Abstract
Background
Initiation of breastfeeding immediately after birth, exclusive breastfeeding, and continuous breastfeeding for at least 2 years lower the risk of newborn deaths. This study was conducted to examine the trends and factors associated with early initiation of breastfeeding, exclusive breastfeeding and duration of breastfeeding in Ethiopia.
Methods
Data for this study were extracted from the Ethiopian Demographic and Health Survey 2016. A total of 5122 children were included in the analysis. Multivariate logistic regression analysis, and Cox proportional hazards model were fitted to find the factors associated with breastfeeding practices. Reported p - values < 0.05 or a 95% Confidence Interval of Odds Ratio/Hazard Ratio excluding one was considered as significant association with early initiation of breastfeeding, exclusive breastfeeding, duration of breastfeeding and independent variables.
Results
About 81.8% of the children initiated breastfeeding within 1 h of birth and during the day before an interview, 47% were exclusively breastfed during the first 6 months. The median duration of breastfeeding was 22 months (22 ± 0.50 months 95% Confidence Interval [CI] 21.01–22.99). Rural residents (Odds Ratio [OR] 0.71, 95% CI 0.51, 0.99), mothers with no antenatal follow up (OR 0.75, 95% CI 0.57, 0.99), caesarean birth (OR 0.80, 95% CI 0.66, 0.96) and home delivery were associated with low initiation of breastfeeding within 1 h of birth. Mothers with no/primary education (OR 0.62, 95% CI 0.40, 0.96), no baby postnatal checkup (OR 0.53, 95% CI 0.39, 0.73), average/larger size of a child at birth (OR 0.80, 95% CI 0.65, 0.99) and deliveries outside of health centers were significantly associated with non-exclusive breastfeeding at the time of the interview. Further, mothers living in Amhara (Hazard Ratio [HR] 1.31, 95% CI 1.05, 1.64), Oromia (HR 1.27, 95% CI 1.04, 1.54), and Benishangul-Gumuz (HR 1.34, 95% CI 1.09, 1.65) regions had a longer duration of breastfeeding while Muslims, employed mothers, multiple births and poor economic level of households were associated with shorter durations of breastfeeding.
Conclusions
Rural residence, female sex, home delivery, caesarean birth, small birthweight baby and large family size were associated with late initiation of breastfeeding. Living in Affar, Somali, and Harari, primary education level of mothers, giving birth outside of health facilities, no antenatal care follow up, and no postnatal check-up were associated with non-exclusive breastfeeding, while younger age mothers, Muslims, giving birth outside of health facilities, and employed mothers were associated with shorter time to cessation of breastfeeding. Providing health education and counseling for mothers during and after pregnancy should be encouraged.
Similar content being viewed by others
Background
Globally, about 800,000 neonatal deaths are attributed to late initiation of breastfeeding and lack of exclusive breastfeeding [1]. Initiation of breastfeeding immediately after birth can reduce the risk of neonatal mortality in the first week of life by 22% globally [2]. Furthermore, exclusive breastfeeding of infants is strongly associated with a lower risk of post neonatal death [3, 4].
By the year 2030, the Sustainable Development Goals (SDG) target reducing neonatal deaths to 12 per 1000 live births, and under-five deaths to less than 25 per 1000 live births through eliminating preventable child deaths [5]. Sub-Saharan African (SSA) countries have the highest neonatal mortality rate, about 28 deaths per 100 live births annually. Ethiopia is one of the SSA countries with a high rate of neonatal and infant mortality. The latest Ethiopian Demographic and Health Survey [6] reported that 92% of children born 5 years preceding the survey, initiated breastfeeding within the first hour after birth, and 58% were exclusively breastfed the day before an interview. Under-five mortality has been declining in Ethiopia, where the majority of deaths occur in the neonatal and infant period caused by lack of important nutrients and by infections [6]. Initiating breastfeeding in the first 1 h after birth can decrease the risk of newborn infant mortality by about 45% and exclusively breastfed children were 14 times more likely to survive the first 6 months of life than non-breastfed children [7]. Under nutrition is the main causes of child mortality, and UNICEF 2010 estimated about 40 to 60% of under-five stunting were subjected to late initiation and non-exclusive breastfeeding [8].
Despite early initiation of breastfeeding, the majority of children do not breastfeed exclusively in the countries of Africa [9]. The World Health Organization (WHO) recommends early newborn breastfeeding initiation within 1 h of birth, exclusive breastfeeding for 6 months, and continued breastfeeding for 2 years or more in conjunction with complementary foods [10,11,12,13].
