Abstract
Background
Restoring vital teeth with indirect restorations may threaten dental pulp integrity. However, the incidence of and influential factors on pulp necrosis and periapical pathosis in such teeth are still unknown. Therefore, this systematic review and meta-analysis aimed to investigate the incidence of and influential factors on pulp necrosis and periapical pathosis of vital teeth following indirect restorations.
Methods
The search was conducted in five databases, using MEDLINE via PubMed, Web of Science, EMBASE, CINAHL, and Cochrane Library. Eligible clinical trials and cohort studies were included. The risk of bias was assessed using Joanna Briggs Institute’s critical appraisal tool and Newcastle–Ottawa Scale. The overall incidences of pulp necrosis and periapical pathosis following indirect restorations were calculated using a random effects model. Subgroup meta-analyses were also performed to determine the potential influencing factors for pulp necrosis and periapical pathosis. The certainty of the evidence was assessed using the GRADE tool.
Results
A total of 5,814 studies were identified, of which 37 were included in the meta-analysis. The overall incidences of pulp necrosis and periapical pathosis following indirect restorations were determined to be 5.02% and 3.63%, respectively. All studies were assessed as having a moderate-low risk of bias. The incidence of pulp necrosis following indirect restorations increased when the pulp status was objectively assessed (thermal/electrical testing). The presence of pre-operative caries or restorations, treatment of anterior teeth, temporization for more than two weeks, and cementation with eugenol-free temporary cement, all increased this incidence. Final impression with polyether and permanent cementation with glass ionomer cement both increased the incidence of pulp necrosis. Longer follow-up periods (> 10 years) and treatment provided by undergraduate students or general practitioners were also factors that increased this incidence. On the other hand, the incidence of periapical pathosis increased when teeth were restored with fixed partial dentures, the bone level was < 35%, and the follow-up was > 10 years. The certainty of the evidence overall was assessed as low.
Conclusions
Although the incidences of pulp necrosis and periapical pathosis following indirect restorations remain low, many factors affect these incidences that should thus be considered when planning indirect restorations on vital teeth.
Database registration
PROSPERO (CRD42020218378).
Similar content being viewed by others
Background
Indirect restorations are composed of artificial materials fabricated outside the oral cavity to restore severely damaged teeth [1, 2]. A broad range of indirect restorations is offered in dentistry, and these may be categorized into partial tooth coverage restorations such as inlays, onlays, and veneers, or full coverage restorations such as crowns or fixed partial dentures (FPD) [3]. Over time, the utilization of indirect restorations has increased in popularity, and the routine implementation of these restorations has become an integral part of the treatment modalities provided by most clinicians [4]. Estimates from the Adult Dental Health Survey in the United Kingdom show that 37% of adults with teeth had indirect restorations, with an average of three restorations per individual [5]. The increased utilization of indirect restorations is expected to allow teeth to be retained for a more extended period, yielding further increases in the maintenance and replacement of existing restorations.
The ultimate goals of indirect restoration are to restore teeth to proper form and function, minimize post-operative sensitivity, and preserve the vitality of the pulp [6, 7]. While tooth preparation and cementation are essential steps for indirect restoration, however, these procedures may induce various insults to the pulp and thus jeopardize pulp vitality. Previous studies have shown that tooth preparation disturbs the odontoblastic process and causes permanent damage to the odontoblasts [8,9,10]. Tooth preparation can also expose the dentinal tubules to the oral environment, creating a pathway for microorganisms to access dental pulp [11]. The desiccation from the air and marginal leakage of restorations may cause additional insults to the tooth pulp [12, 13]. The pulp health of teeth undergoing indirect restorations is also likely to be affected by preexisting cumulative insults from caries, periodontal diseases, trauma, or cracks [1, 2]. Once pulp vitality becomes dysfunctional, the pulp degenerates and may be invaded by microorganisms, eventually leading to total necrosis [14]. Depending on the host defense response and the degree of microbial virulence and their byproduct, untreated pulpal infection may also spread beyond the root apex, leading to periapical pathosis [15, 16].
Examining the scientific evidence for the biological consequences of dental pulp following indirect restorations does not only improve clinician knowledge of how to best diagnose and plan treatment but also allows clinicians to present realistic expectations to patients, as well as to assign the necessary time intervals for recall visits. It has been previously shown that the chance of endodontic diseases following indirect restoration procedures increases over time [17]. Within the past 25 years, a number of reports have also attempted to estimate the incidence of pulp necrosis and periapical pathosis following indirect restorations; however, these have yielded inconclusive findings [1, 2, 6]. Data from a recent systematic review and meta-analysis support the long-term success of the crown and FPD treatments on vital abutment teeth [18]. However, this review included only seven studies and lacked the assessment of various confounding factors such as cement type and examination method. Several other concerns have also been raised about that work, particularly in terms of the methodological approach, soundness, and the certainty of results [19]. The current study thus takes the form of a systematic review and meta-analysis and aims to overcome those limitations while investigating the following:
-
I.
The overall incidence of pulp necrosis and periapical pathosis in vital teeth following indirect restorations.
-
II.
The incidence of pulp necrosis and periapical pathosis among vital teeth restored with single-unit (veneer, inlay, onlay, and crown) versus multiple-unit (FPD) restorations.
-
III.
Subgroup analyses of factors that may influence the incidence of pulp necrosis or periapical pathosis in vital teeth following indirect restorations.
Methods
The protocol of this systematic review was registered prior to commencement in PROSPERO (CRD42020218378) and the review was conducted in accordance with the PRISMA-P guidelines.
Inclusion and exclusion criteria
Studies were included on basis of the following criteria:
-
1.
Study design: clinical trials (randomized and non-randomized) and cohort studies.
-
2.
Participants: studies on humans’ permanent teeth.
-
3.
Intervention: indirect dental restorations (single-unit and/ or FPD) in teeth diagnosed preoperatively with vital pulp and normal apical tissue.
-
4.
Outcome: incidence of pulp necrosis and periapical pathosis.
Any study that did not satisfy at least one inclusion criterion was automatically excluded. Moreover, reviews, animal studies, editorials, and descriptive studies such as case reports and case series were not included in this study. Studies that evaluated the incidence of dentin hypersensitivity or pulpitis with indirect restorations were excluded. Studies that did not include an endodontic diagnosis of the teeth prior to indirect restoration placement or lack the follow-up were also excluded.
