Abstract
Patient-reported outcomes (PROs) reflect the patient’s perspective and are used in rheumatoid arthritis (RA) routine clinical practice. Patient global assessment (PGA) is one of the most widely used PROs in RA practice and research and is included in several composite scores such as the 28-joint Disease Activity Score (DAS28). PGA is often assessed by a single question with a 0–10 or 0–100 response. The content can vary and relates either to global health (e.g., how is your health overall) or to disease activity (e.g., how active is your arthritis). The wordings used as anchors, i.e., for the score of 0, 10, or 100 according to the scale used, and the timing (i.e., this day or this week) also vary. The different possible ways of measuring PGA translate into variations in its interpretation and reporting and may impact on measures of disease activity and consequently achievement of treat-to-target goals. Furthermore, although PGA is associated with objective measures of disease activity, it is also associated with other aspects of health, such as psychological distress or comorbidities, which leads to situations of discordance between objective RA assessments and PGA. Focusing on the role of PGA, its use and interpretation in RA, this review explores its validity and correlations with other disease measures and its overall value for research and routine clinical practice.
Similar content being viewed by others
Background
Patient-reported outcomes (PROs) are increasingly recognized for their value in providing the patient’s perspective on aspects of their condition or their overall health status. Their incorporation into clinical practice and in research in rheumatoid arthritis (RA) is widely supported by international organizations and professional bodies [1, 2], including the European Patients’ Academy on Therapeutic Innovations (EUPATI; http://www.patientsacademy.eu/index.php/en/) and the Patient-Centered Outcomes Research Institute (PCORI; http://www.pcori.org/research-results) in the United States, as well as regulatory agencies such as the Food and Drug Administration (http://www.fda.gov/) and the European Medicines Agency (http://www.ema.europa.eu/ema/), all of whom recognize the patient’s unique position in providing direct feedback on their disease.
Patient global assessment (PGA) is one of the most widely reported PROs in RA. The considerable burden of RA on the individual is related to both inflammation and damage but also to broader aspects of disease, including psychological and societal impact. The use of PROs like the widely used Health Assessment Questionnaire (HAQ) or the PGA allows a more holistic assessment of disease beyond objective measures of inflammation or structural damage, such as acute phase reactants or radiographic damage. Experts from the American College of Rheumatology (ACR), the European League Against Rheumatism (EULAR), and the Outcome Measures in Rheumatology Clinical Trials (OMERACT) have endorsed a “core set” of data for use in RA clinical trials which includes PGA [3, 4]. In recent randomized controlled trials and observational studies in RA, PGA has been reported in 49 % of studies, making it the second most frequently collected PRO after physical function (68 %) [5]. PGA is also incorporated into several of the major outcome and disease activity scores in RA, often as the only PRO: these include the ACR/EULAR remission criteria, the 28-joint count Disease Activity Score (DAS28), the Simplified Disease Activity Index (SDAI), the Clinical Disease Activity Index (CDAI), and the Routine Assessment of Patient Index Data (RAPID3).
However, the use of PGA in RA presents many challenges and limitations. The several possible ways of measuring PGA, including the intended assessment or underlying concept (i.e., global health versus disease activity) and variations in wording/phrasing and time period assessed may lead to differences in interpretation of PGA. Discordance with objective RA measures is also an issue that needs to be addressed. The latter is particularly important in the context of treating to target aiming for remission and shared decision-making [6, 7]. What the different formulations of PGA are, their impact, and justifications for their use remain to be clarified.
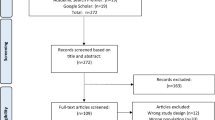
To provide readers with a complete overview regarding PGA in RA, a review of the literature was undertaken based on a hierarchical literature search including hand searches and expert opinion searches covering key publications in the field. The objectives were to explore the value of PGA as an outcome measure in RA, focusing on its psychometric properties (feasibility, validity, reliability, and sensitivity to change). Specifically, this review discusses the validity and impact of different wordings/phrasings and time period assessed as part of PGA on patients’ assessment of disease, as well as discordance between physician global assessment and PGA.
Description and practical application
Concepts behind PGA
PGA was developed in the late 1970s and was initially designed for the measurement of self-assessed pain in RA [8], although it has since been used to evaluate RA more globally. It is interesting to note that the way PGA is used in clinical practice covers, in fact, two very different concepts, one related to global health and the other to overall disease activity. They are both usually used under the heading of PGA without further specification for which is being assessed.
PGA wording and phrasing
It is well-recognized that the wording/specific phrasing used for PROs may result in a varied response [9–12]. In the case of PGA, its exact wording/phrasing was not specified when developed; however, it was suggested that it could be used for two main purposes—either a patient assessment of global health or of disease activity—stemming from the two basic concepts (Table 1) [11, 13]. Over the past years many different wordings/phrasings of PGA have been formulated, covering variations of these two concepts [14–18]. Furthermore, anchor wordings may also vary, e.g., words used to describe the right end of the score (corresponding to scores of 10 or 100) from “worst possible” to “most active” to “very active”, for example.
