Abstract
Frailty describes an age-associated state in individuals with an increased vulnerability and less resilience against adverse outcomes. To score frailty, studies have employed the questionnaires, such as the SF-36 and EQ-5D-3L, or the Frailty Index, a composite score based on deficit accumulation. Furthermore, ageing of the immune system is often accompanied by a state of low-grade inflammation (inflammageing). Here, we aimed to associate 29 circulating markers of inflammageing with frailty measures in a prospective cohort study to understand the mechanisms underlying ageing.
Frailty measures and inflammageing markers were assessed in 317 participants aged 25–90. We determined four different measures of frailty: the Frailty Index based on 31 deficits, the EQ-5D-3L and two physical domains of the SF-36. Serum/plasma levels of inflammageing markers and CMV/EBV seropositivity were measured using different techniques: Quanterix, Luminex or ELISA.
All four measures of frailty strongly correlated with age and BMI. Nineteen biomarkers correlated with age, some in a linear fashion (IL-6, YKL-40), some only in the oldest age brackets (CRP), and some increased at younger ages and then plateaued (CCL2, sIL-6R). After correcting for age, biomarkers, such as IL-6, CRP, IL-1RA, YKL-40 and elastase, were associated with frailty. When corrected for BMI, the number of associations reduced further.
In conclusion, inflammageing markers, particularly markers reflecting innate immune activation, are related to frailty. These findings indicate that health decline and the accumulation of deficits with age is accompanied with a low-grade inflammation which can be detected by specific inflammatory markers.
Similar content being viewed by others
Introduction
There are major differences in how individuals and their immune systems cope with ageing. Ageing of the immune system leads to a number of profound changes to the composition of leukocyte subsets and their functioning [1]. Older age has been associated with increased chronic inflammation, as evidenced by elevated C-reactive protein (CRP), TNF-α and IL-6 levels; a process also known as inflammageing [2,3,4]. Inflammageing is typically characterized by an enhanced innate immune response [5], manifested by increased circulation of proteins associated with macrophages (e.g. soluble CD163 (sCD163), YKL-40, sCD14) and neutrophils (e.g. elastase, PR3, IL-8). Adaptive cells are also vulnerable to the ageing process and a substantial age-associated decline in diversity has been reported [6]. Partly, this has been associated with increased exposure to chronic viral infections such as cytomegalovirus (CMV) and Epstein-Bar virus (EBV), resulting in the expansion of these antigen-specific memory cells, a process known as memory inflationn [6, 7].
Frailty is used to describe a declining health in older adults, resulting in an increased vulnerability to adverse outcomes, most notably: physical impairment, disease and mortality [8,9,10,11]. Frailty largely concerns the ability of an organism to cope with outside stressors, and is more prevalent in individuals with multiple comorbidities or in residents of long term care facilities [8,9,10,11]. It is a dynamic state which tends to increase with age, but can also fluctuate over time [12]. Moreover, an association between frailty and the body mass index (BMI) has been reported; higher frailty scores were found in the most extreme BMI values (both low and high) [13]. Understanding the mechanisms behind frailty is of high relevance since the population is aging worldwide.
There are a number of approaches to measure frailty. A frequently used method to determine an individual’s frailty, is the Frailty Index as described by Rockwood and Mitnitski, which is known to be a better predictor of hospitalization and mortality than age itself [12, 14]. The Frailty Index reflects the accumulation of an individual’s deficits ranging from impaired hearing to the presence of heart failure. Another important instrument to determine this syndrome, the Frailty Phenotype, has been developed by Fried et al., (2001) which measures frailty based on a number of physical assessments such as the grip strength and walking speed [11]. Other instruments capture frailty dimensions by questioning patients on their level of functioning and impairment in various domains (physical, emotional, social, mental), such as the EuroQol-5 Dimensions-3 Level (EQ-5D-3L) and Short-form (SF)-36 [15, 16]. These methods are often employed to assess patient-reported outcomes after interventions, for example during clinical trials, although aspects of these questionnaires are also used as measures of frailty [17].
Considering the accumulation of deficits in frail individuals, we hypothesize that inflammageing occurs more extensively in frail than non-frail individuals, and that specific biomarkers are able to reflect these differences. Therefore, in this study, we investigated the association between frailty scales and serum markers of inflammageing in participants of three different age groups (adults, middle-aged and older adults) of the VITAL study (Vaccines and Infectious disease in the Ageing Populations) [18, 19]. To this end, we selected a number of markers previously associated with frailty(e.g. IL-6, CRP, neopterin, iFABP2) and added additional markers previously linked to systemic inflammation and innate immunity [2,3,4, 20,21,22,23,24]. Four frailty scales were assessed: the Frailty Index, the EQ-5D-3L, and two domains of the SF-36.
Results
Frailty is strongly associated with age and BMI
We first assessed the associations of age, sex and BMI with the four frailty scales: Frailty Index, EQ-5D-3L, and the Physical Functioning and General Health domains of the SF-36 (PF.SF36, HG.SF36). Frailty scales were recorded in all participants divided over three age groups, with the oldest age group (≥ 65 years of age) containing the most participants (Table 1). Participants in the younger age group (25–49 years of age) were more often female than participants in the older groups. The median age of male participants was 7 years higher than that of female participants (p = 0.014; Fig. 1A). We therefore corrected for sex when assessing the effect of age on frailty scales.