Information sources
The search was conducted in October 2021 and updated in December 2022 by a senior researcher (NA) across five databases (MEDLINE via PubMed, Web of Science core collection, EMBASE, CINAHL, and Cochrane Library). The search strategy was built using appropriate free-text terms extracted from relevant studies using the PubReminer tool. These free-text terms were complemented with relevant MeSH/Emtree terms and thus truncated and/or combined with proximity operators. The search was completed using the built-in PubMed tools, then adapted for the other databases. To ensure the capture of all relevant studies, the database search was supplemented with a manual search of Google Scholar (first 300 results) and the Open Grey database (www.opengrey.eu), and forward and backward citations of eligible studies. No filters or restrictions were applied on the date or language of publication during searches. The full applied search strategy for this systematic review is thus shown in Supplementary file 1.
Screening process for eligible studies
The search results obtained from the database and manual searches were checked for duplicates using the “check for duplicates” feature in Mendeley. The de-duplicated study list was then imported into a pre-established Excel template. Two independent researchers (SA and GA) screened the titles and abstracts of these studies and classified them as included, excluded, or undecided based on the inclusion and exclusion criteria. Indecision around any study’s inclusion was resolved by mutual discussion or by consulting senior researchers (KKA and KA). The full text of all potentially eligible studies was then critically examined to determine a final list of included studies, with any disagreements arising being again resolved by mutual discussion and consulting the senior researchers. The corresponding author for any study which needed further clarification was contacted.
Quality assessment, data extraction, and certainty of evidence
The methodological quality and bias risk of the included studies were evaluated by two independent researchers (SA and GA) using the Joanna Briggs Institute (JBI) quality appraisal checklist and the Newcastle–Ottawa Quality Assessment Scale (NOS).
The JBI quality appraisal checklist was applied to assess the quality of all randomized clinical studies. This consists of thirteen items ranging from "true randomization used for assignment of participants to treatment groups" to "design appropriateness and deviation from standard randomized clinical trial design". Each item was answered “yes”, “no”, or “unclear”, and based on the percentage of "yes" answers, each study was classified into the appropriate group, with a low risk of bias at ≥ 75%, moderate risk of bias at ≥ 50%–< 75%, and high risk of bias at < 50%.
The NOS was used to assess the overall quality of all cohort studies. This considers three main domains: 1) sample selection, 2) comparability, and 3) exposure/outcome. The NOS adopted a star awards system, with each study awarded a maximum of one star for each item within sample selection and a maximum of two stars for comparability, based on the study design and analysis and outcome categories. The NOS thus allows generation of an overall quality score for each study out of 9, where scores of 1–3, 4–6, and 7–9 represent high, moderate, and low risk of bias, respectively. Any discrepancies during the quality assessment were resolved by consensus or by consulting senior researchers (KKA and KA). The overall evidence certainty was then assessed by applying the Grading of Recommendations Assessment, Development, and Evaluation (GRADE) tool (https://www.gradepro.org/).
Following the quality assessment, the relevant data obtained from the included studies were extracted by two independent researchers (SA and GA). This data included the authors, publication year, country/region, sample size, patient age and gender, medical history, study design, pre-operative tooth condition (e.g., intact, caries, previously restored), tooth type and location, pre-operative periodontal condition (e.g., probing depth, crown to root ratio, bone level), type of temporary cement, duration of temporization (≤ 2 weeks or > 2 weeks), type of impression material, type of permanent cement, type of indirect restoration (single-unit; FPD), materials used in the fabrication of indirect restorations, assessment method (objective: thermal and /or electrical pulp testing; subjective: clinical examination of signs and symptoms such as pain, tenderness, swelling, and/or sensitivity without specifying the use of thermal or electric pulp testing; periapical radiograph), level of practitioner training and expertise, post-treatment follow-up time (≤ 5 years, > 5–10 years, or > 10 years), and outcome measures (incidence of pulp necrosis and periapical pathosis).
Statistical analysis
The kappa value for the inter-observer agreement was measured according to Cohen's kappa by calculating the probability of agreement minus the probability of random agreement divided by one minus the probability of random agreement. Publication bias was assessed by applying funnel plot, Egger’s, and Begg’s tests, while study heterogeneity was evaluated using Cochran Q (Χ2) and I2 statistics. According to Higgins et al. [20], study heterogeneity is considered low when I2 is between 0 and 25%. A fixed-effects model is used when study heterogeneity is low; otherwise, the data can be regarded as heterogenous, and a random-effects model is used. The data was treated as single arm to enhance the generalizability of the results. The meta-analysis was conducted to determine the overall incidences of pulp necrosis and periapical pathosis following indirect restorations at a 95% confidence interval (CI) using a random-effects model. The number of events (teeth diagnosed with pulp necrosis and/ or periapical pathosis following indirect restorations) out of the total number of vital teeth in each included study was calculated. The incidence of pulp necrosis and periapical pathosis among single-unit and FPD restorations was then analyzed. The incidence of pulp necrosis and periapical pathosis was also examined via subgroup analyses in order to determine the effects of the following factors: the method used to assess pulp status, type of temporary cement used, the time between temporary and permanent cementation, the impression material used, the fabrication material(s) used to create indirect restorations, the permanent cement used, the follow-up time and practitioner's training level. Statistical calculations were performed via MedCalc® Statistical Software (version 19.7.2, Ostend, Belgium; https://www.medcalc.org; 2021), with P-values of less than 0.05 considered statistically significant.
Results
Study selection, characteristics, and risk of bias
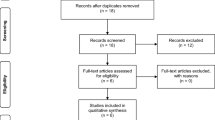
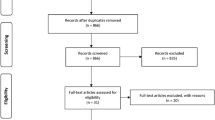
Figure 1 shows the details of the study selection process within a PRISMA flow chart. Thirty-seven studies were included in the final analysis and eighty-nine were excluded (these studies are listed in Supplementary file 2). The total number of teeth included in this review was 11,615. Table 1 shows the baseline characteristics of the included studies.
