Abstract
Background
As health care spending reaches unsustainable levels, improving value has become an increasingly important policy priority. Relatively little research has explored factors driving value. As a first step towards filling this gap, we performed a scoping review of the literature to identify potential drivers of health care value.
Methods
Searches of PubMed, Embase, Google Scholar, Policy File, and SCOPUS were conducted between February and March 2020. Empirical studies that explored associations between any range of factors and value (loosely defined as quality or outcomes relative to cost) were eligible for inclusion. We created a template in Microsoft Excel for data extraction and evaluated the quality of included articles using the Critical Appraisal Skills Programme (CASP) quality appraisal tool. Data was synthesized using narrative methods.
Results
Twenty-two studies were included in analyses, of which 20 focused on low value service utilization. Independent variables represented a range of system-, hospital-, provider-, and patient-level characteristics. Although results were mixed, several consistent findings emerged. First, insurance incentive structures may affect value. For example, patients in Accountable Care Organizations had reduced rates of low value care utilization compared to patients in traditionally structured insurance plans. Second, higher intensity of care was associated with higher rates of low value care. Third, culture is likely to contribute to value. This was suggested by findings that recent medical school graduation and allopathic training were associated with reduced low value service utilization and that provider organizations had larger effects on value than did individual physicians.
Conclusions
System, hospital, provider, and community characteristics influence low value care provision. To improve health care value, strategies aiming to reduce utilization of low value services and promote high value care across various levels will be essential.
Similar content being viewed by others
Background
In 2018, the United States spent $3.6 trillion on health care, accounting for 17.7% of Gross Domestic Product (GDP) [1]. As a percentage of GDP, U.S. health care spending is nearly double the Organisation for Economic Cooperation and Development average, yet this does not translate into superior health outcomes [2]. Moreover, approximately 25% or more of health care spending is considered waste [3].
Researchers, health care managers, and policy makers thus have increasingly begun to focus on improving value in health care. Value is commonly conceptualized as outcomes or quality divided by costs, although the precise definition varies depending on the clinical context and stakeholder perspective. Along with this focus, large-scale initiatives to improve value have emerged. For example, the Affordable Care Act created incentives for improving quality while reducing costs through Medicare Shared Savings and bundled payment programs [4]. In addition, the American Board of Internal Medicine’s Choosing Wisely initiative generated lists of low value services across a range of specialties with the aim of reducing use of services that have little or no benefit to patients [5].
Though research on the quality and cost of care has been performed for decades, emphasis on value is more recent. Researchers seeking to understand barriers and facilitators of high value care have hypothesized that a wide range of factors—including financial incentives, delivery system structure, geography, demographics, medical education, and patient involvement—contribute to health care value and must be optimized to promote high value care [6]. In addition, extensive work has been done to identify and decrease utilization of low value services. Yet empirical studies analyzing drivers of health care value are relatively sparse. We therefore performed a scoping review to identify potential factors driving value in health care.
Understanding factors associated with health care value requires examination of drivers at multiple levels, including system-level factors (such as policies or insurance structures), hospital-level factors, physician- or practice-level factors, and patient-level factors. This review synthesizes existing literature exploring factors associated with value across these levels to begin building an understanding of how we can address disparities in value and, ultimately, create high value health care systems.
Methods
We conducted a scoping review to identify potential drivers of value in health care. Scoping review methodology, as opposed to systematic review methodology, was selected for this study given that our aim was to provide an overview of a broad range of factors as opposed to gathering evidence in favor of a given treatment, for example [7, 8]. This review followed the five core stages of scoping reviews outlined in the methodological framework by Arksey and O’Malley [9].
Search strategy
With the assistance of a research librarian, we searched PubMed, Embase, PolicyFile, and Google Scholar to identify articles using the terms “value,” “health care,” “low value care,” and “high value care,” in their titles. Boolean operators “AND” and “OR” were used to combine search terms where relevant. The search strategy was limited to English-language publications. No limitations were placed on publication date or study design during the search. Google Scholar hits were limited to the first 100 articles. Scopus citation tracking was also used to identify the top 20 cited articles based on the search terms “value” and “health care.” Searches were performed between February and March 2020. The complete search strategy is contained in Appendix 1. Reference lists of studies selected for inclusion after full-text screening were scanned for potentially relevant articles that may have been missed in initial searches. Grey literature was used to provide context for this review but was not used in analyses given the already broad scope of review.
