Abstract
Background
First-phase ejection fraction (EF1; the ejection fraction measured during active systole up to the time of maximal aortic flow) measured by transthoracic echocardiography (TTE) is a powerful predictor of outcomes in patients with aortic stenosis. We aimed to assess whether cardiovascular magnetic resonance (CMR) might provide more precise measurements of EF1 than TTE and to examine the correlation of CMR EF1 with measures of fibrosis.
Methods
In 141 patients with at least mild aortic stenosis, we measured CMR EF1 from a short-axis 3D stack and compared its variability with TTE EF1, and its associations with myocardial fibrosis and clinical outcome (aortic valve replacement (AVR) or death).
Results
Intra- and inter-observer variation of CMR EF1 (standard deviations of differences within and between observers of 2.3% and 2.5% units respectively) was approximately 50% that of TTE EF1. CMR EF1 was strongly predictive of AVR or death. On multivariable Cox proportional hazards analysis, the hazard ratio for CMR EF1 was 0.93 (95% confidence interval 0.89–0.97, p = 0.001) per % change in EF1 and, apart from aortic valve gradient, CMR EF1 was the only imaging or biochemical measure independently predictive of outcome. Indexed extracellular volume was associated with AVR or death, but not after adjusting for EF1.
Conclusions
EF1 is a simple robust marker of early left ventricular impairment that can be precisely measured by CMR and predicts outcome in aortic stenosis. Its measurement by CMR is more reproducible than that by TTE and may facilitate left ventricular structure–function analysis.
Similar content being viewed by others
Background
In conditions where there is impairment of myocardial contractile function early in systole, a length-dependent activation of the myocyte may preserve ejection fraction (EF) at the expense of slower but sustained contraction. This may explain why traditional measures of “systolic function” such as EF and newer measures such as global longitudinal strain (GLS) that measure total contraction over systole may be insensitive in detecting early systolic dysfunction. We have previously demonstrated that first-phase ejection fraction (EF1) as measured by transthoracic echocardiography (TTE), the EF measured up to the time of maximal aortic flow velocity on continuous wave Doppler which corresponds to active systole, is a more sensitive measure than EF or GLS in detecting early systolic dysfunction. EF1 as measured by TTE is of prognostic value in patients with aortic stenosis (AS) [1, 2], the most common form of primary heart valve disease [3]. Although TTE is the most commonly used diagnostic tool for evaluation of LV function in patients with AS, cardiovascular magnetic resonance (CMR) imaging is the gold standard imaging modality for assessing the myocardium, in particular for the quantification of left ventricular (LV) volumes and function, and tissue characterization [4, 5]. Furthermore, the use of CMR facilitates a greater degree of functional-structural correlation, potentially providing insight into mechanisms impairing early systolic function. The objective of the present study was to assess whether CMR might provide more precise measurements of EF1 than TTE and to examine the correlation of CMR EF1 with myocardial fibrosis, afterload and clinical outcomes.
Methods
Patient population
This was a retrospective analysis of an observational cohort of patients with at least mild AS (peak aortic velocity ≥ 2 m/s) who were prospectively recruited from the Edinburgh Heart Centre between March 2012 and August 2014 [6]. We recently reported clinical and prognostic associations of TTE EF1 in this cohort [2]. Exclusion criteria were other valvular heart disease (greater than mild severity), comorbidities with limited life expectancy, contraindications to gadolinium, and acquired or inherited non-ischaemic cardiomyopathies as assessed by history or CMR. Patients underwent clinical evaluation, venous blood sampling for plasma concentrations of high-sensitivity cardiac troponin I (hs-cTnI, ARCHITECT STAT assay, Abbott Laboratories, Abbott Park, Illinois, USA) and brain natriuretic peptide (BNP, Triage assay, Biosite Inc., San Diego, California, USA), electrocardiography, TTE and CMR. Referral for aortic valve intervention was undertaken by the treating cardiologist in accordance with routine practice and contemporary guidelines [2]. The study was approved by the regional ethics committee (10/S1102/24) and conducted in accordance with the Declaration of Helsinki. Written informed consent was obtained from all subjects. The primary outcome was a combination of aortic valve replacement (AVR) and death (identified through medical records and the General Register of Scotland).
