Abstract
Background
Neonatal mortality remains unacceptably high in many low and middle-income countries, including India. A community mobilisation intervention using participatory learning and action with women’s groups facilitated by Accredited Social Health Activists (ASHAs) was conducted to improve maternal and newborn health. The intervention was evaluated through a cluster-randomised controlled trial conducted in Jharkhand and Odisha, eastern India. This aims to assess the cost-effectiveness this intervention.
Methods
Costs were estimated from the provider’s perspective and calculated separately for the women’s group intervention and for activities to strengthen Village Health Sanitation and Nutrition Committees (VHNSC) conducted in all trial areas. Costs were estimated at 2017 prices and converted to US dollar (USD). The incremental cost-effectiveness ratio (ICER) was calculated with respect to a do-nothing alternative and compared with the WHO thresholds for cost-effective interventions. ICERs were calculated for cases of neonatal mortality and disability-adjusted life years (DALYs) averted.
Results
The incremental cost of the intervention was USD 83 per averted DALY (USD 99 inclusive of VHSNC strengthening costs), and the incremental cost per newborn death averted was USD 2545 (USD 3046 inclusive of VHSNC strengthening costs). The intervention was highly cost-effective according to WHO threshold, as the cost per life year saved or DALY averted was less than India’s Gross Domestic Product (GDP) per capita. The robustness of the findings to assumptions was tested using a series of one-way sensitivity analyses. The sensitivity analysis does not change the conclusion that the intervention is highly cost-effective.
Conclusion
Participatory learning and action with women’s groups facilitated by ASHAs was highly cost-effective to reduce neonatal mortality in rural settings with low literacy levels and high neonatal mortality rates. This approach could effectively complement facility-based care in India and can be scaled up in comparable high mortality settings.
Similar content being viewed by others
Background
The state of newborn health in India is of global importance, as India accounts for around a quarter of all neonatal deaths globally, with an estimated 779,000 out of 2.9 million neonatal deaths in 2012 [1, 2]. The national average neonatal mortality rate of 28 masks inequalities between richer and poorer states, as well as within states [3]. Although the proportion of women delivering with a skilled birth attendant has been increasing steadily in India, community interventions remain key to increasing demand for health services, birth preparedness as well as improving care for mothers and newborns at home [4].
A community based intervention called Participatory Learning Approach (PLA) approach with women’s groups reduced neo-natal mortality in the underserved areas of two eastern states of India, Jharkhand and Odisha [5], and the benefits accrued most to the most marginalised [6]. PLA with women’s groups gave similar results in terms of reducing neo-natal mortality in other studies conducted in Nepal, Bangladesh and Malawi [7–11]. A pooled analysis of the randomised control trials conducted in four different country sites India, Bangladesh, Malawi and Nepal also showed significant reduction in maternal mortality through PLA intervention [12].
Participatory Learning Approach (PLA) approach is a capacity building process in which women’s group members invite non group-members, adolescent girls, pregnant women, mothers, and men, frontline service providers for learning, planning, carrying out and evaluating activities in a participatory and sustained basis. Trained facilitators enable this community process. The approach is to engage communities in discussions on issues concerning them, build their understanding on the underlying causes and the cause and effect relationship, explore strengths and resources available and develop feasible strategies to overcome those issues. PLA approach has four phases. Phase one focusses on participatory identification and prioritization of maternal and child health problems besides sensitising community on the issue of ‘equity’ through picture cards and games. Phase two focusses on developing possible strategies for addressing the prioritised problems through different tools like storytelling and role plays. Games are employed to develop the understanding of the community members on cause and effect relationship, intermediate and underlying causes and possible prevention and management. This enables the community members to come up with the strategies together and collectively share the responsibilities among them to implement those strategies. Phase three is the action phase for the group where groups take actions according to the strategies they finalise with respective roles and responsibilities. Phase four is the stage where groups collectively evaluate the progress, learning and challenges throughout the PLA meeting cycle which they have gone through. This gives them idea of what worked well, what are their results, which are the areas where more effort is needed and how was the support from the other stakeholders.