Although the wording/phrasing of PGA remains unstandardized to date, the ACR/EULAR remission criteria do specifically propose the following phrasing related to disease activity: “Considering all the ways your arthritis has affected you, how do you feel your arthritis is today?” [19].
PGA reference period
Aside from different wording/phrasing used for the question stem, the reference periods to describe the time component (i.e., the period of recall the patient should refer to when answering the question) can also vary (Table 1). As we will see in this review, the different formulations of PGA lead to differences in interpretation.
In the context of a EULAR taskforce to standardize data collection across registries, in 2015 we contacted registries and cohorts across Europe to explore outcomes being assessed: 52 out of 67 (78 %) registries were collecting some form of PGA [20]. The versions of the PGA used varied with regard to the concept, wording/phrasing, and reference period used. More recently, a smaller pilot survey in 2016 (unpublished data) indicated that 6/16 (38 %) cohorts were assessing disease activity-PGA (either related to RA or not specifically related to RA) whereas 6/16 (38 %) were assessing global health PGA and 4/16 (25 %) were assessing both concepts. Some wordings as translated by the investigators are shown in Table 1. With regard to the reference period, 41 % reported “today” as being the time reference used, with the second most common being “last week” (35 %).
PGA scoring
Depending on the type of score used, the PGA can range from 0–100 mm, although is often reported from 0–10 cm. Higher scores represent a higher level of disease activity or a worse global health. The proposed definition of “low global assessment” is ≤2.0 (scale 0–10) [21].
PGA may be scored using a numeric rating scale (NRS), a verbally administered NRS, or a visual analogue scale (VAS). The PGA-VAS is classically anchored on an unnumbered 10-cm/100-mm horizontal line but may also be administered as a vertical VAS. The VAS may be anchored at the ends (e.g., with defined adjectives at the ends such as best versus worst) or open. Sometimes the PGA is presented with tick marks at periodic intervals or as a VAS consisting of 21 circles at 0.5-mm intervals, the latter shown to be similar to a classic 10/100 scale [22]. In practice, sometimes these exact definitions are not followed (e.g., the line is not 10 cm long or there are not 21 circles evenly spaced) and these technical difficulties may hamper the use of PGA (as is the case with other PROs). A Likert-style scale may also be used, though its metric properties are different.
A study comparing responses to a global health VAS presented both as a 10/100 cm horizontal scale with no incremental markers and as a vertical 20/100 cm VAS with 1-cm markers concluded that different presentation of scales, order effect, and incremental markers can affect scoring [14]. Another study comparing different scaling of PGA revealed similar construct validity for VAS and NRS but higher sensitivity to change of VAS [23]. Although some differences can be seen in scoring methods for PGA, all methods appear at this point similarly valid. We would, however, recommend the use of either an unnumbered horizontal VAS or a numbered horizontal NRS since these formats are the most usual and most used.
Psychometric properties of PGA
The main strengths and weaknesses of PGA are summarized in Table 2. Below, we review each psychometric property of PGA.
Feasibility
Like other PROs, including, for example, the HAQ, PGA is a very feasible measure. PGA is administered as a simple, single-item (with no subscale), patient-completed question measuring the overall way RA affects the patient and/or disease activity at a specific point in time. There is no cost attached to it, it is practical, and can be self-administered. The single question takes only a few seconds to ask, making it feasible in routine clinical settings but also as an end-point in clinical trials in RA and is one of the main strengths of the PGA, making it one of the most frequently reported domains across published RA studies [6].
Face validity
PGA is a global, “gestalt” measure of disease which appears to encompass many aspects of disease which are important for patients. Physicians’ assessment of RA disease activity is mainly driven by objective criteria, i.e., tender/swollen joint counts and level of inflammation, whereas it seems patients place more focus on overall well-being, levels of pain, and health-related quality of life [24]. The latter, in particular, seems to have the greatest relevance and meaning to patients. However, it is often difficult to capture health-related quality of life with simple questionnaires. In this sense, PGA appears of interest since it may summarize in one simple measure many aspects of disease and health which are important to patients.
Although PGA has high face validity (Table 2), it does present some challenges. A major point is the patient’s interpretation of the PGA, both depending on the concept (i.e., global health versus disease activity) and on the patient’s individual comprehension of this broad question. For both concepts behind PGA, a criticism is that the response to the question may both reflect a broad understanding of the patient’s health and also be influenced by a number of factors, making it difficult to discern what aspect of disease contributes to the overall score. Structural damage (related to disease duration) and other aspects of patients’ lives (such as comorbidities or psychological distress) may have an impact on the scoring of PGA [1].
In both cases of PGA (i.e., global health versus disease activity), interpretation of the question by the patient may depend on duration of disease through a “response shift” (i.e., a change in the meaning of a patient’s self-evaluation) resulting from a better knowledge of symptoms and changes in patient expectations [25]. In the current biologic era, however, cumulative damage is considerably lower despite longer disease duration and therefore the effect and meaning of a response shift may have a different interpretation. Differences in patients’ perceptions regarding internal standards, values, or conceptualization of health-related quality of life can result in “ambiguous” or “paradoxical” findings [25]. For example, patients with long-standing disability may report a good or high quality of life (despite what externally might appear paradoxically untrue) due to several factors, such as acceptance and the opportunity to adjust and achieve stability through several transition phases while living with disability. All these factors need to be taken into account when interpreting individuals’ PGA scores.
