Abstract
Background
Respiratory medicine (RM) and palliative care (PC) physicians’ management of chronic breathlessness in advanced chronic obstructive pulmonary disease (COPD), fibrotic interstitial lung disease (fILD) and lung cancer (LC), and the influence of practice guidelines was explored via an online survey.
Methods
A voluntary, online survey was distributed to RM and PC physicians via society newsletter mailing lists.
Results
450 evaluable questionnaires (348 (77%) RM and 102 (23%) PC) were analysed. Significantly more PC physicians indicated routine use (often/always) of opioids across conditions (COPD: 92% vs. 39%, fILD: 83% vs. 36%, LC: 95% vs. 76%; all p < 0.001) and significantly more PC physicians indicated routine use of benzodiazepines for COPD (33% vs. 10%) and fILD (25% vs. 12%) (both p < 0.001). Significantly more RM physicians reported routine use of a breathlessness score (62% vs. 13%, p < 0.001) and prioritised exercise training/rehabilitation for COPD (49% vs. 7%) and fILD (30% vs. 18%) (both p < 0.001). Overall, 40% of all respondents reported reading non-cancer palliative care guidelines (either carefully or looked at them briefly). Respondents who reported reading these guidelines were more likely to: routinely use a breathlessness score (χ2 = 13.8; p < 0.001), use opioids (χ2 = 12.58, p < 0.001) and refer to pulmonary rehabilitation (χ2 = 6.41, p = 0.011) in COPD; use antidepressants (χ2 = 6.25; p = 0.044) and refer to PC (χ2 = 5.83; p = 0.016) in fILD; and use a handheld fan in COPD (χ2 = 8.75, p = 0.003), fILD (χ2 = 4.85, p = 0.028) and LC (χ2 = 5.63; p = 0.018).
Conclusions
These findings suggest a need for improved dissemination and uptake of jointly developed breathlessness management guidelines in order to encourage appropriate use of existing, evidence-based therapies. The lack of opioid use by RM, and continued benzodiazepine use in PC, suggest that a wider range of acceptable therapies need to be developed and trialled.
Similar content being viewed by others
Background
Breathlessness is a distressing, highly prevalent symptom of advanced chronic respiratory diseases and lung cancer (LC) [1,2,3,4]. It is associated with social isolation [5], high healthcare costs [6, 7] and poor prognosis [8]. Chronic or refractory breathlessness is defined as disabling breathlessness which persists despite optimal disease management [9]. It may be episodic or persistent, and usually becomes increasingly severe with disease progression and at end of life [10]. Management options include non-pharmacological interventions e.g. exercise/rehabilitation, use of a handheld fan, breathing control techniques and walking aids [11]. Pharmacological treatment options are limited to moderate evidence in support of opioids [12, 13]. Thus, breathlessness often remains under-recognised and undertreated.
Recent multinational and national surveys have highlighted considerable variation in treatment approaches for breathlessness between respiratory medicine (RM) and palliative care (PC) physicians [14], and in the approach to breathlessness management in malignant versus non-malignant disease [15]. Barriers to effective management include lack of clinician knowledge and experience [16,17,18]. Furthermore, a survey of 174 Polish Respiratory Society members suggested an inverse relationship between knowledge of PRS guidelines and treatments recommended for people with chronic obstructive pulmonary disease (COPD) [15]. Thus, the aim of this survey was to describe and compare the management practices of RM and PC physicians across Europe for breathlessness in chronic lung diseases and to explore the relationship between the knowledge of guidelines and clinical practice.
Methods
Study design and participants
This survey was conducted as part of the BETTER-B research programme on breathlessness in advanced diseases. An anonymous, voluntary online survey was designed, in English, for distribution to physicians working in RM and PC across Europe. Survey design was informed by previous surveys [14, 15, 17, 18] and current literature [11, 12, 19]. Three case vignettes were developed: one patient with advanced COPD, one with progressive fibrotic interstitial lung disease (fILD) (a case of advanced idiopathic pulmonary fibrosis (IPF)), and one patient with LC (see Additional file 1). Each patient presented with mMRC scale 3–4 breathlessness (3 = Stops for breath after walking 100 yards, or after a few minutes on level ground; 4 = Too breathless to leave the house, or breathless when dressing/undressing) [20] despite optimal management of the underlying disease. Current anxiety or depression was not indicated in any of the three vignettes. The survey focused on: respondent demographics; awareness and knowledge of local, national or international guidelines/recommendations on palliative care for non-malignant lung diseases; use of a breathlessness score in clinical practice; non-pharmacological management strategies; pharmacological management strategies; and attitudes towards referral to PC. Respondents were asked to consider how they would manage each case vignette, or similar patients, by rating management/treatment options.
