Abstract
Background
Cervical Disc Arthroplasty (CDA) seems to be an alternative to Anterior Cervical Decompression and Fusion (ACDF) and was developed to minimize the risk of Adjacent Segment Disease (ASD). The ROTAIO Cervical Disc Prosthesis represents a new unconstrained implant with a variable centre of rotation which should enable physiological facet-guided movement. The aim of this current study was to evaluate the clinical outcomes after arthroplasty using ROTAIO Cervical Disc Prosthesis.
Method
Twenty-seven female and 18 male patients (n = 45) with a mean age of 43.7 ± 7.8 years were prospectively followed up for a maximum of 24 month. Clinical outcomes were assessed by Neck Disability Index (NDI), visual analogue scale (VAS) scores for neck and arm pain, patients´ overall satisfaction and the usage of analgesics. Additionally, radiographic information including ROM of the functional spinal unit (FSU) and signs of adjacent segment disease were recorded.
Results
NDI and VAS scores showed significant improvement 6 months after surgery and at last follow-up (p < 0.001). Concerning overall satisfaction 95.7 % of the patients showed good to excellent results at the last visit and a significant reduction of analgesic usage was observed (p < 0.001). Radiographic measurements showed a mean increase of ROM up to 8.40° in the treated FSU at last follow-up (p < 0.001). No signs of anterior migration or dislocation of the prosthesis and no subsidence was recorded radiographically. There were no major complications and a low rate of secondary procedures (2.2 %).
Conclusion
In the 24-months follow-up the ROTAIO Cervical Disc Prosthesis provided excellent clinical and radiographical results and seems to be safe and effective for the treatment of symptomatic single-level degenerative disc disease.
Similar content being viewed by others
Explore related subjects
Find the latest articles, discoveries, and news in related topics.Background
Cervical spondylosis and degenerative disc disease may result in compression of one or more nerve roots and/or the spinal cord. If non-operative treatment fails, anterior cervical discectomy and fusion (ACDF) is a common treatment for cervical radiculopathy and myelopathy [1]. The procedure shows high patient satisfaction scores and a 95 % arthrodesis rate [2, 3]. Nevertheless the technique causes a loss of segmental motion and a possible need for reoperation because of pseudoarthrosis or adjacent segment degeneration (ASD). In recent years, cervical disc replacement (CDR) has become popular as an alternative to ACDF. Its theoretical and observed advantages include a more physiologic distribution of range of motion (ROM), reduced adjacent level stresses and a lowered rate of ASD. Currently, there are many commercially available artificial discs with different biomechanical properties [3–7].
This study reports the first results of a prospective, two-centre observational clinical trial on a newly developed artificial disc replacement device. There are currently no long term reports about the ROTAIO Cervical Disc Prosthesis (SIGNUS Medizintechnik GmbH, Alzenau, Germany). The study objective was to evaluate the clinical and radiological outcome after a maximum follow up of two years and to compare the results to available data of other artificial disc devices.
Methods
The observation was institutional review board approved (Ethics Commission, Medical University Innsbruck – Austria). All patients at the two centres who met the inclusion/exclusion criteria provided written informed consent and were included in the trial. Patient selection was based on the following inclusion and exclusion criteria. Inclusion criteria: (1) 18 to 65 years of age, (2) a single cervical disc disease between the level C3 and C7, (3) failed conservative treatment of at least 6 weeks or in case of progressive nerve root or spinal cord compression and (4) a minimum Neck Disability Index (NDI) of 15 points (30 %). Exclusion criteria: (1) cervical instability defined by translation on flexion–extension radiographs compared to the adjacent level, (2) non-mobility of the level, (3) fused adjacent levels, (4) neck pain as the solitary symptom, (5) prior surgery at target level, (6) metabolic bone disease or endocrine disorders, (7) pregnancy, (8) traumatic injury of spine, (9) HIV, metastatic cancer, presence of infection and (10) allergy to materials used in the device.
