Abstract
Background
For healthcare systems, an ageing population poses challenges in the delivery of equitable and effective care. Frailty assessment has the potential to improve care in the intensive care setting, but applying assessment tools in critical illness may be problematic. The aim of this systematic review was to evaluate evidence for the feasibility and reliability of frailty assessment in critical care.
Methods
Our primary search was conducted in Medline, Medline In-process, EMBASE, CINAHL, PsycINFO, AMED, Cochrane Database of Systematic Reviews, and Web of Science (January 2001 to October 2017). We included observational studies reporting data on feasibility and reliability of frailty assessment in the critical care setting in patients 16 years and older. Feasibility was assessed in terms of timing of evaluation, the background, training and expertise required for assessors, and reliance upon proxy input. Reliability was assessed in terms of inter-rater reliability.
Results
Data from 11 study publications are included, representing 8 study cohorts and 7761 patients. Proxy involvement in frailty assessment ranged from 58 to 100%. Feasibility data were not well-reported overall, but the exclusion rate due to lack of proxy availability ranged from 0 to 45%, the highest rate observed where family involvement was mandatory and the assessment tool relatively complex (frailty index, FI). Conventional elements of frailty phenotype (FP) assessment required modification prior to use in two studies. Clinical staff tended to use a simple judgement-based tool, the clinical frailty scale (CFS). Inter-rater reliability was reported in one study using the CFS and although a good level of agreement was observed between clinician assessments, this was a small and single-centre study.
Conclusion
Though of unproven reliability in the critically ill, CFS was the tool used most widely by critical care clinical staff. Conventional FP assessment required modification for general application in critical care, and an FI-based assessment may be difficult to deliver by the critical care team on a routine basis. There is a high reliance on proxies for frailty assessment, and the reliability of frailty assessment tools in critical care needs further evaluation.
Prospero registration number
Similar content being viewed by others
Background
As the proportion of older patients admitted to critical care rises [1, 2], there is a pressing need to understand how critical care might best support a population with potentially complex medical, physical and psychosocial concerns. Only recently have studies started to explore the relevance of frailty assessment to the care of critically ill adults [3, 4]. Related to, though distinct from, co-morbidity and disability, frailty is a term used to describe "a condition characterised by loss of biological reserve and vulnerability to poor resolution of homeostasis following a stressor event" [5]. Frailty implies an impaired ability to withstand the physiological disturbance of an acute illness, and although it becomes more prevalent with age it is not exclusive to an older population.
A range of methods to evaluate frailty are described in the literature [5,6,7,8], with the utility of a particular frailty assessment tool dependent on the purpose, setting, time available, and skill of the assessor [9]. For the acutely ill, assessment tools might best be described as one of: a judgment-based measure (e.g. the clinical frailty scale (CFS) [10]); a single physical performance measure (e.g. grip strength); a frailty phenotype (depending on the presence of typically three to five criteria [11]); an extended multidimensional assessment (e.g. Tilburg Frailty Indicator [12, 13]); and a frailty index, the number of accumulated deficits associated with adverse outcome presented as a proportion with respect to the total number (30 or more) of pre-specified possible deficits [14].
Previous systematic reviews have examined the psychometric properties of frailty assessment tools in primarily non-acute settings [6,7,8, 15]. However, the validity and reliability of an assessment tool is largely dependent on the setting and population in which it was developed and validated [8], and frailty assessment in the critically ill poses particular challenges. At the outset of critical illness, there is often a reliance on proxy respondents [4]. Furthermore, frailty is itself an independent risk factor for delirium, can coexist with dementia and is associated with disability [5]. Proxy ratings do not necessarily correspond with a subject's own assessment of function or quality of life during the recovery from critical illness [16,17,18,19]. Last, there is inherent risk of inadvertently ascribing features of acute illness to underlying frailty [20] and of recall bias with retrospective inquiry. Given these concerns, we aimed to systematically review the literature to establish the feasibility and reliability of frailty assessment in the critically ill.
