Abstract
Background
Socioeconomic status (SES) may influence prescribing, concordance and adherence to medication regimens. This review set out to investigate the association between polypharmacy and an individual’s socioeconomic status.
Methods
A systematic review and meta-analyses of observational studies was conducted across four databases. Older people (≥ 55 years) from any healthcare setting and residing location were included. The search was conducted across four databases: Medline (OVID), Web of Science, Embase (OVID) and CINAHL. Observational studies from 1990 that reported polypharmacy according to SES were included. A random-effects model was undertaken comparing those with polypharmacy (≥ 5 medication usage) with no polypharmacy. Unadjusted odds ratios (ORs), 95% confidence intervals (CIs) and standard errors (SE) were calculated for each study.
Results
Fifty-four articles from 13,412 hits screened met the inclusion criteria. The measure of SES used were education (50 studies), income (18 studies), wealth (6 studies), occupation (4 studies), employment (7 studies), social class (5 studies), SES categories (2 studies) and deprivation (1 study). Thirteen studies were excluded from the meta-analysis. Lower SES was associated with higher polypharmacy usage: individuals of lower educational backgrounds displayed 21% higher odds to be in receipt of polypharmacy when compared to those of higher education backgrounds. Similar findings were shown for occupation, income, social class, and socioeconomic categories.
Conclusions
There are socioeconomic inequalities in polypharmacy among older people, with people of lower SES significantly having higher odds of polypharmacy. Future work could examine the reasons for these inequalities and explore the interplay between polypharmacy and multimorbidity.
Similar content being viewed by others
Introduction
The burgeoning impact of polypharmacy, often defined as the use of five or more medications [1], has become an increasing challenge for healthcare professionals. With the growing usage of medication, the term hyper/excessive polypharmacy has also been used, which refers to people typically using ≥ 10 medication at any one time [2]. The increased use of multiple medications has raised some concerns, particularly across older people, as this population is more likely to develop adverse drug events, including drug-drug interactions, non-adherence and falls [3, 4].
Increasing numbers of people are experiencing polypharmacy and this challenge has become a global public health concern. In the United Kingdom (UK), for example, the number of people experiencing polypharmacy has quadrupled over a 20-year period [5], while an Australian based study [6] highlighted a 52% increase in polypharmacy between 2006–2017.
In some contexts, the increasing trend of prescribing medication and the resulting polypharmacy is appropriate and necessary; multiple medications are often required to manage long-term conditions. As such, with rising multimorbidity and increasing life expectancy, polypharmacy may be clinically appropriate and thus reflective of treatment needs [7, 8]. However, there are situations where polypharmacy may be inappropriate and problematic; it is only possible to evaluate medication appropriateness by looking at individual patient preferences, circumstances, and contexts [9].
While previous studies have shown that certain patient-based factors, such as age, are associated with increased levels of polypharmacy, the role of socioeconomic factors such as education, income and occupation, is less clear. The literature suggests that such socioeconomic factors could play an important role in polypharmacy, with studies highlighting factors such as income [10,11,12,13,14] and employment [15,16,17] as possible contributors to the prevalence of polypharmacy. For example, a Swedish study [18] investigated the relationship between polypharmacy, socioeconomic status (SES) and inappropriate medication usage. The results showed that lower levels of education were associated with increased levels of polypharmacy and potential drug-drug interactions. Further to this, some authors have highlighted the rising concerns of low SES on the adverse impact on life expectancy, access to healthcare and multimorbidity. One study [19] has showed that low SES was associated with 2.1-year reduction in life expectancy for men and women aged 40–85 years. Such an impact is important given there is potential that those of lower SES being exposed to higher levels of polypharmacy and thus the associated harms.
Whilst there is significant academic interest on this topic, there is no single review and meta-analysis which draws together the current literature around polypharmacy and how prevalence may differ according to SES. Therefore, this systematic review and meta-analysis aimed to investigate the association between socioeconomic status and the prevalence of polypharmacy, in older people.
Methods
This review was registered with accordance to The International Prospective Register of Systematic Reviews PROSPERO (CRD42021285455) and reported according to Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA).
Data sources
A literature search was conducted across the following databases: Medline (OVID), Web of Science, Embase (OVID) and CINAHL, from inception to July 2021. The search was developed around three key terms: ‘polypharmacy’ ‘socioeconomic status’ and ‘ageing’ which captured the literature surrounding the key purpose of this review. The full search strategy can be found in Supplementary 1. Additional articles were identified through hand searching reference lists and forward citations of eligible articles.
Study selection
Studies included in this review met the following criteria:
-
Population: older people. In line with previous reviews [20] older people were defined as people aged ≥ 55 years. Studies required at least 50% of participants to be over ≥ 55 years.
-
Exposure: lower socioeconomic status
-
Comparison: higher socioeconomic status
-
Outcome: receipt of polypharmacy
-
Setting: all settings were considered, irrespective of country, private or public healthcare systems.
-
Study type: all observational study types including cohort and cross sectional.
To be eligible for inclusion, articles were required to be available as full text and published in English. After discussion with the review team, prescribing practices before 1990 were considered to be less relevant to address the review question, and hence articles published before 1990 were not eligible for inclusion.
Selection criteria and screening
Records were uploaded to End Note and duplicates were removed. Rayyan QCRI was used for screening of titles and abstracts, which was conducted by one reviewer (AI). Two reviewers (CR,ZI) independently reviewed 25% of extracted articles. Full text screening was conducted by one reviewer (AI) and checked by another reviewer (CR,ZI); any discrepancies were resolved through discussion and consensus (AT). The level of agreement between the review team was determined by a Kappa score – 0.85 showing excellent agreement.