Frailty scales are significantly associated with age. Graph A shows the age distribution of the total study population (n = 317) by sex. In B, shown are associations of participant age with the Frailty Index, the EQ-5D-3L (EuroQol-5 Dimensions-3 Level) questionnaire, the PF (physical functioning) and HG (general health) domains of the SF-36 (short-form-36). The significance of the sex-corrected Spearman correlation coefficient is indicated in each graph. The regression line is shown in black and the shaded region represents the confidence interval
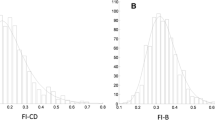
The four frailty scales correlated significantly with age, when corrected for sex (p < 0.0001; Fig. 1B). For the Frailty Index, we observed an accumulation of deficits with increasing age, with the natural logarithm of the slope of the mean at 0.029 (95% confidence interval: 0.022 – 0.036; R2 = 0.52, p < 0.001), which corresponds with previous reports that used this index [25, 26]. However, the highest Frailty Index score found within our study was 0.53, which is slightly lower than the defined submaximal limit of 0.67 [12, 14]. Frailty scales correlated with each other, with the strongest association between the Frailty Index and the number of prescription medications (Spearman’s R = 0.70, Supplementary Fig. S1A).
Frailty measures were also associated with BMI (Supplementary Fig. S1B). Participants with a higher BMI tended to be frailer than participants with a BMI lower than 25. In our study population, male participants had a significantly higher BMI than females (p = 0.006). However, BMI also correlated positively with age (p = 0.003, Z-statistic = 2.96) after controlling for sex.
Changes in concentration of serum inflammageing markers follow different trajectories with age
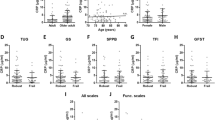
Out of 29 biomarkers measured, 19 of them were significantly associated with age, when corrected for sex (Table 2, Supplementary Fig. S2). The patterns of levels of inflammageing markers were however not uniform: four different trajectories could be identified (Fig. 2A). The levels of six biomarkers increased steadily from young to middle aged to older adults (trajectory a). In the second trajectory, we observed elevated levels of five markers (e.g. CCL2) in middle aged and older adults compared to younger adults, but no further increase in adults over 65 years (trajectory b). The third trajectory is characterized by elevated levels in the older adults only, which is observed for eight markers (e.g. PR3; trajectory c). The final category of ten serum markers was not associated with age (trajectory d).
Trajectories of serum markers of inflammageing in three age groups and their association with innate cells. In A, four different trajectories could be identified, based on statistical significance (Mann Whitney U) between the age groups. Shown are an example of each trajectory, indicating significant or non-significant differences between the groups, and the other markers that follow this pattern. In B, we show the correlations of circulating monocyte and neutrophil counts with the biomarkers. Shown are the Spearman R coefficients, with color coding according to the strength of the association. *: p < 0.05, ***: p < 0.001, ****: p < 0.0001, ns: not significant
As many of the biomarkers that we selected were associated with activation of cells of the innate immune system, we examined whether absolute counts of circulating monocytes or neutrophils correlated with the serum/plasma levels of the biomarkers (Fig. 2B). Interestingly, we show that a number of markers in trajectory a, c and d, but not in trajectory b, associate with monocyte and/or neutrophil counts. The strongest associations were seen for IL-1RA, whose levels correlated with monocyte counts (Spearman R = 0.30) and neutrophil counts (R = 0.47) [7, 27].
Associations of chronic CMV and EBV infections with frailty and inflammageing markers
As chronic infections with CMV and EBV have been associated with ageing of the immune system [7, 27], we investigated their association with the markers of inflammageing stratified by age and sex (Supplementary Fig. S3). Serum levels of the pro-angiogenic protein angiopoietin-2 showed a positive association with both CMV (p = 0.019, Z = 2.35) and EBV (p = 0.007, Z = 2.66) positivity, independent of age and sex. In addition, sCD163 levels were found to be higher in CMV-positive participants (p = 0.0005, Z = 3.49), and CCL-2 levels in EBV-positive participants (p = 0.016, Z = 2.39). For all other markers, no significant association was observed. A significantly higher Frailty Index score was found in participants that were seropositive for CMV (p = 0.048), but not EBV. Age only had a moderate effect on CMV and EBV status, particularly in participants aged over 50 years (Table 1).
Markers of inflammageing associate with frailty in older participants
To explore the interplay between inflammageing and frailty, we correlated the frailty measures in the VITAL cohort with the biomarker levels. First, we associated all biomarkers with the Frailty Index using a principle component analysis (PCA). Due to the strong association of age with the Frailty Index, we performed this analysis in the older participants (Fig. 3). We then colored the individuals based on their Frailty Index score, and show that individuals with increasingly higher scores tended to cluster farther away from individuals in the lowest Frailty Index bracket.
Principal component analysis (PCA) comparing the inflammageing markers in participants over 60 years of age between different classes of scores on the Frailty Index. The log-transformed markers were included in the PCA analysis. Participants (n = 187) were divided into different frailty classes; the red dots represent the participants with the lowest frailty scores and the blue and purple dots the participants with the highest frailty scores. The percentage of variance explained by the Principle Components (PC) 1 and 2 are mentioned on the axis. The eclipses cover 80% of the datapoints
We subsequently aimed to determine which biomarkers are the main drivers of the differential clustering. To this end, we first analysed which of the inflammageing markers associated with frailty as an absolute measure in all participants (Fig. 4A). Out of 29 markers, 21 showed an association with at least one frailty measure (the Frailty Index, EQ-5D-3L and SF-36 domains PF and HG). Even though this implies a relation between markers of inflammageing and frailty, we already showed that age has a strong association with levels of these markers.
