Abstract
Background
With the advancing age of the population, and increasing demands on healthcare services, community participation has become an important consideration for healthy ageing. Low levels of community participation have been linked to increased mortality and social isolation. The extent to which community participation has been measured objectively in older adults remains scarce. This study aims to describe where and how older adults participate in the community and determine the feasibility of measurement methods for community participation.
Methods
This observational cross-sectional study obtained data from 46 community dwelling older adults. A combination of Global Positioning Systems (GPS), accelerometry, and self-reported diaries were used over a 7-day monitoring period. Feasibility of methods were determined by calculating the loss of GPS data, questionnaires, and comparison of self-reported locations with GPS co-ordinates. Relationships between community participation, physical activity, social interactions, health related quality of life, sleep quality and loneliness were explored.
Results
Older adults took a median (IQR) of 15 (9.25–18.75) trips out of home over the 7-day monitoring period, most frequently visiting commercial and recreational locations. In-home activities were mainly sedentary in nature, with out of home activities dependent on location type. Self-reported and GPS measures of trips out of home and the locations visited were significantly correlated (self-report 15.7 (5.6) GPS 14.4 (5.8) (r = 0.94)). Significant correlations between both the number of trips taken from home, with social interactions (r = 0.62) and the minutes of moderate to vigorous physical activity (MVPA) (r = 0.43) were observed. Daily MVPA was higher in participants who visited local walk/greenspaces (r = 0.48).
Conclusion
Participants performed more activities with social interactions out of home and visited commercial locations most frequently. The combination of GPS, accelerometry and self-report methods provided a detailed picture of community participation for older adults. Further research is required with older adults of varying health status to generalise the relationships between community participation, location and physical activity.
Trial registration
Ethical approval was gained from the Flinders University Social and Behavioural Research Ethics Committee (protocol no. 8176).
Similar content being viewed by others
Background
With the increasing age of the population and high prevalence of chronic disease, the demands on healthcare systems continue to grow [1]. By 2057, it is estimated that 22% of the Australian population will be aged 65 years and older [2], with costs of ageing expected to rise from $18 billion in 1996, to $24 billion in 2051 [3]. Despite increasing life expectancy, there is no guarantee of ‘healthy’ ageing or quality of life in the latter years [4, 5]. Therefore, the importance of facilitating healthy ageing has increased.
The term ‘community participation’ is defined as ‘engagement in activities occurring outside the home that are complex in nature, social and nondomestic [6].’ These activities may include, meeting with family or friends, taking part in recreational activities, volunteering and cultural or social activities [7, 8]. ‘Social participation’ is defined as ‘a person’s involvement in activities that provide interaction with others in society or the community [9].’ Older adults who participate in such activities have a lower risk of functional disability, increased health related quality of life (HRQOL) and report lower usage of formal healthcare [10, 11]. Community and social participation are therefore key components of healthy ageing [12] and an important consideration for future healthcare delivery [13].
Participating in the community becomes more difficult with increasing age due to increasing frailty and reduced mobility [6]. In order to remain active out of their homes, older adults need to maintain functional mobility, and overcome personal and environmental barriers [14, 15]. Many older adults become dependent on community resources and planned activities for meaningful engagement and social interactions [16]. Despite the benefits of community participation, the evidence is sparse regarding how and where older people participate in their communities. Understanding these factors mayallow for support and interventions specifically targeting the promotion of participation through the latter stages of life.
Factors that determine community participation are not yet fully understood [17]. However, levels of physical activity (PA) and the preservation of functional mobility is vital for participation in community activities [14]. The World Health Organization defines PA ‘as any bodily movement produced by skeletal muscles that requires energy expenditure [18].’ Adults aged over 65 years are recommended to engage in at least 30 min of moderate intensity PA, five times per week, or 75 min of vigorous activity per week [19,20,21]. Despite these guidelines, levels of PA remain particularly low in this age group [22] with reports older people can spend up to 80% of their day sedentary [23]. High levels of sedentary time have been associated with older individuals with chronic conditions and/or walking difficulties [24]. Therefore, increasing or maintaining PA levels allows older adults to participate in and contribute to society, with active community participation in turn leading to increased levels of PA [25].
Furthermore, the social components of activity are important in keeping older adults motivated and engaged, with social isolation and loneliness known to reduce engagement in both the community and PA [26, 27]. Social isolation is defined as an ‘objective lack of relationships and social interaction’ and loneliness as ‘a subjective and distressing feeling [28].’Older adults have an increased risk of social isolation and loneliness stemming from events such as transitioning into retirement [29]. The risks are also linked to poor sleep quality [28], increased blood pressure [30], impaired cognitive function [31] and depression [32]. Social integration of older adults via community participation has been demonstrated to improve quality of life (QoL) [33]. There is a need to explore the factors associated with community participation for older adults, to inform interventions which can maximise QoL and wellbeing.
When developing strategies to increase community participation in older adults, objective measures are required to gain a detailed picture of baseline levels [34]. Despite this, self-reported methods that lack objectivity and often analyse a specific activity rather than daily patterns, continue to be used [34,35,36,37]. With advances in health monitoring technology, there is the potential to use objective measures to measure components related to community participation [36]. Previous research has successfully combined Global Positioning Systems (GPS) with accelerometry allowing for the assessment of indoor and outdoor PA, reflecting unstructured activity in a normal day [38]. Previous recommendations have combined objective measures of PA and outdoor time [39]. Accelerometers measure body movement in real-time, specifically the intensity, frequency, duration and total volume of activity [40]. GPS is a satellite based navigation system, which allows receivers to calculate exact locations [41]. It has the potential to be applied to the assessment of community participation in older adults by measuring the number of outings away from home as a representation of community participation [42,43,44]. The use of GPS combined with accelerometry can determine specific community locations and intensity of activity, despite this, objective reports of community participation for older adults are lacking [45].
