Abstract
The manifestation of cardiovascular risk factors, such as hypertension, diabetes, and particularly obesity begins in children and adolescents, with deleterious effects for cardiometabolic health at adulthood. Although the impact of diet on cardiovascular risk factors has been studied extensively in adults, showing that their cardiometabolic health is strongly lifestyle-dependent, less is known about this impact in children and adolescents. In particular, little is known about the relationship between their dietary patterns, especially when derived a posteriori, and cardiovascular risk. An adverse association of cardiovascular health and increased intake of sodium, saturated fat, meat, fast food and soft drinks has been reported in this population. In contrast, vitamin D, fiber, mono-and poly-unsaturated fatty acids, dairy, fruits and vegetables were positively linked to cardiovascular health.
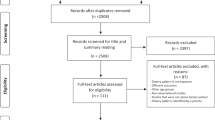
The aim of this review was to summarize current epidemiological and experimental evidence on the impact of nutrients, foods, and dietary pattern on cardiometabolic health in children and adolescents. A comprehensive review of the literature available in English and related to diet and cardiometabolic health in this population was undertaken via the electronic databases PubMed, Cochrane Library, and Medline.
Similar content being viewed by others
Introduction
It is well known that atherosclerosis progresses from childhood and adolescence to adulthood [1]. This process is related to the presence of cardiometabolic risk factors such as glucose intolerance, obesity, high blood pressure, high levels of total and low-density lipoprotein (LDL) cholesterol, and low levels of high-density lipoprotein (HDL) cholesterol. Due to the time course of atherosclerosis, it is difficult to establish a direct relationship between risk exposure and cardiovascular disease events; nonetheless, the available evidence indicates that childhood cardiometabolic risk factors are associated with an increased risk of cardiovascular disease in adulthood [1]. Furthermore, cardiometabolic risk variables in childhood are likely to persist into adulthood [2, 3].
Several studies have shown that hypertensive children have increased intimal-medial thickness (IMT) of the carotid artery [4, 5], increased left ventricular mass, and eccentric left ventricular geometry [6]. Data from the longitudinal Cardiovascular Risk in Young Finns Study indicate that childhood blood pressure and serum lipids are strongly related to adult values of these cardiometabolic risk variables [7]. Additionally, intermediate outcomes such as subclinical measures of atherosclerosis are used to determine the association between risk exposure in childhood and cardiovascular disease risk in adulthood. About 60 % of children with elevated blood pressure have hypertension as adults. This persistence of elevated blood pressure has been associated with the highest risk of increased carotid IMT [8]. Findings from the Muscatine, Cardiovascular Risk in Young Finns, and Bogalusa studies revealed an association between childhood cardiovascular risk factors and adult carotid IMT [9–12].
The increasing obesity epidemic has a particularly detrimental effect on cardiometabolic health in children and adolescents. A recent meta-analysis showed that obese children had a higher risk of an adverse cardiometabolic profile, compared to normal weight children [13]. Furthermore, the risk is especially high when overweight or obesity is maintained from childhood to adulthood [14].
High diet quality is strongly related to cardiometabolic health in adults [15, 16]. The Prevention with Mediterranean Diet study (PREDIMED) demonstrated the protective effect of the Mediterranean diet on cardiovascular disease in older patients with high cardiometabolic risk [17]. This review will focus on childhood diet and its role in the development of cardiovascular risk factors. Early prevention, ideally in childhood, could be the best strategy to avoid incidence of cardiometabolic risk factors and premature mortality; conversely, the adoption of a healthy diet at young ages is crucial for disease prevention. We will provide an overview of several aspects of the diet: main nutrients, certain foods known to play a role in cardiovascular health, and the most studied dietary patterns. Results of included studies are summarized in the Additional file 1: Table S1.
The impact of diet on cardiometabolic health
Na and salt intake
Most of the popular snacks that are very attractive to children contain a large amount of salt. In children, the daily recommended Na intake increases with age. For children younger than one year, the daily recommended salt intake is < 1 g/d (range 0.4−1.3 g/d); newborns and infants need more salt per kg of body weight than older children, in whom the adverse effects from excessive salt consumption are similar to adults. In children aged 1 to 5 and 5 to 10 years, the recommended daily intake is 2 g/d and 4 g/d, respectively; however, the actual salt intake reaches 4.9 g/d and 8.1, respectively. For those aged 10 to 20 years the recommendation is 5 g/d, although actual daily intake ranges from 6.7 to 11.0 g/d [18].
He and MacGregor (2006) [19] published a meta-analysis of randomized clinical trials that investigated the effect of reducing salt intake on blood pressure in children and infants. They showed that a reduced salt consumption (median reduction of 42 % in children and 54 % in infants) led to a significant decrease in blood pressure values:–1.17 mmHg (95 % CI–1.8,–0.56 mmHg) systolic and–1.29 mmHg (95 % CI–1.9,–0.65 mmHg) diastolic in children and–2.47 mmHg (95 % CI–4.0,–0.94 mmHg) systolic in infants. More recent studies confirmed those findings [20–22]. Finally, a study carried out in low-income children aged 3–4 years found a higher risk of elevated systolic blood pressure in those who consumed >1200 mg of sodium/day (3.32, 95 % CI 0.98, 11.2) or had >0.5 waist-to-height ratio (8.81, 95 % CI 2.1, 36.3) [23]. However, in other studies, no association was found between excessive consumption of sodium (i.e., exceeding recommended levels) and future high blood pressure [24, 25].
Fatty acids, nuts, and olive oil
Fatty acids and fats are an important source of energy, and fat makes food more attractive and tasty, especially for children; however, many studies have shown the positive association between fat consumption and obesity [26, 27]. In clinical and observational studies in children, higher consumption of total, unsaturated and saturated fats, and myristic fatty acids was associated with increased total cholesterol [28, 29]. Thorsdottir and Ramel (2003) found that total and saturated fat consumption was associated with incidence of diabetes [30]. Another randomized trial showed that milk low in saturated fatty acids and enriched in omega-3 polyunsaturated fatty acid (PUFA) and oleic acid reduces indices of endothelial cell activation in children aged 8–14 years [31]. In infants, intake of total fat and monounsaturated fats correlated with apolipoprotein A1 (Apo-A1), the main apolipoprotein of HDL-cholesterol, which is responsible for the efflux of cholesterol from the body (rho = 0.18, p = 0.036 and rho = 0.17, p = 0.048, respectively) [32]. The intake of polyunsaturated fatty acids was inversely correlated with apolipoprotein B (Apo-B), the main apolipoprotein of LDL-cholesterol and a marker of cardiovascular disease (rho = −0.17, p = 0.046).
Few studies have investigated the association of cardiovascular risk factors in children with consumption of food items and food groups rich in lipids. Haro-Mora et al. (2011) showed that children consuming only olive oil, among all vegetable oils used in the study, had lower risk of increased body mass index (BMI) Z-scores (OR 0.19 95 % CI 0.04, 0.52), compared with children consuming a combination of other oils [33]. High nut consumption (>1/4 oz. per day) in children 12–18 years old was associated with lower prevalence of overweight and obesity and lower levels of diastolic blood pressure [34]. A 40 % lower risk of overweight (95 % CI 0.43, 0.85) was observed in the top tertile of nuts consumption among healthy children and adolescents attending Seventh Day Adventist schools, where a high proportion of students are vegetarians or vegans in accordance with religious beliefs [35]. Among food groups with lipid-rich content, vegetable oils were associated with low fasting glucose (β = −3.34, 95 % CI–4.1,–0.27) and added fats (cream, butter, lard, creamy dressing, and sauces) were positively associated with higher levels of triglycerides (β =2.70, 95 % CI 0.29, 23.3) [36].
Dairy
Recently, more attention has been paid to the association between dairy products and cardiovascular risk factors in children. Bigornia et al. (2014) showed that 10-year-olds with higher consumption of full-fat and reduced-fat dairy products had 43 % (95 % CI 0.34, 0.94) and 26 % (95 % CI 0.43, 1.3) lower probability of being overweight or having excessive body fat in 3 years, respectively. [37]. Similar results were found in adolescents [38]. In Mexican children, consumption of flavored milk was associated with decreased risk of obesity (OR = 0.88, p = 0.004); a similar association was observed for whole milk, but only in univariate analysis, and there was no association for skimmed milk [39]. Flavored milks usually have higher energy per unit than non-flavored milk; however, the sugar and fat content of flavored milks differs according to the brand. Interestingly, consumption of skimmed milk was associated with increased adiposity in 2-to 4-year-olds, compared to consumption of full-fat milk (OR 1.64 and 1.63, p < 0.001 for 2-year-olds and 4-year-olds, respectively) [40].