The survey was piloted on 20 international expert RM and PC physicians (data not included in the final analyses). Additionally, 10 in-depth interviews were performed among physicians from Germany, Italy, Poland and the UK to minimise measurement error and ensure user acceptability, face validity and comprehensiveness. The survey was launched on 23/04/2019 and closed on 06/08/2019. Survey links were disseminated via newsletter mailing lists to members of the European Respiratory Society (ERS), the European Association for Palliative Care (EAPC) and the British Thoracic Society (BTS), and as a news item feature on the Palliative Care Formulary (PCF) website. Society members were further encouraged to participate through social media posts, blogs, and dissemination among linked national societies and conferences. Approval was granted by the King’s College London (UK) Research Ethics Committee (MRA-18/19-11108). Physicians were informed that by completing the survey, they provided informed consent for use of their anonymised data.
Analysis
Analyses were performed using IBM SPSS Statistics version 25.0 and STATISTICA StatSoft version 12.0. Categories were collapsed or dichotomized for some analyses. Pearson’s chi-square test, Yates’ correction, or Fisher’s exact test were used to compare frequencies and proportions between RM and PC physicians. As there was no significant difference between RM and PC physicians in their knowledge of guidelines on PC for non-malignant lung diseases, the impact of guideline knowledge on clinical practice was analysed as one sample. Answers were dichotomised as: 1—yes, I know of them and have read them carefully and yes, I know of them but have only looked at them briefly versus 2—the three other response options (see Additional file 1). Logistic regressions were carried out to evaluate which respondent characteristics (from Table 1) were independently associated with dichotomised knowledge of guidelines. Variables which presented statistical significance in the univariate analyses (setting of practice, number of COPD patients seen, number of fILD patients seen and number of LC patients seen) were subsequently entered into a multivariate logistic regression model. Significant associations are presented as odds ratios (OR), their respective 95% confidence intervals (CI) and significance levels. Further, knowledge of guidelines was transformed into a 5-point Likert scale: 1—I know that no such guidelines/recommendations exist; 2—I’m not sure if such guidelines/recommendations exist or not; 3—Yes, I know of them but have not read them; 4—Yes, I know of them but have only looked at them briefly; and 5—Yes, I know of them and have read them carefully. Mann–Whitney-Wilcoxon test were used to compare groups for ordinal variables. Kruskal–Wallis test was used to assess differences in ordinal data among three or more independently sampled groups with post hoc Dunn’s multiple comparison.
Results
Respondent characteristics
The survey was opened by 1082 recipients, commenced by 764 respondents with 514 complete and 250 partial responses. Following exclusions, 450 responses were included in the final analyses with 348 (77%) RM and 102 (23%) PC physicians (Table 1 and Fig. 1). RM physicians practiced across 31 and PC across 13 European countries, with largest representation from the UK (18% and 36%, respectively). A further 59 (13%) responses were from non-European countries including India, USA and several South American countries. PC and RM physicians differed according to years in their specialty, settings in which they work, and numbers of patients seen.
Non-pharmacological management of breathlessness
For chronic breathlessness in COPD and fILD, RM physicians most commonly recommended (“often or always”) physical activity (COPD 71%, fILD 61%), pulmonary rehabilitation (COPD 67%, fILD 56%) and breathing techniques (COPD 58%, fILD 42%). By contrast, PC physicians favoured breathing techniques (COPD 73%, fILD 69%), body positioning (COPD 70%, fILD 68%) and the handheld fan (COPD 66%, fILD 64%).
In LC, PC physicians most commonly recommended body positioning, which was selected by significantly fewer RM physicians (72% vs. 32%, p < 0.001). The handheld fan was also more frequently selected by PC physicians with 57% of RM physicians reporting that they “never” recommend the handheld fan in LC. Half of physicians from both specialties reported only “rarely or sometimes” recommending physical activity (RM 52%, PC 54%, p = 0.453) and “never” recommending pulmonary rehabilitation (RM 49%, PC 55%, p = 0.602) for breathlessness in LC. Meditative and cognitive interventions were less commonly recommended (“often or always”) across all three cases by both PC and RM physicians (see Table 2).
Pharmacological management of breathlessness
Opioids were more commonly recommended “often or always” than benzodiazepines or antidepressants by both RM and PC physicians for all three cases (Table 3).
