Abstract
Background
Pregnancy begins with a fertilized ovum that normally attaches to the uterine endometrium. However, an ectopic pregnancy can occur when a fertilized egg implants and grows outside the uterine cavity. Tubal ectopic pregnancy is the most common type (over 95%), with ovarian, abdominal, cervical, broad ligament, and uterine cornual pregnancy being less common. As more cases of ectopic pregnancy are diagnosed and treated in the early stages, the survival rate and fertility retention significantly improve. However, complications of abdominal pregnancy can sometimes be life-threatening and have severe consequences.
Case presentation
We present a case of intraperitoneal ectopic pregnancy with fetal survival. Ultrasound and magnetic resonance imaging showed a right cornual pregnancy with a secondary abdominal pregnancy. In September 2021, we performed an emergency laparotomy, along with additional procedures such as transurethral ureteroscopy, double J-stent placement, abdominal fetal removal, placentectomy, repair of the right uterine horn, and pelvic adhesiolysis, in the 29th week of pregnancy. During laparotomy, we diagnosed abdominal pregnancy secondary to a rudimentary uterine horn. The mother and her baby were discharged eight days and 41 days, respectively, after surgery.
Conclusions
Abdominal pregnancy is a rare condition. The variable nature of ectopic pregnancy can cause delays in timely diagnosis, resulting in increased morbidity and mortality, especially in areas with inadequate medical and social services. A high index of suspicion, coupled with appropriate imaging studies, can help facilitate its diagnosis in any suspected case.
Similar content being viewed by others
Explore related subjects
Find the latest articles, discoveries, and news in related topics.Background
Ectopic pregnancy refers to any pregnancy in which the developing products of conception implant outside the endometrial cavity. Although the actual prevalence is unknown and may be higher because of the lack of standardized reporting systems and available outpatient treatment options, approximately 2% of pregnancies are ectopic [1]. Ectopic pregnancies are the leading cause of first-trimester mortality and are responsible for approximately 4% of all pregnancy-related mortalities [2, 3].
Abdominal pregnancy, which is an embryo or fetus in the abdominal cavity, is extremely rare, and is divided into primary and secondary types. In primary abdominal pregnancy, the embryo embeds in the normal fallopian tubes and ovaries, without uteroplacental fistula, and attaches completely to the peritoneal surface in the early stages of pregnancy [4, 5]. Secondary abdominal pregnancy often occurs after abortion or rupture of the fallopian tube pregnancy [6], and occasionally, it is secondary to ovarian or uterine pregnancy with uterine defects (such as a uterine scar, fissure, or peritoneal fistula). When the embryo falls into the abdominal cavity, part of the villus tissue remains attached to the original implantation site and grows outwards, attached to the pelvic peritoneum and adjacent organ surfaces. Abdominal pregnancy is often accompanied by abnormal placentation and insufficient blood supply, which compromises the ability of the fetus to survive to full term.
Case presentation
A 22-year-old woman, G3P1, was admitted in August 2021 after being referred from a local hospital for amenorrhea of 23 weeks and 5 days duration.
Before referral, an ultrasound scan in the seventh week of her pregnancy showed she had a congenital uterine malformation suspicious of a bicornuate uterus. The scan also revealed an intrauterine pregnancy in one cavity, a live embryo, a small amount of fluid around the pregnancy sac, and what appeared to be some fluid in the other uterus. Her previous pregnancy, five years earlier, culminated in an emergency cesarean section for intrauterine fetal distress. She claimed to have a bicornuate uterus.
After admission, an ultrasound scan showed a live fetus in the abdominal cavity with the placenta on the right side of the abdominal cavity instead of in the endometrium. We diagnosed the woman with a case of abdominal pregnancy.
In September 2021, during the 29th week of her pregnancy, the patient experienced intermittent abdominal pain for 3 h. Magnetic resonance imaging (MRI) (Figs. 1 and 2) revealed an abdominal pregnancy and rupture of the fetal membranes. We performed an emergency laparotomy and found part of the omentum adherent to the anterior abdominal wall and a live fetus of the same gestational age on the left side of the abdominal cavity.
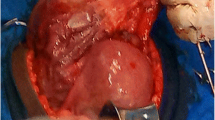
During the surgery, we performed procedures such as transurethral ureteroscopy, double J-stent placement, transabdominal fetal removal, placentectomy (Fig. 3), right uterine cornual repair, and pelvic adhesiolysis. We found that the amniotic membrane had ruptured, but there were no clear ascites or amniotic fluid in the abdominal and pelvic cavities. In the right pelvic cavity, an amniotic sac covered the placenta, which was attached to the right uterine horn. The placental implantation site was approximately 2 cm × 3 cm, the placental size was approximately 15 cm × 10 cm, and the fetal membrane was wrapped around it. The uterus was enlarged, equivalent to the size of a 60-day gestation, soft, and showed no abnormalities in the appearance of the bilateral appendages. The right fallopian tube and the ovarian ligament were approximately 1 cm from the implantation site. We separated the adhesions between the omentum and the anterior abdominal wall, carefully explored the pelvic and abdominal cavities, and found the placenta implanted in the right uterine horn with no evidence of pelvic, abdominal organ, or large vessel involvement.