Breast milk has many benefits of ensuring a healthy child and the survival of a child. Several studies reported that the initiation of breastfeeding within a day was significantly associated with reducing low birthweight related neonatal mortality and infection related neonatal mortality among all live births [14,15,16,17]. Worldwide, 10% of the disease burden in under-five children were due to the non-exclusive breastfeeding. According to The Lancet, estimate suboptimal breastfeeding is a consequence of 1.4 million child deaths and 77% of child deaths are accounted for by non-exclusive breastfeeding in the first 6 months of birth [18]. The highest risk of inappropriate feeding during the first 6 months of life occurs in developing countries where 96% of all infant mortality is due to suboptimal breastfeeding [19]. Nutritional deficits among infants are immediate consequences of delayed breastfeeding and non-exclusive breastfeeding that leads to morbidity and mortality among children [20].
Breastfeeding prevalence is high in Ethiopia. However, the practice of exclusive breastfeeding among 0–6 months age children differs by regions. According to Ethiopian Demographic and Health Survey (DHS) 2016 nearly all children, i.e., 97% are breastfed at some points while only 58% of infants below the age of 6 months are exclusively breastfed. Among Ethiopian regions, the level of early initiation of breastfeeding and the median duration of exclusive breastfeeding are minimal in Affar region, 43% and 2.7 months, respectively, and median duration of predominant breastfeeding among children born 5 years preceding the survey were minimal for Somali region (3.8 months). In addition to breast milk, only 7% of children 6–23 months old receive the least acceptable dietary standards while only 14% of children had a sufficiently diverse diet [6]. In Ethiopia, the Ministry of Health (MoH) established the National Nutrition Program II (NNP II) and the National Guideline on Adolescent, Maternal, Infant, and the Young Child Nutrition initative 2016 targeted promoting optimal feeding and care practices, encouraging mothers to exclusively breastfeed their child for the first 6 months without any additional fluids or foods and continuing breastfeeding up to a child is 2 years old. Nearly three-fourth (73%) of children began breastfeeding within 1 hour of a birth and 92% within a day of birth. Eight percent of children received prelacteal feeding. In Affar region the percentage of prelacteal feeding was 41%.
According to various studies, and WHO/UNICEF report, the factors associated with breastfeeding practice differ with socioeconomic, demographic, behavioral and cultural factors of mothers, place and mode of delivery, professional counseling on breastfeeding, and obstetric and health service related factors [21,22,23]. Identifying factors associated with breastfeeding practices are essential to decrease the neonatal and infant death rates due to preventable causes from lack of necessary nutrients. Despite the fact that a number of studies have been done investigating the factors associated with early initiation time, exclusive breastfeeding and duration of breastfeeding in Ethiopia, breastfeeding practice is still less than optimal and more effort is needed. Thus, this study tries to assess the major risk factors of delayed initiation, exclusive breastfeeding and duration of breastfeeding, with consideration to various demographic, socioeconomic, and health service related factors, based on 2016 Ethiopia Demographic and Health Survey data. It may help to evaluate the Sustainable Development Goals (SDGs), aimed at reducing under-five death rates of 25 deaths per 1000 live births through increasing optimal feeding patterns among infants, and to avoid preventable childhood deaths by 2030 [24].
Methods
Study setting
The data for this study were extracted from the Ethiopian Demographic and Health Survey (EDHS) 2016 [6, 25]. The Central Statistical Agency (CSA) together with the Ministry of Health (MoH) and the Ethiopian Public Health Institute conducted the survey from January 18, 2016 - June 27, 2016 and The United States Agency for International Development (USAID) funded the survey. The nationwide survey has information on a range of socioeconomic and demographic factors of the population. It implemented a two-stage sampling within the nine regions and two administrative cities of a country. In the first stage, 645 enumeration areas (202 in urban areas and 443 in rural areas) were selected with probability proportion to size. The second stage involved selection of 28 households per cluster of an equal probability of being included in the systematic selection of the newly formed household list. The EDHS 2016 has three questionnaires: the household questionnaire, the woman’s questionnaire and the man’s questionnaire. All women of 15–49 years old, who were either a permanent inhabitant or visitors who lived at least one night in the household before the survey, were eligible for the interview. Data were gathered by conducting face-to-face interviews with women that met the eligibility criteria.