From September 2010 to December 2012 (28 months), Ekjut, a charitable organisation registered under Societies Registration Act 1860 and working on maternal, newborn, child health and nutrition (MNCHN) in eastern India in collaboration with University College London–Institute for Global Health, UK, conducted a cluster-randomised controlled trial in five districts of Jharkhand and Odisha, eastern India, to assess the effect of a participatory learning and action (PLA) cycle with women’s groups facilitated by Accredited Social Health Activists (ASHAs) aiming to improve maternal and neonatal health. ASHAs are female community health workers incentivised under the National Health Mission (NHM) of India. They are primarily responsible for mobilising communities to increase demand for maternal and child health care services and promote institutional deliveries [13]. The objective of conducting this study was to see whether conducting PLA meetings by ASHAs with women’s group will achieve reduction in neo-natal mortality as were achieved previously in different trial settings.
It was found that, ASHA facilitated PLA women’s group intervention reduced neonatal mortality by 31 percent in the intervention area compared to the control area. The primary target groups for the PLA intervention were pregnant women and women of reproductive age from the indigenous (tribal) communities. These women were actively encouraged to participate in the women’s group meetings and join the women’s groups. As the focus was to actively target women from the marginalised communities, the results show that home visits by ASHAs in the intervention areas were more among the most marginalised groups compared to the less marginalised groups. Though home care practices for mothers and newborn were increased in both intervention and control areas, significant increase was found in the infants being wrapped in the intervention areas compared to the control areas. Similarly, newborn being placed to mother’s skin within 1 h was significantly increased in the intervention areas compared to the control areas. Proportion of institutional delivery was also found to be high in the intervention area compared to the control area. Since, throughout the intervention, focus was given to the women from the most marginalised community defined as those belonging to scheduled tribe community, being in the first and second lowest asset quintiles and unable to read and write, it was found that reduction in neo-natal mortality was the most among the most marginalised communities [14].
The aim of this paper is to measure the cost-effectiveness of participatory learning and action (PLA) with women’s group facilitated by ASHAs to improve birth outcome as compared to the control area. The analysis was done from the provider’s perspective, where project cost was analysed for reduction in neo-natal mortality using trial data.
Methods
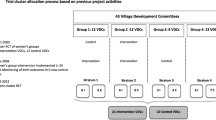
The trial was conducted in 30 purposively created geographical clusters of three underserved districts of Jharkhand (Ranchi, Khunti and Godda) and two districts of Odisha (Mayurbhanj and Rayagada), covering an estimated population of 156,519. 15 clusters were randomly allocated to receive the PLA intervention (estimated population 82,702), and 15 clusters to a control arm (estimated population 73,817) [14] These districts were selected because about half of the population of these districts belong to Scheduled TribeFootnote 1 community. However, in the study population, around 70% of the population belong to Scheduled Tribe community that have very high maternal and neonatal mortalities compared to the state and national average [14].
In the intervention clusters, 137 ASHAs were incentivised to conduct PLA meetings with women’s groups. Also, in both the intervention and control clusters, Ekjut organised monthly meetings with the village health sanitation and nutrition committees (VHSNCs) about their rights and entitlements. The details of PLA meetings and VHSNC meetings are described elsewhere [14]. One intervention cluster (estimated population 6203) was lost to follow up and the trial results have been presented comparing 14 intervention clusters (estimated population 76,499) and 15 control clusters (estimated population 73,817) [14]. The intervention reduced neonatal mortality by 31% (adjusted odds ratio [aOR] 0.69, 95% CI 0.53–0.89) during a 24 months’ intervention period (Jan 1, 2011, to Dec 31, 2012) [14]. We conducted a cost-effectiveness analysis comparing the women’s group intervention facilitated by ASHAs with current practice.
We conducted a cost-effectiveness analysis from the provider’s perspective. We included costs incurred by the organisation (Ekjut) implementing the intervention. Project costs were taken from the organisation’s accounting data. The accounting system was designed so that most costs could be identified separately for different cost centres. As these data are financial or accounting costs, they were converted to economic costs [15].
As suggested by Ramsey et al. [16], the time horizon was determined by the trial duration, i.e. 28 months from September 2010 to December 2012. This includes the start-up period for activities conducted before the intervention began and implementation period. The period between September 2010 and December 2010 was considered as ‘start-up’ period. During this period, we undertook preparatory exercises to start women’s groups and set up a monitoring system to collect data related to births and neonatal deaths.
We used a step-down costing methodology [17]. Costs from project accounts were fed into a customized tool created in MS Excel. The worksheets for entering data allocated costs to one of the following categories: staff, other recurring costs, capital, and joint costs. The costs were further divided into start-up and implementation costs, and between programme components (i.e. Women’s Group, VHSNC Strengthening), and research costs. Table 1 provides an overview of cost categorisations.