Only a few studies have observed a positive association between consumption of milk and dairy products and adiposity in children [41, 42]; the remainder found inverse or no associations in children and adolescents [43]. Most of the studies about milk consumption were done in European populations; however, Lin Lin et al. (2012) found no association between milk or dairy consumption and both general and abdominal obesity surrogates in a Chinese sample of adolescents aged 11–13 years [44]. The researchers explain this difference in outcome, compared to the European population, as a possible confounding by socioeconomic position in European countries.
Although abdominal obesity is also a cardiovascular risk factor, few studies have investigated the association of dairy products consumption with this type of obesity. In a study by Abreu et al. (2012), high milk consumption was associated with lower abdominal obesity, independently of physical activity level: even the participants with low levels of physical activity and high milk consumption had lower odds of abdominal obesity (OR 0.412, 95 % CI 0.20, 0.85), compared to highly active adolescents with low milk consumption (OR 0.928, 95 % CI, 0.56, 1.53) [45].
Other metabolic syndrome factors, such as insulin resistance, increased blood glucose levels, and diabetes mellitus 2, have also been inversely associated with dairy consumption [46]. In a study with school children from low-income households in Buenos Aires, higher milk consumption was associated with higher levels of the insulin sensitivity marker, homeostatic model assessment (HOMA-IR), independently of other healthy-diet factors (β = −0.28, p = 0.026) [47]. However, one study of 8-year-old children compared the effect of milk and meat consumption on insulin resistance, and found a positive association between milk (but not meat) consumption and insulin concentration (103 %), insulin resistance (75 %), and C-reactive protein (26 %) [48]. Additionally, in 10- to 16-year-olds from 11 European countries, milk consumption was correlated with incidence of diabetes (r = 0.829; p = 0.042) [30]. The fat percentage of the milk might also matter; there is a hypothesis that the widespread increase in consumption of low-fat milk and decreased whole milk consumption could be related to an increased inflammation status [49].
Regarding blood pressure, three cohort studies–two in children and one in adolescents–showed an inverse association of dairy consumption with increased blood pressure [43, 50]. Yuan et al. (2013) showed that ≥2 servings per day of dairy products were associated with 1.74 mmHg (p < 0.005) and 0.87 mmHg (p = 0.010) lower systolic and diastolic blood pressure, respectively, in a fully-adjusted model. In their study, daily servings were defined according to the dairy product: milk, 250 ml; yogurt, 175 g; and cheese, 50 g. They excluded other dairy products, such as ice cream, cream, milkshakes, and combination dishes [50]. However, in school-aged children in Mexico, high intake of high-fat dairy (i.e., produced from whole milk) was associated with higher diastolic blood pressure (β = 8.76, 95 % CI 0.75, 2.5) and also with a higher level of HDL-cholesterol (β = 10.37, 95 % CI 0.21, 2.0) [36].
Fruits and vegetables
Many studies have described the beneficial protective association between fruits and vegetables consumption and the development of noncommunicable diseases in children [51]. Although fruits and vegetables are rich in fiber, vitamins, and polyphenols, which makes them a great food for prevention of obesity and other cardiovascular risk factors, many prospective and cross-sectional studies have found no association between fruits and vegetables consumption and childhood obesity [52]. In the last five years, however, some epidemiological and clinical studies [53] have demonstrated a strong protective association between fruits and vegetables consumption and general and abdominal obesity. In school children, fruits and vegetables consumption during school breaks was associated with lower BMI levels [54]. Another study, carried out in school children in the US, found that higher vegetable consumption was associated with 37 % lower odds of being overweight (95 % CI 0.48, 0.94) [35]. More than 3 daily servings of fruits and vegetables were shown to be inversely associated with central adiposity in children [55] and adolescents [56]. In Jamaican adolescents, higher waist circumference (WC) was associated with an absence of fruit consumption (OR 1.75 95 % CI 1.0, 3.0) [57]. The low energy density of fruits and vegetables may explain their protective effect against increased adiposity [58].
More than two servings of fruits and vegetables per day have been associated with reduced blood pressure [59, 60]. The association was even stronger when fruits and dairy products consumption were combined (systolic mean ± SE: 3.03 ± 0.23 (low fruits, vegetables and dairy consumption) vs 1.72 ± 0.45 (high fruits, vegetables and dairy consumption), diastolic mean ± SE: 0.66 ± 0.15 vs 0.25 ± 0.29) [60]. C-reactive protein, a non-specific marker of metabolic disorders and cardiovascular disease, was at the lowest level in children who consumed more vegetables (p = 0.0002) [61].
On the other hand, some studies found positive associations between fruits and vegetables consumption and cardiovascular risk factors such as diabetes [30], high glucose [36], obesity [62], central obesity [62], and metabolic risk factors [63]. This could be explained by underreporting of unhealthy foods or overestimation of foods that are perceived as socially desirable and healthy. There is also a hypothesis about the negative impact in Northern European children of increased consumption of tropical fruits, along with a decrease in apples and pears, on inflammation and incidence of type 1 diabetes, probably due to high fructose content [49].
Vitamins
There is a large gap in the literature on studies of vitamin consumption and the association with cardiovascular risk factors in children and adolescents. The majority of studies are about vitamin D, known to be a strong predictor of type 1diabetes. Other vitamins have received almost no attention from cardiovascular researchers. Therefore, we will necessarily focus on vitamin D and briefly discuss the effect of other vitamins, such as A, E, C, folate, B6 and B12.
Vitamin D
A recent meta-analysis of 12 cross-sectional studies of international databases showed that vitamin D is inversely associated with level of blood triglycerides (r = −0.135, 95 % CI−0.24, −0.03), total cholesterol (r = −0.086, 95 % CI–0.02, 0.04), and LDL-cholesterol (r = −0.025, 95 % CI–0.22, 0.17) and directly associated with HDL-cholesterol (r = 0.156, 95 % CI–0.02, 0.32) in children and adolescents and higher levels of vitamin D are associated with a better lipid profile in children [64]. Higher levels of serum vitamin D was associated with better glucose levels and lipid metabolism and lower general and abdominal adiposity levels, blood pressure, risk of metabolic syndrome, and pubertal development stage in children from different countries [65–74]. In a randomized trial with adolescents, high intake of vitamin D (4000 UI/day) was associated with decreased arterial stiffness, and low intake (200 UI/day) with increased stiffness, but this result was observed in only one of three measurements [75]. Although a recent systematic review showed a lack of consistent evidence for a protective effect of vitamin D against cardiovascular risk factors [76], studies of the association between vitamin D and glucose, diabetes, blood pressure and blood lipids showed inconsistent results.
Other vitamins
The information about consumption of other vitamins in children and adolescents and its association with cardiovascular risk factors is scarce. Increased consumption of carotenoids, vitamin C and E, was associated with decreased general and abdominal adiposity, impaired metabolism of glucose and lipids, and higher risk of metabolic syndrome [77–79].
There are also some findings regarding B vitamins and their favorable impact on cardiovascular health of children and adolescents. Vitamin B12 and folate were associated with decreased levels of homocysteine (β = −0.127 95 % CI −0.24, 0.01; β = −0.156 95 % CI–0.29,–0.03) and lower blood pressure in healthy children and adolescents from different countries [80–83].
