Abstract
Introduction
Implementation of the Surviving Sepsis Campaign (SSC) guidelines has been associated with improved outcome in patients with severe sepsis. Resolution of lactate elevations or lactate clearance has also been shown to be associated with outcome. The purpose of the present study was to examine the compliance and effectiveness of the SSC resuscitation bundle with the addition of lactate clearance.
Methods
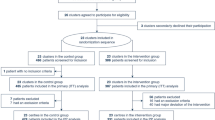
This was a prospective cohort study over 18 months in eight tertiary-care medical centers in Asia, enrolling adult patients meeting criteria for the SSC resuscitation bundle in the emergency department. Compliance and outcome results of a multi-disciplinary program to implement the Primary SSC Bundle with the addition of lactate clearance (Modified SSC Bundle) were examined. The implementation period was divided into quartiles, including baseline, education and four quality improvement phases.
Results
A total of 556 patients were enrolled, with median (25th to 75th percentile) age 63 (50 to 74) years, lactate 4.1 (2.2 to 6.3) mmol/l, central venous pressure 10 (7 to 13) mmHg, mean arterial pressure (MAP) 70 (56 to 86) mmHg, and central venous oxygen saturation 77 (69 to 82)%. Completion of the Primary SSC Bundle over the six quartiles was 13.3, 26.9, 37.5, 45.9, 48.8, and 54.5%, respectively (P <0.01). The Modified SSC Bundle was completed in 10.2, 23.1, 31.7, 40.0, 42.5, and 43.6% patients, respectively (P <0.01). The ratio of the relative risk of death reduction for the Modified SSC Bundle compared with the Primary SSC Bundle was 1.94 (95% confidence interval = 1.45 to 39.1). Logistic regression modeling showed that the bundle items of fluid bolus given, achieve MAP >65 mmHg by 6 hours, and lactate clearance were independently associated with decreased mortality - having odds ratios (95% confidence intervals) 0.47 (0.23 to 0.96), 0.20 (0.07 to 0.55), and 0.32 (0.19 to 0.55), respectively.
Conclusions
The addition of lactate clearance to the SSC resuscitation bundle is associated with improved mortality. In our study patient population with optimized baseline central venous pressure and central venous oxygen saturation, the bundle items of fluid bolus administration, achieving MAP >65 mmHg, and lactate clearance were independent predictors of outcome.
Similar content being viewed by others
Introduction
Despite many advances in our understanding and treatments, epidemiologic studies across the globe have shown an increasing incidence of severe sepsis with a continued high mortality rate [1–3]. As a result, the international Surviving Sepsis Campaign (SSC) developed guidelines to improve the standard of care for severe sepsis. Such guidelines advocate early recognition, broad-spectrum antibiotics, hemodynamic optimization guided by invasive monitoring, corticosteroid, recombinant human activated protein C, and lung protective strategies in the form of the severe sepsis resuscitation and management bundles [4]. While many studies have examined the effectiveness of the bundles only in nonrandomized manners, their successful implementation in America and Europe has been shown to be cost-effective and associated with decreased mortality [5–7].
Crucial to implementing the guidelines and the severe sepsis bundles is the utilization of lactate as an indicator of global organ hypoperfusion and shock. While the etiology of lactate elevations in severe sepsis is debatable, it is well accepted as a resuscitation endpoint, an indicator of severity, and a predictor of short-term and long-term mortality [8–10]. Additionally, persistent elevation of lactate has been shown to be associated with poor outcome, such that a decrease in lactate (or lactate clearance) during resuscitation is an independent predictor for improved mortality [11–13].
Our study was a quality improvement effort in the implementation of the SSC severe sepsis resuscitation bundle in Asia, with the additional aim to examine the effect of lactate clearance as a bundle item. Our hypothesis was that completion of the bundle with addition of lactate clearance will further decrease mortality compared with completion of the bundle without lactate clearance.
Materials and methods
Design and setting
This was a multi-national prospective quality improvement cohort study performed in eight tertiary-care medical centers in China, India, Korea, Singapore, and Taiwan. The study was conducted at all participating centers over an 18-month period starting on 1 July 2008 and ending on 31 December 2009. Participating hospitals implemented the severe sepsis resuscitation bundle as recommended by the SSC guidelines to improve the standard of care, with the additional goal of lactate clearance [4, 14]. The implementation period was divided into 3-month phases: baseline, education, and quality improvement phases 1 to 4. The Institution Review Board of the participating centers approved the study and waived the need for patient's written consent. Patient data gathered during the course of the study were entered into an Institution Review Board-approved database at the study organization center, Loma Linda University, CA, USA.
