of efficacy in subsequent phase 3 trials [27, 28, 107]. Chidamide, a selective HDAC class 1 inhibitor, achieved an ORR of 39% when administered as oral monotherapy in 256 participants with R/R PTCL [108]. As with the other HDAC inhibitors discussed, hematologic events were the most common grade 3/4 AEs, with event rates generally below 30% [40, 102, 103, 106, 108].
As with other classes of epigenetic agents, HDAC inhibitors demonstrate slightly higher clinical activity in patients with T cell lymphomas in combination than when administered as monotherapies. As combination therapy with CHOP, vorinostat achieved an ORR of 100% in 12 participants with untreated PTCL [109]. Chidamide demonstrated an ORR of 51% when combined with chemotherapy in 127 participants with R/R PTCL [108]. Panobinostat in combination with bortezomib produced an ORR of 43% in participants with R/R PTCL (n/N = 10/23) [110]. Romidepsin combined with the antimetabolite pralatrexate demonstrated an ORR of 71% in a phase 1 study in participants with R/R PTCL [41]. Romidepsin in combination with oral azacitidine achieved an ORR of 61% in participants with R/R PTCL (n/N = 15/25) [111]. Key grade ≥ 3 AEs associated with HDAC inhibitors when used as combination therapy include thrombocytopenia (48%), neutropenia (40%), lymphopenia (32%), and anemia (16%) [111].
Future directions
Although several classes of epigenetic treatments have shown moderate antitumor activity as monotherapies, combination regimens with chemotherapy generally had better clinical activity than monotherapy (Table 2). The success of PRMT5 inhibitors (GSK3326595 [112, 113], JNJ-64619178 [114], and PRT811 [115]) and KDM5 inhibitors [116] in preclinical and early phase studies may lead to the development of new classes of selective epigenetic therapies. Possible future combination therapies could include the EZH2 inhibitor tazemetostat and chemotherapies or antibodies. Combination of the HDAC inhibitor vorinostat with phosphatidylinositol 3-kinase inhibitors has demonstrated antitumor effects in preclinical studies with NHL cells [117]. DNA methyltransferase inhibitors have been shown to resensitize CHOP-resistant DLBCL to chemotherapy, and other epigenetic therapies may exploit similar mechanisms [71, 72]; for example, BET inhibitors have shown modest efficacy as monotherapy for treatment of B cell lymphomas [93, 97], but future studies of these inhibitors in combination with chemotherapy may allow higher rates of efficacy at lower doses to reduce the severity of clinical effects.
Studies are also beginning to show that epigenetic modulators can impact lymphoma therapy through promotion of antitumor immunity [118]. In the future, epigenetic therapy is likely to be part of a combination approach using multiple classes of treatment to simultaneously overcome drug resistance mechanisms and boost the patient’s immune system.
Many epigenetic therapies could be more successful in the clinical setting if they were individualized to patient biomarkers. An example of this is the difference in response rates between patients with wild-type and mutant EZH2 FL treated with the EZH2 inhibitor tazemetostat (ORRs of 35% and 69%, respectively [33]), findings that suggest additional research to uncover epigenetic biomarkers is needed to identify patients more likely to benefit from these agents. As such, investigators should consider including epigenetic biomarker end points in their clinical trial designs.
Conclusions
Older classes of epigenetic therapies, such as pan-HDAC inhibitors, are associated with high rates of toxicity and poor target selectivity, but newer classes, such as EZH2 inhibitors, have higher selectivity and better safety profiles and are being tested in a variety of lymphomas. By offering potential synergies with chemotherapies, kinase inhibitors, and antibodies, epigenetic agents can overcome chemoresistance and improve outcomes for patients with lymphomas, while their strong target selectivity can reduce the AEs associated with early epigenetic therapies.
Understanding the distinct mechanisms of emerging epigenetic therapies and the patient subpopulations they are most likely to benefit is key to their clinical implementation for treatment of lymphomas. The diversity of epigenetic therapies allows tailoring treatments to an individual patient’s tumor characteristics and needs and has the potential to greatly improve patient survival and quality of life.