Data extraction and quality appraisal
The following information was extracted using a prepopulated data extraction form: first author, year, study data, participant characteristics, socioeconomic measure, main data extraction in relation to SES and polypharmacy. Data extraction was conducted by one reviewer (AI) and checked by the review team (CR,ZI); any discrepancies were resolved through discussion and consensus (AT). For the quality appraisal, one reviewer (AI) used the relevant critical appraisal tool from the Joanna Briggs Institute (JBI), which was checked (CR,ZI); any discrepancies were resolved through discussion and consensus (AT).
Statistical methods
Random effects meta-analysis was performed to assess the association between a given socioeconomic factor and polypharmacy. Eligibility criteria for studies to be included in the meta-analysis were as follows: i) unadjusted raw data reporting polypharmacy rates for an individual socioeconomic factor ii) total participants/information to identify total number of participants displaying polypharmacy and no polypharmacy for the socioeconomic factor being investigated. Unadjusted odds ratios, confidence intervals and standard errors were then calculated independently by two reviewers (AI, FM). I2 was calculated to determine the degree of heterogeneity amongst the studies. Odd ratios were calculated by comparing the bottom 25% of each study population to the remainder participants for each given socio-economic factor. Log odd ratios and SE were then entered into Revman 5.4 to generate forest plots.
Results
Literature search
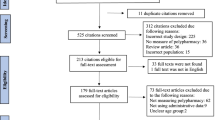
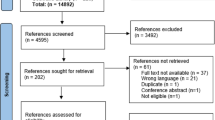
Searches retrieved 20,064 citations. After de-duplication, 13,412 articles were screened for eligibility based on title and abstract. A further 187 articles were progressed to full text screening, which resulted in 54 articles meeting the inclusion criteria (Fig. 1); 13 articles were excluded from the meta-analysis.
Study characteristics
The 54 included studies used a range of measures to assess SES factors. Fifty studies focussed on education [16, 18, 20,21,22,23,24,25,26,27,28,29,30,31,32,33,34,35,36,37,38,39,40,41,42,43,44,45,46,47,48,49,50,51,52,53,54,55,56,57,58,59,60,61,62,63,64,65,66,67], 18 studies on income [16, 23, 30, 32,33,34, 37, 41, 46,47,48, 50, 53, 61, 63, 64, 66, 68], 6 on wealth [22, 27, 45, 57, 67, 69], 4 studies on occupation [23, 44, 48, 57], 7 studies on employment [16, 17, 49, 58, 60, 63, 66], 5 studies on social class [17, 25, 36, 38, 60], 2 used SES categories [31, 70] and 1 used area-level deprivation [20]. Studies were conducted across a range of countries as follow: India [60, 66], Jordan [21], Netherlands [70], Sweden [18, 23, 39, 52], Spain [25], Belgium [26, 30], Pakistan [29, 68], UK [17, 20, 36, 38, 69], China [33, 44, 59, 65], Japan [46, 67], Singapore [40], Kuwait [42], Malaysia [43, 58], Poland [45], Togo [47], Saudi Arabia [55, 61], Taiwan [56], Vietnman [57]. Most studies were conducted within Brazil [28, 31, 32, 37, 41, 48, 50, 51, 53, 62, 63] and the US [16, 24, 27, 34, 35, 49, 54, 64]. One study included participants from across Europe and Israel [22]. Studies ranged in size from 59 [24] to 1,742,336 [52] participants. Full study characteristics can be found in Supplementary 2.
Quality appraisal
The included 54 studies scored in the range 6–8, out of a possible 8 (S2). Articles often scored poorly on identifying and reporting confounders. The majority scored well on displaying inclusion criteria, using appropriate statistical analysis, and describing subjects and setting.
Association between education and polypharmacy
Fifty studies [16, 18, 20,21,22,23,24,25,26,27,28,29,30,31,32,33,34,35,36,37,38,39,40,41,42,43,44,45,46,47,48,49,50,51,52,53,54,55,56,57,58,59,60,61,62,63,64,65,66,67] investigated the association between education and polypharmacy, 38 studies [18, 21,22,23,24,25,26,27,28,29,30,31, 33, 35, 37, 40,41,42, 44, 46,47,48, 50,51,52,53,54,55, 57,58,59,60,61, 63,64,65,66,67] were eligible for meta-analysis giving a pooled OR of 1.21 (95% CI 1.15–1.28; I2 = 94%) for receipt of polypharmacy in those of lower education when compared to higher education (Fig. 2).
Association between income and polypharmacy
Eighteen studies [16, 23, 30, 32,33,34, 37, 41, 46,47,48, 50, 53, 61, 63, 64, 66, 68] investigated the association between income and polypharmacy, 12 studies [23, 30, 33, 37, 41, 46, 47, 50, 53, 61, 64, 66] were eligible for meta-analysis giving a pooled OR of 1.10 (95% CI 0.98–1.23; I2 = 46%) for receipt of polypharmacy in those of a low compared to high income (Fig. 3).
Association between wealth and polypharmacy
Six studies [22, 27, 45, 57, 67, 69] investigated the association between wealth and polypharmacy, 4 studies [22, 57, 67, 69] were eligible for meta-analysis, giving a pooled OR of 1.38 (95% CI 1.31–1.46; I2 = 0%) for receipt of polypharmacy in those of less wealthier backgrounds (Fig. 3).
Association between occupation, employment, and polypharmacy
Four studies [23, 44, 48, 57] reported the association between occupation and polypharmacy, and 7 [16, 17, 49, 58, 60, 63, 66] reported the association between employment and polypharmacy. Three studies [23, 44, 57] assessing occupation and 5 studies [17, 58, 60, 63, 66] assessing employment were eligible for meta-analysis (Fig. 3). A pooled OR of 1.23 (95% CI 0.70 - 2.17; I2 = 92%) was calculated for those in receipt of polypharmacy from lower occupations. Similarly, the pooled OR was 1.34 (95% CI 0.85–2.13; I2 = 76%) for receipt of polypharmacy in unemployed, compared to employed, individuals.