Study selection
Empirical studies that explored potential factors associated with value were eligible for inclusion. There were no limitations placed on the population studied. We defined the primary concept of interest as the value of healthcare. Only articles that used value as the dependent variable were eligible for inclusion. We accepted a broad range of definitions of value for the purposes of this review but required that the operational definition used a combined measure of cost and outcomes/quality or used a set of services considered to be low or high value (which implicitly includes these terms). Examples of cost measures can include expenditures for an episode of care or specific service, or extend to include downstream costs related to an initial episode of care or service. Examples of operational definitions of quality or outcomes, on the other hand, include patient experience, quality of life measures, and life-years lost or gained. Defining value based on a set of services considered to be low value relies on these services having been shown to provide little to no clinical benefit, thus creating an exceedingly high cost-benefit ratio. Studies exploring a broad range of independent variables and their associations with value were considered. No limitations were placed on context for this review, as value is important across all care settings and environments. Opinion-based articles and literature reviews were excluded from analysis. Studies that were not available in full text through NYU libraries were excluded from analysis. Studies about interventions or implementation of interventions to improve value were excluded. A table with full inclusion and exclusion criteria is presented in Appendix 2.
All studies identified through database searches were exported and uploaded into Covidence online software. Duplicates were automatically removed. An initial review of approximately 15 articles was conducted with all 3 authors to ensure agreement on inclusion criteria. One author (S.L.) then screened the remaining records by title and abstract. Potentially relevant articles were included in the full text review. Any articles of questionable eligibility were discussed by all three authors in the initial screening phase or during full text review. The final decision to include or exclude these publications was determined by consensus. Studies meeting all inclusion criteria after full-text review were kept for data extraction. Reference lists of included studies were hand-searched for any articles that may have been missed in initial searches.
Data extraction and quality appraisal
A data extraction template was created in Microsoft Excel. Elements extracted from eligible articles included basic publication information, study design, population, definition of value (stated and/or operational), statistical methods, main results, conclusions, and limitations. The Critical Appraisal Skills Programme (CASP) quality appraisal tool for cohort studies was used to assess methodological quality of included articles [10]. All articles best fit the CASP cohort studies tool. One author (S.L.) completed all data extraction and quality appraisal.
Data analysis
Findings from studies were synthesized using narrative methods, characterizing studies based on the independent variables (i.e. drivers of value) studied. We organized these drivers into four domains, based on the Institute of Medicine’s delivery system framework: the economic environment (insurance characteristics), the organizational environment (health system and practice characteristics), the care team (physician and other care provider characteristics) and the individual patient (patient-level characteristics) [11]. Zotero was used to manage citations for all articles included in the manuscript. Writing of the review followed PRISMA guidelines for scoping reviews [12].
Results
Study selection
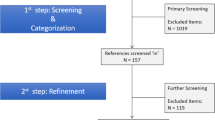
After removing duplicates, a total of 1750 publications were identified through initial searches. An additional 15 publications were identified through hand searching reference lists of articles selected for inclusion. Following screening by title and abstract, 68 were included in the full-text review. Ultimately, 22 studies were found to meet inclusion criteria. The three most common reasons for excluding articles after full text review were that the article did not use value as the dependent variable, focused on implementation of interventions to improve value, or used an ineligible study design (e.g. literature review, opinion-based article). A PRISMA flow-diagram is presented in Fig. 1 to illustrate the study selection process [13].
PRISMA Flow Diagram of Study Selection Process [10]
Characteristics of included studies
Seventeen of the 22 studies exploring factors associated with value in health care were retrospective cohort or cross-sectional studies [14,15,16,17,18,19,20,21,22,23,24,25,26,27,28,29,30]. Three studies used a difference-in-difference or interrupted time series approach [31,32,33] and two used simulation modelling methods [34, 35]. Eighteen studies focused on low value care, two on both low and high value, [23, 29] and two on overall value [27, 35]. Among the included studies, 17 were set in the US, 3 in Canada, [16, 22, 24] 1 in England, [33] and 1 in Australia [34]. Table 1 provides a summary of the methods and major findings of included studies.