We delivered a live male infant in the left sacro-anterior position (LSA) weighing 1200 g, with a body length of 38 cm and a head circumference of 27 cm. The APGAR scores at 1 min and 5 min after birth were 10 and 10, respectively. The placenta weighed approximately 500 g.
The placenta was attached to the right uterine horn, and the left uterine horn was normal. The fetus and placenta entered the abdominal cavity by rupturing the right uterine horn. The placenta was attached to the right uterine horn, sealing the rupture. The surgeon repaired the right uterine horn after delivering the placenta.
The patient had an uneventful recovery and was discharged eight days after surgery. The discharge diagnosis was rudimentary uterine horn pregnancy and secondary abdominal pregnancy. Immediately after birth, the newborn was transferred to the Neonatal Intensive Care Unit (NICU) for further management. He was diagnosed with bronchopulmonary dysplasia, neonatal respiratory distress syndrome, intrauterine infectious pneumonia, premature encephalopathy, jaundice of premature infants, anemia of premature infants (moderate), sclerema neonatorum (mild), hyperthermia, and fetal growth restriction. He also had hypoalbuminemia, hyperkalemia, and vitamin D deficiency. Eventually, he was discharged from the hospital after 41 days of NICU management. A follow-up was scheduled for this patient, but she did not have regular follow-up.
Discussion
This report describes the manifestation, diagnosis, and treatment of a rare clinical condition. The patient’s ultrasound examination at the local hospital suggested a bicornuate uterus. However, during surgery, we found that the patient had a unicornuate uterus instead of a bicornuate uterus, and this rare rudimentary uterine horn pregnancy ended up as a secondary abdominal pregnancy. This highlights the importance of using surgical findings for making a final diagnosis in such cases.
Surgical management of ectopic pregnancy is required when a patient presents with hemodynamic instability, symptoms of an ongoing ruptured ectopic mass (such as pelvic pain), or signs of intraperitoneal bleeding [7]. The terms ‘uterine horn’, ‘bicornuate uterus’ and ‘unicornuate uterus’ are often confused. The uterine horn is a normal part of the female internal genitalia that connects the fallopian tubes to the uterus. A bicornuate uterus describes an irregularly shaped uterus with two cavities of varying dimensions, while a unicornuate uterus has only one fallopian tube and an abnormally shaped uterine cavity. Both bicornuate and unicornuate uteri are congenital uterine anomalies that are relatively rare and can lead to pregnancy complications.
Ectopic pregnancy is a serious acute abdominal condition that occurs in 1 to 2% of all pregnancies. Uterine horn pregnancy is an exceedingly rare condition that arises from the implantation and subsequent growth of a fertilized ovum within a rudimentary horn of the uterus. The muscular wall of the congenitally malformed uterus is often dysplastic and cannot support the growth and development of the fetus. Complete or incomplete rupture of the myometrium usually occurs between 14 and 20 weeks of gestational age. After uterine rupture, the fetus is extruded into the abdominal cavity, and the placenta adheres to the pelvic peritoneum and adjacent organs, as occurred in this case. In an abdominal pregnancy, abnormal placentation and insufficient blood supply make it difficult for the fetus to survive to full term. Fortunately, the placenta was attached to the right uterine horn with adequate blood supply, allowing the fetus to survive until 28 weeks of gestational age.
Diagnosing uterine horn pregnancy is difficult, particularly in the early stages, when typical symptoms are absent or may not appear until the second trimester. Therefore, we should focus on high-risk factors for ectopic pregnancy, such as uterine malformation, assisted reproduction, endometriosis, a history of pelvic inflammatory disease and conservative fallopian tube treatment [8]. Currently, Studdiford’s criteria are often used clinically to diagnose abdominal pregnancy. A primary abdominal pregnancy occurs when the embryo embeds in the normal fallopian tubes and ovaries without uteroplacental fistula and attaches completely to the peritoneal surface in the early stages of pregnancy [5]. Abdominal pregnancies usually present with abdominal or gastrointestinal symptoms during pregnancy [9], but their diagnosis is often challenging. Although prenatal follow-up and ultrasound scans are commonplace, many cases are still missed, and 40–50% of cases are diagnosed during surgery [10]. A careful abdominal examination often reveals a uterus with barely recognizable normal contour but easily palpable fetal limbs, abnormal fetal position, abnormally clear fetal heart sounds, and a loud placental murmur. If the B-mode ultrasound diagnosis is inconclusive or highly suggestive of abdominal pregnancy, MRI should be performed when the patient’s condition is stable [11]. In poor economic areas where MRI examination is unavailable, or the professional skills of B mode ultrasound doctors are limited, clinicians must always have a high index of suspicion in patients with fetal motion pain to enhance the safety of both fetus and mother [12].