Methods
Our review was performed according to recommendations for the systematic review of observational studies [21] and was registered prospectively via PROSPERO (PROSPERO, https://www.crd.york.ac.uk/PROSPERO/display_record.php?RecordID=52073) with registration number: CRD42016052073.
Eligibility criteria
The inclusion criteria were:
-
1.
The study included adult (16 years and over) patients being managed in a critical care environment.
-
2.
The study involved the application of a multidimensional frailty assessment tool.
-
3.
The study presented data relating to the feasibility of frailty assessment in the critically ill (timing of evaluation, the background, training and expertise required for assessors, and reliance upon proxy input), and/or of the reliability of frailty assessment in the critically ill.
Reviews, case reports and case series were excluded; studies that collected data retrospectively were not excluded, but the potential bias associated with retrospective as opposed to prospective study was considered. Data from the control arm of randomised controlled trials (RCTs) were considered for inclusion if the trial eligibility criteria identified a study population that was representative of the general critical care population. Studies were limited to English language publications from 2001 onwards. However, there was no restriction on the basis of publication status, provided eligibility criteria were otherwise met.
Information sources
We searched the following databases from January 2001 to October 2017: Medline, Medline In-process, EMBASE, CINAHL, PsycINFO, AMED, Cochrane Database of Systematic Reviews, and Web of Science. Additional studies were sought from grey literature using the Open Grey database and by screening critical care conference abstracts, from the reference lists of papers and review articles, and through searches for full-text publication of relevant abstracts.
Data management
Two authors independently screened titles and abstracts. An additional author also contributed to hand-searching reference lists of identified papers and review articles. A spreadsheet was used to keep a log of all potentially relevant studies and reasons for inclusion or exclusion. In the event of disagreement following full-text review, consensus was achieved through discussion without recourse to a third author. Data from included studies were extracted using a standardised data collection proforma and additional information sought from trial authors where appropriate.
Data items
Study data extraction included: author, year, publication type, country, methodology and setting. Relevant patient characteristics of studied cohorts included: demographic data (age, gender), presence of co-morbidity, evidence of baseline level of dependence, primary reason for admission, surgical status, and severity of illness (according to established illness severity scales). Timing of frailty assessment was recorded (e.g. with reference to a point in time before the acute illness, at time of referral, at time of admission to critical care, or during recovery from acute illness), and interval between assessments. Information on the participation of the patient in the frailty assessment process was collected, as was the background of the individual(s) making the assessment of frailty.
Outcomes and prioritisation
Feasibility of the frailty measurement tools in critical care was assessed on the basis of time taken to perform the assessment, training, and expertise required to implement, the proportion of potentially eligible patients excluded, and reasons for exclusion (e.g. due to lack of proxy).
Given that frailty state is not static in the context of an acute illness [4, 22], in assessing reliability our primary interest was the contemporaneous measure of inter-rater reliability. Where available, for ordinal scores we extracted the linear weighted kappa in line with consensus-based standards [23].
Risk of bias for individual studies
We did not identify any eligible RCTs, but for observational studies the risk of bias was assessed using the Newcastle-Ottawa checklist [24] according to the domains of selection, comparability, exposure, and outcome. For each domain, a judgement of low, unclear, or high risk of bias was made. Studies were considered as at overall low risk of bias if all domains were judged as low risk; studies were considered high risk if any domains were deemed high risk. Depending on number and risk of studies identified, it was intended that sensitivity analysis might be performed excluding high-risk studies.
Results
Study selection
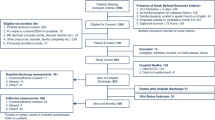
Search results are summarised in the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) [25] diagram (Fig. 1). There were 2180 articles identified, of which 69 were considered potentially eligible. Following full-text review, a total of 11 study publications were included [26,27,28,29,30,31,32,33,34,35,36], representing 8 study cohorts and a total of 7761 patients.