Frailty scales are associated with levels of inflammageing markers. Here, we show the correlation of 29 markers with the outcomes of frailty in participants in the VITAL study (n = 317). In A we show that inflammageing markers were associated with frailty as an absolute measure, only corrected for sex. In B, we show the age and sex-corrected correlations of the markers with the outcomes of frailty. In C, we show age- and sex-corrected associations in 60 plus participants. The inflammageing markers are divided in groups A, B, C, and D based on their trajectory with age, see Fig. 2. Statistical significance of the Spearman’s correlation coefficient is indicated with *: p < 0.05, **: p < 0.01, ***: p < 0.001, ***: p < 0.0001. EQ-5D-3L: (EuroQol-5 Dimensions-3 Level), PF (physical functioning), HG (general health), SF-36 (short-form-36). The effect of age and sex was controlled in univariate correlation analyses using the blocked Spearman rank tests as implemented in the R package coin (v1.4.2) was used with the distribution parameter approximate (nresample = 100,000)
Therefore, we aimed to identify markers that associate with frailty in individuals of the same age. To this end, we analyzed the association of the different frailty measures with markers of inflammageing in all VITAL cohort participants correcting for age and sex as confounders (Fig. 4B). The Frailty Index was associated with four, EQ-5D-3L with six, PF.SF36 with five and HG.SF36 with four inflammageing markers. IL-6 and CRP were associated with all four frailty scales, and innate immune markers YKL-40 and IL-1RA associated with three out of the four frailty scales. The direction of these associations was the same for all markers: a positive correlation with the Frailty Index and a negative correlation with the scores on the EQ-5D-3L and SF-36 domains. The only exception was Elastase, which correlated positively with EQ-5D-3L scores. Additionally, we analysed the associations in the individuals over 60 years, as the frailty scales might perform more precise in the older population. We however showed that this analysis did not lead to substantially different outcomes (Fig. 4C).
We additionally confirmed the predictive value of the biomarkers and age on the Frailty Index using a regression analysis (Table 3). As expected, age was the strongest predictor of the Frailty Index. Additionally, CRP and IL-1RA were discovered as independent predictors of the Frailty Index. We next analyzed the associations separately for male and female participants. Besides age, IL-6 and IL-1RA levels independently predicted the Frailty Index in female participants. In male participants, YKL-40 and PR3 levels were found as independent predictors, with YKL-40 levels positively and PR3 levels negatively associated with the Frailty Index. Thus, this analysis confirms the predictive values of the inflammageing biomarkers (especially CRP, IL-6, IL-1RA and YKL-40) for frailty and reveals sex differences in this prediction.
BMI may partly influence the association between frailty and inflammageing markers
Both CRP and IL-6 have previously been associated with BMI and visceral adiposity [28,29,30], and in our cohort we observe significant associations of BMI with frailty scales. We investigated the associations of 29 markers with BMI in our cohort (Fig. 5A). We observed that seven inflammageing markers were associated with BMI, including IL-6 and CRP. Therefore, we tested associations of frailty scales with inflammageing markers by controlling for confounding effects of BMI, age and sex. These analyses showed reduced numbers of associations for all frailty measures except the Rockwood Frailty Index (Fig. 5B).
Body mass index (BMI) has an important impact on levels of inflammageing markers and plays a role as a confounder in the association between frailty and inflammageing markers. In A, we show the associations of 29 markers with BMI in the VITAL cohort. In B, we show associations of 29 markers with frailty measures corrected for BMI, age and sex. The inflammageing markers are divided in groups A, B, C, and D based on their trajectory with age, see Fig. 2. Statistical significance of the Spearman’s correlation coefficient is indicated with *: p < 0.05, **: p < 0.01, ***: p < 0.001, ***: p < 0.0001
Discussion
In this comprehensive study we aimed to study the association between ageing-associated biomarkers with frailty scales. We showed that frailty is closely related to both age and BMI, requiring us to correct for these factors to truly understand the associations between the biomarkers and frailty. We found several markers, including IL-6, CRP, YKL-40, IL-1RA, PR3 and elastase to be associated with frailty measures. Our findings indicate that frailty is related to dysfunctional immunological processes that arise with ageing, such as low-grade inflammation and neutrophil dysfunction.
Ageing of the immune system is accompanied by increased levels of a wide range of cytokines and other pro-inflammatory markers in the blood [2, 5]. In this study we showed a positive association of age with 19 biomarkers. The underlying mechanisms may vary. Inflammageing is likely caused by increased recognition of danger signals and a reduced barrier function of the mucosa in the gut [2, 3, 31]. Another cause of inflammageing is cellular senescence, which is a cellular fate caused by DNA damage resulting in cells that are prevented from proliferating, but characterized by a resistance to apoptosis and the production of a wide range of pro-inflammatory cytokines [32,33,34]. Finally, BMI tends also to increase with age, and particularly a high fat mass associates with low-grade inflammation [29, 30]. The interplay between these and additional factors leads to a pattern of increasing inflammatory biomarkers with increasing age. Interestingly we observed that the biomarkers’ increase with age follows different patterns: some markers tend to increase continuously, some may increase at middle age but then plateau, and some increase only in the oldest adults. Further studies may reveal whether the distinct underlying causes of inflammageing may explain these different patterns.
The choice of frailty measures is important in studies that investigate the link between frailty and immunological processes. The four main frailty measures in this study likely reflect partially different types of frailty. The Frailty Index [26], focusses on deficits, which typically develop with age, and indeed the Frailty Index strongly correlated with age. The advantage of the Frailty Index is that it is a more objective instrument to measure frailty, rather than the EQ-5D-3L and SF-36 which were solely based on questionnaires. The associations of the Frailty Index with the biomarkers are less impacted by BMI compared those of the EQ-5D-3L and SF-36 domains, as all four associations between the Frailty Index and the biomarkers remained after correcting for BMI. The number of prescribed medications used correlated strongly with the other frailty measures, suggesting its potential use as an easily obtained and objective measure of frailty. Due to the use of home visits, The Frailty phenotype, by Fried et al. (2001), was not used in our analyses since it would require more space to perform the physical tests than generally available in a house in the Netherlands and would be more suitable for a study center or hospital setting.
A number of markers that are typically associated with innate immunity activation were found to be associated with frailty measures. The pro-inflammatory cytokine IL-6 and the closely related acute-phase marker CRP were associated with frailty. IL-6 and CRP have often been proposed as potential markers of frailty [35,36,37,38]. Also TNF-α levels have been found to associate with frailty, however this was not the case for the Frailty Index in this study, nor in another recent study [20]. The association between IL-6/CRP levels and frailty may partly be explained by the close interplay with BMI. IL-6 and CRP levels have been associated with increased adiposity, and adipocytes are potent producers of IL-6, particularly during a state of chronic low-grade inflammation [28, 39]. In this study we show a strong relation between BMI and the frailty measures. When correcting for BMI, the association between IL-6 and three of the frailty measures remained.