Availability of data and materials
Not applicable.
References
Thandra KC, Barsouk A, Saginala K, Padala SA, Barsouk A, Rawla P. Epidemiology of non-Hodgkin's lymphoma. Med Sci. 2021;9.
Hodgkin lymphoma statistics. American Cancer Society Cancer Statistics Center, 2021. Available at: https://cancerstatisticscenter.cancer.org/?_ga=2.108556481.219238712.1625489148-2120540464.1618477006#!/cancer-site/Hodgkin%20lymphoma. Accessed 13 Aug 2021.
Survival rates and factors that affect prognosis (outlook) for non-Hodgkin lymphoma. American Cancer Society, 2022. Available at: https://www.cancer.org/cancer/non-hodgkin-lymphoma/detection-diagnosis-staging/factors-prognosis.html. Accessed 27 Jan 2023.
Baudino TA. Targeted cancer therapy: the next generation of cancer treatment. Curr Drug Discov Technol. 2015;12:3–20.
Chemotherapy side effects. National Health Service, 2020. Available at: https://www.nhs.uk/conditions/chemotherapy/side-effects/. Accessed 1 Feb 2023.
Di M, Huntington SF, Olszewski AJ. Challenges and opportunities in the management of diffuse large B-cell lymphoma in older patients. Oncologist. 2021;26:120–32.
Bezombes C, Pérez-Galán P. Immunotherapies in non-Hodgkin’s lymphoma. Cancers. 2021;13:3625.
Chao MP. Treatment challenges in the management of relapsed or refractory non-Hodgkin’s lymphoma - novel and emerging therapies. Cancer Manag Res. 2013;5:251–69.
Rituxan [package insert]. South San Francisco, CA: Genentech; 2021.
Martin A, Conde E, Arnan M, et al. R-ESHAP as salvage therapy for patients with relapsed or refractory diffuse large B-cell lymphoma: the influence of prior exposure to rituximab on outcome. A GEL/TAMO study. Haematologica. 2008;93:1829–36.
Marcus R, Imrie K, Belch A, et al. CVP chemotherapy plus rituximab compared with CVP as first-line treatment for advanced follicular lymphoma. Blood. 2005;105:1417–23.
Morschhauser F, Fowler NH, Feugier P, et al. Rituximab plus lenalidomide in advanced untreated follicular lymphoma. N Engl J Med. 2018;379:934–47.
Witzig TE, Nowakowski GS, Habermann TM, et al. A comprehensive review of lenalidomide therapy for B-cell non-Hodgkin lymphoma. Ann Oncol. 2015;26:1667–77.
Treanda [package insert]. North Wales, PA: Teva Pharmaceuticals; 2019.
Morrison VA, Shou Y, Bell JA, et al. Treatment patterns and survival outcomes in patients with follicular lymphoma: a 2007 to 2015 Humedica Database Study. Clin Lymphoma Myeloma Leuk. 2019;19:e172–83.
Davis TA, Grillo-López AJ, White CA, et al. Rituximab anti-CD20 monoclonal antibody therapy in non-Hodgkin’s lymphoma: safety and efficacy of re-treatment. J Clin Oncol. 2000;18:3135–43.
Wang L, Qin W, Huo YJ, et al. Advances in targeted therapy for malignant lymphoma. Signal Transduct Target Ther. 2020;5:15.
Marcus R, Davies A, Ando K, et al. Obinutuzumab for the first-line treatment of follicular lymphoma. N Engl J Med. 2017;377:1331–44.
Widakowich C, de Castro G Jr, de Azambuja E, Dinh P, Awada A. Review: side effects of approved molecular targeted therapies in solid cancers. Oncologist. 2007;12:1443–55.
Goldman JW, Mendenhall MA, Rettinger SR. Hyperglycemia associated with targeted oncologic treatment: mechanisms and management. Oncologist. 2016;21:1326–36.
Hanlon A, Brander DM. Managing toxicities of phosphatidylinositol-3-kinase (PI3K) inhibitors. Hematol Am Soc Hematol Educ Program. 2020;2020:346–56.
