Abstract
Background
Nutritional status during pregnancy can have a significant impact on infant and maternal health outcomes. To maintain maternal homeostasis and support fetal growth, adequate macronutrient and energy intake during pregnancy is essential. Therefore, this study sought to systematically review and meta-analyze macronutrient and energy intakes during pregnancy.
Methods
A systematic review and meta-analysis was carried out based on the PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) guidelines. The required data were collected from four databases including: Web of Sciences, ProQuest, Scopus, and PubMed, from 1 January 1980 to 30 May 2023, by using a combination of search terms (dietary pattern" OR "diet quality" OR "food habits" OR "nutrition surveys" OR "diet surveys" OR "food-frequency questionnaire" OR "diet record" OR "dietary recall") AND ( "pregnancy" OR "reproduction" OR "maternal health" OR "neonatal outcomes") among interventional and observational studies. Excel and STATA version 11 were used for data analysis.
Results
Among 7081 published articles, 54 studies were included in the review. Most of the 33 (61%) studies were cohort studies and a total of 135,566 pregnant women were included. The overall average of energy, carbohydrate, fat, and protein intake was 2036.10 kcal/day, 262.17 gr/day, 74.17 gr/day, and 78.21 gr/day, respectively. Also, energy intake during pregnancy was higher in American (2228.31 kcal/day, CI95%: 2135.06–2325.63) and Eastern Mediterranean regions (2226.70 kcal/day, CI95%: 2077.23–2386.92) than other regions (P < 0.001). Energy intake was higher in the third trimester than others (2115.64 kcal/day, CI95%: 1974.15–2267.27). Furthermore, based on the findings, there was a significant difference between energy intake in different World Health Organization (WHO) regions (P < 0.05).
Conclusions
According to the results of meta-analysis, the average total energy was below than average total energy required during pregnancy. More efforts are needed to encourage women to adopt healthy eating habits during pregnancy to support healthy fetal and infant development.
Similar content being viewed by others
Introduction
Nutrient status, as well as adequate dietary intake, during the human gestational period is essential to ensure optimal fetal growth [1]. Nutrient requirements are enhanced during the pregnancy in all the three trimesters, yet scientific evidence shows pregnant women are at increased risk of micro- and macronutrient deficiency [2].
Macronutrients (protein, fat and carbohydrates) are the main sources of energy for the mother and the fetus, which are necessary for tissue growth and fetal cells development [3]. Pregnancy is associated with increased requirements for nutrition intake and maternal energy in order to meet nutritional demands of the developing fetus.
Inadequate diets resulting in nutrient and energy intake deficiencies can have a considerable impact on neonatal health and pregnancy outcomes. Restriction of energy and nutrition disrupt proper development of the fetus and may lead to ailments, including cardiovascular disease, type II diabetes, and hypertension [4]. Chronic energy deficiency commonly occurs among women of reproductive age, as well as pregnant women in developing countries, due to several factors such as poor diet quality, family size, living in rural areas, insufficient meal frequency, and low socioeconomic status [5, 6]. Furthermore, a prior study reported a positive association between energy intake at the end of the third trimester and neonate birth weight. Sharma et al. indicated that higher consumption of carbohydrates may be associated with an increase in birth weight and conversely, increasing fat intake with low birth weight [7]. Additionally, another study showed that reducing dairy, as well as animal proteins, consumption in late pregnancy and enhancing carbohydrate intake in early pregnancy was associated with decreased birth weight [8]. Animal studies have indicated that insufficient dietary protein intake during pregnancy produced offspring with low birth weight [9]. Accordingly, the collective evidence highlights that macronutrients are essential for optimal development of the fetus. Therefore, the aim of the current study was to conduct and systematic review and meta-analysis of maternal macronutrient and energy intake during pregnancy.
Methods
A systematic and meta-analysis study was carried out in 2023. Relevant databases including PROQUEST, SCOPUS, PUBMED and Web of Sciences were searched to identify studies.
Search strategy
The following search terms were used: ("dietary pattern”) OR ("diet quality") OR ( "food habits") OR ( "nutrition surveys") OR ( "diet surveys") OR ( "food-frequency questionnaire") OR ( "diet record") OR ( "dietary recall") AND ( pregnancy) OR (" reproduction") OR ( "maternalhealth") OR ( "neonatal outcomes"). The search terms for each database is shown in Appendix 1.
Inclusion criteria were studies that reported mean or median of energy intake and the percentage or grams of macronutrient (protein, fat, carbohydrate) in healthy pregnant women without having a disease, use food frequency questioner (SO-FFQ), dietary recall, or food dairy(FD) questioners.
Exclusion criteria were: studies that did not report energy, macronutrient (protein, fat, carbohydrate) in healthy pregnant women and countries with special socioeconomic conditions.
Studies were excluded if they were published in a language other than English, examined different specific dietary patterns (such as western, vegetarian, traditional and mixed, prudent and etc.…), did not report the average total macronutrient and energy or diet data included supplements and studies with incomplete information, studies in which women were pregnant under certain conditions (such as IVF). Also, case reports, case series, editorials, letters to the editor, commentaries, and reviews were excluded.