Demographic data
From January 2011 to December 2012, CDRs using the ROTAIO Cervical Disc Prosthesis were performed in 45 patients. All patients were successfully included, 28 patients had their last follow-up 12 months postoperatively and 17 patients were available for 24 months follow-up (mean 16.5 ± 5.8 month) . There were 27 female and 18 male patients with a mean age of 43.7 ± 7.1 years (range: 28–65 years). Seven patients were treated at C4/5, 27 patients at C5/6 and 11 patients at C6/7. All patients showed radiculopathic disorders, 4 of them in combination with mild signs of myelopathy.
Device design
The ROTAIO Cervical Disc Prosthesis (Fig. 1) is intended to be used for disc replacement in the cervical spine (C3-C7). In addition to restoring disc height, its primary function is to maintain physiological movement in the affected segment. The ROTAIO Cervical Disc Prosthesis represents a new unconstrained implant with a variable centre of rotation which should enable physiological facet-guided movement. For maximum coverage of the vertebral body end plates a total of 16 different sizes are available with various surface areas and heights. The prosthesis is pre-mounted on an insertion bracket to avoid the need for intraoperative assembly. Instruments specially developed for use with the implant system are available to ensure safe application.
The prosthesis consists of a superior and an inferior end plate (Titanium alloy to ISO 5832-3) on which the sliding elements (Cobalt-chrome alloy to ISO 5832-12) are anchored and secured by means of a fixation pin. The implant design provides an optimum fit to the anatomy of the intervertebral space. Assembly of ROTAIO is done in an axial direction. This has the effect that the slide plate is radially surrounded by the cover plate, which prevents the sliding plate from dislodgement. For optimum primary stabilization the end plates have a toothed surface. A special blasting treatment of the end plates increases surface area and thus bony integration.
Surgical technique
A standard right-sided anterior approach was routinely performed. The surgical technique was similar to those for a routine anterior cervical decompression. Implantation of the prosthesis was performed strictly following the manufacturer’s specifications and users´ manual. The endplate preparation was - corresponding to the design of the implant - performed using a high-speed drill followed by curetting the endplates with the manufacture´s trial-implant. The posterior longitudinal ligaments were completely removed in all cases. Any remaining superior posterior osteophytes overhanging the endplate were removed. All cases were treated by neurosurgical specialists who attended manufacture´s instruction lectures.
Clinical outcome
Clinical evaluations were performed using standardized questionnaires preoperatively, postoperatively before discharge, 3 to 6, 12 and 24 months after implantation. For the clinical outcome validated self-assessment outcome measures including neck disability index (NDI), patient satisfaction index (PSI), visual analogue scale (VAS) for neck and arm pain and patients overall satisfaction were recorded. Additionally the use of non-steroidal anti-inflammatory drugs (NSAID) was assessed. The NDI ranged from 0 to 50 and VAS scores from 0 to 10. Concerning PSI patients had to answer the question, “Would you like to have the same treatment for the same ailment again?” with (1) definitely yes, (2) probably yes, (3) probably not or (4) definitely not. The use of NSAIDs was defined as: (1) never, (2) seldom; 1 to 3 times a week, (3) often; 3 to 5 times a week or (4) always; 1 or more times a day. The preoperative scores were compared with the follow-up scores. To analyse overall satisfaction, the patient had to rate their improvement in (1) excellent, (2) significantly better, (3) good, (4) mild, (5) no improvement or (6) worsening of ailment. Complications were intended to be recorded during surgery and at final follow-up.
Radiographic outcome
Radiographic imaging observed the prosthesis position and function, possible signs of fusion or adjacent segment degeneration in neutral lateral and dynamic flexion and extension X-rays. To evaluate angular range of motion within the treated functional unit the Cobb-technique on dynamic lateral radiographs was used. For each measurement the mean of two observers were calculated and recorded for analysis. In four patients (index level C6/7) radiographic assessment was not possible because of prominent shoulders obscuring the images. All measurements were performed on source-digitalized images using IMPAX EE imaging software (AGFA HealthCare N.V., Belgium).
