Abstract
Background
EGFR and HER2 overexpression has been reported to play important roles in colorectal cancer (CRC) development and metastasis. Ovarian metastasis is rare yet is one of the most malignant metastases of CRC, but very few studies have focused on its biological features. This study aimed to investigate the expression of EGFR and HER2 in ovarian metastases of CRC and to reveal their clinical significance.
Methods
The expression of HER2 and EGFR in both primary tumours and ovarian metastases was analysed by immunohistochemistry (IHC) in 31 CRC patients with ovarian metastases as well as in the primary tumours of 26 CRC patients with non-ovarian metastases. The overall survival time was calculated with a Kaplan-Meier survival curve and compared with a log-rank test.
Results
HER2 positivity in primary tumours was significantly higher in patients with ovarian metastases than in those with non-ovarian metastases (54.5% vs. 36.4%, P < 0.05). The EGFR-positive rate in primary lesions was not significantly different between patients with ovarian metastases and those with non-ovarian metastases (63.6% vs. 58.3%, P > 0.05). HER2 expression was not correlated with age, primary tumour site, tumour differentiation, tumour diameter or vascular cancer embolus (P > 0.05). The positive rates of HER2 and EGFR in ovarian metastases were 44.8 and 69.0%, respectively. HER2 expression in ovarian metastases was correlated with peritoneal metastasis and bilateral ovarian metastasis (P < 0.05) but not with age, synchronous or metachronous ovarian metastases and the primary tumour site (P > 0.05). There was no significant correlation between EGFR expression and the clinicopathological features in ovarian metastases (P > 0.05). CRC patients with HER2-positive ovarian metastases showed a shortened overall survival time compared to that of CRC patients with HER2-negative metastases (17.0 ± 5.2 vs. 32.0 ± 8.3 months).
Conclusion
Our studies revealed that EGFR and HER2 are highly expressed in the primary tumours and metastases of CRC patients with ovarian metastases. HER2 positivity may be a negative prognostic predictor in patients with ovarian metastases.
Similar content being viewed by others
Background
Colorectal cancer (CRC) is one of the most prevalent cancers worldwide, with 1.01 million new cases and > 0.55 million deaths/year [1]. Although the diagnosis and treatment of CRC has made great progress in recent years, the 5-year survival rate of patients can reach 90.3%, but the survival rate declines to 70.4 and 12.5% for patients diagnosed with regional and metastatic disease, respectively [2]. After the liver, the ovary is the most common metastatic organ in women with CRC [3]. Although the incidence of ovarian metastases is low, women with ovarian metastases have rapid disease progression and a poor prognosis [4, 5]. The overall median survival time of ovarian metastases reported is only 13.6 months [6]; therefore, understanding the mechanism of ovarian metastasis of CRC is of great significance for the prevention and treatment of ovarian metastases.
The human epidermal growth factor receptor family consists of four members: EGFR (HER1, erbB1), HER2 (erbB2, neu), HER3 (erbB3) and HER4 (erbB4), all of which regulate the proliferation and differentiation of various tumour cells [7]. EGFR is positively expressed in 59 to 85% of CRC specimens, and its overexpression is closely related to clinical stage, lymph node metastasis, disease-free survival, poor overall survival, and 5-year recurrence rate [8,9,10]. HER2 is an emerging therapeutic target and prognostic factor for metastatic CRC [11]. The positive expression rate of HER2 protein in CRC tumours varied from 2 to 11%, and this rate increased in more advanced diseases [12].
The expression of HER2 and EGFR and the expression of ovarian metastases in CRC have not been reported. This study compared the expression of HER2 and EGFR in ovarian and non-ovarian metastases in advanced CRC patients and assessed the relationship of their expression levels with clinicopathological variables. We further compared the expression of HER2 and EGFR in primary tumours and ovarian metastases in CRC patients with ovarian metastases and their influence on prognosis.