The 20 studies that explored factors associated with low value used receipt of low value services, as identified using claims data, as the outcome variables. Of these 20 studies, three also looked at costs associated with the specified low value services as an outcome [15, 25, 31]. In contrast to those studies, Weeks et al., invented a composite measure of value to use as the primary outcome variable. Defining value generally as quality divided by expenditures, the authors deconstructed quality into four component pieces which can be summarized as patient experience, care processes, care outcomes, and safety [27]. Data for each of these components was drawn from Hospital Compare. The authors standardized these measures, multiplied the component pieces together, then divided by total expenditures for the episode of care in order to get a measure of value [27]. On the other hand, Braithwaite et al., defined value as incremental benefits over incremental costs and examined incremental changes in life expectancy and costs as the outcome variables [35].
Quality appraisal
Overall, the quality of included studies was high (Appendix 3). All studies had clearly stated objectives. All of the low value studies used large, representative datasets for cohort selection, and claims-based measures to assess receipt of low value services. Weeks et al. used Hospital Compare data, which allowed for examination of a broader definition of value but lacked some granularity given its aggregation of data [27]. Braithwaite et al. used a validated computer simulation of the entire US health care system [35].
Two articles considered to be of lower quality were those by Koehlmoos et al., and Pendrith et al., as these studies did not adjust for potential confounding variables [20, 24]. The remaining 20 studies adjusted for potential confounders and/or conducted sensitivity analyses. In general, most studies included identified patient-level characteristics as the main potential confounders.
In terms of generalizability of the studies, given the data sources and study designs, it is likely that the findings would apply to the local populations studied. It is unclear, however, if a subset of services considered to be low value is representative of all low value care, and thus if the results are generalizable to all low value care. It is also unclear if results would be applicable to different populations or health systems.
Insurance and health system characteristics
Six studies examined associations between insurance characteristics and receipt of low value services [17, 19, 20, 29, 31, 32]. One study examined associations between different value-based insurance designs and incremental changes in life expectancy and cost [35]. One study examined effects of a national efficiency savings program on low value service utilization [33]. Of the studies exploring associations between insurance characteristics and low value service utilization, five studies showed no clear pattern of significant associations between insurance type and low value care [17, 19, 20, 29, 31]. Three of these studies compared low value service utilization in commercial versus public insurance, [17, 19, 29] one compared direct versus purchased care, [20] and one compared those in a Consumer Directed Health Plan versus traditional plan [31]. Barnett et al. found similar rates of low value care in Medicaid, uninsured, and privately uninsured populations [29]. However, they also found that Medicaid patients were less likely than privately insured patients to receive high value services when pooling estimates of high value service utilization whereas uninsured were more likely to receive high value services compared to their privately insured counterparts. The authors speculated that the latter finding may have been due to unmeasured confounding in a highly select population [29].
In contrast to studies that found no associations between insurance type and value, Schwartz et al. found that patients enrolled in a Pioneer Accountable Care Organization (ACO) Medicare plan saw a differential reduction in the use of low value service (− 0.8 services/100 beneficiaries; 95% CI: − 1.2,-0.4) in the first year of the contract compared to those who remained on a traditional Medicare plan [32]. Accountable Care Organizations are groups of healthcare providers that jointly contract with an insurer (typically, Medicare) to provide coordinated care in exchange for a share of any savings. Some also share in any excess costs. In a computer simulation study, Braithwaite et al. found that value-based insurance designs reducing cost-sharing for high value services and increasing cost-sharing for low value services were associated with a 0.24–0.44 gain in life years without increasing spending [35]. Finally, Coronini-Cronberg et al. found mixed effects on low value service utilization across commissioning organizations from a national efficiency savings policy applied to the National Health Service [33].
Hospital characteristics
Two studies included focused on hospital characteristics associated with value [27, 34]. Badgery-Parker et al. used a multilevel modelling design to test the effects of hospital and region on receipt of low value care. They found that hospital is a more significant contributor to low value care than region [34]. Weeks et al. looked at hospital characteristics such as census, beds, number of operations, accreditation, and for-profit status. They found that higher value was associated with higher census, more beds, and more operations [27].