Flow diagram of included studies [25]
Study characteristics
The characteristics of included studies are summarised in Tables 1 and 2. Two research groups presented separate analyses of study cohorts in multiple publications (Bagshaw [26,27,28] and Heyland [33, 34]) but for the purposes of this review each study cohort was considered as a single study. Four studies were conducted in North America [26,27,28,29, 33,34,35], three in Europe (including one large study involving 21 countries) [30, 31, 36] and one in Australia [32]. The majority of studies were multi-centre [26,27,28,29,30, 33,34,35,36] and set in mixed medical-surgical ICUs. The median sample size was 385 patients (range 30–5021). Four of the studies adopted age restrictions: age 50 years or more [26,27,28], 65 years or more [30], and 80 years or more [33, 34, 36]. Only one study explicitly excluded patients with severe cognitive disease, including dementia [29]. The majority of patients were male, and 61% received invasive ventilation.
In the majority of studies, the main aim was assessment of predictive validity (e.g. in terms of mortality, length of stay, disability, and health-related quality of life). In only one study was the primary intention to evaluate reliability of frailty assessment [31], and in only one other was the feasibility of frailty assessment an explicit outcome [32]. However, each of the other six studies included presented data sufficient to enable evaluation of the feasibility of frailty assessment in critical care.
Risk of bias within studies
Six studies were considered at unclear overall risk of bias [26,27,28,29,30,31, 35, 36] and two studies were considered at low overall risk of bias [32,33,34] (Table 3). Regarding selection bias, the Bagshaw, Fisher, and Heyland reports were considered at low risk, since potential differences between patients recruited and not recruited had been explored [26,27,28, 32,33,34]. In terms of comparability, the Fisher, Heyland, and Hope reports were considered at low risk of bias, since in these studies the proxy contribution to assessment of frailty was quantified [32,33,34,35]. Only one study explored the reliability of frailty assessment, for which outcome bias was considered low risk due to the adoption of blinded assessment [31]. No studies were considered high risk and sensitivity analysis was therefore not performed.
Assessment of frailty
All studies evaluated frailty using a clinical frailty scale (CFS) [10]; six studies used a 9-point scale [26,27,28, 30, 31, 35, 36] (see Fig. 2) and two a 7-point scale [29, 33, 34]. Additional scoring systems were used in three studies [30, 33,34,35]. Two studies utilised a frailty phenotype (FP) assessment, identifying frailty on the basis of the following domains: shrinking, weakness, slowness, low-level physical activity, and self-reported exhaustion [11], but modified for use in the critically ill (see Table 4) [30, 35]. Furthermore, Hope and colleagues supplemented these FP domains with questions relating to cognitive and to sensory impairment [35]. One study utilised a frailty index based on a 43-item comprehensive geriatric assessment (CGA) [33, 34].
Clinical frailty scale [10]
Timing of frailty assessment was available in seven studies. Frailty was assessed at critical care admission [30], within the first 24 hours [32, 36] or first 72 hours of critical care admission [29, 33,34,35] (Table 5). A variety of reference points for assessment were adopted: the subject's condition before ICU admission [32], before hospital admission [26,27,28], before onset of critical illness [29], before acute illness and hospital admission [36], 2 weeks before hospital admission [31, 33, 34] or one month before hospital admission [30].
Feasibility of frailty assessment
A member of the research team assessed frailty in five studies [26,27,28,29, 31, 33,34,35]; in three studies critical care doctors with clinical rather than research responsibilities assessed frailty using a CFS [31, 35] or a CFS and FP [30]; in one study critical care nurses and doctors assessed frailty using a CFS [36], and in one study it was the nurse-in-charge or next-of-kin (with nurse guidance) who assigned a CFS score [32] (Table 6). Researchers received specific training to familiarise themselves with the study and assessment tool(s) in four studies [29, 31, 33,34,35]; critical care nurses received CFS training in the form of a series of lectures in one study [32]. In the remaining three studies, training clinical staff to use CFS took place in a staff meeting [30], at the bedside [31, 35] or was deemed not to need particular training "since the description combined with illustration is intuitive" [36]. The times required for training and to perform assessments were for the most part not captured during the course of included studies (Table 6).