Data and study population
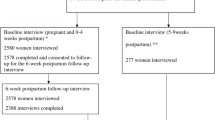
A total of 15,683 eligible women were interviewed in 2016 EDHS. About 5122 children with complete information on timing of breastfeeding initiation, and born 5 years preceding the survey were identified. In the case of more than one child per household, in this study we used data collected only from the last birth. The details of data extraction procedures are presented in Fig. 1.
Variables
This study has three dependent variables: early initiation of breastfeeding (binary outcome categorized as 1 if a mother initiated breastfeeding in the first hour after birth and 0 otherwise), exclusive breastfeeding (binary outcome categorized as 1 if a mother did not feed the baby anything else excepts of syrups and medicines apart from breast milk on the day before the interview during the first 6 months after birth and 0 otherwise), and the duration of breastfeeding the last child of the respondent (calculated as the number of months that the mother reports having breastfed her baby). The data on breastfeeding practices and associated factors were taken from the woman’s questionnaire.
The main independent variables were mother’s education, father’s education attainment, maternal age, wealth index of household, religion, place of residence, region of residence, professional antenatal and postnatal care, place of delivery, mode of delivery, type of birth, sex of child, size of child at birth, employment status of mother and parity was selected from the available similar studies on the subject [26,27,28,29,30,31,32,33,34]. The DHS use five wealth quintiles. Households are given scores based on the number and kinds of consumer goods they own, ranging from a television to a bicycle or car, in addition to housing characteristics such as source of drinking water, toilet facilities, and flooring materials. These scores are derived using principal component analysis. National wealth quintiles are compiled by assigning the household score to each usual (de jure) household member, ranking each person in the household population by her or his score, and then dividing the distribution into five equal categories, each comprising 20% of the population.
Data analysis
Descriptive characteristics of the subjects were presented as frequencies and percentages to summarize the distribution of selected background characteristics of mothers and children. To examine the socioeconomic and demographic factors associated with early initiation and exclusive breastfeeding (odds ratios with their 95% confidence intervals), logistic regression analysis was performed using Stata statistical package version 13 [35]. Further, a Cox’s Proportional Hazards model was employed to examine factors associated with time to cessation of breastfeeding. Multicollinearity between covariates was checked using the variance inflation factor (VIF) and the goodness of fit of the fitted models was checked using the likelihood ratio test (LRT).
Results
Descriptive statistics of breastfeeding practice by some characteristics
The median duration of breastfeeding was 22 ± 0.50 months (95% CI 21.01–22.99), while that of mean duration was 28.92 ± 0.32 months (95% CI 28.29–29.56). Table 1 shows that the percentage of early initiation of breastfeeding was lower in the Affar region (54.7%) followed by the Amhara (75.1%) and the Tigray regions (78.9%), respectively, while the highest percentage was observed in Dire Dawa (95.4%) and Harari (93.7%) regions.
The percentage of exclusive breastfeeding was low in the Somali region (27.7%) and the Affar region (30.5%). More than three-quarters (83.5%) of the mothers were from rural areas. About 80.6% of rural newborns initiate breastfeeding within 1 h of birth compared to 87.8% of urban newborns. The percentage exclusive breastfeeding was almost uniform in both rural and urban residents, 47.2 and 46.7%, respectively.
More than two-thirds (68.7%) of the mothers had no formal education at all. The percentage of early initiating of breastfeeding (80.3%) and exclusive breastfeeding (46.6%) was lowest among uneducated mothers. Similarly, more than half (52.2%) of fathers were illiterate. Nearly half (48.9%) of the children included were females. Male babies had a higher proportion of exclusive breastfeeding (47.5%) than that of females. Table 1 also shows that 65.3% of the mothers delivered outside of health facilities. Babies born outside of health facilities had a smaller percentage (79.4%) of early initiation of breastfeeding.
Only 8.5% of babies had a postnatal check-up. And 62.4% of mothers had attended antenatal care at least once. About 71.6% of mothers were unemployed. More than half (53.1%) were from a poor economic level. Moreover, children born from unemployed women and poor wealth indices had a lower percentage of early initiation of breastfeeding and exclusive breastfeeding practices 80.3 and 75.3%, respectively. Similarly, children with a small birthweight, cesarean birth, and being born of a large family (7 or higher), had a lower percentage of early initiation of breastfeeding, i.e. 79, 76.9 and 56.2%, respectively (Table 1).