Cardiovascular magnetic resonance and EF1
Detailed CMR protocols in this cohort have been described [6]. All baseline scans were performed on a 3 T CMR scanner (MAGNETOM Verio, Siemens Healthineers, Erlangen, Germany). Late-gadolinium enhancement (LGE) imaging was performed 15 min after intravenous administration of 0.1 mmol/kg gadobutrol and independently assessed by two investigators (CC and MD). T1 mapping was performed using the modified Look-Locker inversion recovery sequence [2]. Native T1, extracellular volume fraction (ECV%) and indexed extracellular volume (iECV = ECV% x LV diastolic myocardial volume indexed to body surface area) were measured [2, 6, 7]. Both ECV% and iECV included non-infarct and excluded infarct LGE [2]. GLS was measured using cvi42 (Circle Cardiovascular Imaging, Calgary, Alberta, Canada). A fully automated strain analysis was carried out with two-dimensional GLS as the primary assessment.
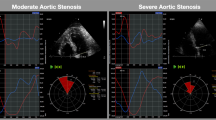
CMR EF1 was retrospectively analysed by one observer (HG) blinded to patient characteristics and outcomes using cvi42. Time to peak aortic valve flow was derived from the phase contrast aortic valve flow-time curve (Fig. 1). LV volumes were measured using short-axis 3D stack following the recommendations of the Society for Cardiovascular Magnetic Resonance [8].
Representative cardiovascular magnetic resonance (CMR) images and measures of aortic valve flow and left ventricular (LV) volume from a patient in the series. Left ventricular volume was measured from CMR short-axis stack 3D, aortic valve flow was measured from phase contrast flow images and time to peak aortic valve flow was derived from the aortic valve flow-time curve. First-phase ejection fraction (EF1) was then calculated using equation: EF1 = (EDV-V1)/EDV%, where EDV is end-diastolic volume and V1 is volume at time of peak aortic valve flow
CMR EF1 was then calculated using the following equation [1]:
where EDV is end-diastolic volume and V1 is LV volume at the time of peak aortic flow (Fig. 1). V1 was measured from the frame closest to peak aortic velocity estimated from the number of frames per unit time multiplied by the time to peak aortic velocity. We also examined a similar metric to EF1 that can be derived entirely from the integral of aortic flow over time: aortic flow-derived volume up to the time of peak flow (SV1) expressed as a ratio of aortic flow-derived volume over systole (SV). In the absence of mitral regurgitation SV1/SV is theoretically equal to EF1/EF and avoids the limitation of phase contrast and cine imaging not being measured concurrently.
Intra- and inter-observer variability in measurements of CMR EF1 was assessed in 40 randomly selected subjects by two observers by Bland–Altman analysis calculating the SD of the difference between readings and coefficient of variation defined as the SD expressed as a percentage of the mean measurement.
Transthoracic echocardiography and EF1
TTE was performed in all patients according to American Society of Echocardiography guidelines [9]. The detailed protocol and measurement of EF1 by TTE have been previously described [2]. AS severity was defined by aortic valve area (AVA) and mean pressure gradient (MPG) according to current guidelines [10, 11]. Valvuloarterial impedance (Zva = [systolic blood pressure + mean aortic valve gradient]/stroke volume), a validated prognostic measure of global LV afterload in AS, was also calculated and indexed to body surface area [12].
Statistical analysis
Continuous variables were tested for normality with the Shapiro–Wilk test and are presented as median [interquartile range (IQR)] or mean ± standard deviation (SD). Non-normally distributed continuous variables were log2-transformed for regression models. CMR GLS was log2-transformed after addition of a constant (greatest GLS + 1). The Pearson correlation coefficient and Bland–Altman analysis were used for comparing CMR and TTE EF1. Intra- and inter-observer variability for CMR EF1 and TTE EF1 was assessed by the standard deviations of differences and by Bland–Altman plots.
CMR EF1 was dichotomized using a previously defined cut-off value derived from our previous work using TTE, adjusted for the mean difference between values of CMR and TTE EF1. Univariable and multivariable linear regression modelling was performed to identify the associations between CMR EF1 and relevant clinical and CMR variables including age (per decade), male sex, Zva, infarct LGE, iECV, hs-cTnI and brain natriuretic peptide (BNP). These models were constructed with haemodynamic and CMR parameters followed by the addition of biochemistry and clinical parameters. Infarct LGE and iECV are conceptually distinct assessments and as such were chosen over other fibrosis measures. Cumulative event rates were examined using Kaplan–Meier curves for the combined primary outcomes of AVR or all-cause mortality. Assumptions for proportionality were checked and the time-dependent association between CMR EF1 and the primary outcome assessed using Cox proportional hazard models, with the covariables of age (per decade), male sex, New York Heart Association (NYHA) dyspnoea class, MPG, EF1, infarct LGE and iECV. Two-sided p-values < 0.05 were considered statistically significant. Analysis was performed using R version 3.5.0 (R Foundation for Statistical Computing, Vienna, Austria).