Bundle implementation and lactate clearance
Based on existing hospital staffing and resources, three hospitals adopted a sepsis team model of implementation championed by intensivists. The severe sepsis resuscitation bundle was initiated in the emergency department (ED) and completed in the ICU. Patient care was delivered by a focused multi-disciplinary team led by the attending intensivist, similar to the well-accepted trauma team model. The other five participating hospitals implemented the bundle via a nonteam model, which was championed solely by the ED, with initiation and completion of the bundle by ED physicians and nurses as part of ED standard care.
Delivery of the bundle included lactate measurement, blood cultures obtained prior to antibiotics, early antibiotic administration, hemodynamic monitoring and support, and mechanical ventilation per guidelines [4]. Hemodynamic monitoring was achieved by central venous catheter insertion for continuous monitoring of central venous pressure (CVP) and central venous oxygen saturation (ScvO2). Intra-arterial blood pressure monitoring with insertion of a radial or femoral arterial catheter was preferred, especially if patients were on a vasoactive agent. Hemodynamic support included the use of crystalloid fluids, vasoactive and inotropic agents, and packed red blood cell transfusion as appropriate to target optimal CVP, mean arterial pressure (MAP), and ScvO2 as previously defined by the early goal-directed therapy (EGDT) protocol [15]. Corticosteroid, glucose control, and lung-protective strategies were provided at the discretion of the treating physicians, and were not considered part of the resuscitation bundle. Recombinant human activated protein C was not available at the participating hospitals.
During the study period, bundle completion was monitored for compliance in each of the implementation phases. A physician champion at each of the participating hospitals completed weekly audits of the bundle implementation. A bundle compliance checklist was completed for each consecutive patient meeting enrollment criteria for the study (see below). Other information recorded for each patient included demographics, laboratories, Acute Physiology and Chronic Health Evaluation (APACHE) II score, vital signs, hemodynamic measurements, source of infection, therapeutic interventions up to 72 hours including ED and ICU lengths of stay, and in-hospital mortality.
Completion of the Primary SSC Bundle included all of the following items: lactate measured; blood cultures before antibiotics; antibiotics administered by 3 hours; fluid bolus given; achieve CVP >8 mmHg by 6 hours; achieve MAP >65 mmHg by 6 hours; and achieve ScvO2 >70% by 6 hours (Table 1). Completion of the Modified SSC Bundle was defined as completion of the Primary SSC Bundle and lactate clearance. Lactate clearance was defined as any decrease in lactate within 12 hours from baseline, or an initial lactate <2.0 mmol/l [12, 16].
Patient selection
Adult patients over 18 years of age and meeting criteria for initiating the severe sepsis resuscitation bundle in the ED were considered for enrollment during the weekly audit of bundle implementation. The inclusion criteria were: two of four systemic inflammatory response syndrome criteria; suspected or confirmed infection; and systolic blood pressure <90 mmHg after a 1 liter crystalloid fluid bolus, lactate ≥4 mmol/l, or two or more organ dysfunctions. The systemic inflammatory response syndrome criteria included: temperature >38.3°C or <36°C; heart rate >90 beats per minute; respiratory rate >20 breaths per minute or arterial partial pressure of carbon dioxide <32 mmHg; or a white blood cell count >12, 000 per mm3 or <4, 000 per mm3, or bands greater than 10%. Organ dysfunction was defined as: creatinine >2.0 mg/dl or an increase >0.5 mg/dl; PaO2/FiO2 <300; platelet count <100, 000/μl; International Normalized Ratio >1.5; partial thromboplastin time >60 seconds; or total bilirubin >2.0 mg/dl.
Patients with trauma, active seizures, acute pulmonary edema due to heart failure, a need for emergent surgery, active bleeding, acute stroke, or a do-not-resuscitate order were excluded from the study.
Outcome measures
The primary measures were compliance and in-hospital mortality associated with completion of the Primary SSC Bundle and the Modified SSC Bundle. Secondary measures included bundle items independently associated with in-hospital mortality.
