Abstract
Background
The objective of this study was to describe the prevalence, incidence, prognostic factors, and outcomes of venous thromboembolism in critically ill patients receiving contemporary thrombosis prophylaxis.
Methods
We conducted a pooled analysis of two prospective cohort studies. The outcomes of interest were in-hospital pulmonary embolism or lower extremity deep vein thrombosis (PE-LDVT), in-hospital nonleg deep vein thrombosis (NLDVT), and 90-day mortality. Multivariable logistic regression analysis was used to evaluate the association between predefined baseline prognostic factors and PE-LDVT or NLDVT. Cox regression analysis was used to evaluate the association between PE-LDVT or NLDVT and 90-day mortality.
Results
A total of 2208 patients were included. The prevalence of any venous thromboembolism during 3 months before ICU admission was 3.6% (95% CI 2.8–4.4%). Out of 2166 patients, 47 (2.2%; 95% CI 1.6–2.9%) developed PE-LDVT and 38 patients (1.8%; 95% CI 1.2–2.4%) developed NLDVT. Renal replacement therapy (OR 3.5 95% CI 1.4–8.6), respiratory failure (OR 2.0; 95% CI 1.1–3.8), and previous VTE (OR 3.6; 95% CI 1.7–7.7) were associated with PE-LDVT. Central venous catheters (OR 5.4; 95% CI 1.7–17.8) and infection (OR 2.2; 95% CI 1.1–4.3) were associated with NLDVT. Occurrence of PE-LDVT but not NLDVT was associated with increased 90-day mortality (HR 2.7; 95% CI 1.6–4.6, respectively, 0.92; 95% CI 0.41–2.1).
Conclusion
Thrombotic events are common in critically ill patients, both before and after ICU admittance. Development of PE-LDVT but not NLDVT was associated with increased mortality. Prognostic factors for developing PE-LDVT or NLDVT despite prophylaxis can be identified at ICU admission and may be used to select patients at higher risk in future randomized clinical trials.
Trial registration
NCT03773939.
Similar content being viewed by others
Background
Critically ill patients are at increased risk of developing venous thromboembolism (VTE), including both deep vein thrombosis (DVT) and pulmonary embolism (PE) [1, 2]. PE and lower extremity DVT (PE-LDVT) are often regarded as two manifestations of the same disease. Venous thrombosis may also occur at other sites, which has been referred to as nonleg deep vein thrombosis (NLDVT) [3,4,5]. Both PE-LDVT and NLDVT are associated with adverse outcomes [1,2,3, 6]. Thrombosis prophylaxis reduces the incidence of VTE and guidelines recommend pharmacologic prophylaxis for all critically ill patients if not contraindicated [7,8,9].
Despite prophylactic measures, thrombotic complications may still occur in critically ill patients. Two large randomized trials reported VTE incidences up to 6% in critically ill patients despite thrombosis prophylaxis [10, 11], while cohort studies reported incidences up to 37% [12,13,14,15]. NLDVT occurred in 2.2% of the patients in the PROTECT randomized trial [3]. Several prognostic factors for the development of VTE have been identified in critically ill patients, including central venous catheters, higher illness severity scores, renal failure, a history of VTE, higher body mass index, and vasopressor therapy [1, 13, 16]. The latter three were also recognized to be associated with failure of thrombosis prophylaxis in a post hoc analysis of the PROTECT trial [17].
Most studies on VTE incidence, prognostic factors, and outcomes are 5 to 10 years old, and methods and use of thrombosis prophylaxis as well as the overall level of care have improved over this period of time [7, 18]. Several of the previous studies excluded patients at risk of bleeding, which may have led to selection bias [10, 14, 17]. Most studies screened all patients for ‘asymptomatic’ thrombosis, although the clinical significance of these events remains to be established [19, 20].
More data on prognostic factors for failure of contemporary thrombosis prophylaxis in critically ill patients are needed to identify the target population for future high-quality randomized clinical trials. The objective of this study is to describe the prevalence, incidence, prognostic factors, and outcomes of both PE-LDVT and NLDVT in an unselected cohort of critically ill patients receiving routine thrombosis prophylaxis.