Two studies excluded patient involvement in frailty assessment in their methodology [32,33,34]. Of these, availability of a family member was a requirement for study enrolment in Heyland's study [33, 34]. In Fisher's study, the CFS assessment was expected to be made by the next-of-kin under the guidance of the bedside nurse, using a standardised introduction; however, CFS assessment was made by the nurse-in-charge if the next-of-kin was unavailable in the first 24 hours of critical care admission [32]. The researchers reported that when no assessment had been made, patients were more likely to have been post-operative or to have had a shorter critical care stay. In Le Maguet [30], 31% of patients were able to interact with an interviewer to enable assessment, and in Hope [35], 42% patients contributed to frailty assessment. In the other three studies, patient participation was not recorded.
Where recorded, a proxy was involved in 58% [35], 69% [30], 73% [32] and 100% [33, 34] of frailty assessments (Table 6). Fisher found that it was not possible to approach the next of kin for involvement in assessment in 27% cases within the first 24 hours of critical care admission; however, since the nurse in charge could make a CFS assessment on the basis of medical records, this did not prohibit frailty assessment [32]. Flaatten did not specify the contribution of patient or proxy to assessment, but noted that CFS assessment was achieved in 99.8% of cases included [36]. Hope noted that in some instances surrogates were unable to answer questions relating to an assessment of frailty according to FP assessment, for example, according to domains of weight loss (5% of cases) or loss of energy (3% of cases) [35]. Le Maguet also found that "several components of the FP score, notably those that evaluate performance, were difficult to explore in ICU patients" [30]. Overall, screened patients excluded from enrolment due to lack of proxy availability ranged from 0 to 45% in five studies [29, 30, 32,33,34,35]: the highest exclusion rate was in Heyland's study, in which frailty was assessed according to a 43-item CGA and a CFS, and in which family involvement was an absolute requirement for enrolment [33, 34].
Reliability of frailty assessment
Reliability of frailty assessment was assessed in only one study, which evaluated the inter-rater reliability of frailty assessment using a CFS as a comparison between two groups, a group of medical students and a group of critical care doctors. Linear weighted kappa was 0.64 (95% confidence intervals 0.40 to 0.87, p < 0.0001), suggesting good agreement. However, this was a small (n = 30), single-centre study comparing only two groups of assessors (medical students and critical care doctors, excluding other members of the clinical team), and which did not make reference to the relative contributions of the critical care patient or a proxy.
Discussion
In assessing the feasibility of frailty assessment, we have made a distinction between those primarily involved in clinical and in research roles in view of anticipated differences in training and time available to apply assessment tools. Though not well-described, clinical staff for the most part appear to have received relatively little training with regards the application of frailty assessment tools compared with those described as "research coordinator" or "study personnel." Despite this, the high proportion of patients among included studies undergoing frailty assessment using the judgement-based CFS by clinical staff is likely to reflect its simplicity and ease of application [36]. Indeed CFS assessment seemed achievable even in the absence of family contact [32].
With regard to other assessment methods, the two studies utilising FP assessment reported difficulties with some components of FP assessment, despite making adaptations for a critically ill population. However, FP assessment was used by both clinical [30] and research staff [35]. The early phase of critical illness typically precludes elements of frailty assessment, which require demonstration rather than description (e.g. grip strength and gait speed), though such assessment appears feasible for ICU survivors much nearer to hospital discharge [37]. The consequences of such modifications for frailty classification and predictive validity in this population are uncertain [38]. FI-CGA was used to assess frailty in only one study, and although the time required to administer the 43-item questionnaire to a family member by the research coordinator was not recorded, it is unclear whether this would be too time-consuming to be feasibly delivered by a critical care team on a routine basis. Recent research has reported the development and validation of a 36-item electronic frailty index (eFI) using routinely available electronic medical record (EMR) data [39], which may be an attractive approach for critical care but requires further validation in this context.