Association between social class, SES and polypharmacy
Five studies [17, 25, 36, 38, 60] reported the association between social class and polypharmacy, and 2 studies [31, 70] focused on SES and polypharmacy. Three studies [17, 25, 60] assessing social class were eligible for meta-analysis and the pooled OR was 1.31 (95% CI 1.21–1.42; I2 = 0%) for receipt of polypharmacy in those of lower social class compared to higher social class. Two studies [31, 70] assessing SES were eligible for meta-analysis and the pooled OR was 1.03 (95% CI 0.67–1.59; I2 = 97%) for receipt of polypharmacy for those of lower, compared to higher, SES.
Discussion
Main finding
This systematic review and meta-analysis found that, overall, polypharmacy is associated with lower socioeconomic status. In particular, pooled estimates revealed a significant association when using education as a marker of SES: those of lower educational backgrounds had 21% higher odds to be in receipt of polypharmacy when compared to those of higher education. Significant associations were also observed when wealth and social class were used as SES measures. Similar trends were observed for income, occupation, employment and SES categories, although the results did not reach statistical significance. The majority of the studies included in this review used education as a marker of socioeconomic status, while fewer studies used socioeconomic measures such as occupation, income and social class.
Comparison with other reviews
To the best of our knowledge this is the first systematic review and meta-analysis that has been carried out exploring the relationship between polypharmacy and socioeconomic status; focusing on an ageing population irrespective of co-morbidities or drug class. A previous review revealed that there were significant associations between socioeconomic factors, such as education and deprivation, and multimorbidity whereby people of lower socioeconomic status have a higher risk of multimorbidity [71]. This work, unlike our review, did not focus on polypharmacy or older people, but can be used as a possible justification of our findings. Given, older people with multimorbidity are more likely to use more medications, and people of lower SES have higher risk of developing multimorbidity, may help explain – at least in part – some of our findings. However, the interplay between multimorbidity and polypharmacy is likely to be complex and should be the subject of further investigation. For example, those of higher SES may still have high levels of multimorbidity but their social status has the potential influence to ensure that they can better manage their conditions, have access to better healthcare services, reduced waiting time to see healthcare professionals, all factors of which have the potential to influence medication usage. Some of the literature has touched on the aspect of healthcare access [72] and the so called ‘wealth health’ gradient, showcasing that socioeconomic status has a direct influence on healthy ageing. Others have also revealed the potential influence that patients have on the medication that is prescribed to them [73, 74]. Those of higher SES are often better at navigating healthcare systems (both public and private) and are potentially more able to obtain multiple clinical opinions for their concerns resulting in an increased likelihood of being prescribed the medications they want or believe they need. Prosser et al. [75] showcases prescribing of medication is often patient mediated, and thus more costly, beneficial treatment may be prescribed to those that are more proactive in their health, often those of higher SES.
Other reviews that have been conducted which investigate treatment adherence and subsequent factors have all revealed that socioeconomic status plays an integral role [76,77,78,79]. Whilst these reviews are not primarily focused on polypharmacy or the ageing population, they provide important information on medication usage: treatment adherence. The reviews have shown statistical significance whereby socioeconomic factors, such as lower income, unemployment, and lower education, are associated with medication non-adherence. It can therefore be suggested that non-adherence to medication could play an important role in deteriorating health and has a subsequent effect in the rise of multimorbidity and polypharmacy. It is also worth noting that, although we calculated unadjusted odds ratios for the meta-analysis, many of the studies included in this review did adjust for multimorbidity in their analysis and still yielded statistical significant results—with a higher odds of polypharmacy in older people of lower socioeconomic status.
Individual socioeconomic factor results
To conceptualise socioeconomic status, this systematic review included studies employing different methods to assess socioeconomic status, including education, income, and employment.
With respect to education status, the overall findings of the review revealed that older people with lower educational backgrounds are of greater odds of polypharmacy. The literature suggests there are several reasons as to why this may be the case. Firstly, individuals with lower levels of education can be viewed as playing a less proactive role in preventive measures to improve/maintain their health, and thus are of greater risks of developing conditions that would likely result in them taking multiple medications [80, 81]. Secondly, some have suggested those of lower education are less likely to challenge healthcare professionals and be less involved with shared decision making [82, 83]. This, therefore, may have the potential for people to take additional medication without requiring a detailed explanation from their healthcare professional [84, 85]. Such patients are also seen to be less concerned in asking key questions regarding their medical care [86], thus it can be questioned whether they are truly aware of the potential additional harm that may be associated with taking multiple medications. However, other researchers have argued that people with lower levels of education may be less likely to approach healthcare professionals for medication and thus inevitably display lower levels of medication usage [87].
Previous work has shown that people entitled to free medications were more likely to display higher levels of polypharmacy [88]. In most instances, unemployed individuals, or individuals with lower income would be entitled to free prescription coverage and as there is no direct cost to the patient, they would be more likely to show higher medication usage. These findings can be used to support our results when assessing employment or income as a marker of socioeconomic status—that is unemployment or low income is associated with more polypharmacy. Out of pocket cost of medication, has a clear influence on the likelihood of individuals not wanting to take more medication. However, this can also be influenced by education attainment, and often people with higher income are more likely to have higher education attainment. As previously discussed, people with higher education attainment maybe more proactive in making decisions about their health and also be aware of the risks associated with polypharmacy.