However, opioids were selected “often or always” by significantly more PC in both COPD (92% vs. 39%, p < 0.001) and fILD (83% vs. 36%, p < 0.001). This was also observed for LC, although the difference was smaller (95% vs. 76%, p < 0.001). Conversely, larger proportions of RM physicians stated they would never initiate opioids in severe COPD (16% vs. 1%) or fILD (18% vs. 1%). The three commonest reasons selected by RM physicians for not, or only rarely, initiating opioids for patients with severe COPD or fILD were: risk of respiratory depression (COPD 20%, fILD 14%), risk of unpleasant side-effects (COPD 15%, fILD 12%) and insufficient knowledge or experience in prescribing opioids in these patients (15% for both COPD and fILD). Benzodiazepines were less frequently selected by RM physicians across cases. Specifically, one-third (32%) stated that they would “never” select benzodiazepines for COPD and fILD. Conversely, 33% and 25% of PC physicians would “often or always” recommend benzodiazepines for COPD and fILD respectively (compared to RM: 10% and 12%, p < 0.001). One fifth or fewer physicians from both specialties would routinely recommend antidepressants in the management of breathlessness, across all three cases. Among those who would consider antidepressants for COPD, 30% of RM and 47% of PC physicians, stated they would not use antidepressants solely for the management of breathlessness. When used, selective serotonin reuptake inhibitors (SSRIs) were more commonly selected than other classes of antidepressants by more than half of RM physicians (Table 4). PC physicians favoured both SSRIs and noradrenergic and specific serotonergic antidepressant (NaSSAs), such as mirtazapine.
Prioritised treatment and referrals to palliative care
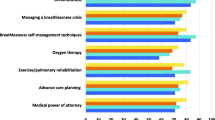
RM physicians most commonly prioritised exercise/rehabilitation for COPD (49%), and drug treatment for LC (58%) (Table 5).
For fILD, their prioritised treatment was more evenly balanced between drug treatment (24%), exercise/rehabilitation (30%), and re-assessment of oxygen prescription (24%). PC physicians prioritised drug treatment regardless of diagnosis but especially for LC (75%). Across all three cases, most RM physicians stated that they would refer such patients to PC to provide ongoing palliation of breathlessness and other symptoms or for advice about palliation of breathlessness (COPD 73%, fILD 71%, LC 93%).
Knowledge of PC practice guidelines and use of a breathlessness score
Only 15% of RM, and 17% of PC physicians reported that they knew of and had read carefully any local, national or international guidelines or recommendations on PC for non-malignant respiratory diseases (Table 6). Where examples of guidelines were given, these were predominantly national guidelines (e.g. British Thoracic Society Guidelines for Management of COPD, Spanish COPD Guidelines (GesEPOC), Danish respiratory society position paper on palliative care in patients with chronic progressive non-malignant lung diseases). Almost half of both specialties responded that no such guidelines/recommendations existed, or that they were unsure whether guidelines existed. Over two-thirds (62%) of RM physicians reported routinely using a breathlessness score in clinical practice (often or always) compared to 13% of PC physicians.
Relationship between knowledge of guidelines and clinical practice
Respondents who treated a higher number of COPD patients a year reported greater knowledge of clinical guidelines for PC in non-malignant lung disease (read them either carefully or looked at them briefly) (OR 1.45; [CI 1.18–1.79]; p < 0.001). Physicians who read guidelines either carefully or looked at them briefly more often used a breathlessness score routinely in clinical practice (χ2 = 13.8; p < 0.001) and more often reported routine use of opioids to relieve chronic breathlessness in severe COPD (χ2 = 12.58; p < 0.001). They also more frequently used the handheld fan in COPD (χ2 = 8.75; p = 0.003), fILD (χ2 = 4.85; p = 0.028) and LC (χ2 = 5.63; p = 0.018). Moreover, they were more open to refer breathless people with fILD to PC (χ2 = 5.83; p = 0.016), and to use pulmonary rehabilitation in COPD (χ2 = 6.41, p = 0.011). The subsequent comparison between knowledge of guidelines (transformed into Likert scale) and clinical practice supported these relationships (Fig. 2). There was no clear relationship between knowledge of guidelines and treatment with benzodiazepines and antidepressants. However, for fILD antidepressants were used more frequently by respondents who reported they had read guidelines or looked at them briefly (χ2 = 6.25; p = 0.044).
Relationship between the knowledge of guidelines/recommendations on palliative care for non-malignant lung diseases and the routine use of a breathlessness score in clinical practice. Legend: Knowledge of guidelines was evaluated by a 5-point Likert scale: 1 - I know that no such guidelines/recommendations exist; 2 - I’m not sure if such guidelines/recommendations exist or not; 3 - Yes, I know of them but have not read them; 4 - Yes, I know of them but have only looked at them briefly; 5 - Yes, I know of them and have read them carefully. Kruskal-Wallis test was implemented to assess the difference in ordinal data among all independently sampled groups, with subsequent post-hoc test (Dunn’s test) for multiple comparison
Discussion
This is the first multinational survey to compare the experiences and attitudes of RM and PC physicians in the management of chronic refractory breathlessness in advanced COPD, fILD and LC. The responses reveal significant differences in choice of management strategy by specialty and by diagnosis. Our findings suggest a relationship between knowledge of clinical guidelines and routine use of the handheld fan, opioids, and physical activity/pulmonary rehabilitation in COPD, all of these being interventions for which there is a strong evidence base [11, 12, 21]. Although we cannot interpret this association as causality, it is possible that physicians who read guidelines are more likely to implement the evidence-based interventions recommended therein.