Materials and methods
Study design
This study is a pooled analysis of two prospective cohort studies: the Simple Intensive Care studies I (SICS-I) and the Simple Intensive Care studies II (SICS-II) including its pilot data [21, 22]. We performed the current analysis following a pre-published protocol (Clinicaltrials.gov, NCT03773939). Both the SICS-I and the SICS-II are single-center cohort studies that have been conducted in the University Medical Center Groningen. Inclusion criteria for both cohorts were the age of 18 years or older, unplanned Intensive Care Unit (ICU) admission, and an expected ICU stay of more than 24 h. Exclusion criteria were planned admission, inability or refusal to provide informed consent, and for the SICS-I also inability to include patients without interfering with clinical care (e.g., in case of continuous resuscitation efforts or mechanical circulatory support). The local institutional review board approved both cohort studies (2015/004 and 2018/203) and the current analysis (2019/078). Following national guidelines all patients received thrombosis prophylaxis with nadroparin 2850 IU once daily, provided there were no contraindications. In case of contraindications, patients received compression stockings. Pneumatic compression devices are not routinely used in our hospital. This study is reported according to the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) guideline [23].
Data collection
Patient characteristics, such as demographical data, medication use, comorbidities, and severity of illness scores were registered at ICU admission. Candidate prognostic factors for the development of either PE-LDVT or NLDVT were defined a priori. These were either established prognostic factors for VTE or had been incorporated in previous VTE risk assessment models [24]. All factors were assessed once at ICU admission. We considered the following candidate predictors: active cancer, acute infection, acute renal failure, age, body mass index (BMI), cardiovascular failure, a central venous catheter (CVC), estrogen therapy, sex, limb paralysis, major surgery, mechanical ventilation, multiple trauma, previous VTE, respiratory failure, stroke, thrombophilic disorder, and vasopressor use. All candidate prognostic factors, including their a priori set definitions and units of measurement are listed in Additional file 1: Table S1. We applied the following post hoc changes to the protocol: age and BMI were assessed as continuous variables, renal replacement therapy was assessed as a separate predictor (in addition to renal failure), and reduced mobility was not assessed. All data had been prospectively collected within the SICS-II cohort, but some were not registered in SICS-I (CVC, estrogen use, major surgery, active cancer, multiple trauma, previous VTE, and thrombophilic disorder). The missing data for the patients included in the SICS-I cohort were manually retrieved from electronic health records.
Outcome definitions
The outcomes of interest were in-hospital PE-LDVT, in-hospital NLDVT, and 90-day mortality. In-hospital PE-LDVT was defined as any objectively proven pulmonary embolism or lower extremity deep vein thrombosis during ICU or subsequent hospital stay. Lower extremity deep vein thrombosis was defined as acute thrombosis of the proximal lower-extremity veins (iliac, femoral, or popliteal), confirmed by compression ultrasonography, venography, CT, MRI, or autopsy. Pulmonary embolism was defined as acute thrombosis within the pulmonary vasculature as shown by ventilation-perfusion scan, CT angiography, or autopsy. Deep vein thrombosis in any other site was registered separately and referred to as NLDVT following previous reports [3]. NLDVTs included deep venous thrombosis in the jugular, subclavian, axillary, or brachial veins, but also thrombosis in the cava, mesenteric, portal, splenic, or renal veins. Superficial venous thrombotic events (i.e., cephalic or basilic vein thrombosis) and distal lower-extremity vein thromboses were not included under either of the two abovementioned outcome definitions. No screening protocol for the detection of PE-LDVT or NLDVT was used. Mortality was assessed at 90 days after ICU admittance based on the municipal record database.
Statistical analysis
Data are presented as means with standard deviations (SD) or medians with interquartile ranges [IQR] depending on distributions. Effect estimates are presented as odds ratios (ORs) or hazards ratios (HRs) with 95% confidence intervals (CIs). We considered a two-sided p value < 0.05 statistically significant and performed no corrections for multiplicity. All analyses were performed using R software (R core team, 2019, version 3.6.0).
Prevalence, incidence, and anatomical location
We made a distinction between prevalent and incident events: any PE-LDVT or NLDVT diagnosed within 3 months before ICU admission was defined as a prevalent event, while events occurring after ICU admission were defined as incident. We registered the anatomical location for each event.