Strengths and limitations
This systematic review and meta-analysis showcased comprehensive findings in relation to the association of socioeconomic status on polypharmacy in older people. Whilst our approach was comprehensive and the methodology robust, we do acknowledge that our work has limitations. Firstly, the definition we used to conceptualise older people (≥ 55 years) was arbitrary – the appropriateness of which can be debated. It is important to acknowledge that our approach was in keeping with previous reviews in the field of older people and polypharmacy. For example, the work of Davies et al. was used to help establish our definition of older people; our initial scoping searches also supported using the ≥ 55 years definition, as this conservative approach enabled the inclusion of key literature, and ensured that articles were not excluded for being too broad in their inclusion criteria. Another advantage to this review was that included studies were from a variety of low, middle, and high-income countries. Whilst this is advantageous, it is important to acknowledge that studies undertaken in a variety of healthcare systems have been included, this also contributes to the large heterogeneity observed. In some cases, it was challenging to ascertain how studies assessed different socioeconomic factors; for example, the definition of ‘high’ education varied across studies. To account for these variations and differences, when conducting the meta-analysis, the decision was made to compare the lowest 25% of each population (in terms of SES factor) to the remainder of the population. This approach also ensured that all participants within the included studies were included and factored into the meta-analysis.
Future work
Whilst this review highlights that there are socioeconomic inequalities in polypharmacy – whereby people of lower SES are more likely to receive polypharmacy, the work does not explore the potential causes of this. It would be useful to understand how people of lower socioeconomic status engage with medication reviews, with such reviews having the potential to aid deprescribing decisions and possibly reduce polypharmacy. Previous work has shown that certain populations (e.g. ethnic minority communities), struggle to engage in medication review services [89, 90]. Whilst this review has demonstrated that there is socioeconomic inequalities in polypharmacy, it is important that policies be put in place to enable healthcare professionals to work towards reducing such inequalities and not exacerbate them further. At present, certain patient demographic (e.g. age) or medication-related factors (e.g. using a high risk medication) may trigger a medication review. Our work suggests that other factors, such as SES, could be used to trigger for medication related review services. Indeed, health inequalities have been at the forefront of healthcare policy formulation for many years, particularly in the UK, especially since the wide-spread appreciation of the existence of a ‘postcode lottery’ [91]. This concept suggests that healthcare standards and subsequently polypharmacy and medication utilisation can be influenced by an individual’s geographic location. For example, people living in the North of England are more likely to use an opioid analgesic, compared to people living the South of England [92]. If factors such as education/poor healthcare literacy play a critical role in polypharmacy it is important for healthcare professionals to understand the needs of their patients and factor these into consultations.
Conclusion and implications
There are significant socioeconomic inequalities in polypharmacy among older people, whereby people with lower SES have higher odds of being in receipt of polypharmacy. This association was found using a range of markers of SES including education, and social class. Future work could examine the reasons for these inequalities and explore the interplay between polypharmacy and multimorbidity.
Availability of data and materials
All data generated or analysed during this study are included in this published article [and its supplementary information files].
References
Gnjidic D, Hilmer SN, Blyth FM, Naganathan V, Waite L, Seibel MJ, et al. Polypharmacy cutoff and outcomes: Five or more medicines were used to identify community-dwelling older men at risk of different adverse outcomes. J Clin Epidemiol. 2012;65:989–95. https://doi.org/10.1016/j.jclinepi.2012.02.018.
Masnoon N, Shakib S, Kalisch-Ellett L, Caughey GE. What is polypharmacy? A systematic review of definitions. BMC Geriatr. 2017;17(1):230. https://doi.org/10.1186/S12877-017-0621-2.
Maher RL Jr, Hanlon JT, Hajjar ER. Clinical Consequences of Polypharmacy in Elderly. Expert Opin Drug Saf. 2014;13(1):57–65. https://doi.org/10.1517/14740338.2013.827660.
Guthrie B, Makubate B, Hernandez-Santiago V, Dreischulte T. The rising tide of polypharmacy and drug-drug interactions: population database analysis 1995–2010. BMC Med. 2015;13:74. https://doi.org/10.1186/s12916-015-0322-7.
Gao L, Maidment I, Matthews FE, Robinson L, Brayne C. Medication usage change in older people (65+) in England over 20 years: Findings from CFAS I and CFAS II. Age Ageing. 2018;47:220–5. https://doi.org/10.1093/ageing/afx158.
Page AT, Falster MO, Litchfield M, Pearson SA, Etherton-Beer C. Polypharmacy among older Australians, 2006–2017: a population-based study. Med J Aust. 2019;211:71–5. https://doi.org/10.5694/mja2.50244.
Khezrian M, McNeil CJ, Murray AD, Myint PK. An overview of prevalence, determinants and health outcomes of polypharmacy. Ther Adv Drug Saf. 2020;11:2042098620933741. https://doi.org/10.1177/2042098620933741.
Whitty CJM, MacEwen C, Goddard A, Alderson D, Marshall M, Calderwood C, et al. Rising to the challenge of multimorbidity. The BMJ 2020;368 https://doi.org/10.1136/bmj.l6964.
Todd A, Jansen J, Colvin J, McLachlan AJ. The deprescribing rainbow: a conceptual framework highlighting the importance of patient context when stopping medication in older people. BMC Geriatr. 2018;18:295. https://doi.org/10.1186/s12877-018-0978-x.
Abu Farha RK, Mukattash TL, Al-Sakran L, Abu Hammour K, Zawiah M. Prevalence and predictors of polypharmacy in Jordanian hospitalised patients: A cross-sectional Study. Int J Clin Pract. 2021;75:e13742. https://doi.org/10.1111/ijcp.13742.
Assari B. Race/Ethnicity, Socioeconomic Status, and Polypharmacy among Older Americans. Pharmacy. 2019;7:41. https://doi.org/10.3390/pharmacy7020041.
Silva IR, Goncalves LG, Chor D, Fonseca MD, Mengue SS, Acurcio FDA, et al. Polypharmacy, socioeconomic indicators and number of diseases: results from ELSA-Brasil. Rev Bras Epidemiol. 2020;23:e200077. https://doi.org/10.1590/1980-549720200077.
Chiang-Hanisko L, Williams CL, Newman D, Tappen RM. Medication Use Among Ethnically Diverse Older Adults in the United States. Res Gerontol Nurs. 2015;8:273–85. https://doi.org/10.3928/19404921-20150429-01.