Statistical analysis
Statistical analyses were performed using IBM SPSS Statistics Version 20. The trial was designed to detect an absolute difference between pre- and postoperative data of one standard deviation with a power of 80 % at a two sided significance level (probability (p)-value) of 0.05 and a maximal dropout rate of 20 %. Comparisons were performed with the use of an unpaired t-test, or in case of nonparametric values with a Mann-Whitney-U test. Because data analysis did not show a statistically significant difference (p > 0.05) between the 12 months and the 24 months follow-up the results are presented combined under the term “last follow up”.
Results and discussion
Clinical evaluation
Neck disability index
At every time point postoperatively the patients were significantly improved from their preoperative NDI-scores (Table 1). The mean NDI had improved from 21.6 ± 9.8 preoperatively to 10.6 ± 8.3 at 3 to 6 months postoperative (p < 0.001) and to 10.5 ± 9.3 (p < 0.001) at last follow-up, with an average improvement rate of 51.5 %. A significant reduction of NDI scores was reached within 4 to 6 weeks after treatment and reached a plateau by 3 to 6 month after surgery.
Neck pain
Significant improvement of the neck pain score occurred early postoperatively to 6 months postoperatively and was maintained at last follow-up (Table 1). The mean preoperative score for neck pain was 5.3 ± 2.8, decreased to 2.4 ± 1.8 (p < 0.001) at the 3 to 6 month visit and was as well improved to 3.3 ± 2.7 (p < 0.001) at last follow-up. A worsening of neck pain during follow up was observed only in one patient (2.2 %).
Arm pain
The mean VAS score for arm pain improved significantly from 5.9 ± 3.1 preoperatively to 1.9 ± 1.8 (p < 0.001) at 3 to 6 months postoperatively and to 2.8 ± 2.7 at the last follow-up (p < 0.001) (Table 1).
Used NSAIDs
Concerning the use of NSAIDs, preoperatively 51.9 % of the patients “always”, 14.8 % “often”, 14.8 % “seldom” and 18.5 % “never” used painkillers (Table 1). At the 3 to 6 months follow up 48.9 % of the patients “never”, 23.3 % “seldom”, 16.3 % “often” and 9.3 % “always” used NSAIDs (p < 0.001). At the last follow-up a significant reduction was observed as well. 45.8 % of the patients rated their use of painkillers with “never”, 33.3 % with “seldom”, 8.3 % with “often” and 12.5 % with “always” (p < 0.001).
Overall success
The analyses of patient overall satisfaction (Table 2) at last follow-up showed good to excellent results in 95.7 % of the cases. In detail: 34.8 % showed excellent improvement. 43.5 % of the patients quoted the postoperative result as significantly better, 19.5 % rated their physical condition as good. 2.2 % (one patient) described no improvement of his ailments. No patient showed a worsening at last follow up. Concerning PSI at 3 to 6 months follow-up 65.9 % of the patients answered the question, “Would you like to have the same treatment for the same ailment again?” with “definitely yes” and 31.7 % of the patients with “probably yes”. One patient (2.2 %) answered the question with “probably not”.
Radiographic evaluation
Forty-one patients could be enrolled to radiological follow-up measurements (Fig. 2). There were no signs of anterior migration or dislocation of the prosthesis. Subsidence was defined as a decrease of more than 2 mm in functional spinal unit (FSU) from 3 months to last follow-up and was observed in no patient. The sagittal alignment was well restored in all cases. In one case (2.2 %) the radiographical one-year follow-up showed a bridging bone ventrally to the prosthesis and mild signs of adjacent segment disease like new anterior osteophytes (Fig. 3). Overall the analyses of dynamic flexion and extension X-rays showed no malfunction of the prosthesis. Concerning the ROM a significantly increased motion was detected at every time point. The mean cervical spine motion in flexion-extension at the index level improved from 6.3° ± 2.9° preoperatively to 8.4° ± 2.5° at 3 to 6 month after surgery (p < 0.001) and to 8.6° ± 2.8° at last follow-up (p < 0.001).