The incidence of abdominal pregnancy among all ectopic pregnancies is less than 1%, but the mortality rate is much higher than that of tubal pregnancy [13, 14]. Therefore, surgery is recommended immediately after the diagnosis of abdominal pregnancy. However, in rare cases, if maternal and fetal monitoring is normal, pregnancy may continue into the fetal survival period [15].
As the placenta can attach to the uterine wall, intestine, mesentery, liver, spleen, bladder, or ligaments, women with abdominal pregnancies are at high risk of bleeding during surgery. In 2018, Marcelin et al. reported an advanced abdominal pregnancy treated with embolization of the placenta after removal of the fetus by laparotomy. Following reduced blood supply, the placenta was resected four weeks later, with reduced blood loss and risk of organ injury [16]. Preoperative evaluation and preparation are critical, including preoperative vascular embolization, uterine artery embolization, ureteral stenting, intestinal preparation, adequate blood preparation, and involvement of a multidisciplinary rescue team. The management of the placenta should be considered carefully. Removing the placenta after the delivery of the fetus during surgery would depend on the placental attachment site and whether the fetus is alive or dead.
We reviewed the literature to identify other case reports of abdominal ectopic pregnancies. We searched PubMed and Google Scholar using the search terms “unicornuate uterus,” “bicornuate uterus,” “ectopic pregnancy,” “abdominal ectopic pregnancy,” and “heterotopic pregnancy”. The reported cases and data are summarized in Table 1. The literature described different laparoscopic approaches for rudimentary horn pregnancies, most of which involved pregnancies in the first or second trimester. With the help of ultrasound, the diagnosis was missed in only one case. The preoperative diagnosis in these cases included isthmic, ectopic, tubal ectopic, cornual, abdominal, rudimentary horn pregnancies, and even acute abdomen. The pregnancy was in the left horn in 4 of the 11 cases, and one case involved a ruptured abdominal pregnancy.
Conclusions
Abdominal pregnancy resulting from uterine horn pregnancy is extremely rare. Early diagnosis is crucial for patients at high-risk, including those with uterine malformations, a history of ectopic pregnancy or pelvic inflammatory disease, and those who underwent assisted reproduction. A high index of suspicion and appropriate investigations are necessary to identify this condition. Secondary abdominal pregnancy arises when the pregnancy is located outside the uterus, leading to potentially adverse maternal and fetal issues. Failure to diagnose a uterine horn pregnancy promptly could cause cornual rupture and internal hemorrhage. This case report emphasizes the importance of early detection and management of abdominal pregnancy.
Availability of data and materials
The datasets used and/or analyzed in this study are available from the corresponding author upon reasonable request.
Abbreviations
- MRI:
-
Magnetic Resonance Imaging
- LSA:
-
Left Sacro-Anterior
- HCG:
-
Human Chorionic Gonadotropin
- RHP:
-
Rudimentary Horn Pregnancy
- LS-RHE:
-
Laparoscopic Rudimentary Horn Excision
References
Hofseth LJ, Hebert JR, Chanda A, Chen H, Love BL, Pena MM, et al. Early-onset colorectal cancer: initial clues and current views. Nat Rev Gastroenterol Hepatol. 2020;17:352–64.
Berg CJ, Callaghan WM, Syverson C, Henderson Z. Pregnancy-related mortality in the United States, 1998 to 2005. Obstet Gynecol. 2010;116:1302–9.
Creanga AA, Shapiro-Mendoza CK, Bish CL, Zane S, Berg CJ, Callaghan WM. Trends in ectopic pregnancy mortality in the United States: 1980–2007. Obstet Gynecol. 2011;117:837–43.
Thang NM, Anh NTH, Thanh PH. Rectal ectopic pregnancy: A case report. Medicine. 2021;100:e24626.
Dubey S, Satodiya M, Garg P, Rani M. Primary abdominal pregnancy: a case report. J Clin Diagn Res. 2016;10:QD04.
Fessehaye A, Gashawbeza B, Daba M, Arusi M, Terefe T. Abdominal ectopic pregnancy complicated with a large bowel injury: a case report. J Med Case Rep. 2021;15:1–5.