Statistical analysis
Univariate analyses were conducted on patient demographics, laboratories, hemodynamics, and therapies provided to the patient to assess normality and to test the assumptions of the parametric and nonparametric statistical tests conducted. Taken into consideration were the following: age, gender, APACHE II score, care team model, bundle completion, mechanical ventilation, therapies in either the ED or ICU, length of stay in the ED, ICU, and hospital, hemodynamic characteristics, laboratory measurements, and infection source. The best measure of central tendency and the corresponding measure of variation for each of these factors stratified by lactate clearance status were determined, reported, and tested for differences using Pearson's chi-square test, Wilcoxon's sum-rank test, or Student's two-sample t test as appropriate.
Trends in quarterly compliance to the bundle implementation for the Primary and Modified SSC Bundles were assessed using analysis of variance for completion of the individual bundle items over each of the six quartiles. Comparisons of compliance to the Primary and Modified SSC Bundles were made using Pearson's chi-square test.
Multivariable logistic regression analysis was performed for each of eight different models that sequentially included another bundle item into a base model. The base model included only the measurement of serum lactate (lactate measured), adjusted for the effects of age, gender, APACHE II score, and mechanical ventilation status. The -2 log-likelihood for the model including all covariates was reported and used to compare models with each sequentially included covariate. The corresponding chi-square P value for the difference in -2 log-likelihood identified models that significantly improved with the inclusion of the new covariate. A Bonferroni correction was performed to account for multiple comparisons.
Statistical significance was defined at P <0.05. All analyses were performed using SAS version 9.2 (SAS Institute Inc., Cary, NC, USA).
Results
Five-hundred and fifty-six patients were enrolled in the study, with median (25th to 75th percentile) age 63 (50 to 74) years, APACHE II score 22 (16 to 27), and lactate 4.1 (2.2 to 6.3) mmol/l (Table 2). Patients had a median (25th to 75th percentile) length of stay of 5 (3 to 9) hours in the ED and 4 (2 to 8) days in the ICU, and a total hospital stay of 9 (4 to 16) days. A total of 67.1% of patients were in septic shock on presentation, and 53.1% required mechanical ventilation within 72 hours. Baseline (25th to 75th percentile) CVP, MAP, and ScvO2 values were 10 (7 to 13) mmHg, 70 (56 to 86) mmHg, and 77 (69 to 82)%, respectively. Pneumonia (41.9%) was the most common source of infection. In-hospital mortality was 29.9%.
Patients having lactate clearance had all Primary SSC Bundle items completed significantly more than those patients without lactate clearance (Table 2). Patients with lactate clearance had lower APACHE II score (P <0.01) and baseline lactate (P <0.01). The lactate clearance group had lower CVP and MAP but higher ScvO2 at baseline compared with the patients without lactate clearance (P <0.05). Patients with lactate clearance were more in the team care model than the nonteam model (P < 0.01) and received more fluid resuscitation both in the ED and ICU (P <0.01), with a shorter length of stay in the ED (P <0.01). Patients with lactate clearance had mortality of 20.5% compared with 43.6% in those patients with no lactate clearance (P <0.01).
Completion of the Primary SSC Bundle over the six quartiles of implementation was 13.3, 26.9, 37.5, 45.9, 48.8, and 54.5%, respectively (P <0.01). The Modified SSC Bundle (including lactate clearance) was completed in 10.2, 23.1, 31.7, 40.0, 42.5, and 43.6% patients, respectively (P <0.01) (Table 3 and Figure 1). Patients with the Primary SSC Bundle completed compared with not completed had mortality of 24.5% (95% confidence interval = 18.6 to 31.2) versus 32.7% (95% confidence interval = 27.9 to 37.8) (P = 0.04). Patients with the Modified SSC Bundle completed compared with not completed had mortality of 17.9% (95% confidence interval = 12.3 to 24.7) versus 34.8% (95% confidence interval = 30.1 to 39.7) (P <0.01) (Figure 2). Completion of the Primary SSC Bundle resulted in a relative risk of death reduction (RRR) of 0.251 (95% confidence interval = 0.007 to 0.442), and completion of the Modified SSC Bundle had a relative risk of death reduction of 0.486 (95% confidence interval = 0.274 to 0.642). The ratio of the relative risk of death reduction for the Modified SSC Bundle compared with the Primary SSC Bundle was 1.94 (95% confidence interval = 1.45 to 39.1).
