Abstract
Background
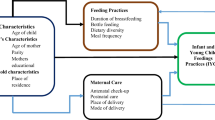
Optimal nutrition during the first two years of a child’s life is critical for the reduction of morbidity and mortality. In Ghana, majority of children miss out on optimal nutrition and only few (13%) of children receive a Minimum Acceptable Diet (MAD). Several studies have investigated the influence of community-level factors on infants and young children feeding (IYCF) practices. However, little is known about the influence of maternal factors on IYCF practices in rural settings. Therefore, this study assessed the influence of maternal factors on the feeding indicators and nutritional status of children aged 6–23 months in two administrative districts in Ghana.
Methods
Data were collected among 935 mothers who had children aged 6–23 months and accessed 21 Child Welfare Clinics within the study area. The study involved a face- to-face interview using structured questionnaires to capture maternal characteristics, dietary intake and anthropometric measurements of children. Multivariate logistic regression was used to study the association between maternal factors and child nutrition outcomes (MAD, dietary diversity score (DDS) and anthropometric indicators) using Stata 16.0 software.
Results
Being employed (AOR = 3.07, 95% CI: 1.71—5.49, p < 0.001) and attaining secondary or higher education (AOR = 2.86, 95% CI: 1.42—5.78, p = 0.003) were significant predictors of children receiving MAD. Similarly, having an average decision-making autonomy increased the child’s odds of receiving MAD (AOR = 1.68, 95% CI: 1.02—2.76, p = 0.040). Children of mothers who attained secondary or a higher level of education (AOR = 0.59, 95% CI: 0.36 -0.97, p = 0.040) and those whose mothers were employed (AOR = 0.71, 95% CI: 0.47—1.07, p = 0.043) were associated with a reduced risk of underweight and stunting respectively. Children of mothers with average financial independence status were more likely to receive diversified meals (AOR = 1.55, 95% CI: 1.01–2.38, p = 0.045).
Conclusions
High educational level and being employed have positive influence on MAD, stunting and underweight of children. High decision-making power and average financial independence of mothers are good predictors of children receiving MAD. Family planning, women empowerment in decision-making, providing employment opportunities for mothers and promoting girl-child education are recommended.
Similar content being viewed by others
Background
The first months of a child’s life (0–23 months) are a very critical phase during which rapid physical and mental development occurs [1]. Consequently, the United Nations Children’s Fund (UNICEF) advocates for and recommends age-appropriate complementary foods and feeding practices to support both physical growth and brain development during the early days of life, before a child attains two years [2].
According to the 2015 Ghana Demographic and Health Survey (GDHS), 19% of children under five years of age were stunted (short for their age), 5% were wasted (thin for their height), and 11% were underweight (low weight for their age) [3]. The national prevalence rates for stunting, wasting and underweight indicate that some positive strides have been achieved in Ghana, particularly when these rates are benchmarked against those in other African countries. However, these figures are still higher than the World Health Organization’s (WHO’s) classification of low prevalence [4]. Again, the prevalence figures for stunting and wasting are higher than the thresholds developed by the WHO–UNICEF Technical Expert Advisory Group on Nutrition Monitoring [5]. Therefore, notwithstanding the progress made, there is still the need to investigate the drivers of child malnutrition in Ghana. This has become necessary in view of the fact that there has been no steady downward trend of the indicators, particularly those that assess compliance to recommended Infant and Young Child Feeding (IYCF) practices which influence the nutritional status of children under two years.
Regarding complementary feeding, findings from the GDHS (2014) revealed that overall, only 15% of breastfed children were able to meet the minimum standards of feeding practices with respect to their dietary diversity score (DDS) and meal feeding frequency (MFF) [3]. Among non-breastfed children aged between 6 and 23 months, only 5% were fed with other milk or milk products at least twice a day, received the minimum meal frequency (MMF) of four solid or semi-solid foods and ate from at least four food groups, apart from the milk or milk products food group [3].
However, in Ghana, regional variations exist with respect to the proportions of children fed on a minimum acceptable diet (MAD)- ranging from 26.9% in the Central Region, 8.5% in the Upper East Region and 4.3% in the Eastern Region. In addition, there are rural–urban disparities with respect to all the IYCF indicators. Whereas 33.5% of children in urban settings were fed from four (4) or more food groups, only 23.6% met the minimum dietary diversity score (DDS) requirement. Similarly, 14.4% of urban children compared with 12.3% of rural children received minimum acceptable diet. Overall, only 13% of children aged between 6 and 23 months were fed a minimum acceptable diet [3]. The reasons behind the regional and habitat differences in MAD in Ghana can be mainly attributed to food insecurity issues confronting most households as a result of worse climatic conditions resulting in poor crop yield and harvest in these regions. In addition, the Eastern Region as a result of the mountainous nature of its geographical location and inaccessible roads makes it difficult to transport food stuffs to most of the districts within the region as compared with regions located in the coastal belt. These findings from the 2014 GDHS reveal that there exists a significant gap in explaining why, in spite of the implementation of the IYCF guidelines, policies and several interventions in Ghana, there is still low compliance with the recommended feeding practices.
Sub-optimal feeding and undernutrition in children is as a result of several complex, multifaceted and interconnected factors. Studies have revealed that factors at the community [6, 7], household [8, 9], maternal [8, 10] and individual [7, 8] levels influence the feeding practices and nutritional status of children. Given that a mother is a child’s primary caregiver and responsible for meal planning, cooking and feeding of children, a study that examines how maternal socio-economic characteristics influence the nutritional status of children under-two years is key towards addressing childhood undernutrition.
Furthermore, most of the previous studies that were conducted to assess the determinants of the nutritional status of children in Ghana focused on children under- five years [11,12,13,14] and these relationships are yet to be determined among children under two (2) years. Again, these previous studies did not focus on some maternal variables (parity, financial independence and participation in decision-making at the household level) and how they influence feeding practices and nutritional status of children under two (2) years. This study therefore focused on children under two years because it is an early stage in life to identify probable determinants of sub-optimal feeding practices and poor nutritional status before it results in irreversible outcomes of stunting and poor cognitive development. This is imperative because basic nutrition interventions when implemented early in life can avert a quarter of child mortalities and one-third of chronic malnutrition [15].
Therefore, this study assessed maternal factors associated with the various IYCF indicators (MDD and MAD) of infants and young children aged between 6 and 23 months.
In addition, the study assessed maternal factors that influence the nutritional status (using the anthropometric indicators of stunting, underweight and wasting) of infants and young children aged between 6 and 23 months.