Fiber
The effect of fiber intake on cardiovascular health of children and on non-communicable disease in general has not been well studied; even the recommended intake is still under debate [84, 85]. Fiber is a complex nutrient that includes many different compounds, and it has a very strong protective effect against obesity and other cardiovascular risk factors in adults. In light of the modern obesity epidemic among children and adolescents, more attention should be paid to this diet component. Children who eat a high-fiber breakfast have lower insulin resistance and fasting insulin levels in fully adjusted models; however, blood lipids and blood pressure were not affected [86]. In Latino children, higher intake of soluble fiber was associated with lower WC (β = 0.069, p = 0.036), and participants with no metabolic syndrome traits had significantly higher intake of soluble fiber, compared to children who had 3 metabolic syndrome traits (5.2 vs 4.1 g/day) [87]. In adolescents, total fiber intake was negatively associated with abdominal obesity (r = −0.224 for girls, p < 0.015;–0.272 for boys, p < 0.028) and inflammatory marker plasma C-reactive protein (r = −0.230 for girls,–0.308 for boys, p < 0.05) [88]. In adolescent girls, fiber intake was positively correlated with percentage of body fat (r = 0.22, p < 0.01), but this could be due to a high consciousness of healthy food choices among obese girls [89]. Another international study in adolescents showed a positive association of energy-adjusted fiber with percentage of body fat (β = 1.7 95 % CI 0.51, 2.9), waist to height ratio (β = 0.009 95 % CI 0.00, 0.02) and LDL-cholesterol (β = 0.031 95 % CI 0.00, 0.06), but at the same time soluble fiber was inversely associated with serum fasting glucose (β = −0.01 95 % CI −0.02, 0.00) [90].
Cereals and grains
Cereals and grains are the foundation of the plant-based diet, but there are considerably fewer studies about this food group in children and the results are rather consistent. In adolescents and US children, breakfast cereals intake was associated with significantly lower BMI (mean 20.7 vs 21.61, the highest tertile of cereals consumption vs no consumption, p < 0.05) and better diet quality; this finding was not dependent on sugar content [91]. In US children, consumption of ≥1.5 servings of grains per day was associated with 40 % lower risk of being obese, in comparison with the lowest quartile of grains consumption, even after adjustment for other dietary predictors such as dairy products, fruits, and vegetables [35, 92]. In US adolescents, higher consumption of whole grains was also associated with lower cardiovascular risk, based on factors such as lower levels of C-peptide (only in girls), fasting insulin, homocysteine (only in boys), higher levels of folates in serum and red blood cells [61, 93], and lower WC (mean of 7.50 vs 6.30 servings/day, WC < 85th percentile vs WC ≥ 85th percentile, p < 0.001)) [94]. In a French study, a significant inverse association between obesity and consumption of whole grains and cereals was found in adults, but not in children [95].
Meat
The impact of meat consumption on cardiovascular health is a subject of debate in both adult and pediatric populations. Study results are not consistent, as the quality and type of meat plays an important role and can change the direction of the association. In Iranian students aged 11 to 18 years, the frequency of red meat consumption was directly associated with dyslipidemia (β = 0.04 for total cholesterol, 0.04 for triglycerides,–0.05 for HDL-cholesterol, p < 0.05) [96]. In Finnish girls aged 6 to 8 years, the consumption of red meat was associated with higher metabolic risk score, but after adjustment for energy it was no longer significant (β = 0.09) [63]. Consumption of poultry, but not red or processed meat, was associated with higher homocysteine levels in adolescents (6.06 [5.8, 6.3] in the 5th quintile vs 5.55 [5.4, 5.8] in the 1st quintile, p for trend <0.001) [97]. In another study, US boys from the lowest quartile of central adiposity reported consuming less meat (p for trend = 0.025 for children and 0.047 for adolescents), but central adiposity was not related to higher meat consumption [94]. However, in a study of adolescent girls, higher consumption of lean meat was found to be protective against elevated levels of LDL-cholesterol and an unhealthy ratio of LDL to HDL cholesterol [98]. Surprisingly, in Mexican school-age children the consumption of red and processed meat was associated with lower glucose levels (β = −7.75, p = 0.02) [36], which could be due to selective food energy misreporting (i.e., self-reporting of energy consumption different from actual levels for particular food groups consumed).
Elevated BMI and weight satisfaction [99] are predictors of energy misreporting, which increases with age [100] and has been found to be a common issue among obese participants in a dietary survey [101]. In children, selective energy underreporting (a type of energy misreporting in which reported energy consumption is below the actual level for particular food groups) was associated with higher intake from fruits and vegetables, compared to plausible energy reporters [100].
Fast food, sugar-sweetened beverages
Several reviews discuss the issue of soft drink consumption and obesity development in children and adolescents, and most of the analyzed studies demonstrate the direct association between this risk factor and the health outcome [102]. Prospective studies revealed a direct association between sugar-sweetened beverages consumption in childhood and future obesity [103]. Studies in children and adolescents from different countries showed a direct association of soft drinks consumption with BMI, waist circumference (WC), overweight, general and abdominal obesity [39, 57, 104–108]. However, consumption of sugar-sweetened beverages was not associated with any obesity measurements in Spanish adolescents [109]. In a recent prospective study in Australian adolescents, increased consumption of sugar-sweetened beverages over time was associated with increased cardiometabolic risk score in girls (OR 3.2 95 % CI 1.6, 6.2), decreased level of HDL-cholesterol in boys and increased level of triglycerides, BMI and WC in both sexes [110]. In Finnish girls aged 6 to 8 years, soft drinks consumption was associated with a higher metabolic risk score (β = 0.11, p < 0.05) [63]. In a Mexican school-age population, higher consumption of sugar-sweetened beverages was associated with higher diastolic blood pressure (β = 6.01, p = 0.01) and glucose level (β = 7.10, p = 0.004) [36]. It is of interest that He et al. (2008) found an association between salt intake and soft drinks consumption in UK children; they showed that 50 % lower salt consumption (approximately 3 g/d less) was associated with a reduced intake of sweetened beverages by approximately 2.3 drinks per week [111].
With fast food, the findings are rather similar to the studies on soft drinks. In UK 13-year-olds, consumption of fast food was associated with increased BMI z-scores (β = 0.08, 95 % CI 0.03, 0.14), higher percentage of body fat (β = 2.06, 95 % CI 1.3, 2.8), and increased odds of obesity (OR 1.23, 95 % CI 1.0, 1.5) [112]. In Lebanese children, high consumption of fast food also was associated with 3 times increased risk of being overweight (95 % CI 1.2, 8.7) in comparison with low consumption [113]. However, Poti et al. (2014) studied the diet of US children and adolescents after excluding fast food from their analysis, and discovered that the Western diet is probably more responsible for the association with overweight and obesity than the fast food consumption itself (β = 5.9, 95 % CI 1.3, 10.5) [114]. Sugar-sweetened beverages, fast food, and various cardiovascular risk factors have been the focus of other studies, most of them with similar results and association trends that show a negative impact on cardiovascular health. These food items are also widely studied within the framework of dietary patterns, particularly the Western dietary pattern, defined by post-hoc analysis.
Dietary patterns
Post-hoc dietary patterns
Many studies in children and adolescents from different countries have analyzed the association of dietary patterns with cardiovascular risk factors. The main dietary patterns derived in those studies are Western or Unhealthy patterns (normally characterized by higher consumption of red meat, meat derivatives, sweets, pastries, fast food, sugar-sweetened beverages, fried foods, and snacks) and Healthy or Traditional patterns (usually distinguished by increased intake of plant-based foods and fish). A majority of these studies showed positive associations between the Western dietary patterns and cardiovascular risk factors, such as obesity and increased triglycerides, and between the Traditional pattern and a healthier cardiovascular profile [115]. However, not all Traditional dietary patterns are associated with better health. Joung et al. (2012) showed that the traditional Korean “Rice & Kimchi” pattern was associated with increased triglycerides and decreased HDL-cholesterol in comparison with other dietary patterns, such as “Noodle & Mushroom” and “Bread & Meat & Fruit & Milk” [115]. Many studies analyzed the association of dietary patterns with adiposity, and confirmed a positive association of a Western dietary pattern and an inverse association of a Healthy dietary pattern with general and abdominal adiposity [114, 116–126]. However, in Scottish children and adolescents, no association was established between healthy or unhealthy patterns and obesity [127].
Other cardiovascular risk factors have also been widely studied. In Mexican [128] and Greek [129] children, analogs of the Western pattern were associated with insulin resistance, with 1.92 and 2.51 higher odds than in the Healthy pattern, respectively. Several studies have paid special attention to metabolic syndrome in children. In Australian and Korean children, the Western dietary pattern in girls was associated with increased risk of metabolic syndrome, and the Healthy pattern was associated with improved glucose and lipid metabolism [118, 130]. In Ecuadorian adolescents, two patterns emerged: “rice-rich non-animal fat pattern” and “wheat-dense animal-fat pattern”, both of them were associated with several cardiovascular risk factors. The first was associated with increased glucose levels in urban adolescents (p for trend < 0.01) and the latter with increased levels of total (p for trend 0.02) and LDL-cholesterol (p for trend 0.04) among rural participants [131].