Data extraction
Study characteristics were extracted into a predetermined table in the Excel software that collected information including author, year of publication, participant number, study design, country, average age, trimesters of pregnancy, dietary assessment tools, average of total macronutrient and energy intake.
A total of 54 papers were included in the meta-analysis and all relevant data were extracted. Supplementary data are shown in Fig. 1. Mean energy intakes were extracted from the studies. Also, SD and confidence interval’s (CI) were calculated using the following approach.
Calculating confidence intervals
The upper limit and lower limit were calculated using the following formula [10, 11].
*X̄ is the sample mean, σ is the standard deviation, and n is the sample size. Assuming a confidence level of 95%: Z = 1.960.
All energy units, except kilocalories, were converted to kilocalories. When macronutrient percentages were given, we converted them to grams if they could be converted manually, otherwise they were excluded.
gr/day carbohydrate or protein = Energy * % carbohydrate or protein / 4 and for fat it is 9.
We estimated the sample mean from the sample size, median, mid-range, and/or mid-quartile range [12]:
In the studies where the sample quartile was given, the mean and standard deviation were calculated using the following formula. Also, studies that reported median information were converted to the mean [13, 14].
*Scenario S2 reports the first and third quartiles instead of the minimum and the maximum, together with the median and the sample size.
standard deviation:
The standard error of the mean (SE) was converted to the standard deviation(SD) using the formula [15].
SD = SE *√n.
n = sample size.
Decimals of the mean and standard deviation were rounded.
However, some macronutrients were not reported within the included studies.
Statistical analysis
Mean of macronutrient and energy intake pooled odds were calculated with a random-effect restricted maximum likelihood (REML) model and 95% confidence intervals. We inferred heterogeneity between studies using the I2 statistic. By using subgroup analysis, and taking into account region, questionnaire, trimester of pregnancy, and study design, we assessed the heterogeneity of studies. Publication bias was assessed using Egger's test. All data analysis was carried out using STATA software.
Results
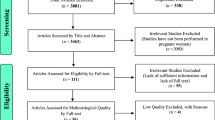
All articles were imported into Endnote software version 16, where duplicates were removed. Subsequently, the title and abstract of articles were studied and they were included if were relevant to the topic. Following this, the authors read the full text, and eligible studies with selection criteria were obtained. Briefly, the flow diagram for the studies selection is presented in Fig. 1.
As shown in the PRISMA flow diagram (Fig. 1), 7081 published papers were identified from (Web of Sciences, ProQuest, Scopus, and PubMed) in 1 January 1980 to 30 may 2023, of which, 2459 cases were duplicates and removed. After reading the titles and abstracts, 2824 articles were excluded due to being unrelated to the topic. Also, 1744 articles were excluded after reviewing the full texts of remaining articles. Therefore, a total of 54 studies were included in this review. Two of the studies were randomized controlled trial (RCTs), 33 were cohort, 15 studies were cross-sectional, and 4 of them were case–control studies. The basic characteristics of the included studies are presented in Table 1. The age of the participants ranged from 23 ± 3 (years) [16], to 37 ± 4 years [17]. Out of the total studies included, most of the studies were conducted in America [18,19,20,21,22,23,24,25,26,27,28,29,30,31,32,33,34,35,36,37,38,39,40]. Additionally, four studies were from the Eastern Mediterranean region [41,42,43,44], followed by 13 from the western pacific region [16, 45,46,47,48,49,50,51,52,53,54,55,56], 11 from European region [17, 37, 57,58,59,60,61,62,63,64,65,66], and two were conducted in South East Asia [67, 68]. In total, the sample size was 135,566 participants, ranging from 28 in Lebrun [24] to 92,448 in Miura [69]. Only 24 studies used the dietary recall method, and most of the dietary assessments were realized using the food frequency questionnaire, whilst 11 used foods dairy questionnaire.
Study quality assessment
The CASP* checklist was used to evaluate the quality of the studies. In total, 54 studies entered the meta-analysis phase. These studies are shown in Table 1.
* The CASP (Critical Appraisal Skills Program) checklists are a set of checklists that contain prompt questions to help evaluate research studies.
Total protein intake
Analysis showed that total protein intake amongst pregnant women in different countries, albeit with different assessment instruments of food intake, was 78.21 gr/day (95% CI: 74.19–82.44) (Fig. 2).
The highest of daily energy intake from protein was found in Forsythe study (19–25% According to the difference of energy in recall and FFQ questionnaires). According to the results, there was a significant difference between the amount of protein consumed during pregnancy in different studies (p < 0.001).
Total carbohydrate intake
All countries showed a high intake of carbohydrate, ranging from 170gr/day in Greece (95% CI: 164.10–176.11) to 345gr/day (95% CI: 342.18–347.85) in China (Fig. 3). Also, there was a significant difference between the amount of carbohydrate intake during pregnancy in different studies (p < 0.001).
Total fat intake
Across the WHO regions, total fat intake amongst pregnant women was 74.17 gr/day (95% CI: 68.74–80.03), the lowest amount of fat intake was in the Cheng study conducted in China 32 gr/day (95% CI: 30.29–33.81), and the highest intake was in the Gao study conducted in China in 2013 (106 gr/day, 95% CI: 98.09–114.55) (Fig. 4). According to our results, there was a significant difference between the amount of fat consumed during pregnancy in different studies.