Costs that could be easily identified with different programme components (women’s group, VHSNC strengthening and research costs) were allocated to them directly. Joint costs (for example general administration, office running costs and utility charges) were not easily identifiable with programme components and were initially put under joint costs. Joint costs were then allocated to the program components in proportion to their costs in relation to the total costs, in order to get the final total cost of the program components. For allocating staff time, monthly time sheets were completed after discussing with the concerned staff. Staff time was allocated to the above programme components and joint costs using completed time sheets. The same basis for allocation was taken for different costs items, including fuel, travel, communication and maintenance costs. Capital costs were converted into yearly expenditure with a depreciation of 10% on diminishing value. Start-up costs were capitalised over the project life cycle, assuming that these investments would have effects until the end of the project. As suggested by Gilson et al. [18], all costs related to newborn births and deaths surveillance were considered as research costs and were excluded from the cost analysis.
All costs were inflated to estimate their present value of 2107 price and converted to 2017 US dollar prices [USD1 = 68.07 Indian rupees (INR)] [19].
To examine the effect of variations in some uncertain variables on the incremental cost per DALY averted, we performed a series of one-way sensitivity analyses. This was done to check the robustness of our findings to assumptions. Table 2 describes the variables tested while performing these sensitivity analyses. These included the discount rate for both costs and outcomes, exchange rate, changing the number of neonatal deaths averted using the confidence interval for the odds ratio for the reduction in neonatal mortality from the parent trial, and changing the life-expectancy at birth in the calculation of DALY.
Results
161 women’s groups were created in the intervention area. Each women’s group had undergone 33 meetings by the end of intervention period. 137 ASHAs facilitated these participatory learning and action meetings. Table 3 provides an overview of the intervention costs. The total unit cost for facilitating a women’s group was USD 24 and the total unit cost per women’s group was USD 790. The average intervention cost per person was USD 1.66 (USD 1.99 including VHSNC strengthening costs) and average intervention cost per livebirth was USD 35.31 (USD 42.28 including VHSNC strengthening costs).
The total intervention cost of ASHAs facilitating women’s group’s using participatory learning and action was USD 127,230 (USD 152,318 inclusive of VHSNC strengthening cost). During the implementation period (Jan 1, 2011 to Dec 31, 2012), we identified 3700 births (including 3,603 livebirths) in the intervention arm, and 3519 births (including 3439 livebirths) in the control arm. The neonatal mortality rate during the follow up period between 2011 and 2012 was 30 per 1000 livebirths in the intervention arm and 44 per 1000 livebirths in the control arm. We observed a 31% reduction in neonatal mortality (adjusted odds ratio [aOR] 0.69, 95% CI 0.53–0.89) in the intervention arm compared to the control arm [14]. After adjusting for the number of livebirths in the intervention and control arms, we found that the intervention averted 50 neonatal deaths in the intervention areas (refer Table 4).
For calculating DALY averted, disability weight for neo-natal death was taken of 1. The life expectancy of Japanese women [20] of 86 years [21] was taken as standard value. Discount rate for discounting future lives was taken of 3% and age of onset of neo-natal death was taken 0 year. Using these parameters, years of life lost due to premature deaths (YLLs) for one child was estimated to be 30.81 years. Hence, for averting 50 children’s deaths, the total years of life lost due to premature deaths (YLLs) averted or DALYs averted were estimated to be 1541 [22].
Table 5 provides an overview of the cost-effectiveness results. The cost of the intervention per DALY averted was USD 83/DALY (USD 99/DALY, inclusive of VHSNC strengthening cost) and the cost per newborn death averted was USD 2545 for the women’s group intervention only (USD 3046 inclusive of VHSNC strengthening cost) at 2017 prices. According to WHO, an intervention can be considered highly cost-effective if the cost per life year saved or DALY averted is less than the per capita Gross Domestic Product (GDP) of that country [23]. The women’s group intervention can therefore be considered as ‘highly cost-effective’ as it is much less than India’s per capita GDP in 2017 (USD 1830) [24].