Results
Patient characteristics and major events
Of the 166 patients in the original cohort, 25 were excluded due to suboptimal CMR images (Fig. 2). Thus, 141 patients, including 28 with mild, 41 with moderate, and 72 with severe AS were included in the final analysis. Twenty-five patients classified as severe AS due to an aortic valve area < 1 cm2 had a mean gradient < 40 mmHg. Ninety-four patients experienced an event with a median time to event of 13.3 (IQR: 2.0 to 36.1) months, including 78 who had AVR and 16 who died without AVR. Patients with reduced (≤ 20%) CMR EF1 (n = 74) were of similar age but had worse NYHA class, more severe AS than those with preserved CMR EF1 (> 20%) (Table 1). There was no difference in EF or GLS between those with reduced or preserved CMR EF1 (Table 1).
Comparison of CMR EF1 and TTE EF1
Of the 141 patients in whom EF1 was measured by CMR, 126 had measurements of EF1 by both CMR and TTE with a median of 4 (IQR: 5) days between CMR and TTE. There was no significant difference in heart rate (65 ± 13 vs 64 ± 11 bpm, p = 0.286) on the CMR and TTE visit days. CMR EF1 correlated with TTE EF1 (r = 0.51, p < 0.001) but there was a small but significant systematic bias with mean ± SD difference between CMR EF1 and TTE EF1 of -5.0 ± 7.8% (Fig. 3a, b). Intra-and inter-observer variation for CMR EF1 was 2.3% and 2.5% units respectively for the SD of the difference between intra- and inter-observer readings giving coefficients of variation of 12.4% and 13.8% respectively (Fig. 3c, d). For TTE EF1, intra- and inter-observer variation was greater with SDs of 4.3% and 4.6% (each p < 0.01 compared to values by CMR) and coefficients of variation of 16.8% and 17.7% for intra- and inter-observer readings respectively (Fig. 3e, f). There was a relatively poor correlation between SV1/SV and CMR EF1/EF (R = 0.23, p = 0.006) and between SV1/SV and TTE EF1/EF (R = 0.17, p = 0.046).
CMR EF1 and other clinical characteristics
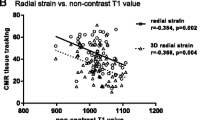
CMR EF1 fell progressively with increasing severity of AS: mild 24.7 ± 4.5%, moderate 21.9 ± 7.3% and severe 14.5 ± 6.1% AS. On univariate linear regression, CMR EF1 correlated with mean gradient and Zva (Table 2). None of the measures of fibrosis were correlated with CMR EF1 and stepwise multivariate linear regression models using the pre-specified covariables (Table 3) demonstrated Zva (p < 0.05) to be independently associated with CMR EF1.
Prediction of events by CMR EF1
ROC curve analyses (Fig. 4) demonstrated that mean aortic valve gradient had the largest area under the curve (AUC, 0.88). CMR EF1 (0.73) was a better discriminator of the primary outcome than other functional parameters, including CMR GLS (0.69) and CMR EF (0.55). A threshold for CMR EF1 of 20% (defined by our previously obtained threshold of 25% by TTE, adjusted for the 5% mean difference between CMR EF1 and TTE EF1) yielded a sensitivity of 74% and a specificity of 66%. Kaplan–Meier analysis (Fig. 5) showed that the probability of event-free survival was lower in those patients with a low CMR EF1 (Fig. 5, log-rank p < 0.001). On univariate and multivariable Cox regression analysis, CMR EF1 was a strong predictor of the primary outcome (Table 4). The adjusted hazard ratio for CMR EF1 was 0.93 (95% confidence intervals 0.89–0.97, p = 0.001) per % change in EF1. When the analysis was restricted to patients with severe AS, the hazard ratio for CMR EF1 was similar (0.90, 95% confidence intervals 0.86–0.94, p < 0.001) to that in the whole cohort. Patients with a low SV1/SV (defined as < = 34%, on ROC analysis) had a lower rate of event-free survival compared to those with a high SV1/SV (log-rank p = 0.04). There was no significant difference in the prediction of outcome by CMR and TTE EF1. iECV was associated with outcome on univariate analysis but not after adjusting for CMR EF1 (Table 4) [13].