Our survey, in common with findings of previous national and international surveys [14, 15], found that the majority of RM physicians focus on pulmonary rehabilitation and physical activity as treatment options for breathlessness in COPD, whereas PC physicians prioritize drug treatment, most commonly an opioid. Promotion of physical activity and pulmonary rehabilitation by RM physicians is in line with international COPD practice guidelines informed by a robust evidence base [21], and indeed pulmonary rehabilitation was more likely to be favoured by respondents who reported knowledge of clinical guidelines. RM physicians prioritised drug treatment only in the LC case, and almost one fifth stated that they would never initiate opioids in severe COPD or fILD. This reluctance to initiate opioids is somewhat at odds with moderate evidence in support of low-dose opioids for chronic breathlessness in malignant and non-malignant disease [12, 13], and recommendations in current prominent international and national practice guidelines [22,23,24]. Again, physicians who read guidelines either carefully or looked at them briefly more often reported routine use of opioids to relieve chronic breathlessness in severe COPD. As in prior surveys [14, 15, 17, 18], RM physicians identified risk of respiratory depression to be the principal barrier to opioid prescription.
Over one-third of both PC and RM physicians reported they would routinely initiate benzodiazepines for breathlessness in LC. A quarter of PC physicians and 12% of RM physicians also reported they would routinely recommend benzodiazepines for breathlessness in fILD and 33% of PC physicians would routinely recommend also for COPD. Trials for benzodiazepines have failed to provide evidence of benefit [19], therefore, it is concerning that our survey indicates continued routine use despite this lack of evidence. In COPD, use of benzodiazepines is contrary to international practice guidelines [22]. Recent evidence suggesting an association between higher-dose benzodiazepines and mortality in fILD should also prompt caution [25]. However, guidance documents on the use of benzodiazepines for breathlessness are in some cases conflicting and at odds with current evidence. The Global Initiative for Chronic Obstructive Lung Disease (GOLD) stipulates that there is no evidence for benzodiazepine use for breathlessness in COPD [22], but benzodiazepines remain a recommended treatment option for breathlessness at rest, alone or in combination with opioids, in UK National Institute for Health and Care Excellence (NICE) Guidelines on Idiopathic Pulmonary Fibrosis [26]. Prominent PC guidelines for advanced cancer also recommend benzodiazepines for intractable breathlessness, but only in combination with opioids, and where there is co-existent anxiety. A presence of anxiety was not included in any of the case vignettes presented in our survey, however it is possible that co-existent anxiety was considered by respondents when indicating their use of benzodiazepines [27]. Without consistent, evidence-based guidelines, it is difficult, even for physicians who read all available guidelines carefully, to implement best practice across all disease settings.
Consistent with current good practice—given the lack of evidence to support their use—routine use of antidepressants in the management of breathlessness were infrequent in our survey in both RM and PC physicians, and across conditions. Moreover, one third of RM and almost half of PC physicians stated they would not use antidepressants solely for the management of breathlessness. We found no clear relationship between knowledge of guidelines and use of antidepressants. Despite promising effects in pilot work [28,29,30], the antidepressant sertraline did not provide any benefit over placebo in the symptomatic relief of breathlessness in a recent double-blind randomized trial [16]. The NaSSA mirtazapine is a promising candidate for the palliation of breathlessness, with definitive randomized controlled trials awaited to determine its efficacy and safety in advanced disease [31,32,33].
Although PC physicians prioritised drug treatments, our results show they are also open to a wider range of non-pharmacological, self-help interventions including breathing techniques, anxiety management and the handheld fan compared to RM physicians. This is in keeping with guidance for the management of breathlessness in advanced disease which recommend a combination of non-pharmacological and pharmacological interventions, with an emphasis on self-help strategies [11, 34, 35]. The handheld fan, facial cooling, mobility aids and neuromuscular electrical stimulation are all evidence-based non-pharmacological interventions for chronic refractory breathlessness [11]. Notably, more than half of RM physicians reported never recommending use of a handheld fan in breathless patients irrespective of diagnosis. This is perhaps surprising given the evidence supporting a role for this simple portable intervention, which has no major side-effects, in reducing recovery time from episodic breathlessness [36]. Better knowledge of clinical practice guidelines was related to more frequent use of the handheld fan in breathless people across conditions. It is possible that non-pharmacological treatment choices are influenced by the settings in which physicians predominantly work as well local availability of services.
Encouragingly, most RM physicians reported they would refer breathless patients with non-malignant lung disease to PC services. Randomised trial and meta-analysis evidence indicates that integrated, holistic breathlessness services reduce patient distress and may improve psychological outcomes [35, 37,38,39,40,41]. The COVID-19 pandemic, has highlighted, more than ever, the importance of integrated care. The breathlessness management section of the COVID-19 rapid guideline for managing symptoms (including at the end of life) in the community, is a great example of the benefits of cross-specialty working and knowledge exchange [42].