A priori dietary patterns
Significantly fewer studies have used a dietary index, compared to post-hoc dietary patterns. A fairly recent review by Lazarou and Newby (2011) found only 38 studies published through mid-2010 that analyzed the diet-disease relationship using a dietary index in children and adolescents of developed countries [132]. Most of those studies (22, or 57.9 %) were looking at the association between the index scores and anthropometric measurements; only 13 of the studies found a small but statistically significant inverse association between the index values and BMI; almost half of the papers analyzing health outcomes showed an association with such cardiovascular risk factors as high blood pressure, blood lipids, and inflammation markers. It is important to highlight that all studies using a dietary index had a cross-sectional design. In UK children, better scores on a Diet Quality Index and Healthy Diet Indicator were associated with lower body fat (−5.1 %, p = 0.023 and–4.9 %, p = 0.026, between 1st and 5th quintiles, respectively) and WC (−3.0 %, p = 0.005 and–2.5 %, p = 0.033, respectively) and other surrogate obesity markers; this was not the case for the Mediterranean Diet Score [133]. However, in an Australian study that validated the Dietary Guideline Index for Children and Adolescents, this index showed a weak but positive association with BMI Z-scores (β = 1.13 95 % CI 0.32, 2.0 for 4-to 7-year-olds and β = 1.12 95 % CI 0.42, 1.8 for 16- to 18-year-olds) [134].
Vegetarian diet and mediterranean diet
Few studies have considered a vegetarian diet and the health of children and adolescents. Sabate and Wien (2010) showed that most of the available studies were carried out in the Seventh Day Adventist population, in which a large percentage of people follow plant-based dietary patterns, ranging from vegetarians, who consume dairy foods and eggs, to vegans, who avoid all animal products. Results showed that vegetarian children and adolescents have lower BMI, WC, and LDL-cholesterol and higher HDL-cholesterol [135]. However, not all studies showed a clear inverse association of obesity with cardiovascular risk factors, and some of them did not reach statistical significance in the association with a plant-based diet, but they found a direct inverse association between animal products consumption and the health outcomes studied. It is important to note that in many studies the vegetarian diet was inversely associated with obesity surrogate markers, independently of physical activity. Robinson-O’Brien et al. (2009) also confirmed that vegetarian adolescents, but not children, were less obese (p < 0.007) or overweight (p < 0.044) than non-vegetarians, but at the same time, extremely unhealthful weight-control behavior (p < 0.001) and binge eating (p < 0.001) was more popular among vegetarian adolescents than among their non-vegetarian peers [136].
More studies of the diet-disease relationship have analyzed the Mediterranean diet, another traditional plant-based dietary pattern, than vegetarian diet (s). One study in children showed an inverse association between adherence to the Mediterranean diet, measured by the KIDMED index, and arterial stiffness, which is an indicator of higher risk of developing cardiovascular diseases (β = −0.114, p = 0.026) [137]. In the Mediterranean adolescent population in Balearic Islands, higher adherence to the Mediterranean diet was associated with decreased prevalence of metabolic syndrome and the associated risk factors. However, it was also associated with lower levels of HDL-cholesterol in girls (OR 0.25, 95 % CI 0.05, 0.27, first vs last quartiles) [138]. In an international study in European children, a high food-frequency-based Mediterranean Diet Score (fMDS) was associated with lower risk of overweight/obesity (OR 0.85, 95 % CI 0.77, 0.94, lower fMDS vs higher fMDS) and percentage of fat mass (β = −0.22, 95 % CI–0.43,–0.01) independently of physical activity. Furthermore, the fMDS was associated with lower levels of obesity surrogate markers (BMI, WC and waist-to-height ratio) in prospective analysis [139]. Surprisingly, high adherence to the Mediterranean diet was associated with higher salt intake. Every unit increase in the KIDMED index was associated with 10 % increase of sodium intake above the median, >1500 mg/day (95 % CI 1.1, 1.1). The authors clarify that the main source of salt was bread, cheese, and breakfast cereals, which form part of the traditional Mediterranean diet [140]. Other studies found no prospective or cross-sectional association between Mediterranean diet score and cardiovascular risk factors in children [141, 142]. In a non-Mediterranean (UK) population of children, the Mediterranean Diet Score showed no association with obesity or overweight [133]. The few available studies about Mediterranean and vegetarian diets in children and adolescents highlight the favorable and promising role of plant food based dietary patterns, as a complex of healthy food choices, in prevention of cardiovascular risk factors in this population.
Conclusion
Although most of the studies in children have shown results similar to the analogous studies in adults, many topics studied in adults have not been addressed in children. Vitamins (except vitamin D), polyphenols, and fiber are areas for future development of nutrients research. Food groups such as dairy, fast food, and soft drinks have been studied more extensively than others, but even in these groups, the results are inconsistent. Dietary patterns are a relatively new topic of research, with very few studies in children, both a priori and a posteriori. A special gap exists in studies of a priori dietary patterns - very little research has been done on vegetarian diets, the Mediterranean diet, and dietary indexes. Underreporting of foods perceived as unhealthy and overreporting of those perceived as healthy is another problem that results in errors in the analysis of associations between cardiovascular risk factors and foods such as fruits and vegetables. This topic is still not very clearly understood in the adult population, and is even less studied in children. Future studies should focus on the diet’s mechanism of action and on establishing recommendations for healthy dietary habits in children, taking into account age, ethnicity, and health status. Additionally, there is a clear need for interventional studies, not only related to childhood obesity, which is already well developed, but focused on other cardiovascular risk factors as well.
Abbreviations
- 25 (OH) D:
-
25-hydroxy vitamin D test
- Apo-A1:
-
apolipoprotein A1
- Apo-B:
-
apolipoprotein B
- BMI:
-
body mass index
- FMDS:
-
food-frequency-based mediterranean diet score
- HDL:
-
high-density lipoprotein
- HELENA:
-
healthy lifestyle in Europe by nutrition in adolescence
- HOMA-IR:
-
homeostatic model assessment
- IMT:
-
intimal-medical thickness
- LDL:
-
low-density lipoprotein cholesterol
- PREDIMED:
-
prevention with mediterranean diet
- PUFA:
-
polyunsaturated fatty acid
- WC:
-
waist circumference
References
Berenson GS. Cardiovascular risk begins in childhood: a time for action. Am J Prev Med. 2009;37(1 Suppl):S1–2.
Baker JL, Olsen LW, Sorensen TI. Childhood body-mass index and the risk of coronary heart disease in adulthood. N Engl J Med. 2007;357(23):2329–37.
Camhi SM, Katzmarzyk PT, Broyles S, Srinivasan SR, Chen W, Bouchard C, et al. Predicting adult body mass index-specific metabolic risk from childhood. Metab Syndr Relat Disord. 2010;8(2):165–72.
Tonstad S, Joakimsen O, Stensland-Bugge E, Leren TP, Ose L, Russell D, et al. Risk factors related to carotid intima-media thickness and plaque in children with familial hypercholesterolemia and control subjects. Arterioscler Thromb Vasc Biol. 1996;16(8):984–91.
De Jongh S, Lilien MR, Op’t Roodt J, Stroes ES, Bakker HD, Kastelein JJ. Early statin therapy restores endothelial function in children with familial hypercholesterolemia. J Am Coll Cardiol. 2002;40(12):2117–21.
Sorof JM, Alexandrov AV, Cardwell G, Portman RJ. Carotid artery intimal-medial thickness and left ventricular hypertrophy in children with elevated blood pressure. Pediatrics. 2003;111(1):61–6.
Juhola J, Magnussen CG, Viikari JS, Kahonen M, Hutri-Kahonen N, Jula A, et al. Tracking of serum lipid levels, blood pressure, and body mass index from childhood to adulthood: the Cardiovascular Risk in Young Finns Study. J Pediatr. 2011;159(4):584–90.