Energy intake
Among 54 studies, data on energy intake was extracted from 52 studies. The overall average energy intake was 2036.10 kcal/day (95% CI: 1959.31–2115.89), ranging from 1150 kcal/day (95% CI: 1027.81–1286.72) in Brantsæter.et al. to 3307 kcal/day (95% CI: 3096.59–3531.71) in the Duarte study (Fig. 5). We found a significant difference between the amount of energy intake during pregnancy.
Energy intake
By contrasting levels of intake of energy in countries, we found that participants from Mexico had a higher daily energy intake than those from Norway. Based on the division of geographical regions into five regions, the highest average energy was seen in the American and Eastern Mediterranean regions and the lowest in the Western Pacific regions (Fig. 6).
According to Table 2, the average energy using the questionnaires were significantly different, although higher values were observed in studies using the FFQ questionnaire (Fig. 7).
In the cohort studies, the lowest and the highest mean intake were reported in the case–control studies (Fig. 8). In addition, the overall average energy intake was the highest in the third trimester of pregnancy (Fig. 9).
Discussion
This systematic review and meta-analysis summarizes the extant evidence related to the food-derived energy and macronutrient intakes of pregnant women in different countries.
This investigation revealed that total average energy intake of pregnant women was 2036.10 kcal/day (recommended energy intake during pregnancy is set at 200 to 300 kcal/day (FAO/WHO/UNU, 1985; NRC, 1989) above non-pregnant levels about 2200–2500 kcal/day) [73]. In this meta-analysis study, this average is lower than the recommended normal average. In addition, we found that, on average, an intake of 109 kcal/day and 49 kcal/day less than women from developed countries, middle and low -income countries, respectively [74,75,76]. Moreover, the range of energy intake in WHO regions was between 1867 -2228 kcal/day and the highest mean was in the American and Eastern Mediterranean regions. Our findings were consistent with two other reports [76, 77], but the range of energy in these studies was 7710 to 9260 kJ/day.
Contrary to the results of this study, in the meta-analysis study that was conducted in Indonesia and Malaysia, the average energy intake based on the type of study was the highest in cross-sectional studies (1895 kcal/day) and the lowest in case–control studies (1220 kcal/day). This may be due to the difference in the region, the number of studies of each type of study, and trimester of pregnancy [78].
According to our results, average energy intake was higher when using the FFQ questionnaire and the lowest in 24-h recall. This is similar to a previous study [79], however, in contrast with the Shatenstein study [23]. This difference might be due different regions, sample sizes, and study designs. Heterogeneity among countries is expected due to different levels of income, food access and food security. Diet can be influenced by several factors at the macro and micro level. The reported differences between countries could be the result of macro level factors (macro environment) referring to structures such as food systems (access to land and food production), nutrition policies and reforms, mass media and culture. The macro environment influences the micro level factors which in turn influence the diet of the population.
In this study, similar to a prior study, the third trimester of pregnancy had the highest daily energy intake compared to other trimesters [78]. Since energy intake is the main cause of weight gain during pregnancy, the mother's diet should be a sufficient source of energy to meet the usual needs of the mother, as well as the needs of the growing fetus, which includes the synthesis of new tissues (placenta, embryo and amniotic fluid) and the growth of existing tissue (fat tissue of the mother, breast and uterus) [80]. However, energy demands vary widely during pregnancy, so energy intake should be adjusted based on pre-pregnancy body mass index (BMI), metabolic rate, and physical activity level. In the last month of pregnancy, the fetus grows rapidly, which is associated with an increase in the weight of the fetus, and the mother's nutritional needs also increase. Another study showed that energy intake in pregnant women in the third trimester has a strong positive correlation with birth weight [81]. Contrary to these studies, Gennaro found that energy intake in the third trimester of pregnancy was not high [82], this could be because the consumption of nutrients among the participants in the third trimester of pregnancy was constant.
According to our results, the mean of protein intakes (78.21 gr/day) was higher than in the previous studies (52.4 g/d and 64.3 g/d) [75, 83]. The recommended amount of protein for pregnant women is 60 to 70 g per day [84]. This suggests that the protein intake of pregnant women may have improved over the past few decades. A simultaneous reduction in maternal urea synthesis, urinary urea excretion, and amino acid concentration, occurs in early pregnancy and remains low throughout pregnancy. In well-nourished pregnant women, these physiological changes conserve nitrogen and increase protein to ensure sufficient nutrients are provided to the fetus [85].
In addition, in a meta-analysis study conducted in the Eastern Mediterranean region [86], like our study, the intake of carbohydrates was high in most countries. In general, it is recommended that pregnant women should consume 175 g/day of carbohydrates [84]. The average carbohydrate intake in the present review (262.17 g/d) was similar to two previous reports (297,269 g/d) [74, 76] and more than normal range. Generally, these similarities and differences may reflect the impact of macro-level socioeconomic inequalities that affect access and choice of food options and shape the dietary patterns of populations [87]. The type of carbohydrates consumed (low or high glycemic sources) affects the fetus and mother during pregnancy. Eating high-glycemic carbohydrates leads to excessive maternal weight gain and overgrowth of the fetus-pair, while low-glycemic carbohydrate consumption increases the normal weight of the mother and produces infants with normal weight [88].