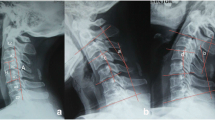
Flexion (a), neutral (b) and extension (c) x-ray showing the successful operation – especially the variable mechanical centre of rotation (CR) of the device moving forward and backward (white arrows) - of a ROTAIO cervical disc prosthesis at the level C6-C7 in a 52 years old female patient, 6 month after implantation
Complications
Self-limiting dysphagia was detected in three patients, which was probably due to traction or laryngeal nerve irritation during surgery. There was no other minor or major complication and no implant-related complication such as subsidence or fractured vertebrae.
Secondary procedures
In one male patient revision surgery at the index level was required (2.2 %). Caused by implantation of an undersized and too ventrally positioned prosthesis the patient suffered from increasing neck pain (Fig. 4). A few weeks after the 12 months follow-up the prosthesis was removed and the patient was treated with ACDF.
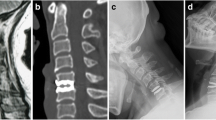
X-ray in neutral position (a: lateral view; b: anterior view) showing an undersized and too ventrally positioned ROTAIO cervical disc prosthesis at the level C5-C6 (white arrows) in a 38 years old male patient, 3 month after implantation. Within the first 12 month of follow up the patient suffered from progressive neck pain
Discussion
ACDF is a successful treatment and has shown high patient satisfaction rates for years. During the last two decades the effectiveness of CDR in treating cervical degenerative disc diseases has been analysed and in summary CDR after anterior neurological decompression may be deemed as an alternative to fusion in selected patients [5, 8–11]. Till now biomechanics, clinical and radiological effectiveness of most current available artificial discs prosthesis have been studied [1, 4, 5, 12–14]. As a newly established device the ROTAIO cervical disc prosthesis has only been in use for a few years. This is the first prospective study that analyses its clinical and radiographic reliability.
The results of this study demonstrated promising clinical and radiological outcomes. Concerning the NDI the observation showed a significant improvement of 51.5 % (p < 0.001) after implantation which correlates with present studies of other available cervical disc prosthesis [4–6]. Analysis of VAS showed a significant reduction of neck and arm pain early after surgery which might primarily be related to sufficient decompression during surgery and the in-hospital pain management. At last follow-up the improvement of arm and neck pain was significant as well and was also confirmed by a significant reduction of used NSAIDs. Regarding overall satisfaction 95.7 % of the patients achieved good to excellent improvement which is in-line with reports that observed the early results of other established cervical disc prostheses and also ACDFs [1, 3, 5, 8, 9, 11, 15–18]. High patient satisfaction rates were also reinforced by evaluating the PSI which has shown that 77.3 % of the patients would definitely have liked to have the same treatment for the same ailment again at the last follow up.
According to prior clinical trials of cervical arthroplasty subsequent secondary surgical intervention was defined as any revision, removal, reoperation or supplemental fixation [1, 4–6]. Until the last follow-up in one case (2.2 %) an increase of neck and arm pain was observed and subsequent secondary surgical intervention was required to remove a probably undersized prosthesis. As published by Sasso et al [1], Burkus et al [7] and Anderson and Hashimoto [19] for other disc prostheses the results of this study show a very low rate of secondary procedures and no prostheses related complications during or after surgery. According to Li et al [6] proper selection of patients, exact intraoperative strategy and adequate neural decompression is required to achieve satisfactory clinical outcomes.