Table 6 describes the results of the sensitivity analyses. We found that the cost per DALY averted varied from USD 25/DALY (USD 30/DALY inclusive of VHSNC strengthening cost) to USD 273/DALY (USD 326/DALY inclusive of VHSNC strengthening cost) in response to changes in the uncertain variables. The variations in cost-effectiveness results were significant when the outcome was discounted at 6%, and when neonatal mortality reduction was set at the lower end of the confidence interval observed during the trial. The sensitivity analysis does not change the conclusion that the intervention is highly cost-effective.
Discussion
The women’s group PLA intervention facilitated by ASHAs was a highly cost-effective intervention to reduce neonatal mortality, according to WHO standards. In 2017, India’s expected GDP per capita would be USD 1830 and our estimate of cost life year saved (USD 83) falls well below this threshold. A comparison of ASHA-facilitated PLA women’s group intervention with similar PLA women’s group interventions implemented by Ekjut in India shows that this intervention was somewhat less cost-effective than previous ones. The cost per DALY of the previous two women’s group interventions led by Ekjut with its own trained and supported facilitators were USD 42 between 2005 and 2008 and USD 26 between 2008 and 2009 after inflating them to 2017 USD [5, 25]. However, the intervention was more cost-effective than other interventions with women’s groups practising participatory learning and action to improve maternal and newborn health in other parts of the world. The cost per DALY averted or life year saved using participatory women’s groups in Makwanpur district, Nepal, between 2000 and 2003 was USD 163 after inflating it to 2017 USD [7, 8]. Similarly, the cost per DALY averted for PLA with women’s group intervention under Perinatal Care Project in Bangladesh between 2009 and 2011 ranged from USD 263 to USD 469 after inflating them to 2017 USD [9]. Also, the cost per DALY averted for a similar intervention in rural Malawi between 2005 and 2009 was USD 140 (including both neonatal and maternal deaths averted) and MaiKhanda between 2008 and 2010 was USD 89 for community intervention (CI) after inflating them to 2017 USD [10, 11].
If the women’s group intervention was implemented on a larger scale, average costs would, in all likelihood, be reduced due to economies of scale. These might even outweigh the reduced effectiveness of interventions often documented in scale up programmes [26]. Also, costs may be further reduced if the coverage per district would increase because in the current trial, management and support structure created to support the intervention could have potentially served a larger geographical area and larger population. This could have also saved many more lives and hence could have lowered the cost per life year saved, without additional support/management cost. Training costs could also be further reduced as during the trial, a cascading training plan was used where support staff were centrally trained in four phases, followed by decentralised training of ASHAs in five phases. If the intervention was scaled up to a larger geographical area, a pool of trainers from different blocks (large administrative areas of 100,000 population) could be created to provide trainings to ASHAs directly in their respective blocks.
Ministry of Health and Family Welfare (MoHFW), Government of India (GoI) has decided to scale up ASHA facilitated PLA to reduce maternal and neonatal mortality in ten Indian states and issued government order in this regard to the NHM in all ten states. National Health System Resource Centre (NHSRC) working under MoHFW, GoI and Ekjut is providing technical support to all ten states’ NHM in scaling up PLA. NHM in Jharkhand has already implemented ASHA facilitated PLA on maternal and newborn care across the state of Jharkhand. However, for training of ASHAs, a slightly modified mechanism is being tried out. In the trial setting, Ekjut imparted trainings to all ASHAs from the intervention area and after that, ASHAs conducted PLA meetings with women’s group. In this scaling up model, instead of imparting PLA trainings directly to approximate 40,000 ASHAs working across the state, trainings will be imparted to approximate 2000 “ASHA facilitators” (supervisors) from the state. Each “ASHA facilitator” supports and supervises approximate 20 ASHAs from 20 villages and hamlets. These “ASHA facilitators” will be trained to conduct PLA meetings with women’s groups. They will then provide on-the-job trainings to the ASHAs they supervise. In the proposed scale up model, one “ASHA facilitator” will conduct a women’s group PLA meeting every month in ten villages together with the ASHAs from these villages and in the presence of ten other ASHAs from the neighbouring villages whom they supervise. This on the job, observational training will enable the visiting ASHAs to conduct similar meetings in their own villages. Every month, “ASHA facilitators” will rotate between their two groups of ten villages and conduct PLA meetings. This arrangement will reduce the costs of training substantially and enable faster scale up across the state. The reduction in start-up time for women’s group meetings will also cut a substantial amount of time, operational and management costs that would have been incurred if the ASHAs had been trained directly instead of through on-the-job training by “ASHA facilitators”. In Jharkhand, the scale up is being done in collaboration with the state’s National Health Mission; management and support structures are already in place, and the incremental costs for supporting PLA by the existing staff will be much less compared to what it would have been if a separate support structure had been created for this. A large scale controlled study has been planned and will be conducted by University College London–Institute for Global Health, UK. This will be done by prospective monitoring of births and deaths through a robust surveillance system. This evaluation will cover around ten million population to assess whether scaling up of ASHA facilitated PLA with women’s groups through this method is as effective as the previous ones in terms of reducing maternal and neo-natal deaths. It would also be wise to assess the cost-effectiveness of the revised scaling up model.