American College of Obstetricians and Gynecologists. ACOG Practice Bulletin No. 193: tubal ectopic pregnancy. Obstetrics Gynecol. 2018;131:e91-e103.
Ku CW, Ong I, Chan JKY, Ee TX. Abdominal heterotopic pregnancy post-IVF double embryo transfer. BMJ Case Rep. 2022;15:e246649.
Hailu FG, Yihunie GT, Essa AA, Tsega WK. Advanced abdominal pregnancy, with live fetus and severe preeclampsia, case report. BMC Pregnancy Childbirth. 2017;17:243.
Sib SR, Ouédraogo I, Sanogo M, Kiemtoré S, Sawadogo YA, Zamané H, et al. A full term abdominal pregnancy with an isthmic tubal implantation of the placenta. BMC Pregnancy Childbirth. 2018;18:448.
Diagnosis and Management of Ectopic Pregnancy: Green-top Guideline No. 21. BJOG. 2016;123:e15-e55.
Paluku JL, Kalole BK, Furaha CM, Kamabu EM, Mohilo GM, Kataliko BK, et al. Late abdominal pregnancy in a post-conflict context: case of a mistaken acute abdomen - a case report. BMC Pregnancy Childbirth. 2020;20:238.
Fessehaye A, Gashawbeza B, Daba M, Arusi M, Terefe T. Abdominal ectopic pregnancy complicated with a large bowel injury: a case report. J Med Case Rep. 2021;15:127.
Yoder N, Tal R, Martin JR. Abdominal ectopic pregnancy after in vitro fertilization and single embryo transfer: a case report and systematic review. Reprod Biol Endocrinol. 2016;14:69.
Sarr ISS, Faye M, Faye PM, Seck M, Ka O, Dieng M. Acute intestinal occlusion revealing abdominal pregnancy: a case study. Pan Afr Med J. 2018;31:155.
Marcelin C, Kouchner P, Bintner M, Linard M, Boukerrou M, Goupil J. Placenta embolization of advanced abdominal pregnancy. Diagn Interv Imaging. 2018;99:265–6.
Thang NM, Thi Huyen Anh N, Hai Thanh P. Rectal ectopic pregnancy: A case report. Medicine (Baltimore). 2021;100:e24626.
Dicker D, Nitke S, Shoenfeld A, Fish B, Meizner I, Ben-Rafael Z. Laparoscopic management of rudimentary horn pregnancy. Hum Reprod. 1998;13:2643–4.
Yahata T, Kurabayashi T, Ueda H, Kodama S, Chihara T, Tanaka K. Laparoscopic management of rudimentary horn pregnancy A case report. J Reprod Med. 1998;43:223–6.
Edelman AB, Jensen JT, Lee DM, Nichols MD. Successful medical abortion of a pregnancy within a noncommunicating rudimentary uterine horn. Am J Obstet Gynecol. 2003;189:886–7.
Chakravarti S, Chin K. Rudimentary uterine horn: management of a diagnostic enigma. Acta Obstet Gynecol Scand. 2003;82:1153–4.
Sönmezer M, Taskin S, Atabekoğlu C, Güngör M, Unlü C. Laparoscopic management of rudimentary uterine horn pregnancy: case report and literature review. Jsls. 2006;10:396–9.
Henriet E, Roman H, Zanati J, Lebreton B, Sabourin JC, Loic M. Pregnant noncommunicating rudimentary uterine horn with placenta percreta. Jsls. 2008;12:101–3.
Acknowledgements
None.
Funding
This work was supported by the Guizhou Province Science and Technology Support Project (QKH [2019] 2810) and the National Natural Science Foundation of China (GPPH-NSFC-2019–28).
Author information
Authors and Affiliations
Contributions
XZ: Conceptualization, Writing—Original Draft. YZ: Formal analysis. ZS: Data Curation. TY: Visualization. YY: Software. RW: Writing – Review & Editing, Funding acquisition. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
This study was approved by the Ethics Committee of the Guizhou Provincial People’s Hospital. All procedures were performed under the relevant guidelines and regulations. Written informed consent was obtained from the patient for her participation in this case report and accompanying images.
Consent for publication
Written informed consent was obtained from the patient for publication. There are no identifying images or other personal or clinical details of the patient that compromise her anonymity in this manuscript.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Zheng, X., Zhou, Y., Sun, Z. et al. Abdominal pregnancy secondary to uterine horn pregnancy: a case report. BMC Pregnancy Childbirth 23, 412 (2023). https://doi.org/10.1186/s12884-023-05704-4
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12884-023-05704-4