A high proportion of enrolled patients were invasively ventilated and only a minority able to participate directly in frailty assessment. There is clearly a heavy reliance on proxy input for frailty assessment in this population, particularly when detailed information is required [32,33,34], and Heyland's study illustrates the difficulty of coordinating the availability of assessor and an appropriate family member when FI-CGA assessment is made by a limited number of trained individuals.
A dependence on proxy input is also highly relevant when considering the reliability of frailty assessment in the critically ill. We identified only one small clinical study that investigated the inter-rater reliability of CFS assessment between a group of critical care doctors and a group of medical students [31]. Although there was a good level of agreement, the study did not capture the relative contributions of the patient or their proxies to frailty assessment. Furthermore, we found no study that had attempted to compare assessment of frailty between clinical staff and critically ill patients or their relatives, or to evaluate the influence of clinical background, seniority, and training on frailty assessment. When carefully selected, other investigators have identified a high level of agreement between subject and proxy in terms of functional status after critical illness [40]. However, the retrospective nature of frailty assessment (in the manner identified in included studies) makes it prone to recall bias, particularly in the context of acute and sub-acute chronic illness [14, 41]. Furthermore, subjective elements (e.g. "exhaustion" [30, 35]) rather than observable criteria may be especially susceptible to differences between proxy and subject ratings [42, 43]. The reliability of frailty assessment by clinicians is an important issue; in other settings, escalation decision-making following emergency admission may be made on the basis of a perception of baseline cognitive and functional status, which at best only modestly correlates with that of patient or relative [44].
There are several strengths to this review. We prospectively registered our review protocol and have followed rigorous methodology to identify, evaluate, and summarise the current evidence on feasibility and reliability of frailty assessments in the critically ill. However, we recognise some limitations. Assessment of the feasibility and reliability of frailty assessment was the intended outcome of only two of the eight studies included, and this is reflected in absent or incomplete data on factors that may have contributed to inclusion or exclusion of patients (e.g. to "missed caregiver"), the background of assessor, the training and time taken to perform assessment, background of any proxies, and the relative involvement of patient and proxy in the assessments. As a consequence, for the purposes of evaluating feasibility and/or reliability of frailty assessment in the critically ill, only two studies were considered at low overall risk of bias.
However, our review has a number of implications for clinical practice. We found evidence that frailty assessment can feasibly be performed by different clinical members of the critical care team (whether physician, nurse or medical student), that patient participation in such assessment will be achieved in a minority of cases, and that a qualifying proxy is usually required. We found limited data indicating that frailty can be reliably assessed by clinicians in the critical care setting. Given the challenges inherent in frailty assessment in critical illness, more research is needed regarding the reliability of frailty assessment tools in critical care before frailty assessment can be used to aid clinical decision-making and/or trigger interventions.
This review highlights areas for future research. Frailty is a dynamic state, and frailty assessment in the context of variations in health trajectories prior to critical illness needs exploration. Further study is required to compare the relative performance of frailty assessment tools in critical care, taking into account the reference point for assessment, the background and training of the assessor(s), the capacity of the patient, and the relationship between patient and proxy. In particular, the relative performance of frailty assessment using routinely captured data versus bedside frailty assessment should be evaluated in this population. Last, a clearer understanding of the training required and the time taken to make an assessment of frailty needs to be considered in the context of the potential benefits of making that assessment.
Conclusions
This review has found little evidence of reliability and only limited evidence on the feasibility of frailty assessment in the critically ill. CFS was the most widely applied assessment tool by clinical staff, conventional FP assessment required modification for general application in critical care, and FI-based assessment may be difficult to deliver by the critical care team on a routine basis. Additional research is required to investigate the resource implications of routine use of frailty tools, to evaluate reliability when used by a range of clinical personnel, to investigate the use of routinely available EMR data for identifying frailty, and to study reliability in the presence or absence of clinical proxies before recommending widespread application in routine critical care practice.