To scale-up PLA with women’s group through ASHAs across the country, we calculated the approximate scale-up costs. Four major cost components, which are important for scaling PLA with women’s groups through ASHAs are—trainings of ASHAs on PLA meeting cycle, printing of ASHA modules, printing of picture cards and incentives to ASHAs for organising PLA women’s group meetings. It was assumed that the current management and supervision mechanism already put in place to manage and supervise ASHAs’ work under National Health Mission (NHM) at the national and state levels will take care of ASHA facilitated PLA with women’s group program. Hence, no incremental costs related to management and supervision of this program were considered for assessing the total incremental costs of ASHA facilitated PLA with women’s groups. There are around 9,00,000 ASHAs working across the country [14]. Table 7 gives details of budgetary outlay for scaling up ASHA facilitated PLA. The total approximate budgetary outlay to support PLA with women’s group through ASHAs across the country would be around INR 378 crores. This is around 0.77% of the total health budget allocated for the year 2017–2018 and around 1.39% of the total budget allocated for National Health Programme (NHM) during the same year, which is primarily initiated to improve indicators like maternal mortality ratio (MMR), infant mortality rate (IMR), under-five mortality rate (U5MR) and total fertility rate (TFR) through different schemes. This shows that, ASHA facilitated PLA women’s group program can easily be scaled up by the government across India through a large network of ASHAs without substantial budgetary outlay. This will not only make community empowered and aware about maternal and newborn care practices but also lead to increase in uptake of existing maternal and child care programs being run under the umbrella of NHM. ASHAs are community health workers and have been given responsibilities of increasing uptake of ante-natal checkups, institutional deliveries, home visits and counselling, immunisation and disseminating information related to maternal and child care. Facilitating PLA with women’s groups will not only give ASHAs a platform to disseminate information related to maternal and child care but also improve their interpersonal skill and building community awareness and knowledge which lead to increase in demand of available services related to maternal and child care. This will make the job of the ASHAs easier and strengthen their relation with the community members.
Participatory learning and action with women’s groups facilitated by ASHAs is well suited to high mortality settings in India, particularly in underserved areas where access to health facilities and supply-side interventions is limited. PLA can only bring down avoidable deaths to some extent, due to changes in home care practices and community action for maternal and newborn health. However, to further reduce maternal and neonatal mortality rates, it would need to strengthen the public health system so that women and children can easily access quality health services. There is also evidence that marginalised mothers benefit the most from this approach [6, 22]. The approach works best if the coverage of a women’s group is about 450–700 population, and at least a third of the pregnant women participate in the women’s groups meetings [23]. PLA with women’s group intervention is recommended for those areas where marginalised population are living, where maternal and neonatal mortality rates are very high and where there is limited reach of government health services. In such places, this intervention is effective within limited resources, by cutting down the delays in identifying risks and seeking care, and in changing practices at home. Together with efforts to increase access to quality, facility-based maternal and newborn care, community interventions such as participatory learning and action with women’s groups can save lives.
Conclusion
Participatory learning and action with women’s groups has been proven to reduce neonatal mortality in high-risk areas of India and is highly cost effective. There is substantial potential for replicating the intervention in other parts of India through Government systems. In India, the intervention can be taken up by ASHAs through regular government programmes in a cost-effective manner. The government can also use innovative models for scaling up participatory learning and action with women’s groups, thereby reducing the cost of scale up without compromising the quality of intervention. This would further improve the cost-effectiveness of the intervention so that government can use its limited resources efficiently.
Notes
Scheduled Tribe (ST) is an officially designated group recognised in the Constitution of India. The tribes under this group are historically disadvantaged indigenous people in India.