Therefore, the primary aim of this study was to describe community participation (specifically by location type and frequency) in community-dwelling older adults and characterise the types of activities in which they engaged. The secondary aim was to investigate the factors associated with community participation, including PA, social interaction, HRQOL, sleep quality and loneliness. The tertiary aim was to determine feasibility of a 7-day monitoring protocol using GPS, accelerometry and self-reported diaries with older adults, and to determine the validity of associated quantitative and qualitative measures.
Methods
This study used an observational cross-sectional design. Ethical approval was gained from the Flinders University Social and Behavioural Research Ethics Committee (protocol no. 8176). Written informed consent was obtained from all participants. Data were collected from November 2018 to May 2019. Methods combined quantitative and qualitative measures of community participation and physical activity, to provide a data rich picture of participation [46].
Participants
For inclusion, participants had to live in metropolitan Adelaide, be able to walk independently (+/− walking aids), speak and understand English, have sufficient cognition to understand the study information and be aged 65 years or over. Individuals were excluded if they were living in residential care facilities. Participants were recruited using flyers advertising the study through local Councils, community centres, social media forums and organisations for older adults. Interested individuals were invited to contact the Principal Researcher (CG) who screened potential participants for eligibility over the phone. The Standardised Mini Mental State Examination (SMMSE) was completed with potential participants to determine whether they had sufficient cognitive capacity to participate in the study, with a score above 25 required for participation [47].
Outcomes
Community participation
Community participation was measured using GPS (Qstarz BT1000XT) to calculate the number of trips away from home, type of location visited and the number of in- and out-of-home activities. The Qstarz BT1000XT device is deemed to be accurate to within 10 m for 79% of ≈68,000 GPS points [48] and a popular device with researchers [42]. GPS data provided co-ordinates of the beginning and end locations of identified ‘loops’ for individual trips. The co-ordinates were viewed on the street view of Google maps [49] to identify the location visited. The types of location were then grouped into the following categories: residential, recreational, commercial, health, local walk/ greenspace, central business district (CBD) and place of worship [8] (Table 1). For each type of location visited out of home, activity diaries were cross-referenced to ascertain the purpose of the visit and to identify possible social interactions. For example, in a commercial location, grocery shopping was identified as a domestic task, yet attending a walking group in a shopping centre was deemed an important social component of community participation.
Self-reported participation diaries were completed by participants to provide the context of community participation. Diaries reported the time, activity, duration, location and social interactions out of the home. Participants recorded sleep and device non-wear. An excerpt is provided in Additional file 3. This information was used to cross-check with the objective data, the accuracy of location where GPS data were missing, and report participation in specific activities.
Community participation- influencing factors
Physical activity was objectively measured with GeneActiv wrist-worn accelerometers, fitted to the non-dominant wrist. GeneActiv accelerometers have been deemed reliable and valid for classifying the intensity of PA in adults [50]. Accelerometer data were used to determine times participants were sedentary, and engaging in light, moderate or vigorous activity. To determine overall daily PA, GeneActiv .bin files were converted to 60-s epoch files and analysed using Cobra software (Francois Frayasse, University of South Australia). Cut points developed by Esliger [50] were used (adjusted for the sampling frequency and epochs) to identify activity intensity (light 283, moderate 605 and vigorous 1697). Sleep was identified using a combination of visual analysis of the activity trace, and self-reported sleep diaries, and subsequently excluded from the analysis.
The number of social interactions experienced were self-reported by participants in participation diaries (Additional file 3), with the total number and location of social interactions identified. HRQOL was measured using the AQOL-8D questionnaire, deemed valid and reliable with larger samples [40]. AQOL-8D utility algorithm was used to calculate scores [51] which were compared with the general population [52], across the following categories: Independent living (IL), Pain, Senses, Mental health, Happiness, Coping, Self-worth and Relationships, with higher scores indicative of greater quality of life. Sleep quality was measured using the Pittsburgh Sleep Quality Index (PSQI), an instrument used to measure the quality and patterns of sleep in older adults [53]. PSQI scores were calculated manually, with scores of 6 and above used to identify poor sleep quality [53]. Levels of loneliness were measured using the De Jong Gierveld loneliness scale which has been validated to measure general, emotional and social loneliness [54]. Scores were calculated, with a score of 6 representing ‘most lonely’ (on a scale of 0–6) [54].
Feasibility of community participation measurement
Loss of GPS hours were calculated to determine the completeness of data collection, according to the expected number of cells recorded [n = 120,960 (5 s epochs)] [44]. The self-reported locations and number of trips out-of-home (total) were manually checked against GPS co-ordinates to determine the accuracy of self-reported location (community participation). Data were linked to Google Maps [49] for graphic representation of where participants were in the community. A maximum time-difference of 10 min was accepted for reported location analysis [55]. On study completion, a 15-item feasibility questionnaire to determine participant experiences of wearing the deviceswas completed [56].
Procedure
Eligible participants attended a face-to-face meeting with the researcher, either in their own home or at the university. At this meeting, participants completed demographic, AQOL-8D, PSQI and De Jong Gierveld loneliness questionnaires and were measured for height and weight using standardised procedures.
Participants were fitted with a Qstarz BT1000XT GPS device (Fig. 1) and GeneActiv triaxial accelerometer (Fig. 2) with device instructions. The researcher explained how to use the devices and assisted with setup for each participant. The GPS device was worn on a lanyard around the neck, attached to a belt loop, on a waist belt or in the participant’s pocket (depending on preference and comfort). The device measured 72.2 mm (L) × 46.5 mm (W) × 20.0 mm (H), weighed 8.5 g and had a battery life of 42 h. The GeneActiv accelerometer was fitted comfortably to the participant’s non-dominant wrist. The device measured 43 mm (L) × 40 mm (W) × 13 mm (H) and weighed 16 g.