Although our findings suggest a relationship between knowledge of clinical guidelines and routine use of a breathlessness score, use of a breathlessness score is by no means adopted as routine practice, especially among PC physicians. Scoring and documentation of breathlessness is an important part of clinical assessment providing insights into disease burden and prognosis not captured by lung function alone [43]. In our survey, 62% of RM physicians reported using a breathlessness score in routine clinical practice, compared to only 13% of PC physicians. One potential explanation for this difference is that use of the mMRC Dyspnoea Score and/or COPD Assessment Test score is advocated by GOLD in the refined “ABCD” assessment of COPD disease severity [22], for which there is no counterpart in PC medicine. It is also possible that PC physicians assess breathlessness as part of a holistic assessment using tools such as the Integrated Palliative Care Outcome Scale [44] or Edmonton Symptom Assessment Scale [45] rather than a breathlessness score.
Strengths and limitations
This multinational survey was the first to explore the management practices of physicians in RM and PC across a range of chronic advanced lung diseases. Particular attention was paid to non-malignant diseases, including ILD for which the evidence base for symptom management is poor and PC expertise remains conspicuously inaccessible [2]. However, our fILD case considered a patient with idiopathic pulmonary fibrosis specifically, thus the findings may not be generalizable to non-fibrotic ILD. The survey was distributed via society newsletter mailing lists, however as these lists contain non-physician members (e.g. researchers, students, academics, allied health professionals) it is difficult to calculate the exact response rate for our survey or consider the characteristics of non-responders. Responder bias therefore needs to be considered. Unfortunately, there was a high number of incomplete questionnaires (n = 250) which could not be included in the analysis as responses allowing identification of respondents’ specialty were missing. However, the analysed sample size is comparable to other recent surveys.(14, 15) The majority of responses were from the UK and therefore our findings may not represent practice across different healthcare systems. Finally, self-reported knowledge and attitudes to management of case vignettes may not reflect actual clinical practice.
Conclusions
This survey of RM and PC physicians reveals substantial differences in the approach to clinical management of chronic refractory breathlessness between specialties, and between malignant and non-malignant lung disease. The findings suggest that knowledge of clinical practice guidelines influences evidence-based treatment choices, but there was also evidence of deviation from current recommendations, particularly related to the use of benzodiazepines. There is a need for randomized clinical trials of new drug treatments, including antidepressants, to clarify clinical efficacy and reduce ambiguities in current practice recommendations. Most RM physicians welcomed the opportunity for shared care with PC colleagues. Together, these findings emphasise the need for improved dissemination and uptake of joint, evidence-based clinical practice guidelines, developed and ratified by major palliative care and respiratory societies, to reduce the significant burden of chronic refractory breathlessness in advanced respiratory disease.
Availability of data and materials
The datasets used and/or analysed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- BTS:
-
British Thoracic Society
- CI:
-
Confidence Interval
- COPD:
-
Chronic Obstructive Pulmonary Disease
- EAPC:
-
European Association of Palliative Care
- ERS:
-
European Respiratory Society
- fILD:
-
Fibrotic Interstitial Lung Disease
- GOLD:
-
The Global Initiative for Chronic Obstructive Lung Disease
- ILD:
-
Interstitial Lung Disease
- IPF:
-
Idiopathic Pulmonary Fibrosis
- LC:
-
Lung Cancer
- mMRC:
-
Modified Medical Research Council Dyspnea Scale
- NaSSA:
-
Noradrenergic and Specific Serotonergic Antidepressant
- NICE:
-
National Institute for Health and Care Excellence
- OR:
-
Odds Ratio
- RM:
-
Respiratory Medicine
- PC:
-
Palliative Care
- PCF:
-
Palliative Care Formulary
- SSRI:
-
Selective Serotonin Reuptake Inhibitor
- UK:
-
United Kingdom
- USA:
-
Unites States of America
References
Edmonds P, Karlsen S, Khan S, Addington-Hall J. A comparison of the palliative care needs of patients dying from chronic respiratory diseases and lung cancer. Palliat Med. 2001;15(4):287–95.
Kreuter M, Bendstrup E, Russell AM, Bajwah S, Lindell K, Adir Y, et al. Palliative care in interstitial lung disease: living well. Lancet Respir Med. 2017;5(12):968–80.
Wysham NG, Cox CE, Wolf SP, Kamal AH. Symptom burden of chronic lung disease compared with lung cancer at time of referral for palliative care consultation. Ann Am Thorac Soc. 2015;12(9):1294–301.