Mortality differences for the Surviving Sepsis Campaign bundles. Mortality differences for the Primary Surviving Sepsis Campaign (SSC) Bundle and the Modified SSC Bundle (includes lactate clearance). Patients with the Primary SSC Bundle completed compared with not completed had mortality of 24.5% (95% confidence interval = 18.6 to 31.2) versus 32.7% (95% confidence interval = 27.9 to 37.8). Patients with the Modified SSC Bundle completed compared with not completed had mortality of 17.9% (95% confidence interval = 12.3 to 24.7) versus 34.8% (95% confidence interval = 30.1 to 39.7). The ratio of the relative risk of death reduction for the Modified SSC Bundle compared with the Primary SSC Bundle was 1.94 (95% confidence interval = 1.45 to 39.1).
Logistic regression models with sequential inclusion of each bundle item as the independent variable showed that the bundle items of fluid bolus given, achieve MAP >65 mmHg by 6 hours, and lactate clearance were independently associated with decreased mortality - having odds ratios (95% confidence interval) of 0.47 (0.23 to 0.96), 0.20 (0.07 to 0.55), and 0.32 (0.19 to 0.55), respectively, in the final model (Table 4).
Discussion
The rationale for implementing the severe sepsis care bundles has been that the compliance to the bundle would translate into better patient outcomes. Several studies showed that improvements in survival were related to the number of bundle interventions completed [16–18]. Recently, another study showed that mortality was significantly lower even if completion of the 6-hour resuscitation bundle was achieved later at 18 hours compared with not completing the bundle at all [19]. Despite a number of observational studies indicating protocol-driven EGDT and the severe sepsis bundle to be associated with reduced mortality, EGDT is underused even with formal bundle implementation in place [20]. Many potential barriers ranging from patient to clinician to organizational factors have been identified as stifling the more widespread compliance to the bundle. In the present study, we showed that implementation of the SSC resuscitation bundle in Asia was achievable with a compliance >50% after 1 year of quality improvement. Overall compliance was expectedly less throughout the study period with the addition of lactate clearance as a bundle item.
Our patients with optimal baseline CVP and ScvO2 contrast those of the original study examining EGDT. Optimizing preload remains a cornerstone for resuscitation of patients in shock; however, the use of CVP as a measure of fluid responsiveness has been challenged [21]. Evidence demonstrated a poor relationship between CVP and blood volume as well as its ability to predict a hemodynamic response to a fluid bolus. Irrespective of the debate and contrast to the low initial CVP observed in the original EGDT study, our patients did not require much fluid administration according to the target CVP recommended during the 6 hours of the resuscitation bundle. With respect to targeting ScvO2, the original EGDT study examined a patient population with initial ScvO2 <50% [15]. This finding has not been consistently observed in other studies, including ours. Another study showed that the number of severe sepsis patients with ScvO2 <50% was only 1%, with the rest of the patients having normal mean mixed venous oxygen saturation (SvO2) or ScvO2 values [22]. In fact, some studies have shown supranormal levels of ScvO2, which is probably due to the lack of effective tissue oxygen extraction that is seen in patients with sepsis [23].
Given the barriers and controversies in implementing EGDT, an approach utilizing noninvasive hemodynamic monitoring technology has been suggested [24, 25]. Alternative to searching for the ideal technology, lactate monitoring for resolution of tissue hypoperfusion in septic shock seems practical and makes physiologic sense. A decreased in lactate (or lactate clearance) of ≥10% has been shown to be associated with improved 60-day survival [12, 13]. Recently, lactate clearance >10% instead of ScvO2 >70% as an endpoint in the EGDT protocol was shown to result in similar amount of fluids, vasopressors, inotropes, blood transfusions, and in-hospital mortality [26]. Furthermore, a more aggressive approach at lactate clearance of 20% or higher every 2 hours, in addition to optimizing CVP, MAP, and ScvO2 during the first 8 hours, in mixed ICU patients resulted in decreased mortality [27]. One of our study investigators (HBN) previously included lactate clearance with EGDT in a 6-hour ED severe sepsis bundle and showed that lactate clearance was associated with decreased mortality [16]. In the present study we also found that the addition of lactate clearance to the SSC bundle was associated with greater improvement in outcome.