Trends of breastfeeding practices are presented in Figs. 2 and 3. The percentage of early initiation of breastfeeding within increases from 51% in 2000 to 69% in 2005, then it fell to 52% after 5 years in 2011 and rose to 73% in 2016. Similarly, percentages of exclusive breastfeeding increase significantly from 38% in 2000 to 58% in 2016. Both initiations of breastfeeding and exclusive breastfeeding show a decreasing trend from 2005 to 2011. Overall, this shows that the percentages of both early initiations of breastfeeding and exclusive breastfeeding increased from 2000 to 2016. The median duration of breastfeeding in Ethiopia decreased from 25.20 months in 2000 to 23.90 months in 2016. See Fig. 2.
The two outstanding stages, three and 5 months in Fig. 3 indicate that the period when a child terminated exclusive breastfeeding.
The Kaplan-Meier survival functions presented in Figs. 4, 5, 6 and 7 indicate a consistently falling time to cessation of breastfeeding. The Kaplan-Meier survival function of rural women on Fig. 5 was above that of urban women, indicating that, on average, rural women breastfed for a longer time compared to urban women. Similarly, the survival function of females on Fig. 6 lies below that of male children. On the other hand, Fig. 7 shows mothers with secondary or higher education level have a longer time to cessation of breastfeeding, i.e., educated mothers breastfed for a longer time compared to that of illiterate mothers.
Factors associated with early initiation of breastfeeding
Multivariate logistic regression analysis to examine factors associated with early initiation of breastfeeding is presented in Table 2. The goodness of fit was also checked using the likelihood ratio tests (LRT). Consequently, the result of likelihood ratio test, provided 1521.32 (p - value < 0.0001), would imply good fit for the model. Thus, the null hypothesis, there is no difference between the model with no predictor variables and the model with explanatory variables was rejected. Accordingly, regions of residence, place of residence, religion of mother, sex of a child, place of delivery, mode of delivery, birthweight of a child, baby postnatal checkup and parity, were covariates significantly correlated with early initiation of breastfeeding.
The region of residence of mothers was associated with early initiation of breastfeeding. The odds of early initiation of breastfeeding was lower among women residing in all regions except Harari compared to that of Dire Dawa (p - value < 0.01). Urban residents were 29% more likely to initiate breastfeeding early than mothers in the rural areas (OR 0.71, 95% CI 0.51, 0.99). The odds of delayed initiation of breastfeeding among Coptic orthodox was 1.89 (OR 1.89, 95% CI 1.02, 3.50) times higher than traditional/others. The male newborn was 1.18 times more likely to initiate breastfeeding late than a female (OR 1.18, 95% CI 1.01, 1.37). Regarding the place of delivery, mothers who delivered outside the health facility had higher odds of not initiating breastfeeding within 1 h of birth (OR 1.55, 95% CI 1.25, 1.91). The odds of delaying initiation of breastfeeding was lower among normal deliveries compared to cesarean birth (OR 0.10, 95% CI 0.06, 0.15), as were average size at birth compared to small birthweight (OR 0.80, 95% CI 0.66, 0.96) and newborn from small family size compared to those of seven and higher family size (OR 0.69, 95% CI 0.49, 0.97).
Factors associated with exclusive breastfeeding
In multivariate logistic regression analysis, the independent variables region, mother’s age, father’s educational level, place of delivery, baby postnatal checkup, antenatal care during pregnancy, mode of delivery, and weight of the child at birth were significantly associated with exclusive breastfeeding. Mothers that lived in Affar (OR 0.17, 95% CI 0.10, 0.28), Somali (OR 0.16, 95% CI 0.09, 0.26), and Harari regions (OR 0.28, 95% CI 0.16, 0.49) were less likely to exclusively breastfeed compared to mothers living in the Dire Dawa region, whereas those from Tigray, Oromia, Benishangul-Gumuz regions and the Addis Ababa city had a higher odds of exclusive breastfeeding compared to Dire Dawa. A woman that had primary education was less likely to practice exclusive breastfeeding (OR 0.62, 95% CI 0.40, 0.96) compared to a secondary or higher education. Moreover, the odds of exclusive breastfeeding among babies born outside of health facilities, and mothers with no breastfeeding counseling during antenatal following up was lower (OR 1.56, 95% CI 1.22, 1.99) and (OR 1.50, 95% CI 1.15, 1.95), respectively, as compared to being born in health facilities and at least four antenatal follows up, respectively. Furthermore, a baby receiving a postnatal check (OR 0.53, 95% CI 0.39, 0.73) and children born of a medium sized at birth (OR 0.80, 95% CI 0.65, 0.99) were more likely to be exclusively breastfed (Table 2).