Participants were asked to wear the GeneActiv device continually for the 7-day monitoring period (inclusive of sleeping, showering and swimming- as the devices were waterproof). GPS devices were to be worn whenever participants left their home and were removed for water-based activities and overnight for charging. Participants were asked to carry out their normal daily routines whilst wearing the devices. Devices were synchronised to begin recording and obtain 7-days of 24-h data, recording at 5-s epochs, with GeneActiv devices recording at a frequency of 75 Hz. Reminder signs were provided to the participants; the first was to be placed near the bed to prompt charging of the GPS device each night, the second was meant to be placed near the exit to the home to prompt participants to take the GPS device with them.
Participants were provided with the option to receive daily reminders to charge the GPS device via text message during the monitoring period. On day three, all participants were contacted via telephone to discuss any issues and to provide a reminder to charge the GPS device. During the monitoring period, participants kept a written diary detailing their activities. On completion of the study, participants attended an exit meeting where the researcher collected the devices and participation diaries. Participants were then invited to complete the feasibility questionnaire.
Data processing
Signal loss from GPS devices is a common and well-documented issue [43, 44, 57], therefore quality measures were prospectively determined for the inclusion of data sets in the analysis. To be included, GPS data required a minimum of 8- h (480 min) for each day, complete for five of the seven days monitored [58]. For the accelerometer data, to be included in the analysis, a minimum of four valid days, defined as the recording of at least 8-h of waking time, with at least one weekend day required [59, 60].
For the determination of community participation, GPS data were downloaded as .csv files using QSTARZ DataViewer Version 1.37.000 software [61]. GPS data were cleaned to remove title lines that were recorded when GPS signal had been interrupted. GPS data recorded prior to the start of accelerometry monitoring were also removed. Accelerometry data were downloaded using GeneActiv PC Software version 3.2 as .bin files and converted into 5-s epoch .csv files. GPS and accelerometry files were then combined using time stamps with Python coding software version 2.7.14 [62]. These methods allowed for the detection of when and where participants participated in community activity, following recommendations for proper data handling and maintenance of correct time stamps [63]. Self-reported diary entries were recorded in an Excel spreadsheet, where locations reported were grouped into residential, recreational, commercial, health, local walk/greenspace, CBD and place of worship [44]. Activities such as gardening were noted as in-home activities, and reports of social interaction were identified according to location.
Data analysis
Data were entered and analysed using the Statistical Package for Social Sciences (SPSS) [64] with identifying information removed. Questionnaire responses were entered by a researcher and crosschecked by a research assistant. Descriptive analyses were performed for participant demographic data. The normality of data was determined using Z scores [65] with means and standard deviations (SD) reported for normally distributed data, and median and IQR for non-normally distributed data. Spearman correlations were performed to identify the relationships between the number of social interactions, the number of minutes of MVPA, HRQOL, loneliness, and sleep quality scores with the total number of trips away from home and with the number of trips to different locations [66]. Paired t-tests (significance set to alpha of 0.05) were used to determine the accuracy of self-reported location with GPS locations with significance set at < 0.01 for Spearman’s, due to multiple correlations [67, 68].
Results
Participant characteristics
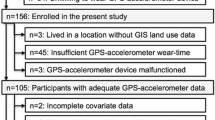
A total of 46 participants (n = 33, 72% female), mean age 74 years (SD 5) participated in the study. The sample demonstrated ‘normal’ cognition [47] with a mean SMMSE score of 29.2 out of 30 (SD 1.3). Thirty-nine percent of participants were married/in de facto relationships and 61 percent were either single, separated or widowed. Participants self-reported an average of two chronic conditions each and all participants reported their general health as good or above (Table 2).
Valid Data sets were obtained for 44 of the 46 recruited participants. Data were excluded from one participant due to equipment malfunction (GeneActiv device). One further data set was excluded as the participation diary was not completed and therefore could not be included in comparisons of self-reported and GPS locations. Following exclusions, of the 7392 h of expected GPS data, 6983 h were recorded. Two participants requested reminders to charge the GPS device and received text messages on days 1, 2, 4, 5 and 6.
Community participation
Overall, participants reported a median (IQR) of 15 (8–18) in-home activities and 18 (14–25) out-of-home activities over the 7-day period, with median (IQR) of 15 (9–19) GPS trips out-of-home. Nine participants reported a single day where they did not leave the house. The median (IQR) number of locations visited outside of the home are presented in Fig. 3, with commercial locations the most frequently visited location type (median 6, range: 3–7), followed by recreational 4 (2–6), local walk/greenspaces 2 (0–6), residential 2 (0–4), CBD 1 (0–2), health 0 (0–1) and place of worship 0 (0–1).
The type of in-home activities reported are detailed in Additional file 1and were mainly sedentary in nature, including reading the paper, computer work, watching television and listening to the radio. The type of out-of-home activities varied with the location (Additional file 1).
Community participation- influencing factors
Physical activity varied between participants, with a daily median of 67 min of moderate-vigorous physical activity (MVPA) (IQR 38–89). A daily median (IQR) of 223 (195–294) minutes were spent performing light activity, 65 (36–89) minutes moderate intensity activity and 20 s (0–117) of vigorous activity. Twenty-seven (61%) participants performed no vigorous activity. The mean sleep time was 480 (SD 58) minutes per night andon average, participants spent 659 min (SD 91) per day sedentary. Wear time was examined for each participant by manually reviewing the GeneActiv activity trace for each day of data collection. There was 100% compliance for the 24 h/d, 7d monitoring protocol for the GeneActiv devices (1440 min/d wear time each day for all participants).