Missing data
Missing values were considered missing at random. Variables with less than 25% missing values were imputed with multiple imputations using chained equations using the mice package [25, 26]. The imputation model included baseline patient characteristics, all candidate prognostic factors, the Nelson–Aalen estimate of the cumulative hazard, and outcome variables. We created 30 imputed datasets with 20 iterations each. The imputed data were visually inspected and compared to observed data to assess the plausibility of imputations. Model convergence was monitored using iteration plots.
Models
Binary logistic regression analysis was conducted on each imputed dataset to determine baseline prognostic factors for the development of both PE-LDVT and NLDVT, including all a priori defined variables as candidate predictors (Additional file 1: Table S1). Patients with prevalent thrombotic events that had occurred within 24 h before ICU admission were excluded from all regression analyses because they had already achieved the outcome of interest. Univariable associations were assessed and a p value < 0.25 was used as threshold for inclusion in the multivariable models. A stepwise backward elimination method was used for constructing the multivariable models. Anticoagulant medication was entered in all multivariable models as a categorical variable (none, thrombosis prophylaxis, or therapeutic anticoagulation) because of its potential influence on the prognostic value of candidate factors. Parameter estimates were combined using Rubin’s rules at each stage of variable selection [27, 28]. Multicollinearity was assessed by analyzing variance inflation factors. We conducted two sensitivity analyses (S1 and S2) to assess the robustness of our findings. First, we reconstructed all logistic models on a complete case basis, excluding cases with missing data (S1). Second, we reconstructed all logistic models after excluding all PE-LDVTs or NLDVTs detected during the first two days of ICU admission, as these may represent prevalent instead of incident events (S2).
As a post hoc exploratory analysis, we used a multivariable Cox regression model on each imputed dataset to estimate the association between PE-LDVT or NLDVT, and 90-day mortality. The model was adjusted for the time-fixed covariates age, sex, admission type (medical, surgical, or other), APACHE IV score, and vasopressor therapy at ICU admission. PE-LDVT and NLDVT were included as time-dependent exposures to account for immortal time bias [29]. Parameter estimates were combined using Rubin’s rules.
Deviations from the protocol
The protocol was initially designed to describe the derivation and validation of a risk assessment model for the prediction of PE-LDVT in the ICU. The current study is a descriptive analysis of the main findings in the derivation cohorts (SICS-I and SICS-II). Recruitment for the external validation cohort is still ongoing. Decisions that were made on a post hoc basis in the current analysis have been marked as such in the preceding paragraphs.
Results
Study population
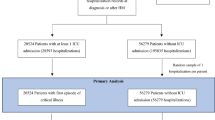
Recruitment occurred from 27 March 2015 to 22 July 2017 (SICS-I cohort) and 14 March 2018 to 10 July 2019 (SICS-II cohort). A total of 4987 patients were assessed for eligibility, of whom 2812 were eligible for inclusion, and 2208 were included (Additional file 1: Figure S1). Table 1 lists the baseline characteristics for this analysis (the two merged cohorts). Most patients were admitted for medical reasons, and 389 (17.6%) used therapeutic anticoagulant medication at home. The median hospital stay after ICU admission was 12 days (IQR 6–22). The number and frequency of missing values are provided in Additional file 1: Table S2.
Prevalence of any thrombotic event before ICU admission
In the previous 3 months before ICU admission 79 patients had developed any thrombotic event accounting for a prevalence of 3.6% (95% CI 2.8–4.4%). Fifty-one of these patients (2.3%) had PE-LDVT and 28 (1.3%) NLDVT. In 42 of these patients (1.9%) the thrombotic event had occurred within 24 h before ICU admission, and these patients were excluded from further analyses.
Pulmonary embolism and lower extremity deep vein thrombosis
Out of 2166 patients, 47 (2.2%; 95% CI 1.6–2.9%) developed PE-LDVT either during ICU or subsequent hospital stay: DVT occurred in 15 patients and PE in 31 patients (Table 2). In one patient both DVT and PE were detected. The location of PE was subsegmental in 7 patients (22%), segmental in 18 patients (56%), central in 6 patients (19%), and unspecified in one (3%). Median time from ICU admission to development of PE-LDVT was 8.0 days (IQR 2.5–17.5). Results from univariable analyses are displayed in Additional file 1: Table S3. In multivariable analyses, renal replacement therapy (OR 3.5 95% CI 1.4–8.6; p < 0.01), respiratory failure (OR 2.0; 95% CI 1.1–3.8; p = 0.02), and a history of VTE (OR 3.6; 95% CI 1.7–7.7; p < 0.01) were statistically significant associated with the development of PE-LDVT (Fig. 1). Development of PE-LDVT was associated with increased risk of 90-day mortality (HR 2.7; 95% CI 1.6–4.6; p < 0.01).