Methods
Study design
The study adopted a cross-sectional design in which quantitative data were collected.
Study setting
The Eastern Region of Ghana was selected for this study because, according to the GDHS (2015) report, only 4.3% of children residing in that region received a minimum acceptable diet compared to the national average of 13%. Specifically, this study was conducted in two districts − the Kwahu Afram Plains North District (KAPND) and the Kwahu Afram Plains South District (KAPSD) − which were ranked as the first and second districts with the highest prevalence of underweight children in the Eastern Region in both 2016 and 2017 (Eastern Region Health Directorate, 2016; 2017).
Study population
The study participants included 935 mothers with their under-two-year-old children who were randomly selected from 21 randomly selected Child Welfare Clinics (CWCs) in the two districts. These mothers accessed the CWCs for growth monitoring and promotion services for their young children.
Inclusion criteria
Eligibility criteria for infants included healthy singleton infants with ages between 0 and 23 months, gestational ages between 37 and 42 weeks, birthweight between 2,500 and 4,000 g, and without metabolic or physical problems. The gestational age and birth weight of the children were considered because available evidence indicates that a short gestational age, pre-term/premature or low birthweight infants are at higher risk of growth and nutritional deficits during the first year of life [16, 17]. The eligibility criteria for prospective study participants were assessed by checking the child’s health record booklet with the assistance of the nurses in-charge at the CWCs. Specifically, information on each child’s birthweight, birth defects or medication conditions was obtained from the health record booklet and formed the basis for determining their eligibility to participate in the study.
Exclusion criteria
Children who were twins were excluded from this study since the evidence regarding the differences between their nutritional status and that of singletons is inconsistent [18]. In addition, children whose twin siblings died during labour or birth were not considered. A child was also excluded if he/she had a chronic or congenital illness or any medical condition that interfered with either feeding (e.g. cleft palate) or the taking of body measurements.
Sample size
The sample size required for the study was estimated using the prevalence of underweight among children under-five years for the Kwahu Afram Plains North and South Districts in 2016, which are 22.0% and 16.3% respectively (District Health Directorate Report, 2016). The prevalence of underweight was used because it is a composite indicator reflecting both chronic and acute malnutrition and therefore, related to both stunting and wasting. This ensured that all the three indices of nutritional status were captured. On the average, prevalence for both the North and South districts was 19.2%, and the minimum sample size was estimated using the formula:
\(\mathrm n\:=\:\mathrm Z^{2\ast}\mathrm p^\ast(1-\mathrm p)/\mathrm e^2\) where Z = confidence level, p = proportion of underweight children in the combined districts and e = precision [19].
With a confidence level of 95%, Z = 1.96, e = 2.8% and p = 10.8%, the minimum sample size estimated was 765 children. Making a provision of 20% contingencies, a sample size of 912 (rounded up to 950) infants and children aged between 6 and 23 months was estimated for this study.
Sampling method
A two-stage sampling strategy was employed in this study. Firstly, a total number of 21 health facilities (constituting one-third of total health facilities) were randomly selected from a total of 63 health facilities within the two districts. Secondly, mothers and their children aged between 6 and 23 months were recruited from the 21 randomly selected health facilities for the study. The total number of infants and young children who visit the CWCs in the selected health facilities on a monthly basis was obtained. Based on this information, the study participants were randomly selected proportionally to obtain the sample size.
Ethical considerations and participant approval
Ethical approval and clearance for the study was granted by the Dodowa Health Research Centre’s (DHRC) Institutional Review Board (IRB) of the Ghana Health Service (Reference/Identification: DHRCIRB/04/02/18) and the IRB of the University of Cape Coast (Reference/Identification: UCCIRB/CHLS/2018/02). Permission to conduct the study was also obtained from the Regional Health Directorate, the two District Health Management Teams (DHMT) and the Directors of Health Services in the 21 health facilities which were selected for the study. Informed consent to participate in the study was obtained from all study participants and mothers consented on behalf of their children. The participants consented to participant in the study by either thumb-printing or signing an informed-consent form. To ensure data confidentiality, participants were assigned unique identifiers instead of names.
All data collection methods were carried out in accordance with relevant ethical guidelines of the Ghana Health Service Ethical Review Committee and the University of Cape Coast Ethical Review Board. The regulations involved in the conduct of this research involving study participants also took into consideration the Helsinki Declaration.
Study instrument
A structured questionnaire was used. The questionnaire solicited for information on socio-demographic characteristics of the mother such as marital status, parity, highest level of education attained, employment status and caregiver's autonomy (decision-making power and financial independence). In addition, information on background characteristics of the index child such as sex, age, birth order and birth weight were collected. Furthermore, information on each caregiver's feeding practices for the index child was obtained by administering a 24-h dietary recall and a seven-day food group frequency questionnaire (FGFQ).
Anthropometric assessment of children
Anthropometric measurement was carried out to determine the nutritional status of the children by accessing for height-for-age z-score (HAZ), weight-for-age z-score (WAZ) and weight-for-height z-score (WHZ). The recumbent length of children who were unable to stand upright was measured using an infantometer (UNICEF model, item no. 0114500). The World Health Organization’s guidelines for taking weight and length/height in children were followed for all the anthropometric measurements [20]. Children’s heads were held vertically against the head plate with the back, body and legs straight and flat in the centre of the measuring board, the knees straightened, the heels and feet firmly positioned by the researcher vertically against the footplate. Both length and height measurements were taken to the nearest 0.1 cm. A beam balance scale was used to take their weights to the nearest 0.1 kg. All weighing scales were calibrated daily using certified standardized weight test loads of 10 kg and 25 kg by setting it to zero prior to taking weight measurements. It was ensured that all weights were measured with light clothing and no shoes. Both height and weight measurements were taken in duplicates and the average recorded.
Dietary assessment of children
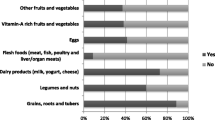
A single 24-h Dietary recall (24HDR) method and a seven-day food group frequency questionnaire (FFQ) were used to collect information on all foods (including school meals) and beverages consumed by the children. The mothers were asked to recall all the foods and drinks given to the child during the previous day and also the number of times that they fed their children the previous day. Information about the number of times (food group frequency) a child had eaten from a particular food group during the past seven days was collected using a food group frequency questionnaire. The seven food groups included grains/roots/tubers; legumes/nuts; dairy; flesh foods; eggs; vitamin A-rich fruits and vegetables; other fruits and vegetables [21]. Mothers were asked to recall the number of days in a week that children ate from each of the seven food groups.