Overall, participants reported a median (IQR) of 2 (0–7) in-home social interactions and 11.5 (8–17) out-of-home social interactions over the 7-days. A median (IQR) of 16.5 (10–21) social interactions were reported over the 7-days (positively skewed 0.24). The median (IQR) number of locations of social interactions over the 7-days is presented in Fig. 4. The most common location type for social interactions was recreational, median (IQR) 3 (1–4) and commercial 3 (1–5) followed by residential 2 (0–4). No social interactions were reported at health, local walk/greenspaces, CBDor places of worship.
The mean (SD) AQOL-8D score for the HRQOL for the general population aged between 65 to 74 years old is 0.83 (0.22) [52], which is matched closely by the participant mean (SD) 0.84 (0.75) in this sample. The study sample reported higher Mental Super Dimension (MSD) scores, mean (SD) 0.84 (0.77), when compared with the general population 0.50 (0.01) which combined mental health, coping, self-worth and relationships [69]. Sleep quality ranged from 1 to 14 on the PSQI with a mean of 5.41 (SD 3) with higher scores indicative of poor sleep quality, 19 (43%) participants scored over 6 [53] indicating poor sleep quality. The study sample detected two participants who scored five out of six on the De Jong Gierveld Loneliness Scale, suggesting feelings of loneliness. The overall mean of the sample was 1.4 (SD 1.4), representing a non-lonely group.
Positive correlations were found between both the trips away from home and social interactions (0.62) and trips away from home and minutes of daily MVPA (0.43) (Table 3). There was a positive correlation between visits to local walk/greenspaces and minutes of daily MVPA (0.48). Increasing age was correlated with reduced minutes of MVPA (0.42). No significant associations were found between trips away from home and HRQOL, loneliness or sleep quality.
Feasibility of community participation measurement
Loss of GPS data ranged from 0 to 91 h (0–54%) per participant, after excluding one data set that did not meet the quality standards for analysis, the overall range was 0 to 50 h lost with a mean of 9.3 h (SD 11.8) over the 7-day monitoring period. The responses to the feasibility questionnaire indicated that devices were easy to carry (82%), comfortable to wear (54%), easy to remember to charge (54%) and remember when leaving the house (59%). Participants also reported that the reminder flyers were useful to assist with charging and remembering devices. Participants reported that participating in the study did not impact their normal routine (78%), disrupt sleep (100%) and was not time consuming (89%).
To determine whether there were differences between out-of-home self-reported locations and GPS co-ordinates, paired t-tests were performed (Table 4). Participants self-reported a significantly higher number of trips out of the home compared with GPS data (p < 0.001). Participant differences between GPS and self-reported trips out of home is provided in Fig. 5. Participants also self-reported a higher number of out-of-home trips to recreational (p = 0.005) and commercial (p = 0.002) locations than observed in the GPS data (Table 4) (t(43) = 3.284, p = 0.002).
Discussion
This study describes the community participation of older adults living in the community, including the types of activities engaged in, and factors associated with participation. Feasibility of monitoring community participation using both objective (GPS, GeneActiv) and self-reported methods (diary) was also explored. Participants performed more activities with social interactions out of home and visited commercial locations most frequently. Additionally, they were very active in terms of daily MVPA, with visits to local walk/greenspaces positively associated with increased activity. The combination of monitoring methods used in this study was feasible with this group of community dwelling older adults.
The self-reported general health of the older adults in this study was good or better, similar to 70% of older adults in Australia [2]. The participants in this study were active, engaging in over an hour of at least moderate intensity PA per day. Interestingly this is slightly higher than that demonstrated in community dwelling older adults in Germany who recorded 49 (± 39) minutes per day (mean age of 65–89) [70] using triaxial GT3X accelerometers are comparable to the Esliger cut points as per this study analysis [50]. Overall, participants HRQOL scores matched Australian population norms for adults aged 65 and over [3, 52], and demonstrated higher Mental Super Dimension (MSD) scores, which could reflect the health status, independence and social participation demonstrated by the participantsin this study [69].
Participants in our study had a lower sleep quality compared to a Chinese cohort when measured using the PSQI outcome measure [71]. This study sample deemed themselves healthier than the general population and were more active than other samples of older adults, measured with comparable methods [70, 72]. Sample bias could have contributed to the high levels of community participation described in this study. It is more likely that a healthy group would self-nominate for a study measuring community participation and physical activity, than would be experienced by the general population and less healthy groups. Thus, the need for interventions and awareness of the importance of community participation could therefore be more urgent than indicated from this sample.
Community participation
The majority of reported social interactions experienced out of home, at recreational and commercial locations, may reflect the high numbers of people and interactions required to access services in these locations (i.e. gaining access to leisure facilities through a receptionist). These results suggest older adults participate in more activities and social interactions out of home than in residential settings. Social interaction is important for keeping older adults motivated and engaged [26] and maintaining cognitive function [31]. Services promoting trips to residential and recreational locations could increase social interactions to promote healthy ageing. Interventions providing social interactions for people who are unable to participate in the community are an important consideration to maximise healthy ageing and should also be considered.
Our findings suggest that higher numbers of trips out of home are related to increased MVPA, with visits to local walk/greenspaces inclusive of PA which reflects previous findings [73]. Services promoting visits to local walk/greenspaces could assist with increasing the physical activity levels of older adults. In-home activities were mainly sedentary in nature, with sedentary time high in this active group, accounting for over 10 h per day [74]. These findings agree with previous research where older adults were found to spend 80% (534 min) of their day sitting [56]. Self-reported diaries highlighted activities that participants engaged in between eating an evening meal and going to bed were predominantly sedentary, concurring with previous research that this time of day can be problematic for accruing sedentary time, with television watching commonly occurring during this time of the day [75,76,77]. Despite participants meeting the MVPA recommendations [19], they spent a lot of time sedentary which suggests there is an opportunity to increase activity and reduce sedentary time even in an active community-dwelling population. Presumably less active older adults with varying levels of health participate in the community far less, which demonstrates the need to increase PA both in and outside of the home.