Discussion
To our knowledge, this is the first study to derive CMR EF1. Previous studies have demonstrated TTE EF1 to be a strong predictor of major cardiac events in AS patients[1, 2]. Consistent with our previously published TTE data in this cohort, we found that CMR EF1 fell with increasing AS severity, had similar associations with assessments of LV afterload, myocardial fibrosis and outcomes, but had less variability than TTE EF1. CMR EF1 was lower (mean difference: -5.0 ± 7.8%) than by TTE. There was modest correlation between CMR EF1 and TTE EF1 (r = 0.51, p < 0.001). However, CMR EF1 and TTE EF1 were obtained on different occasions and therefore could have been influenced by both physiological variation and variation inherent in the measurement technique. With regard to the latter, CMR is regarded as the gold-standard for volumetric measurements but has limited temporal resolution, whereas TTE has greater temporal resolution but suffers from sub-optimal endocardial definition. Our data demonstrated that, compared to TTE, CMR is associated with an approximate halving of the variability of EF1 measurement suggesting that precision in volumetric assessments had a greater influence than that of temporal resolution. This suggests that CMR is the preferred modality for the measurement of EF1. However, it is likely that technological improvements to both modalities will improve EF1 precision. In particular, for CMR, higher temporal resolution achieved through a greater number of phases per cardiac cycle or through more sophisticated post-processing to define the time of peak aortic flow is likely to improve precision further. It is possible that other measures of early systolic function might perform as well or better than EF1. However, in the present study SV1/SV, which theoretically should provide a measure of EF1/EF and can be derived from phase contrast measurements alone correlated poorly with EF1/EF and was a relatively poor predictor of outcome. This may be due to errors in measurement of flow, limited temporal resolution of aortic flow or the presence of mild mitral regurgitation.
In the present study, where the majority of clinical events were AVR, MPG was, as expected, the most important predictor of outcome. However, CMR EF1 was a powerful predictor of AVR or death with a threshold of 20%, independent of AS severity. This is consistent with our TTE EF1 data[1, 2], allowing for the mean difference of 5% between CMR EF1 and TTE EF1. The prognostic value of EF1 demonstrates the importance of examining LV function in early systole over the portion of the cardiac cycle in which there is active contraction. The marked discordance between EF1 and overall LVEF in relation to outcomes is consistent with length-dependent regulation of sarcomere function acting as a homeostatic mechanism to preserve EF when initial contraction is impaired.
CMR allows the correlation of systolic LV function with structural change in the myocardium. That iECV was a predictor of outcome on univariate but not on multivariable analysis once EF1 was included in the model suggests that impact of iECV on outcome is mediated through its functional effects on early systolic contraction. This would be consistent with early expansion of the extracellular matrix due to chronic increased afterload as well as later apoptosis of myocytes and replacement fibrosis, both of which may occur prior to the onset of symptoms or a deterioration in overall ejection fraction [14, 15]. The combined power of CMR to assess early systolic function by EF1 as well as the underling myocardial structure may offer new insights into a variety of cardiac pathologies characterised by myocardial fibrosis and help refine the structural measures most closely related to function and hence to prognosis.
Limitations
The present study has several limitations. Firstly, this is a post-hoc analysis of a single centre observational cohort with a relatively small sample size. Our observations regarding EF1 are consistent with two prior reports of TTE EF1 in AS, one of which was conducted in this cohort, but are subject to confounding. Conclusions regarding causality cannot be drawn from the cross-sectional correlations presented. Both CMR and TTE EF1 were measured from a single beat, which did not account for beat-to-beat variation, a weakness common to many haemodynamic measurements. Phase contrast (flow) and cine imaging were not obtained at the same time and this could have contributed to variation in EF1. However, the majority of patients were in sinus rhythm and variability of CMR-derived EF1 was less than that of TTE-derived EF1. CMR and TTE were not performed on the same day but in most subjects were performed within 5 days. CMR EF1 requires adequate short axis 3D stack image quality and could not be measured in 25 patients. Larger prospective studies will be required to determine the relative prognostic power of CMR and TTE EF1.