Reliability
Data on the reliability of PGA, which refers to the reproducibility in a test–retest setting, are reassuring [26–28]. Studies have shown the PGA intraclass correlation coefficient (as a measure of test–retest reliability) to be generally acceptable to high, though lower than ones noted for physician global assessment [29, 30]. The data available in the literature do not allow us to directly compare reliability of PGA–global health versus PGA–disease activity; although when tested separately, both appear to have acceptable reliability.
Sensitivity to change
Sensitivity to change indicates that the measure will improve when the underlying conceptual framework (here, either global health or disease activity) improves. PGA has been shown to be sensitive to change, which makes it a very useful clinical measure in assessing RA, particularly in clinical trials. PGA detects improvement after active treatment better than, for example, tender joint count [31]. Table 3 summarizes key findings in this area. Furthermore, PGA has been shown to discriminate active treatment from placebo in randomized controlled trials, with treatment-associated changes being congruent with measures of inflammation, suggesting close reflection of other criteria related to the RA process, such as joint counts [32].
In support of the above, in an analysis of the efficiencies to distinguish active treatment from control treatments in clinical trials, among the seven RA core set measures, the highest relative efficiencies were for the physician global estimate followed by PGA and physical function [33]. “Objective” measures of disease, such as acute phase reactants and tender and swollen joint counts, were not superior to “subjective” global estimates of the physician or patient self-report measures of physical function or pain to differentiate active from control treatments. These findings challenge the view that laboratory and clinical examination findings are more robust than patient self-report measures in assessing and monitoring disease progression and treatment response in RA [33].
Consequences of different wordings/phrasings
The heterogeneity in the wording/phrasing of PGA requires caution when interpreting the results [34]. The DAS28 is one of the most commonly used composite scores in routine clinical practice; the PGA component of the score carries a small weighting of 0.014, which may still result in differences to the overall DAS28 score (the maximum difference being 1.4 when holding the other variables constant and using first a PGA-VAS score of 0 mm, then of 100 mm). French et al. [11] performed a study where DAS28 was calculated in the same patients when using different PGAs. Five different versions of the PGA-VAS were assessed based on: (1) “Feeling” (“How do you feel concerning your arthritis over the last week?”); (2) Disease activity (“How active has your disease been this week?”); (3) “Well-being” (“How has your overall well-being been this week?”); (4) “Best/worst” (“If 0 is the best you have ever been and 100 is the worst you have ever been, where do you think you have been over the last week?”); and (5) “Arthritis impact measurement scales” (AIMS; “Considering all the ways your arthritis affects you….”). All PGA-VAS versions correlated strongly with each other (rho = 0.67–0.87, p < 0.0001) [11]. However, when the phrasing of PGA varied there was a difference in DAS28 scores, the largest being 0.63 points. Such differences in score, though small, could have clinical implications, i.e., on the eligibility for biologic disease-modifying anti-rheumatic drugs in countries where access to these drugs is restricted based on strict DAS28 cutoffs.
However, although there are differences at the individual level according to the concepts, wordings/phrasing used, and time period assessed, these differences do not always reflect differences at the group level [11, 12]. Direct comparison between studies is limited due to differences in techniques used to assess the PGA and the population used. Although this has not been explored, it is possible PGA interpretation may be different in clinical trials versus in “clinical practice”, in particular given population selection and the often multiple use of PROs in studies.
Table 4 summarizes the main aspects of the PGA and key messages presented in this review.
Interpretation of PGA levels for remission
Both DAS28-based remission and ACR/EULAR defined remission criteria incorporate PGA into their scores [2, 35]. ACR/EULAR Boolean-based remission is defined as PGA ≤1 using a 0–10 VAS. Therefore, PGA plays a major role in determining fulfillment of remission criteria in RA [6, 7, 35, 36]. In fact, PGA appears to be often a limiting factor for remission—i.e., in patients with no visible inflammation, remission may not be reached because of PGA. In a study based on the DREAM remission induction cohort, ACR/EULAR remission was present in 20.1 % of the patients. In 108 out of 512 patients, the PGA score was >1 using a 0–10 VAS despite fulfillment of the remaining criteria (TJC28, SJC28, and C-reactive protein in mg/dl ≤1). The specific wording of questions and anchors used for the PGA were: “Considering all of the ways your arthritis affects you, mark “X” on the scale for how well you are doing” (“very well” to “very poor”)” [37]. Similarly, close to half the patients without visible inflammation in the ESPOIR cohort did not achieve ACR/EULAR remission because of PGA levels above 1/10 cm [38]. Thus, near-remission defined as three of the four criteria (PGA excluded) is the most frequent status [36–39]. Many of these patients have a PGA above 1 but still quite low (usual values are around 2/10) [40], perhaps suggesting a need for revising the remission cutoff value for PGA. Another question relates to the phrasing of PGA in the remission criteria: would using the “disease activity” formulation make more sense than using the “global health” formulation? Unpublished results based on the ESPOIR French early arthritis cohort indicate that the disease activity wording will lead to less states of near-remission.