As observed in this and previous studies [86, 89], fat intake was found to be high in some countries. However, women in some developed countries showed slightly higher fat intake than women in Villanueva study and our study (86 vs 71 and 74 g/day) [74, 76]. It is recommended that approximately 40–90 g of fat needed each day [90]. A higher intake of saturated fatty acids, at the same time as a lower intake of other macronutrients (including refined sugar), is associated with an increase in infant fat mass. In addition, excessive consumption of saturated fats is associated with increased infant obesity, weight for age, and waist-to-hip ratio at six months of age, and causes obesity, insulin resistance, and cardiovascular diseases at older ages. Therefore women should be encouraged to limit saturated fatty acids especially [91].
Different reports among countries may be due to the differences in structures such as food systems (access to land and food production), different income levels, different dietary assessment methodologies culture, small sample sizes, mass media, and nutrition policies. Moreover, the environment can affect micro-level factors, which in turn affect the population's diet.
Maternal nutrition is a key factor in the intrauterine environment, necessary for fetal development. As an important modifiable factor, maternal diet can be easily intervened at low cost and low risk. Impaired maternal nutrition during critical periods of development may have long-term effects on fetal tissue development and is a risk factor associated with chronic diseases and metabolism in adulthood, including diabetes and cardiovascular disease.
Limitations
There are limitations in this study that should be noted. The included studies used a combination of dietary assessment tools, which may introduce a measurement bias, including under or over reporting. We also faced challenges in using the collected information, where among the macronutrients, protein was reported more than fat and carbohydrate in different regions, which makes it difficult to estimate the distribution of macronutrient intake. In addition, multiple studies in individual countries may unreasonably influence the total nutrient intake of the region. In some studies, different specific dietary patterns were used that were not applied in this study. For the average of fat and carbohydrates, if two questionnaires were used, only one of the questionnaires was considered. One of the strengths of this study was the use of robust meta-analytical methods and systematic review guidelines, in addition to comprehensively considering studies carried out in different countries covering the 5 continents.
Conclusions
In general, the average total energy in this study was less than the average total energy required during pregnancy. The importance of maintaining a healthy and varied diet during pregnancy should not be overlooked. Indeed, nutritional deficiencies during pregnancy, especially in deprived and high-risk populations, are still one of the biggest public health problems. Health policies should prioritize the establishment of sustainable food systems that enable healthy and sustainable food choices and promote healthy eating patterns to enable nutrient intake to meet the needs of the mother and of the baby.
Availability of data and materials
All data and materials used in this research are available via the corresponding author on request.
Abbreviations
- WHO:
-
World Health Organization
- RCTs:
-
Randomized controlled trial
- BMI:
-
Body mass index
- SQ –FFQ:
-
Semi-quantitative Food frequency questionnaire
- 24 h-R:
-
24- Dietary recall
- FD:
-
Food dairy
References
Looman M, Geelen A, Samlal RA, Heijligenberg R, Klein Gunnewiek JM, Balvers MG, et al. Changes in micronutrient intake and status, diet quality and glucose tolerance from preconception to the second trimester of pregnancy. Nutrients. 2019;11(2):460.
Concina F, Pani P, Carletti C, Rosolen V, Knowles A, Parpinel M, et al. Nutrient intake during pregnancy and adherence to dietary recommendations: The mediterranean phime cohort. Nutrients. 2021;13(5):1434.
Taylor RM, Blumfield ML, Ashton LM, Hure AJ, Smith R, Buckley N, et al. Macronutrient Intake in Pregnancy and Child Cognitive and Behavioural Outcomes. Children. 2021;8(5):425.
Najpaverova S, Kovarik M, Kacerovsky M, Zadak Z, Hronek M. The relationship of nutritional energy and macronutrient intake with pregnancy outcomes in Czech pregnant women. Nutrients. 2020;12(4):1152.
Wubie A, Seid O, Eshetie S, Dagne S, Menber Y, Wasihun Y, et al. Determinants of chronic energy deficiency among non-pregnant and non-lactating women of reproductive age in rural Kebeles of Dera District, North West Ethiopia, 2019: Unmatched case control study. PLoS ONE. 2020;15(10):e0241341.
Tejayanti T. Determinants of chronic energy deficiency and low body mass index of pregnant women in Indonesia. Jurnal Kesehatan Reproduksi. 2019;10(2):173–80.
Sharma SS, Greenwood DC, Simpson NA, Cade JE. Is dietary macronutrient composition during pregnancy associated with offspring birth weight? An observational study. Br J Nutr. 2018;119(3):330–9.
Godfrey K, Robinson S, Barker D, Osmond C, Cox V. Maternal nutrition in early and late pregnancy in relation to placental and fetal growth. BMJ. 1996;312(7028):410.
Yang J, Chang Q, Tian X, Zhang B, Zeng L, Yan H, et al. Dietary protein intake during pregnancy and birth weight among Chinese pregnant women with low intake of protein. Nutr Metab. 2022;19(1):1–12.