The incidence of pulp necrosis following indirect restoration was investigated in all included studies, while periapical pathosis was only reported in fifteen studies. Thirty-two of the included studies were cohort study designs and five were randomized clinical trials, and all of them were written in English. Based on the NOS scale, the methodological qualities of the cohort studies were judged as having moderate (16 studies) to low risk of bias (16 studies), while according to the JBI quality appraisal checklist, four randomized clinical trials scored as having a low risk of bias, and one randomized clinical trial was rated as having a moderate risk of bias. A detailed summary of these JBI and NOS assessments is provided in Supplementary files 3 and 4. The interobserver agreement for assessing study selection and risk of bias was rated as excellent (kappa 0.92) [54]. As an indication of publication biases, the funnel plot (Supplementary file 5) and the statistical results for both Begg's and Egger's tests showed no publication bias across any included studies (Begg’s test = 0.07, P = 0.555; Egger’s test = 1.74, P = 0.073).
Meta-analysis
The overall incidences of pulp necrosis and periapical pathosis following indirect restorations were 5.02% (Fig. 2A) and 3.63% (Fig. 2B), respectively. The incidence of pulp necrosis was relatively similar across those teeth restored with single-unit and those with FPD (single-unit = 5.46%; FPD = 5.01%; Fig. 3A). However, the incidence of periapical pathosis was higher in teeth restored with FPD than in teeth restored with single-unit restorations (FPD = 4.59%; single unit = 2.20%; Fig. 3B). A summary of the subgroup meta-analysis results for influential factors on the incidence of pulp necrosis and periapical pathosis is presented in Table 2.
Assessment method
Eight studies used subjective methods [4, 17, 23, 24, 33, 37, 45, 49], twenty-four studies used objective methods [1, 6, 22, 25,26,27, 30,31,32, 34, 36, 39,40,41,42,43,44, 46,47,48, 50,51,52,53], and five studies used periapical radiographs [21, 28, 29, 35, 38] to evaluate the incidence of pulp necrosis following indirect restoration. The incidence of pulp necrosis was highest in teeth assessed using objective tools (5.66%), followed by periapical radiographs (4.95%), and subjective examination (3.91%).
Temporary cement type and temporization period
Fifteen studies described the type of temporary cement (eugenol-based cement or eugenol-free cement) used for provisional restorations [6, 17, 25, 27, 28, 32,33,34, 37, 38, 47,48,49,50,51], and eight studies stated the time lapse between the temporization and permanent cementation (≤ 2 weeks or > 2 weeks) [6, 26, 34, 37, 38, 47, 49, 50]. Teeth temporized with eugenol-based cement and those with a short duration (≤ 2 weeks) before placement of indirect restorations had low incidences of pulp necrosis (eugenol-based cement = 3.34%; ≤ 2 weeks = 1.47%), whereas teeth temporized with eugenol-free cement or for longer periods (> 2 weeks) exhibited higher incidences of pulp necrosis (eugenol-free cement = 5.77%; > 2 weeks = 4.25%). Subgroup meta-analysis of the incidence of periapical pathosis could not be performed due to limited data.
Impression material
Eighteen studies reported the type of impression materials used in the fabrication of indirect restorations [4, 21, 23, 26,27,28, 31,32,33, 36,37,38, 44, 45, 47, 48, 51, 52]; one study used compound material [28], another study used reversible hydrocolloid material [37], and three studies used more than one type of impression material [4, 31, 45]. The incidence of pulp necrosis was 3.27% when the compound material was used, but lower when reversible hydrocolloid material was used (1.19%). Thirteen studies used a single type of elastomeric impression material (polyether or polyvinyl siloxane) [21, 23, 26, 27, 32, 33, 36, 38, 44, 47, 48, 51, 52]. The incidence of pulp necrosis was higher when the impression was taken using polyether (4.02%) than where polyvinyl siloxane was used (3.17%). Subgroup meta-analysis of the incidence of periapical pathosis could not be performed due to limited data.
Fabrication material
Five studies did not report the type of fabrication material used in the construction of indirect restorations [6, 22, 28, 39, 51], while twenty-two studies included different types of fabrication materials [4, 17, 24,25,26,27, 29,30,31,32,33,34,35,36,37,38, 40, 44, 45, 47, 52, 53]. A subgroup meta-analysis of the ten studies [1, 21, 23, 41,42,43, 46, 48,49,50] that used a single type of fabrication material (ceramic or porcelain-fused-to-metal [PFM]) was thus performed. The incidences of pulp necrosis among teeth restored with ceramic and PFM materials were quite similar (ceramic: 5.59%; PFM: 5.71%). Subgroup meta-analysis of the incidence of periapical pathosis could not be performed due to limited data.
Permanent cement type
Twenty-nine studies reported the type of permanent cement used for indirect restorations [4, 17, 21, 23, 25,26,27,28, 30,31,32,33,34, 36,37,38, 40,41,42,43,44,45,46,47,48,49,50, 52, 53]. Of these, seventeen studies used a single type of permanent cement for cementation of indirect restorations [17, 21, 23, 26,27,28, 31, 32, 38, 41,42,43,44, 46, 47, 50, 53], and sixteen of these were included in the meta-analysis [17, 21, 23, 26,27,28, 31, 32, 38, 41,42,43,44, 46, 47, 53]. Teeth cemented with Glass Ionomer Cement (GIC) had the highest incidence of pulp necrosis (5.33%), followed by zinc phosphate cement (4.92%), and resin (3.37%). On the other hand, Uzgur et al. [50], in their study that featured a relatively large sample size found an extremely low incidence of pulp necrosis (1.1%) in teeth cemented permanently with zinc polycarboxylate. However, this study was excluded from the subgroup meta-analysis because it was the only study that used zinc polycarboxylate as permanent cement for indirect restorations. Subgroup meta-analysis of the incidence of periapical pathosis could not be performed due to limited data.
Post-treatment follow-up period
The follow-up periods across the included studies were categorized into groups as ≤ 5 years, > 5–10 years, or > 10 years. A subgroup meta-analysis revealed that as the follow-up time increases, the incidence of pulp necrosis increases. Teeth with the longest follow-up times (> 10 years) following indirect restorations had a higher incidence of pulp necrosis than teeth after > 5–10 years or ≤ 5 years of follow-up time (> 10 years = 6.74%; > 5–10 years = 5.53%; ≤ 5 years = 3.53%). Similar results were also observed for the incidence of periapical pathosis, with teeth with > 10 years follow-up having the highest incidence (4.05%), followed by those at > 5–10 years (3.88%), and those at ≤ 5 years (2.26%) follow-up period.