Overall, the high frequency of near-remission raises the question of whether the way remission is defined needs to be better clarified, i.e., should it reflect absence of inflammation alone or absence of inflammation and symptoms? The current amalgamation of joint counts and C-reactive protein with PGA indeed leads to some difficulties of interpretation, particularly in cases of near-remission. Furthermore, the predictive validity of near-remission is of clear importance, predicting long-term outcomes of these patients. Our unpublished results indicate near-remission predicts radiographic progression over 3 years in early RA, as well as ACR/EULAR remission, in the ESPOIR cohort, suggesting near-remission is a possible valid and even sufficient predictive outcome in early RA [40, 41]. In the context of treating to target, more work is needed on how to best interpret levels of PGA when aiming for remission.
What are the elements explaining PGA?
PGA is a wide-reaching measure which may mean different things for different people. Data are available on the main drivers of PGA at the group level. PGA reflects both disease activity and other factors. Given PGA is assessed to provide information additional to joint counts or acute phase reactants, it is expected there might be some but not complete overlap.
PGA is explained by RA disease activity
Disease activity (i.e., RA inflammatory status) explains a large part of PGA. Pain is a major cause of distress in patients with RA and this, along with joint damage, is among the important aspects/domains of RA that affect patients’ lives and will contribute to how the PGA is scored. Most studies indeed support that pain and functional incapacity (evaluated by HAQ), are the most important drivers of PGA, and these outcomes are indirectly reflecting RA disease activity. Furthermore, fatigue plays a role and has also been found to be an important determinant of PGA [13]. However, joint counts and acute phase reactants are not strong drivers of PGA [12, 36]. In several studies pain is the single main driver of PGA and may explain up to 75 % of the PGA result, whether the concept is global health or disease activity [11, 13]. This high contribution from pain is multifactorial but strongly related to the inflammatory status [42]. This probably contributes to its high responsiveness in trials. We should recognize, however, that pain itself is multifactorial.
With regard to concepts underlying PGA, as expected the disease activity-PGA is more related to inflammation than the global health-PGA. Data from the Quantitative Standard Monitoring of Patients with RA (QUEST-RA) study support that the PGA is explained by different drivers depending on the wording used [12].
PGA is explained by non-RA factors
Over and above disease activity, PGA is affected by other factors, including RA-related factors such as structural damage and non-RA factors such as demographic characteristics, education level, and perhaps culture and geographic origin (Table 1) [36, 43]. Furthermore, interpretation of the question by the patient may depend on duration of disease through a “response shift” resulting from better familiarity with symptoms and changes in patient expectations, as mentioned above.
In the QUEST-RA study, psychological distress was an important driver of PGA and was influenced by the different wording used for the PGA: it was driving more importantly global health than the disease activity wording [13]. There is conflicting evidence on the impact of comorbidities on PGA: a cross-sectional study of US Hispanics with RA showed no association between comorbidities, including depression and fibromyalgia, and PGA [44]. In contrast, based on a study of 50 female patients with RA, in those with co-existing fibromyalgia, significantly higher subjective items, including the PGA (using global health wording) were noted [45]. Differences in the study population and design, as well as the collection and recording of comorbidity data, could account for the variations seen between studies.
Discordance between PGA and physician global assessment
It is interesting to compare PGA to another global, “gestalt” assessment of disease, which is the physician global assessment. Physician global assessment is a well-validated outcome which is recognized as part of the RA core set [3]. Evidence suggests that discordance exists between patient and physician assessment of RA disease activity, with studies consistently showing that PGA is very often scored higher than physician global assessment [13, 43, 46–49]. Discordance in most studies is defined as a difference of ≥3/10 points between the PGA and physician global assessment [12]. The prevalence of discordance using this definition was found to be around 43 % in a recent meta-analysis, indicating a different understanding or perspective of the same general concept [48].
What studies have shown to date is that variables that are important to patients are not the same as those valued by physicians as reflecting disease activity (Table 5). Generally, more objective measures of disease, e.g., joint counts and elevated acute phase reactants, lead to a higher physician global assessment whereas pain and altered quality of life without visible signs of inflammation, but also comorbidities and psychological distress, will lead to higher PGA (Table 5) [50]. In such cases of discordance, it is important to discuss the patient’s psychological status as well as personal life factors since the solutions will not always lie in immunosuppressive drugs but rather might depend on non-pharmacological interventions. This discordance may act as a clue to the presence of non-disease severity factors influencing the PGA.