Abbreviations
- ADLs:
-
Activities of daily living
- CFS:
-
Clinical frailty scale
- CGA:
-
Comprehensive geriatric assessment
- eFI:
-
Electronic frailty index
- EMR:
-
Electronic medical record
- FI:
-
Frailty index
- FP:
-
Frailty phenotype
- ICU:
-
Intensive care unit
- IQR:
-
Interquartile range
- PRISMA:
-
Preferred Reporting Items for Systematic Reviews and Meta-Analyses
- SD:
-
Standard deviation
- TFI:
-
Tilburg Frailty Indicator
References
Bagshaw SM, Webb SA, Delaney A, George C, Pilcher D, Hart GK, Bellomo R. Very old patients admitted to intensive care in Australia and New Zealand: a multi-centre cohort analysis. Crit Care. 2009;13(2):R45.
Ihra GC, Lehberger J, Hochrieser H, Bauer P, Schmutz R, Metnitz B, Metnitz PG. Development of demographics and outcome of very old critically ill patients admitted to intensive care units. Intensive Care Med. 2012;38(4):620–6.
Muscedere J, Waters B, Varambally A, Bagshaw SM, Boyd JG, Maslove D, Sibley S, Rockwood K. The impact of frailty on intensive care unit outcomes: a systematic review and meta-analysis. Intensive Care Med. 2017;43(8):1105–22.
McDermid RC, Stelfox HT, Bagshaw SM. Frailty in the critically ill: a novel concept. Crit Care. 2011;15(1):301.
Clegg A, Young J, Iliffe S, Rikkert MO, Rockwood K. Frailty in elderly people. Lancet. 2013;381(9868):752–62.
de Vries NM, Staal JB, van Ravensberg CD, Hobbelen JS, Olde Rikkert MG. Nijhuis-van der Sanden MW. Outcome instruments to measure frailty: a systematic review. Ageing Res Rev. 2011;10(1):104–14.
Dent E, Kowal P, Hoogendijk EO. Frailty measurement in research and clinical practice: a review. Eur J Intern Med. 2016;31:3–10.
Sutton JL, Gould RL, Daley S, Coulson MC, Ward EV, Butler AM, Nunn SP, Howard RJ. Psychometric properties of multicomponent tools designed to assess frailty in older adults: a systematic review. BMC Geriatr. 2016;16:55.
Buta BJ, Walston JD, Godino JG, Park M, Kalyani RR, Xue QL, Bandeen-Roche K, Varadhan R. Frailty assessment instruments: systematic characterization of the uses and contexts of highly-cited instruments. Ageing Res Rev. 2016;26:53–61.
Rockwood K, Song X, MacKnight C, Bergman H, Hogan DB, McDowell I, Mitnitski A. A global clinical measure of fitness and frailty in elderly people. CMAJ. 2005;173(5):489–95.
Fried LP, Tangen CM, Walston J, Newman AB, Hirsch C, Gottdiener J, Seeman T, Tracy R, Kop WJ, Burke G, et al. Frailty in older adults: evidence for a phenotype. J Gerontol A Biol Sci Med Sci. 2001;56(3):M146–56.
Gobbens RJ, van Assen MA, Luijkx KG, Wijnen-Sponselee MT, Schols JM. The Tilburg Frailty Indicator: psychometric properties. J Am Med Dir Assoc. 2010;11(5):344–55.
Jones DM, Song X, Rockwood K. Operationalizing a frailty index from a standardized comprehensive geriatric assessment. J Am Geriatr Soc. 2004;52(11):1929–33.
Hogan DB, Maxwell CJ, Afilalo J, Arora RC, Bagshaw SM, Basran J, Bergman H, Bronskill SE, Carter CA, Dixon E, et al. A scoping review of frailty and acute care in middle-aged and older individuals with recommendations for future research. Can Geriatr J. 2017;20(1):22–37.
Apostolo J, Cooke R, Bobrowicz-Campos E, Santana S, Marcucci M, Cano A, Vollenbroek-Hutten M, Germini F, Holland C. Predicting risk and outcomes for frail older adults: an umbrella review of frailty screening tools. JBI Database System Rev Implement Rep. 2017;15(4):1154–208.
Neumann PJ, Araki SS, Gutterman EM. The use of proxy respondents in studies of older adults: lessons, challenges, and opportunities. J Am Geriatr Soc. 2000;48(12):1646–54.