Practitioner training level
Twenty-nine studies reported the level of practitioner training during the placement of indirect restorations on vital teeth [4, 6, 17, 21, 24, 26, 28, 30, 31, 33,34,35,36,37,38,39,40, 42,43,44,45,46,47,48,49,50, 52, 53, 55]. Ten studies included more than one level of training without specifying the incidence of pulp necrosis for each training level [21, 24, 30, 31, 36, 38, 42, 49, 53, 55]. Nineteen studies ascribed the incidence of pulp necrosis to one level of training (undergraduate students or general practitioners or prosthodontists), and these were included in the meta-analysis [4, 6, 17, 26, 28, 33,34,35, 37, 39, 40, 43,44,45,46,47,48, 50, 52]. The incidence of pulp necrosis in teeth restored with indirect restorations by undergraduate students or general practitioners was higher than in teeth treated by prosthodontists (undergraduate students = 5.68%; general practitioners = 4.44%; prosthodontists = 1.87%). Subgroup meta-analysis of the incidence of periapical pathosis could not be performed due to limited data.
Pre-operative tooth condition and tooth location
Eight studies reported the pre-operative tooth condition (intact, caries, previously restored and /or crowned, wear, fracture, and amelogenesis imperfecta) before the placement of indirect restorations [6, 17, 26, 33, 36, 38, 47, 52]. However, only one study investigated the effect of pre-operative tooth condition on the incidence of pulp necrosis following indirect restorations, and this showed teeth with pre-operative caries, fillings, or crowns had a higher incidence of pulp necrosis (13%) as compared to intact teeth (5%) [6]. The incidence of pulp necrosis in relation to the tooth location in the jaw (maxillary versus mandibular teeth and anterior versus posterior teeth) was reported in two studies [1, 6]. According to one, maxillary anterior teeth had the highest incidence of pulp necrosis following indirect restorations (30.2%), followed by maxillary posterior (23.7%), mandibular posterior (6.1%), and mandibular anterior (0%) teeth [1]. Conversely, the other study found that mandibular anterior teeth had the highest incidence of pulp necrosis (11.8%) as compared to maxillary anterior (9.4%), maxillary posterior (7.5%), and mandibular posterior (7.1%) teeth [6].
Pre-operative periodontal condition
The influence of pre-operative periodontal condition (probing depth, crown to root ratio, bone level, furcation involvement, and tooth mobility) on the incidence of pulp necrosis and/or periapical pathosis were investigated in only a single study [36]. Bone level was the only periodontal factor found to influence the incidence of periapical pathosis. Specifically, teeth with a pre-operative bone level < 35% had a higher incidence of periapical pathosis (1.4%) than teeth with a bone level ≥ 35% (0%) [36].
Certainty of evidence
The certainty of the evidence was rated as low for all outcome measures based on the assessment of the certainty parameters. A detailed summary of the certainty of the evidence is provided in Supplementary file 6.
Discussion
Through the systematic search and meta-analysis, a strong body of evidence could be built regarding the number of vital teeth that may develop pulp necrosis and/or periapical pathosis after indirect restorations. This work is the first study that has assessed the incidence of pulp necrosis and periapical pathosis following indirect restorations of vital teeth as well as the potential factors that influence such incidence in this manner. Our findings revealed that the incidence of pulp necrosis and periapical pathosis following indirect restorations was relatively low. The incidence of pulp necrosis was found to be consistent for teeth restored via single-unit or FPD restorations. However, FPD-restored teeth had a higher incidence of periapical pathosis than teeth restored with single-unit restorations. According to subgroup meta-analyses, the incidence of pulp necrosis and periapical pathosis in vital teeth treated with indirect restorations appeared to be influenced by several factors.
As shown in this study, teeth restored with FPD have a higher incidence of periapical pathosis than teeth restored using single-unit restorations. FPD restorations are thought to generate higher occlusal forces than single-unit restorations, including vertical and transverse forces, potentially generating additional axial forces and stress gradients in the root, and supporting bone which may result in periapical radiographic changes. Consistent with the previous studies [1, 17], our finding revealed that the incidence of pulp necrosis among teeth restored with indirect restorations was influenced by the methods of assessing pulp status. Teeth assessed clinically by objective examination had a higher incidence of pulp necrosis than those assessed subjectively or by periapical radiographs. This could be related to the fact that the incidence of pulp necrosis may be underestimated when subjective and/or radiological assessment is used only as a diagnostic tool, as pulp necrosis can occur in the absence of radiographic changes or clinical signs and symptoms develop [56]. It should be noted that all the included studies used 2-dimensional periapical radiographs to assess periapical pathosis even though this method is widely acknowledged as being less accurate than cone-beam computed tomography (CBCT) [57, 58].
Another factor that influences the incidence of pulp necrosis following indirect restoration is the type of temporary cement used. Interestingly, teeth temporized with eugenol-containing cement demonstrated a lower incidence of pulp necrosis than teeth temporized with eugenol-free cement. Eugenol-containing cement has a wide-ranging disparity between toxicity to the pulp in absence of dentin protection relative to its safety when applied to dentin [59]. Although the biological effects of temporary cement are impacted by the thickness of dentin, several studies have highlighted the unique properties of eugenol-based cement, including antioxidant and sedative effects, lower dentin hypersensitivity, and the prevention of inflammatory responses in the pulp [59,60,61]. This could explain the lower incidence of pulp necrosis in teeth temporized with eugenol-containing cement. Meanwhile, the incidence of pulp necrosis is also influenced by the duration of temporization before permanent cementation. Our findings revealed that teeth temporized for more than two weeks had more pulp necrosis events than teeth temporized for two weeks or less. Results from previous studies showed that temporary cement has poor sealing abilities that may be associated with higher microleakage during long-term temporization [60, 62]. This drawback of temporary cement is further worsened in the presence of marginal gaps or ill-fitting provisional restorations, thus exposing the dentinal tubules to more irritants that may jeopardize pulp health.