Wang X, Wu S, Chen Y, et al. Fatal adverse events associated with programmed cell death ligand 1 inhibitors: a systematic review and meta-analysis. Front Pharmacol. 2020;11:5.
Waldman AD, Fritz JM, Lenardo MJ. A guide to cancer immunotherapy: from T cell basic science to clinical practice. Nat Rev Immunol. 2020;20:651–68.
Azad N, Zahnow CA, Rudin CM, Baylin SB. The future of epigenetic therapy in solid tumours–lessons from the past. Nat Rev Clin Oncol. 2013;10:256–66.
Feng S, De Carvalho DD. Clinical advances in targeting epigenetics for cancer therapy. FEBS J. 2021;289:1214–39.
Tazverik [package insert]. Cambridge, MA: Epizyme; 2020.
FDA grants accelerated approval of ISTODAX as treatment for patients with peripheral T-cell lymphoma who have received at least one prior therapy. Celgene, 2011. Available at: https://s24.q4cdn.com/483522778/files/doc_news/archive/798164.pdf. Accessed 13 Aug 2021.
Istodax [package insert]. Summit, NJ: Celgene Corporation; 2021.
Fimepinostat. Curis, Inc., 2021. Available at: https://www.curis.com/pipeline/fimepinostat/. Accessed: August 13, 2021.
Zolinza [package insert]. Whitehouse station, NJ: Merck & Co., Inc.; 2020.
Blum KA, Liu Z, Lucas DM, et al. Phase I trial of low dose decitabine targeting DNA hypermethylation in patients with chronic lymphocytic leukaemia and non-Hodgkin lymphoma: dose-limiting myelosuppression without evidence of DNA hypomethylation. Br J Haematol. 2010;150:189–95.
Nieto Y, Valdez BC, Thall PF, et al. Double epigenetic modulation of high-dose chemotherapy with azacitidine and vorinostat for patients with refractory or poor-risk relapsed lymphoma. Cancer. 2016;122:2680–8.
Morschhauser F, Tilly H, Chaidos A, et al. Tazemetostat for patients with relapsed or refractory follicular lymphoma: an open-label, single-arm, multicentre, phase 2 trial. Lancet Oncol. 2020;21:1433–42.
Kirschbaum M, Frankel P, Popplewell L, et al. Phase II study of vorinostat for treatment of relapsed or refractory indolent non-Hodgkin’s lymphoma and mantle cell lymphoma. J Clin Oncol. 2011;29:1198–203.
Ogura M, Ando K, Suzuki T, et al. A multicentre phase II study of vorinostat in patients with relapsed or refractory indolent B-cell non-Hodgkin lymphoma and mantle cell lymphoma. Br J Haematol. 2014;165:768–76.
Chen R, Frankel P, Popplewell L, et al. A phase II study of vorinostat and rituximab for treatment of newly diagnosed and relapsed/refractory indolent non-Hodgkin lymphoma. Haematologica. 2015;100:357–62.
Straus DJ, Hamlin PA, Matasar MJ, et al. Phase I/II trial of vorinostat with rituximab, cyclophosphamide, etoposide and prednisone as palliative treatment for elderly patients with relapsed or refractory diffuse large B-cell lymphoma not eligible for autologous stem cell transplantation. Br J Haematol. 2015;168:663–70.
Maruyama D, Tobinai K, Makita S, et al. First-in-human study of the EZH1/2 dual inhibitor DS-3201b in patients with relapsed or refractory non-Hodgkin lymphomas — preliminary results [abstract]. Blood. 2017;130:4070.
Olsen EA, Kim YH, Kuzel TM, et al. Phase IIb multicenter trial of vorinostat in patients with persistent, progressive, or treatment refractory cutaneous T-cell lymphoma. J Clin Oncol. 2007;25:3109–15.
Coiffier B, Pro B, Prince HM, et al. Results from a pivotal, open-label, phase II study of romidepsin in relapsed or refractory peripheral T-cell lymphoma after prior systemic therapy. J Clin Oncol. 2012;30:631–6.