Li M, Harris I, Lu ZK. Differences in proxy-reported and patient-reported outcomes: assessing health and functional status among medicare beneficiaries. BMC Med Res Methodol. 2015;15:62.
Scales DC, Tansey CM, Matte A, Herridge MS. Difference in reported pre-morbid health-related quality of life between ARDS survivors and their substitute decision makers. Intensive Care Med. 2006;32(11):1826–31.
Dinglas VD, Gifford JM, Husain N, Colantuoni E, Needham DM. Quality of life before intensive care using EQ-5D: patient versus proxy responses. Crit Care Med. 2013;41(1):9–14.
Hilmer SN, Perera V, Mitchell S, Murnion BP, Dent J, Bajorek B, Matthews S, Rolfson DB. The assessment of frailty in older people in acute care. Australas J Ageing. 2009;28(4):182–8.
Stroup DF, Berlin JA, Morton SC, Olkin I, Williamson GD, Rennie D, Moher D, Becker BJ, Sipe TA, Thacker SB. Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis Of Observational Studies in Epidemiology (MOOSE) group. JAMA. 2000;283(15):2008–12.
Turner G, Clegg A: Best practice guidelines for the management of frailty: a British Geriatrics Society, Age UK and Royal College of General Practitioners report; 2014.
Mokkink LB, Terwee CB, Patrick DL, Alonso J, Stratford PW, Knol DL, Bouter LM, de Vet HC. The COSMIN checklist for assessing the methodological quality of studies on measurement properties of health status measurement instruments: an international Delphi study. Qual Life Res. 2010;19(4):539–49.
The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses [http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp]. Accessed 10 Apr 2017.
Moher D, Liberati A, Tetzlaff J, Altman DG, Group P. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med. 2009;6(7):e1000097.
Bagshaw SM, Stelfox HT, McDermid RC, Rolfson DB, Tsuyuki RT, Baig N, Artiuch B, Ibrahim Q, Stollery DE, Rokosh E, et al. Association between frailty and short- and long-term outcomes among critically ill patients: a multicentre prospective cohort study. Can Med Assoc J. 2014;186(2):E95–E102.
Bagshaw SM, Stelfox HT, Johnson JA, McDermid RC, Rolfson DB, Tsuyuki RT, Ibrahim Q, Majumdar SR. Long-Term Association Between Frailty and Health-Related Quality of Life Among Survivors of Critical Illness: a prospective multicenter cohort study. Crit Care Med. 2015;43(5):973–82.
Bagshaw M, Majumdar SR, Rolfson DB, Ibrahim Q, McDermid RC, Stelfox HT. A prospective multicenter cohort study of frailty in younger critically ill patients. Crit Care. 2016;20(1):175. Erratum in: Crit Care. 2016;20(1):223.
Brummel NE, Bell SP, Girard TD, Pandharipande PP, Jackson JC, Morandi A, Thompson JL, Chandrasekhar R, Bernard GR, Dittus RS, et al. Frailty and subsequent disability and mortality among patients with critical illness. Am J Respir Crit Care Med. 2017;196(1):64–72.
Le Maguet P, Roquilly A, Lasocki S, Asehnoune K, Carise E, Saint Martin M, Mimoz O, Le Gac G, Somme D, Cattenoz C, et al. Prevalence and impact of frailty on mortality in elderly ICU patients: a prospective, multicenter, observational study. Intensive Care Med. 2014;40(5):674–82.
Pugh RJ, Thorpe CM, Subbe CP. A critical age: can we reliably measure frailty in critical care? Crit Care. 2017;21(1):121.
Fisher C, Karalapillai DK, Bailey M, Glassford NG, Bellomo R, Jones D. Predicting intensive care and hospital outcome with the Dalhousie Clinical Frailty Scale: a pilot assessment. Anaesth Intensive Care. 2015;43(3):361–8.