Feasibility of community participation measurement
Valid data sets were obtained from all participants except two, with self-reported and GPS locations similar on analysis, providing a detail rich picture of community participation. GPS data loss for this study was approximately 6%, acceptable data loss of 13% has previously been reported with a population of stroke survivors [57]. The compliance with the 24 h, 7d wear protocol with the GeneActiv accelerometer was excellent, with none of the participants removing the device during data collection. The successful retrieval of full data sets could be due to high levels of cognition and motivation to follow the protocol, or the reminders included in the protocol to ensure participant adherence. Participants reported that the flyers were useful as a reminder to charge the GPS device and take the devices when leaving the house. Self-reported diaries provided a backup, to determine location and often provided detailed descriptions of the location and activity performed that could not be interpreted from GPS or accelerometry alone [78].
The number of trips out of home were significantly higher when self-reported than detected by GPS, as were trips to recreational and commercial locations. Differences could be due to short-duration trips taken which were not detected by the GPS device, or signal drop out. Despite being significantly different, the difference in visits to recreational and commercial locations equates to half a trip more over the 7-days, which accounts for the difference in self-reported total visits out of home. Clinically these differences would not be important when considering the planning of interventions. The combination of GPS, accelerometry and self-report was feasible with community dwelling older adults and can provide detailed information.
Study strengths and limitations
This study has several methodological strengths and limitations. The study used a cross-sectional design so was unable to determine causal relationships of factors contributing to community participation. The study sample was very active and living independently in the community, with all participants capable of walking independently, therefore the results are not generalisable to all older adults. The potential impact of social desirability bias with potential changes in behaviour of participants as they were wearing monitoring devices and knew the aim of the study was to measure community participation, also needs to be considered.
Sleep scores, as well as other variables may have been affected by the extreme temperatures experienced during data collection. Weather conditions have previously been identified as an important consideration when using this methodology [16]. In this study, monitoring occurred over Summer and Autumn in Adelaide, between the 17th of November 2018 and the 10th of May 2019. As a result, 22 participants carried devices on days with maximum temperatures over 35 degrees Celsius. It is possible that the hot weather may have impacted on daily activity, as well as the types and frequency of trips out of the home. Despite strict protocol, we are unable to guarantee that participants carried the GPS devices for the duration of the monitoring period. However, cross checking GPS data against diary entries were performed to reduce this limitation.
Participants self-reported their social interactions which limits the study, as we are unable to be certain that all participants recorded social interaction in the same way. However, as a measure of social interaction, diaries provided details of social experiences and were analysed as best possible. As far as the authors are aware is the first study to combine GPS, accelerometry and self-reported diaries to determine community participation in community-dwelling older adults.
Conclusion
This study suggests that community dwelling older adults are more socially and physically active out of home. Despite self-reported community participation and GPS locations being similar on analysis, the use of combined methods to provide data rich pictures of community participation is recommended for future studies. This active sample demonstrates the opportunity to increase PA and minimise sedentary behaviour at home, with considerations for both in home activity and community participation required in less active groups to increase PA. Further research is required with other groups of older adults of varying health status (e.g. transitional or residential care) in order to establish possible relationships between community participation, location and PA, in order to design interventions that promote active healthy ageing.
Availability of data and materials
The datasets analysed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- HRQOL:
-
Health related quality of life
- QoL:
-
Quality of life
- PA:
-
Physical activity
- GPS:
-
Global Positioning Systems
- SMMSE:
-
Standardised Mini Mental State Examination
- CBD:
-
Central business district
- PSQI:
-
Pittsburgh Sleep Quality Index
- MVPA:
-
Moderate vigorous physical activity
References
United Nations: World Population Ageing. 2015. http://www.un.org/en/development/desa/population/publications/pdf/ageing/WPA2015_Report.pdf. Accessed 26/08/2020.
Australian Institute of Health and Welfare. Older Australia at a glance. 2018. https://www.aihw.gov.au/reports/older-people/older-australia-at-a-glance. Accessed 26/08/2020.
Department of Health and Aged Care: The Ageing Australian Population and Future Health Costs: 1996–2051. 1999. https://www1health.gov.au/internet/main/publishing.nsf/Content/EAEB162136E3A27ECA257BF0001B0959/$File/ocpanew7.pdf. Accessed 26 Aug 2020.
Sho-Jen C, Huei-Kung Y, Yu-Chi C, Chun-Yen C, Lien W-C, Yang PY, Hu G-C. Physical activity and risk of cardiovascular disease among older adults. Int J Gerontol. 2013;7:133–6.
Beard JR, Officer A, de Carvalho IA, Sadana R, Pot AM, Michel JP, Lloyd-Sherlock P, Epping-Jordan JAE, Peeters GMEE(G), Mahanani WR, Thiyagarajan JA, Chatterji S. The world report on ageing and health: a policy framework for healthy ageing. Lancet. 2016;387(10033):2145–54. https://doi.org/10.1016/S0140-6736(15)00516-4.
Chang F-H, Coster WJ, Helfrich CA. Community participation measures for people with disabilities: a systematic review of content from an international classification of functioning, disability and health perspective. Arch Phys Med Rehabil. 2013;94(4):771–81. https://doi.org/10.1016/j.apmr.2012.10.031.
Vaughan M, Lavalley MP, Alheresh R, Keysor JJ. Which features of the environment impact community participation of older adults? A systematic review and meta-analysis. J Aging Health. 2016;28(6):957–78. https://doi.org/10.1177/0898264315614008.
Theis KA, Furner SE. Shut-in? Impact of Chronic Conditions on Community Participation Restriction among Older Adults. J Aging Res. 2011. https://doi.org/10.4061/2011/759158.