Prognostic factors for PE-LDVT and NLDVT: results from the main analysis. All analyses were adjusted for anticoagulant use in addition to the other variables. CI confidence interval, CVC central venous catheter, NLDVT nonleg deep vein thrombosis, OR odds ratio, PE-LDVT pulmonary embolism and lower extremity deep vein thrombosis, RRT renal replacement therapy, VTE venous thromboembolism
Nonleg deep vein thrombosis
A total of 38 patients (1.8%; 95% CI 1.2–2.4%) developed NLDVT. Nineteen patients (50%) developed thrombosis of the upper-extremity veins, 13 (34%) developed portal vein thrombosis and 6 (16%) developed NLDVT in another location (e.g., in mesenteric, renal or splenic veins). Median time from ICU admission to the development of NLDVT was 8.5 days (IQR 1.5–21). Results from univariable analyses are displayed in Additional file 1: Table S3. In multivariable analyses, CVC (OR 5.4; 95% CI 1.7–17.8; p = 0.01) and infection (OR 2.2; 95% CI 1.1–4.3; p = 0.03) were statistically significant associated with the development of NLDVT (Fig. 1). There was no statistically significant association between NLDVT and 90-day mortality (HR 0.92; 95% CI 0.41–2.1; p = 0.85). No patients developed both PE-LDVT and NLDVT.
Sensitivity analyses
In the complete case analysis (S1), the association between CVC presence and PE-LDVT development was statistically significant, in contrast to the main analysis (Fig. 2). For all other prognostic factors, the complete case analysis confirmed the main analysis. Results from the sensitivity analysis excluding all patients with outcome events during the first two days after ICU admission (S2) were fully concurrent with the main analysis (Fig. 2).
Prognostic factors for PE-LDVT and NLDVT: results from the main analysis and sensitivity analyses. All analyses were adjusted for anticoagulant use in addition to the other variables. Main: main analysis including CVC as a predictor, results, therefore, differ slightly from the text and Fig. 1; S1: sensitivity analysis 1, the complete case analysis; S2: sensitivity analysis 2, excluding patients with outcome events detected within the first two days of ICU admission. CI confidence interval, CVC central venous catheter, NLDVT nonleg deep vein thrombosis, OR odds ratio, PE-LDVT pulmonary embolism and lower extremity deep vein thrombosis, RRT renal replacement therapy, VTE venous thromboembolism
Discussion
In this analysis of two prospective cohorts of acutely admitted critically ill patients, we observed 2.2% incident PE-LDVT and 1.8% NLDVT after ICU admission. The prevalence of any thrombotic event 90 days before ICU admission was 3.6%. Since we did not employ any systematic screening, these data reflect VTEs that were detected due to clinical signs or symptoms that prompted further diagnostic evaluation. Development of PE-LDVT but not NLDVT was associated with increased 90-day mortality in a multivariable cox regression model adjusted for several confounding factors. Baseline prognostic factors for PE-LDVT development were renal replacement therapy, admittance for respiratory failure, and a history of VTE; while baseline prognostic factors for NLDVT were CVC presence and admittance for acute infection. A high proportion of patients received antiplatelet, prophylactic, or therapeutic anticoagulation at the time of their ICU admission, and interestingly, despite the use of therapeutic anticoagulant medication at the time of ICU admission, several patients still developed venous thromboembolism. We did not register details on therapeutic anticoagulant medication use at the time of PE-LDVT development, and it is possible therapy was temporarily halted due to invasive procedures. Our data on prognostic factors for development of thrombosis despite routine prophylactic strategies can be used by clinicians for crude risk assessment, and may be used to select patients at high risk of thrombotic complications in future randomized clinical trials.