Radiographic analysis showed no dislocation, anterior migration or malfunction of the prosthesis. As reported by Heller et al ROM values measured radiographically can be influenced by the radiographic technique itself, patient´s motivation or other – unknown – factors [5]. Nevertheless most authors observed motion preservation at the implanted level and characterized it as one of the fundamental benefits of CDR [1, 3, 4, 16, 20]. In the present study the prosthesis maintained physiological segmental motion with a mean flexion-extension difference of 8.4° in the 3 to 6 month visit and 8.6° at the last follow-up. According to Heller et al [4] an increasing ROM probably is a sign of less pain and higher patient´s motivation. Additionally a restored lordotic sagittal alignment was observed in all cases thus compared to other available CDR devices the ROTAIO prosthesis does not show a lordotic design like e.g. the Discover disc [6]. A fact that might be an advantage over prostheses like the Bryan disc, for which segmental kyphosis of the index level – persisting for more than 6 months postoperatively - was reported by Pickett et al [20]. The radiographic analysis also showed a low rate (2.2 %) of spontaneous fusion as measured by presence of bridging bone. This result may be a consequence of the preserved ROM but according to the works of Heller et al [5] it could also be influenced by patient selection. The authors describe that patients with significant spondylosis may have a greater likelihood of spontaneous fusion [5].
Adjacent segment disease (ASD) following uninstrumented ACDF has been reported to occur in 25 % of patients within 10 years and shows an incidence of 2.9 % per year [21, 22]. Based on the rationale that CDR helps to preserve the biomechanics of the spine in the index level and in addition also in the adjacent segments the potential for decreasing ASD was one of the most striking arguments for total disc arthroplasty. As reported by Riew et al [22] it is quite challenging to compare rates of radiographic or symptomatic ASD across the available literature because authors use substantially different definitions for their analysis and because there is no direct relationship between radiographic and symptomatic ASD. In the present study radiographic ASD was defined as new anterior osteophyte formation or enlargement of existing osteophytes and the rate of reoperation at the level directly adjacent to the treated level. In one case (2.2 %) anterior bridging bone at the index level and new osteophyte formations in the adjacent cranial level was observed. The low rate of ASD goes in line with the results of other authors and may be artificially low because of the definition as mentioned above and the follow up with a maximum period of just 24 month [1, 7, 22, 23] thus e.g. Park et al [24] reported that adjacent-level anterior disc space ossification (ALOD) occurs within the first 12 months after treatment and that patients with no ossification at 24 months are very unlikely to progress to advanced ossification. Furthermore - according to the work of Nunley et al [25] – over and above the device design there may be lots of different factors influencing the development of an ASD like e.g. age, sex, smoking habit or coexisting diseases.
Concerning the development of symptomatic ASD the results of this study show a mild increase of the mean VAS regarding neck pain from the 6 months visit to the last follow up ( 2.42 to 3.33; p > 0.05). Nevertheless this may be associated to the prosthesis or may be a part of degenerative spine´s natural history, long-term follow-up is necessary to evaluate if differences in adjacent segment motion and radiographical degeneration will affect the development of clinical ASD. To what extent the new design of the ROTAIO cervical disc prosthesis is able to reduce the risk of ASD and how far the device could protect the uncovertebral and facet joints from overload must be the aim of upcoming biomechanical analysis.
Overall new technology such as artificial disc devices requires long-term follow up to assess durability, the biologic compatibility and the response of the prosthesis to its environment. Typically failure of other joint arthroplasty does not occur before five to ten years after surgery. Therefore spinal disc prostheses similarly need to be assessed repetitively and for a longer period [1, 18]. Nevertheless based on clinical outcome according to the significant reduction of NDI and VAS scores, the high overall satisfaction and the evaluated safety of the device the ROTAIO prosthesis may be deemed as a good alternative for currently available cervical disc prostheses.
Limitations
There are some limitations in this study including the small number of patients, the lack of an ACDF control group and the limited follow up. Moreover the biomechanical behaviour of the ROTAIO disc in axial rotation and lateral bending has not been evaluated. Additionally the comparison with other kinds of artificial discs may provide further insights into the characteristics of different CDR devices.
Conclusions
The early results of this prospective, observational study show that cervical disc arthroplasty with the ROTAIO Cervical Disc Prosthesis seems to be safe and effective for the treatment of symptomatic single-level degenerative disc disease. Additionally patients had significantly improved NDI and VAS scores, showed a lower rate of NSAID-use and an excellent overall success at last follow-up. Thus, according to recent studies of other cervical disc prostheses the results confirm and support the role of total disc replacement as an alternative to ACDF, studies focusing on clinical long-term outcome and especially on preserving ASD are warranted.