Nadjarzadeh A, Mehrsai A, Mostafavi E, Gohari MR, Shidfar F. The association between dietary antioxidant intake and semen quality in infertile men. Med J Islam Repub Iran. 2013;27(4):204.
https://www.calculator.net/confidence-interval-calculator.html.
https://www.math.hkbu.edu.hk/~tongt/papers/median2mean.html.
Luo D, Wan X, Liu J, Tong T. Optimally estimating the sample mean from the sample size, median, mid-range, and/or mid-quartile range. Stat Methods Med Res. 2018;27(6):1785–805.
Wan X, Wang W, Liu J, Tong T. Estimating the sample mean and standard deviation from the sample size, median, range and/or interquartile range. BMC Med Res Methodol. 2014;14:1–13.
Cyrus A, Kabir A, Goodarzi D, Moghimi M. The effect of adjuvant vitamin C after varicocele surgery on sperm quality and quantity in infertile men: a double blind placebo controlled clinical trial. Int Braz J Urol. 2015;41:230–8.
Li M, Halldorsson TI, Bjerregaard AA, Che Y, Mao Y, Hu W, et al. Relative validity and reproducibility of a food frequency questionnaire used in pregnant women from a rural area of China. Acta Obstet Gynecol Scand. 2014;93(11):1141–9.
Athanasiadou E, Kyrkou C, Fotiou M, Tsakoumaki F, Dimitropoulou A, Polychroniadou E, et al. Development and validation of a Mediterranean oriented culture-specific semi-quantitative food frequency questionnaire. Nutrients. 2016;8(9):522.
De La Rosa VY, Hoover J, Du R, Jimenez EY, MacKenzie D, Team NS, et al. Diet quality among pregnant women in the Navajo Birth Cohort Study. Matern Child Nutr. 2020;16(3):e12961.
Ancira-Moreno M, O’Neill MS, Rivera-Dommarco JÁ, Batis C, Rodríguez Ramírez S, Sánchez BN, et al. Dietary patterns and diet quality during pregnancy and low birthweight: The PRINCESA cohort. Matern Child Nutr. 2020;16(3):e12972.
Hu Z, Tylavsky FA, Kocak M, Fowke JH, Han JC, Davis RL, et al. Effects of maternal dietary patterns during pregnancy on early childhood growth trajectories and obesity risk: the CANDLE study. Nutrients. 2020;12(2):465.
Baddour SE, Virasith H, Vanstone C, Forest J-C, Giguère Y, Charland M, et al. Validity of the Willett food frequency questionnaire in assessing the iron intake of French-Canadian pregnant women. Nutrition. 2013;29(5):752–6.
Mahmassani HA, Switkowski KM, Scott TM, Johnson EJ, Rifas-Shiman SL, Oken E, et al. Maternal diet quality during pregnancy and child cognition and behavior in a US cohort. Am J Clin Nutr. 2022;115(1):128–41.
Shatenstein B, Xu H, Luo Z-C, Fraser W. Relative Validity of a Food Frequency Questionnaire: For Pregnant Women. Can J Diet Pract Res. 2011;72(2):60–9.
Lebrun A, Plante A-S, Savard C, Dugas C, Fontaine-Bisson B, Lemieux S, et al. Tracking of dietary intake and diet quality from late pregnancy to the postpartum period. Nutrients. 2019;11(9):2080.
Savard C, Lemieux S, Lafrenière J, Laramée C, Robitaille J, Morisset A-S. Validation of a self-administered web-based 24-hour dietary recall among pregnant women. BMC Pregnancy Childbirth. 2018;18(1):1–10.
Landman JP, Hall JSE. Dietary patterns and nutrition in pregnancy in Jamaica. J Trop Pediatr. 1989;35(4):185–90.
Schwedhelm C, Lipsky LM, Temmen CD, Nansel TR. Eating patterns during pregnancy and postpartum and their association with diet quality and energy intake. Nutrients. 2022;14(6):1167.
Emond JA, Karagas MR, Baker ER, Gilbert-Diamond D. Better diet quality during pregnancy is associated with a reduced likelihood of an infant born small for gestational age: An analysis of the prospective New Hampshire birth cohort study. J Nutr. 2018;148(1):22–30.
Brown JE, Buzzard IM, Jacobs DR Jr, Hannan PJ, Kushi LH, Barosso GM, et al. A food frequency questionnaire can detect pregnancy-related changes in diet. J Am Diet Assoc. 1996;96(3):262–6.
Gonzalez-Nahm S, Østbye T, Hoyo C, Kravitz RM, Benjamin-Neelon SE. Associations among food security, diet quality, and dietary intake during pregnancy in a predominantly African American group of women from North Carolina. J Acad Nutr Diet. 2022;122(3):565–72.
Shin D, Lee KW, Song WO. Pre-pregnancy weight status is associated with diet quality and nutritional biomarkers during pregnancy. Nutrients. 2016;8(3):162.
Pick ME, Edwards M, Moreau D, Ryan EA. Assessment of diet quality in pregnant women using the Healthy Eating Index. J Am Diet Assoc. 2005;105(2):240–6.