Hyttinen V, Jyrkka J, Saastamoinen LK, Vartiainen A-K, Valtonen H. Patient- and health care-related factors associated with initiation of potentially inappropriate medication in community-dwelling older persons. Basic Clin Pharmacol Toxicol. 2019;124:74–83. https://doi.org/10.1111/bcpt.13096.
Mayer S, Osterle A. Socioeconomic determinants of prescribed and non-prescribed medicine consumption in Austria. Eur J Public Health. 2015;25:597–603. https://doi.org/10.1093/eurpub/cku179.
Assari S, Saqib M, Wisseh C, Bazargan M. Social Determinants of Polypharmacy in First Generation Mexican Immigrants in the United States. Int J Travel Med Glob Health. 2019;7:86–90. https://doi.org/10.15171/ijtmgh.2019.19.
Thomas HF, Sweetnam PM, Janchawee B, Luscombe DK. Polypharmacy among older men in South Wales. Eur J Clin Pharmacol. 1999;55(5):411–5. https://doi.org/10.1007/s002280050649.
Haider SI, Johnell K, Weitoft GR, Thorslund M, Fastbom J. The influence of educational level on polypharmacy and inappropriate drug use: A register-based study of more than 600,000 older people. J Am Geriatr Soc. 2009;57:62–9. https://doi.org/10.1111/j.1532-5415.2008.02040.x.
Stringhini S, Carmeli C, Jokela M, Avendaño M, Muennig P, Guida F, et al. Socioeconomic status and the 25 × 25 risk factors as determinants of premature mortality: a multicohort study and meta-analysis of 1·7 million men and women. The Lancet. 2017;389:1229–37. https://doi.org/10.1016/S0140-6736(16)32380-7.
Davies LE, Kingston A, Todd A, Hanratty B. Characterising polypharmacy in the very old: Findings from the Newcastle 85+ Study. PLoS One. 2021;16:e0245648. https://doi.org/10.1371/journal.pone.0245648.
Al-Qerem W, Jarrar YB, Al-Sheikh I, Elmaadani A. The prevalence of drug-drug interactions and polypharmacy among elderly patients in Jordan. Biomedical Research (India). 2018;29:2561–9. https://doi.org/10.4066/biomedicalresearch.29-18-618.
Midão L, Giardini A, Menditto E, Kardas P, Costa E. Polypharmacy prevalence among older adults based on the survey of health, ageing and retirement in Europe. Arch Gerontol Geriatr. 2018;78:213–20. https://doi.org/10.1016/j.archger.2018.06.018.
Haider SI, Johnell K, Thorslund M, Fastbom J. Analysis of the association between polypharmacy and socioeconomic position among elderly aged > or =77 years in Sweden. Clin Ther. 2008;30(2):419–27. https://doi.org/10.1016/j.clinthera.2008.02.010.
Golchin N, Isham L, Meropol S, Vince A, Frank S. Polypharmacy in the elderly. J Res Pharm Pract. 2015;4:85. https://doi.org/10.4103/2279-042X.155755.
Carmona-Torres JM, Cobo-Cuenca AI, Recio-Andrade B, Laredo-Aguilera JA, Martins MM, Rodríguez-Borrego MA. Prevalence and factors associated with polypharmacy in the older people: 2006–2014. J Clin Nurs. 2018;27:2942–52. https://doi.org/10.1111/jocn.14371.
Wauters M, Elseviers M, Vaes B, Degryse J, Dalleur O, vanderStichele R, et al. Polypharmacy in a Belgian cohort of community-dwelling oldest old (80+). Acta Clin Belg. 2016;71:158–66. https://doi.org/10.1080/17843286.2016.1148298.
Charlesworth CJ, Smit E, Lee DSH, Alramadhan F, Odden MC. Polypharmacy among adults aged 65 years and older in the United States: 1988 - 2010. J Gerontol - Series A Biol Sci Med Sci. 2015;70:989–95. https://doi.org/10.1093/gerona/glv013.
Rozenfeld S, Fonseca MJ, Acurcio FA. Drug utilization and polypharmacy among the elderly: a survey in Rio de Janeiro City, Brazil. Revista panamericana de salud publica = Pan American Journal of Public Health. 2008;23(1):34–43. https://doi.org/10.1590/s1020-49892008000100005.
Sarwar MR, Iftikhar S, Sarfraz M. Influence of education level of older patients on polypharmacy, potentially inappropriate medications listed in Beer’s criteria, and unplanned hospitalization: A cross-sectional study in Lahore Pakistan. Medicina (Lithuania). 2018;54:57. https://doi.org/10.3390/medicina54040057.
Walckiers D, van der Heyden J, Tafforeau J. Factors associated with excessive polypharmacy in older people. Archives of Public Health. 2015;73:1–2. https://doi.org/10.1186/s13690-015-0095-7.
Ramos LR, Tavares NUL, Bertoldi AD, Farias MR, Oliveira MA, Luiza VL, et al. Polypharmacy and polymorbidity in older adults in Brazil: A public health challenge. Rev Saude Publica 2016;50 https://doi.org/10.1590/S1518-8787.2016050006145.
Carvalho MF, Romano-Lieber NS, Bergsten-Mendes G, Secoli SR, Ribeiro E, Lebrão ML, Duarte YA. Polypharmacy among the elderly in the city of São Paulo, Brazil-SABE Study Polifarmácia entre idosos do Município de São Paulo - Estudo sabe. Revista Brasileira De Epidemiologia. 2012;15(4):817–27. https://doi.org/10.1590/s1415-790x2012000400013.
Lu J, Yang M, Luo L, Hao Q, Dong B. Polypharmacy among nonagenarians/centenarians in rural China. Intern Med J. 2014;44:1193–9. https://doi.org/10.1111/imj.12534.