Methods
Patient information
A total of 31cases of CRC ovarian metastases from the Department of Gastrointestinal Surgery, Guangxi Medical University Affiliated Cancer Hospital from June 2013 to December 2017 were selected. The average age was 50.0 ± 11.0 years. There were 14 cases of synchronous metastases, 17 cases of metachronous metastases, 12 cases of unilateral ovarian metastases, and 19 cases of bilateral metastases; 20 cases had paired primary lesions and ovarian metastases, 9 cases had ovarian metastases only, and 2 cases had primary tumours only. The inclusion criteria were as follows: (1) postoperative diagnosis of primary CRC based on histopathology; and (2) ovarian metastases confirmed by postoperative pathology. Besides histological analysis, expressions of CK7, CA125, CK20, CEA, CDX2, PAX8 were also determined by immunohistochemistry to confirm ovarian metastasis when necessary. The exclusion criterion was the presence of primary ovarian cancer or ovarian metastases derived from other cancers. At the same time, retrospective analysis of third-stage patients with non-ovarian metastases who were treated at our hospital as the control group were selected as controls for EGFR or HER2. The inclusion criteria for the controls were (1) female patients with primary colorectal tumours confirmed by postoperative histopathology; (2) no ovarian metastases detected by computed tomography; and (3) previous confirmation of the HER2 or EGFR expression status with immunohistochemistry (IHC). In total, 22 patients were included in the HER2 control group, with an average age of 65.4 ± 14.5 years; four cases had liver metastases, one case had bladder metastasis, two cases had peritoneal metastasis, and 15 cases had tumour deposits in perirectal/mesorectal adipose tissues. The EGFR control group included 24 patients, with an average age of 67.6 ± 11.9 years, six cases had liver metastases, one had lung metastases, two had bone metastases (1 combined with lung metastases), one had bladder metastases, two had abdominal metastases, and 13 cases had tumour deposits in perirectal/mesorectal adipose tissues. The study was approved by the Ethics Committee of the Affiliated Cancer Hospital of Guangxi Medical University, and all patients signed informed consent.
Immunohistochemical analysis
Surgical specimens were fixed in 10% neutral formaldehyde solution, dehydrated, embedded in paraffin, and serially sectioned at a thickness of 4 μm. Serial sections from the same blocks were used for HER2 and EGFR analysis. Specimen sections were dewaxed by xylene, rehydrated with a standard ethanol gradient, and subjected to high temperature and high pressure for antigen retrieval. The slices were incubated in H2O2 for 10 min at room temperature, subjected to dropwise addition of the corresponding primary antibody followed by incubation at 4 °C overnight, rinsed with phosphate buffered saline (PBS), and subjected to dropwise addition of secondary antibody. A DAB solution was added to visualize the antibody binding, after which the sections were rinsed with distilled water, counterstained with haematoxylin, dehydrated with an ethanol gradient, and fixed with xylene and gelatin. Mouse anti-human HER2/c-erB-2 monoclonal antibody (product number: ZM-0065, clone number: UMAB36) and mouse anti-human EGFR monoclonal antibody (product number: ZM-0093, clone number: UMAB95) were purchased from Beijing Zhongshan Jinqiao Company. A ready-to-use rapid IHC MaxVision™2 detection kit (cat. KIT-5920) was purchased from Fuzhou Maixin Co., Ltd. The experimental procedure was carried out according to the manufacturer’s instructions. The negative control slices were incubated with PBS instead of primary antibody.
Scoring system
HER2 is mostly localized to the cell membrane, while EGFR is expressed in the cell membrane and cytoplasm. HER2 expression was scored as described in the VENTANA study [13]: (−), no tumour cell staining or less than 10% cell membrane staining; (+), > 10% cells had weak or almost undetectable cell membrane staining; (++), > 10% cells were weak to moderate cell membrane staining; and (+++), > 10% of cells have strong cell membrane staining. EGFR expression was determined according to the staining intensity and the number of positive cells. The staining intensity was scored as follows: no staining, 0 points; staining faintly visible, 1 point; weak-medium staining, 2 points; and strong staining, 3 points. The number of positively stained cells was scored as follows: ≤ 10% positive cells, 1 point; 11 to 50%, 2 points; 51 to 80%, 3 points, and ≥ 80%, 4 points. The total score was calculated by multiplying the staining score by the positive cell number score. The expression of EGFR was determined as follows: 0 to 2 points, (−); 3 to 5 points, (+); 6 to 8 points, (++); and 9 to 12 points, (+++). For both HER2 and EGFR, (−) and (+) were considered negative, whereas (++) and (+++) were considered positive. All the results were independently assessed by two highly experienced pathologists in a double-blinded manner and agreed upon by consensus.
Follow-up
All patients in this group were followed up mainly by outpatient review and telephone. The recorded survival time was from the time of diagnosis of ovarian metastases to the time of death or the last follow-up (August 2018).