We did not include critically ill patients with coronavirus disease 2019 (COVID-19) since the SICS-I and SICS-II studies were conceived before the pandemic. The incidence of VTE in COVID-19 is high, consistent with previous reports on other viral pneumonias, for example as caused by H1N1 [30, 31]. Results from a study on incidence and prognostic factors of VTE in unselected critically ill patients would be heavily influenced if a large proportion of included patients suffered from a single condition associated with high risk of VTE. Therefore, we believe that as the burden of the pandemic ultimately lowers, and the proportion of critically ill patients with COVID-19 ‘normalizes,’ our results and conclusions should remain valid.
The incidence of thrombotic events in this study reflects daily clinical practice, and is lower than most previous studies that have reported incidences up to 37% [10, 11, 13,14,15]. In contrast, the prevalence of VTE before ICU admittance was high, which may be a reflection of baseline comorbidities. Several factors may account for the observed VTE incidence. We limited follow-up to the in-hospital period which may have led to an underestimation as previous studies have shown up to a third of events may occur weeks after discharge [32]. Also, mortality is a competing risk for VTE and may have precluded development of symptomatic events. In contrast, many of the previous studies applied stringent selection criteria, focused on particular very ill subgroups, or employed VTE screening methods, all of which in turn may have contributed to detecting a higher VTE incidence. Whether early detection and treatment of ‘asymptomatic’ VTEs through screening will improve the overall prognosis of critically ill patients still needs to be established. Previous data suggested a poor relationship between asymptomatic and symptomatic events in thromboprophylaxis trials, suggesting not all asymptomatic VTE will eventually evolve to become symptomatic [19]. Nevertheless, traditional signs and symptoms of VTE may be unreliable in critically ill patients, prohibiting a symptom-based dichotomization. Recently, in a pre-planned subgroup analysis from the PREVENT trial, Arabi and colleagues found a beneficial effect of VTE surveillance on 90-day mortality, which suggests that asymptomatic events do contribute to poor outcomes [20]. Only a well-designed randomized trial will be able to elucidate this question. Such a trial could focus on early VTE detection or, alternatively, treat high-risk patients with a higher dose of thrombosis prophylaxis.
Prognostic factors and outcomes of PE-LDVT were different from those of NLDVT, reflecting that these events should be regarded as separate entities [4]. Occurrence of PE-LDVT and not NLDVT was associated with increased 90-day mortality. This is in line with recent cohort studies in which critically ill patients who developed PE-LDVT (or a comparable composite) had higher mortality rates, while NLDVT was not associated with increased mortality [3, 15, 16]. Our study also replicates results from earlier studies that used surveillance ultrasound to detect VTE, confirming the value of previous VTE and renal failure as a prognostic factors for PE-LDVT in critically ill patients [1, 13, 17]. In contrast, respiratory failure was not previously identified as a prognostic factor, while sex, BMI, and vasopressor use could not be confirmed to be associated with PE-LDVT. Prognostic factors for NLDVT were CVC presence and acute infection. The first finding is not surprising, given that CVCs are a well-known risk factor for thrombosis [2, 33]. The latter is a new finding that needs confirmation in a follow-up study. In contrast to previous results, malignancy was not associated with NLDVT [3].
Our study has several strengths and limitations. One of its main strengths is the prospective design with high quality data collection and a priori defined candidate prognostic factors to assess both PE-LDVT and NLDVT in an unselected critically ill population receiving contemporary thrombosis prophylaxis. We applied statistical methods to handle missing data and performed sensitivity analyses to assess our findings’ robustness. Nevertheless, several limitations should be recognized. First, although the inclusion criteria were broad, the single center design limits the external validity of our findings and we encourage replication in an independent sample. Second, we did not collect data on non-pharmacological prophylactic interventions, such as compression stockings or mechanical compression devices, and were therefore unable to acknowledge for these in the analyses. Third, follow-up was limited to the hospital stay, which may have led to underestimating the PE-LDVT incidence as previous studies have estimated that up to one third of all events may occur after hospital discharge [32]. Relying on symptomatic events may have further contributed to a lower VTE incidence, although systematic screening may in turn lead to overdiagnosis. Fourth, we did not collect data on time-dependent prognostic factors that may have arisen during ICU admission. Fifth, the incidence of PE-LDVT and NLDVT was lower than anticipated, which increases the risk of model overfitting and led to wide confidence intervals. Finally, several events were detected shortly after ICU admission, and may represent prevalent instead of incident events. Still, excluding these events in a sensitivity analysis did not substantially impact the results.