Data collected using the 24HDR was used to estimate the minimum dietary diversity score (MDD) of the children. A child was considered to have met the requirement of being fed on a minimum dietary diversity if he/she ate from at least four out of the seven food groups during the day or night preceding the survey. The number of times that children had been offered meals in the past 24 h was used to estimate the minimum meal feeding frequency (MFF) of the children. The minimum acceptable diet (MAD) was estimated using the minimum DDS and the MFF. The children were sub-divided into four groups (less than 6 months, 6–8 months, 9–11 months, and 12 months and above) during the analysis of the feeding practices data to represent the variations in feeding recommendations for their different age groups. The scoring system for the IYCF indicators were dependent on the age group of each child and the current WHO feeding recommendations for that particular age group.
Assessment of nutritional status
The WHO Anthro software (World Health Organization, 2011) was used to transform the weight and length/height of the infants into the growth indices -weight-for-age, weight-for-length and length-for-age z-scores. Infants with z-scores less than -2 standard deviations from the median reference length-for-age/ height-for-age, weight-for-height/weight-for-length and weight-for-age z-scores were classified as stunted, wasted and underweight, respectively.
Assessment of child feeding indicators
Dietary diversity score (DDS)
The WHO recommends that children aged between 6 and 23 months should be given foods from at least four food groups each day to meet their minimum dietary diversity score. On the basis of this recommendation, a child in any age group who was not fed from any food group or fed from only three or less food groups in a day earned a score of 0. A score of 1 was assigned to a child who was fed from four food groups, and a score of 2 was given to children in the age groups 6–8 months and 9–12 months if more than 4 food groups are consumed. The scoring system that was applied in the study was based on the scoring pattern for the feeding indicator of dietary diversity score as applied in previous studies [22, 23]. A child aged between 13 and 23 months was given a score of 3 if she consumed more than four food groups within a 24-h period before the caregiver is interviewed. This is because of WHO’s emphasis on feeding children above 12 months from a wide variety of foods and gradually substituting their usual infant foods with family foods.
Meal feeding frequency (MFF) score
Meal feeding frequency (MFF) score refers to the number of times that a child consumes solid or semi-solid foods within a day, including meals and snack. The MFF scoring pattern applied in this study was based on WHO’s recommendations on the number of meals that children belonging to the various age-groups should be fed daily in addition to breastfeeding and as described and applied in previous studies [22, 23]. On the basis of WHO’s recommendations, a score of zero (0) was given to children aged 6–8 months who were fed complementary foods 0–1 times, 1 when fed two times, and a score of 2 when fed more than two times (> 2) over a 24-h period prior to interviewing the mother. For children in the age groups of 9–12 months and 13–23 months, a score of 0 was awarded if a child was fed 0–2 times in a day, a score of 1 was given when a child ate complementary foods three times in a day, and a score of 2 was awarded when a child ate complementary foods more than three times in a day [21].
Minimum acceptable diet (MAD)
It is a composite indicator for assessing feeding practices among 6–23 months old children and considers whether the child has been fed a minimum number of times (MFF) and on a diversified diet (MDD) daily [21]. Scoring and coding of the MAD indicator was done by applying the scoring pattern of previous studies [22, 23]
Coding of maternal decision-making power and financial independence
A mother’s household decision-making autonomy was based on responses to 15 questions which covered themes on decisions in the respondent’s household about obtaining healthcare, large household purchases, visits to family or relatives, and child healthcare. Each of the questions had four (4) response options – respondent alone, respondent and husband/partner jointly, husband/partner alone and any other household member which were coded as 4, 3, 2 and 1 respectively. The total scores which were between 15 and 60 were re-categorised as low (15–30), medium/average (31- 45) and high (46–60) decision making power similar to the coding of mother’s household decision-making level in related studies [24, 25].
Control and access over finances or financial independence of a mother was assessed based on her responses to 12 questions. Seven (7) of the questions assessed a mother’s ability to have control over money to buy perishable food items, clothes, medicine, toiletries, jewelry, gifts for parents or other family members. Each of the questions had two response options namely- respondent has control (Yes) and no control (No). “Yes” and “No” were coded as 1 and 0 respectively. The other 5 questions assessed the mother’s ability to save a portion of the money she had earned, spend her earnings as she wished and have a say in how the household’s overall income should be spent. Each of these 5 questions were given three response options – no/never, yes/some of the time and yes/ all the time which were coded as 0, 1 and 2 respectively. The total scores ranged between 0 and 17 and were categorised into low (0–8), medium/average (9–12) and high (13–17) financial independence similar to the coding of levels in related studies [24, 26].
Data quality control
The questionnaire was first developed in English and translated to the two local dialects (Ewe and Akan) and back to English to maintain its consistency and readjustments of inconsistent and inaccurate data. Prior to the actual data collection, the questionnaire was pretested on 20 women at Bruben CHPS Zone to ascertain the reliability, language clarity and simplicity of the tools. The questionnaire was checked for completeness daily by the supervisors and the principal investigator. The data collection period was between August and December, that is the minor rainy season, when food is usually in abundance to the beginning of the dry season (December) when food is a little bit scarce.
Variables of the study
Dependent variables
Dietary diversity score (poor, average, good), minimum acceptable diet (adequate, inadequate) and anthropometric indicators (height-for-age z-score [not stunted, stunted], weight-for-age z-score [not underweight, underweight] and weight-for-height z-score [not wasted, wasted]).
Independent variables
Maternal- related variables which were categorical in nature included age (< 20, 20–30, 31–40, > 40) marital status (single [never married], cohabiting, married, separated/divorced, widowed) number of living children (parity) (1–3, 4–6, > 6), number of mothers with children under two years of age (1, 2, 3), employment status (not employed in the last 12 months, not currently employed but worked in past 12 months, currently employed),work status/schedule throughout the year (work throughout the year, work seasonally/part of the year, work only once in a while), form of remuneration/payment (cash only, cash and in kind, in kind only), mother’s highest level of education attained (none, primary, JHS/JSS, secondary, tertiary) decision making power (low, medium/average) and financial independence (low, medium/average, high).
Statistical analysis
Socio-demographic characteristics of study participants were described using frequencies and their corresponding percentages. Multinomial logistic regression was used to examine the association between maternal-related factors and the outcome dietary diversity score (DDS) which was a categorical variable with three levels. Binary logistic regression was employed to determine the association between maternal-related factors and minimum acceptable diet (MAD) which was the outcome with two levels. Binary logistic regression was used to determine the influence of maternal factors on anthropometric indicators (height-for-age, weight-for-height and weight-for-age outcomes). The regression models were constructed by firstly determining the independent maternal factors that were significant in the bivariate models at the significance level of 0.05. Subsequently, all the maternal factors that were significant in the bivariate models were used to construct the multivariate models. All statistical tests were two-tailed and p-values < 0.05 were considered to be statistically significant. Stata software (version 15.0) was used for the statistical analysis.