The suggestion that lactate clearance can be a replacement for the more dynamic endpoint of ScvO2 should be viewed with caution. ScvO2 as a surrogate to mixed venous oxygen saturation reflects the balance between oxygen delivery and oxygen consumption. Lactate elevation has been shown to be a surrogate for oxygen debt, or oxygen deficit accumulated over time [28, 29]. Lactate clearance indicates the success of resuscitation in improving tissue perfusion and repayment of the oxygen debt. But the decrease in lactate also depends on the rate of production and metabolism in the muscle, kidney, and liver. Furthermore, normal lactate with persistent microcirculatory blood flow alterations can still suggest an unpaid oxygen debt [30].
The tenet of EGDT is to optimize oxygen delivery, resolving the oxygen transport imbalance, in the hope of improving tissue perfusion. Patients in the original EGDT study had significant hypovolemia, oxygen deficit, and hypoperfusion, with baseline ScvO2 <50% and lactate >7 mmol/l, indicating an oxygen-delivery-dependent state [15]. A low ScvO2 and high lactate have been shown to be independently associated with morbidity and mortality [31]. Achieving the ScvO2 >70% target at 6 hours was the only bundle element associated with reduction of in-hospital mortality [18]. The recent studies advocating lactate clearance as a therapeutic endpoint enrolled patients already having a normal ScvO2 at baseline [26, 27]. In those patients, therefore, fluid resuscitation alone may be adequate to resolve tissue hypoperfusion, achieving lactate clearance, whereas patients with low initial ScvO2 will require blood transfusion and inotrope therapy to increase oxygen delivery [32].
In our study, we enrolled patients using the same inclusion criteria as the original EGDT study, but the targeted hemodynamic endpoints of CVP and ScvO2 were already optimal prior to therapy. We found that the fluid bolus, achieving MAP >65 mmHg, and lactate clearance were independent predictors of outcome. In our relative hemodynamically stable patients and in those patients in previous studies having optimal CVP and ScvO2, therefore, targeting MAP and lactate clearance may be adequate [22, 33]. Our results would suggest that in these patients the requirement for specialized technology to monitor ScvO2 during the early treatment of septic shock might be avoided.
Our study had several limitations as it was a quality improvement effort aimed at improving the care delivery for severe sepsis patients, rather than a randomized examination of the effectiveness of the bundle and lactate clearance. The sample size was small for a multi-national study; however, we succeeded in showing that the resuscitation bundle can be implemented with a moderate level of compliance in developed and developing countries in Asia. We did not study the 24-hour management bundle including recombinant human activated protein C, since recombinant human activated protein C was not available in the study sites. Lactate clearance as a bundle item in our study was more of an observation of a resuscitation endpoint rather than part of a guided treatment protocol. We considered patients with initial lactate <2 mmol/l as achieving the lactate clearance criteria. Our results were similar when we excluded these patients from the analysis, however, and none of the patients with the initial normal lactate had increased values after successful initiation of the bundle (data not shown). Finally, our approach of adding lactate clearance to the bundle supports previous usage of monitoring lactate in addition to hemodynamic parameters of CVP, MAP, and ScvO2[16, 27].
Conclusions
Our study demonstrated that adding lactate clearance as a component of the SSC resuscitation bundle resulted in a more significant mortality improvement, with an almost twofold increase in the relative risk of death reduction. Our data are consistent with previous studies and suggest that lactate clearance is a viable quality improvement goal for hospitals implementing the SSC guidelines to optimize outcome in patients with severe sepsis and septic shock.
Key messages
-
Implementation of the SSC resuscitation bundle at multiple hospitals in Asia significantly increased compliance over 18 months and was associated with improved outcome.
-
Lactate clearance or the decrease in lactate after initiation of the SSC resuscitation bundle is associated with further improvement in outcome.
-
In severe sepsis patients with hemodynamic stability, reflected by optimized baseline CVP and ScvO2, the bundle items of fluid bolus administration, achieving MAP >65 mmHg, and lactate clearance were independent predictors of outcome.
-
Our study results do not imply that fluid resuscitation alone and the goals of MAP >65 mmHg and lactate clearance are adequate in those patients with evidence of significant organ hypoperfusion; that is, low ScvO2 and high lactate levels.