Abbreviations
- ASHAs:
-
Accredited Social Health Activists
- VHSNCs:
-
Village Health Sanitation and Nutrition Committees
- USD:
-
United States dollar
- ICER:
-
incremental cost-effectiveness ratio
- WHO:
-
World Health Organisation
- DALYs:
-
disability-adjusted life years
- GDP:
-
Gross Domestic Product
- PLA:
-
participatory learning and action
- NHM:
-
National Health Mission
- aOR:
-
adjusted odds ratio
- INR:
-
Indian rupees
- LYS:
-
life year saved
- CHOICE:
-
choosing intervention which are cost effective
- GBD:
-
global burden of disease
References
UNICEF. State of the World’s Children 2015: Maternal and Newborn Health; 2015.
Lawn JE, Blencowe H, Oza S, et al. Every newborn: progress, priorities, and potential beyond survival. Lancet. 2014;384:189–205.
World Health Organisation. State of inequality: maternal, newborn and child health; 2015.
Lassi ZS, Haider BA, Bhutta ZA. Community-based intervention packages for reducing maternal and neonatal morbidity and mortality and improving neonatal outcomes. Cochrane Database Syst Rev. 2010;2010(11):CD007754.
Tripathy P, Nair N, Barnett S, Mahapatra R, Borghi J, Rath S, Gope R, Mahto D, Sinha R, Lakshminarayana R. Effect of a participatory intervention with women’s groups on birth outcomes and maternal depression in Jharkhand and Orissa, India: a cluster-randomised controlled trial. Lancet. 2010;375(9721):1182–92.
Houweling TA, Tripathy P, Nair N, Rath S, Rath S, Gope R, Sinha R, Looman CW, Costello A, Prost A. The equity impact of participatory women’s groups to reduce neonatal mortality in India: secondary analysis of a cluster-randomised trial. Int J Epidemiol. 2013;42(2):520–32. doi:10.1093/ije/dyt012
Manandhar DS, Osrin D, Shrestha BP, Mesko N, Morrison J, Tumbahangphe KM, Tamang S, Thapa S, Shrestha D, Thapa B, Shrestha JR. Effect of a participatory intervention with women’s groups on birth outcomes in Nepal: cluster-randomised controlled trial. Lancet. 2004;364(9438):970–9.
Borghi J, Thapa B, Osrin D, Jan S, Morrison J, Tamang S, Shrestha BP, Wade A, Manandhar DS, Anthony MD. Economic assessment of a women’s group intervention to improve birth outcomes in rural Nepal. Lancet. 2005;366(9500):1882–4.
Fottrell E, Azad K, Kuddus A, Younes L, Shaha S, Nahar T, Aumon BH, Hossen M, Beard J, Hossain T, Pulkki-Brannstrom AM. The effect of increased coverage of participatory women’s groups on neonatal mortality in Bangladesh: a cluster randomized trial. JAMA Pediatr. 2013. doi:10.1001/jamapediatrics.2013.2534.
Lewycka S, Mwansambo C, Rosato M, Kazembe P, Phiri T, Mganga A, Chapota H, Kainja E, Newell ML, Greco G, Pulkki-Brännström AM. Effect of women’s groups and volunteer peer counselling on rates of mortality, morbidity, and health behaviours in mothers and children in rural Malawi (MaiMwana): a factorial, cluster-randomised controlled trial. Lancet. 2013;381(9879):1721–35.
Colbourn T, Pulkki-Brännström AM, Nambiar B, Kim S, Bondo A, Banda L, Makwenda C, Batura N, Haghparast-Bidgoli H, Hunter R, Costello A. Cost-effectiveness and affordability of community mobilisation through women’s groups and quality improvement in health facilities (MaiKhanda trial) in Malawi. Cost Effect Resour Alloc. 2015;13(1):1. doi:10.1186/s12962-014-0028-2.
Prost A, Colbourn T, Seward N, Azad K, Coomarasamy A, Copas A, Houweling TA, Fottrell E, Kuddus A, Lewycka S, MacArthur C. Women’s groups practising participatory learning and action to improve maternal and newborn health in low-resource settings: a systematic review and meta-analysis. Lancet. 2013;381(9879):1736–46.
National Health Mission, Ministry of Health and Family Welfare, Government of India. Communitisation: About Accredited Social Health Activist (ASHA). http://nrhm.gov.in/communitisation/asha/about-asha.html. Accessed 10 Jan 2016.