We also included a number of markers that have less often been studied in the context of frailty. We found that YKL-40 levels associated with frailty measures, and even after correcting for age and BMI the association with the Frailty Index and EQ-5D-3L remained. YKL-40, (chitinase-3-like protein 1) is produced by certain types of neutrophils and macrophages and was previously found to play a role in orchestrating angiogenesis, tissue fibrosis, inflammation, oxidative tissue injury, and extracellular remodeling responses [40,41,42,43,44,45]. As a biomarker that likely reflects immune activation and potentially peripheral macrophage or even microglial activation, YKL-40 has been associated with neurodegenerative diseases, including a role as a prognostic marker [46, 47]. Elevated YKL-40 levels have been also reported to be associated with atherosclerosis and cerebrovascular disease [48, 49]. In a study with 80-year old participants, YKL-40 levels associated with all-cause mortality, which also implies a link with frailty [50]. Our results are in line with those previous observations.
The level of IL-1RA, an antagonist of pro-inflammatory IL-1 signaling, was also associated with age-corrected frailty, even though this relation was largely lost when we corrected for BMI. Indeed, IL-1RA levels have been associated with the risk for cardiovascular disease, which likely plays a prominent role in frailty [51]. IL-1RA release is stimulated by inflammatory mediators including IL-1β and IL-6, in which is thought of as a negative feedback mechanism [52]. Moreover, IL-1RA levels appeared to be closely associated with innate cells counts in the blood. Similarly, levels of neopterin, a marker of global immune activation described to increase with age, were associated with sex-corrected frailty, as previously described [23]. However, this association did not persist when we corrected for age and/or BMI.
We also showed that two neutrophil-associated markers, PR3 and Elastase, associated negatively with frailty, despite their positive association with age. Both PR3 and Elastase are important proteases that neutrophils use to induce their extravasation from the blood and migration within the tissue [53]. Elastase can be found in free form or bound to its inhibitor A1AT, but here only the free form of Elastase was associated with frailty. One study has investigated neutrophil dysfunction in the context of frailty [54]. Here they discovered that elastase activity, measured indirectly via AαVal360 levels, was reduced in frail older adults. Interestingly, elastase levels in this study and AαVal360 levels in the study by Wilson et al. do increase with age, but also associate negatively with frailty. Potentially, the dysfunctional neutrophils contribute to the delayed disposal of pathogens, resulting in lower thresholds for inflammatory responses.
An additional finding in this study was the observed association of serum angiopoietin-2 levels with both anti-CMV and EBV seropositivity. The association of angiopoietin-2 levels with chronic CMV and EBV infections has not been reported before, but increased angiopoietin-2 levels have been related to chronic hepatitis C infection [55]. Angiopoietin-2 is an inflammation-associated protein that promotes angiogenesis, the formation of new small blood vessels [56]. Angiogenesis is instigated by angiopoietin-2 by disrupting the homeostatic angiopoietin-1 – Tie2 signaling in the presence of vascular endothelial growth factor (VEGF). Potentially, the variety of liver manifestations that are associated with CMV and EBV infection explain the higher angiopoietin levels; a comparable mechanism was observed in patients with chronic hepatitis C [55, 57]. In addition to angiopoietin-2, we also found an association of macrophage activation marker sCD163 with anti-CMV seropositivity, confirming a prior report [58], and monocyte chemoattractant CCL2 with anti-EBV antibodies. We considered the CMV and EBV status of the participants due to the link with immune ageing [7, 27], however we found no additional overlap in markers associated with frailty and markers associated with CMV and EBV status.
Strengths of this study include the use of a broad prospective cohort with participants from a large age range (25–92 years old). Additionally, we used both objective and subjective determinants of frailty and focus on a comprehensive set of markers that were associated with mechanisms behind inflammageing. Frailty associations with inflammageing markers were performed with sophisticated analyses in which we corrected for the confounders age, sex and BMI. Weaknesses include the fact that male participants in this study were on average older than the female participants. This confounder, was however corrected for in most on the analyses. Also, the Fried Frailty Index was not used, due to logistical constraints. Finally, acknowledge a limitation in our statistical approach, as we did not perform p-value adjustments. Instead, we utilized a permutation test approach, which offers a robust method for assessing the statistical significance of Spearman's correlation between variables while also accounting for potential confounders. Our choice of biomarkers was guided by a priori hypotheses, and applying stringent p-value adjustments, like Bonferroni correction, might lead to a heightened risk of Type II errors and mask potentially meaningful biomarker patterns.
Conclusion
We here show that several inflammageing markers are independently associated with frailty, even when corrected for age, sex and BMI. These associations provide clues on reasons why ageing affects people differently with regards to their physical health and resilience against stressors. These biomarkers could potentially be employed in ageing studies to assess frailty instead or in addition to the Frailty Index or questionnaires, that are both time consuming and less consistent between different studies. The immunological mechanisms and cellular source of these frailty-associated biomarkers require further studies to validate the observed markers herein in a global inflammageing signature. Thus, it would be important to associate these biomarkers to extensive immunophenotyping of the same participants at the same visit. The main goal of the VITAL cohort concerns the investigation of the vaccine responses in the ageing population. Therefore, future studies will aim to associate both frailty measures and inflammageing markers with outcomes of vaccination.