Conclusions
In conclusion, thrombotic events are common in critically ill patients, both before and after ICU admittance. Development of PE-LDVT but not NLDVT was associated with increased mortality. Prognostic factors for developing PE-LDVT or NLDVT despite prophylaxis can be identified at ICU admission and may be used to select patients at higher risk in future randomized clinical trials.
Availability of data and materials
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- APACHE IV:
-
Acute Physiology and Chronic Health Evaluation
- BMI:
-
Body mass index
- CVC:
-
Central venous catheter
- DVT:
-
Deep vein thrombosis
- ICU:
-
Intensive care unit
- IQR:
-
Interquartile range
- NLDVT:
-
Nonleg deep vein thrombosis
- OR:
-
Odds ratio
- PE:
-
Pulmonary embolism
- PE-LDVT:
-
Pulmonary embolism or lower extremity deep vein thrombosis
- SD:
-
Standard deviation
- SICS:
-
Simple Intensive Care Studies
References
Cook D, Crowther M, Meade M, Rabbat C, Griffith L, Schiff D, et al. Deep venous thrombosis in medical-surgical critically ill patients: prevalence, incidence, and risk factors. Crit Care Med. 2005;33:1565–71.
Minet CC, Potton L, Bonadona AA, Hamidfar-Roy RR, Somohano CA, Lugosi M, et al. Venous thromboembolism in the ICU: main characteristics, diagnosis and thromboprophylaxis. Crit Care. 2015;19:287. https://doi.org/10.1186/s13054-015-1003-9.
Lamontagne F, McIntyre L, Dodek P, Heels-Ansdell D, Meade M, Pemberton J, et al. Nonleg venous thrombosis in critically Ill adults a nested prospective cohort study. JAMA Intern Med. 2014;174:689–96. https://doi.org/10.1001/jamainternmed.2014.169.
Spyropoulos AC. Upper vs. lower extremity deep vein thrombosis: outcome definitions of venous thromboembolism for clinical predictor rules or risk factor analyses in hospitalized patients. J Thromb Haemost. 2009;7:1041–2. https://doi.org/10.1111/j.1538-7836.2009.03351.x.
Watson HG. Upper extremity deep vein thrombosis—not the same disease at a different site. J Thromb Haemost. 2008;6:1267–8. https://doi.org/10.1111/j.1538-7836.2008.03061.x.
Kahn SR. How I treat postthrombotic syndrome. Blood. 2009;114:4624–31. https://doi.org/10.1182/blood-2009-07-199174.
Beitland S, Sandven I, Kjaervik LK, Sandset PM, Sunde K, Eken T. Thromboprophylaxis with low molecular weight heparin versus unfractionated heparin in intensive care patients: a systematic review with meta-analysis and trial sequential analysis. Intensive Care Med. 2015;41:1209–19. https://doi.org/10.1007/s00134-015-3840-z.
Schunemann HJ, Cushman M, Burnett AE, Kahn SR, Beyer-Westendorf J, Spencer FA, et al. American Society of Hematology 2018 guidelines for management of venous thromboembolism: prophylaxis for hospitalized and nonhospitalized medical patients. Blood Adv. 2018;2:3198–225. https://doi.org/10.1182/bloodadvances.2018022954.
NICE Guideline. Venous thromboembolism in over 16s: reducing the risk of hospital-acquired deep vein thrombosis or pulmonary embolism 2018.
The PROTECT Investigators for the Canadian Critical Care Trials Group and the Australian and New Zealand Intensive Care Society Clinical Trials Group. Dalteparin versus unfractionated heparin in critically Ill patients. N Engl J Med. 2011;364:1305–14. https://doi.org/10.1056/NEJMoa1014475.
Arabi YM, Al-Hameed F, Burns KEA, Mehta S, Alsolamy SJ, Alshahrani MS, et al. Adjunctive intermittent pneumatic compression for venous thromboprophylaxis. N Engl J Med. 2019;380:1305–15. https://doi.org/10.1056/NEJMoa1816150.