As elastomeric impression materials (e.g., polyethers and polyvinyl siloxanes) have high accuracy and excellent properties, they are often used for indirect restorations [63]. The current findings revealed that the incidence of pulp necrosis was higher when polyether impression material was applied to teeth than polyvinyl siloxane. Generally, the shorter the contact between the tooth structure and impression materials, the less damage will be caused to the dental pulp [64]. However, polyethers have been found to be more toxic to fibroblast cells than polyvinyl siloxanes in human and animal studies [65,66,67,68]. Nonetheless, pulp necrosis does not appear to be impacted by the fabrication material applied to indirect restorations (i.e., PFM or ceramics). The similar incidence of pulp necrosis in these materials may be due to sufficient remaining dentinal thickness that protects the dental pulp [69, 70]. Our study also examined the impacts that permanent cement had on the incidence of pulp necrosis following indirect restorations. Although there is only one study that has examined polycarboxylate cement using a large sample, the cement has been found to have minimal impacts on dental pulp in comparison to other cement types [50]. This could be due to the biocompatibility properties of polycarboxylate cement which produces less fluoride (15–20%) than other cement types [71]. However, the incidence of pulp necrosis was highest with GIC cement due to the high acidity of GIC and the release of many fluoride ions which damage the dental pulp [71,72,73].
It is essential to implement long-term follow-up protocols after indirect restorations so that biological failures can be detected as early as possible. Our findings revealed that the incidence of pulp necrosis following indirect restorations increases as follow-up time is increased. From a clinical perspective, the increase in the incidence of pulp necrosis over time may be linked to the degree of irritation to the dental pulp from issues such as recurrent caries or trauma [6, 74]. Recent findings also revealed that elderly individuals have a greater risk of developing pulp necrosis [75]. Thus, it is reasonable to hypothesize that longer follow-ups enable aging-related changes to affect the pulp, which can result in fibrosis and reduced innervation. One of the most remarkable findings of this study is that practitioner training levels largely impact pulp necrosis following indirect restorations. The incidence of pulp necrosis was greater in teeth treated by general practitioners and undergraduate students than prosthodontists, which is in line with other research findings [76,77,78,79]. Moreover, experienced practitioners are more knowledgeable regarding treatment planning and have learned from previous failures [80]. Thus, it is important to consider the practitioner's competence level during indirect restoration procedures to ensure that the best clinical outcomes are achieved.
In this systematic review, only one study investigated the influence of pre-operative tooth conditions on the incidence of pulp necrosis. In that study, a higher incidence of pulp necrosis was observed in teeth with pre-operative caries, restorations, or previous crowns [6]. Teeth with intact enamel and healthy dentin-pulp complexes typically have protective mechanisms against external insults, whereas teeth that have been structurally compromised due to caries, trauma, or restorations may suffer from stress pulp conditions [69, 81]. Tooth preparation for indirect restoration may further irritate the pulp of compromised teeth, leading to pulpal death [82]. With regard to tooth type and location, a limited number of studies have investigated the incidence of pulp necrosis following indirect restorations [1, 6]. In the current study, maxillary and mandibular anterior teeth demonstrated a higher incidence of pulp necrosis than posterior teeth. This observation could be explained by the fact that anterior teeth are smaller than posterior teeth and removing the enamel and dentin during tooth preparation results in a thin dentinal structure near the pulp [6]. The clinical implication of this observation is particularly crucial in circumstances where the tooth's longitudinal axis must be modified during preparation. Rotated teeth, teeth with higher axial inclinations, and teeth with severe discoloration are examples of situations where additional reduction of tooth structure is required to obtain the proper angle of parallelism [1]. It is also noteworthy to mention that the distribution of teeth according to their types and locations in the relevant studies [1, 6] was not identical, meaning that the impacts of tooth type and location on pulp necrosis have not yet been examined.
The current study's findings showed limited evidence to support the influence of pre-operative bone level on the incidence of pulp necrosis and/or periapical pathosis in teeth restored with indirect restorations. In one study with a small sample size, periapical pathosis was more evident in teeth with a < 35% pre-operative bone level than in teeth with a ≥ 35% bone level [36]. Several histological studies have shown that bacterial plaque deposition on exposed root surfaces is associated with pathological changes in the adjacent pulp tissue, as this allows bacterial products to invade the pulp via exposed dentinal tubules and accessory canals [83, 84]. It is thus reasonable to assume that the greater alveolar bone loss, the greater the risk of bacterial irritants reaching and infecting the pulp; however, further longitudinal studies are required.
One of the strengths of the current systematic review is that it featured an extensive and comprehensive database search, thus capturing all available evidence on the research question with no restrictions on publication date or language. Furthermore, the nature of the included studies was focused on clinical trials and cohort studies, types of studies that provide a lot of evidence supporting observations of the incidences of pulp necrosis and periapical pathosis following indirect restorations. Another important strength was the use of subgroup analyses for those factors that influence the incidence of pulp necrosis and periapical pathosis following indirect restorations. These analyses undoubtedly added further insights into the potential impact of these factors on the incident of pulp necrosis and periapical pathosis. Finally, the GRADE tool was used to evaluate the certainty of the evidence in each measured outcome, revealing a low level of evidence.
However, the presence of high heterogeneity among the included studies is one of the current study's limitations. This could be due to the different clinical settings and methodologies used in included studies. Although a subgroup meta-analysis was performed, heterogeneity remained, and thus the results should be interpreted with caution. Furthermore, due to the limited number of studies reporting on pre-operative tooth conditions, tooth types, and per-operative periodontal conditions, a subgroup meta-analysis of these factors could not be performed. Another limitation is the small number of randomized clinical trials included, and more standardized clinical trials are required. A subgroup meta-analysis for partial versus full-coverage restorations was also not conducted, as the majority of the studies involved different designs for indirect restorations without specifying the incidence of pulp necrosis or periapical pathosis for each design.
Conclusions
With a low-level of evidence, this study indicated that the incidence of pulp necrosis and periapical pathosis in vital teeth following indirect restorations was relatively low. Moreover, single-unit and multiple-unit restorations had the same level of impact on pulp necrosis, although single-unit restorations demonstrated a lower incidence of periapical pathosis than FPD. Many factors can influence pulp necrosis and periapical pathosis, although not all have been examined in this work. Thus, these factors must be carefully considered when planning indirect restorations.
Availability of data and materials
The data used to support the findings of this study are available within the article and its supplementary files.
References
Cheung GS, Lai SC, Ng RP. Fate of vital pulps beneath a metal-ceramic crown or a bridge retainer. Int Endod J. 2005;38(8):521–30.