Factors associated with duration of breastfeeding
From the multivariate Cox’s proportional hazard model analysis presented in Table 3, region, mother’s age, religion, wealth index, place of delivery, professional antenatal care, type of birth, baby weight at birth, employment status of mothers and parity were significantly associated with the duration of breastfeeding. Mothers who were living in Amhara (HR 1.31, 95% CI 1.05, 1.64), Oromia (HR 1.27, 95% CI 1.04, 1.54), and Benishangul-Gumuz (HR 1.34, 95% CI 1.09, 1.65) had a longer duration of breastfeeding than those who were residing in Dire Dawa.
Younger age mothers had a shorter duration of breastfeeding compared those 40 years and older. The average duration of breastfeeding were short (HR 0.76, 95% CI 0.60, 0.96) for mothers who were Muslims compared to that of traditional/others. Mothers who gave birth outside of health facilities had a shorter duration of breastfeeding compared to their counterparts who delivered in the health center. Furthermore, mothers who were not working, with poor wealth index and a single child had a longer duration of breastfeeding. Moreover, babies with a larger or average birthweight had a shorter duration of breastfeeding. Being born in a small family size also had a significant risk of early termination of breastfeeding (p - values < 0.001) (Table 3).
Discussion
The present study set out to examine the factors associated with early initiation of breastfeeding, exclusive breastfeeding and duration of breastfeeding and trends in Ethiopia. The percentages of children who initiated breastfeeding in the first hour and exclusively breastfeed differs by region. Prior studies also reported only 42.20% babies born in Affar region were initiating breastfeeding within 1 h after birth [36] and only 50% of children in the Somali region was initiated breastfeeding early [37]. In contrast a cross-sectional study conducted in the Gozamin district [38] which reported 74.10% of the prevalence of the exclusive breastfeeding.
Initiating breastfeeding in the first hour was higher compared to a study conducted in Uganda [26], Tanzania [27] and Nigeria [28] which reported 56, 46.10, and 37%, respectively. The practice of exclusive breastfeeding was congruent with a similar previous study conducted in Uganda [26] which reported 46%, and in East Gojjam zone, Amhara regional state [29] reported 50.10%. In contrast, a study done in a Rajkot district of India 62% [30], Dilla Zuria District, Gedeo Zone 57.60% [31], Enderta woreda, of Tigray regional, state 70.20% [32], Ghana 64% [33], and Nigeria 56.60% [34] reported a higher proportion of exclusive breastfeeding. These differences might be the variation in health service utilization, culture, socioeconomic status of the study participants’, taboos about breastfeeding (colostrum) and methodological approaches used in the studies [39].
In the multivariate logistic regression analysis, it was found that mothers that lived in rural areas were less likely to initiate breastfeeding within 1 h of birth as compared to mothers that live in urban areas. This finding is consistent with previous studies conducted in Uganda [26], Nigeria [28], Tanzania [27, 40] and Ethiopia [41]. The possible explanation for this difference might be the higher percentage of rural women who delivered outside of health centers (i.e., home) without a health professional birth assistant. Additionally, home delivery and caesarean type birth were associated with delayed initiation of breastfeeding. The result is comparable with previous studies from Tanzania [27], Sri Lanka [42], Nigeria [28], India [43], Nepal [44], and a systematic review and meta-analysis of world literature [45]. This might be attributed to the fact that mothers who delivered into health centers could have a better chance of getting professional advice on feeding colostrum to her baby.
Mothers who had no education at all or only primary education were less likely to feed breast milk exclusively for the first 6 months. This finding is in agreement with previous studies reported in Ethiopia [46,47,48], Malaysia [49], and Nigeria [34, 50]. Maternal and child health care services such as postnatal and antenatal care, were risk factors of exclusive breastfeeding; i.e., mothers who received professional postnatal and antenatal care were more likely to exclusively breastfeed their infant. Several studies recognized that following health care services enable mothers to be aware of the benefits of exclusive breastfeeding to child and will get sufficient knowledge on nutrient content of breast milk enough for children during the first 6 months [51,52,53].
In this study, we observed that younger age mothers, Muslims, and employed women had terminated breastfeeding their baby at an earlier period. This finding is consistent with a study conducted in Kuwait [54] and Gondar town, Ethiopia [55]. The possible explanation of this might be that younger women are interested to have more children and employed mothers spend more of their time at the work place.
Children born of mothers that delivered at home and who are multiple births were more likely to terminate breastfeeding earlier [56]. Infants with an average or large birthweight were more likely to a short duration of breastfeeding.
Strength of the study
It uses a nationally representative survey data set, which enhance inferences for the entire country level.