Amengual JE, Lichtenstein R, Lue J, et al. A phase 1 study of romidepsin and pralatrexate reveals marked activity in relapsed and refractory T-cell lymphoma. Blood. 2018;131:397–407.
Chen IC, Sethy B, Liou JP. Recent update of HDAC inhibitors in lymphoma. Front Cell Dev Biol. 2020;8:576391.
Janku F, Park H, Call SG, et al. Safety and efficacy of vorinostat plus sirolimus or everolimus in patients with relapsed refractory Hodgkin lymphoma. Clin Cancer Res. 2020;26:5579–87.
Zhang J, Yang C, Wu C, Cui W, Wang L. DNA methyltransferases in cancer: biology, paradox, aberrations, and targeted therapy. Cancers. 2020;12.
Tobiasson M, Abdulkadir H, Lennartsson A, et al. Comprehensive mapping of the effects of azacitidine on DNA methylation, repressive/permissive histone marks and gene expression in primary cells from patients with MDS and MDS-related disease. Oncotarget. 2017;8:28812–25.
Giri AK, Aittokallio T. DNMT inhibitors increase methylation in the cancer genome. Front Pharmacol. 2019;10:385.
Hoang NM, Rui L. DNA methyltransferases in hematological malignancies. J Genet Genom. 2020;47:361–72.
Sarkar S, Goldgar S, Byler S, Rosenthal S, Heerboth S. Demethylation and re-expression of epigenetically silenced tumor suppressor genes: sensitization of cancer cells by combination therapy. Epigenomics. 2013;5:87–94.
Song Y, Wu F, Wu J. Targeting histone methylation for cancer therapy: enzymes, inhibitors, biological activity and perspectives. J Hematol Oncol. 2016;9:49.
Zhao Z, Shilatifard A. Epigenetic modifications of histones in cancer. Genome Biol. 2019;20:245.
Dimopoulos K, Søgaard Helbo A, Fibiger Munch-Petersen H, et al. Dual inhibition of DNMTs and EZH2 can overcome both intrinsic and acquired resistance of myeloma cells to IMiDs in a cereblon-independent manner. Mol Oncol. 2018;12:180–95.
Herviou L, Kassambara A, Boireau S, et al. Targeting EZH2 in multiple myeloma could be promising for a subgroup of MM patients in combination with IMiDs [abstract 311]. Blood. 2016;128:311.
Morschhauser F, Salles G, Batlevi CL, et al. Taking the EZ way: targeting enhancer of zeste homolog 2 in B-cell lymphomas. Blood Rev. 2022;56:100988.
Béguelin W, Popovic R, Teater M, et al. EZH2 is required for germinal center formation and somatic EZH2 mutations promote lymphoid transformation. Cancer Cell. 2013;23:677–92.
Lee CH, Holder M, Grau D, et al. Distinct stimulatory mechanisms regulate the catalytic activity of polycomb repressive complex 2. Mol Cell. 2018;70:435-48.e5.
Béguelin W, Teater M, Meydan C, et al. Mutant EZH2 induces a pre-malignant lymphoma niche by reprogramming the immune response. Cancer Cell. 2020;37:655-73.e11.
Béguelin W, Teater M, Gearhart MD, et al. EZH2 and BCL6 cooperate to assemble CBX8-BCOR complex to repress bivalent promoters, mediate germinal center formation and lymphomagenesis. Cancer Cell. 2016;30:197–213.
Kim HJ, Cantor H, Cosmopoulos K. Overcoming immune checkpoint blockade resistance via EZH2 inhibition. Trends Immunol. 2020;41:948–63.
Kim H, Ronai ZA. PRMT5 function and targeting in cancer. Cell Stress. 2020;4:199–215.
Litzler LC, Zahn A, Meli AP, et al. PRMT5 is essential for B cell development and germinal center dynamics. Nat Commun. 2019;10:22.