Results
Socio-demographic characteristics of participants
Most of the mothers (65.6%) had number of children between 1 and 3 (Table 1). Approximately 75% (75.2%) and 36% (35.6%) were married and employed respectively. About 18% (17.9%) of the caregivers reported that they did not receive any remuneration for work they were engaged in at the time of the study. Most of the mothers (33.9%) had JHS/JSS and 17.8% of them had no formal education. Slightly above half of the mothers had average decision- making power (51.1%) and low financial independence (52.5%). With regard to the children, the proportion of females (50.2%) was slightly larger than that of the males (49.8%). The highest proportion of children were between the ages of 12 and 24 months (35.2%).
Feeding practices of the children
The majority (63%) of the children had inadequate minimum dietary diversity score (63.0%) and highest proportion (77.9%) did not receive minimum acceptable diet (Table 2). However, most of them (59.6%) of them had adequate minimum meal frequency (Table 2).
In the multivariate multinomial logistic model, maternal factors that were associated with the DDS of children were marital status, employment status, work schedule throughout the year, mother’s highest level of education and financial independence of mothers (Table 3). Children whose mothers were married (AOR = 2.82, 95% CI: 1.45–5.52, p = 0.002) and those whose mothers were separated, divorced or widowed (AOR = 3.07, 95% CI: 1.11–8.48, p = 0.030) had increased likelihood of having a good DDS as compared to those whose mothers had never married. Regarding marital status, children of married mothers were 2.82 times more likely to have a good DDS compared with those whose mothers were single (AOR = 2.82, 95% CI: 1.45—5.52, p < 0.002). Similarly, children of mothers who were separated, divorced or widowed were 3.07 times more likely to have a good DDS compared with those whose mothers were single (AOR = 3.07, 95% CI: 1.11—8.48, p = 0.030) (Table 3). Children of mothers who were currently employed (AOR = 2.74, 95% CI: 1.61—4.68, p < 0.001) and those with mothers not currently employed but worked in the past 12 months (AOR = 1.68, 95% CI: 1.02—2.78, p = 0.042) had higher odds of having a good DDS. Children whose mothers worked only once a while were 48% less likely to have average DDS as compared to those whose mothers worked consistently throughout the year (AOR = 0.52, 95% CI: 0.28—0.98, p = 0.044). Children who had mothers with primary (AOR = 2.79, 95% CI: 1.55—5.02, p = 0.001), JHS/JSS (AOR = 2.65, 95% CI: 1.46—4.80, p = 0.001) and secondary or higher level of education (AOR = 3.15; 96% CI:1.57—6.33, p = 0.001) were more likely to have a good DDS as compared to those whose mothers had no formal education. In addition, children whose mothers had secondary or higher level of education (AOR = 2.02; 96% CI:1.00—4.06, p = 0.049) had increased likelihood of having an average DSS. Children of mothers with average (AOR = 1.64, 95% CI: 1.05—2.55, p = 0.029) and high (AOR = 1.55, 95% CI: 1.01—2.38, p = 0.045) financial independence statuses were more likely to have a good DDS compared to those of mothers with a low level of financial independence (Table 3).
In the multivariate logistic regression, the maternal factors that were associated with the outcome MAD were employment status, highest level of education attained and decision-making power (Table 4). The children of mothers who were currently employed (AOR = 3.07, 95% CI: 1.71—5.49, p < 0.001) and those whose mothers were not employed during the survey but worked in the past 12 months prior to the survey (AOR = 1.96, 95% CI: 1.10—3.47, p = 0.022) had increased likelihood of receiving MAD as compared to those whose mothers were not employed in the last 12 months prior to the survey. Children whose mothers had primary (AOR = 2.44, 95% CI = 1.24—4.75, p = 0.009), JHS/JSS (AOR = 2.24, 95% CI = 1.15—4.33, p = 0.017) and secondary or higher level of education (AOR = 2.86, 95% CI = 1.42—5.78, p = 0.003) were more likely to receive MAD compared to children whose mothers had no formal education. Additionally, children of mothers with an average decision-making autonomy had higher odds of receiving MAD (AOR = 1.68, 95% CI = 1.02—2.76, p = 0.040) (Table 4).
Association between maternal-related factors and children’s nutritional status
The various multivariate binary logistic regressions in Table 5 shows that the number of children under two years of age that a mother had was a predictor of stunting (HAZ) and underweight (WAZ). Children of mothers who had 2 or 3 children under two years were more likely to be stunted (AOR = 1.88, 95% CI: 1.23—2.87, p = 0.003) in comparison with those whose mothers had only one child under two years of age. Similarly, children whose mothers had 2 or 3 children under 2 years had higher odds of being underweight (AOR = 1.53, 95% CI: 1.02 – 2.30, p = 0.039). Children of currently employed mothers were 29% less likely to be stunted compared to those whose mothers were not employed in the last 12 months prior to the survey (AOR = 0.71, 95% CI: 0.47 – 0.97, p = 0.043). The children whose mothers had primary (AOR = 0.55, 95% CI: 0.35 – 0.88, p = 0.012), JHS/JSS (AOR = 0.55, 95% CI: 0.36 – 0.89, p = 0.015) and secondary or higher level (AOR = 0.49, 95% CI: 0.28 – 0.86, p = 0.014) of education had lower odds of being wasted as compared to those whose mothers had no formal education. Additionally, children of mothers who had secondary or higher level of education had reduced risk of being underweight (AOR = 0.59, 95% CI: 0.36 – 0.97, p = 0.040). Compared with children whose mothers had low financial independence, those whose mothers had average financial independence were 44% less likely to be wasted (AOR = 0.66, 95% CI: 0.45 – 0.95, p = 0.025).