Statistics
All data were statistically analysed using SPSS 22. Comparisons of EGFR and HER2 expression between groups were using the Wilcoxon rank sum test. Comparisons of data according to HER2 or EGFR expression were performed by Fisher’s exact probability method. The correlation of HER2 and EGFR expression was performed by Spearman’s ranked correlation coefficient. Survival analysis was established according to the Kaplan-Meier method. Comparison of survival times was carried out using log-rank test. A P-value less than 0.05 was considered statistically significant.
Results
HER2 expression and clinicopathological features in primary tumours
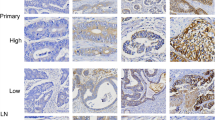
HER2 is mainly expressed in the cell membrane (Fig. 1 a-d). The primary tumour HER2-positive rate in ovarian metastatic CRC patients was 54.5%, which was significantly higher than that in HER2 control patients (36.4%, P < 0.05) (Table 1). There was no significant correlation in the expression of HER2 with age, tumour site, tumour differentiation, tumour diameter, number of positive mesenteric lymph nodes or vascular cancer embolus (P > 0.05). There was no significant correlation between the expression of HER2 and the clinicopathological features in CRC patients with non-ovarian metastasis (P > 0.05) (see Table 2).
Assessment of protein expression of HER2 and EGFR by IHC staining. (× 400). a, c, Positive expression of HER2 in the primary lesion and ovarian metastases, respectively. b, d, Negative expression of HER2 in primary tumours and ovarian metastases, respectively. e, g, Positive expression of EGFR in primary lesion and ovarian metastases, respectively. f, h, Negative expression of EGFR in primary tumours and ovarian metastases, respectively
EGFR expression and clinicopathological features in primary tumours
EGFR was localized to the cell membrane and cytoplasm (Fig. 1e-h). There was no significant difference in the expression of EGFR between CRC patients with ovarian metastasis and those with non-ovarian metastasis (P > 0.05, Table 2). The positive rate of EGFR expression in the CRC ovarian metastasis group was 63.6%. No significant difference was found between the expression of EGFR and the clinicopathological variables (P > 0.05, Table 3).
Expression and clinicopathological features of HER2 and EGFR in ovarian metastases
The positive rate of HER2 in ovarian metastases was 44.8% (13/29). The expression of HER2 in ovarian metastases was associated with peritoneal metastasis and bilateral ovarian infiltration (P < 0.05, Table 4). HER2 expression in ovarian metastases showed no significant relationship with age, synchronous or metachronous ovarian metastasis, or primary site (P > 0.05, Table 4).
The positive expression rate of EGFR in ovarian metastases was 65.5% (19/29). There was no significant difference in EGFR expression between ovarian metastases and the clinicopathological features (P > 0.05, Table 4).
Ten of 29 ovarian metastases were both EGFR and HER2 positive, 10′ cases were EGFR positive only, and 3 cases were HER2 positive only. The remaining 6 cases were negative for both EGFR and HER2. The correlation coefficient between EGFR and HER2 expression was r = 0.155 (P = 0.422), indicating that HER2 and EGFR expression in ovarian metastases was independent of one another.
In paired primary tumours and ovarian metastases samples, 5 out of 20 cases were HER2 positive in both primary tumours and ovarian metastases, 4 cases were HER2 positive in only primary tumours, and 5 cases were only positive in ovarian metastases, 9 cases were EGFR positive in both primary tumours and ovarian metastases, 5 cases were EGFR positive in only primary tumours, and 3 cases were only positive in ovarian metastases. The EGFR-positive rate was 69.0% in ovarian metastases, which was concordant with the 63.6% observed in the matched primary tumours (Tables 1 and 4).
Relationship between HER2 expression and the prognosis of patients with CRC and ovarian metastases
Among all patients with ovarian metastases, the median survival time in metastases HER2-negative patients was 32.0 ± 8.3 months [CI 95%: 15.80–48.19], compared to 17.0 ± 5.2 months [CI 95%:6.76–27.24] in HER2-positive patients (Fig. 2).
Discussion
EGFR and HER2 are all reported to be involved in the development and progress of CRC [8,9,10,11]. But their role in CRC ovarian metastases have not been clarified. In this respect, we analysed their expression and investigated their clinical importance in CRC patients with ovarian metastases.