Bochyńska A, Lüscher-Firzlaff J, Lüscher B. Modes of interaction of KMT2 histone H3 lysine 4 methyltransferase/COMPASS complexes with chromatin. Cells. 2018;7:17.
Liu MK, Sun XJ, Gao XD, Qian Y, Wang L, Zhao WL. Methylation alterations and advance of treatment in lymphoma. Front Biosci. 2021;26:602–13.
Sermer D, Pasqualucci L, Wendel HG, Melnick A, Younes A. Emerging epigenetic-modulating therapies in lymphoma. Nat Rev Clin Oncol. 2019;16:494–507.
Lai AY, Fatemi M, Dhasarathy A, et al. DNA methylation prevents CTCF-mediated silencing of the oncogene BCL6 in B cell lymphomas. J Exp Med. 2010;207:1939–50.
Li G, Tian Y, Zhu WG. The roles of histone deacetylases and their inhibitors in cancer therapy. Front Cell Dev Biol. 2020;8:576946.
Plch J, Hrabeta J, Eckschlager T. KDM5 demethylases and their role in cancer cell chemoresistance. Int J Cancer. 2019;144:221–31.
Shi J, Vakoc CR. The mechanisms behind the therapeutic activity of BET bromodomain inhibition. Mol Cell. 2014;54:728–36.
Dacogen FDA approval history. Drugs.com, 2010. Available at: https://www.drugs.com/history/dacogen.html. Accessed 13 Aug 2021.
Dacogen overview. European Medicines Agency, 2016. Available at: https://www.ema.europa.eu/en/medicines/human/EPAR/dacogen#authorisation-details-section. Accessed: August 13, 2021.
Fan H, Lu X, Wang X, et al. Low-dose decitabine-based chemoimmunotherapy for patients with refractory advanced solid tumors: a phase I/II report. J Immunol Res. 2014;2014:371087.
Martin P, Bartlett NL, Rivera IIR, et al. A phase I, open label, multicenter trial of oral azacitidine (CC-486) plus R-CHOP in patients with high-risk, previously untreated diffuse large B-cell lymphoma, grade 3B follicular lymphoma, or transformed lymphoma [abstract]. Blood. 2017;130:192.
Clozel T, Yang S, Elstrom RL, et al. Mechanism-based epigenetic chemosensitization therapy of diffuse large B-cell lymphoma. Cancer Discov. 2013;3:1002–19.
Villar MV, Spreafico A, Moreno V, et al. 537MO First-in-human study of JNJ-64619178, a protein arginine methyltransferase 5 (PRMT5) inhibitor, in patients with advanced cancers [abstract]. Ann Oncol. 2020;31:S470.
Crump M, Coiffier B, Jacobsen ED, et al. Phase II trial of oral vorinostat (suberoylanilide hydroxamic acid) in relapsed diffuse large-B-cell lymphoma. Ann Oncol. 2008;19:964–9.
Duvic M, Talpur R, Ni X, et al. Phase 2 trial of oral vorinostat (suberoylanilide hydroxamic acid, SAHA) for refractory cutaneous T-cell lymphoma (CTCL). Blood. 2007;109:31–9.
Ribrag V, Kim WS, Bouabdallah R, et al. Safety and efficacy of abexinostat, a pan-histone deacetylase inhibitor, in non-Hodgkin lymphoma and chronic lymphocytic leukemia: results of a phase II study. Haematologica. 2017;102:903–9.
Duvic M, Dummer R, Becker JC, et al. Panobinostat activity in both bexarotene-exposed and -naïve patients with refractory cutaneous T-cell lymphoma: results of a phase II trial. Eur J Cancer. 2013;49:386–94.
Ellis L, Pan Y, Smyth GK, et al. Histone deacetylase inhibitor panobinostat induces clinical responses with associated alterations in gene expression profiles in cutaneous T-cell lymphoma. Clin Cancer Res. 2008;14:4500–10.
Oki Y, Kelly KR, Flinn I, et al. CUDC-907 in relapsed/refractory diffuse large B-cell lymphoma, including patients with MYC-alterations: results from an expanded phase I trial. Haematologica. 2017;102:1923–30.