Levasseur M, Richard L, Gauvin L, Raymond E. Inventory and Analysis of Definitions of Social Participation Found in the Aging Literature: Proposed Taxonomy of Social Activities. Soc Sci Med. 2010;71(12):2141–9 Web.
Ashida T, Kondo N, Kondo K. Social participation and the onset of functional disability by socioeconomic status and activity type: The JAGES cohort study. Prev Med. 2016;89:121–8. https://doi.org/10.1016/j.ypmed.2016.05.006.
Munford LA, Sidaway M, Blakemore A, Sutton M, Bower P. Associations of participation in community assets with health-related quality of life and healthcare usage: a cross-sectional study of older people in this community. BMJ Open. 2017;7(2):e012374. https://doi.org/10.1136/bmjopen-2016-012374.
Johnson KJ, Mutchler JE. The emergence of a positive gerontology: from disengagement to social involvement. Gerontologist. 2014;54(1):93–100. https://doi.org/10.1093/geront/gnt099.
George A, Mehra V, Scott K, Sriram V. Community participation in health systems research: a systematic review assessing the state of research, the nature of interventions involved and the features of engagement with communities. PLoS One. 2015;10(10):e0141091. https://doi.org/10.1371/journal.pone.0141091.
Aird R, Buys L. Active aging: exploration into self-ratings of "being active," out-of-home physical activity, and participation among older Australian adults living in four different settings. J Aging Res. 2015;501823. https://doi.org/10.1155/2015/501823.
Papageorgiou N, Marquis R, Dare J. Identifying the enablers and barriers to community participation amongst older adults. Br J Occup Ther. 2016;79(12):742–51. https://doi.org/10.1177/0308022616656195.
van Den Berg P, Kemperman A, de Kleijn B, Borgers A. Locations that support social activity participation of the aging population. Int J Environ Res Public Health. 2015;12(9):10432–49. https://doi.org/10.3390/ijerph120910432.
Pritchard E, Barker A, Day L, Clemson L, Brown T, Haines T. Factors impacting the household and recreation participation of older adults living in the community. Disabil Rehabil. 2015;37(1):56–63. https://doi.org/10.3109/09638288.2014.902508.
WHO. Global Strategy on Diet, Physical Activity and Health. Geneva: World Health Organisation; 2018.
Nelson ME, Rejeski WJ, Blair SN, Duncan PW, Judge JO, King AC, Macera CA, Castaneda-Sceppa C. Physical activity and public health in older adults: recommendation from the American College of Sports Medicine and the American Heart Association. Med Sci Sports Exerc. 2007;39(8):1435–45. https://doi.org/10.1249/mss.0b013e3180616aa2.
Surgeon General's report on Physical Activity and Health. JAMA. 1996;276:522. https://doi.org/10.1001/jama.1996.03540070018010.
Piercy K, Troiano R, Ballard R, Carlso S, Fulton J, Galuska D, George SM, Olson R. The physical activity guidelines for Americans. JAMA. 2018;320(19):2020–8. https://doi.org/10.1001/jama.2018.14854.
Eberhardt M, Ingram I, Makuc DM, et al. Urban and rural health Chartbook: Health, United States; 2001.
Harvey JA, Chastin SF, Skelton DA. How sedentary are older people? A systematic review of the amount of sedentary behavior. J Aging Phys Act. 2015;23(3):471–87. https://doi.org/10.1123/japa.2014-0164.
Rosenberg D, Walker R, Greenwood-Hickman MA, Bellettiere J, Xiang Y, Richmire KR, Higgins M, Wing D, Larson EB, Crane PK, AZ LC. Device-assessed physical activity and sedentary behavior in a community-based cohort of older adults. BMC Public Health. 2020;20:1256.
WHO. Reducing risks, promoting healthy life. Geneva: World Health Organization; 2002.
Yarcheski A, Mahon NE, Yarcheski TJ, Cannella BL. A meta-analysis of predictors of positive health practices. J Nurs Scholarsh. 2004;36(2):102–8. https://doi.org/10.1111/j.1547-5069.2004.04021.x.
Özkan Tuncay F, Fertelli T, Mollaoğlu M. Effects of loneliness on illness perception in persons with a chronic disease. J Clin Nurs. 2018;27:1494–500.
Coyle CE, Dugan E. Social isolation, loneliness and health among older adults. J Aging Health. 2012;24(8):1346–63. https://doi.org/10.1177/0898264312460275.
Shu-Chuan JY, Sing KL. Living alone, social support, and feeling lonely among the elderly. Soc Behav Pers. 2004;32:129–38.
Hawkley LC, Thisted RA, Masi CM, Cacioppo JT. Loneliness predicts increased blood pressure: 5-year cross-lagged analyses in middle-aged and older adults. Psychol Aging. 2010;25(1):132–41. https://doi.org/10.1037/a0017805.
Wilson RS, Krueger KR, Arnold SE, Schneider JA, Kelly JF, Barnes LL, Tang Y, Bennett DA. Loneliness and risk of Alzheimer disease. Arch Gen Psychiatry. 2007;64(2):234–40. https://doi.org/10.1001/archpsyc.64.2.234.
Cacioppo JT, Hawkley LC, Thisted RA. Perceived social isolation makes me sad: 5-year cross-lagged analyses of loneliness and depressive symptomatology in the Chicago health, aging, and social relations study. Psychol Aging. 2010;25(2):453–63. https://doi.org/10.1037/a0017216.
Rowland DT. Population aging: the transformation of societies. Dordrecht: Springer; 2012.
Law M. Participation in the occupations of everyday life. Am J Occup Ther. 2002;56(6):640–9. https://doi.org/10.5014/ajot.56.6.640.
Brusilovskiy E, Klein AK, Salzer MS. Using global positioning systems to study health-related mobility and participation. Soc Sci Med. 2016;161:134–42. https://doi.org/10.1016/j.socscimed.2016.06.001.