Abbreviations
- APACHE:
-
Acute Physiology and Chronic Health Evaluation
- CVP:
-
central venous pressure
- ED:
-
emergency department
- EGDT:
-
early goal-directed therapy
- MAP:
-
mean arterial pressure
- PaO2/FiO2:
-
partial pressure of oxygen/fraction of inspired oxygen
- ScvO2:
-
central venous oxygen saturation
- SSC:
-
Surviving Sepsis Campaign.
References
Dombrovskiy VY, Martin AA, Sunderram J, Paz HL: Rapid increase in hospitalization and mortality rates for severe sepsis in the United States: a trend analysis from 1993 to 2003. Crit Care Med 2007, 35: 1244-1250. 10.1097/01.CCM.0000261890.41311.E9
Harrison DA, Welch CA, Eddleston JM: The epidemiology of severe sepsis in England, Wales and Northern Ireland, 1996 to 2004: secondary analysis of a high quality clinical database, the ICNARC Case Mix Programme Database. Crit Care 2006, 10: R42. 10.1186/cc4854
Shen HN, Lu CL, Yang HH: Epidemiologic trend of severe sepsis in Taiwan from 1997 through 2006. Chest 2010, 138: 298-304. 10.1378/chest.09-2205
Dellinger RP, Levy MM, Carlet JM, Bion J, Parker MM, Jaeschke R, Reinhart K, Angus DC, Brun-Buisson C, Beale R, Calandra T, Dhainaut JF, Gerlach H, Harvey M, Marini JJ, Marshall J, Ranieri M, Ramsay G, Sevransky J, Thompson BT, Townsend S, Vender JS, Zimmerman JL, Vincent JL: Surviving Sepsis Campaign: international guidelines for management of severe sepsis and septic shock: 2008. Crit Care Med 2008, 36: 296-327. 10.1097/01.CCM.0000298158.12101.41
Ferrer R, Artigas A, Levy MM, Blanco J, Gonzalez-Diaz G, Garnacho-Montero J, Ibanez J, Palencia E, Quintana M, de la Torre-Prados MV: Improvement in process of care and outcome after a multicenter severe sepsis educational program in Spain. JAMA 2008, 299: 2294-2303. 10.1001/jama.299.19.2294
Levy MM, Dellinger RP, Townsend SR, Linde-Zwirble WT, Marshall JC, Bion J, Schorr C, Artigas A, Ramsay G, Beale R, Parker MM, Gerlach H, Reinhart K, Silva E, Harvey M, Regan S, Angus DC: The Surviving Sepsis Campaign: results of an international guideline-based performance improvement program targeting severe sepsis. Crit Care Med 2010, 38: 367-374. 10.1097/CCM.0b013e3181cb0cdc
Suarez D, Ferrer R, Artigas A, Azkarate I, Garnacho-Montero J, Goma G, Levy MM, Ruiz JC: Cost-effectiveness of the Surviving Sepsis Campaign protocol for severe sepsis: a prospective nation-wide study in Spain. Intensive Care Med 2011, 37: 444-452. 10.1007/s00134-010-2102-3
Jansen TC, van Bommel J, Bakker J: Blood lactate monitoring in critically ill patients: a systematic health technology assessment. Crit Care Med 2009, 37: 2827-2839. 10.1097/CCM.0b013e3181a98899
Mikkelsen ME, Miltiades AN, Gaieski DF, Goyal M, Fuchs BD, Shah CV, Bellamy SL, Christie JD: Serum lactate is associated with mortality in severe sepsis independent of organ failure and shock. Crit Care Med 2009, 37: 1670-1677. 10.1097/CCM.0b013e31819fcf68
Okorie ON, Dellinger P: Lactate: biomarker and potential therapeutic target. Crit Care Clin 2011, 27: 299-326. 10.1016/j.ccc.2010.12.013
Bakker J, Gris P, Coffernils M, Kahn RJ, Vincent JL: Serial blood lactate levels can predict the development of multiple organ failure following septic shock. Am J Surg 1996, 171: 221-226. 10.1016/S0002-9610(97)89552-9
Nguyen HB, Rivers EP, Knoblich BP, Jacobsen G, Muzzin A, Ressler JA, Tomlanovich MC: Early lactate clearance is associated with improved outcome in severe sepsis and septic shock. Crit Care Med 2004, 32: 1637-1642. 10.1097/01.CCM.0000132904.35713.A7
Arnold RC, Shapiro NI, Jones AE, Schorr C, Pope J, Casner E, Parrillo JE, Dellinger RP, Trzeciak S: Multicenter study of early lactate clearance as a determinant of survival in patients with presumed sepsis. Shock 2009, 32: 35-39. 10.1097/SHK.0b013e3181971d47
Sepsis Bundle. Surviving Sepsis Campaign and Institute for Healthcare Improvement[http://wwwihiorg/IHI/Topics/CriticalCare/Sepsis]
Rivers E, Nguyen B, Havstad S, Ressler J, Muzzin A, Knoblich B, Peterson E, Tomlanovich M: Early goal-directed therapy in the treatment of severe sepsis and septic shock. N Engl J Med 2001, 345: 1368-1377. 10.1056/NEJMoa010307