Currow DC, Abernethy AP, Allcroft P, Banzett RB, Bausewein C, Booth S, et al. The need to research refractory breathlessness. Eur Respir J. 2016;47(1):342–3.
Gysels M, Higginson IJ. Access to services for patients with chronic obstructive pulmonary disease: the invisibility of breathlessness. J Pain Symptom Manage. 2008;36(5):451–60.
Dzingina MD, Reilly CC, Bausewein C, Jolley CJ, Moxham J, McCrone P, et al. Variations in the cost of formal and informal health care for patients with advanced chronic disease and refractory breathlessness: a cross-sectional secondary analysis. Palliat Med. 2017;31(4):369–77.
Hutchinson A, Pickering A, Williams P, Bland JM, Johnson MJ. Breathlessness and presentation to the emergency department: a survey and clinical record review. BMC Pulm Med. 2017;17(1):53.
Nishimura H, Tokuyama K, Arakawa H, Ohki Y, Sato A, Kato M, et al. Airway responsiveness and airway remodeling after chronic exposure to procaterol and fenoterol in guinea pigs in vivo. Int Arch Allergy Immunol. 2002;129(4):320–6.
Johnson MJ, Yorke J, Hansen-Flaschen J, Lansing R, Ekstrom M, Similowski T, et al. Towards an expert consensus to delineate a clinical syndrome of chronic breathlessness. Eur Respir J. 2017;49(5):1602277.
Weingaertner V, Scheve C, Gerdes V, Schwarz-Eywill M, Prenzel R, Bausewein C, et al. Breathlessness, functional status, distress, and palliative care needs over time in patients with advanced chronic obstructive pulmonary disease or lung cancer: a cohort study. J Pain Symptom Manage. 2014;48(4):569–81.
Booth S, Moffat C, Burkin J, Galbraith S, Bausewein C. Nonpharmacological interventions for breathlessness. Curr Opin Support Palliat Care. 2011;5(2):77–86.
Barnes H, McDonald J, Smallwood N, Manser R. Opioids for the palliation of refractory breathlessness in adults with advanced disease and terminal illness. Cochrane Database Syst Rev. 2016;3:CD011008.
Ekstrom M, Bajwah S, Bland JM, Currow DC, Hussain J, Johnson MJ. One evidence base; three stories: do opioids relieve chronic breathlessness? Thorax. 2018;73(1):88–90.
Smallwood N, Currow D, Booth S, Spathis A, Irving L, Philip J. Differing approaches to managing the chronic breathlessness syndrome in advanced COPD: a multi-national survey of specialists. COPD. 2018;15(3):294–302.
Brozek B, Damps-Konstanska I, Pierzchala W, Barczyk A, Currow DC, Jassem E, et al. End-of-life care for patients with advanced lung cancer and chronic obstructive pulmonary disease: survey among Polish pulmonologists. Pol Arch Intern Med. 2019;129(4):242–52.
Currow DC, Abernethy AP, Ko DN. The active identification and management of chronic refractory breathlessness is a human right. Thorax. 2014;69(4):393–4.
Hadjiphilippou S, Odogwu SE, Dand P. Doctors’ attitudes towards prescribing opioids for refractory dyspnoea: a single-centred study. BMJ Support Palliat Care. 2014;4(2):190–2.
Young J, Donahue M, Farquhar M, Simpson C, Rocker G. Using opioids to treat dyspnea in advanced COPD: attitudes and experiences of family physicians and respiratory therapists. Can Fam Phys. 2012;58(7):e401–7.
Simon ST, Higginson IJ, Booth S, Harding R, Weingartner V, Bausewein C. Benzodiazepines for the relief of breathlessness in advanced malignant and non-malignant diseases in adults. Cochrane Database Syst Rev. 2016;10:CD007354.
Mahler DA, Wells CK. Evaluation of clinical methods for rating dyspnea. Chest. 1988;93(3):580–6.
McCarthy B, Casey D, Devane D, Murphy K, Murphy E, Lacasse Y. Pulmonary rehabilitation for chronic obstructive pulmonary disease. Cochrane Database Syst Rev. 2015;2:CD003793.
Global Initiative for Chronic Obstructive Lung Disease: 2020 Report. 2020. https://goldcopd.org/gold-reports/.
Mahler DA, Selecky PA, Harrod CG, Benditt JO, Carrieri-Kohlman V, Curtis JR, et al. American College of Chest Physicians consensus statement on the management of dyspnea in patients with advanced lung or heart disease. Chest. 2010;137(3):674–91.
Marciniuk DD, Goodridge D, Hernandez P, Rocker G, Balter M, Bailey P, et al. Managing dyspnea in patients with advanced chronic obstructive pulmonary disease: a Canadian Thoracic Society clinical practice guideline. Can Respir J. 2011;18(2):69–78.