Voortman T, Régine PMS-T, Bergen NE, Jaddoe VWV, Looman CWN, Kiefte-de Jong JC, et al. Validation of a Semi-Quantitative Food-Frequency Questionnaire for Dutch Pregnant Women from the General Population Using the Method or Triads. Nutrients. 2020;12(5):1341 PubMed PMID: 2408500313. English.
Dubois L, Diasparra M, Bédard B, Colapinto CK, Fontaine-Bisson B, Tremblay RE, et al. Adequacy of nutritional intake during pregnancy in relation to prepregnancy BMI: results from the 3D Cohort Study. Br J Nutr. 2018;120(3):335–44.
Forsythe HE, Gage B. Use of a multicultural food-frequency questionnaire with pregnant and lactating women. Am J Clin Nutr. 1994;59(1 SUPPL.):203S–S206.
Duarte ACOR, Pinho Ld, Silveira MF, Botelho EM. Validation of a food frequency questionnaire for pregnant women attending primary care facilities. J Hum Growth Dev. 2020;30(1):75–83.
Freitas‐Vilela AA, Smith AD, Kac G, Pearson RM, Heron J, Emond A, Hibbeln JR, Castro MB, Emmett PM. Dietary patterns by cluster analysis in pregnant women: Relationship with nutrient intakes and dietary patterns in 7‐year‐old offspring. Matern Child Nutr. 2017;13(2):e12353.
Lepsch J, Vaz JS, Moreira JD, Pinto TJP, Soares-Mota M, Kac G. Food frequency questionnaire as an indicator of the serum composition of essential n-3 and n-6 polyunsaturated fatty acids in early pregnancy, according to body mass index. J Hum Nutr Diet. 2015;28(1):85–94.
Reyes-López MA, González-Leyva CP, Rodríguez-Cano AM, Rodríguez-Hernández C, Colin-Ramírez E, Estrada-Gutierrez G, Muñoz-Manrique CG, Perichart-Perera O. Diet quality is associated with a high newborn size and reduction in the risk of low birth weight and small for gestational age in a group of Mexican pregnant women: an observational study. Nutrients. 2021;13(6):1853.
Vilela AAF, Farias DR, Eshriqui I, Vaz JdS, Franco-Sena AB, Castro MBT, et al. Prepregnancy healthy dietary pattern is inversely associated with depressive symptoms among pregnant Brazilian women. J Nutr. 2014;144(10):1612–8.
Mohammadshahi M, Zakerzadeh M, Hashemi S, Haidari F. Dietary Patterns in Pregnancy and Infants' Anthropometric Parameters at Birth. Hayat. 2013;19(1).
Papazian T, Hout H, Sibai D, Helou N, Younes H, El Osta N, et al. Development, reproducibility and validity of a food frequency questionnaire among pregnant women adherent to the Mediterranean dietary pattern. Clin Nutr. 2016;35(6):1550–6.
Alamolhoda SH, Simbar M, Mirmiran P, Mirabi P. The effectiveness of low trans-fatty acids dietary pattern in pregnancy and the risk of gestational diabetes mellitus. Caspian J Intern Med. 2019;10(2):197–204 PubMed PMID: WOS:000477894300010. English.
Tayyem R, Allehdan S, Mustafa L, Thekraallah F, Al-Asali F. Validity and reproducibility of a food frequency questionnaire for estimating macro-and micronutrient intakes among pregnant women in Jordan. J Am Coll Nutr. 2020;39(1):29–38.
Li S, Liu D, Kang Y, Qu P, Mi B, Zhu Z, et al. Associations of B Vitamin-Related Dietary Pattern during Pregnancy with Birth Outcomes: A Population-Based Study in Northwest China. Nutrients. 2022;14(3):600 PubMed PMID: 2627824290. English.
Yang J, Kang Y, Cheng Y, Zeng L, Yan H, Dang S. Maternal dietary patterns during pregnancy and congenital heart defects: a case-control study. Int J Environ Res Public Health. 2019;16(16):2957.
Gao H, Stiller CK, Scherbaum V, Biesalski HK, Wang Q, Hormann E, et al. Dietary intake and food habits of pregnant women residing in urban and rural areas of Deyang city, Sichuan Province. China Nutrients. 2013;5(8):2933–54.
Li M, Shi J, Luo J, Long Q, Yang Q, Ouyang Y, et al. Diet quality among women with previous gestational diabetes mellitus in rural areas of Hunan Province. Int J Environ Res Public Health. 2020;17(16):1–16.
Gete DG, Waller M, Mishra GD. Changes in dietary patterns from preconception to during pregnancy and its association with socio-demographic and lifestyle factors. Public Health Nutr. 2021.
Ogawa K, Seung-Chik J, Kobayashi M, Morisaki N, Sago H, Fujiwara T. Validation of a food frequency questionnaire for Japanese pregnant women with and without nausea and vomiting in early pregnancy. J Epidemiol. 2017;27(5):201–8 PubMed PMID: 1908079676. English.
Chen LW, Aris IM, Bernard JY, Tint MT, Chia A, Colega M, Gluckman PD, Shek LP, Saw SM, Chong YS, Yap F. Associations of maternal dietary patterns during pregnancy with offspring adiposity from birth until 54 months of age. Nutrients. 2016;9(1):2.