Discussion
The increasing emphasis on the patients’ perspective of health in considering priorities and making treatment choices has resulted in PROs being a core part of routine assessment of disease in RA and also an end-point in clinical trials and observational studies. Recent guidelines are characterized by a shift from the traditional approach of physician-led physical examination and investigations such as laboratory tests and radiographs (the “biomedical model”) to a more patient-centered approach to care [51]. PGA is one of the most commonly captured and reported PROs, mainly due to its simplicity and its feasibility in both clinical practice and registers as well as in clinical trial settings. It is strongly correlated with other self-reported outcomes and carries important patient information. Therefore, despite the controversy regarding the value of PROs including the PGA, these represent the only way to assess some of the aspects related to RA, for example, symptoms, justifying that clinician-reported outcomes and PROs should be considered as complementary to each other [52].
The lack of homogeneity in the concepts, wordings/phrasings, and time period assessed by PGA threatens the validity of PGA since it may lead to modified responses resulting from the diversity of formulations [15]. Such diversity can influence clinical and treatment decision-making, highlighting the importance of standardizing (where appropriate) and validating the question phrasing as part of capturing information on PGA. We suggest that emphasis is placed on reducing heterogeneity in wording/phrasing and time period of the PGA in order to enable more uniform capture (and hence interpretation) of information across clinical and research settings.
The discordance between PGA and physician global assessment demonstrated in many studies to date suggests that perceptions of disease activity by patients may be influenced by different factors, resulting in different aspects of disease being measured. Such discordance can negatively influence medical care, adherence to treatment, and disease outcomes. Despite this, the use of PROs such as PGA is particularly informative, bringing additional information and perspective, especially given the observed discordance of assessment between physicians and patients [52]. Like other PROs, it is of particular value when changes in clinical measurements or laboratory or radiographic outcomes may not translate into meaningful benefits for patients. In particular, the ease of use and feasibility of PGA, with little or no training of patients required to complete it, means that it can be easily incorporated into busy clinical settings. However, it is important that this contribution of patients to disease activity scores via the PGA is evaluated in a standardized way.
We feel the lack of a standardized definition on the concept, wording/phrasing, and time period assessed as part of PGA represents one of its weaknesses. This does not preclude the possibility of having more than one version of PGA; however, it requires clarity with regard to what version is selected and for which purpose (e.g., PGA for disease activity or PGA for global health). We advocate the use of a homogeneous wording in a specific context, e.g., for repeated measures it is important to use the same wording/phrasing. This is particularly important in routine clinical practice since it may lead to incorrect interpretations regarding, for example, response to treatment.
In terms of practical recommendations, the suggestion of the authors is that phrasing of PGA may at this stage be proposed as capturing (1) either global health or disease activity which is (2) related to arthritis and captured by the reference period of (3) today/this point in time. Examples would be the formulation proposed in the RAPID 3 score for global health or the one proposed in the EULAR/ACR remission criteria for disease activity (Table 6) [37].
The choice between the two concepts will depend on the objective of the measurement of the PGA. The global health question gives more holistic information on patient status since it includes to a wider extent elements such as comorbidities and psychological distress. The disease activity-PGA is more in line with more objective measures of disease and assesses more closely the inflammatory burden.
Conclusions
PGA is a key outcome measure in RA with clear validity and usefulness. However, the lack of a “gold standard” in terms of its wording/phrasing and time period assessed necessitates more research into this field in order to avoid pitfalls in interpretation and, consequently, in the achievement of treatment targets. In this review, we propose homogenized wordings which may be considered for future studies. Importantly, a clear understanding of what PGA measures and potential sources of variation in its reporting is key to accurate interpretation. Furthermore, this review gives insights into factors associated with and affecting PGA—for example, its close association with pain, mood, and fatigue and issues around discordance with physician global assessment. This may be informative in guiding interventions to improve care and overall quality of life for RA patients.
Abbreviations
- ACR:
-
American College of Rheumatology
- DAS:
-
Disease Activity Score
- DAS28:
-
28-joint count Disease Activity Score
- DREAM:
-
Dutch Rheumatoid Arthritis Monitoring (registry)
- EGA:
-
Evaluated global assessment
- ESPOIR:
-
Etude et Suivi des POlyarthrites Indifferenciées Récentes (cohort)
- ESR:
-
Erythrocyte sedimentation rate
- EULAR:
-
European League Against Rheumatism
- HAQ:
-
Health Assessment Questionnaire
- NRS:
-
Numeric rating scale
- PGA:
-
Patient global assessment
- PROs:
-
Patient reported outcomes
- QUEST-RA:
-
Quantitative Standard Monitoring of Patients with Rheumatoid Arthritis
- RA:
-
Rheumatoid arthritis
- RAPID 3:
-
Routine Assessment of Patient Index Data
- SJC:
-
Swollen joint count
- TJC:
-
Tender joint count
- VAS:
-
Visual analogue scale
References
Boers M, Kirwan JR, Wells G, Beaton D, Gossec L, d’Agostino M-A, et al. Developing core outcome measurement sets for clinical trials: OMERACT filter 2.0. J Clin Epidemiol. 2014;67(7):745–53.
Smolen JS, Landewé R, Breedveld FC, Buch M, Burmester G, Dougados M, et al. EULAR recommendations for the management of rheumatoid arthritis with synthetic and biological disease-modifying antirheumatic drugs: 2013 update. Ann Rheum Dis. 2014;73(3):492–509.