Juhola J, Magnussen CG, Berenson GS, Venn A, Burns TL, Sabin MA, et al. Combined effects of child and adult elevated blood pressure on subclinical atherosclerosis: the International Childhood Cardiovascular Cohort Consortium. Circulation. 2013;128(3):217–24.
Raitakari OT, Juonala M, Kahonen M, Taittonen L, Laitinen T, Maki-Torkko N, et al. Cardiovascular risk factors in childhood and carotid artery intima-media thickness in adulthood: the Cardiovascular Risk in Young Finns Study. JAMA. 2003;290(17):2277–83.
Raitakari OT, Juonala M, Viikari JS. Obesity in childhood and vascular changes in adulthood: insights into the Cardiovascular Risk in Young Finns Study. Int J Obes. 2005;29 Suppl 2:S101–4.
Davis PH, Dawson JD, Riley WA, Lauer RM. Carotid intimal-medial thickness is related to cardiovascular risk factors measured from childhood through middle age: The Muscatine Study. Circulation. 2001;104(23):2815–9.
Li S, Chen W, Srinivasan SR, Bond MG, Tang R, Urbina EM, et al. Childhood cardiovascular risk factors and carotid vascular changes in adulthood: the Bogalusa Heart Study. JAMA. 2003;290(17):2271–6.
Friedemann C, Heneghan C, Mahtani K, Thompson M, Perera R, Ward AM. Cardiovascular disease risk in healthy children and its association with body mass index: systematic review and meta-analysis. BMJ. 2012;345:e4759.
Juonala M, Magnussen CG, Berenson GS, Venn A, Burns TL, Sabin MA, et al. Childhood adiposity, adult adiposity, and cardiovascular risk factors. N Engl J Med. 2011;365(20):1876–85.
Mente A, De Koning L, Shannon HS, Anand SS. A systematic review of the evidence supporting a causal link between dietary factors and coronary heart disease. Arch Intern Med. 2009;169(7):659–69.
Schroder H, Salas-Salvado J, Martinez-Gonzalez MA, Fito M, Corella D, Estruch R, et al. Baseline adherence to the Mediterranean diet and major cardiovascular events: Prevencion con Dieta Mediterranea trial. JAMA. 2014;174(10):1690–2.
Estruch R, Ros E, Salas-Salvado J, Covas MI, Corella D, Aros F, et al. Primary prevention of cardiovascular disease with a Mediterranean diet. N Engl J Med. 2013;368(14):1279–90.
Lava SA, Bianchetti MG, Simonetti GD. Salt intake in children and its consequences on blood pressure. Berlin, Germany: Pediatric nephrology; 2014.
He FJ, MacGregor GA. Importance of salt in determining blood pressure in children: meta-analysis of controlled trials. Hypertension. 2006;48(5):861–9.
Shi L, Krupp D, Remer T. Salt, fruit and vegetable consumption and blood pressure development: a longitudinal investigation in healthy children. Br J Nutr. 2014;111(4):662–71.
Yang Q, Zhang Z, Kuklina EV, Fang J, Ayala C, Hong Y, et al. Sodium intake and blood pressure among US children and adolescents. Pediatrics. 2012;130(4):611–9.
Rosner B, Cook NR, Daniels S, Falkner B. Childhood blood pressure trends and risk factors for high blood pressure: the NHANES experience 1988–2008. Hypertension. 2013;62(2):247–54.
Vitolo MR, Da Costa Louzada ML, Rauber F, Campagnolo PD. Risk factors for high blood pressure in low income children aged 3–4 years. Eur J Pediatr. 2013;172(8):1097–103.
Brion MJ, Ness AR, Davey Smith G, Emmett P, Rogers I, Whincup P, et al. Sodium intake in infancy and blood pressure at 7 years: findings from the Avon Longitudinal Study of Parents and Children. Eur J Clin Nutr. 2008;62(10):1162–9.
Kelishadi R, Gheisari A, Zare N, Farajian S, Shariatinejad K. Salt intake and the association with blood pressure in young Iranian children: first report from the middle East and north Africa. Int J Prev Med. 2013;4(4):475–83.
McGloin AF, Livingstone MB, Greene LC, Webb SE, Gibson JM, Jebb SA, et al. Energy and fat intake in obese and lean children at varying risk of obesity. Int J Obes Relat Metab Disord. 2002;26(2):200–7.
Ailhaud G, Guesnet P. Fatty acid composition of fats is an early determinant of childhood obesity: a short review and an opinion. Obes Rev. 2004;5(1):21–6.
Nicklas TA, Dwyer J, Feldman HA, Luepker RV, Kelder SH, Nader PR. Serum cholesterol levels in children are associated with dietary fat and fatty acid intake. J Am Diet Assoc. 2002;102(4):511–7.
Cheng HH, Wen YY, Chen C. Serum fatty acid composition in primary school children is associated with serum cholesterol levels and dietary fat intake. Eur J Clin Nutr. 2003;57(12):1613–20.
Thorsdottir I, Ramel A. Dietary intake of 10- to 16-year-old children and adolescents in central and northern Europe and association with the incidence of type 1 diabetes. Ann Nutr Metab. 2003;47(6):267–75.
Romeo J, Warnberg J, Garcia-Marmol E, Rodriguez-Rodriguez M, Diaz LE, Gomez-Martinez S, et al. Daily consumption of milk enriched with fish oil, oleic acid, minerals and vitamins reduces cell adhesion molecules in healthy children. Nutr Metab Cardiovasc Dis. 2011;21(2):113–20.
Hoppu U, Isolauri E, Koskinen P, Laitinen K. Diet and blood lipids in 1–4 year-old children. Nutr Metab Cardiovasc Dis. 2013;23(10):980–6.
Haro-Mora JJ, Garcia-Escobar E, Porras N, Alcazar D, Gaztambide J, Ruiz-Orpez A, et al. Children whose diet contained olive oil had a lower likelihood of increasing their body mass index Z-score over 1 year. Eur J Endocrinol. 2011;165(3):435–9.
O’Neil CE, Keast DR, Nicklas TA, Fulgoni VL. 3rd: Out-of-hand nut consumption is associated with improved nutrient intake and health risk markers in US children and adults: National Health and Nutrition Examination Survey 1999–2004. Nutr Res. 2012;32(3):185–94.
Matthews VL, Wien M, Sabate J. The risk of child and adolescent overweight is related to types of food consumed. Nutr J. 2011;10:71.
Perichart-Perera O, Balas-Nakash M, Rodriguez-Cano A, Munoz-Manrique C, Monge-Urrea A, Vadillo-Ortega F. Correlates of dietary energy sources with cardiovascular disease risk markers in Mexican school-age children. J Am Diet Assoc. 2010;110(2):253–60.
Bigornia SJ, LaValley MP, Moore LL, Northstone K, Emmett P, Ness AR, et al. Dairy intakes at age 10 years do not adversely affect risk of excess adiposity at 13 years. J Nutr. 2014;144(7):1081–90.
Hasnain SR, Singer MR, Bradlee ML, Moore LL. Beverage intake in early childhood and change in body fat from preschool to adolescence. Child Obes. 2014;10(1):42–9.
Beck AL, Tschann J, Butte NF, Penilla C, Greenspan LC. Association of beverage consumption with obesity in Mexican American children. Public Health Nutr. 2014;17(2):338–44.
Scharf RJ, Demmer RT, DeBoer MD. Longitudinal evaluation of milk type consumed and weight status in preschoolers. Arch Dis Child. 2013;98(5):335–40.
Dixon LB, Pellizzon MA, Jawad AF, Tershakovec AM. Calcium and dairy intake and measures of obesity in hyper-and normocholesterolemic children. Obes Res. 2005;13(10):1727–38.
Wiley AS. Dairy and milk consumption and child growth: Is BMI involved? An analysis of NHANES 1999–2004. Am J Hum Biol. 2010;22(4):517–25.
Dror DK, Allen LH. Dairy product intake in children and adolescents in developed countries: trends, nutritional contribution, and a review of association with health outcomes. Nutr Rev. 2014;72(2):68–81.
Lin SL, Tarrant M, Hui LL, Kwok MK, Lam TH, Leung GM, et al. The role of dairy products and milk in adolescent obesity: evidence from Hong Kong’s “Children of 1997” birth cohort. PLoS One. 2012;7(12):e52575.