Tripathy P, Nair N, Sinha R, Rath S, Gope RK, Rath S, Roy SS, Bajpai A, Singh V, Nath V, Ali S. Effect of participatory women’s groups facilitated by Accredited Social Health Activists on birth outcomes in rural eastern India: a cluster-randomised controlled trial. Lancet Global Health. 2016;4(2):e119–28.
Batura N, Pulkki-Brännström AM, Agarwal P, Bagra A, Haghparast-Bidgoli H, Bozzani F, Colbourn T, Greco G, Hossain T, Sinha R, Thapa B. Collecting and analysing cost data for complex public health trials: reflections on practice. Global Health Action. 2014;7:23257.
Ramsey S, Willke R, Briggs A, Brown R, Buxton M, Chawla A, et al. Good research practices for cost-effectiveness alongside clinical trials: the ISPOR Force Report. Value Health. 2005;8:521–33.
Conteh L, Waler D. How to do (or not to do) Cost and unit cost calculations using step-down accounting. Health Policy Plan. 2004;19:127–35.
Gilson L, Mkanje R, Grosskurth H, Mosha F, Picard J, Gavyole A, et al. Cost-effectiveness of improved treatment services for sexually transmitted diseases in preventing HIV-1 infection in Mwanza Region, Tanzania. Lancet. 1997;350:1805–9.
World Currency Exchange Rates and Currency Exchange Rate History. http://www.exchange-rates.org/. Accessed 30 Jan 2017.
Drummond MF, Sculpher MJ, Torrence GW, O’Brien BJ, Stoddart GL. Methods for the Economic Evaluation of Health Care Programmes. Oxford: Oxford University Press; 2005.
http://www.who.int/mediacentre/news/releases/2014/world-health-statistics-2014/en/. Accessed 25 Jan 2017.
Fox-Rushby JA, Hanson K. Calculating and presenting disability adjusted life years (DALYs) in cost-effectiveness analysis. Health Policy Plan. 2001;16(3):326–31.
WHO Cost effectiveness and strategic planning (WHO-CHOICE). Threshold values for intervention cost-effectiveness by Region. http://www.who.int/choice/costs/CER_levels/en/. Accessed 10 Jan 2016.
The World Bank. Data: GDP per capita (current USD). http://data.worldbank.org/indicator/NY.GDP.PCAP.CD. Accessed 30 Jan 2016.
Roy SS, Mahapatra R, Rath S, Bajpai A, Singh V, Rath S, Nair N, Tripathy P, Gope RK, Sinha R, Costello A. Improved neonatal survival after participatory learning and action with women’s groups: a prospective study in rural eastern India. Bull World Health Org. 2013;91(6):426–33.
Hanson C, Manzi F, Mkumbo E, Shirima K, Penfold S, Hill Z, et al. Effectiveness of a home-based counselling strategy on neonatal care and survival: a cluster-randomised trial in six districts of rural Southern Tanzania. PLoS Med. 2015;12(9):e1001881. doi:10.1371/journal.pmed.1001881.
Authors’ contributions
RS, PKT, NN, RG, SR and AP participated in the design of the study. RS and HHB designed the analysis framework and did the data analysis. RS wrote the first draft of the paper and coordinated all subsequent inputs. All authors read and approved the final manuscript.
Acknowledgements
The authors would like to thank the communities and group members who participated in the study. We would like to express our gratitude to all the colleagues particularly interviewers and Accredited Social Health Activists (ASHAs) who were the part of the study. We especially thank Amit Kumar Ojha and Birendra Mahto from Ekjut for providing all the cost data for doing the analysis.
Competing interests
The authors declare that they have no competing interests.
Data availability statements
Please contact author for data requests.
Ethics approval and consent to participate
The study was approved through an independent ethical research committee chaired by Dr. Alok K. Debdas in Jamshedpur, India and through the Research Ethics Committee of University College London (UK). Individual informed consent was sought from all the participants and those were recorded through a signature or thumbprint.
Role of the funding source
The funders had no role in study design, data collection, analysis, interpretation, or writing of the report.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated.
About this article
Cite this article
Sinha, R.K., Haghparast-Bidgoli, H., Tripathy, P.K. et al. Economic evaluation of participatory learning and action with women’s groups facilitated by Accredited Social Health Activists to improve birth outcomes in rural eastern India. Cost Eff Resour Alloc 15, 2 (2017). https://doi.org/10.1186/s12962-017-0064-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12962-017-0064-9