Perry BA, Turner LW. A prediction model for polypharmacy: Are older, educated women more susceptible to an adverse drug event? J Women Aging. 2001;13:39–51. https://doi.org/10.1300/J074v13n04_04.
Prithviraj GK, Koroukian S, Margevicius S, Berger NA, Bagai R, Owusu C. Patient characteristics associated with polypharmacy and inappropriate prescribing of medications among older adults with cancer. J Geriatr Oncol. 2012;3:228–37. https://doi.org/10.1016/j.jgo.2012.02.005.
Rawle MJ, Richards M, Davis D, Kuh D. The prevalence and determinants of polypharmacy at age 69: A British birth cohort study. BMC Geriatr. 2018;18:1–2. https://doi.org/10.1186/s12877-018-0795-2.
Loyola Filho AI, de Uchoa E, Firmo JOA, Lima-Costa MF. Influence of income on the association between cognitive impairment and polypharmacy: Bambuí Project. Revista De Saúde Pública. 2008;42(1):89-99. https://doi.org/10.1590/S0034-89102008000100012.
Chen YF, Dewey ME, Avery AJ. Self-reported medication use for older people in England and Wales. J Clin Pharm Ther. 2001;26:129–40. https://doi.org/10.1046/j.1365-2710.2001.00333.x.
Doheny M, Schön P, Orsini N, Fastbom J, Burström B, Agerholm J. Socio-demographic differences in polypharmacy and potentially inappropriate drug use among older people with different care needs and in care settings in Stockholm, Sweden. Scand J Public Health 2021:140349482110183 https://doi.org/10.1177/14034948211018384.
Tan YW, Suppiah S, Bautista MAC, Malhotra R. Polypharmacy among community-dwelling elderly in Singapore: Prevalence, risk factors and association with medication non-adherence. PoSH. 2019;28:224–31. https://doi.org/10.1177/2010105819868485.
Neves SJF, de Oliveira Marques AP, Leal MCC, da Silva DA, Medeiros TS, de Arruda IKG. Epidemiology of medication use among the elderly in an urban area of northeastern Brazil. Rev Saude Publica. 2013;47:759–68. https://doi.org/10.1590/S0034-8910.2013047003768.
Badawy NA, Labeeb SA, Alsamdan MF, Alazemi BF. Prevalence and Risk of Polypharmacy among Community-Dwelling, Elderly Kuwaiti Patients. Med Princ Pract. 2020;29:166–73. https://doi.org/10.1159/000503298.
Ong SM, Lim YMF, Sivasampu S, Khoo EM. Variation of polypharmacy in older primary care attenders occurs at prescriber level. BMC Geriatr. 2018;18:1–2. https://doi.org/10.1186/s12877-018-0750-2.
Li J, Chattopadhyay K, Xu M, Chen Y, Hu F, Wang X, et al. Prevalence and predictors of polypharmacy prescription among type 2 diabetes patients at a tertiary care department in Ningbo, China: A retrospective database study. PLoS One. 2019;14(7):e0220047. https://doi.org/10.1371/journal.pone.0220047.
Neumann-Podczaska A, Tobis S, Antimisiaris D, Mossakowska M, Puzianowska-Kuznicka M, Chudek J, et al. Polypharmacy in Polish Older Adult Population—A Cross-Sectional Study: Results of the PolSenior Project. Int J Environ Res Public Health. 2022;19:1030. https://doi.org/10.3390/ijerph19031030.
Aoki T, Ikenoue T, Yamamoto Y, Kise M, Fujinuma Y, Fukuma S, et al. Attributes of primary care in relation to polypharmacy: A multicenter cross-sectional study in Japan. Int J Qual Health Care. 2017;29:378–83. https://doi.org/10.1093/intqhc/mzx035.
Gbeasor-Komlanvi FA, Zida-Compaore WIC, Dare IH, Diallo A, Darre TP, Potchoo Y, et al. Medication Consumption Patterns and Polypharmacy among Community-Dwelling Elderly in Lomé (Togo) in 2017. Curr Gerontol Geriatr Res 2020;2020 https://doi.org/10.1155/2020/4346035.
Almeida NA, Reiners AAO, Azevedo RC, Silva AMC, Cardoso JDC, Souza LC. Prevalence of and factors associated with polypharmacy among elderly persons resident in the community. Revista Brasileira de Geriatria e Gerontologia. 2017;20:138–48. https://doi.org/10.1590/1981-22562017020.160086.
Murphy CC, Fullington HM, Alvarez CA, Betts AC, Lee SJC, Haggstrom DA, et al. Polypharmacy and patterns of prescription medication use among cancer survivors. Cancer. 2018;124:2850–7. https://doi.org/10.1002/cncr.31389.
Marques P de P, Assumpção D de, Rezende R, Neri AL, Francisco PMSB. Polypharmacy in community-based older adults: results of the Fibra study. Revista Brasileira de Geriatria e Gerontologia 2019;22 https://doi.org/10.1590/1981-22562019022.190118.
da Silva MRR, Diniz LM, dos Santos JBR, Reis EA, da Mata AR, de Araújo VE, et al. Drug utilization and factors associated with polypharmacy in individuals with diabetes mellitus in Minas Gerais. Brazil Ciencia e Saude Coletiva. 2018;23:2565–74. https://doi.org/10.1590/1413-81232018238.10222016.
Morin L, Johnell K, Laroche ML, Fastbom J, Wastesson JW. The epidemiology of polypharmacy in older adults: Register-based prospective cohort study. Clin Epidemiol. 2018;10:289–98. https://doi.org/10.2147/CLEP.S153458.
Pereira KG, Peres MA, Iop D, Boing AC, Boing AF, Aziz M, et al. Polifarmácia em idosos: Um estudo de base populacional. Rev Bras Epidemiol. 2017;20:335–44. https://doi.org/10.1590/1980-5497201700020013.