Bajwah S, Davies JM, Tanash H, Currow DC, Oluyase AO, Ekstrom M. Safety of benzodiazepines and opioids in interstitial lung disease: a national prospective study. Eur Respir J. 2018;52(6):1801278.
NICE. Idiopathic pulmonary fibrosis in adults: diagnosis and management. Clinical guideline [CG163]. 2017. https://www.nice.org.uk/guidance/cg163.
Simon ST, Pralong A, Radbruch L, Bausewein C, Voltz R. The palliative care of patients with incurable cancer. Dtsch Arztebl Int. 2020;116(7):108–15.
Papp LA, Weiss JR, Greenberg HE, Rifkin A, Scharf SM, Gorman JM, et al. Sertraline for chronic obstructive pulmonary disease and comorbid anxiety and mood disorders. Am J Psychiatry. 1995;152(10):1531.
Perna G, Cogo R, Bellodi L. Selective serotonin re-uptake inhibitors beyond psychiatry: are they useful in the treatment of severe, chronic, obstructive pulmonary disease? Depress Anxiety. 2004;20(4):203–4.
Smoller JW, Pollack MH, Systrom D, Kradin RL. Sertraline effects on dyspnea in patients with obstructive airways disease. Psychosomatics. 1998;39(1):24–9.
Higginson IJ, Wilcock A, Johnson MJ, Bajwah S, Lovell N, Yi D, et al. Randomised, double-blind, multicentre, mixed-methods, dose-escalation feasibility trial of mirtazapine for better treatment of severe breathlessness in advanced lung disease (BETTER-B feasibility). Thorax. 2020;75(2):176–9.
Lovell N, Bajwah S, Maddocks M, Wilcock A, Higginson IJ. Use of mirtazapine in patients with chronic breathlessness: a case series. Palliat Med. 2018;32(9):1518–21.
Lovell N, Wilcock A, Bajwah S, Etkind SN, Jolley CJ, Maddocks M, et al. Mirtazapine for chronic breathlessness? A review of mechanistic insights and therapeutic potential. Expert Rev Respir Med. 2019;13(2):173–80.
Boland J, Martin J, Wells AU, Ross JR. Palliative care for people with non-malignant lung disease: summary of current evidence and future direction. Palliat Med. 2013;27(9):811–6.
Brighton LJ, Miller S, Farquhar M, Booth S, Yi D, Gao W, et al. Holistic services for people with advanced disease and chronic breathlessness: a systematic review and meta-analysis. Thorax. 2019;74(3):270–81.
Luckett T, Phillips J, Johnson MJ, Farquhar M, Swan F, Assen T, et al. Contributions of a hand-held fan to self-management of chronic breathlessness. Eur Respir J. 2017;50(2):1700262.
Farquhar MC, Prevost AT, McCrone P, Brafman-Price B, Bentley A, Higginson IJ, et al. Is a specialist breathlessness service more effective and cost-effective for patients with advanced cancer and their carers than standard care? Findings of a mixed-method randomised controlled trial. BMC Med. 2014;12:194.
Farquhar MC, Prevost AT, McCrone P, Brafman-Price B, Bentley A, Higginson IJ, et al. The clinical and cost effectiveness of a Breathlessness Intervention Service for patients with advanced non-malignant disease and their informal carers: mixed findings of a mixed method randomised controlled trial. Trials. 2016;17:185.
Higginson IJ, Bausewein C, Reilly CC, Gao W, Gysels M, Dzingina M, et al. An integrated palliative and respiratory care service for patients with advanced disease and refractory breathlessness: a randomised controlled trial. Lancet Respir Med. 2014;2(12):979–87.
Bajwah S, Oluyase AO, Yi D, Gao W, Evans CJ, Grande G, et al. The effectiveness and cost-effectiveness of hospital-based specialist palliative care for adults with advanced illness and their caregivers. Cochrane Database Syst Rev. 2020;9:CD012780.
Bausewein C, Jolley C, Reilly C, Lobo P, Kelly J, Bellas H, et al. Development, effectiveness and cost-effectiveness of a new out-patient Breathlessness Support Service: study protocol of a phase III fast-track randomised controlled trial. BMC Pulm Med. 2012;12:58.
NICE. COVID-19 rapid guideline: managing symptoms (including at the end of life) in the community. 2020.
van der Molen T, Miravitlles M, Kocks JW. COPD management: role of symptom assessment in routine clinical practice. Int J Chron Obstruct Pulmon Dis. 2013;8:461–71.
Murtagh FE, Ramsenthaler C, Firth A, Groeneveld EI, Lovell N, Simon ST, et al. A brief, patient- and proxy-reported outcome measure in advanced illness: validity, reliability and responsiveness of the Integrated Palliative care Outcome Scale (IPOS). Palliat Med. 2019;33(8):1045–57.