Schultz DJ, Brasel KJ, Washington L, Goodman LR, Quickel RR, Lipchik RJ, et al. Incidence of asymptomatic pulmonary embolism in moderately to severely injured trauma patients. J Trauma. 2004;56:723–7.
Minet C, Lugosi M, Savoye PY, Menez C, Ruckly S, Bonadona A, et al. Pulmonary embolism in mechanically ventilated patients requiring computed tomography: prevalence, risk factors, and outcome. Crit Care Med. 2012;40:3202–8. https://doi.org/10.1097/CCM.0b013e318265e461.
Beitland S, Wimmer H, Lorentsen T, Jacobsen D, Drægni T, Brunborg C, et al. Venous thromboembolism in the critically ill: a prospective observational study of occurrence, risk factors and outcome. Acta Anaesthesiol Scand. 2019;63:630–8. https://doi.org/10.1111/aas.13316.
Kaplan D, Charles Casper T, Gregory Elliott C, Men S, Pendleton RC, Kraiss LW, et al. VTE incidence and risk factors in patients with severe sepsis and septic shock. Chest. 2015;148:1224–30. https://doi.org/10.1378/chest.15-0287.
Viarasilpa T, Panyavachiraporn N, Marashi SM, Van Harn M, Kowalski RG, Mayer SA. Prediction of symptomatic venous thromboembolism in critically ill patients: the ICU-venous thromboembolism score. Crit Care Med. 2020;48:E470–9. https://doi.org/10.1097/CCM.0000000000004306.
Lim W, Meade M, Lauzier F, Zarychanski R, Mehta S, Lamontagne F, et al. Failure of anticoagulant thromboprophylaxis: risk factors in medical-surgical critically ill patients. Crit Care Med. 2015;43:401–10. https://doi.org/10.1097/CCM.0000000000000713.
Lauzier F, Muscedere J, Deland E, Kutsogiannis DJ, Jacka M, Heels-Ansdell D, et al. Thromboprophylaxis patterns and determinants in critically ill patients: a multicenter audit. Crit Care. 2014;18:R82. https://doi.org/10.1186/cc13844.
Chan NC, Stehouwer AC, Hirsh J, Ginsberg JS, Alazzoni A, Coppens M, et al. Lack of consistency in the relationship between asymptomatic DVT detected by venography and symptomatic VTE in thromboprophylaxis trials. Thromb Haemost. 2015;114:1049–57. https://doi.org/10.1160/TH14-12-1006.
Arabi YM, Burns KEA, Alsolamy SJ, Alshahrani MS, Al-Hameed FM, Arshad Z, et al. Surveillance or no surveillance ultrasonography for deep vein thrombosis and outcomes of critically ill patients: a pre-planned sub-study of the PREVENT trial. Intensive Care Med. 2020;46:737–46. https://doi.org/10.1007/s00134-019-05899-1.
Hiemstra B, Eck RJ, Koster G, Wetterslev J, Perner A, Pettilä V, et al. Clinical examination, critical care ultrasonography and outcomes in the critically ill: Cohort profile of the Simple Intensive Care Studies-I. BMJ Open. 2017;7:8–11. https://doi.org/10.1136/bmjopen-2017-017170.
Wiersema R, Castela Forte JN, Kaufmann T, De Haas RJ, Koster G, Hummel YM, et al. Observational study protocol for repeated clinical examination and critical care ultrasonography within the simple intensive care studies. J Vis Exp. 2019;2019:58802. https://doi.org/10.3791/58802.
von Elm E, Altman D, Egger M, Stuart P, Gotzsche P, Vandenbroucke J. The strengthening the reporting of observational studies in epidemiology (STROBE) statement: guidelines for reporting observational Studies. Ann Intern Med. 2007;147:573–7.
Stuck AK, Spirk D, Schaudt J, Kucher N. Risk assessment models for venous thromboembolism in acutely ill medical patients. A systematic review. Thromb Haemost. 2017;117:801–8. https://doi.org/10.1160/TH16-08-0631.
van Buuren S, Groothuis-Oudshoorn K. mice: multivariate imputation by chained equations in R. J Stat Softw. 2011. https://doi.org/10.18637/jss.v045.i03.