Physician and practice characteristics
Seven studies focused on physician and/or practice characteristics [14,15,16, 21, 23, 28, 30]. Two additional studies explored physician characteristics in addition to patient characteristics, [18, 22] and one study explored physician characteristics in addition to insurance characteristics [29]. Physician characteristics associated with reduced use of low value services include more recent medical school graduation, allopathic training, smaller patient panel, and being female [15, 16]. Mafi et al. also found that Advanced Practice Clinicians (APCs) had comparable low value service utilization to physicians [21] and Barnett et al. found that safety-net and non-safety net providers had comparable low value service utilization [29].
Investigating both physician and practice variation in low value service utilization, Schwartz et al. found that physician characteristics account for relatively little variation in provision of low value services while organizations contribute substantially more to variation in low value service provision [28] Another study by Schwartz et al. demonstrated a standard deviation of 10 low value services per 100 beneficiaries between provider organizations, further supporting that low value service utilization varies substantially across provider organizations [30]. Other articles identified more specific practice characteristics that may contribute to variation in rates of low value service utilization. For example, fee-for-service practices had higher rates of low value service utilization than capitated practices, [16] community health centers had higher rates of high value care and lower rates of low value care than private practices, [23] and hospital-based practices had higher use of low value services than community-based practices [14]. In addition, two studies showed higher specialist to primary care provider ratios were associated with greater low value care utilization [18, 22].
Patient characteristics
Three studies explored patient characteristics associated with low value care [24,25,26] in addition to the two studies that explored both physician and patient characteristics [18, 22].. Two studies found that being female was associated with higher rates of low value care utilization compared to being male [24, 25]. Two studies showed that black and Hispanic patients had received low value services more frequently [18, 26]. In contrast, Reid et al. found decreased low value spending among black beneficiaries [25]. Four studies showed that higher income was associated with increased rates of low value care utilization [18, 22, 24, 25]. Three studies showed that region was associated with low value care utilization, although patterns for this varied [22, 24, 25].
Discussion
In this review examining factors associated with health care value, we identified 22 studies exploring a range of system- (including insurance), hospital-, provider-, and patient-level characteristics and their associations with value. Across the 22 studies included, almost all [20] focused on utilization of low value services as the dependent variable. Although included studies showed mixed results, several more consistent findings emerged, many of which are reminiscent of findings from past research on factors associated with health care quality and factors associated with health care spending.
One overarching finding from studies included in this review is that incentive schemes may be important drivers of low value service utilization, but only when structured certain ways. For example, in the included articles, neither consumer-directed health plans nor public vs private insurance were associated with low value service utilization, but ACO enrollment was associated with reduced utilization of low value services and value-based insurance design was predicted to increase life expectancy while keeping expenditures constant [32, 35]. ACOs are designed with a primary aim of improving value, and these findings suggest that such a structure may in fact be helpful in doing so. ACO and Alternative Quality Contract enrollment has also been shown to be associated with reduced spending and higher quality, although associations with quality have been less consistently shown [36,37,38,39].
This review also illustrated considerable variation in value by region, hospital, and provider type [22, 24, 25, 27, 28, 30, 34]. Similarly, previously published research has shown regional variation in quality and spending [40,41,42] as well as variation in readmission rates by hospital [43]. In many cases, the associations found with value were similar to those found with quality. For instance, much like Weeks et al. found that higher volume hospitals tended to have higher value, Birkmeyer et al. showed that higher hospital volume was associated with lower surgical mortality—an important element of hospital quality [44]. However, it is important to note that value and quality are distinct. Weeks et al., for instance, found that 50% of the hospitals in the highest or lowest value quintiles were not in the highest or lowest quality quintiles, respectively [27].
Additionally, this review underscored that greater intensity of care (defined as higher ratio of specialists to primary care providers, hospital-based, and fee-for-service payment structure) was associated with higher utilization of low value services [14, 16, 18, 22]. This trend is similarly reflected in quality and cost literature. For example, Wennberg et al. found that greater intensity of hospital care was associated with lower quality care and lower patient experience ratings [45]. In terms of cost, Barnett et al., found that hospital-based physician networks were associated with higher costs and higher intensity of care [46].