Materials and methods
The VITAL cohort
The VITAL cohort consists of individuals aged 25–90. Younger (age 25–49) and middle-aged (age 50–64) participants were employees recruited from Health institutes at the Utrecht Science Park and Spaarne Hospital (Hoofddorp). The older participants (age ≥ 65) were recruited from a previous study on influenza in older adults [59, 60]. These cut-offs have often been used in the field of ageing and gerontology and follow the American Medical Associations’ age designations. We excluded individuals with previous adverse reactions to vaccination or for whom blood drawing may be harmful. We also excluded immunocompromised individuals due to disease, or immune-mediating medication, such as high-dose glucocorticoids or chemotherapy during the study or in the previous three years. Also, participants were excluded if they did not receive an influenza vaccination in the 2018–2019 season. Participants were recruited for the VITAL longitudinal intervention cohort which aims aim at getting a better insight of the influence of age and age-related changes on vaccine-induced immune responses, and at gaining knowledge on the trajectory of immune decline in older adults and middle-aged adults in comparison to adults [18, 19]. Here, we included clinical data, questionnaires and serum and plasma samples from 317 participants at the first study visit in 2019, which was prior to influenza vaccination. Blood was drawn from each participant; serum and EDTA-plasma were stored within 8 h at -80 °C until further use.
Assessment of frailty status in the VITAL cohort
As our main determinant for frailty, we designed a Frailty Index for the VITAL cohort, following the criteria that were described by Rockwood and Minitski [25]. The deficits that are included in the Frailty Index should meet defined criteria. These criteria state that: each deficit counts equally in the Frailty Index; the included deficits must cover a range of functions; deficits are associated with health; the prevalence of the deficit increases with age; the parameter (whether or not someone has the deficit) is measured in ≥ 95% of the study population; the deficit is present in ≥ 1% of the study population; and the deficit does not occur in > 80% of the study population < 80 years [12, 14, 25, 26, 61]. The Frailty Index in the VITAL cohort contains 31 deficits, which is within the recommended range of 30–40 deficits (see Supplementary Table S1 for the full list of deficits and scoring methods). Deficits included in the Frailty Index covered a range of systems, including cardiovascular, gastrointestinal, sensory, motor and neural systems. If participants were missing data for ≥ 20% of the deficits, the Frailty Index could not be determined. The Frailty Index results in a score ranging from 0 (least frail) to 1 (most frail), although scores above 0.67 have been reported to be too high to be compatible with life.
Two additional methods for defining frailty were based on self-reported questionnaires, comprising the EQ-5D-3L and the SF-36. The EQ-5D-3L is a questionnaire on five dimensions: mobility, self-care, usual activities, pain/discomfort and anxiety/depression [16]. For each dimension, the participants scored their health on three levels. Using the population norms of the Netherlands, a composite score ranging from -1 (most frail) to 1 (least frail) was set. The SF-36, a set of generic, coherent, and easily administered quality-of-life measures, comprises 36 multiple-choice questions [15]. The complete SF-36 questionnaire results in scores in eight domains, ranging from 0 (most frail) to 100 (least frail). In this study, we only used data from two domains, PF and HG, as they displayed the most variation in scores. Additionally, we compared the four measures of frailty with the Health Rating score and the number of prescription medications. The Health Rating score, ranging from 0 (most frail) to 10 (least frail) was a simple rating scored by the participant based on the question “I rate my health with a score of …”. The number of prescription medications included every type of medication that was prescribed by a physician, also including ointments, eye/ear drops and specific vitamins. Prescription medications that are not indicative of a frail state (contraception, malaria prophylaxis, and one-time sedation for medical procedures) were not included in the number of medications.
Laboratory measurements
Levels of biomarkers reflecting inflammageing were measured with different techniques in serum or plasma samples of the VITAL participants (Supplementary Table S2). Twenty biomarkers were measured at the University Medical Center Groningen (UMCG) in the Netherlands, using either Luminex multiplex assays or ELISA assays. An additional nine markers were assessed in Cimi-Paris (France), by ELISA or by the high-sensitivity Quanterix assays (Simoa or Corplex). For technical information, including dilutions and standard curve ranges, see Supplementary Table S2. Samples that were above or below the range of the standard curve were set at a fixed value, as indicated in Supplementary Table S2. Assays were performed in accordance with the manufacturer’s recommendations. The absolute number of monocytes and neutrophils was assessed by the DxH 500 Hematology Analyzer (Beckman Coulter).
Tests to determine CMV and EBV status at the first visit, based on immunoglobulin G antibodies against CMV and EBV, was performed by multiplex immunoassay (MIA), as described before [27, 62]. For CMV, a concentration of < 4 relative units (RU) ml − 1 was categorized as seronegative, ≥ 4 and < 7.5 RU ml − 1 as borderline, and ≥ 7.5 RU ml − 1 as seropositive. For EBV, a concentration of < 16 RU ml − 1 was categorized as seronegative, ≥ 16 AU ml − 1, and < 22 RU ml − 1 as borderline and ≥ 22 RU ml − 1 as seropositive.
Statistics
Statistical analysis and data visualization were done in R (v4.2.1) statistical programming language. Associations between two continuous variables (frailty vs age and frailty vs cytokine measurements) were tested with the permutational framework for Spearman correlation test test implemented in the coin (v1.4.2) R package. The analysis considered sex as a ‘block’ for stratification and the null distribution of the test statistic was approximated via Monte-Carlo resampling (nresample = 100,000). The associations of the different frailty measures with cytokines in older adults included two different approaches. First comparison tested associations without correcting for sex and age and second comparison included stratification combined for age and sex to avoid cofounding in this study. To stratify based on BMI, we categorized participants into lean (less than 25), overweight (between 25.0 and 30) and obese (above 30).
Additionally, multiple regression analyses were performed in IBM SPSS Statistics 28 with the Frailty Index scores as dependable outcome and age and the biomarkers as predictable variables. Due to the non-normal distribution of the data, the Frailty Index scores and biomarker levels were log transformed. Participants with missing data were also excluded from the analysis. This analysis was performed for all participants, and separately for female and male participants. Multicollinearity was checked with VIF statistics < 10 and thereafter the collinearity diagnostics.