Diverse rates of HER2 overexpression have been reported in CRC, with rates of membrane HER2 expression ranging from 2 to 11% due to a number of factors, including analysis of distinct subgroups of patients with heterogeneous clinicopathological features, use of different antibodies for IHC and diverse scoring systems (see review by Siena et al. [12]). More recent studies consistently indicated that HER2 overexpression accounts for approximately 2% of all CRCs [14, 15] and 7%~ 11% of stage III or IV tumours [14, 16, 17] are HER2 positive. Shan et al. reported that the HER2 positive rate in female CRC patients was 21.4% (6/26) vs. 8.4% (5/59) in males [17]. In our study, the HER2 positivity in primary tumours was 36.4% (8/22) in metastatic CRC patients with non-ovarian metastases. The observed differences may be caused by the stricter criteria they followed [18]. To date, very few cases with ovarian metastasis have been included in previous studies. In patients with ovarian metastases, the HER2 positive rate was even higher (Table 2), as 12 of 22 primary tumours (54.5%) and 13 of 29 ovarian metastases were HER2 positive in our study.
Recent studies showed that distal carcinomas were more likely to be HER2 or EGFR positive than proximal carcinomas despite the tests used [18, 19]. Higher frequencies of HER2 overexpression were found in rectal cancer than in descending colon or right colon cancers [15]. The results of our research showed that in patients with non-ovarian metastases, the frequency of HER2 overexpression in rectal cancer was higher than colon cancer though the differences was not statically significant due to small sample size. However, in patients with ovarian metastases, the frequency in rectal cancer and colon cancers were similar (Table 2). Among all ovarian metastases, a higher frequency of HER2 positivity in ovarian metastases was correlated with peritoneal metastasis and bilateral ovarian metastasis (P < 0.05) but not with age, synchronous or metachronous ovarian metastases or primary tumour location (P > 0.05) (Table 4).
Previous studies showed inconsistent results regarding the prognostic role of HER2 in CRC [14, 20,21,22]. Earlier studies proposed that HER2 overexpression was a negative prognostic factor [20, 21], but a recent trial concluded that HER2 amplification was not associated with patient outcomes [14, 22]. Nevertheless, for female patients with ovarian metastasis, HER2 overexpression in ovarian metastases indicated a worse overall survival time than that in HER2-negative patients (Fig. 2). However, whether HER2 overexpression could predict a higher risk of ovarian metastasis remains unknown. In addition, HER2 was reported to be a negative biomarker for EGFR-targeted treatments such as cetuximab and panitumumab in CRC [6, 23]. Thus, HER2 status should be considered when developing treatment strategies for those patients.
The role of EGFR was an important player in initiation and progression in CRC. EGFR overexpression was detected in 80–90% of colorectal tumours [8]. In the ERBITUX-OUEST study, 194 (58%) of metastatic CRC cases were EGFR positive [24]. Another study showed that 65% of the primary CRC tumours, 66% of the metastases, and 43% of the matched primary CRC metastases were EGFR positive [25]. In our study, the positive rates of EGFR were 63.6 and 58.3% in primary tumours of patients with ovarian and non-ovarian metastases, respectively (Table 1), which was in line with previous studies. Unlike HER2 positivity, EGFR positivity was not significantly correlated with clinicopathological features in CRC patients with ovarian metastases (P > 0.05).
Conclusions
In conclusion, our studies revealed that HER2 and EGFR are highly expressed in ovarian metastases and primary tumours of CRC patients with ovarian metastases. In addition, HER2 positivity could be a negative prognosis predictor in patients with ovarian metastases.
Abbreviations
- CA125:
-
Cancer Antigen 125
- CDX2:
-
Caudal Type Homeobox 2
- CEA:
-
carcinoembryonic antigen
- CK20:
-
Cytokeratin 20
- CK7:
-
Cytokeratin 7
- CRC:
-
colorectal cancer
- EGFR:
-
Epidermal growth factor receptor
- HER2 (ERBB2, neu):
-
Erb-b2 receptor tyrosine kinase 2
- HER3 (ERBB3):
-
Erb-b2 receptor tyrosine kinase 3
- HER4 (ERBB4):
-
Erb-b2 receptor tyrosine kinase 4
- IHC:
-
immunohistochemistry
- PAX8:
-
Paired box 8
- PBS:
-
phosphate buffered saline
References
Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2018.