Studies included in this review also highlighted physician characteristics associated with value, showing that recent medical school graduation and allopathic training was associated with lower utilization of low value services [16, 18]. It is plausible that this finding reflects changing medical school cultures at allopathic institutions, which are now placing a greater emphasis on value. Tsugawa et al. found that patients treated by older physicians had higher 30-day mortality rates compared to those treated by younger physicians; this difference was not observed in high volume providers nor when comparing readmission rates [47]. They also found slightly higher costs in older physicians [47]. In contrast, Mehrotra et al. found that more recent medical school graduates tended to have higher cost profiles [48]. This discrepancy could reflect several factors including change over time in medical education, lack of concordance between overall spending and spending on low value services, or, given that one of the articles on physician characteristics associated with low value service utilization was set in Canada, there could also be differences across countries. Additionally, Schwartz et al. found that provider organizations had much larger effects on low value service utilization than individual physician characteristics, providing further support for the role of value culture and potentially explaining some of this uncertainty [28].
Higher income and female sex were associated with lower value care in several studies included in this review. Interestingly, opposite results have been found with studies of quality and cost individually. Okunrintemi et al. found that low income patients reported lower quality of care, greater difficulty accessing care, and worse experiences of care compared to high income patients [49]. Epstein et al. also found that patients of a lower socioeconomic status had longer hospital stays and higher charges compared to those with a higher socioeconomic status [50]. Bird et al. showed that women tended to receive higher quality of care than men except in areas related to cardiovascular disease and adverse drug-disease interactions [51]. These differences again highlight the difference between low value service utilization and provision of high quality care.
Importantly, studies included in this review overwhelmingly focused on low value, highlighting current limitations in data and metrics and raising the question of whether patterns of low value service utilization are reflective of value more generally. Although reducing utilization of low value services may seem to be a logical approach to improving value, it is likely insufficient to create a high value health care system. As described in this review, there was a paradoxical finding that high volume was associated with high value, whereas greater intensity of care was associated with higher utilization of low value services. This seeming contradiction provides evidence of a rift between what is deemed high value (including excellent patient outcomes) and the mere absence of low value service utilization. Moreover, studies have repeatedly found that efforts to influence utilization tend to change rates of both appropriate and inappropriate care [52, 53].
By contrast, only four articles in this review explored factors associated with high value (or value) in health care, possibly because high value is often conflated with high quality. In fact, Oronce et al. and Barnett et al. operationalized high value using lists of services that are frequently considered to be quality process measures. But high value and high quality are not the same construct. A health system providing high quality care at very high cost is likely not high value; a system providing both high quality care and excessive low value services is also not high value. These tradeoffs are explicitly addressed in cost effectiveness literature, but this review illustrates that they have had limited use to date when identifying “high value” care.
Strengths and limitations
This scoping review provides an overview of the literature exploring factors associated with value in health care. It is the first to bring together this body of literature as a step towards understanding and utilizing the complex interplay of system-, hospital-, physician-, and patient-level characteristics driving value.
This review has several limitations which are important to address. First, as a scoping review, this relied on title searches to identify relevant articles. Thus, it is possible that relevant studies were missed given the constraints of the search. However, we searched reference lists of included studies to identify additional articles. Second, studies included explored a range of factors that may affect value, with value having been defined using different lists of low value services and different levels of sensitivity and specificity. Consequently, study findings did not elucidate a consistent factor driving value, and comparability and implications of results must be interpreted with caution. Third, given that included studies were primarily observational, we cannot establish causality. Fourth, given the heterogeneity of studies included, it was not possible to conduct a meta-analysis or combine the findings in any quantitative manner. Finally, although three researchers were involved in the planning of the study and any questions that arose regarding inclusion and exclusion criteria, only one reviewer selected articles for inclusion and appraised the quality, making it prone to researcher bias. Pre-determined criteria were used for article selection and standardized templates were used for data extraction in an effort to mitigate this bias, but we acknowledge that this is nonetheless a major limitation of this study.
Conclusion
A complex interplay of system-, hospital-, provider-, and patient-level factors appear to be driving value in health care. In this review, we found evidence supporting the role of insurance incentive schemes, intensity of care, and culture as key drivers of health care value. Although there exists some overlap between factors driving quality of care and factors driving health care value, we found they are not identical, and thus the two constructs must be considered as distinct entities. Moreover, drivers of high value care and drivers of low value care appear to differ. This is especially important to consider when developing interventions to improve value in health care and establishing standards for defining and measuring value. To effectively improve health care value, developing interventions to address drivers across multiple levels of care as well as novel measurement strategies to capture both high and low value practices will be essential.
Availability of data and materials
Not applicable; no additional data available.