George S, Gough C. Evidence for the positive association of physical activity and healthy ageing in longitudinal observational studies. Aust Occup Ther J. 2018;65(4):338–9. https://doi.org/10.1111/1440-1630.12502.
Slootmaker SM, Schuit AJ, Chinapaw MJM, Seidell JC, van Mechelen W. Disagreement in physical activity assessed by accelerometer and self-report in subgroups of age, gender, education and weight status.(Research)(Report). Int J Behav Nutr Phys Act. 2009;6:17.
Nguyen DM, Lecoultre V, Sunami Y, Schutz Y. Assessment of physical activity and energy expenditure by GPS combined with accelerometry in real-life conditions. J Phys Act Health. 2013;10:880.
Kerr J, Sallis JF, SAelens BE, Cain KL, Conway TL, Frank LD, King AC. Outdoor physical activity and self rated health in older adults living in two regions of the U.S. Int J Behav Nutr Phys Act. 2012;9:89.
Strath SJ, Brage S, Ekelund U. Integration of physiological and accelerometer data to improve physical activity assessment. Med Sci Sports. 2005;37(11):563–71.
Gao Z. Technology in Physical Activity and Health Promotion. London: Routledge; 2017. https://doi.org/10.4324/9781315526171.
Gough C, Weber H, George S, Maeder A, Lewis L. Location monitoring of physical activity and participation in community dwelling older people: a scoping review. Disabil Rehabil. 2019. p. 1–14. https://doi.org/10.1080/09638288.2019.1618928.
Kerr J, Duncan S, Schipperjin J. Using global positioning Systems in Health Research: a practical approach to data collection and processing. Am J Prev Med. 2011;41(5):532–40. https://doi.org/10.1016/j.amepre.2011.07.017.
Hordacre B, Barr C, Crotty M. Use of an activity monitor and GPS device to assess community activity and participation in transtibial amputees. Sensors (Basel, Switzerland). 2014;14(4):5845–59.
Li F, Fisher J, Bauman A, Ory M, Chodzko-Zajko W, Harmer P, Bosworth M, Cleveland M. Neighborhood influences on physical activity in middle-aged and older adults: a multilevel perspective. J Aging Phys Act. 2005;13(1):87–114. https://doi.org/10.1123/japa.13.1.87.
Creswell JW. Research design : qualitative, quantitative, and mixed methods approaches. Fifth edition. Thousand oaks, California: SAGE Publications, Inc.; 2018.
Molloy DW. Standardised mini-mental state examination (SMMSE) guidelines for administration and scoring instructions; 2014.
Schipperijn J, Kerr J, Duncan S, Madsen T, Demant Klinker C, Troelsen J. Dynamic accuracy of GPS receivers for use in health research: a novel method to assess GPS accuracy in real-world settings. Front Public Health. 2014;2. https://doi.org/10.3389/fpubh.2014.00021.
Google: Google Maps. 2018.
Esliger WD, Rowlands AV, Hurst TL, Catt M, Murray P, Eston R. Validation of the GENEA accelerometer. Med Sci Sports Exerc. 2011;43(6):1085–93. https://doi.org/10.1249/MSS.0b013e31820513be.
Richardson J, Sinha K, Iezzi A, Khan MA. Modelling utility weights for the assessment of quality of life (AQoL)-8D. Qual Life Res. 2014;23(8):2395–404. https://doi.org/10.1007/s11136-014-0686-8.
Richardson J, Khan MA, Chen G, Iezzi A, Maxwell A. Population norms and Australian profile using hte assessment of quality of life (AQoL) 8D utility instrument: Monash University Centre for Health Economics; 2012.
Buysse DJ, Reynolds CF, Monk TH, Berman SR, Kupfer DJ. The Pittsburgh sleep quality index: a new instrument for psychiatric practice and research. Psychiatry Res. 1989;28(2):193–213. https://doi.org/10.1016/0165-1781(89)90047-4.
Tomás JM, Pinazo-Hernandis S, Donio-Bellegarde M, Hontangas PM. Validity of the de Jong Gierveld loneliness scale in Spanish older population: competitive structural models and item response theory. Soc Behav Health Perspect. 2017;14(4):429–37.
Fillekes MP, Kim E-K, Trumpf R, Zijlstra W, Giannouli E, Weibel R. Assessing older adults’ daily mobility: a comparison of GPS-derived and self-reported mobility indicators. Sensors. 2019;19(20):4551. https://doi.org/10.3390/s19204551.
Lewis LK, Rowlands AV, Gardiner PA, Standage M, English C, Olds T. Small steps: preliminary effectiveness and feasibility of an incremental goal-setting intervention to reduce sitting time in older adults. Maturitas. 2016;85:64–70. https://doi.org/10.1016/j.maturitas.2015.12.014.
McCluskey A, Ada L, Dean CM, Vargas J. Feasibility and validity of a wearable GPS device for measuring outings after stroke. ISRN Rehabil. 2012;2012:1–8. https://doi.org/10.5402/2012/823180.
Carlson JA, Jankowsja M, Meseck K, Godbole S, Natarajan L, Raab F, Demchak B, Patrick K, Kerr J. Validity of PALMS GPS scoring of active and passive travel compared to SenseCam. Med Sci Sports Exerc. 2015;47(3):662–7. https://doi.org/10.1249/MSS.0000000000000446.
Tinlin L, Fini N, Bernhardt J, Lewis L, Olds T, English C. Best practice guidelines for the measurement of physical activity levels in stroke survivors: a secondary analysis of an observational study. Int J Rehabil Res. 2018;41(1):14–9. https://doi.org/10.1097/MRR.0000000000000253.