Felson DT, Anderson JJ, Boers M, Bombardier C, Chernoff M, Fried B, et al. The American College of Rheumatology preliminary core set of disease activity measures for rheumatoid arthritis clinical trials. The Committee on Outcome Measures in Rheumatoid Arthritis Clinical Trials. Arthritis Rheum. 1993;36(6):729–40.
Kirwan JR, Minnock P, Adebajo A, Bresnihan B, Choy E, de Wit M, et al. Patient perspective: fatigue as a recommended patient centered outcome measure in rheumatoid arthritis. J Rheumatol. 2007;34(5):1174–7.
Kilic L, Erden A, Bingham CO, Gossec L, Kalyoncu U. The reporting of patient-reported outcomes in studies of patients with rheumatoid arthritis: a systematic review of 250 articles. J Rheumatol. 2016;43:1300–5.
Masri KR, Shaver TS, Shahouri SH, Wang S, Anderson JD, Busch RE, et al. Validity and reliability problems with patient global as a component of the ACR/EULAR remission criteria as used in clinical practice. J Rheumatol. 2012;39(6):1139–45.
Curtis JR, Shan Y, Harrold L, Zhang J, Greenberg JD, Reed GW. Patient perspectives on achieving treat-to-target goals: a critical examination of patient-reported outcomes. Arthritis Care Res (Hoboken). 2013;65(10):1707–12.
Scott PJ, Huskisson EC. Measurement of functional capacity with visual analogue scales. Rheumatol Rehabil. 1977;16(4):257–9.
Kirwan JR, Bartlett SJ, Beaton DE, Boers M, Bosworth A, Brooks PM, et al. Updating the OMERACT filter: implications for patient-reported outcomes. J Rheumatol. 2014;41(5):1011–5.
Hewlett S, Nicklin J, Bode C, Carmona L, Dures E, Engelbrecht M, et al. Translating patient reported outcome measures: methodological issues explored using cognitive interviewing with three rheumatoid arthritis measures in six European languages. Rheumatology (Oxford). 2016;55:1009–16.
French T, Hewlett S, Kirwan J, Sanderson T. Different wording of the Patient Global Visual Analogue Scale (PG-VAS) affects rheumatoid arthritis patients’ scoring and the overall Disease Activity Score (DAS28): a cross-sectional study. Musculoskeletal Care. 2013;11(4):229–37.
Khan NA, Spencer HJ, Abda EA, Alten R, Pohl C, Ancuta C, et al. Patient’s global assessment of disease activity and patient’s assessment of general health for rheumatoid arthritis activity assessment: are they equivalent? Ann Rheum Dis. 2012;71(12):1942–9.
Khan NA, Spencer HJ, Abda E, Aggarwal A, Alten R, Ancuta C, et al. Determinants of discordance in patients’ and physicians’ rating of rheumatoid arthritis disease activity. Arthritis Care Res (Hoboken). 2012;64(2):206–14.
Harrison MJ, Boonen A, Tugwell P, Symmons DPM. Same question, different answers: a comparison of global health assessments using visual analogue scales. Qual Life Res. 2009;18(10):1285–92.
Kalyoncu U, Dougados M, Daurès J-P, Gossec L. Reporting of patient-reported outcomes in recent trials in rheumatoid arthritis: a systematic literature review. Ann Rheum Dis. 2009;68(2):183–90.
Smedstad LM, Kvien TK, Moum T, Vaglum P. Correlates of patients’ global assessment of arthritis impact. A 2-year study of 216 patients with RA. Scand J Rheumatol. 1997;26(4):259–65.
van Gestel AM, Haagsma CJ, van Riel PL. Validation of rheumatoid arthritis improvement criteria that include simplified joint counts. Arthritis Rheum. 1998;41(10):1845–50.
Meenan RF, Gertman PM, Mason JH. Measuring health status in arthritis. The arthritis impact measurement scales. Arthritis Rheum. 1980;23(2):146–52.
Felson DT, Smolen JS, Wells G, Zhang B, van Tuyl LHD, Funovits J, et al. American College of Rheumatology/European League against Rheumatism provisional definition of remission in rheumatoid arthritis for clinical trials. Ann Rheum Dis. 2011;70(3):404–13.
Chatzidionysiou K, Nikiphorou E, Gossec L, Hyrich K, Filip C, van Eijk-Hustings Y, et al. The EULAR Task Force for standardising minimum data collection in rheumatoid arthritis observational research: results of a hierarchical literature review. Ann Rheum Dis. 2016;75(Suppl 2):166.
Wells GA, Boers M, Shea B, Brooks PM, Simon LS, Strand CV, et al. Minimal disease activity for rheumatoid arthritis: a preliminary definition. J Rheumatol. 2005;32(10):2016–24.
Pincus T, Bergman M, Sokka T, Roth J, Swearingen C, Yazici Y. Visual analog scales in formats other than a 10 centimeter horizontal line to assess pain and other clinical data. J Rheumatol. 2008;35(8):1550–8.