Bruera E, Kuehn N, Miller MJ, Selmser P, Macmillan K. The Edmonton Symptom Assessment System (ESAS): a simple method for the assessment of palliative care patients. J Palliat Care. 1991;7(2):6–9.
Acknowledgements
Our thanks go to the ERS, EAPC and Palliative Care Formulary for disseminating the survey among their members. We would also like to thank Dr Natasha Smallwood for sharing her survey structure with us.
BETTER-B research consortium
BETTER-B (BETterTreatmEnts for Refractory Breathlessness in Palliative and End of Life Care) is an international, multicentre study, at the centre of which is a randomised controlled pragmatic trial of mirtazapine to alleviate breathlessness in palliative and end of life care (EudraCT 2019-002001-21), led by King’s College London, Cicely Saunders Institute, Department of Palliative Care, Policy & Rehabilitation, UK. Chief Investigator—Professor Irene Higginson (KCL, UK). Co-Investigators—UCD, Ireland: Professor Karen Ryan; AUSL, Italy: Dr. Massimo Costantini, Dr. Domenico Merlo; UMK, Poland: Assistant Professor Malgorzata Krajnik; KOELN, Germany: Dr. Steffen Simon; GUM, Poland: Professor Ewa Jassem; UCSC, Italy: Professor Giovanni Gambassi; UMUEN, Germany: Professor Claudia Bausewein; NOTTS, UK: Dr. Andrew Wilcock; UTS, Australia: Professor David Currow; ERS: Ms. Valerie Vaccaro; KCL, UK: Dr. Sabrina Bajwah, Dr. Matthew Maddocks. Co-Sponsor Representatives—KCL, UK: Ms. Jackie Pullen, Ms. Amy Holton; UCD, Ireland: Professor Peter Doran, Ms. Rabia Hussain, Ms. Anna Malara. Project Managers—KCL, UK: Dr. Nilay Hepgul, Dr. Adejoke Oluyase. Clinical Trials Research Unit—LEEDS, UK: Professor Julia Brown (co-investigator), Dr. Sarah Brown, Mr. Alasdair Fellows, Mr. Richard Brindle, Mrs. Claire Dimbleby, Mrs. Geraldine Murden, Ms. Eszter Katona, Ms. Fiona Walker. Health Economics—TCD, Ireland: Professor Charles Normand (co-investigator), Dr. Samantha Smith, Ms. Jingjing Jiang. Consortium members—KCL, UK: Mrs. Hinna Mir, Dr. Caroline Jolley, Ms. Olivia Dix, Ms. Margaret Ogden; UCD, Ireland: Ms. Brenda Molloy, Dr. Emer Kelly; Ms. Faye Regan, AUSL, Italy: Dr. Silvia Tanzi, Dr. Candida Bonelli; UMK, Poland: Ms. Agnieszka Arendt-Nowakowska, Ms. Malgorzata Fopka-Kowalczyk, Ms. Sabina Panfilak; KOELN, Germany: Mrs. Yvonne Eisenmann, Dr. Anne Pralong, Professor Raymond Voltz; GUM, Poland: Mr. Mateusz Kirjak, Mr. Piotr Janowiak; UMUEN, Germany: Mr. Jeremias Bazata; NOTTS, UK: Dr. Charlotte Bolton, Dr. Gisli Jenkins; ELF: Mrs. Pippa Powell; HULL, UK: Professor Miriam Johnson.
Funding
BETTER-B is funded by the European Union’s Horizon2020 research and innovation programme under grant agreement No. 825319. We also thank Cicely Saunders International for support towards the breathlessness research programme at the Cicely Saunders Institute, which contributed to this study. Higginson is an NIHR Senior Investigator Emeritus. BETTER-B is also supported by the National Institute for Health Research (NIHR) Applied Research Collaboration South London (NIHR ARC South London) at King’s College Hospital NHS Foundation Trust. The views expressed are those of the author(s) and not necessarily those of the European Commission, the NIHR or the Department of Health and Social Care.
Author information
Authors and Affiliations
Consortia
Contributions
MK, IJH, CJ, AW, EJ, ST, STS acquired funding, led the conception and design of the survey, agreed the interpretation of results and wrote the report. MK led the detailed design and piloting of the survey. NH led the implementation of the survey, initial data analysis and first draft of the report. TB contributed to data analysis. All authors contributed to the interpretation of results, read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Approval was granted by the King’s College London (UK) Research Ethics Committee (MRA-18/19-11108). Physicians were informed that by completing the survey, they provided informed consent for use of their anonymised data.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Additional file 1.
Copy of survey questions.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Krajnik, M., Hepgul, N., Wilcock, A. et al. Do guidelines influence breathlessness management in advanced lung diseases? A multinational survey of respiratory medicine and palliative care physicians. BMC Pulm Med 22, 41 (2022). https://doi.org/10.1186/s12890-022-01835-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12890-022-01835-0