Innerd P, Catt M, Collerton J, Davies K, Trenell M, Kirkwood TBL, Jagger C. A comparison of subjective and objective measures of physical activity from the Newcastle 85+ study. Age Ageing. 2015;44(4):691–4. https://doi.org/10.1093/ageing/afv062.
Qstarz International Co: QSTARZ Data Viewer Version 1.37.000 software. 2019.
Python Software foundation. Python Languare reference, Version 3.7, available at http://www.python.org. Accessed 27 June 2018.
Hurvitz PM. GPS and accelerometer time stamps: proper data handling and avoiding pitfalls. In: Proceedings of the 1st International ACM SIGSPATIAL Workshop on Smart Cities and Urban Analytics. Bellevue, WA, USA: ACM; 2015. p. 94–100.
IBM Corp. IBM SPSS statistics for windows, version 25. Armonk: IBM Corp; 2018.
Warner RA. Chapter 2 - Using Z Scores for the Display and Analysis of Data. In: Optimizing the Display and Interpretation of Data. Boston: Elsevier; 2016. p. 7–51.
MacFarland TW, Yates JM. In: MacFarland TW, Yates JM, editors. Introduction to Nonparametric Statistics for the Biological Sciences Using R. Cham: Springer International Publishing; 2016. p. 249–97.
Kalinowski P, Fidler F. Interpreting significance: the differences between statistical significance, effect size, and practical importance. Newborn Infant Nurs Rev. 2010;10(1):50–4. https://doi.org/10.1053/j.nainr.2009.12.007.
Cleophas TJ, Zwinderman AH. The Analysis of Efficacy Data. In: Cleophas TJ, Zwinderman AH, editors. Statistics Applied to Clinical Studies. Netherlands: Dordrecht: Springer; 2012. p. 15–39.
Maxwell A, Ozmen M, Iezzi A, Richardson J. Deriving population norms for the AQoL-6D and AQoL-8D multi-attribute utility instruments from web-based data. Qual Life Res. 2016;25(12):3209–19. https://doi.org/10.1007/s11136-016-1337-z.
Ortlieb S, Dias A, Gorzelniak L, Nowak D, Karrasch S, Peters A, Kuhn KA, Horsch A, Schulz H. KORA study group: exploring patterns of accelerometry-assessed physical activity in elderly people. Int J Behav Nutr Phys Act. 2014;11(1):28. https://doi.org/10.1186/1479-5868-11-28.
Zhang HS, Li Y, Qui DX, Zhao J, Luo JL, Lin WQ, Wang JJ, Wang PX. A community-based cross-sectional study of sleep quality in middle-aged and older adults. Qual Life Res. 2017;26(4):923–33. https://doi.org/10.1007/s11136-016-1408-1.
Lohne-Seiler H, Hansen BH, Kolle E, Anderssen SA. Accelerometer-determined physical activity and self-reported health in a population of older adults (65-85 years): a cross-sectional study. BMC Public Health. 2014;14(1):284. https://doi.org/10.1186/1471-2458-14-284.
Stewart OT, Moudon AV, Fesinmeyer MD, Zhou C, Saelens BE. The association between park visitation and physical activity measured with accelerometer, GPS, and travel diary. Health Place. 2016;38:82–8. https://doi.org/10.1016/j.healthplace.2016.01.004.
Matthews CE, Chen KY, Freedson PS, Buchowski MS, Beech BM, Pate RR, Troiana RP. Amount of time spent in sedentary behaviors in the United States, 2003-2004. Am J Epidemiol. 2008;167(7):875–81. https://doi.org/10.1093/aje/kwm390.
Reid NN, Healy MG, Daly GR, Baker WP, Eakin AE, Dunstan DA, Owen NA, Gardiner PA. Twelve-year television viewing time trajectories and physical function in older adults. Med Sci Sports Exerc. 2017;49(7):1359–65. https://doi.org/10.1249/MSS.0000000000001243.
Hu FB, Li TY, Colditz GA, Willet WC, Manson JE. Television watching and other sedentary behaviors in relation to risk of obesity and type 2 diabetes mellitus in women. JAMA. 2003;289(14):1785–91. https://doi.org/10.1001/jama.289.14.1785.
Veitch J, Abbott G, Kaczynski AT, Wilhelm Stanis SA, Besenyi GM, Lamb KE. Park availability and physical activity, TV time, and overweight and obesity among women: findings from Australia and United States. Health Place. 2016;38:96–102. https://doi.org/10.1016/j.healthplace.2015.12.004.
Moran M, Cauwenberg JV, Hercky-Linnewiel R, Cerin E, Deforche B, Plaut P. Understanding the relationships between the physical environment and physical activity in older adults: a systematic review of qualitative studies. Int J Behav Nutr Phys Act. 2014;11(1). https://doi.org/10.1186/1479-5868-11-79.
Acknowledgements
The authors would like to thank Heather Paull for her assistance with data entry.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
CG, LKL, AM and SG were responsible for study conception and design. CB provided statistical advice. CG was responsible for recruitment, data collection and drafting the manuscript with support from LKL, CB, AM and SG. CG, LKL and CB were responsible for data analysis and management. All authors critically reviewed the manuscript for content and style and approved the final version of the manuscript for submission.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Ethical approval was gained from the Flinders University Social and Behavioural Research Ethics Committee (protocol no. 8176). Written informed consent was obtained from all participants.
Consent for publication
Consent for publication of results was obtained.
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Additional file 1.
In-home and out of home activities (Sedentary and active).
Additional file 2.
Process of data analysis.
Additional file 3.
Participant diary excerpt.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Gough, C., Lewis, L.K., Barr, C. et al. Community participation of community dwelling older adults: a cross-sectional study. BMC Public Health 21, 612 (2021). https://doi.org/10.1186/s12889-021-10592-4
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12889-021-10592-4






 represents extreme outlier)
represents extreme outlier)
 represents extreme outlier)
represents extreme outlier)