Bazargan M, Smith J, Movassaghi M, Martins D, Yazdanshenas H, SaleheMortazavi S, et al. Polypharmacy among underserved older african American adults. J Aging Res. 2017;2017:6026358. https://doi.org/10.1155/2017/6026358.
Salih S, Yousuf M, Durihim H, Almodaimegh H, Tamim H. Prevalence and associated factors of polypharmacy among adult Saudi medical outpatients at a tertiary care center. J Family Community Med. 2013;20:162–7. https://doi.org/10.4103/2230-8229.121987.
Chan DC, Hao YT, Wu SC. Polypharmacy among disabled Taiwanese elderly: a longitudinal observational study. Drugs & aging. 2009;26(4):345–54. https://doi.org/10.2165/00002512-200926040-00005.
Bui DHT, Nguyen BX, Truong DC, Meyrowitsch DW, Søndergaard J, Gammeltoft T, et al. Polypharmacy among people living with type 2 diabetes mellitus in rural communes in Vietnam. PLoS One. 2021;16(4):e0249849. https://doi.org/10.1371/journal.pone.0249849.
Lim LM, McStea M, Chung WW, Azmi NN, Aziz SAA, Alwi S, et al. Prevalence, risk factors and health outcomes associated with polypharmacy among urban community-dwelling older adults in multiethnic Malaysia. PLoS One. 2017;12(3):e0173466. https://doi.org/10.1371/journal.pone.0173466.
Zhang XM, Jiao J, Guo N, Bo HX, Xu T, Wu XJ. Association of polypharmacy with falls among older Chinese inpatients: A nationwide cohort study. Geriatr Gerontol Int. 2021;21:810–7. https://doi.org/10.1111/ggi.14245.
Nitya S, Ramya G, Kiruthika S, Meenakshi R, Devi J, Suganya G, et al. Drug utilization pattern and factors associated with polypharmacy and excessive polypharmacy in geriatric medical out-patients at a rural health training centre in India. J Family Med Prim Care. 2021;10:2636. https://doi.org/10.4103/jfmpc.jfmpc_2417_20.
Aljawadi MH, Khoja AT, Alaboud NM, AlEnazi ME, Al-Shammari SA, Khoja TA, et al. Prevalence of Polypharmacy and Factors Associated with it Among Saudi Older Adults – Results from the Saudi National Survey for Elderly Health (SNSEH). SPJ. 2022;30:230–6. https://doi.org/10.1016/j.jsps.2022.01.003.
Rezende GR, Amaral TLM, Amaral CA, Vasconcellos MTL, Monteiro GTR. Prevalência e fatores associados à polifarmácia em idosos residentes em Rio Branco, Acre, Brasil: estudo transversal de base populacional, 2014. Epidemiol Serv Saude. 2021;30:e2020386. https://doi.org/10.1590/S1679-49742021000200013.
Gomes MS, Amorim WW, Morais RS, Gama RS, Graia LT, Queiroga HM, et al. Polypharmacy in older patients at primary care units in Brazil. Int J Clin Pharm. 2019;41:516–24. https://doi.org/10.1007/s11096-018-00780-5.
Rasu R, Agbor-Bawa W, Rianon N. Impact of polypharmacy on seniors’ self-perceived health status. South Med J. 2017;110:540–5. https://doi.org/10.14423/SMJ.0000000000000688.
Yang M, Lu J, Hao Q, Luo L, Dong B. Does residing in urban or rural areas affect the incidence of polypharmacy among older adults in western China? Arch Gerontol Geriatr. 2015;60:328–33. https://doi.org/10.1016/j.archger.2014.11.004.
Panda M, Pathak R, Islam F, Agarwalla R, Singh V, Singh F. Interplay of multimorbidity and polypharmacy on a community dwelling frail elderly cohort in the peri-urban slums of Delhi. India J Family Med Prim Care. 2020;9:1647. https://doi.org/10.4103/jfmpc.jfmpc_945_19.
Masumoto S, Sato M, Maeno T, Ichinohe Y, Maeno T. Potentially inappropriate medications with polypharmacy increase the risk of falls in older Japanese patients: 1-year prospective cohort study. Geriatr Gerontol Int. 2018;18:1064–70. https://doi.org/10.1111/ggi.13307.
Sarwar MR, Atif M, Scahill S, Saqib A, Qamar-uz-Zaman M, Babar Z. Drug utilization patterns among elderly hospitalized patients on poly-pharmacy in Punjab. Pakistan J Pharm Policy Pract. 2017;10:23. https://doi.org/10.1186/s40545-017-0112-z.
Slater N, White S, Frisher M. Central nervous system (CNS) medications and polypharmacy in later life: cross-sectional analysis of the English Longitudinal Study of Ageing (ELSA). BMJ Open. 2020;10:e034346. https://doi.org/10.1136/bmjopen-2019-034346.
Sinnige J, Braspenning JC, Schellevis FG, Hek K, Stirbu I, Westert GP, et al. Inter-practice variation in polypharmacy prevalence amongst older patients in primary care. Pharmacoepidemiol Drug Saf. 2016;25:1033–41. https://doi.org/10.1002/pds.4016.
Pathirana TI, Jackson CA. Socioeconomic status and multimorbidity: a systematic review and meta-analysis. Aust N Z J Public Health. 2018;42:186–94. https://doi.org/10.1111/1753-6405.12762.
McMaughan DJ, Oloruntoba O, Smith ML. Socioeconomic Status and Access to Healthcare: Interrelated Drivers for Healthy Aging. Front Public Health. 2020;8:231. https://doi.org/10.3389/fpubh.2020.00231.
Mamdani MM, Tu K, Austin PC, Alter DA. Influence of Socioeconomic Status on Drug Selection for the Elderly in Canada. Ann Pharmacother. 2002;36:804–8. https://doi.org/10.1345/aph.1A044.