Discussion
The findings indicate that 63.0% of the children had an inadequate minimum dietary diversity score (DDS), implying that the diet of a lot of the children in the two districts lack diversity. The finding is similar to a study conducted in Ghana in which only 24.7% of the children had a dietary diversity score of at least 4 out of 7 food groups [11]. However, unlike the situation with respect to the DDS, more than 50% of the children met the minimum feeding frequency (MFF) requirement recommended for their age. In other related studies, it was also observed that whereas most children met the requirement for the minimum feeding frequency, less than half were fed on meals prepared from a wide range of food groups [27, 28]. This could be because although most of the children may be eating meals frequently in the day, these meals are monotonous cereal and starch-based diets, without much variety. Another possible reason that can be adduced for the high MFF but low DDS is that, in the current population, most of the households mainly feed on their farm produce. If they do not grow different food crops, there is a high probability that they would be feeding on monotonous meals. It was observed in a study conducted in rural Ethiopia that households which do not feed mainly on their own agricultural produce are more likely to consume more diverse diets [29]. Likewise, another study revealed that dietary diversity score was significantly higher among non-farming households than farming households [30]. The implication of this finding is the need to educate farming households in rural settings on the importance of feeding children on diversified foods and not only from farm produce or advocate for interventions that encourage diversification of farm production.
A related finding was that most of the children (77.9%) were not receiving a minimum acceptable diet (MAD), largely because the majority of the children were not being fed on highly diversified meals from different food groups although the data suggested that they ate frequently during the day. These results confirm previous studies that most children with ages between 6 and 23 months do not receive a minimum acceptable diet, mainly because they are not fed from a wide range of different food groups, in spite of the majority meeting the requirement for a minimum meal frequency [27, 31].
The study revealed that children whose mothers have highest level of education and also being employed throughout the year are received an adequate DDS and MAD. This finding corroborates the findings of studies conducted in the Philippines [32], Timor-Leste [33], six south Asian countries [34], Ethiopia [35] and Kenya [36]. This finding could be attributed to the ability of educated mothers to read, understand and apply information from nutrition education materials provided when they access child health facilities. Besides, women who attain high levels of education may be more likely to have access to more nutritional information and understand educational messages delivered through different media outlets. This ultimately assist them to follow optimal child feeding practices. In addition, highly educated mothers are more likely to secure jobs with regular monthly salaries which empower them to have more resources to provide their children with adequate and varied meals. It is therefore not surprising that this study observed a relationship between the educational level of a mother and her employment status. A meta-analysis of 50 Demographic and Health Surveys, reported that children of employed women, compared with those of unemployed women, had higher odds of achieving a minimum DDS and MAD [37]. However, the findings are contrary to conventional wisdom advocating for maternal employment in other studies in Bangladesh [38] and Vietnam [39], where maternal employment was found to be detrimental to child’s feeding and nutritional status. This observation was made because although maternal employment increased the income levels of mothers, it ended up decreasing the quantity of time that was spent caring for the nutritional needs of their children.
Children of married mothers were found to be more likely to have a good DDS and be fed on a minimum acceptable diet, compared with those whose mothers were single. These findings are in line with that of studies conducted in India [40], Ethiopia [41] and Benin [42] in which children of single mothers had low DDS and MFF. This finding accentuates the important role of fathers or husbands in ensuring that their children are optimally fed, and the entire household is food-secured. Another explanation is the high poverty levels among single mothers who often single-handedly have to provide for all the needs of their children, including their dietary intakes. This finding is contrary to observations in studies conducted in Ethiopia [43] and China [44] that children of single mothers have a better DDS compared with those of married mothers. The differences in these findings could be attributed to the time spent by mothers to care for male-partners, sometimes to the disadvantage of children, which may adversely influence their nutritional intakes. In other cases, married women, particularly in impoverished settings, who are likely to be confronted by food insecurity may aim at pleasing their husbands by feeding them first, giving them the best part of the meal and large portion sizes, to the detriment of their children and themselves. This assertion is confirmed by an earlier study which found that, mothers in poverty-stricken areas in Bangladesh feed their husbands first and later on eat the leftovers with their children [45].
One of the findings also revealed that children of mothers with at least an average financial independence were more likely to have a good DDS, just as observed in similar studies in Lao People's Democratic Republic [24] and Uganda [25]. This might be explained by the fact that such mothers were employed and therefore in a better position to provide nutritious and highly diversified diets for their children. Indeed, the data showed that more than 65% of the mothers with high financial independence were employed at the time of the study, whereas majority (70.7%) of the mothers with low financial independence were not employed. In situations where women are uneducated and unemployed, they are likely to depend on their spouses for financial resources to meet their own needs and those of their children. Such mothers may lack the purchasing power to provide a sufficiently varied diet for their children. In addition, their opinions on financial decisions and the allocation of resources in the household may not be considered by the head of the household, mainly because they may hardly contribute any monetary resources to the total income of the household and its upkeep. Again, such women with low autonomy may not even have much control over their own money earned from selling farm produce or from their small businesses.
Similarly, mothers who had at least an average ability to participate in decision-making at the household level were more likely to feed their children on a minimum acceptable diet as reported in related studies conducted in Nepal [46], Timor-Leste [33] and Bangladesh [47]. A possible explanation for this finding is that when mothers are involved in household decision-making, it could empower them to feed diversified foods to ensure optimal growth of their children. Another explanation is that in this study population, majority of mothers (78.0%) reported that their husbands made final decisions on how the household income should be used. Therefore, assuming a low proportion of the household income is allocated to food then the one in charge of preparing food, most probably the mother, may have to ensure that the money she had at hand met their dietary needs.
With respect to the association observed between maternal factors and the anthropometric indicators, parity of a mother was a significant predictor variable of underweight and stunting in children, corroborating previous studies [48, 49]. This could be due to the fact that, as the number of children increases, it causes a strain on family resources, as well as predisposing the children more to growth failures. A possible reason is that having a large number of children may lead to competition for both household resources and mother’s time and strength required for care-giving. Competition for the limited available dietary resources at home might cause each child to receive sub-optimal care, which includes feeding frequently and adequately on different nutritious food sources. In the present study, the highest level of educational attainment by a mother was a significant predictor variable of both underweight and wasting in children. This finding confirms the results of previous studies that a high educational level of mothers impacts the nutritional status of children [50,51,52,53]. There are plausible explanations as to why a higher maternal education reduces the risk of wasting and underweight among children. First, mothers who are educated to a higher level are at an advantage in processing interpreting and applying nutrition and health information that concerns their children's nutritional and health needs. Such information as is likely to be possessed by educated mothers can enable them to make informed decisions about their children’s nutrition and health care, thus leading to improved child and better health outcomes, such as a reduced risk of wasting and underweight in children. The study revealed that mother's current employment status and financial independence have influence on stunting, and this finding is in line with findings from other developing countries, such as the Lao People's Democratic Republic [24], Malawi [54] and India [55]. The plausible explanation might be that employed mothers may earn a regular income and use it beneficially for their children's health and nutrition.