Conclusions
EF1, a simple and robust marker of early LV impairment, be measured accurately by CMR, and predicts outcome in AS. Its measurement by CMR is more reproducible than that by TTE and may facilitate LV structure–function analysis.
Availability of data and materials
The datasets used and/or analysed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- AS:
-
Aortic stenosis
- AVA:
-
Aortic valve area
- BNP:
-
Brain natriuretic peptide
- CMR:
-
Cardiovascular magnetic resonance
- ECV:
-
Extracellular volume fraction
- EDV:
-
End-diastolic volume
- EF:
-
Ejection fraction
- EF1:
-
First-phase ejection fraction
- GLS:
-
Global longitudinal strain
- hs-cTnl:
-
High-sensitivity cardiac troponin I
- LGE:
-
Late gadolinium enhancement
- LOA:
-
Limit of agreement
- LV:
-
Left ventricle/left ventricular
- LVMI:
-
Left ventricular mass index
- MPG:
-
Mean pressure gradient
- NYHA:
-
New York Heart Association
- ROC:
-
Receiver-operating characteristic
- SVI:
-
Stroke volume index
- TTE:
-
Transthoracic echocardiography
- V1:
-
Volume at the time of peak aortic flow
- Zva:
-
Valvuloarterial impedance
References
Gu H, Saeed S, Boguslavskyi A, Carr-White G, Chambers JB, Chowienczyk P. First-phase ejection fraction is a powerful predictor of adverse events in asymptomatic patients with aortic stenosis and preserved total ejection fraction. JACC Cardiovasc Imaging. 2019;12(1):52–63.
Bing R, Gu H, Chin C, Fang L, White A, Everett RJ, Spath NB, Park E, Jenkins WS, Shah AS, Mills NL, Flapan AD, Chambers JB, Newby DE, Chowienczyk P, Dweck MR. Determinants and prognostic value of echocardiographic first-phase ejection fraction in aortic stenosis. Heart. 2020;106(16):1236–43.
Thaden JJ, Nkomo VT, Enriquez-Sarano M. The global burden of aortic stenosis. ProgCardiovasc Dis. 2014;56(6):565–71.
Pellikka PA, She L, Holly TA, Lin G, Varadarajan P, Pai RG, Bonow RO, Pohost GM, Panza JA, Berman DS, Prior DL, Asch FM, Borges-Neto S, Grayburn P, Al-Khalidi HR, Miszalski-Jamka K, Desvigne-Nickens P, Lee KL, Velazquez EJ, Oh JK. Variability in ejection fraction measured by echocardiography, gated single-photon emission computed tomography, and cardiac magnetic resonance in patients with coronary artery disease and left ventricular dysfunction. JAMA Netw Open. 2018;1(4):e181456.
Pontone G, Guaricci AI, Andreini D, Solbiati A, Guglielmo M, Mushtaq S, Baggiano A, Beltrama V, Fusini L, Rota C, Segurini C, Conte E, Gripari P, Dello Russo A, Moltrasio M, Tundo F, Lombardi F, Muscogiuri G, Lorenzoni V, Tondo C, Agostoni P, Bartorelli AL, Pepi M. Prognostic benefit of cardiac magnetic resonance over transthoracic echocardiography for the assessment of ischemic and nonischemic dilated cardiomyopathy patients referred for the evaluation of primary prevention implantable cardioverter-defibrillator therapy. CircCardiovasc Imaging. 2016. https://doi.org/10.1161/CIRCIMAGING.115.004956.
Chin CWL, Everett RJ, Kwiecinski J, Vesey AT, Yeung E, Esson G, Jenkins W, Koo M, Mirsadraee S, White AC, Japp AG, Prasad SK, Semple S, Newby DE, Dweck MR. Myocardial fibrosis and cardiac decompensation in aortic stenosis. JACC Cardiovasc Imaging. 2017;10(11):1320–33.
Treibel TA, Kozor R, Schofield R, Benedetti G, Fontana M, Bhuva AN, Sheikh A, Lopez B, Gonzalez A, Manisty C, Lloyd G, Kellman P, Diez J, Moon JC. Reverse myocardial remodeling following valve replacement in patients with aortic stenosis. J Am CollCardiol. 2018;71(8):860–71.