The PCA was performed using log-transformed concentrations of CRP, sCD14, Calprotectin, IL-8, Elastase, PR3, Angiopoietin-2, C5a, CCL2, sCD25, sCD163, CXCL10, sGP130, sIL-6R, IL1RA, PTX-3, YKL-40, Neopterin, iFABP2, GM-CSF, TNFα, IL-6 and IL-10. Only participants above 60 years of age and with complete data on these markers were included. We used the cut-off of 60 years of age and older, rather than 65, to have sufficient power to cluster the participants based on biomarker levels. The PCA was performed using the prcomp function (factoextra package) and visualized with the ggplot2 package in RStudio 2022.07.2.. Individuals were grouped and colored based on the Frailty Index score. The eclipses cover 80% of the data point per frailty group. The amount of variance explained by Principle Components (PC) 1 and 2 are mentioned on the axis.
Availability of data and materials
The datasets analysed during the current study are available from the corresponding author on reasonable request.
References
Fali T, Vallet H, Sauce D. Impact of stress on aged immune system compartments: Overview from fundamental to clinical data. Exp Gerontol. 2018;105:19–26.
Franceschi C, Bonafè M, Valensin S, Olivieri F, De Luca M, Ottaviani E, et al. Inflamm-aging: an evolutionary perspective on immunosenescence. Ann N Y Acad Sci. 2000;908(1):244–54.
Franceschi C, Garagnani P, Parini P, Giuliani C, Santoro A. Inflammaging: a new immune–metabolic viewpoint for age-related diseases. Nat Rev Endocrinol. 2018;14(10):576.
Frasca D, Blomberg BB. Inflammaging decreases adaptive and innate immune responses in mice and humans. Biogerontology. 2016;17:7–19.
Pinti M, Appay V, Campisi J, Frasca D, Fülöp T, Sauce D, et al. Aging of the immune system: focus on inflammation and vaccination. Eur J Immunol. 2016;46(10):2286–301.
O’Hara GA, Welten SP, Klenerman P, Arens R. Memory T cell inflation: understanding cause and effect. Trends Immunol. 2012;33(2):84–90.
Pawelec G, Derhovanessian E. Role of CMV in immune senescence. Virus Res. 2011;157(2):175–9.
Cesari M, Calvani R, Marzetti E. Frailty in older persons. Clin Geriatr Med. 2017;33(3):293–303.
Donatelli NS, Somes J. What is Frailty? J Emerg Nurs. 2017;43(3):272–4.
Hoogendijk EO, Afilalo J, Ensrud KE, Kowal P, Onder G, Fried LP. Frailty: implications for clinical practice and public health. The Lancet. 2019;394(10206):1365–75.
Fried LP, Tangen CM, Walston J, Newman AB, Hirsch C, Gottdiener J, et al. Frailty in older adults: evidence for a phenotype. J Gerontol A Biol Sci Med Sci. 2001;56(3):M146–57.
Rockwood K, Song X, Mitnitski A. Changes in relative fitness and frailty across the adult lifespan: evidence from the Canadian National Population Health Survey. CMAJ. 2011;183(8):487.
Rietman ML, Van Der ADL, Van Oostrom SH, Picavet H, Dollé M, Van Steeg H, et al. The association between BMI and different frailty domains: a U-shaped curve? J Nutr Health Aging. 2018;22:8–15.
Searle SD, Mitnitski A, Gahbauer EA, Gill TM, Rockwood K. A standard procedure for creating a frailty index. BMC Geriatr. 2008;8(1):1–10.
Aaronson NK, Muller M, Cohen PD, Essink-Bot M, Fekkes M, Sanderman R, et al. Translation, validation, and norming of the Dutch language version of the SF-36 Health Survey in community and chronic disease populations. J Clin Epidemiol. 1998;51(11):1055–68.
Mangen MJ, Bolkenbaas M, Huijts SM, van Werkhoven CH, Bonten MJ, de Wit GA. Quality of life in community-dwelling Dutch elderly measured by EQ-5D-3L. Health Qual Life Outcomes. 2017;15(1):1–6.
Curran D, Kim JH, Matthews S, Dessart C, Levin MJ, Oostvogels L, et al. Recombinant Zoster Vaccine Is efficacious and safe in frail individuals. J Am Geriatr Soc. 2021;69(3):744–52.
Cevirgel A, Shetty SA, Vos M, Nanlohy NM, Beckers L, Bijvank E, et al. Identification of aging-associated immunotypes and immune stability as indicators of post-vaccination immune activation. Aging Cell. 2022;21(10):e13703.
Van Baarle D, Bollaerts K, Del Giudice G, Lockhart S, Luxemburger C, Postma MJ, et al. Preventing infectious diseases for healthy ageing: The VITAL public-private partnership project. Vaccine. 2020;38(37):5896–904.
Samson LD, Buisman A, Ferreira JA, Picavet HSJ, Verschuren WM, Boots AM, et al. Inflammatory marker trajectories associated with frailty and ageing in a 20-year longitudinal study. Clin Transl Immun. 2022;11(2):e1374.
Xu Y, Liu X, Liu X, Chen D, Wang M, Jiang X, et al. The roles of the gut microbiota and chronic low-grade inflammation in older adults with frailty. Front Cell Infect Microbiol. 2021;11: 675414.
Valdiglesias V, Marcos-Pérez D, Lorenzi M, Onder G, Gostner JM, Strasser B, et al. Immunological alterations in frail older adults: a cross sectional study. Exp Gerontol. 2018;112:119–26.
Teixeira-Gomes A, Laffon B, Valdiglesias V, Gostner JM, Felder T, Costa C, et al. Exploring early detection of frailty syndrome in older adults: evaluation of oxi-immune markers, clinical parameters and modifiable risk factors. Antioxidants. 2021;10(12):1975.
Justice JN, Ferrucci L, Newman AB, Aroda VR, Bahnson JL, Divers J, et al. A framework for selection of blood-based biomarkers for geroscience-guided clinical trials: report from the TAME Biomarkers Workgroup. Geroscience. 2018;40:419–36.
Mitnitski AB, Mogilner AJ, Rockwood K. Accumulation of deficits as a proxy measure of aging. Sci World J. 2001;1:323–36.