Yavorek A, Bhagavatula P, Patel K, Szabo A, Ibrahim M. The Incidence of Root Canal Therapy after Full-Coverage Restorations: A 10-Year Retrospective Study. J Endodontics. 2020;46(5):605–10.
Brunton PA, Ratnayake J, Loch C, Veerasamy A, Cathro P, Lee R. Indirect Restorations and Fixed Prosthodontics: Materials and Techniques Used by General Dentists of New Zealand. Int J Dentistry. 2019;2019:5210162.
Olley RC, Andiappan M, Frost PM. An up to 50-year follow-up of crown and veneer survival in a dental practice. J Prosthet Dent. 2018;119(6):935–41.
Lynch CD, Hale R, Chestnutt IG, Wilson NHF. Reasons for placement and replacement of crowns in general dental practice. Br Dent J. 2018;225(3):229–34.
Kontakiotis EG, Filippatos CG, Stefopoulos S, Tzanetakis GN. A prospective study of the incidence of asymptomatic pulp necrosis following crown preparation. Int Endod J. 2015;48(6):512–7.
Al-Manei KK, Ban Owaiwid A, AlDhafiri R, Al-Manei K, AlHarran S, Alsulaimani R. Shear Bond Strength of E. Max Ceramic Restoration to Hydraulic Calcium Silicate Based Cement (Biodentine): An In Vitro Study. Eur Endod J. 2020;5(3):288–94.
Galler KM, Weber M, Korkmaz Y, Widbiller M, Feuerer M: Inflammatory Response Mechanisms of the Dentine-Pulp Complex and the Periapical Tissues. Int J Mol Sci 2021:22(3):1480.
Kawashima N, Okiji T. Odontoblasts: Specialized hard-tissue-forming cells in the dentin-pulp complex. Congenit Anom (Kyoto). 2016;56(4):144–53.
Cavalcanti BN, Otani C, Rode SM. High-speed cavity preparation techniques with different water flows. J Prosthet Dent. 2002;87(2):158–61.
Pashley DH. Dentin-predentin complex and its permeability: physiologic overview. J Dental Res. 1985;64 Spec No:613–20.
Bergenholtz G, Cox CF, Loesche WJ, Syed SA. Bacterial leakage around dental restorations: its effect on the dental pulp. J Oral Pathol. 1982;11(6):439–50.
Cotton WR. Pulp response to an airstream directed into human cavity preparations. Oral Surg Oral Med Oral Pathol. 1967;24(1):78–88.
Manoil D, Al-Manei K, Belibasakis GN. A Systematic Review of the Root Canal Microbiota Associated with Apical Periodontitis: Lessons from Next-Generation Sequencing. Proteomics Clin Appl. 2020;14(3):e1900060.
Gomes B, Herrera DR. Etiologic role of root canal infection in apical periodontitis and its relationship with clinical symptomatology. Braz Oral Res. 2018;32(suppl 1): e69.
Al-Manei K, Ghorbani M, Naud S, Al-Manei KK, Sobkowiak MJ, Lund B, Hazirolan G, Sällberg Chen M, Özenci V. Clinical Microbial Identification of Severe Oral Infections by MALDI-TOF Mass Spectrometry in Stockholm County: an 11-Year (2010 to 2020) Epidemiological Investigation. Microbiol Spectr. 2022;10(6):e0248722.
Valderhaug J, Jokstad A, Ambjørnsen E, Norheim PW. Assessment of the periapical and clinical status of crowned teeth over 25 years. J Dent. 1997;25(2):97–105.
Kohli S, Bhatia S, Al-Haddad A, Pulikkotil SJ, Jamayet NB: Pulpal and Periapical Status of the Vital Teeth Used as Abutment for Fixed Prosthesis-A Systematic Review and Meta-Analysis. J Prosthodont. 2022;31(2):102–114.
Javed F, Haji Z, Khan FR: Comments on Pulpal and Periapical Status of the Vital Teeth Used as Abutment for Fixed Prosthesis: A Systematic Review and Meta-Analysis. J Prosthodont 2022;31(2):93.
Higgins JP, Thompson SG, Deeks JJ, Altman DG. Measuring inconsistency in meta-analyses. BMJ. 2003;327(7414):557–60.
Aziz AM, El-Mowafy O, Tenenbaum HC, Lawrence HP. Clinical performance of CAD-CAM crowns provided by predoctoral students at the University of Toronto. J Prosthet Dent. 2022;127(5):729–36.
Bergenholtz G, Nyman S. Endodontic complications following periodontal and prosthetic treatment of patients with advanced periodontal disease. J Periodontol. 1984;55(2):63–8.
Chaar MS, Passia N, Kern M. Long-term clinical outcome of posterior metal-ceramic crowns fabricated with direct metal laser-sintering technology. J Prosthodont Res. 2020;64(3):354–7.
Cheung GS. A preliminary investigation into the longevity and causes of failure of single unit extracoronal restorations. J Dent. 1991;19(3):160–3.
Denner N, Heydecke G, Gerds T, Strub JR. Clinical comparison of postoperative sensitivity for an adhesive resin cement containing 4-META and a conventional glass-lonomer cement. Int J Prosthodont. 2007;20(1):73–8.
Derchi G, Marchio V, Borgia V, Özcan M, Giuca MR, Barone A. Twelve-year longitudinal clinical evaluation of bonded indirect composite resin inlays. Quintessence Int. 2019;50(6):448–54.
Encke BS, Heydecke G, Wolkewitz M, Strub JR. Results of a prospective randomized controlled trial of posterior ZrSiO(4)-ceramic crowns. J Oral Rehabil. 2009;36(3):226–35.
Ericson S, Hedegård B, Wennström A. Roentgenographic study of vital abutment teeth. J Prosthet Dent. 1966;16(5):981–7.
Fayyad MA. al-Rafee MA: Failure of dental bridges: III–Effect of some technical factors. J Oral Rehabil. 1996;23(10):675–8.
Forrer FA, Schnider N, Brägger U, Yilmaz B, Hicklin SP. Clinical performance and patient satisfaction obtained with tooth-supported ceramic crowns and fixed partial dentures. J Prosthet Dent. 2020;124(4):446–53.
Hämmerle CH, Ungerer MC, Fantoni PC, Brägger U, Bürgin W, Lang NP. Long-term analysis of biologic and technical aspects of fixed partial dentures with cantilevers. Int J Prosthodont. 2000;13(5):409–15.