Siegel R, Desantis C, Jemal A. Colorectal cancer statistics, 2014. CA Cancer J Clin. 2014;64(2):104–17.
Si Y, Lee J-I, Kim S-H, Kim J-H, Kim HJ, Lee YS, Cho HM, Kim JG, Oh ST, Lee IK. Clinicopathological characteristics of ovarian metastasis from colorectal Cancer. Journal of the Korean Surgical Society. 2010;79(4):287.
Wenhua Li 1 HW, Jian Wang 3 , Fangfang LV 1 , Xiaodong Zhu 1 and Zhonghua Wang 1,4*: ovarian metastases resection from extragenital primary sites: outcome and prognostic factor analysis of 147 patients. BMC Cancer 2012, 12:278 2012.
Lee SJ, Lee J, Lim HY, Kang WK, Choi CH, Lee JW, Kim TJ, Kim BG, Bae DS, Cho YB, et al. Survival benefit from ovarian metastatectomy in colorectal cancer patients with ovarian metastasis: a retrospective analysis. Cancer Chemother Pharmacol. 2010;66(2):229–35.
Qiang Feng WP, Zhao-Xu Zheng, Jian-Jun Bi, Xing-Hua Yuan: Clinicopathologic characteristics and prognostic factors of 63 gastric cancer patients with metachronous ovarian metastasis. Cancer Biol Med 2013;10:86–91 2013.
a1 OMNRLHe: The ErbB signaling network:receptor heterodimerization in development and cancer EMBO J,2000,19(13):3159—3167. 2000.
Rego RL, Foster NR, Smyrk TC, Le M, O'Connell MJ, Sargent DJ, Windschitl H, Sinicrope FA. Prognostic effect of activated EGFR expression in human colon carcinomas: comparison with EGFR status. Br J Cancer. 2010;102(1):165–72.
Lee W-S, Jeong Heum B, Jung Nam L, Woon Kee L: Mutations in K-ras and epidermal growth factor receptor expression in Korean patients with stages III and IV colorectal Cancer. Int J Surg Pathol 2011, 19(2):145–151.
Cappuzzo F, Finocchiaro G, Rossi E, Janne PA, Carnaghi C, Calandri C, Bencardino K, Ligorio C, Ciardiello F, Pressiani T, et al. EGFR FISH assay predicts for response to cetuximab in chemotherapy refractory colorectal cancer patients. Ann Oncol. 2007;19(4):717–23.
Sawada K, Nakamura Y, Yamanaka T, Kuboki Y, Yamaguchi D, Yuki S, Yoshino T, Komatsu Y, Sakamoto N, Okamoto W, et al. Prognostic and predictive value of HER2 amplification in patients with metastatic colorectal Cancer. Clin Colorectal Cancer. 2018;17(3):198–205.
Siena S, Sartore-Bianchi A, Marsoni S, Hurwitz HI, McCall SJ, Penault-Llorca F, Srock S, Bardelli A, Trusolino L: Targeting the human epidermal growth factor receptor 2 (HER2) oncogene in colorectal cancer. Annals of oncology : official journal of the European Society for Medical Oncology 2018, 29(5):1108–1119.
Ruschoff J, Hanna W, Bilous M, Hofmann M, Osamura RY, Penault-Llorca F, van de Vijver M, Viale G. HER2 testing in gastric cancer: a practical approach. Modern pathology : an official journal of the United States and Canadian Academy of Pathology, Inc. 2012;25(5):637–50.
Richman SD, Southward K, Chambers P, Cross D, Barrett J, Hemmings G, Taylor M, Wood H, Hutchins G, Foster JM, et al. HER2 overexpression and amplification as a potential therapeutic target in colorectal cancer: analysis of 3256 patients enrolled in the QUASAR, FOCUS and PICCOLO colorectal cancer trials. J Pathol. 2016;238(4):562–70.
Ingold Heppner B, Behrens HM, Balschun K, Haag J, Kruger S, Becker T, Rocken C. HER2/neu testing in primary colorectal carcinoma. Br J Cancer. 2014;111(10):1977–84.
Valtorta E, Martino C, Sartore-Bianchi A, Penaullt-Llorca F, Viale G, Risio M, Rugge M, Grigioni W, Bencardino K, Lonardi S, et al. Assessment of a HER2 scoring system for colorectal cancer: results from a validation study. Modern pathology : an official journal of the United States and Canadian Academy of Pathology, Inc. 2015;28(11):1481–91.