Limitation of the study
This study is a retrospective report based on mother’s recall/perception of the events that took place for the past 5 years from the time of breastfeeding initiation to termination. The major limitations were it is subject to recall bias. The other weakness of the study was that some important possible factors that could affect the practice are missed due to incompleteness of information.
Conclusions
The study has examined the factors that are associated with early initiation of breastfeeding, exclusiveness, and the duration of breastfeeding in Ethiopia, based on Ethiopian DHS 2016 data.
Regional differences, place of residence, place of delivery, professional antenatal and postnatal care, education of mother, employment status of mothers, birth type, age of mother, wealth index, religion, mode of delivery, size of a baby at birth and parity were significant independent variables associated with breastfeeding practices in Ethiopia. Suboptimal breastfeeding patterns still exist in Ethiopia. Providing health education and counseling for mothers during and after pregnancy in the study setting are important to encourage mothers to deliver at health centers and get professional counseling on early initiation and exclusive breastfeeding.
Availability of data and materials
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- CSA:
-
Central Statistics Agency
- DHS:
-
Demographic and Health Survey
- EDHS:
-
Ethiopia Demographic and Health Survey
- HR:
-
Hazard Ratio
- LRT:
-
Likelihood Ratio Test
- MoH:
-
Ministry of Health
- NNP II:
-
National Nutrition Programme II
- OR:
-
Odds Ratio
- SDGs:
-
Sustainable Development Goals
- SSA:
-
Sub-Saharan Africa
- UNICEF:
-
United Nations Children’s Fund
- USAID:
-
United States Agency for International Development
- VIF:
-
Variance Inflation Factor
- WHO:
-
World Health Organization
References
WHO. 10 facts on breastfeeding. Geneva: World Health Organization; 2012. www.who.int/features/factfiles/breastfeeding/en/
Edmond KM, Kirkwood BR, Amenga-Etego S, Owusu-Agyei S, Hurt LS. Effect of early infant feeding practices on infection specific neonatal mortality: an investigation of the causal links with observational data from rural Ghana. Am J Clin Nutr. 2007;86(4):1126–31.
WHO/UNICEF: Global strategy on infant and young child feeding. 2002. www.who.int/nutrition/publications/infantfeeding/9241562218/en/index.htm
WHO/UNICEF: Global strategy for infant and young child feeding. 2003. http://www.breastfeedingcanada.ca/documents.
UN. Transforming our world: the 2030 agenda for sustainable development. New York: UN; 2015.
Central Statistics Agency (CSA) [Ethiopia] and ICF International. Ethiopia demographic and health survey 2016. Addis Ababa and Rockville: Central Statistical Agency (CSA) and ICF International; 2016.
Mullany LC, Katz J, Li YM, Khatry SK, LeClerq SC, Darmstadt GL, et al. Breast-feeding patterns, time to initiation, and mortality risk among newborns in southern Nepal. J Nutr. 2008;138(3):599–603.
UNICEF: A successful start in life: improving breastfeeding in West and Central Africa. 2010. https://www.unicef.org/infobycountry/files/wcaro_improving_breastfeeding_en.pdf
Notzon F. Trends in infant feeding in developing countries. Pediatrics. 1984;74(4):648–66.
WHO/UNICEF. Baby-friendly hospital initiative: revised, updated and expanded for integrated care. Geneva: Word Health Organization; 2009. https://www.who.int/nutrition/publications/infantfeeding/bfhi_trainingcourse/en/
WHO. Nutrition; promoting proper feeding for infants and young children. Geneva: Word Health Organization; 2017.
WHO. Guideline: protecting, promoting and supporting breastfeeding in facilities providing maternal and newborn services. Geneva: Word Health Organization; 2017.
WHO, UNICEF. Global strategy for infant and young child feeding. Geneva: Word Health Organization; 2003.
Edmond KM, Zandoh C, Quigley MA, Amenga-Etego S, Owusu-Agyei S, Kirkwood BR. Delayed breastfeeding initiation increases risk of neonatal mortality. Pediatrics. 2006;117(3):380–6.
Berkat S, Sutan R. The effect of early initiation of breastfeeding on neonatal mortality among low birth weight in Aceh Province, Indonesia: an unmatched case control study. Adv Epidemiol. 2014;2014(ID 358692):1–7.
UNICEF: Level & trends in child mortality, 2012.
Debes AK, Kohli A, Walker N, Edmond K, Mullany LC. Time to initiation of breastfeeding and neonatal mortality and morbidity: a systematic review. BMC Public Health. 2013;13(Suppl 3):S19.