Abreu S, Santos R, Moreira C, Santos PC, Vale S, Soares-Miranda L, et al. Relationship of milk intake and physical activity to abdominal obesity among adolescents. Pediatr Obes. 2014;9(1):71–80.
Huang TT, McCrory MA. Dairy intake, obesity, and metabolic health in children and adolescents: knowledge and gaps. Nutr Rev. 2005;63(3):71–80.
Hirschler V, Oestreicher K, Beccaria M, Hidalgo M, Maccallini G. Inverse association between insulin resistance and frequency of milk consumption in low-income Argentinean school children. J Pediatr. 2009;154(1):101–5.
Hoppe C, Molgaard C, Vaag A, Barkholt V, Michaelsen KF. High intakes of milk, but not meat, increase s-insulin and insulin resistance in 8-year-old boys. Eur J Clin Nutr. 2005;59(3):393–8.
Landin-Olsson M, Hillman M, Erlanson-Albertsson C. Is type 1 diabetes a food-induced disease? Med Hypotheses. 2013;81(2):338–42.
Yuan WL, Kakinami L, Gray-Donald K, Czernichow S, Lambert M, Paradis G. Influence of dairy product consumption on children’s blood pressure: results from the QUALITY cohort. J Acad Nutr Diet. 2013;113(7):936–41.
Musaiger AO, Al-Hazzaa HM. Prevalence and risk factors associated with nutrition-related noncommunicable diseases in the Eastern Mediterranean region. Int J Gen Med. 2012;5:199–217.
Newby PK. Plant foods and plant-based diets: protective against childhood obesity? Am J Clin Nutr. 2009;89(5):1572s–87s.
Silveira JA, Taddei JA, Guerra PH, Nobre MR. Effectiveness of school-based nutrition education interventions to prevent and reduce excessive weight gain in children and adolescents: a systematic review. J Pediatr. 2011;87(5):382–92.
Abril V, Manuel-y-keenoy B, Sola R, Garcia JL, Nessier C, Rojas R, et al. Prevalence of overweight and obesity among 6-to 9-year-old school children in Cuenca, Ecuador: relationship with physical activity, poverty, and eating habits. Food Nutr Bull. 2013;34(4):388–401.
Downs SM, Marshall D, Ng C, Willows ND. Central adiposity and associated lifestyle factors in Cree children. Appl Physiol Nutr Metab. 2008;33(3):476–82.
Al-Hazzaa HM, Abahussain NA, Al-Sobayel HI, Qahwaji DM, Musaiger AO. Lifestyle factors associated with overweight and obesity among Saudi adolescents. BMC Public Health. 2012;12:354.
Francis DK, Van den Broeck J, Younger N, McFarlane S, Rudder K, Gordon-Strachan G, et al. Fast-food and sweetened beverage consumption: association with overweight and high waist circumference in adolescents. Public Health Nutr. 2009;12(8):1106–14.
Vernarelli JA, Mitchell DC, Hartman TJ, Rolls BJ. Dietary energy density is associated with body weight status and vegetable intake in U.S. children. J Nutr. 2011;141(12):2204–10.
Damasceno MM, De Araujo MF, De Freitas RW, De Almeida PC, Zanetti ML. The association between blood pressure in adolescents and the consumption of fruits, vegetables and fruit juice--an exploratory study. J Clin Nurs. 2011;20(11–12):1553–60.
Moore LL, Singer MR, Bradlee ML, Djousse L, Proctor MH, Cupples LA, et al. Intake of fruits, vegetables, and dairy products in early childhood and subsequent blood pressure change. Epidemiol. 2005;16(1):4–11.
Qureshi MM, Singer MR, Moore LL. A cross-sectional study of food group intake and C-reactive protein among children. Nutr Metab. 2009;6:40.
Abreu S, Santos R, Moreira C, Santos PC, Mota J, Moreira P. Food consumption, physical activity and socio-economic status related to BMI, waist circumference and waist-to-height ratio in adolescents. Public Health Nutr. 2014;17(8):1834–49.
Eloranta AM, Lindi V, Schwab U, Kiiskinen S, Venalainen T, Lakka HM, et al. Dietary factors associated with metabolic risk score in Finnish children aged 6–8 years: the PANIC study. Eur J Nutr. 2014;53(6):1431–9.
Kelishadi R, Farajzadegan Z, Bahreynian M. Association between vitamin D status and lipid profile in children and adolescents: a systematic review and meta-analysis. Int J Food Sci Nutr. 2014;65(4):404–10.
Aypak C, Turedi O, Yuce A. The association of vitamin D status with cardiometabolic risk factors, obesity and puberty in children. Eur J Pediatr. 2014;173(3):367–73.
Hirschler V, Maccallini G, Molinari C, Ines U, Castano LA, Sanchez M, et al. Association between vitamin D and Apo B concentrations in Argentinean Indian children. Clin Chim Acta. 2014;429:147–51.
Ha CD, Cho JK, Lee SH, Kang HS. Serum vitamin D, physical activity, and metabolic risk factors in Korean children. Med Sci Sports Exerc. 2013;45(1):102–8.
Lee SH, Kim SM, Park HS, Choi KM, Cho GJ, Ko BJ, et al. Serum 25-hydroxyvitamin D levels, obesity and the metabolic syndrome among Korean children. Nutr Metab Cardiovasc Dis. 2013;23(8):785–91.
Choi DP, Oh SM, Lee JM, Cho HM, Lee WJ, Song BM, et al. Serum 25-hydroxyvitamin D and insulin resistance in apparently healthy adolescents. PLoS One. 2014;9(7):e103108.
Chung SJ, Lee YA, Hong H, Kang MJ, Kwon HJ, Shin CH, et al. Inverse relationship between vitamin D status and insulin resistance and the risk of impaired fasting glucose in Korean children and adolescents: the Korean National Health and Nutrition Examination Survey (KNHANES) 2009–2010. Public Health Nutr. 2014;17(4):795–802.
Kelly A, Brooks LJ, Dougherty S, Carlow DC, Zemel BS. A cross-sectional study of vitamin D and insulin resistance in children. Arch Dis Child. 2011;96(5):447–52.
Parikh S, Guo DH, Pollock NK, Petty K, Bhagatwala J, Gutin B, et al. Circulating 25-hydroxyvitamin D concentrations are correlated with cardiometabolic risk among American black and white adolescents living in a year-round sunny climate. Diabetes Care. 2012;35(5):1133–8.
Moreira C, Moreira P, Abreu S, Santos PC, Moreira-Silva I, Povoas S, et al. Vitamin D intake and cardiometabolic risk factors in adolescents. Metab Syndr Relat Disord. 2014;12(3):171–7.
Oliveira RM, Novaes JF, Azeredo LM, Candido AP, Leite IC. Association of vitamin D insufficiency with adiposity and metabolic disorders in Brazilian adolescents. Public Health Nutr. 2014;17(4):787–94.
Dong Y, Stallmann-Jorgensen IS, Pollock NK, Harris RA, Keeton D, Huang Y, et al. A 16-week randomized clinical trial of 2000 international units daily vitamin D3 supplementation in black youth: 25-hydroxyvitamin D, adiposity, and arterial stiffness. J Clin Endocrinol Metab. 2010;95(10):4584–91.
Dolinsky DH, Armstrong S, Mangarelli C, Kemper AR. The association between vitamin D and cardiometabolic risk factors in children: a systematic review. Clin Pediatr. 2013;52(3):210–23.
Gunanti IR, Marks GC, Al-Mamun A, Long KZ. Low serum concentrations of carotenoids and vitamin E are associated with high adiposity in Mexican-American children. J Nutr. 2014;144(4):489–95.
Beydoun MA, Canas JA, Beydoun HA, Chen X, Shroff MR, Zonderman AB. Serum antioxidant concentrations and metabolic syndrome are associated among U.S. adolescents in recent national surveys. J Nutr. 2012;142(9):1693–704.
Garcia OP, Ronquillo D, Del Carmen CM, Martinez G, Camacho M, Lopez V, et al. Zinc, iron and vitamins A, C and e are associated with obesity, inflammation, lipid profile and insulin resistance in Mexican school-aged children. Nutr. 2013;5(12):5012–30.