In the current study, a significant association was found between a mother’s employment status and her financial independence. Further analysis of the data revealed that more than 65% of the mothers with high financial independence were employed at the time of the study whereas majority (70.7%) of the mothers with low financial independence were not employed at the time of the study. These findings suggest that the financial status of mothers who are employed improves and ultimately have a positive impact on their children’s dietary intakes and growth. However, studies carried out in Tanzania [56], Nepal [57] and Bangladesh [38] have found out that unemployed mothers are less likely to have stunted children, compared with employed mothers. The possible reason attributed to this finding by some of the authors is that unemployed mothers may have adequate time to provide their children with nutritious meals. Hence, this could have contributed to the prevention of stunting.
In addition, findings from the current study indicate that a mother's ability to actively participate in decision making at the household level protects her children from wasting. Findings of studies conducted in Nigeria [58], (Bangladesh, Nepal, Pakistan, and Myanmar) [59] and Burkina Faso [60] supports this finding. The possible reason attributed to this finding is that mothers with high decision-making power have control over resources and are likely to take decisions independently. This may subsequently influence choices positively to promote the survival and growth of their children. The findings thus contribute data for rural farming settings which can guide development of nutrition interventions for mothers to help tackle the problems of childhood undernutrition. For example, the findings suggest that educating and empowering mothers to be gainfully employed in order for them to be financially independent is vital in improving their children’s nutritional status.
One of the strength of this study is that, the sex distribution of children who participated in this study reflects the national situation of having slightly more females than males. Additionally, two height and weight measurements were taken on each child to minimize measurement variability and great emphasis was placed on daily calibration of the weight measuring instruments. Maternal autonomy factors like financial-independence and decision-making power were included in this study unlike previous related studies in Ghana. Although, strengths of this study have been outlined, it also has some few limitations. The study has a limitation of being cross-sectional and therefore causality cannot be established. Besides, the use of the 24-h dietary recall tool and a seven-day food group frequency questionnaire (FFQ) to assess dietary intakes relied on participants’ self-reported data, which were prone to recall and social desirability biases.
Since this is a cross-sectional study, it will be appropriate to conduct further studies which have longitudinal designs. Such longitudinal studies will enable researchers to assess for seasonal variations and its impact on feeding and nutritional status of children. Again, in future studies, a form for recording daily dietary intake of children could be given to individuals in selected households who can read and write to assist mothers to complete, (especially in cases where mothers are unable to read or write). By employing such a method, recall bias of children’s dietary intake is likely to be reduced among mothers. Also, another suggestion for further studies is to assess the influence of other maternal factors such as nutritional knowledge, access to nutrition education materials, counselling services and maternal dietary diversity scores on dietary intake and nutritional status of children. Future studies could assess how the other dimensions of maternal autonomy such as freedom of association, freedom of physical movement, access to economic resources/control over assets, barriers to health care access and attitude toward violence (wife-beating by husband, and experience of violence at home) influence the nutrition of children.
Conclusions
Maternal factors such as a high educational level, stable employment, decision-making power at the household-level, financial independence and low parity contribute to ensuring optimal dietary intakes and improved nutritional status of young children. Therefore, education on the importance of child nutrition, family planning, crop diversification, women empowerment in decision-making, providing employment opportunities for mothers and improvement in girl-child education are recommended in child nutrition health interventions in rural settings.
Availability of data and materials
The datasets generated and/or analyzed during the current study are not publicly available due to some sensitive information on women autonomy issues in the cultural setting of participants which could compromise the privacy and anonymity of mothers who participated in the study but are available from the corresponding author (cbuxton@ucc.edu.gh) or the University of Cape Coast, Institutional Review Board at irb@ucc.edu.gh on reasonable request.
Abbreviations
- 24HDR:
-
24-Hour Dietary recall
- AOR:
-
Adjusted Odds Ratio
- CWC:
-
Child Welfare Clinics
- DHMT:
-
District Health Management Teams
- FFQ:
-
Food frequency questionnaire
- GDHS:
-
Ghana Demographic Health Survey
- GHS:
-
Ghana Health Service
- GSS:
-
Ghana Statistical Service
- HAZ:
-
Height-for-age
- IYCF:
-
Infant and Young Child Feeding
- KAPND:
-
Kwahu Afram Plains North District
- KAPSD:
-
Kwahu Afram Plains South District
- LAZ:
-
Length-for-age
- MAD:
-
Minimum Acceptable Diet
- MDD:
-
Minimum Dietary Diversity
- MFF:
-
Minimum Feeding Frequency
- MMF:
-
Minimum Meal Frequency
- UNICEF:
-
The United Nations Children’s Fund
- WAZ:
-
Weight-for-age z-score
- WHO:
-
World Health Organization
- WHZ:
-
Weight-for-height z-score
- WLZ:
-
Weight-for-length z-score
References
UNICEF. From the first hour of life: making the case for improved infant and young child feeding everywhere. New York: UNICEF; 2016. p. 8.
UNICEF. Nutrition, for every child: UNICEF Nutrition Strategy 2020–2030. New York: United Nations Children’s Fund: UNICEF,; 2020.
Gss G, Demographic IG, Health survey,. Rockville, Maryland. USA: Ghana Statistical Service (GSS), Ghana Health Service (GHS) and ICF International; 2014. p. 2015.
United Nations Children’s Fund (UNICEF), World Health Organization, International Bank for Reconstruction and Development/The World Bank. Levels and trends in child malnutrition: key findings of the 2019 Edition of the Joint Child Malnutrition Estimates. Geneva: World Health Organization; 2019. Licence: CC BY-NC-SA 3.0 IGO.
De Onis M, Borghi E, Arimond M, Webb P, Croft T, Saha K, De-Regil LM, Thuita F, Heidkamp R, Krasevec J, Hayashi C. Prevalence thresholds for wasting, overweight and stunting in children under 5 years. Public Health Nutr. 2019;22(1):175–9.
Ghosh S. Factors responsible for childhood malnutrition: A review of the literature. Curr Res Nutr Food Sci J. 2020;8(2):360–70.
Khanam M, Shimul SN, Sarker AR. Individual-, household-, and community-level determinants of childhood undernutrition in Bangladesh. Health Serv Res Manage Epidemiol. 2019;16(6):2333392819876555.
Adedokun ST, Yaya S. Factors associated with adverse nutritional status of children in sub-Saharan Africa: evidence from the demographic and health surveys from 31 countries. Matern Child Nutr. 2021;17(3):e13198.
Mkhize M, Sibanda M. A review of selected studies on the factors associated with the nutrition status of children under the age of five years in South Africa. Int J Environ Res Public Health. 2020;17(21):7973.