References
NHE Fact Sheet | CMS. Available from: https://www.cms.gov/Research-Statistics-Data-and-Systems/Statistics-Trends-and-Reports/NationalHealthExpendData/NHE-Fact-Sheet. [cited 2020 Jun 25].
U.S. Health Care from a Global Perspective, 2019. Commonwealth Fund. Available from: https://www.commonwealthfund.org/publications/issue-briefs/2020/jan/us-health-care-global-perspective-2019. [cited 2020 Jun 25].
Shrank WH, Rogstad TL, Parekh N. Waste in the US health care system: estimated costs and potential for savings. JAMA. 2019;322(15):1501–9.
Innovation Models | CMS Innovation Center. Available from: https://innovation.cms.gov/innovation-models#views=models. [cited 2020 Jul 22].
Our Mission. Choosing Wisely. Available from: https://www.choosingwisely.org/our-mission/. [cited 2020 Jul 22].
Moriates C, Arora V, Shah N, editors. Understanding Value-Based Healthcare. McGraw-Hill Education; 2015. Available from: https://accessmedicine-mhmedical-com.ezproxy.med.nyu.edu/book.aspx?bookid=1371. [cited 2022 Mar 29].
Colquhoun HL, Levac D, O’Brien KK, Straus S, Tricco AC, Perrier L, et al. Scoping reviews: time for clarity in definition, methods, and reporting. J Clin Epidemiol. 2014;67(12):1291–4.
Munn Z, Peters MDJ, Stern C, Tufanaru C, McArthur A, Aromataris E. Systematic review or scoping review? Guidance for authors when choosing between a systematic or scoping review approach. BMC Med Res Methodol. 2018;18(1):143.
Arksey H, O’Malley L. Scoping studies: towards a methodological framework. Int J Soc Res Methodol. 2005;8(1):19–32.
Critical aAppraisal Skills Programme. CASP Cohort Study Checklists. 2018. Available from: https://casp-uk.net/wp-content/uploads/2018/01/CASP-Cohort-Study-Checklist_2018.pdf. [cited 2020 Jun 25].
National Academy of Engineering (US) and Institute of Medicine (US) Committee on Engineering and the Health Care System. In: Reid PP, Compton WD, Grossman JH, Fanjiang G, editors. Building a better delivery system: a new engineering/health care partnership. Washington (DC): National Academies Press (US); 2005. (The National Academies Collection: Reports funded by National Institutes of Health). Available from: http://www.ncbi.nlm.nih.gov/books/NBK22832/. [cited 2022 Apr 10].
Tricco AC, Lillie E, Zarin W, O’Brien KK, Colquhoun H, Levac D, et al. PRISMA extension for scoping reviews (PRISMA-ScR): checklist and explanation. Ann Intern Med. 2018;169(7):467.
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gøtzsche PC, Ioannidis JPA, et al. The PRISMA statement for reporting systematic reviews and Meta-analyses of studies that evaluate health care interventions: explanation and elaboration. PLoS Med. 2009;6(7):e1000100.
Mafi JN, Wee CC, Davis RB, Landon BE. Association of primary care practice location and ownership with the provision of low-value care in the United States. JAMA Intern Med. 2017;177(6):838–45.
Barreto TW, Chung Y, Wingrove P, Young RA, Petterson S, Bazemore A, et al. Primary care physician characteristics associated with low value care spending. J Am Board Fam Med. 2019;32(2):218–25.
Bouck Z, Ferguson J, Ivers NM, Kerr EA, Shojania KG, Kim M, et al. Physician characteristics associated with ordering 4 low-value screening tests in primary care. JAMA Netw Open. 2018;1(6):e183506–6.
Charlesworth CJ, Meath TH, Schwartz AL, KJ MC. Comparison of low-value Care in Medicaid vs commercially insured populations. JAMA Intern Med. 2016;176(7):998–1004.
Colla CH, Morden NE, Sequist TD, Schpero WL, Rosenthal MB. Choosing wisely: prevalence and correlates of low-value health care services in the United States. J Gen Intern Med. 2015;30(2):221–8.
Colla CH, Morden NE, Sequist TD, Mainor AJ, Li Z, Rosenthal MB. Payer type and low-value care: comparing choosing wisely services across commercial and Medicare populations. Health Serv Res. 2018;53(2):730–46.