Odubanjo E, Bennett K, Feely J. Influence of socioeconomic status on the quality of prescribing in the elderly - a population based study. Br J Clin Pharmacol. 2004;58:496–502. https://doi.org/10.1111/j.1365-2125.2004.02179.x.
Prosser H, Almond S, Walley T. Influences on GPs' decision to prescribe new drugs-the importance of who says what. Family practice. 2003;20(1):61–8. https://doi.org/10.1093/fampra/20.1.61.
Yeam CT, Chia S, Tan HCC, Kwan YH, Fong W, Seng JJB. A systematic review of factors affecting medication adherence among patients with osteoporosis. Osteoporos Int. 2018;29:2623–37. https://doi.org/10.1007/s00198-018-4759-3.
Kvarnström K, Westerholm A, Airaksinen M, Liira H. Factors contributing to medication adherence in patients with a chronic condition: A scoping review of qualitative research. Pharmaceutics. 2021;13:1100. https://doi.org/10.3390/pharmaceutics13071100.
Mann DM, Woodward M, Muntner P, Falzon L, Kronish I. Predictors of nonadherence to statins: A systematic review and meta-analysis. Ann Pharmacother. 2010;44:1410–21. https://doi.org/10.1345/aph.1P150.
Lemstra M, Blackburn D, Crawley A, Fung R. Proportion and Risk Indicators of Nonadherence to Statin Therapy: A Meta-analysis. Can J Cardiol. 2012;28:574–80. https://doi.org/10.1016/j.cjca.2012.05.007.
Rosemann T, Laux G, Szecsenyi J, Grol R. The Chronic Care Model: congruency and predictors among primary care patients with osteoarthritis. Qual Saf Health Care. 2008;17:442–6. https://doi.org/10.1136/qshc.2007.022822.
Cramm JM, Nieboer AP. A longitudinal study to identify the influence of quality of chronic care delivery on productive interactions between patients and (teams of) healthcare professionals within disease management programmes. BMJ Open. 2014;4:e005914–e005914. https://doi.org/10.1136/bmjopen-2014-005914.
Protheroe J, Nutbeam D, Rowlands G. Health literacy: a necessity for increasing participation in health care. Br J Gen Pract. 2009;59:721–3. https://doi.org/10.3399/bjgp09X472584.
Smith SK, Dixon A, Trevena L, Nutbeam D, McCaffery KJ. Exploring patient involvement in healthcare decision making across different education and functional health literacy groups. Soc Sci Med. 2009;69:1805–12. https://doi.org/10.1016/j.socscimed.2009.09.056.
Abdulrahman KA. What Do Patient’s Expect Of Their General Practitioners? J Family Community Med. 2003;10:39–45.
Plaza-Zamora J, Legaz I, Osuna E, Pérez-Cárceles MD. Age and education as factors associated with medication literacy: a community pharmacy perspective. BMC Geriatr. 2020;20:501. https://doi.org/10.1186/s12877-020-01881-5.
Katz MG, Jacobson TA, Veledar E, Kripalani S. Patient Literacy and Question-asking Behavior During the Medical Encounter: A Mixed-methods Analysis. J Gen Intern Med. 2007;22:782–6. https://doi.org/10.1007/s11606-007-0184-6.
Stirbu I, Kunst AE, Mielck A, Mackenbach JP. Inequalities in utilisation of general practitioner and specialist services in 9 European countries. BMC Health Serv Res. 2011;11:288. https://doi.org/10.1186/1472-6963-11-288.
Varley A, Cullinan J. Are payment methods for prescription drugs associated with polypharmacy in older adults in Ireland? Evidence from the TILDA cohort study. BMJ Open. 2020;10:e036591. https://doi.org/10.1136/bmjopen-2019-036591.
Robinson A, Sile L, Govind T, Guraya HK, O’Brien N, Harris V, et al. ‘He or she maybe doesn’t know there is such a thing as a review’: A qualitative investigation exploring barriers and facilitators to accessing medication reviews from the perspective of people from ethnic minority communities. Health Expect. 2022;25(4):1432–43. https://doi.org/10.1111/hex.13482.
Robinson A, Elarbi M, Todd A, Husband A. A qualitative exploration of the barriers and facilitators affecting ethnic minority patient groups when accessing medicine review services: Perspectives of healthcare professionals. Health Expect. 2022;25:628–38. https://doi.org/10.1111/hex.13410.
Russell J, Greenhalgh T, Lewis H, Mackenzie I, Maskrey N, Montgomery J, et al. Addressing the ‘postcode lottery’ in local resource allocation decisions: a framework for clinical commissioning groups. J R Soc Med. 2013;106:120–3. https://doi.org/10.1177/0141076813479192.
Todd A, Akhter N, Cairns J-M, Kasim A, Walton N, Ellison A, et al. The Pain Divide: a cross-sectional analysis of chronic pain prevalence, pain intensity and opioid utilisation in England. BMJ Open. 2018;8:e023391. https://doi.org/10.1136/bmjopen-2018-023391.
Acknowledgements
Not applicable.
Funding
This research is funded by the National Institute for Health and Care Research (NIHR) [Applied Research Collaboration North East and North Cumbria (NIHR200173)].
Author information
Authors and Affiliations
Contributions
AI and AT were a major contributor in writing the manuscript and conducting the search. HK, BH contributed to the search strategy. ZI and CR contributed to reviewing included papers and data extraction. FM and AI both contributed to the meta-analysis. This article has been approved by all the co-authors, meets all conditions of the ICMJE and we can also confirm that there is no conflict of interest. The author(s) read and approved the final manuscript.
Authors information
Not applicable.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Iqbal, A., Richardson, C., Iqbal, Z. et al. Are there socioeconomic inequalities in polypharmacy among older people? A systematic review and meta-analysis. BMC Geriatr 23, 149 (2023). https://doi.org/10.1186/s12877-023-03835-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12877-023-03835-z