Loy SL, Marhazlina M, Nor Azwany Y, Hamid Jan JM. Development, validity and reproducibility of a food frequency questionnaire in pregnancy for the Universiti Sains Malaysia birth cohort study. Malays J Nutr. 2011;17(1):1–18.
Miura K, Takamori A, Hamazaki K, Tsuchida A, Tanaka T, Origasa H, et al. Dietary patterns during pregnancy and health-related quality of life: The Japan Environment and Children’s Study. PLoS ONE. 2020;15(7):e0236330.
Yang J, Dang S, Cheng Y, Qiu H, Mi B, Jiang Y, et al. Dietary intakes and dietary patterns among pregnant women in Northwest China. Public Health Nutr. 2017;20(2):282–93.
Zhang H, Qiu X, Zhong C, Zhang K, Xiao M, Yi N, Xiong G, Wang J, Yao J, Hao L, Wei S. Reproducibility and relative validity of a semi-quantitative food frequency questionnaire for Chinese pregnant women. Nutr J. 2015;14:1–0.
Cheng Y, Yan H, Dibley MJ, Shen Y, Li Q, Zeng L. Validity and reproducibility of a semi-quantitative food frequency questionnaire for use among pregnant women in rural China. Asia Pac J Clin Nutr. 2008;17(1):166–77.
McGowan CA, Curran S, McAuliffe FM. Relative validity of a food frequency questionnaire to assess nutrient intake in pregnant women. J Hum Nutr Diet. 2014;27(SUPPL2):167–74.
McGowan CA, McAuliffe FM. Maternal dietary patterns and associated nutrient intakes during each trimester of pregnancy. Public Health Nutr. 2014;16(1):97–107.
Hinojosa-Nogueira D, Romero-Molina D, Giménez-Asensio MJ, Gonzalez-Alzaga B, Lopéz-Flores I, Cueva SP, Rufián-Henares JÁ, Hernández AF, Lacasaña M. Validity and Reproducibility of a Food Frequency Questionnaire to Assess Nutrients Intake of Pregnant Women in the South-East of Spain. Nutrients. 2021;13(9):3032.
Pinto E, Severo M, Correia S, dos Santos SI, Lopes C, Barros H. Validity and reproducibility of a semi-quantitative food frequency questionnaire for use among Portuguese pregnant women. Matern Child Nutr. 2010;6(2):105–19.
Darke SJ, Disselduff MM, Try GP. Frequency distributions of mean daily intakes of food energy and selected nutrients obtained during nutrition surveys of Merent groups of people in Great Britain between 1968 and 1971. Br J Nutr. 1980;44(3):243–52.
Thomas Berube L, Messito MJ, Woolf K, Deierlein A, Gross R. Correlates of Prenatal Diet Quality in Low-Income Hispanic Women. J Acad Nutr Diet. 2019;119(8):1284–95.
Vioque J, Navarrete-Muñoz EM, Gimenez-Monzó D, García-de-la-Hera M, Granado F, Young IS, et al. Reproducibility and validity of a food frequency questionnaire among pregnant women in a Mediterranean area. Nutr J. 2013;2013(12):26 PubMed PMID: 1313245487; 23421854. English.
Apostolopoulou A, Magriplis E, Tsekitsidi E, Oikonomidou AC, Papaefstathiou E, Tsakiridis I, et al. Development and validation of a short culture-specific food frequency questionnaire for Greek pregnant women and their adherence to the Mediterranean diet. Nutrition. 2021;90:111357.
Brantsæter AL, Haugen M, Alexander J, Meltzer HM. Validity of a new food frequency questionnaire for pregnant women in the Norwegian Mother and Child Cohort Study (MoBa). Matern Child Nutr. 2008;4(1):28–43.
Mouratidou T, Ford F, Fraser RB. Validation of a food-frequency questionnaire for use in pregnancy. Public Health Nutr. 2006;9(4):515–22.
Angkasa D, Agustina R, Khusun H, Prafiantini E. Validation of a semi-quantitative food frequency questionnaire for estimating dietary omega-3 fatty acids intake among urban Indonesian pregnant women. Malays J Nutr. 2019;25(2):321–35.
Joshi K, Gadgil M, Pandit A, Otiv S, Kothapalli KSD, Brenna JT. Dietary pattern regulates fatty acid desaturase 1 gene expression in Indian pregnant women to spare overall long chain polyunsaturated fatty acids levels. Mol Biol Rep. 2019;46(1):687–93.
Miura K, Takamori A, Hamazaki K, Tsuchida A, Tanaka T, Origasa H, Inadera H, Japan Environment and Children’s Study Group. Dietary patterns during pregnancy and health-related quality of life: The Japan Environment and Children’s Study. Plos one. 2020;15(7):e0236330.
Perreault M, Xu VY, Hamilton S, Wright D, Foster W, Atkinson SA. Validation of a food frequency questionnaire for bone nutrients in pregnant women. Can J Diet Pract Res. 2016;77(3):133–9.
Cole ZA, Gale CR, Javaid MK, Robinson SM, Law C, Boucher BJ, Crozier SR, Godfrey KM, Dennison EM, Cooper C. Maternal dietary patterns during pregnancy and childhood bone mass: a longitudinal study. J Bone Miner Res. 2009;24(4):663–8.