Sterne JAC, White IR, Carlin JB, Spratt M, Royston P, Kenward MG, et al. Multiple imputation for missing data in epidemiological and clinical research: potential and pitfalls. BMJ. 2009;338:b2393. https://doi.org/10.1136/bmj.b2393.
Wood A, White I, Royston P. How should variable selection be performed with multiply imputed data? Stat Med. 2008;27:3227–46. https://doi.org/10.1002/sim.3177.
Austin PC, Lee DS, Ko DT, White IR. Effect of variable selection strategy on the performance of prognostic models when using multiple imputation. Circ Cardiovasc Qual Outcomes. 2019;12:1–14. https://doi.org/10.1161/CIRCOUTCOMES.119.005927.
Shintani AK, Girard TD, Eden SK, Arbogast PG, Moons KGM, Ely EW. Immortal time bias in critical care research: Application of time-varying cox regression for observational cohort studies. Crit Care Med. 2009;37:2939–45. https://doi.org/10.1097/CCM.0b013e3181b7fbbb.
Klok FA, Kruip MJHA, van der Meer NJM, Arbous MS, Gommers D, Kant KM, et al. Incidence of thrombotic complications in critically ill ICU patients with COVID-19. Thromb Res. 2020;191:145–7. https://doi.org/10.1016/j.thromres.2020.04.041.
Obi AT, Tignanelli CJ, Jacobs BN, Arya S, Park PK, Wakefield TW, et al. Empirical systemic anticoagulation is associated with decreased venous thromboembolism in critically ill influenza A H1N1 acute respiratory distress syndrome patients. J Vasc Surg Venous Lymphat Disord. 2019;7:317–24. https://doi.org/10.1016/j.jvsv.2018.08.010.
Spyropoulos AC, Anderson FAJ, FitzGerald G, Decousus H, Pini M, Chong BH, et al. Predictive and associative models to identify hospitalized medical patients at risk for VTE. Chest. 2011;140:706–14. https://doi.org/10.1378/chest.10-1944.
Kahale LA, Tsolakian IG, Hakoum MB, Matar CF, Barba M, Yosuico VE, et al. Anticoagulation for people with cancer and central venous catheters. Cochrane Database Syst Rev. 2018. https://doi.org/10.1002/14651858.CD006468.pub6.
Acknowledgements
We are very grateful to all members of the SICS study group for their participation in data collection.
Funding
Ruben J. Eck is supported by a personal grant from the ‘Groninger AGIKO programme,’ funded by the University of Groningen. This programme supports young clinicians who combine medical specialist training with obtaining a PhD degree. The university had no role in the design or conduct of the study, analysis or interpretation of the data, review or approval of the manuscript, or the decision to submit the manuscript for publication.
Author information
Authors and Affiliations
Contributions
RJ, LH, RW, and BH collected data. RJ and CHLT conducted the analyses. IvdH and FK conceived the study. RJ, ROB, KM, IvdH and FK designed the protocol for this analysis. CHLT, NG, ROB, KM, IvdH, KM, and FK critically reviewed the manuscript for important intellectual content. All authors critically reviewed the manuscript and agreed with the final version and findings. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
In unresponsive patients, informed consent was first obtained from the legal representatives. Consent for the use of the study data was asked at a later time if the patient recovered consciousness. If the patient died before consent was obtained, the study data was used, and the legal representatives were informed of the study. The local institutional review board (METc Groningen) approved both cohort studies (2015/004 and 2018/203) and the current analysis (2019/078).
Consent for publication
Not applicable.
Competing interests
KM reports grants from Bayer, Sanquin, and Pfizer; speaker fees from Bayer, Sanquin, Boehringer Ingelheim, BMS, and Aspen; travel support from Bayer, and consulting fees from Uniqure outside the submitted work; other authors have disclosed no potential conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Additional file 1
. Table S1. Prognostic factor definitions. Table S2. Missing data. Table S3. Prognostic factors for PE-LDVT and NLDVT: univariable analyses. Figure S1. Flow-chart of patient inclusion.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Eck, R.J., Hulshof, L., Wiersema, R. et al. Incidence, prognostic factors, and outcomes of venous thromboembolism in critically ill patients: data from two prospective cohort studies. Crit Care 25, 27 (2021). https://doi.org/10.1186/s13054-021-03457-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s13054-021-03457-0