Saleh A, Syahrul S, Hadju V, Andriani I, Restika I. Role of maternal in preventing stunting: a systematic review. Gac Sanit. 2021;1(35):S576–82.
Frempong RB, Annim SK. Dietary diversity and child malnutrition in Ghana. Heliyon. 2017;3(5):e00298.
Acquah E, Darteh EK, Amu H, Adjei DK. Predictors of underweight in children under-five years in Ghana. Ghana Med J. 2019;53(1):71–8.
Boah M, Azupogo F, Amporfro DA, Abada LA. The epidemiology of undernutrition and its determinants in children under five years in Ghana. PLoS ONE. 2019;14(7):e0219665.
Aryeetey R, Atuobi-Yeboah A, Billings L, Nisbett N, van den Bold M, Toure M. Stories of Change in Nutrition in Ghana: a focus on stunting and anemia among children under-five years (2009–2018). Food Security. 2021;8:1–25.
Mekonnen M, Kinati T, Bekele K, Tesfa B, Hailu D, Jemal K. Infant and young child feeding practice among mothers of children age 6 to 23 months in Debrelibanos district, North Showa zone, Oromia region, Ethiopia. PLoS ONE. 2021;16(9):e0257758.
Gutbrod T, Wolke D, Soehne B, Ohrt B, Riegel K. Effects of gestation and birth weight on the growth and development of very low birthweight small for gestational age infants: a matched group comparison. Arch Dis Child Fetal Neonatal Ed. 2000;82(3):F208–14.
Zoleko-Manego R, Mischlinger J, Dejon-Agobé JC, Basra A, Mackanga JR, Akerey Diop D, Adegnika AA, Agnandji ST, Lell B, Kremsner PG, Matsiegui PB. Birth weight, growth, nutritional status and mortality of infants from Lambaréné and Fougamou in Gabon in their first year of life. PLoS ONE. 2021;16(2):e0246694.
Bentil HJ, Steiner-Asiedu M, Lartey A. Comparison of the complementary feeding practices between mothers with twins and mothers with singletons. Pan Afr Med J. 2016;24:52.
Suresh KP, Chandrashekara S. Sample size estimation and power analysis for clinical research studies. J human Reprod Sci. 2012;5(1):7.
World Health Organization. WHO child growth standards: length/height-for-age, weight-for-age, weight-for-length, weight-for-height and body mass index-for-age: methods and development. Geneva: WHO Press, World Health Organization; 2006.
WHO, USAID, UCDavis IF. IF. Indicators for assessing infant and young child feeding practices. Geneva: World Health Organization; 2008.
Chaudhary SR, Govil S, Lala MK, Yagnik HB. Infant and young child feeding index and its association with nutritional status: a cross-sectional study of urban slums of Ahmedabad. J Fam Community Med. 2018;25(2):88.
Lohia N, Udipi SA. Infant and child feeding index reflects feeding practices, nutritional status of urban slum children. BMC Pediatr. 2014;14(1):1–1.
Kamiya Y, Nomura M, Ogino H, Yoshikawa K, Siengsounthone L, Xangsayarath P. Mothers’ autonomy and childhood stunting: evidence from semi-urban communities in Lao PDR. BMC Womens Health. 2018;18(1):1–9.
Ickes S, Mandel MP, Roberts A. The maternal domain: social support, decision-making, psychological health and child feeding and anthropometry in Uganda. FASEB J. 2016;30:891–6.
Abate KH, Belachew T. Women’s autonomy and men’s involvement in child care and feeding as predictors of infant and young child anthropometric indices in coffee farming households of Jimma Zone, South West of Ethiopia. PLoS ONE. 2017;12(3):e0172885.
Ali M, Arif M, Shah AA. Complementary feeding practices and associated factors among children aged 6–23 months in Pakistan. PLoS ONE. 2021;16(2):e0247602.
Ariyo O, Aderibigbe OR, Ojo TJ, Sturm B, Hensel O. Determinants of appropriate complementary feeding practices among women with children aged 6–23 months in Iseyin, Nigeria. Scientific African. 2021;1(13):e00848.
Hirvonen K, Hoddinott J. Agricultural production and children’s diets: evidence from rural Ethiopia. Agric Econ. 2017;48(4):469–80.
Christian AK, Marquis GS, Colecraft EK, Lartey A, Soueida R. Household food insecurity but not dietary diversity is associated with children’s mean micronutrient density adequacy in rural communities across Ghana. Nutrition. 2019;1(65):97–102.
Sema A, Belay Y, Solomon Y, Desalew A, Misganaw A, Menberu T, Sintayehu Y, Getachew Y, Guta A, Tadesse D. Minimum Dietary Diversity Practice and Associated Factors among Children Aged 6 to 23 Months in Dire Dawa City, Eastern Ethiopia: A Community-Based Cross-Sectional Study. Glob Pediatr Health. 2021;8:2333794X21996630.
Guirindola MO, Maniego ML, Silvestre CJ, Acuin CC. Determinants of meeting the minimum acceptable diet among Filipino children aged 6–23 months. Philipp J Sci. 2018;147(March):75–89.
Bonis-Profumo G, Stacey N, Brimblecombe J. Maternal diets matter for children’s dietary quality: Seasonal dietary diversity and animal-source foods consumption in rural Timor-Leste. Matern Child Nutr. 2021;17(1):e13071.
Tariqujjaman M, Hasan MM, Mahfuz M, Hossain M, Ahmed T. Association between mother’s education and infant and young child feeding practices in South Asia. Nutrients. 2022;14(7):1514.
Molla A, Egata G, Getacher L, Kebede B, Sayih A, Arega M, Bante A. Minimum acceptable diet and associated factors among infants and young children aged 6–23 months in Amhara region, Central Ethiopia: community-based cross-sectional study. BMJ Open. 2021;11(5):e044284.
Kemboi S, Mungiria-Mituki D, Ramkat R, Termote C, Covic N, Cheserek MJ. Variation in the factors associated with diet quality of children aged 6 to 23 months in low and high Agroecological zones of Rongai Subcounty Kenya. Food Nutr Bull. 2020;41(2):186–99.
Oddo VM, Ickes SB. Maternal employment in low-and middle-income countries is associated with improved infant and young child feeding. Am J Clin Nutr. 2018;107(3):335–44.
Jakaria M, Bakshi RK, Hasan MM. Is maternal employment detrimental to children’s nutritional status? Evidence from Bangladesh. Rev Dev Econ. 2022;26(1):85–111.