Dickinson M, Kamdar M, Huntly BJP, et al. A phase I study of molibresib (GSK525762), a selective bromodomain (BRD) and extra terminal protein (BET) inhibitor: results from part 1 of a phase I/II open label single agent study in subjects with non-Hodgkin’s lymphoma (NHL) [abstract]. Blood. 2018;132:1682.
Knutson SK, Kawano S, Minoshima Y, et al. Selective inhibition of EZH2 by EPZ-6438 leads to potent antitumor activity in EZH2-mutant non-Hodgkin lymphoma. Mol Cancer Ther. 2014;13:842–54.
Italiano A, Soria JC, Toulmonde M, et al. Tazemetostat, an EZH2 inhibitor, in relapsed or refractory B-cell non-Hodgkin lymphoma and advanced solid tumours: a first-in-human, open-label, phase 1 study. Lancet Oncol. 2018;19:649–59.
Munakata W, Shirasugi Y, Tobinai K, et al. Phase 1 study of tazemetostat in Japanese patients with relapsed or refractory B-cell lymphoma. Cancer Sci. 2021;112:1123–31.
Amorim S, Stathis A, Gleeson M, et al. Bromodomain inhibitor OTX015 in patients with lymphoma or multiple myeloma: a dose-escalation, open-label, pharmacokinetic, phase 1 study. Lancet Haematol. 2016;3:e196-204.
Yamagishi M, Hori M, Fujikawa D, et al. Targeting excessive EZH1 and EZH2 activities for abnormal histone methylation and transcription network in malignant lymphomas. Cell Rep. 2019;29:2321-37.e7.
Batlevi CL, Park SI, Phillips T, et al. Interim analysis of the randomized phase 1b/3 study evaluating the safety and efficacy of tazemetostat plus lenalidomide and rituximab in patients with relapsed/refractory follicular lymphoma [poster 2207]. Presented at: Annual Meeting and Exposition of the American Society of Hematology; 2021.
Patel K, Bailey N, Miller K, et al. Trial in progress: SYMPHONY-2, a phase 2, single-arm, open-label, multicenter study of tazemetostat in combination with rituximab for the treatment of relapsed or refractory follicular lymphoma [poster 3541]. Presented at: Annual Meeting and Exposition of the American Society of Hematology; 2021.
Yang F, Zhao N, Ge D, Chen Y. Next-generation of selective histone deacetylase inhibitors. RSC Adv. 2019;9:19571–83.
Batlevi CL, Crump M, Andreadis C, et al. A phase 2 study of mocetinostat, a histone deacetylase inhibitor, in relapsed or refractory lymphoma. Br J Haematol. 2017;178:434–41.
Persky DO, Li H, Rimsza LM, et al. A phase I/II trial of vorinostat (SAHA) in combination with rituximab-CHOP in patients with newly diagnosed advanced stage diffuse large B-cell lymphoma (DLBCL): SWOG S0806. Am J Hematol. 2018;93:486–93.
Budde LE, Zhang MM, Shustov AR, et al. A phase I study of pulse high-dose vorinostat (V) plus rituximab (R), ifosphamide, carboplatin, and etoposide (ICE) in patients with relapsed lymphoma. Br J Haematol. 2013;161:183–91.
Subramanian S, Bates SE, Wright JJ, Espinoza-Delgado I, Piekarz RL. Clinical toxicities of histone deacetylase inhibitors. Pharmaceuticals. 2010;3:2751–67.
Forero-Torres A, Rosen S, Smith DC, et al. Preliminary results from an ongoing phase 1/2 study of INCB057643, a bromodomain and extraterminal (BET) protein inhibitor, in patients (pts) with advanced malignancies [abstract]. Blood. 2017;130:4048.
Postel-Vinay S, Herbschleb K, Massard C, et al. First-in-human phase I dose escalation study of the bromodomain and extra-terminal motif (BET) inhibitor BAY 1238097 in subjects with advanced malignancies [abstract]. Eur J Cancer. 2016;69:S7–8.