Brasileiro RS, Escrivao MA, Taddei JA, D’Almeida V, Ancona-Lopez F, Carvalhaes JT. Plasma total homocysteine in Brazilian overweight and non-overweight adolescents: a case–control study. Nutr Hosp. 2005;20(5):313–9.
Shen MH, Chu NF, Wu DM, Chang JB. Plasma homocyst (e) ine, folate and vitamin B (12) levels among school children in Taiwan: The Taipei Children Heart Study. Clin Biochem. 2002;35(6):495–8.
De Moraes AC, Gracia-Marco L, Iglesia I, Gonzalez-Gross M, Breidenassel C, Ferrari M, et al. Vitamins and iron blood biomarkers are associated with blood pressure levels in European adolescents. The HELENA study. Nutr. 2014;30(11–12):1294–300.
Tamai Y, Wada K, Tsuji M, Nakamura K, Sahashi Y, Watanabe K, et al. Dietary intake of vitamin B12 and folic acid is associated with lower blood pressure in Japanese preschool children. Am J Hypertens. 2011;24(11):1215–21.
Niinikoski H, Ruottinen S. Is carbohydrate intake in the first years of life related to future risk of NCDs? Nutr Metab Cardiovasc Dis. 2012;22(10):770–4.
Edwards CA, Parrett AM. Dietary fibre in infancy and childhood. Proc Nutr Soc. 2003;62(1):17–23.
Donin AS, Nightingale CM, Owen CG, Rudnicka AR, Perkin MR, Jebb SA, et al. Regular breakfast consumption and type 2 diabetes risk markers in 9-to 10-year-old children in the child heart and health study in England (CHASE): a cross-sectional analysis. PLoS Med. 2014;11(9):e1001703.
Ventura EE, Davis JN, Alexander KE, Shaibi GQ, Lee W, Byrd-Williams CE, et al. Dietary intake and the metabolic syndrome in overweight Latino children. J Am Diet Assoc. 2008;108(8):1355–9.
Parikh S, Pollock NK, Bhagatwala J, Guo DH, Gutin B, Zhu H, et al. Adolescent fiber consumption is associated with visceral fat and inflammatory markers. J Clin Endocrinol Metab. 2012;97(8):E1451–7.
Vagstrand K, Barkeling B, Forslund HB, Elfhag K, Linne Y, Rossner S, et al. Eating habits in relation to body fatness and gender in adolescents--results from the ‘SWEDES’ study. Eur J Clin Nutr. 2007;61(4):517–25.
Lin Y, Huybrechts I, Vereecken C, Mouratidou T, Valtuena J, Kersting M, et al. Dietary fiber intake and its association with indicators of adiposity and serum biomarkers in European adolescents: the HELENA study. Eur J Nutr. 2014.
Albertson AM, Thompson DR, Franko DL, Holschuh NM. Weight indicators and nutrient intake in children and adolescents do not vary by sugar content in ready-to-eat cereal: results from National Health and Nutrition Examination Survey 2001–2006. Nutr Res. 2011;31(3):229–36.
Choumenkovitch SF, McKeown NM, Tovar A, Hyatt RR, Kraak VI, Hastings AV, et al. Whole grain consumption is inversely associated with BMI Z-score in rural school-aged children. Public Health Nutr. 2013;16(2):212–8.
Hur IY, Reicks M. Relationship between whole-grain intake, chronic disease risk indicators, and weight status among adolescents in the National Health and Nutrition Examination Survey, 1999–2004. J Acad Nutr Diet. 2012;112(1):46–55.
Bradlee ML, Singer MR, Qureshi MM, Moore LL. Food group intake and central obesity among children and adolescents in the Third National Health and Nutrition Examination Survey (NHANES III). Public Health Nutr. 2010;13(6):797–805.
Bellisle F, Hebel P, Colin J, Reye B, Hopkins S. Consumption of whole grains in French children, adolescents and adults. Br J Nutr. 2014;1–11.
Kelishadi R, Pour MH, Zadegan NS, Kahbazi M, Sadry G, Amani A, et al. Dietary fat intake and lipid profiles of Iranian adolescents: Isfahan Healthy Heart Program--Heart Health Promotion from Childhood. Prev Med. 2004;39(4):760–6.
Lutsey PL, Steffen LM, Feldman HA, Hoelscher DH, Webber LS, Luepker RV, et al. Serum homocysteine is related to food intake in adolescents: the Child and Adolescent Trial for Cardiovascular Health. Am J Clin Nutr. 2006;83(6):1380–6.
Bradlee ML, Singer MR, Moore LL. Lean red meat consumption and lipid profiles in adolescent girls. J Hum Nutr Diet. 2014;27 Suppl 2:292–300.
Farajian P, Bountziouka V, Risvas G, Panagiotakos DB, Zampelas A. Anthropometric, lifestyle and parental characteristics associated with the prevalence of energy intake misreporting in children: the GRECO (Greek Childhood Obesity) study. Br J Nutr. 2015;113(7):1120–8.
Bornhorst C, Huybrechts I, Ahrens W, Eiben G, Michels N, Pala V, et al. Prevalence and determinants of misreporting among European children in proxy-reported 24 h dietary recalls. Br J Nutr. 2013;109(7):1257–65.
Rosell MS, Hellenius ML, De Faire UH, Johansson GK. Associations between diet and the metabolic syndrome vary with the validity of dietary intake data. Am J Clin Nutr. 2003;78(1):84–90.
Morgan RE. Does consumption of high-fructose corn syrup beverages cause obesity in children? Pediatr Obes. 2013;8(4):249–54.
Perez-Morales E, Bacardi-Gascon M, Jimenez-Cruz A. Sugar-sweetened beverage intake before 6 years of age and weight or BMI status among older children; systematic review of prospective studies. Nutr Hosp. 2013;28(1):47–51.
Collison KS, Zaidi MZ, Subhani SN, Al-Rubeaan K, Shoukri M, Al-Mohanna FA. Sugar-sweetened carbonated beverage consumption correlates with BMI, waist circumference, and poor dietary choices in school children. BMC Public Health. 2010;10:234.
Linardakis M, Sarri K, Pateraki MS, Sbokos M, Kafatos A. Sugar-added beverages consumption among kindergarten children of Crete: effects on nutritional status and risk of obesity. BMC Public Health. 2008;8:279.
Gibson S, Neate D. Sugar intake, soft drink consumption and body weight among British children: further analysis of National Diet and Nutrition Survey data with adjustment for under-reporting and physical activity. Int J Food Sci Nutr. 2007;58(6):445–60.
Li M, Dibley MJ, Sibbritt DW, Yan H. Dietary habits and overweight/obesity in adolescents in Xi’an City, China. Asia Pac J Clin Nutr. 2010;19(1):76–82.
Papandreou D, Andreou E, Heraclides A, Rousso I. Is beverage intake related to overweight and obesity in school children? Hippokratia. 2013;17(1):42–6.
Gomez-Martinez S, Martin A, Romeo J, Castillo M, Mesena M, Baraza JC, et al. Is soft drink consumption associated with body composition? A cross-sectional study in Spanish adolescents. Nutr Hosp. 2009;24(1):97–102.
Ambrosini GL, Oddy WH, Huang RC, Mori TA, Beilin LJ, Jebb SA. Prospective associations between sugar-sweetened beverage intakes and cardiometabolic risk factors in adolescents. Am J Clin Nutr. 2013;98(2):327–34.
He FJ, Marrero NM, MacGregor GA. Salt intake is related to soft drink consumption in children and adolescents: a link to obesity? Hypertension. 2008;51(3):629–34.
Fraser LK, Clarke GP, Cade JE, Edwards KL. Fast food and obesity: a spatial analysis in a large United Kingdom population of children aged 13–15. Am J Prev Med. 2012;42(5):e77–85.
Nasreddine L, Naja F, Akl C, Chamieh MC, Karam S, Sibai AM, et al. Dietary, lifestyle and socio-economic correlates of overweight, obesity and central adiposity in Lebanese children and adolescents. Nutr. 2014;6(3):1038–62.
Poti JM, Duffey KJ, Popkin BM. The association of fast food consumption with poor dietary outcomes and obesity among children: is it the fast food or the remainder of the diet? Am J Clin Nutr. 2014;99(1):162–71.