Rockwood K, Mitnitski A. Frailty in relation to the accumulation of deficits. J Gerontol A Biol Sci Med Sci. 2007;62(7):722–7.
Samson LD, van den Berg SP, Engelfriet P, Boots AM, Hendriks M, de Rond LG, et al. Limited effect of duration of CMV infection on adaptive immunity and frailty: insights from a 27-year-long longitudinal study. Clin Transl Immunol. 2020;9(10):e1193.
Fried SK, Bunkin DA, Greenberg AS. Omental and subcutaneous adipose tissues of obese subjects release interleukin-6: depot difference and regulation by glucocorticoid. J Clin Endocrinol Metab. 1998;83(3):847–50.
Maachi M, Pieroni L, Bruckert E, Jardel C, Fellahi S, Hainque B, et al. Systemic low-grade inflammation is related to both circulating and adipose tissue TNFα, leptin and IL-6 levels in obese women. Int J Obes. 2004;28(8):993–7.
Heilbronn LK, Campbell LV. Adipose tissue macrophages, low grade inflammation and insulin resistance in human obesity. Curr Pharm Des. 2008;14(12):1225–30.
Thevaranjan N, Puchta A, Schulz C, Naidoo A, Szamosi JC, Verschoor CP, et al. Age-associated microbial dysbiosis promotes intestinal permeability, systemic inflammation, and macrophage dysfunction. Cell Host Microbe. 2017;21(4):455-466 e4.
Hernandez-Segura A, Nehme J, Demaria M. Hallmarks of cellular senescence. Trends Cell Biol. 2018;28(6):436–53.
Cohn RL, Gasek NS, Kuchel GA, Xu M. The heterogeneity of cellular senescence: insights at the single-cell level. Trends Cell Biol 2022.
Ovadya Y, Krizhanovsky V. Senescent cells: SASPected drivers of age-related pathologies. Biogerontology. 2014;15(6):627–42.
Samson LD, Boots AMH, Verschuren WM, Picavet HSJ, Engelfriet P, Buisman A. Frailty is associated with elevated CRP trajectories and higher numbers of neutrophils and monocytes. Exp Gerontol. 2019;125: 110674.
Xu Y, Wang M, Chen D, Jiang X, Xiong Z. Inflammatory biomarkers in older adults with frailty: a systematic review and meta-analysis of cross-sectional studies. Aging Clin Exp Res. 2022:1–17.
Gale CR, Baylis D, Cooper C, Sayer AA. Inflammatory markers and incident frailty in men and women: the English Longitudinal Study of Ageing. Age. 2013;35(6):2493–501.
Puzianowska-Kuźnicka M, Owczarz M, Wieczorowska-Tobis K, Nadrowski P, Chudek J, Slusarczyk P, et al. Interleukin-6 and C-reactive protein, successful aging, and mortality: the PolSenior study. Immunity Ageing. 2016;13(1):1–12.
Khanna D, Khanna S, Khanna P, Kahar P, Patel BM. Obesity: A chronic low-grade inflammation and its markers. Cureus. 2022;14(2):e22711.
Van Sleen Y, Jiemy WF, Pringle S, Van der Geest KS, Abdulahad WH, Sandovici M, et al. A distinct macrophage subset mediating tissue destruction and neovascularization in giant cell arteritis: implication of the YKL-40/Interleukin-13 receptor α2 Axis. Arthritis Rheumatol. 2021;73(12):2327–37.
Johnson SC, Suárez-Calvet M, Suridjan I, Minguillón C, Gispert JD, Jonaitis E, et al. Identifying clinically useful biomarkers in neurodegenerative disease through a collaborative approach: the NeuroToolKit. Alzheimer’s Res Therapy. 2023;15(1):25.
Brosseron F, Maass A, Kleineidam L, Ravichandran KA, Kolbe C, Wolfsgruber S, et al. Serum IL-6, sAXL, and YKL-40 as systemic correlates of reduced brain structure and function in Alzheimer’s disease: results from the DELCODE study. Alzheimer’s Res Therapy. 2023;15(1):13.
Li Y, Chen Z, Wang Q, Lv X, Cheng Z, Wu Y, et al. Identification of hub proteins in cerebrospinal fluid as potential biomarkers of Alzheimer’s disease by integrated bioinformatics. J Neurol. 2023;270(3):1487–500.
Yeo IJ, Lee C, Han S, Yun J, Hong JT. Roles of chitinase 3-like 1 in the development of cancer, neurodegenerative diseases, and inflammatory diseases. Pharmacol Ther. 2019;203:107394.
Zhao T, Su Z, Li Y, Zhang X, You Q. Chitinase-3 like-protein-1 function and its role in diseases. Signal Transduct Target Ther. 2020;5(1):201.
Baldacci F, Lista S, Cavedo E, Bonuccelli U, Hampel H. Diagnostic function of the neuroinflammatory biomarker YKL-40 in Alzheimer’s disease and other neurodegenerative diseases. Expert Rev Proteomics. 2017;14(4):285–99.
Baldacci F, Lista S, Palermo G, Giorgi FS, Vergallo A, Hampel H. The neuroinflammatory biomarker YKL-40 for neurodegenerative diseases: advances in development. Expert Rev Proteomics. 2019;16(7):593–600.
Wang Y, Li B, Jiang Y, Zhang R, Meng X, Zhao X, et al. YKL-40 is associated with ultrasound-determined carotid atherosclerotic plaque instability. Front Neurol. 2021;12:622869.
Park HY, Jun C, Jeon S, Choi S, Kim H, Choi D, et al. Serum YKL-40 levels correlate with infarct volume, stroke severity, and functional outcome in acute ischemic stroke patients. PLoS ONE. 2012;7(12):e51722.
Johansen JS, Pedersen AN, Schroll M, Jørgensen T, Pedersen BK, Bruunsgaard H. High serum YKL-40 level in a cohort of octogenarians is associated with increased risk of all-cause mortality. Clin Exp Immunol. 2008;151(2):260–6.