Heyland DK, Garland A, Bagshaw SM, Cook D, Rockwood K, Stelfox HT, Dodek P, Fowler RA, Turgeon AF, Burns K, et al. Recovery after critical illness in patients aged 80 years or older: a multi-center prospective observational cohort study. Intensive Care Med. 2015;41(11):1911–20.
Heyland D, Cook D, Bagshaw SM, Garland A, Stelfox HT, Mehta S, Dodek P, Kutsogiannis J, Burns K, Muscedere J, et al. The very elderly admitted to ICU: a quality finish? Crit Care Med. 2015;43(7):1352–60.
Hope AA, Hsieh SJ, Petti A, Hurtado-Sbordoni M, Verghese J, Gong MN. Assessing the usefulness and validity of frailty markers in critically ill adults. Ann Am Thorac Soc. 2017;14(6):952–9.
Flaatten H, De Lange DW, Morandi A, Andersen FH, Artigas A, Bertolini G, Boumendil A, Cecconi M, Christensen S, Faraldi L, et al. The impact of frailty on ICU and 30-day mortality and the level of care in very elderly patients (>/= 80 years). Intensive Care Med. 2017;43(12):1820–1828.
Baldwin MR, Reid MC, Westlake AA, Rowe JW, Granieri EC, Wunsch H, Dam TT, Rabinowitz D, Goldstein NE, Maurer MS, et al. The feasibility of measuring frailty to predict disability and mortality in older medical intensive care unit survivors. J Crit Care. 2014;29(3):401–8.
Theou O, Cann L, Blodgett J, Wallace LM, Brothers TD, Rockwood K. Modifications to the frailty phenotype criteria: Systematic review of the current literature and investigation of 262 frailty phenotypes in the Survey of Health, Ageing, and Retirement in Europe. Ageing Res Rev. 2015;21:78–94.
Clegg A, Bates C, Young J, Ryan R, Nichols L, Ann Teale E, Mohammed MA, Parry J, Marshall T. Development and validation of an electronic frailty index using routine primary care electronic health record data. Age Ageing. 2016;45(3):353–60.
Ahasic AM, Van Ness PH, Murphy TE, Araujo KL, Pisani MA. Functional status after critical illness: agreement between patient and proxy assessments. Age Ageing. 2015;44(3):506–10.
Iwashyna TJ. Trajectories of recovery and dysfunction after acute illness, with implications for clinical trial design. Am J Respir Crit Care Med. 2012;186(4):302–4.
Carod-Artal FJ, Ferreira Coral L, Stieven Trizotto D, Menezes MC. Self- and proxy-report agreement on the Stroke Impact Scale. Stroke. 2009;40(10):3308–14.
Oczkowski C, O'Donnell M. Reliability of proxy respondents for patients with stroke: a systematic review. J Stroke Cerebrovasc Dis. 2010;19(5):410–6.
Rodriguez-Molinero A, Lopez-Dieguez M, Tabuenca AI, de la Cruz JJ, Banegas JR. Physicians' impression on the elders' functionality influences decision making for emergency care. Am J Emerg Med. 2010;28(7):757–65.
Acknowledgements
The authors are very grateful for the assistance of Deidre Andre, Research Librarian at the University of Leeds, with the design and conduct of the search strategies, and to Nia Morris, Clinical Librarian at Betsi Cadwaldr University Health Board, for her help re-running the search strategies. We are also extremely grateful for the additional information provided by the following study authors: Nathan Brummel, Hans Flaatten, Daren Heyland, Aluko Hope and Philippe Seguin.
Funding
This study was unfunded.
Availability of data and material
The datasets used and/or analysed during the current study are available from the corresponding author on reasonable request.
Author information
Authors and Affiliations
Contributions
RP, CT, CS, NL, and AC conceived the idea for this systematic review. RP and AC contributed to design of the review. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated.
About this article
Cite this article
Pugh, R., Ellison, A., Pye, K. et al. Feasibility and reliability of frailty assessment in the critically ill: a systematic review. Crit Care 22, 49 (2018). https://doi.org/10.1186/s13054-018-1953-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s13054-018-1953-9