Abbreviations
- CDA:
-
Cervical disc arthroplasty
- ACDF:
-
Anterior cervical decompression and fusion
- ASD:
-
Adjacent segment disease
- NDI:
-
Neck disability index
- VAS:
-
Visual analogue scale
- ROM:
-
Range of motion
- FSU:
-
Functional spinal unit
- C1-n:
-
Cervical vertebra 1-n
- NSAID:
-
Non-steroidal anti-inflammatory drugs
- CDR:
-
Cervical disc replacement
- PSI:
-
Patient satisfaction index
References
Sasso RC, Anderson PA, Riew KD, Heller JG. Results of cervical arthroplasty compared with anterior discectomy and fusion: four-year clinical outcomes in a prospective, randomized controlled trial. Orthopedics. 2011;34:889.
Fraser JF, Härtl R. Anterior approaches to fusion of the cervical spine: a metaanalysis of fusion rates. J Neurosurg Spine. 2007;6:298–303.
Upadhyaya CD, Wu JC, Trost G, Haid RW, Traynelis VC, Tay B, et al. Analysis of the three United States Food and Drug Administration investigational device exemption cervical arthroplasty trials. J Neurosurg Spine. 2012;16:216–28.
Phillips FM, Lee JY, Geisler FH, Cappuccino A, Chaput CD, DeVine JG, et al. A prospective, randomized, controlled clinical investigation comparing PCM cervical disc arthroplasty with anterior cervical discectomy and fusion. 2-year results from the US FDA IDE clinical trial. Spine (Phila Pa 1976). 2013;38:E907–18.
Heller JG, Sasso RC, Papadopoulos SM, Anderson PA, Fessler RG, Hacker RJ, et al. Comparison of BRYAN cervical disc arthroplasty with anterior cervical decompression and fusion: clinical and radiographic results of a randomized, controlled, clinical trial. Spine (Phila Pa 1976). 2009;34:101–7.
Li J, Liang L, Ye XF, Qi M, Chen HJ, Yuan W. Cervical arthroplasty with Discover prosthesis: clinical outcomes and analysis of factors that may influence postoperative range of motion. Eur Spine J. 2013;22:2303–9.
Burkus JK, Haid RW, Traynelis VC, Mummaneni PV. Long-term clinical and radiographic outcomes of cervical disc replacement with the Prestige disc: results from a prospective randomized controlled clinical trial. J Neurosurg Spine. 2010;13:308–18.
Sasso RC, Smucker JD, Hacker RJ, Heller JG. Artificial disc versus fusion: a prospective, randomized study with 2-year follow-up on 99 patients. Spine (Phila Pa 1976). 2007;32:2933–40.
Nabhan A, Ahlhelm F, Shariat K, Pitzen T, Steimer O, Steudel WI, et al. The ProDisc-C prosthesis: clinical and radiological experience 1 year after surgery. Spine (Phila Pa 1976). 2007;32:1935–41.
Garrido BJ, Taha TA, Sasso RC. Clinical outcomes of Bryan cervical disc arthroplasty a prospective, randomized, controlled, single site trial with 48-month follow-up. J Spinal Disord Tech. 2010;23:367–71.
Goffin J, Van CF, van LJ, Casey A, Kehr P, Liebig K, et al. Intermediate follow-up after treatment of degenerative disc disease with the Bryan Cervical Disc Prosthesis: single-level and bi-level. Spine (Phila Pa 1976 ). 2003;28:2673–8.
Goffin J, van LJ, Van CF, Lipscomb B. A clinical analysis of 4- and 6-year follow-up results after cervical disc replacement surgery using the Bryan Cervical Disc Prosthesis. J Neurosurg Spine. 2010;12:261–9.