Schulz-Menger J, Bluemke DA, Bremerich J, Flamm SD, Fogel MA, Friedrich MG, Kim RJ, von Knobelsdorff-Brenkenhoff F, Kramer CM, Pennell DJ, Plein S, Nagel E. Standardized image interpretation and post processing in cardiovascular magnetic resonance: Society for Cardiovascular Magnetic Resonance (SCMR) board of trustees task force on standardized post processing. J CardiovascMagnReson. 2013;15:35.
Lang RM, Bierig M, Devereux RB, Flachskampf FA, Foster E, Pellikka PA, Picard MH, Roman MJ, Seward J, Shanewise JS, Solomon SD, Spencer KT, Sutton MS, Stewart WJ, Chamber Quantification Writing Group; American Society of Echocardiography’s Guidelines and Standards Committee; European Association of Echocardiography. Recommendations for chamber quantification: a report from the American Society of Echocardiography’s Guidelines and Standards Committee and the Chamber Quantification Writing Group, developed in conjunction with the European Association of Echocardiography, a branch of the European Society of Cardiology. J Am SocEchocardiogr. 2005;18(12):1440–63.
Baumgartner H, Hung J, Bermejo J, Chambers JB, Edvardsen T, Goldstein S, Lancellotti P, LeFevre M, Miller F Jr, Otto CM. Recommendations on the echocardiographic assessment of aortic valve stenosis: a focused update from the European Association of Cardiovascular Imaging and the American Society of Echocardiography. J Am SocEchocardiogr. 2017;30(4):372–92.
Baumgartner H, Falk V, Bax JJ, De Bonis M, Hamm C, Holm PJ, Iung B, Lancellotti P, Lansac E, Rodriguez Munoz D, Rosenhek R, Sjogren J, Tornos Mas P, Vahanian A, Walther T, Wendler O, Windecker S, Zamorano JL, Group ESCSD. 2017 ESC/EACTS Guidelines for the management of valvular heart disease. Eur Heart J. 2017;38(36):2739–91.
Briand M, Dumesnil JG, Kadem L, Tongue AG, Rieu R, Garcia D, Pibarot P. Reduced systemic arterial compliance impacts significantly on left ventricular afterload and function in aortic stenosis: implications for diagnosis and treatment. J Am CollCardiol. 2005;46(2):291–8.
Baron RM, Kenny DA. The moderator-mediator variable distinction in social psychological research: conceptual, strategic, and statistical considerations. J PersSocPsychol. 1986;51(6):1173–82.
Bing R, Dweck MR. Myocardial fibrosis: why image, how to image and clinical implications. Heart. 2019;105(23):1832–40.
Piek A, de Boer RA, Sillje HH. The fibrosis-cell death axis in heart failure. Heart Fail Rev. 2016;21(2):199–211.
Acknowledgements
Authors would like to thank Louise Keehn’s input in performing the CMR EF1 inter-observer analysis.
Funding
HG supported by National Institute for Health Research, UK (ICA-CL-2018-04-ST2-012); RB and MD supported by Sir Jules Thorn Charitable Trust, UK (15/JTA); MD, DEN, HG and PC supported by British Heart Foundation, UK (PG/19/23/34259); DEN supported by Wellcome Trust, UK (WT103782AIA).
Author information
Authors and Affiliations
Contributions
HG: design of the work, data acquisition, the analysis, interpretation of data, drafted the work; RB: design of the work, data acquisition, analysis and interpretation of data, substantively revised the work; CC: data acquisition; LF: data acquisition; AW: data acquisition; RE: data acquisition; NS: data acquisition; EP: data acquisition; WJ: data acquisition; JC: substantively revised the work; DN: substantively revised the work; AC: substantively revised the work; MD: design of the work, substantively revised the work; PC: design of the work, interpretation of data, substantively revised the work. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
The study was approved by the regional ethics committee (10/S1102/24) and conducted in accordance with the Declaration of Helsinki. Written informed consent was obtained from all subjects.
Consent for publication
All authors agreed to publication.
Competing interests
Haotian Gu and Phil Chowienczyk are named on a patent application for EF1. Other authors have no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Gu, H., Bing, R., Chin, C. et al. First-phase ejection fraction by cardiovascular magnetic resonance predicts outcomes in aortic stenosis. J Cardiovasc Magn Reson 23, 73 (2021). https://doi.org/10.1186/s12968-021-00756-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12968-021-00756-x