McGowan CA, McAuliffe FM. Maternal dietary patterns and associated nutrient intakes during each trimester of pregnancy. Public Health Nutr. 2013;16(1):97–107.
Luke B. Nutrition during pregnancy: Part i, weight gain; part ii, nutrient supplements. JAMA. 1991;265(2):281–2.
Romero-Villanueva D, Dickinson F, Batún JL, Castillo-Burguete MT, Azcorra H. The associations between maternal socioeconomic factors and adequacy of energy and macronutrient intakes in pregnant women from Yucatan Mexico. Food Nutr Bull. 2022;43(2):148–58.
Lee SE, Talegawkar SA, Merialdi M, Caulfield LE. Dietary intakes of women during pregnancy in low-and middle-income countries. Public Health Nutr. 2013;16(8):1340–53.
Blumfield ML, Hure AJ, Macdonald-Wicks L, Smith R, Collins CE. Systematic review and meta-analysis of energy and macronutrient intakes during pregnancy in developed countries. Nutr Rev. 2012;70(6):322–36.
Caulfield L, Elliot V. Nutrition of Adolescent Girls and Women of Reproductive Age in Low-and Middle-Income Countries: Current Context and Scientific Basis for Moving Forward. Arlington, VA: USAID/Strengthening Partnerships, Results, and Innovations in Nutrition Globally (SPRING) Project. 2015.
Agustina R, Rianda D, Lasepa W, Birahmatika FS, Stajic V, Mufida R. Nutrient intakes of pregnant and lactating women in Indonesia and Malaysia: Systematic review and meta-analysis. Front Nutr. 2023;10:1030343.
Juton C, Castro-Barquero S, Casas R, Freitas T, Ruiz-León AM, Crovetto F, et al. Reliability and concurrent and construct validity of a food frequency questionnaire for pregnant women at high risk to develop fetal growth restriction. Nutrients. 2021;13(5):1629.
Parrettini S, Caroli A, Torlone E. Nutrition and metabolic adaptations in physiological and complicated pregnancy: focus on obesity and gestational diabetes. Front Endocrinol. 2020;11:611929.
Ernawati R, Purwaka BT, Prasetyo B. Nutritional status of third trimester pregnant women correlates positively with birth weight. Majalah Obstetri Ginekologi. 2017;25(2):41–7.
Gennaro S, Biesecker B, Fantasia HC, Nguyen M, Garry D. Nutrition profiles of African [corrected] American women in the third trimester. MCN Am J Matern Child Nurs. 2011;36(2):120–6 (PubMed PMID: 21350375. Pubmed Central PMCID: PMC4017625. Epub 2011/02/26. eng).
McGuire JS, Popkin BM. Helping women improve nutrition in the developing world: beating the zero sum game: The World Bank; 1990.
Gluckman SP, Hanson M, Seng CY, Bardsley A, Gluckman P, Hanson M, et al. 33Macronutrients and fibre requirements during pregnancy. Nutrition and Lifestyle for Pregnancy and Breastfeeding: Oxford University Press; 2014.
Elango R, Ball RO. Protein and amino acid requirements during pregnancy. Adv Nutr. 2016;7(4):839S–S844.
Doggui R, Al-Jawaldeh H, El Ati J, Barham R, Nasreddine L, Alqaoud N, et al. Meta-analysis and systematic review of micro-and macro-nutrient intakes and trajectories of macro-nutrient supply in the eastern mediterranean region. Nutrients. 2021;13(5):1515.
Kearney J. Food consumption trends and drivers. Philos Trans R Soc B Biol Sci. 2010;365(1554):2793–807.
Clapp JF III. Maternal carbohydrate intake and pregnancy outcome. Proc Nutr Soc. 2002;61(1):45–50.
Yusuf H, Subih HS, Obeidat BS, Sharkas G. Associations of macro and micronutrients and antioxidants intakes with preeclampsia: A case-control study in Jordanian pregnant women. Nutr Metab Cardiovasc Dis. 2019;29(5):458–66.
Tsakiridis I, Kasapidou E, Dagklis T, Leonida I, Leonida C, Bakaloudi DR, et al. Nutrition in pregnancy: a comparative review of major guidelines. Obstet Gynecol Surv. 2020;75(11):692–702.
Obstetricians Io, Gynaecologists RCoPoI, Strategy DoC, Programmes HSE. Clinical practice guideline. nutrition during pregnancy. 2013.
Acknowledgements
Not applicable.
Funding
No financial assistance was received for this project.
Author information
Authors and Affiliations
Contributions
MKh and FGk conceived the research idea and contributed to the methods/search strategy utilized. FGk conducted the initial literature search; MKh and FGk contributed to reviewing search results. FGk and FBb conducted data extraction and completed data analysis with MKh , CC and AAm. Native text was done by CC. All authors contributed to interpretation of results and critiquing of the manuscript. All authors reviewed and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Khammarnia, M., Ansari-Moghaddam, A., kakhki, F.G. et al. Maternal macronutrient and energy intake during pregnancy: a systematic review and meta-analysis. BMC Public Health 24, 478 (2024). https://doi.org/10.1186/s12889-024-17862-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12889-024-17862-x