Koehlmoos TP, Madsen CK, Banaag A, Haider AH, Schoenfeld AJ, Weissman JS. Assessing low-value health care services in the military health system. Health Aff Proj Hope. 2019;38(8):1351–7.
Mafi JN, Wee CC, Davis RB, Landon BE. Comparing use of low-value health care services among U.S. advanced practice clinicians and physicians. Ann Intern Med. 2016;165(4):237–44.
McAlister FA, Lin M, Bakal J, Dean S. Frequency of low-value care in Alberta, Canada: a retrospective cohort study. BMJ Qual Saf. 2018;27(5):340–6.
Oronce CI, Fortuna RJ. Differences in rates of low-value and high-value care between community health centers and pri-vate practices. J Gen Intern Med. 2018;33(2 Supplement 1):161.
Pendrith C, Bhatia M, Ivers NM, Mecredy G, Tu K, Hawker GA, et al. Frequency of and variation in low-value care in primary care: a retrospective cohort study. CMAJ Open. 2017;5(1):E45–51.
Reid RO, Rabideau B, Sood N. Low-value health care services in a commercially insured population. JAMA Intern Med. 2016;176(10):1567–71.
Schpero WL, Morden NE, Sequist TD, Rosenthal MB, Gottlieb DJ, Colla CH. For selected services, blacks and Hispanics more likely to receive low-value care than whites. Health Aff (Millwood). 2017;36(6):1065–9.
Weeks WB, Kotzbauer GR, Weinstein JN. Using publicly available data to construct a transparent measure of health care value: a method and initial results. Milbank Q. 2016;94(2):314–33.
Schwartz AL, Jena AB, Zaslavsky AM, McWilliams JM. Analysis of physician variation in provision of low-value services. JAMA Intern Med. 2019;179(1):16–25.
Barnett ML, Linder JA, Clark CR, Sommers BD. Low-value medical Services in the Safety-net Population. JAMA Intern Med. 2017;177(6):829–37.
Schwartz AL, Zaslavsky AM, Landon BE, Chernew ME, McWilliams JM. Low-value service use in provider organizations. Health Serv Res. 2018;53(1):87–119.
Reid RO, Rabideau B, Sood N. Impact of consumer-directed health plans on low-value healthcare. Am J Manag Care. 2017;23(12):741–8.
Schwartz AL, Chernew ME, Landon BE, McWilliams JM. Changes in low-value services in year 1 of the medicare pioneer accountable care organization program. JAMA Intern Med. 2015;175(11):1815–25.
Coronini-Cronberg S, Bixby H, Laverty AA, Wachter RM, Millett C. English National Health Service’s savings plan may have helped reduce the use of three ‘low-value’ procedures. Health Aff (Millwood). 2015;34(3):381–9.
Badgery-Parker T, Feng Y, Pearson SA, Levesque JF, Dunn S, Elshaug AG. Exploring variation in low-value care: a multilevel modelling study. BMC Health Serv Res. 2019;19(1):345.
Braithwaite RS, Omokaro C, Justice AC, Nucifora K, Roberts MS. Can broader diffusion of value-based insurance design increase benefits from US health care without increasing costs? Evidence from a computer simulation model. PLoS Med. 2010;7(2):e1000234.
Song Z, Rose S, Safran DG, Landon BE, Day MP, Chernew ME. Changes in health care spending and quality 4 years into global payment. N Engl J Med. 2014;371(18):1704–14.
McWilliams JM, Landon BE, Chernew ME. Changes in health care spending and quality for Medicare beneficiaries associated with a commercial ACO contract. JAMA. 2013;310(8):829–36.
McWilliams JM, Hatfield LA, Chernew ME, Landon BE, Schwartz AL. Early performance of accountable care organizations in Medicare. N Engl J Med. 2016;374(24):2357–66.
McWilliams JM, Chernew ME, Landon BE, Schwartz AL. Performance differences in year 1 of pioneer accountable care organizations. N Engl J Med. 2015;372(20):1927–36.
Zhang Y, Baik SH, Fendrick AM, Baicker K. Comparing local and regional variation in health care spending. N Engl J Med. 2012;367(18):1724–31.
Manheim LM, Feinglass J, Shortell SM, Hughes EFX. Regional variation in Medicare hospital mortality. Inquiry. 1992;29(1):55–66.