Sun Y, Han J, Wang Z, Li X, Sun Y, Hu Z. Safety and efficacy of bromodomain and extra-terminal inhibitors for the treatment of hematological malignancies and solid tumors: a systematic study of clinical trials. Front Pharmacol. 2020;11:621093.
Mita MM, Mita AC. Bromodomain inhibitors a decade later: a promise unfulfilled? Br J Cancer. 2020;123:1713–4.
Abramson JS, Blum KA, Flinn IW, et al. BET inhibitor CPI-0610 is well tolerated and induces responses in diffuse large B-cell lymphoma and follicular lymphoma: preliminary analysis of an ongoing phase 1 study [abstract]. Blood. 2015;126:1491.
Younes A, Sureda A, Ben-Yehuda D, et al. Panobinostat in patients with relapsed/refractory Hodgkin’s lymphoma after autologous stem-cell transplantation: results of a phase II study. J Clin Oncol. 2012;30:2197–203.
Lemonnier F, Dupuis J, Sujobert P, et al. Treatment with 5-azacytidine induces a sustained response in patients with angioimmunoblastic T-cell lymphoma. Blood. 2018;132:2305–9.
Bates SE, Eisch R, Ling A, et al. Romidepsin in peripheral and cutaneous T-cell lymphoma: mechanistic implications from clinical and correlative data. Br J Haematol. 2015;170:96–109.
Whittaker SJ, Demierre MF, Kim EJ, et al. Final results from a multicenter, international, pivotal study of romidepsin in refractory cutaneous T-cell lymphoma. J Clin Oncol. 2010;28:4485–91.
Piekarz RL, Frye R, Turner M, et al. Phase II multi-institutional trial of the histone deacetylase inhibitor romidepsin as monotherapy for patients with cutaneous T-cell lymphoma. J Clin Oncol. 2009;27:5410–7.
O’Connor OA, Horwitz S, Masszi T, et al. Belinostat in patients with relapsed or refractory peripheral T-cell lymphoma: results of the pivotal phase II BELIEF (CLN-19) study. J Clin Oncol. 2015;33:2492–9.
Sawas A, Ma H, Shustov A, et al. Belinostat induces high overall response rate (ORR) in patients with relapsed or refractory angioimmunoblastic T-cell lymphoma (AITL) [abstract]. Blood. 2019;134:4050.
Yuan XG, Huang YR, Yu T, Jiang HW, Xu Y, Zhao XY. Chidamide, a histone deacetylase inhibitor, induces growth arrest and apoptosis in multiple myeloma cells in a caspase-dependent manner. Oncol Lett. 2019;18:411–9.
Piekarz RL, Frye R, Prince HM, et al. Phase 2 trial of romidepsin in patients with peripheral T-cell lymphoma. Blood. 2011;117:5827–34.
Bristol Myers Squibb statement on Istodax (romidepsin) relapsed/refractory peripheral T-cell lymphoma U.S. indication [press release]. Bristol Myers Squibb, 2021. Available at: https://news.bms.com/news/corporate-financial/2021/Bristol-Myers-Squibb-Statement-on-Istodax-romidepsin-Relapsed-Refractory-Peripheral-T-cell-Lymphoma-U.S.-Indication/default.aspx. Accessed: September 20, 2021.
Shi Y, Jia B, Xu W, et al. Chidamide in relapsed or refractory peripheral T cell lymphoma: a multicenter real-world study in China. J Hematol Oncol. 2017;10:69.
Oki Y, Younes A, Copeland A, et al. Phase I study of vorinostat in combination with standard CHOP in patients with newly diagnosed peripheral T-cell lymphoma. Br J Haematol. 2013;162:138–41.
Tan D, Phipps C, Hwang WY, et al. Panobinostat in combination with bortezomib in patients with relapsed or refractory peripheral T-cell lymphoma: an open-label, multicentre phase 2 trial. Lancet Haematol. 2015;2:e326–33.