Shan L, Lv Y, Bai B, Huang X, Zhu H. Variability in HER2 expression between primary colorectal cancer and corresponding metastases. J Cancer Res Clin Oncol. 2018.
Missiaglia E, Jacobs B, D'Ario G, Di Narzo AF, Soneson C, Budinska E, Popovici V, Vecchione L, Gerster S, Yan P et al: Distal and proximal colon cancers differ in terms of molecular, pathological, and clinical features. Annals of oncology : official journal of the European Society for Medical Oncology 2014, 25(10):1995–2001.
Nam SK, Yun S, Koh J, Kwak Y, Seo AN, Park KU, Kim DW, Kang SB, Kim WH, Lee HS. BRAF, PIK3CA, and HER2 oncogenic alterations according to KRAS mutation status in advanced colorectal cancers with distant metastasis. PLoS One. 2016;11(3):e0151865.
Osako T, Miyahara M, Uchino S, Inomata M, Kitano S, Kobayashi M. Immunohistochemical study of c-erbB-2 protein in colorectal cancer and the correlation with patient survival. Oncology. 1998;55(6):548–55.
Kapitanovic S, Radosevic S, Kapitanovic M, Andelinovic S, Ferencic Z, Tavassoli M, Primorac D, Sonicki Z, Spaventi S, Pavelic K, et al. The expression of p185(HER-2/neu) correlates with the stage of disease and survival in colorectal cancer. Gastroenterology. 1997;112(4):1103–13.
Kruszewski WJ, Rzepko R, Ciesielski M, Szefel J, Zielinski J, Szajewski M, Jasinski W, Kawecki K, Wojtacki J. Expression of HER2 in colorectal cancer does not correlate with prognosis. Dis Markers. 2010;29(5):207–12.
Martin V, Landi L, Molinari F, Fountzilas G, Geva R, Riva A, Saletti P, De Dosso S, Spitale A, Tejpar S, et al. HER2 gene copy number status may influence clinical efficacy to anti-EGFR monoclonal antibodies in metastatic colorectal cancer patients. Br J Cancer. 2013;108(3):668–75.
Metges J, Gamelin E, Volant A, Capitain O, Ramee J, Raoul J, Douillard J, Etienne P, Cumin I, Dupuis O: EGFR expression is unreliable to decide for Cetuximab treatment in patients with metastatic colorectal Cancer: results from “ERBITUX-OUEST”. Open Journal of Internal Medicine 2016, 06(02):56–67.
Bibeau F, Boissiere-Michot F, Sabourin JC, Gourgou-Bourgade S, Radal M, Penault-Llorca F, Rochaix P, Arnould L, Bralet MP, Azria D, et al. Assessment of epidermal growth factor receptor (EGFR) expression in primary colorectal carcinomas and their related metastases on tissue sections and tissue microarray. Virchows Archiv : an international journal of pathology. 2006;449(3):281–7.
Funding
The present study was supported by the Guangxi Science and Technology Department Science and Technology Research Development Key Project (No. AB16380202 and AB18221086).
Availability of data and materials
The datasets used and/or analyzed during the present study are available from the corresponding author on reasonable request.
Author information
Authors and Affiliations
Contributions
JLL, YF and YL conceived and designed the study. SHL, JLL, HQC and LSL conducted immunohistochemisty analysis. JLL,SHL,XWM, HL, JZ, JX, BQG collected specimens and patients’ information. YF and JLL analyzed, interpreted the data and drafted the manuscript. YF and YL revised and approved the final version of the manuscript to be published. All authors read and approved the final version of the manuscript.
Corresponding authors
Ethics declarations
Ethics approval and consent to participate
Written informed consent for this research was obtained from the patients prior to surgery. The ethics review committee of the Affiliated Cancer Hospital of Guangxi Medical University approved the present study.
Competing interests
The authors declare that they have no conflicts of interest.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated.
About this article
Cite this article
Li, JL., Lin, SH., Chen, HQ. et al. Clinical significance of HER2 and EGFR expression in colorectal cancer patients with ovarian metastasis. BMC Clin Pathol 19, 3 (2019). https://doi.org/10.1186/s12907-019-0085-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12907-019-0085-8