Nguyen HB, Corbett SW, Steele R, Banta J, Clark RT, Hayes SR, Edwards J, Cho T, Wittlake WA: Implementation of a bundle of quality indicators for the early management of severe sepsis and septic shock is associated with decreased mortality. Crit Care Med 2007, 35: 1105-1112. 10.1097/01.CCM.0000259463.33848.3D
Girardis M, Rinaldi L, Donno L, Marietta M, Codeluppi M, Marchegiano P, Venturelli C: Effects on management and outcome of severe sepsis and septic shock patients admitted to the intensive care unit after implementation of a sepsis program: a pilot study. Crit Care 2009, 13: R143. 10.1186/cc8029
Castellanos-Ortega A, Suberviola B, Garcia-Astudillo LA, Holanda MS, Ortiz F, Llorca J, Delgado-Rodriguez M: Impact of the Surviving Sepsis Campaign protocols on hospital length of stay and mortality in septic shock patients: results of a three-year follow-up quasi-experimental study. Crit Care Med 2010, 38: 1036-1043. 10.1097/CCM.0b013e3181d455b6
Coba V, Whitmill M, Mooney R, Horst HM, Brandt MM, Digiovine B, Mlynarek M, McLellan B, Boleski G, Yang J, Conway W, Jordon J: Resuscitation bundle compliance in severe sepsis and septic shock: improves survival, is better late than never. J Intensive Care Med 2011, in press.
Mikkelsen ME, Gaieski DF, Goyal M, Miltiades AN, Munson JC, Pines JM, Fuchs BD, Shah CV, Bellamy SL, Christie JD: Factors associated with nonadherence to early goal-directed therapy in the ED. Chest 2010, 138: 551-558. 10.1378/chest.09-2210
Marik PE, Baram M, Vahid B: Does central venous pressure predict fluid responsiveness? A systematic review of the literature and the tale of seven mares. Chest 2008, 134: 172-178. 10.1378/chest.07-2331
van Beest PA, Hofstra JJ, Schultz MJ, Boerma EC, Spronk PE, Kuiper MA: The incidence of low venous oxygen saturation on admission to the intensive care unit: a multi-center observational study in The Netherlands. Crit Care 2008, 12: R33. 10.1186/cc6811
Pope JV, Jones AE, Gaieski DF, Arnold RC, Trzeciak S, Shapiro NI: Multicenter study of central venous oxygen saturation (ScvO 2 ) as a predictor of mortality in patients with sepsis. Ann Emerg Med 2010, 55: 40-46. e41 10.1016/j.annemergmed.2009.08.014
Gunn SR, Fink MP, Wallace B: Equipment review: the success of early goal-directed therapy for septic shock prompts evaluation of current approaches for monitoring the adequacy of resuscitation. Crit Care 2005, 9: 349-359. 10.1186/cc3725
Coen D, Vaccaro A, Cazzaniga M, Cortellaro F, Monti G, Tombini V: Toward a noninvasive approach to early goal-directed therapy. Chest 2011, 139: 726-727. 10.1378/chest.10-2632
Jones AE, Shapiro NI, Trzeciak S, Arnold RC, Claremont HA, Kline JA: Lactate clearance vs central venous oxygen saturation as goals of early sepsis therapy: a randomized clinical trial. JAMA 2010, 303: 739-746. 10.1001/jama.2010.158
Jansen TC, van Bommel J, Schoonderbeek FJ, Sleeswijk Visser SJ, van der Klooster JM, Lima AP, Willemsen SP, Bakker J: Early lactate-guided therapy in intensive care unit patients: a multicenter, open-label, randomized controlled trial. Am J Respir Crit Care Med 2010, 182: 752-761. 10.1164/rccm.200912-1918OC
Siegel JH, Fabian M, Smith JA, Kingston EP, Steele KA, Wells MR, Kaplan LJ: Oxygen debt criteria quantify the effectiveness of early partial resuscitation after hypovolemic hemorrhagic shock. J Trauma 2003, 54: 862-880; discussion 880. 10.1097/01.TA.0000066186.97206.39
Barbee RW, Reynolds PS, Ward KR: Assessing shock resuscitation strategies by oxygen debt repayment. Shock 2010, 33: 113-122. 10.1097/SHK.0b013e3181b8569d
Sakr Y, Dubois MJ, De Backer D, Creteur J, Vincent JL: Persistent microcirculatory alterations are associated with organ failure and death in patients with septic shock. Crit Care Med 2004, 32: 1825-1831. 10.1097/01.CCM.0000138558.16257.3F
Ranucci M, Isgro G, Carlucci C, De La Torre T, Enginoli S, Frigiola A: Central venous oxygen saturation and blood lactate levels during cardiopulmonary bypass are associated with outcome after pediatric cardiac surgery. Crit Care 2010, 14: R149.