Ioannidis A, Bindl A. Clinical prospective evaluation of zirconia-based three-unit posterior fixed dental prostheses: Up-to ten-year results. J Dent. 2016;47:80–5.
Johnson GH, Powell LV, DeRouen TA. Evaluation and control of post-cementation pulpal sensitivity: zinc phosphate and glass ionomer luting cements. J Am Dent Assoc. 1993;124(11):38–46.
Jokstad A, Mjör IA. Ten years’ clinical evaluation of three luting cements. J Dent. 1996;24(5):309–15.
Karlsson S. A clinical evaluation of fixed bridges, 10 years following insertion. J Oral Rehabil. 1986;13(5):423–32.
Mohamed Khazin S, Abdullah D, Liew AKC, Soo E, Ahmad Tarib N: Pulpal and periapical disease in crowned vital teeth: A prospective matched cohort study. Aust Endod J 2022;48(1):8–19.
Lockard MW. A retrospective study of pulpal response in vital adult teeth prepared for complete coverage restorations at ultrahigh speed using only air coolant. J Prosthet Dent. 2002;88(5):473–8.
Lundgren GP, Vestlund GM, Dahllöf G. Crown therapy in young individuals with amelogenesis imperfecta: Long term follow-up of a randomized controlled trial. J Dent. 2018;76:102–8.
Lundqvist P, Nilson H. A clinical re-examination of patients treated with pinledge-crowns. J Oral Rehabil. 1982;9(5):373–87.
Piemjai M, Adunphichet N. Impact of hybrid layer formation on the 15-year survival, complications, and failures of full-coverage retainers. J Prosthodont Res. 2022;66(1):131–40.
Rauch A, Reich S, Schierz O. Chair-side generated posterior monolithic lithium disilicate crowns: clinical survival after 6 years. Clin Oral Investig. 2017;21(6):2083–9.
Reich S, Schierz O. Chair-side generated posterior lithium disilicate crowns after 4 years. Clin Oral Investig. 2013;17(7):1765–72.
Reichen-Graden S, Lang NP. Periodontal and pulpal conditions of abutment teeth. Status after four to eight years following the incorporation of fixed reconstructions. Schweiz Monatsschr Zahnmed. 1989;99(12):1381–5.
Rinke S, Gersdorff N, Lange K, Roediger M. Prospective evaluation of zirconia posterior fixed partial dentures: 7-year clinical results. Int J Prosthodont. 2013;26(2):164–71.
Rinke S, Lange K, Roediger M, Gersdorff N. Risk factors for technical and biological complications with zirconia single crowns. Clin Oral Investig. 2015;19(8):1999–2006.
Rinke S, Pfitzenreuter T, Leha A, Roediger M, Ziebolz D. Clinical evaluation of chairside-fabricated partial crowns composed of zirconia-reinforced lithium silicate ceramics: 3-year results of a prospective practice-based study. J Esthet Restor Dent. 2020;32(2):226–35.
Scheibenbogen A, Manhart J, Kunzelmann KH, Hickel R. One-year clinical evaluation of composite and ceramic inlays in posterior teeth. J Prosthet Dent. 1998;80(4):410–6.
Selz CF, Strub JR, Vach K, Guess PC. Long-term performance of posterior InCeram Alumina crowns cemented with different luting agents: a prospective, randomized clinical split-mouth study over 5 years. Clin Oral Investig. 2014;18(6):1695–703.
Tinschert J, Schulze KA, Natt G, Latzke P, Heussen N, Spiekermann H. Clinical behavior of zirconia-based fixed partial dentures made of DC-Zirkon: 3-year results. Int J Prosthodont. 2008;21(3):217–22.
Uzgur Z, Uzgur R, Çolak H, Ercan E, Dallı M. Analysis of Endodontic Complications Following Fixed Prosthodontic Rehabilitation. Int J Prosthodont. 2016;29(6):565–9.
Walther W. Risk of endodontic treatment after insertion of conical crown retained dentures: a longitudinal study. Endod Dent Traumatol. 1995;11(1):27–31.
Wolleb K, Sailer I, Thoma A, Menghini G, Hammerle CH. Clinical and radiographic evaluation of patients receiving both tooth- and implant-supported prosthodontic treatment after 5 years of function. Int J Prosthodont. 2012;25(3):252–9.
Zitzmann NU, Büren AV, Glenz F, Rohr N, Joda T, Zaugg LK. Clinical outcome of metal- and all-ceramic resin-bonded fixed dental prostheses. J Prosthodont Res. 2021;65(2):243–8.
Chmura Kraemer H, Periyakoil VS, Noda A. Kappa coefficients in medical research. Stat Med. 2002;21(14):2109–29.
Roediger M, Gersdorff N, Huels A, Rinke S. Prospective evaluation of zirconia posterior fixed partial dentures: four-year clinical results. Int J Prosthodont. 2010;23(2):141–8.
Frisk F, Hakeberg M. A 24-year follow-up of root filled teeth and periapical health amongst middle aged and elderly women in Göteborg. Sweden Int Endodontic J. 2005;38(4):246–54.
Patel S, Wilson R, Dawood A, Mannocci F. The detection of periapical pathosis using periapical radiography and cone beam computed tomography - part 1: pre-operative status. Int Endod J. 2012;45(8):702–10.
Lo Giudice R, Nicita F, Puleio F, Alibrandi A, Cervino G, Lizio AS, Pantaleo G. Accuracy of Periapical Radiography and CBCT in Endodontic Evaluation. Int J Dentistry. 2018;2018:2514243.
Brännström M, Nyborg H. Pulp reaction to a temporary zinc oxide/eugenol cement. J Prosthet Dent. 1976;35(2):185–91.
Baldissara P, Comin G, Martone F, Scotti R. Comparative study of the marginal microleakage of six cements in fixed provisional crowns. J Prosthet Dent. 1998;80(4):417–22.
Bagis B, Atilla P, Cakar N, Hasanreisoglu U. An immunohistochemical evaluation of cell adhesion molecules in human dental pulp after tooth preparation and application of temporary luting cements. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2009;107(1):137–44.
Lewinstein I, Chweidan H, Matalon S, Pilo R. Retention and marginal leakage of provisional crowns cemented with provisional cements enriched with chlorhexidine diacetate. J Prosthet Dent. 2007;98(5):373–8.