Black RE, Allen LH, Bhutta ZA, Caulfield LE, de Onis M, Ezzati M, et al. Maternal and child undernutrition: global and regional exposures and health consequences. Lancet. 2008;371(9608):243–60.
Sefene A, Birihanu D, Awoke W, Taye T. Determinants of exclusive breastfeeding practice among mothers of children age less than 6 month in Bahir Dar city administration, Northwest Ethiopia; a community based cross-sectional survey. Sci J Clin Med. 2013;2(6):153–9.
Al-Jawaldeh A, Azza AF. Malnutrition, mortality and breastfeeding practices in the eastern Mediterranean region: a review of the current status. J Pediatr Care. 2018;4(1):2.
WHO: Infant and young child feeding, 2009,
UNICEF: Programming guide: infant and young child feeding, 2011.
WHO/UNICEF: Acceptable medical reasons for use of breastmilk substitutes, 2009
UNICEF. Progress for every child in the SDG era. New York; 2018. https://www.unicef.org/media/56516/file.
Measure DHS. The DHS program: demographic and health surveys. Rockville: ICF Macro. 2016.
Bbaale E. Determinants of early initiation, exclusiveness, and duration of breastfeeding in Uganda. J Health, Popul Nutr. 2014;32(2):249–60.
Victor R, Baines SK, Agho KE, Dibley MJ. Determinants of breastfeeding indicators among children less than 24 months of age in Tanzania: a secondary analysis of the 2010 Tanzania Demographic and Health Survey. BMJ Open. 2013;3:e001529.
Yahya WB, Adebayo SB. Modelling the trend and determinants of breastfeeding initiation in Nigeria. Child Dev Res. 2013;2013(ID 530396):1–9.
Tewabe T, Mandesh A, Gualu T, Alem G, Mekuria G, Zeleke H. Exclusive breastfeeding practice and associated factors among mothers in Motta town, East Gojjam zone, Amhara Regional State, Ethiopia, 2015: a cross-sectional study. Int Breastfeed J. 2017;12:12.
Chudasama RK, Amin CD, Parikh YN. Prevalence of exclusive breastfeeding and its determinants in first 6 months of life: a prospective study. Online J Health Allied Sci. 2009;8(1):1–7.
Reddy S, Abuka T. Determinants of exclusive breastfeeding practice among mothers of children under two years old in Dilla Zuria district, Gedeo Zone, Snnpr, Ethiopia, 2014. J Pregnancy Child Health. 2014;3:1.
Teka B, Assefa H, Haileslassie K. Prevalence and determinant factors of exclusive breastfeeding practices among mothers in Enderta woreda, Tigray, North Ethiopia: a cross-sectional study. Int Breastfeed J. 2015;10:2.
Tampah-Naah AM, Kumi-Kyereme A. Determinants of exclusive breastfeeding among mothers in Ghana: a cross-sectional study. Int Breastfeed J. 2013;8:13.
Chineke HN, Iwu AC, Diwe KC, Duru CB, Uwakwe KA, Emmanuel EE, Oluoha UR, Madubueze UC, Ndukwu EU, Ohale I. The practice of exclusive breast-feeding and its sociodemographic determinants amongst nursing mothers at a tertiary health care institution in South East, Nigeria. Open J Prev Med. 2017;7:63–73.
StataCorp. Stata statistical software: release 13. College Station: StataCorp LP; 2013.
Liben LM, Wuneh AG, Zepro NB, Mulugeta A. Factors associated with prelacteal feeding in Afar regional state, northeastern Ethiopia: a cross sectional study. Int J Res-Granthaalayah. 2017;5(7):116–27.
Guled RA, Nik Bin Mamat NM, Abu Bakar WAM, Assefa N, Belachew T. Knowledge, attitude and practice of mothers/caregivers on infant and young child feeding in Shabelle Zone, Somali Region, Eastern Ethiopia: a cross sectional study. Revelation Sci. 2016;6(2):42–54.
Hunegnaw MT, Gezie LD, Teferra AS. Exclusive breastfeeding and associated factors among mothers in Gozamin district, Northwest Ethiopia: a community based cross-sectional study. Int Breastfeed J. 2017;12:30.
Sellen DW. Infant and young child feeding practices among African pastoralist: the Datoga of Tanzania. J Biosoc Sci. 1998;30(4):481–99.