Lati C, Guthrie LC, Ward MM. Comparison of the construct validity and sensitivity to change of the visual analog scale and a modified rating scale as measures of patient global assessment in rheumatoid arthritis. J Rheumatol. 2010;37(4):717–22.
Gossec L, Dougados M, Rincheval N, Balanescu A, Boumpas DT, Canadelo S, et al. Elaboration of the preliminary Rheumatoid Arthritis Impact of Disease (RAID) score: a EULAR initiative. Ann Rheum Dis. 2009;68(11):1680–5.
Schwartz CE, Andresen EM, Nosek MA, Krahn GL. Response shift theory: important implications for measuring quality of life in people with disability. Arch Phys Med Rehabil. 2007;88(4):529–36.
Bombardier C, Raboud J. A comparison of health-related quality-of-life measures for rheumatoid arthritis research. The Auranofin Cooperating Group. Control Clin Trials. 1991;12(4 Suppl):243S–56S.
Buchbinder R, Bombardier C, Yeung M, Tugwell P. Which outcome measures should be used in rheumatoid arthritis clinical trials? Clinical and quality-of-life measures’ responsiveness to treatment in a randomized controlled trial. Arthritis Rheum. 1995;38(11):1568–80.
Uhlig T, Kvien TK, Pincus T. Test-retest reliability of disease activity core set measures and indices in rheumatoid arthritis. Ann Rheum Dis. 2009;68(6):972–5.
Hernández-Cruz B, Cardiel MH. Intra-observer reliability of commonly used outcome measures in rheumatoid arthritis. Clin Exp Rheumatol. 1998;16(4):459–62.
Rohekar G, Pope J. Test-retest reliability of patient global assessment and physician global assessment in rheumatoid arthritis. J Rheumatol. 2009;36(10):2178–82.
Wells G, Li T, Maxwell L, Maclean R, Tugwell P. Responsiveness of patient reported outcomes including fatigue, sleep quality, activity limitation, and quality of life following treatment with abatacept for rheumatoid arthritis. Ann Rheum Dis. 2008;67(2):260–5.
Strand V, Cohen S, Crawford B, Smolen JS, Scott DL. Patient-reported outcomes better discriminate active treatment from placebo in randomized controlled trials in rheumatoid arthritis. Rheumatology (Oxford). 2004;43(5):640–7.
Pincus T, Richardson B, Strand V, Bergman MJ. Relative efficiencies of the 7 rheumatoid arthritis Core Data Set measures to distinguish active from control treatments in 9 comparisons from clinical trials of 5 agents. Clin Exp Rheumatol. 2014;32(5 Suppl 85):S47–54.
Anderson JK, Zimmerman L, Caplan L, Michaud K. Measures of rheumatoid arthritis disease activity: Patient (PtGA) and Provider (PrGA) Global Assessment of Disease Activity, Disease Activity Score (DAS) and Disease Activity Score with 28-Joint Counts (DAS28), Simplified Disease Activity Index (SDAI), Cl. Arthritis Care Res (Hoboken). 2011;63 Suppl 1:S14–36.
Balogh E, Madruga Dias J, Orr C, Mullan R, Harty L, FitzGerald O, et al. Comparison of remission criteria in a tumour necrosis factor inhibitor treated rheumatoid arthritis longitudinal cohort: patient global health is a confounder. Arthritis Res Ther. 2013;15(6):R221.
Studenic P, Smolen JS, Aletaha D. Near misses of ACR/EULAR criteria for remission: effects of patient global assessment in Boolean and index-based definitions. Ann Rheum Dis. 2012;71(10):1702–5.
Vermeer M, Kuper HH, van der Bijl AE, Baan H, Posthumus MD, Brus HLM, et al. The provisional ACR/EULAR definition of remission in RA: a comment on the patient global assessment criterion. Rheumatology (Oxford). 2012;51(6):1076–80.
Aletaha D, Machold KP, Nell VPK, Smolen JS. The perception of rheumatoid arthritis core set measures by rheumatologists. Rheumatology (Oxford). 2006;45(9):1133–9.
Shahouri SH, Michaud K, Mikuls TR, Caplan L, Shaver TS, Anderson JD, et al. Remission of rheumatoid arthritis in clinical practice: application of the American College of Rheumatology/European League Against Rheumatism 2011 remission criteria. Arthritis Rheum. 2011;63(11):3204–15.
Gossec L, Gaujoux-Viala C, Rat A-C, Fautrel B, Saraux A, Guillemin F, et al. OP0003 Are patient global and fatigue predictive of structural outcomes, 3 years later, in patients in remission in early arthritis? Results from the french espoir cohort. Ann Rheum Dis. 2014;71 Suppl 3:53–3.
Gossec L, Kirwan J, Paternotte S, Balanescu A, Boumpas D, de Wit M, et al. FRI0071 Does psychological status drive patient global assessment for rheumatoid arthritis patients who do not have any clinical signs of inflammation? an exploratory analysis of near-remission using the rheumatoid arthritis impact of disease (RAID) score. Ann Rheum Dis. 2014;72 Suppl 3:A393–3.