Pandey P, Mantri S, Bhasin A, Deogade SC. Mechanical Properties of a New Vinyl Polyether Silicone in Comparison to Vinyl Polysiloxane and Polyether Elastomeric Impression Materials. Contemp Clin Dent. 2019;10(2):203–7.
Langeland K, Langeland LK. Pulp reactions to crown preparation, impression, temporary crown fixation, and permanent cementation. J Prosthet Dent. 1965;15:129–43.
Rajasimhan NV, Jayaraman S, Ali DJ, Subramanian B. Evaluation of cytotoxicity levels of poly vinyl ether silicone, polyether, and poly vinyl siloxane impression materials: An in vitro study. J Indian Prosthodont Soc. 2019;19(4):332–7.
Roberta T, Federico M, Federica B, Antonietta CM, Sergio B, Ugo C. Study of the potential cytotoxicity of dental impression materials. Toxicol In Vitro. 2003;17(5–6):657–62.
Sydiskis RJ, Gerhardt DE. Cytotoxicity of impression materials. J Prosthet Dent. 1993;69(4):431–5.
Boraldi F, Coppi C, Bortolini S, Consolo U, Tiozzo R. Cytotoxic Evaluation of Elastomeric Dental Impression Materials on a Permanent Mouse Cell Line and on a Primary Human Gingival Fibroblast Culture. Materials (Basel). 2009;2(3):934–44.
Murray PE, Smith AJ, Windsor LJ, Mjör IA. Remaining dentine thickness and human pulp responses. Int Endod J. 2003;36(1):33–43.
Schmalz G. Pulp Reactions to Dental Materials. In: The Dental Pulp: Biology, Pathology, and Regenerative Therapies. edn. Edited by Goldberg M. Berlin, Heidelberg: Springer Berlin Heidelberg; 2014. p. 169–83.
Pameijer CH: 6 - Biocompatibility of luting cements for dental applications. In: Biocompatibility of Dental Biomaterials. edn. Edited by Shelton R: Woodhead Publishing; Sawston. 2017: 77–94.
Hill EE, Lott J. A clinically focused discussion of luting materials. Aust Dent J. 2011;56(Suppl 1):67–76.
Smith DC, Ruse ND. Acidity of glass ionomer cements during setting and its relation to pulp sensitivity. J Am Dent Assoc. 1986;112(5):654–7.
McCabe PS, Dummer PM. Pulp canal obliteration: an endodontic diagnosis and treatment challenge. Int Endod J. 2012;45(2):177–97.
Zilinskaite-Petrauskiene I, Haug SR: A Comparison of Endodontic Treatment Factors, Operator Difficulties and perceived Oral Health-Related Quality of Life between Elderly and Young Patients. J Endodontics 2021;47(12):1844–1853.
Cushen SE, Turkyilmaz I. Impact of operator experience on the accuracy of implant placement with stereolithographic surgical templates: an in vitro study. J Prosthet Dent. 2013;109(4):248–54.
Kozlovsky A, Rapaport A, Artzi Z. Influence of operator skill level on the clinical outcome of non-surgical periodontal treatment: a retrospective study. Clin Oral Investig. 2018;22(8):2927–32.
Sonkar J, Maney P, Yu Q, Palaiologou A. Retrospective study to identify associations between clinician training and dental implant outcome and to compare the use of MATLAB with SAS. Int J Implant Dent. 2019;5(1):28.
Alsulaimani RS, Al-Manei KK. S AA, AlAqeely RS, S AMA-S, E MA-M: Effects of Clinical Training and Case Difficulty on the Radiographic Quality of Root Canal Fillings Performed by Dental Students in Saudi Arabia. Iran Endod J. 2015;10(4):268–73.
Frankenberger R, Reinelt C, Petschelt A, Krämer N. Operator vs. material influence on clinical outcome of bonded ceramic inlays. Dent Mater. 2009;25(8):960–8.
Wisithphrom K, Murray PE, About I, Windsor LJ. Interactions between cavity preparation and restoration events and their effects on pulp vitality. Int J Periodontics Restorative Dent. 2006;26(6):596–605.
Whitworth JM, Walls AW, Wassell RW. Crowns and extra-coronal restorations: endodontic considerations: the pulp, the root-treated tooth and the crown. Br Dent J. 2002;192(6):315–20 323–317.
Li X, Hu L, Ma L, Chang S, Wang W, Feng Y, Xu Y, Hu J, Zhang C, Wang S. Severe periodontitis may influence cementum and dental pulp through inflammation, oxidative stress, and apoptosis. J Periodontol. 2019;90(11):1297–306.
Wan L, Lu HB, Xuan DY, Yan YX, Zhang JC. Histological changes within dental pulps in teeth with moderate-to-severe chronic periodontitis. Int Endod J. 2015;48(1):95–102.
Acknowledgements
Special thanks go to Dr. Abhishek Kumar, BDS, Ph.D., Karolinska Institute, for his feedback during the conduction of the study.
Funding
This project was registered and supported by the Research Center College of Dentistry (CDRC), King Saud University (FR0559). Open access funding provided by Karolinska Institute.
Author information
Authors and Affiliations
Contributions
CRediT roles: Conceptualization and design of the study: KKA and KA. Acquisition of the data: KKA, SA, GA, KA, and NA. Formal analysis: NA. Validation and visualization: KKA, KA, and NA. Writing the original draft: KKA and KA. Review and editing: KKA, SA, GA, KA, and NA. Project administration: KA. The author(s) read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Not applicable.
Consent for publication
All authors agreed to publish this work.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Additional file 1: Supplementary file 1.
Database search strategy.
Additional file 2: Supplementary file 2.
list of excluded articles.
Additional file 3: Supplementary file 3.
Quality assessment of the included RCT studies.
Additional file 4: Supplementary file 4.
Quality assessment of the included cohort studies.
Additional file 5: Supplementary file 5.
Funnel plots.
Additional file 6: Supplementary File 6.
GRADE assessment.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Al-Manei, K.K., Alzaidi, S., Almalki, G. et al. Incidence and influential factors in pulp necrosis and periapical pathosis following indirect restorations: a systematic review and meta-analysis. BMC Oral Health 23, 195 (2023). https://doi.org/10.1186/s12903-023-02826-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12903-023-02826-1