Herder C, De Las Heras Gala T, Carstensen-Kirberg M, Huth C, Zierer A, Wahl S, et al. Circulating levels of interleukin 1-receptor antagonist and risk of cardiovascular disease: meta-analysis of six population-based cohorts. Arterioscler Thromb Vasc Biol. 2017;37(6):1222–7.
Perrier S, Darakhshan F, Hajduch E. IL-1 receptor antagonist in metabolic diseases: Dr Jekyll or Mr Hyde? FEBS Lett. 2006;580(27):6289–94.
Sun Z, Yang P. Role of imbalance between neutrophil elastase and α1-antitrypsin in cancer development and progression. Lancet Oncol. 2004;5(3):182–90.
Wilson D, Drew W, Jasper A, Crisford H, Nightingale P, Newby P, et al. Frailty is associated with neutrophil dysfunction which is correctable with phosphoinositol-3-kinase inhibitors. J Gerontol: Series A. 2020;75(12):2320–5.
Salcedo X, Medina J, Sanz-Cameno P, García-Buey L, Martín-Vilchez S, Borque MJ, et al. The potential of angiogenesis soluble markers in chronic hepatitis C. Hepatology. 2005;42(3):696–701.
Milam KE, Parikh SM. The angiopoietin-Tie2 signaling axis in the vascular leakage of systemic inflammation. Tissue Barriers. 2015;3(1–2): e957508.
Bunchorntavakul C, Reddy KR. Epstein-Barr Virus and Cytomegalovirus Infections of the Liver. Gastroenterol Clin North Am. 2020;49(2):331–46.
Vita S, Lichtner M, Marchetti G, Mascia C, Merlini E, Cicconi P, et al. Brief report: soluble CD163 in CMV-infected and CMV-uninfected subjects on virologically suppressive antiretroviral therapy in the ICONA cohort. J Acquir Immune Defic Syndr. 2017;74(3):347–52.
Van Beek J, Veenhoven RH, Bruin JP, Van Boxtel RA, De Lange MM, Meijer A, et al. Influenza-like illness incidence is not reduced by influenza vaccination in a cohort of older adults, despite effectively reducing laboratory-confirmed influenza virus infections. J Infect Dis. 2017;216(4):415–24.
Kaaijk P, Swaans N, Nicolaie AM, Bruin JP, van Boxtel RA, de Lange MM, et al. Contribution of influenza viruses, other respiratory viruses and viral co-infections to influenza-like illness in older adults. Viruses. 2022;14(4):797.
Rockwood K, Blodgett JM, Theou O, Sun MH, Feridooni HA, Mitnitski A, et al. A frailty index based on deficit accumulation quantifies mortality risk in humans and in mice. Sci Rep. 2017;7(1):1–10.
Tcherniaeva I, den Hartog G, Berbers G, van der Klis F. The development of a bead-based multiplex immunoassay for the detection of IgG antibodies to CMV and EBV. J Immunol Methods. 2018;462:1–8.
Acknowledgements
The VITAL project has received funding from the Innovative Medicines Initiative 2 Joint Undertaking (JU) under grant agreement No. 806776 and the Dutch Ministry of Health, Welfare and Sport. The JU receives support from the European Union's Horizon 2020
research and innovation programme. The authors thank Wivine Burny, Carole Desion, Roberto Zoffoli and Daniel Laroque, partners in the VITAL consortium, for their feedback on this study. We also thank the volunteers for participating in this study.
Funding
This research has been performed in the context of the VITAL consortium. The VITAL project has received funding from the Innovative Medicines Initiative 2 Joint Undertaking (JU) under grant agreement No. 806776 and the Dutch Ministry of Health, Welfare and Sport. The JU receives support from the European Union's Horizon 2020 research and innovation programme and EFPIA-members.
Author information
Authors and Affiliations
Contributions
JvB, AMB and DvB conceptualized the clinical study. YvS, MCAV, NGM collected the data. YvS, SAS and MvdH performed the statistical analysis. DvB and DS supervised the study. YVS wrote the original draft. SAS, MvdH, AMB, JvB, DvB, EJMT and DS were involved in writing, review and editing. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Approval from the institutional review board for this study was obtained from the Medical Research Ethics Committee Utrecht (EudraCT Number: 2019–000836–24) and all participants signed for informed consent. All procedures were in accordance with the declaration of Helsinki.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Additional file 1:
Supplementary Table S1. Full list of the deficits and their scoring as included in the frailty index developed in this study. Supplementary table S2. technical information on each assay used to obtain biomarker concentrations. Supplementary Figure S1. correlations of frailty measures with each other and BMI. In A, Spearman correlation coefficients and cell colors are shown indicating the strength and direction of the associations. **: p<0.01. In B, correlations of each frailty measure with BMI are shown. Strength and significance of the sex-corrected Spearman correlation coefficient is indicated in each graph.Supplementary Figure S2. Associations of all 29 biomarkers with age. Shown are individual values and moving medians (IQR) for each biomarker. Biomarkers marked with a * showed a significant association with age (p<0.05). Supplementary Figure S3. associations of inflammageing markers with CMV and EBV status. Shown are sex-corrected associations of the biomarkers with CMV- and EBV-status. Angiopoietin-2 levels were significantly higher in participants that were seropositive for CMV- and EBV antibodies compared to participants that were seronegative. A similar association of sCD163 levels was found with CMV status, and CCL2 levels with EBV status. Statistical testing was done with the Wilcoxon signed rank test, ‘+’ indicates statistical significance (p<0.05). CMV: cytomegalovirus, EBV: Epstein-Barr virus.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
van Sleen, Y., Shetty, S.A., van der Heiden, M. et al. Frailty is related to serum inflammageing markers: results from the VITAL study. Immun Ageing 20, 68 (2023). https://doi.org/10.1186/s12979-023-00391-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12979-023-00391-3