McKellar MR, Landrum MB, Gibson TB, Landon BE, Fendrick AM, Chernew ME. Geographic variation in quality of care for commercially insured patients. Health Serv Res. 2017;52(2):849–62.
Krumholz HM, Wang K, Lin Z, Dharmarajan K, Horwitz LI, Ross JS, et al. Hospital-readmission risk — isolating hospital effects from patient effects. N Engl J Med. 2017;377(11):1055–64.
Birkmeyer JD, Siewers AE, Finlayson EVA, Stukel TA, Lucas FL, Batista I, et al. Hospital volume and surgical mortality in the United States. N Engl J Med. 2002;346(15):1128–37.
Wennberg JE, Bronner K, Skinner JS, Fisher ES, Goodman DC. Inpatient care intensity and patients’ ratings of their hospital experiences. Health Aff (Millwood). 2009;28(1):103–12.
Barnett ML, Christakis NA, O’Malley AJ, Onnela J-P, Keating NL, Landon BE. Physician patient-sharing networks and the cost and intensity of care in US hospitals. Med Care. 2012;50(2):152–60.
Tsugawa Y, Newhouse JP, Zaslavsky AM, Blumenthal DM, Jena AB. Physician age and outcomes in elderly patients in hospital in the US: observational study. BMJ. 2017;357:j1797.
Mehrotra A, Reid RO, Adams JL, Friedberg MW, McGlynn EA, Hussey PS. Physicians with the least experience have higher cost profiles than do physicians with the Most experience. Health Aff (Millwood). 2012;31(11):2453–63.
Okunrintemi V, Khera R, Spatz ES, Salami JA, Valero-Elizondo J, Warraich HJ, et al. Association of Income Disparities with patient-reported healthcare experience. J Gen Intern Med. 2019;34(6):884–92.
Epstein AM, Stern RS, Weissman JS. Do the poor cost more? A multihospital study of patients’ socioeconomic status and use of hospital resources. N Engl J Med. 1990;322(16):1122–8.
Bird CE, Elliott MN, Adams JL, Schneider EC, Klein DJ, Dembosky JW, et al. How do gender differences in quality of care vary across Medicare advantage plans? J Gen Intern Med. 2018;33(10):1752–9.
Baicker K, Taubman SL, Allen HL, Bernstein M, Gruber JH, Newhouse JP, et al. The Oregon experiment — effects of Medicaid on clinical outcomes. N Engl J Med. 2013;368(18):1713–22.
Finkelstein A, Taubman S, Wright B, Bernstein M, Gruber J, Newhouse JP, et al. The Oregon health insurance experiment: evidence from the first year*. Q J Econ. 2012;127(3):1057–106.
Acknowledgements
Not applicable.
Funding
This study was supported by a grant from the Agency for Healthcare Research and Quality (R01HS022882). The AHRQ had no role in the design and conduct of the study; collection, management, analysis, or interpretation of the data; or preparation, review or approval of the manuscript.
Author information
Authors and Affiliations
Contributions
SNL, JP, and LIH conceived of the project. SNL identified and selected articles for inclusion, extracted data, and conducted quality appraisal. SNL, JP, and LIH discussed any articles of questionable eligibility together. SNL synthesized findings and drafted the manuscript. JP provided administrative and operational support. LIH supervised the project and contributed to manuscript writing. All authors discussed the results and contributed to the final manuscript. The corresponding author attests that all listed authors meet authorship criteria and that no others meeting the criteria have been omitted. The author(s) read approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Not applicable. This study was not human subjects research and therefore did not require approval by the NYU Institutional Review Board.
Consent for publication
Not applicable.
Competing interests
All authors have completed the Unified Competing Interest form at www.icmje.org/coi_disclosure.pdf (available on request from the corresponding author) and declare no competing interests with regard to the submitted work.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Additional file 1: Appendix 1.
Search Strategy. Appendix 2. Full Set of Inclusion and Exclusion Criteria.
Additional file 2: Appendix 3.
Summary of Quality Appraisal.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Landon, S.N., Padikkala, J. & Horwitz, L.I. Identifying drivers of health care value: a scoping review of the literature. BMC Health Serv Res 22, 845 (2022). https://doi.org/10.1186/s12913-022-08225-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12913-022-08225-6