Studenic P, Radner H, Smolen JS, Aletaha D. Discrepancies between patients and physicians in their perceptions of rheumatoid arthritis disease activity. Arthritis Rheum. 2012;64(9):2814–23.
Nicolau G, Yogui MM, Vallochi TL, Gianini RJ, Laurindo IMM, Novaes GS. Sources of discrepancy in patient and physician global assessments of rheumatoid arthritis disease activity. J Rheumatol. 2004;31(7):1293–6.
Diaz-Correa L, Nieves-Plaza M, Santiago-Casas YC, González-Rivera T, Rios G, Vilá LM. Discordance of patient-physician assessments of general health in a US Hispanic population with rheumatoid arthritis—ACR Meeting 2013 abstracts. http://acrabstracts.org/abstract/discordance-of-patient-physician-assessments-of-general-health-in-a-us-hispanic-population-with-rheumatoid-arthritis/.
Nawito Z, Rady HM, Maged LA. The impact of fibromyalgia on disease assessment in rheumatoid arthritis patients. Egypt Rheumatol. 2013;35(3):115–9.
Kaneko Y, Kuwana M, Kondo H, Takeuchi T. Discordance in global assessments between patient and estimator in patients with newly diagnosed rheumatoid arthritis: associations with progressive joint destruction and functional impairment. J Rheumatol. 2014;41(6):1061–6.
Furu M, Hashimoto M, Ito H, Fujii T, Terao C, Yamakawa N, et al. Discordance and accordance between patient’s and physician’s assessments in rheumatoid arthritis. Scand J Rheumatol. 2014;43(4):291–5.
Barton JL, Imboden J, Graf J, Glidden D, Yelin EH, Schillinger D. Patient-physician discordance in assessments of global disease severity in rheumatoid arthritis. Arthritis Care Res (Hoboken). 2010;62(6):857–64.
Hirsh JM, Boyle DJ, Collier DH, Oxenfeld AJ, Caplan L. Health literacy predicts the discrepancy between patient and provider global assessments of rheumatoid arthritis activity at a public urban rheumatology clinic. J Rheumatol. 2010;37(5):961–6.
Wolfe F, Michaud K, Pincus T, Furst D, Keystone E. The disease activity score is not suitable as the sole criterion for initiation and evaluation of anti-tumor necrosis factor therapy in the clinic: discordance between assessment measures and limitations in questionnaire use for regulatory purposes. Arthritis Rheum. 2005;52(12):3873–9.
Gossec L, Dougados M, Dixon W. Patient-reported outcomes as end points in clinical trials in rheumatoid arthritis. RMD Open. 2015;1(1):e000019.
Pope JE, Khanna D, Norrie D, Ouimet JM. The minimally important difference for the health assessment questionnaire in rheumatoid arthritis clinical practice is smaller than in randomized controlled trials. J Rheumatol. 2009;36(2):254–9.
Lassere MN, van der Heijde D, Johnson KR, Boers M, Edmonds J. Reliability of measures of disease activity and disease damage in rheumatoid arthritis: implications for smallest detectable difference, minimal clinically important difference, and analysis of treatment effects in randomized controlled trials. J Rheumatol. 2001;28(4):892–903.
Ward MM. Clinical measures in rheumatoid arthritis: which are most useful in assessing patients? J Rheumatol. 1994;21(1):17–27.
Desthieux C, Hermet A, Granger B, Fautrel B, Gossec L. Patient-physician discordance in global assessment in rheumatoid arthritis: a systematic literature review with metaanalysis. Arthritis Care Res (Hoboken). 2016. doi:10.1002/acr.22902. [Epub ahead of print]
Davis JM, Crowson CS, Bongartz T, Michet CJ, Matteson EL, Gabriel SE. Prevalence and correlates of patient-physician discordance in early rheumatoid arthritis—ACR Meeting 2014 abstracts. http://acrabstracts.org/abstract/prevalence-and-correlates-of-patient-physician-discordance-in-early-rheumatoid-arthritis/.
Funding
The work of the RA Task Force is funded by EULAR; this work is derived from that taskforce.
Authors’ contributions
EN is the main fellow in the EULAR Task Force undertaking the literature review, preparing and writing the manuscript with supervision from senior author LG. LG provided expert opinion on the literature search strategy and hand searches. HR and KC contributed to the writing of the manuscript, discussing the literature, and presentation of findings. EN and LG discussed the manuscript at each stage of its development. CD, CZ, YEH, WD, KH, JA, and LG provided critical review of the manuscript. All authors read and approved the final manuscript.
Competing interests
The authors’ declare that they have no competing interests.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated.
About this article
Cite this article
Nikiphorou, E., Radner, H., Chatzidionysiou, K. et al. Patient global assessment in measuring disease activity in rheumatoid arthritis: a review of the literature. Arthritis Res Ther 18, 251 (2016). https://doi.org/10.1186/s13075-016-1151-6
Published:
DOI: https://doi.org/10.1186/s13075-016-1151-6