Joung H, Hong S, Song Y, Ahn BC, Park MJ. Dietary patterns and metabolic syndrome risk factors among adolescents. Korean J Pediatr. 2012;55(4):128–35.
Pala V, Lissner L, Hebestreit A, Lanfer A, Sieri S, Siani A, et al. Dietary patterns and longitudinal change in body mass in European children: a follow-up study on the IDEFICS multicenter cohort. Eur J Clin Nutr. 2013;67(10):1042–9.
Shroff MR, Perng W, Baylin A, Mora-Plazas M, Marin C, Villamor E. Adherence to a snacking dietary pattern and soda intake are related to the development of adiposity: a prospective study in school-age children. Public Health Nutr. 2014;17(7):1507–13.
Ambrosini GL, Huang RC, Mori TA, Hands BP, O’Sullivan TA, De Klerk NH, et al. Dietary patterns and markers for the metabolic syndrome in Australian adolescents. Nutr Metab Cardiovasc Dis. 2010;20(4):274–83.
Howe AS, Black KE, Wong JE, Parnell WR, Skidmore PM. Dieting status influences associations between dietary patterns and body composition in adolescents: a cross-sectional study. Nutr J. 2013;12:51.
Cutler GJ, Flood A, Hannan PJ, Slavin JL, Neumark-Sztainer D. Association between major patterns of dietary intake and weight status in adolescents. Br J Nutr. 2012;108(2):349–56.
Smith AD, Emmett PM, Newby PK, Northstone K. Dietary patterns and changes in body composition in children between 9 and 11 years. Food Nutr Res. 2014;58.
Rodriguez-Ramirez S, Mundo-Rosas V, Garcia-Guerra A, Shamah-Levy T. Dietary patterns are associated with overweight and obesity in Mexican school-age children. Arch Latinoam Nutr. 2011;61(3):270–8.
Shang L, O’Loughlin J, Tremblay A, Gray-Donald K. The association between food patterns and adiposity among Canadian children at risk of overweight. Appl Physiol Nutr Metab. 2014;39(2):195–201.
Manios Y, Kourlaba G, Grammatikaki E, Androutsos O, Ioannou E, Roma-Giannikou E. Comparison of two methods for identifying dietary patterns associated with obesity in preschool children: the GENESIS study. Eur J Clin Nutr. 2010;64(12):1407–14.
Bahreynian M, Paknahad Z, Maracy MR. Major dietary patterns and their associations with overweight and obesity among Iranian children. Int J Prev Med. 2013;4(4):448–58.
Shang X, Li Y, Liu A, Zhang Q, Hu X, Du S, et al. Dietary pattern and its association with the prevalence of obesity and related cardiometabolic risk factors among Chinese children. PLoS One. 2012;7(8):e43183.
Craig LC, McNeill G, Macdiarmid JI, Masson LF, Holmes BA. Dietary patterns of school-age children in Scotland: association with socio-economic indicators, physical activity and obesity. Br J Nutr. 2010;103(3):319–34.
Romero-Polvo A, Denova-Gutierrez E, Rivera-Paredez B, Castanon S, Gallegos-Carrillo K, Halley-Castillo E, et al. Association between dietary patterns and insulin resistance in Mexican children and adolescents. Ann Nutr Metab. 2012;61(2):142–50.
Karatzi K, Moschonis G, Barouti AA, Lionis C, Chrousos GP, Manios Y. Dietary patterns and breakfast consumption in relation to insulin resistance in children. The Healthy Growth Study. Public Health Nutr. 2014;17(12):2790–7.
Park SJ, Lee SM, Kim SM, Lee M. Gender specific effect of major dietary patterns on the metabolic syndrome risk in Korean pre-pubertal children. Nutr Res Pract. 2013;7(2):139–45.
Ochoa-Aviles A, Verstraeten R, Lachat C, Andrade S, Van Camp J, Donoso S, et al. Dietary intake practices associated with cardiovascular risk in urban and rural Ecuadorian adolescents: a cross-sectional study. BMC Public Health. 2014;14:939.
Lazarou C, Newby PK. Use of dietary indexes among children in developed countries. Adv Nutr. 2011;2(4):295–303.
Jennings A, Welch A, Van Sluijs EM, Griffin SJ, Cassidy A. Diet quality is independently associated with weight status in children aged 9–10 years. J Nutr. 2011;141(3):453–9.
Golley RK, Hendrie GA, McNaughton SA. Scores on the dietary guideline index for children and adolescents are associated with nutrient intake and socio-economic position but not adiposity. J Nutr. 2011;141(7):1340–7.
Sabate J, Wien M. Vegetarian diets and childhood obesity prevention. Am J Clin Nutr. 2010;91(5):1525s–9s.
Robinson-O’Brien R, Perry CL, Wall MM, Story M, Neumark-Sztainer D. Adolescent and young adult vegetarianism: better dietary intake and weight outcomes but increased risk of disordered eating behaviors. J Am Diet Assoc. 2009;109(4):648–55.
Lydakis C, Stefanaki E, Stefanaki S, Thalassinos E, Kavousanaki M, Lydaki D. Correlation of blood pressure, obesity, and adherence to the Mediterranean diet with indices of arterial stiffness in children. Eur J Pediatr. 2012;171(9):1373–82.
Mar Bibiloni M, Martinez E, Llull R, Maffiotte E, Riesco M, Llompart I, et al. Metabolic syndrome in adolescents in the Balearic Islands, a Mediterranean region. Nutr Metab Cardiovasc Dis. 2011;21(6):446–54.
Tognon G, Hebestreit A, Lanfer A, Moreno LA, Pala V, Siani A, et al. Mediterranean diet, overweight and body composition in children from eight European countries: cross-sectional and prospective results from the IDEFICS study. Nutr Metab Cardiovasc Dis. 2014;24(2):205–13.
Magriplis E, Farajian P, Pounis GD, Risvas G, Panagiotakos DB, Zampelas A. High sodium intake of children through ‘hidden’ food sources and its association with the Mediterranean diet: the GRECO study. J Hypertens. 2011;29(6):1069–76.
McCourt HJ, Draffin CR, Woodside JV, Cardwell CR, Young IS, Hunter SJ, et al. Dietary patterns and cardiovascular risk factors in adolescents and young adults: the Northern Ireland Young Hearts Project. Br J Nutr. 2014;112(10):1685–98.
Farajian P, Risvas G, Karasouli K, Pounis GD, Kastorini CM, Panagiotakos DB, et al. Very high childhood obesity prevalence and low adherence rates to the Mediterranean diet in Greek children: the GRECO study. Atherosclerosis. 2011;217(2):525–30.
Acknowledgments
The authors appreciate the English revision by Elaine Lilly, PhD (Writer’s First Aid). This research was supported by a grant (2FD097-0297-CO2-01) from Fondo Europeo de Desarrollo Regional (FEDER); by a national scholarship from Spain’s Ministry of Education for PhD training to prepare university professors (FPU: AP2010-3198); by portions of grants from Spain’s Ministry of Health (Ministerio de Sanidad y Consumo, Instituto de Salud Carlos III: FEDER [PI11/01900], FEDER [CB06/02/0029] and Red Investigación Cardiovascular, Programa HERACLES [RD12/0042]) and from the Catalan government’s agency that supports university research groups (AGAUR: 2014 SGR 240), and the King Abdullah scholarship program [2014, ID 2631]. The CIBERESP and CIBEROBN networks are an initiative of the Instituto de Salud Carlos III, Madrid, Spain.
Author information
Authors and Affiliations
Corresponding author
Additional information
Competing interests
The authors declare no conflict of interest.
Authors’ contributions
ANF and HS delimited the topics of the article; ANF, EN, RAB, MF, and HS performed a bibliographic search; ANF and HS wrote the paper. All authors read and approved the submitted version of the manuscript.
Additional file
Additional file 1: Table S1.
Effect of diet on cardiovascular risk factors in children and adolescents. (DOCX 232 kb)
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated.
About this article
Cite this article
Funtikova, A.N., Navarro, E., Bawaked, R.A. et al. Impact of diet on cardiometabolic health in children and adolescents. Nutr J 14, 118 (2015). https://doi.org/10.1186/s12937-015-0107-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12937-015-0107-z