Lee MJ, Dumonski M, Phillips FM, Voronov LI, Renner SM, Carandang G, et al. Disc replacement adjacent to cervical fusion: a biomechanical comparison of hybrid construct versus two-level fusion. Spine (Phila Pa 1976). 2011;36:1932–9.
Phillips FM, Tzermiadianos MN, Voronov LI, Havey RM, Carandang G, Dooris A, et al. Effect of two-level total disc replacement on cervical spine kinematics. Spine (Phila Pa 1976). 2009;34:E794–9.
Amit A, Dorward N. Bryan cervical disc prosthesis: 12-month clinical outcome. Br J Neurosurg. 2007;21:478–84.
Boselie TF, Willems PC, van MH, de Bie RA, Benzel EC, van SH. Arthroplasty versus fusion in single-level cervical degenerative disc disease: a cochrane review. Spine (Phila Pa 1976 ). 2013;38:E1096–107.
Goffin J, Casey A, Kehr P, Liebig K, Lind B, Logroscino C, et al. Preliminary clinical experience with the Bryan Cervical Disc Prosthesis. Neurosurgery. 2002;51:840–5.
Zigler JE, Delamarter R, Murrey D, Spivak J, Janssen M. ProDisc-C and anterior cervical discectomy and fusion as surgical treatment for single-level cervical symptomatic degenerative disc disease: five-year results of a Food and Drug Administration study. Spine (Phila Pa 1976). 2013;38:203–9.
Anderson PA, Hashimoto R. Total disc replacement in the cervical spine: a systematic review evaluating long-term safety. Evid Based Spine Care J. 2012;3:9–18.
Pickett GE, Mitsis DK, Sekhon LH, Sears WR, Duggal N. Effects of a cervical disc prosthesis on segmental and cervical spine alignment. Neurosurg Focus. 2004;17:E5.
Hilibrand AS, Carlson GD, Palumbo MA, Jones PK, Bohlman HH. Radiculopathy and myelopathy at segments adjacent to the site of a previous anterior cervical arthrodesis. J Bone Joint Surg Am. 1999;81:519–28.
Riew KD, Schenk-Kisser JM, Skelly AC. Adjacent segment disease and C-ADR: promises fulfilled? Evid Based Spine Care J. 2012;3:39–46.
Mummaneni PV, Burkus JK, Haid RW, Traynelis VC, Zdeblick TA. Clinical and radiographic analysis of cervical disc arthroplasty compared with allograft fusion: a randomized controlled clinical trial. J Neurosurg Spine. 2007;6:198–209.
Park JB, Watthanaaphisit T, Riew KD. Timing of development of adjacent-level ossification after anterior cervical arthrodesis with plates. Spine J. 2007;7:633–6.
Nunley PD, Jawahar A, Kerr III EJ, Gordon CJ, Cavanaugh DA, Birdsong EM, et al. Factors affecting the incidence of symptomatic adjacent-level disease in cervical spine after total disc arthroplasty: 2- to 4-year follow-up of 3 prospective randomized trials. Spine (Phila Pa 1976). 2012;37:445–51.
Acknowledgement
The authors declare that there are no conflicts of interest and no funds (from National Institutes of Health; Welcome Trust; Howard Hughes Medical Institute; or others) have been received in support of this study.
Author information
Authors and Affiliations
Corresponding author
Additional information
Competing interests
One of the authors is a consultant to SIGNUS Medizintechnik GmbH. The authors declare that no funds have been received in support of this study. No benefits in any form have been or will be received from a commercial party related directly or indirectly to the subject of this article.
Authors’contributions
JO, JL, SH, GAS, CT, CL have made substantial contributions to conception and design. All authors read and approved the final manuscript
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated.
About this article
Cite this article
Obernauer, J., Landscheidt, J., Hartmann, S. et al. Cervical arthroplasty with ROTAIO® cervical disc prosthesis: first clinical and radiographic outcome analysis in a multicenter prospective trial. BMC Musculoskelet Disord 17, 11 (2016). https://doi.org/10.1186/s12891-016-0880-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12891-016-0880-7