Shirima R, Greiner T, Kylberg E, Gebre-Medhin M. Exclusive breast-feeding is rarely practised in rural and urban Morogoro, Tanzania. Public Health Nutr. 2001;4(2):147–54.
Setegn T, Gerbaba M, Belachew T. Determinants of timely initiation of breastfeeding among mothers in Goba Woreda, South East Ethiopia: a cross-sectional study. BMC Public Health. 2011;11:217.
Senarath U, Dibley MJ, Godakandage SP, Jayawickrama H, Wickramasinghe A, Agho KE. Determinants of infant and young child feeding practices in Sri Lanka: second-ary data analysis of demographic and health survey 2000. Food Nutr Bull. 2010;31(2):352–65.
Patel A, Badhoniya N, Khadse S, Senarath U, Agho KE, Dibley MJ. Infant and young child feeding indicators and determinants of poor feeding practices in India: secondary data analysis of national family health survey 2005–06. Food Nutr Bull. 2010;31(2):314–33.
Pandey S, Tiwari K, Senarath U, Agho KE, Dibley MJ. Determinants of infant and young child feeding practices in Nepal: secondary data analysis of demographic and health survey 2006. Food Nutr Bull. 2010;31(2):334–51.
Prior E, Santhakumaran S, Gale C, Philipps LH, Modi N, Hyde MJ. Breastfeeding after caesarean delivery: a systematic review and meta-analysis of world literature. Am J Clin Nutr. 2012;95(5):1113–35.
Taddele M, Abebe L, Fentahun N. Exclusive breastfeeding and maternal employment in Ethiopia. A comparative cross-sectional study. Int J Nutr Food Sci. 2014;3(6):497–503.
Alemayehu T, Haidar J, Habte D. Determinants of exclusive breast feeding practice in Ethiopia. Ethiop J Health Dev. 2009;23(1):13–8.
Seid AM, Yesuf ME, Koye DN. Prevalence of exclusive breastfeeding practices and associated factors among mothers in Bahir Dar city, Northwest Ethiopia: a community based cross-sectional study. Int Breastfeed J. 2013;8:14.
Tan KL. Factors associated with exclusive breastfeeding among infants under six months of age in peninsular Malaysia. Int Breastfeed J. 2011;6:2.
Okafor IP, Olatona FA, Olufemi OA. Breastfeeding practices of mothers of young children in Lagos, Nigeria. Niger J Paediatr. 2014;41(1):43–7.
Mekuria G, Endris M. Exclusive breastfeeding and associated factors among mothers in Debre Markos, Northwest Ethiopia. Int Breastfeed J. 2015;10:1.
Torres A. Peer intervention strategies for breastfeeding promotion among low income Latinas in the US. a literature review. 2011. (Doctoral dissertation, California Polytechnic State University, San Luis Obispo). https://digitalcommons.calpoly.edu/fsnsp/6.
Abada TS, Trovato F, Lalu N. Determinants of breastfeeding in the Philippines: a survival analysis. Soc Sci Med. 2001;52(1):71–81.
Dashti M, Scott JA, Edwards CA, Al-sunghayer M. Determinants of the initiation and duration of breastfeeding among women in Kuwait. Int Breastfeed J. 2010;5:7.
Chekol DA, Biks GA, Gelaw YA, Melsew YA. Exclusive breastfeeding and mothers’ employment status in Gondar town, Northwest Ethiopia: a comparative cross-sectional study. Int Breastfeed J. 2017;12:27.
Hunegnaw MT, Gelaye KA, Ali BM. Factors associated with the time to cessation of breastfeeding among mothers who have index children aged two to three years in Debre Markos, Northwest Ethiopia: a retrospective follow up study. BMC Pediatr. 2018;18:77.
Acknowledgements
The authors are grateful to ICF macro (Calverton, USA) for providing the 2016 DHS data of Ethiopia.
Declaration
Author, declare that the research is our original work, and all sources of materials used have been duly acknowledged.
Funding
The author has no support or funding to report.
Author information
Authors and Affiliations
Contributions
BT involved from the inception to design, acquisition of data, analysis and interpretation and drafting the manuscript and edit the manuscript for the final submission. The author read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Competing interests
The author declares that he has no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated.
About this article
Cite this article
Woldeamanuel, B.T. Trends and factors associated to early initiation of breastfeeding, exclusive breastfeeding and duration of breastfeeding in Ethiopia: evidence from the Ethiopia Demographic and Health Survey 2016. Int Breastfeed J 15, 3 (2020). https://doi.org/10.1186/s13006-019-0248-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s13006-019-0248-3