Bui QN, Hoang TX, Le NT, Tran TS. Women’s employment and well-being of children under 5 years in Vietnam. Asia Pacific Journal of Public Health. 2018;30(8):708–16.
Dhami MV, Ogbo FA, Diallo TM, Olusanya BO, Goson PC, Agho KE. Global Maternal and Child Health Research Collaboration (GloMACH). Infant and young child feeding practices among adolescent mothers and associated factors in India. Nutrients. 2021;13(7):2376.
Abebe H, Gashu M, Kebede A, Abata H, Yeshaneh A, Workye H, Adane D. Minimum acceptable diet and associated factors among children aged 6–23 months in Ethiopia. Ital J Pediatr. 2021;47(1):1.
Mitchodigni IM, Amoussa Hounkpatin W, Ntandou-Bouzitou G, Avohou H, Termote C, Kennedy G, Hounhouigan DJ. Complementary feeding practices: determinants of dietary diversity and meal frequency among children aged 6–23 months in Southern Benin. Food Security. 2017;9(5):1117–30.
Agize A, Jara D, Dejenu G. Level of knowledge and practice of mothers on minimum dietary diversity practices and associated factors for 6–23-month-old children in Adea Woreda, Oromia. Ethiopia BioMed Res Int. 2017;2017:7204562.
Tian X, Wang H. The impact of having one parent absent on children’food consumption and nutrition in China. Nutrients. 2019;11(12):3077.
Lentz EC. Complicating narratives of women’s food and nutrition insecurity: Domestic violence in rural Bangladesh. World Dev. 2018;1(104):271–80.
Kulkarni S, Frongillo EA, Cunningham K, Moore S, Blake CE. Women’s bargaining power and child feeding in Nepal: Linkages through nutrition information. Matern Child Nutr. 2020;16(1):e12883.
Khandoker, S., & Singh, A. (2021). Women’s decision making autonomy in household and its effect on dietary diversity: evidence from nationally representative panel data of Bangladesh.
Sobgui CM, Fezeu LK, Diawara F, Diarra H, Afari-Sefa V, Tenkouano A. Predictors of poor nutritional status among children aged 6–24 months in agricultural regions of Mali: a cross-sectional study. BMC nutrition. 2018;4(1):1–3.
Sserwanja Q, Kamara K, Mutisya LM, Musaba MW, Ziaei S. Rural and urban correlates of stunting among under-five children in Sierra Leone: a 2019 Nationwide cross-sectional survey. Nutr Metab Insights. 2021;14:11786388211047056.
Javid N, Pu C. Maternal stature, maternal education and child growth in Pakistan: a cross-sectional study. AIMS Public Health. 2020;7(2):380.
Le K, Nguyen M. Shedding light on maternal education and child health in developing countries. World Dev. 2020;1(133):105005.
Li Z, Kim R, Vollmer S, Subramanian SV. Factors associated with child stunting, wasting, and underweight in 35 low-and middle-income countries. JAMA network open. 2020;3(4):e203386.
Vikram K, Vanneman R. Maternal education and the multidimensionality of child health outcomes in India. J Biosoc Sci. 2020;52(1):57–77.
Chilinda ZB, Wahlqvist ML, Lee MS, Huang YC. Higher maternal autonomy is associated with reduced child stunting in Malawi. Sci Rep. 2021;11(1):1–2.
Kumar R, Lakhtakia S. Women’s empowerment and child stunting in India: an investigation. Journal of Population and Social Studies [JPSS]. 2021;29:47–66.
Debela BL, Gehrke E, Qaim M. Links between maternal employment and child nutrition in rural Tanzania. Am J Agr Econ. 2021;103(3):812–30.
Kondratjeva O, Sam AG, Mishra K. Impact of mother’s employment on children’s nutrition: evidence from Nepal; 2021.
Ariyo T, Jiang Q. Maternal autonomy and childhood undernutrition: Analysis of 2018 Nigeria demographic and health survey. J Child Health Care. 2022;17:13674935221108012.
Anik AI, Rahman MM, Rahman MM, Tareque MI, Khan MN, Alam MM. Double burden of malnutrition at household level: A comparative study among Bangladesh, Nepal, Pakistan, and Myanmar. PLoS ONE. 2019;14(8):e0221274.
Heckert J, Olney DK, Ruel MT. Is women’s empowerment a pathway to improving child nutrition outcomes in a nutrition-sensitive agriculture program?: Evidence from a randomized controlled trial in Burkina Faso. Soc Sci Med. 2019;1(233):93–10.
Acknowledgements
The authors would like to acknowledge the tremendous efforts of the Research Team from the District Health Management Team (DHMT) for assisting with data collection and engaging with the study participants. The DHMT research team includes Mr. David Kwame Tsotorvor, Mrs. Victoria Parkoo, Mr Fabrics Asinyo, Mr Frank Kwasi Arthur and Mr Isaac Manford. The authors appreciate the study participants for providing a receptive environment for the study to be conducted. We also acknowledge all the support, technical advice and assistance in many ways given by the District Health Directors, Mr. Robert Kweku Bio and Mrs. Joana Amankwah, during the data collection period in the two districts.
Funding
The authors received no specific funding for this work.
Author information
Authors and Affiliations
Contributions
CNA conceived the idea for the study, administered 24-h recalls and conducted interviews and collected anthropometric data and wrote the initial manuscript; GA conducted statistical analysis and testing and informed interpretations of the findings; DTD and SA were involved in the conceptualization, provided advise on the data analysis, reviewed the nutrition analyses and informed interpretations and supervised the entire study. All authors contributed to the design of the study approved the final draft of the manuscript before submission.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Ethical clearance was obtained from the Institutional Review Board at the University of Cape Coast (Reference/Identification: UCCIRB/ CHLS/2018/02) and the Dodowa Health Research Centre’s (DHRC) Institutional Review Board (IRB) of the Ghana Health Service (Reference/Identification: DHRCIRB/04/02/18). Informed consent to participate in the study was obtained from all study participants. We also received written or thumb-printed consent from mothers of all selected children. All data collection methods were carried out in accordance with relevant ethical Guidelines of the Ghana Health Service Ethical Review Committee and the University of Cape Coast Ethical Review Board. The regulations involved in the conduct of this research involving humans also took into consideration the Helsinki Declaration.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Nsiah-Asamoah, C., Adjei, G., Agblorti, S. et al. Association of maternal characteristics with child feeding indicators and nutritional status of children under-two years in Rural Ghana. BMC Pediatr 22, 581 (2022). https://doi.org/10.1186/s12887-022-03651-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12887-022-03651-1