Falchi L, Ma H, Klein S, et al. Combined oral 5-azacytidine and romidepsin are highly effective in patients with PTCL: a multicenter phase 2 study [abstract]. Blood. 2021;137:2161–70.
Protein arginine methyltransferase 5 inhibitor PRT543. National Cancer Institute, National Institutes of Health, 2022. Available at: https://www.cancer.gov/publications/dictionaries/cancer-drug/def/protein-arginine-methyltransferase-5-inhibitor-prt543. Accessed 27 Jan 2023.
Siu LL, Rasco DW, Vinay SP, et al. METEOR-1: a phase I study of GSK3326595, a first-in-class protein arginine methyltransferase 5 (PRMT5) inhibitor, in advanced solid tumours [abstract 4380]. Ann Oncol. 2019;30:v159.
Brehmer D, Beke L, Wu T, et al. Discovery and pharmacological characterization of JNJ-64619178, a novel small-molecule inhibitor of PRMT5 with potent antitumor activity. Mol Cancer Ther. 2021;20:2317–28.
Zhang Y, Lin H, Wang M, et al. Discovery of PRT811, a potent, selective, and orally bioavailable brain penetrant PRMT5 inhibitor for the treatment of brain tumors [abstract 2919]. Cancer Res Rev. 2020;80(suppl 16):2919.
Heward J, Konali L, D’Avola A, et al. KDM5 inhibition offers a novel therapeutic strategy for the treatment of KMT2D mutant lymphomas. Blood. 2021;138:370–81.
Ranganna K, Selvam C, Shivachar A, Yousefipour Z. Histone deacetylase inhibitors as multitarget-directed epi-drugs in blocking PI3K oncogenic signaling: a polypharmacology approach. Int J Mol Sci 2020;21.
Jones PA, Ohtani H, Chakravarthy A, De Carvalho DD. Epigenetic therapy in immune-oncology. Nat Rev Cancer. 2019;19:151–61.
Acknowledgements
Medical writing and editorial support were provided by Claire L. Jarvis, PhD, Duprane Young, PhD, and Sherri Damlo, ELS, of Peloton Advantage, LLC, an OPEN Health company, and funded by Epizyme, Inc, an Ipsen company.
Funding
This study was sponsored by Epizyme, Inc, an Ipsen company. Medical writing and editorial support were provided by Peloton Advantage, LLC, an OPEN Health company, and funded by Epizyme, Inc, an Ipsen company.
Author information
Authors and Affiliations
Contributions
All authors collaborated in the preparation, critical review, and revision of this manuscript. All authors granted final approval of the manuscript for submission.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Competing interests
Allison C. Rosenthal has nothing to disclose. Javier L. Munoz has served as a consultant for Abbvie/Pharmacyclics, ADC Therapeutics, Alexion, Bayer, BeiGene, Bristol Myers Squibb, Debiopharm, Epizyme, Inc, an Ipsen company, Fosunkite, Genmab, Gilead/Kite Pharma, Innovent, Janssen, Juno/Celgene, Karyopharm, Kyowa, Seagen, and Servier; has received research funding from Bayer, Celgene, Genentech, Gilead/Kite Pharma, Incyte, Janssen, Merck, Millennium, Pharmacyclics, Portola, and Seagen; has received honoraria from Curio, Kyowa, OncView, Physicians’ Education Resource, Seagen, and Targeted Oncology; and has served on speakers’ bureaus for Acrotech/Aurobindo, AstraZeneca, Bayer, BeiGene, Celgene/Bristol Myers Squibb, Genentech/Roche, Gilead/Kite Pharma, Kyowa, Pharmacyclics/Janssen, Seagen, and Verastem. J. C. Villasboas has received institutional funds from Epizyme, Inc, an Ipsen company, and acted as a principal investigator on a clinical trial for Epizyme, Inc, an Ipsen company.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Rosenthal, A.C., Munoz, J.L. & Villasboas, J.C. Clinical advances in epigenetic therapies for lymphoma. Clin Epigenet 15, 39 (2023). https://doi.org/10.1186/s13148-023-01452-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s13148-023-01452-6