Sauneuf B, Charbonneau P: Lactate clearance and central venous oxygen saturation in early sepsis. JAMA 2010, 303: 2031. author reply 2031-2032
Ho BC, Bellomo R, McGain F, Jones D, Naka T, Wan L, Braitberg G: The incidence and outcome of septic shock patients in the absence of early-goal directed therapy. Crit Care 2006, 10: R80. 10.1186/cc4918
Acknowledgements
The authors thank all members of the ATLAS (Asia neTwork to reguLAte Sepsis care) Investigators team who contributed to the study design and data collection: Sungwon Na, MD, Severance Hospital, Republic of Korea; Win Sen Kuan, MBBS, Malcolm Mahadevan, MBBS, National University Hospital, Singapore; Imron Subhan, MD, Mahesh Joshi, MD, Apollo Health City, Hyderabad, India; Chih-huang Li, MD, Chang-Gung Memorial Hospital, Keelung City, Taiwan; Pinak Shrikhande, MD, Amit Varma, MD, Fortis Healthcare, New Delhi, India; Shyr Chyr Chen, MD, National Taiwan University, Taipei, Taiwan; Niraj Tyagi, MD, and Sumit Ray, MD, Gangaram Hospital, New Delhi, India; and Zhu Ying, MD, and Lu Yiming, MD, Ruijin Hospital, Shanghai, China. They also thank the physicians, nurses, and administrators at the participating hospitals for their contribution and for improving patient care during the course of the present study.
Author information
Authors and Affiliations
Consortia
Corresponding author
Additional information
Competing interests
The investigator meetings for the present study were supported by Edwards Lifesciences, Asia Pacific, Singapore, in the form of administrative support and travel funding. HBN received funding support from Edwards Lifesciences, Asia Pacific, Singapore, to lead the study investigator meetings. The study sites received educational support from Edwards Lifesciences, Asia Pacific, Singapore, on the use of continuous ScvO2 monitoring. Edwards Lifesciences did not participate in the design of the study or the decision to submit this manuscript for publication.
Authors' contributions
HBN provided leadership and oversight in all aspects of the study, including study design, data collection, data analysis, and manuscript preparation. WSK, PS, MM, C-HL, and SR contributed to the study design, data collection, and preparation of the manuscript. MB and AD contributed to the data analysis and preparation of the manuscript. All authors read and approved the final manuscript.
Authors’ original submitted files for images
Below are the links to the authors’ original submitted files for images.
Rights and permissions
This article is published under an open access license. Please check the 'Copyright Information' section either on this page or in the PDF for details of this license and what re-use is permitted. If your intended use exceeds what is permitted by the license or if you are unable to locate the licence and re-use information, please contact the Rights and Permissions team.
About this article
Cite this article
Nguyen, H.B., Kuan, W.S., Batech, M. et al. Outcome effectiveness of the severe sepsis resuscitation bundle with addition of lactate clearance as a bundle item: a multi-national evaluation. Crit Care 15, R229 (2011). https://doi.org/10.1186/cc10469
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1186/cc10469