Abstract
Background
Bacterial vaginosis (BV) is a common gynecologic diagnosis characterized by dysbiosis of the vaginal microbiota. It is often accompanied by vaginal symptoms such as odor and discharge, but can be asymptomatic. Despite over 50 years of research, the etiology of BV is not well understood, which is a major impediment to treatment and prevention of BV.
Results
Here we report on the temporal dynamics of 25 vaginal communities over a 10 week period using samples collected daily from women who were diagnosed with symptomatic BV (15 women), asymptomatic BV (6 women), and women who did not have BV (4 women).
Conclusion
This unique resource of samples and data will contribute to a better understanding of the role that the vaginal microbes have in the natural history of BV and lead to improved diagnosis and treatment.
Similar content being viewed by others
Background
Bacterial vaginosis (BV) is the most common vaginal condition of women of reproductive age, resulting in millions of healthcare visits annually in the United States alone [1]. Women with BV typically report symptoms that include a thin vaginal discharge and a fishy malodor [2]; however, a substantial portion of affected women are asymptomatic [3]. Although the etiology of BV is incompletely understood, it is well-documented that BV is accompanied by, and perhaps caused by, disruption of the vaginal ecosystem that is reflected in alterations to the composition and structure of vaginal microbial communities [4, 5]. In women with BV, there are reduced proportions of lactic acid–producing bacteria (primarily Lactobacillus spp.) and increases in the number and diversity of facultative and strictly anaerobic bacteria, including species of Gardnerella, Prevotella and other taxa of the order Clostridiales [4]. BV has been shown to be an independent risk factor for adverse outcomes, including preterm delivery and low infant birth weight, the development of pelvic inflammatory disease [6] and increased risk of acquiring sexually transmitted infections and HIV [7–10]. National surveys estimate that the prevalence of BV among US women is 29% [11], and, despite the high burden of this disease, the events that precipitate BV remain obscure. BV is particularly troubling for patients and clinicians, as recurrence of BV following antibiotic treatment is common [12] and the arsenal of treatment includes just two antibiotics, namely, topical or oral metronidazole and clindamycin [2].
In clinical settings, BV is often diagnosed based on the criteria described by Amsel et al. [13], wherein three of the following four signs must be evident: (1) a homogeneous, white, noninflammatory discharge that smoothly coats the vaginal walls; (2) the presence of clue cells (squamous epithelial cells covered with adherent bacteria) upon microscopic examination; (3) a vaginal fluid pH over 4.5; and (4) a fishy odor after addition of 10% KOH to vaginal secretion samples. In research and laboratory settings, BV has also been diagnosed by scoring a Gram-stained vaginal smear [14–16]. One scoring method described by Nugent et al.[14] reflects the relative abundance of large Gram-positive rods (lactobacilli), Gram-negative and Gram-variable rods and cocci (including, G. vaginalis, Prevotella, Porphyromonas and peptostreptococci) and curved Gram-negative rods (Mobiluncus). The relative proportions of these different bacterial morphotypes give rise to a score that ranges from 0 to 10. A score of 0 to 3 is considered healthy, 4 to 6 is intermediate and 7 to 10 is indicative of BV. A weakness of diagnostic tests based on Gram-stained smears is the subjective nature of assessing bacterial cell morphology [17]. Gram staining can be performed on self-collected vaginal smears [18], which is critical for the success of longitudinal, field-based studies [19, 20].
Previous studies of BV have focused largely on women who presented to their physicians with symptoms or cohorts of women who were treated for BV and followed for extended observational periods with infrequent sampling. In one such study, Srinivasan et al. followed women diagnosed with BV daily for 7 days, then at 2, 3 and 4 weeks, and used quantitative PCR to determine the abundance of specific populations in vaginal samples [21]. The study demonstrated that vaginal microbiota are dynamic and that antibiotic treatment for BV rapidly reduces the number of facultative and strictly anaerobic species, but these bacteria later reemerged. These findings are consistent with the well-known phenomena of recurrent BV, in which the signs and symptoms of BV are alleviated by antibiotic use but return in the days and weeks that follow a course of therapy. These patterns of recurrence suggest that the vaginal environments of these women select for various populations of anaerobes. A better understanding of the events and conditions that cause shifts in the composition of the vaginal microbiome is needed to devise therapies that reduce the incidence of BV and its recurrence following antibiotic therapy.
In this study, we sought to evaluate the spectrum of events that occur in vaginal microbial communities prior to, during and after episodes of BV by characterizing the composition and dynamics of vaginal bacterial communities using high-throughput 454 pyrosequencing of barcoded V1 to V3 regions of 16S rRNA genes. To do this, we conducted a high-resolution prospective study in which samples were collected daily from 135 women of reproductive age over two menstrual cycles. Behaviors and events that took place before, during and after BV episodes were recorded. Herein we report our initial findings on the daily composition and relative abundance of bacteria in vaginal samples from 25 women, 15 of whom experienced symptomatic BV (SBV), 6 who were diagnosed with asymptomatic BV (ABV) and 4 who remained healthy during the 10-week study. These women were selected on the basis of their clinical examinations and the longitudinal patterns of changes in Nugent scores.
Methods
Participants and sample collection
Between September 2009 and July 2010, 135 nonpregnant women of reproductive age were enrolled in a longitudinal study at the University of Alabama at Birmingham. The clinical study protocol was approved by the Institutional Review Board of the University of Alabama at Birmingham and the University of Maryland School of Medicine. Written informed consent was appropriately obtained from all participants.
At study entry, participants were asked to answer a lengthy questionnaire on demographics as well as medical, dental, obstetric, hygiene, sexual and behavioral histories. They were also asked to self-collect three midvaginal swabs daily for ten weeks. The first Copan ESwab (Copan Diagnostics, Murrieta, CA, USA) was placed in RNAlater (Ambion, Austin, TX, USA) for use in future metatranscriptomics analyses. A second Copan ESwab was placed in Amies liquid transport medium for use later in extracting genomic DNA. Third, a Starplex double-headed Dacron swab (Starplex Scientific, Cleveland, TN, USA) was stored dry in a tube for later use in metabolomic and metaproteomic analyses. One of the Dacron swabs was also used to prepare a smear that was later Gram-stained for Nugent scoring. In addition, the participants measured their vaginal pH using the CarePlan VpH test glove (Inverness Medical Innovations, Waltham, MA, USA). Finally, participants completed a diary each day to record hygienic practices and sexual activities using a standardized form on which all responses were precoded. Pelvic examinations were performed at the time of enrollment and at weeks 5 and 10 or at interim times if the participant reported vaginal symptoms. A diagnosis of SBV was made when three of four Amsel criteria were recorded by the clinician and the participants reported symptoms spontaneously or upon direct questioning. ABV was defined as a finding of three of four Amsel criteria, but without self-report of any vaginal symptoms. Women diagnosed with SBV were treated for BV using standard of care practices [22]. Women with ABV were not treated. Clinical and selected daily behavioral data are described in Additional file 1.
DNA extraction and purification
Genomic DNA was extracted from vaginal swabs that had been stored in Amies liquid transport medium at -80°C. We used a validated procedure [23–25] that includes steps for enzymatic and physical lysis of bacterial cells followed by purification of genomic DNA using a QIAsymphony robotic platform and QIAGEN CellFree 500 kits (QIAGEN, Valencia, CA, USA) according to the manufacturer’s protocol. This procedure provided between 2.5 and 5 μg of high-quality genomic DNA from 300 μl of each sample resuspended from a vaginal swab (Additional file 2).
Polymerase chain reaction amplification and sequencing of the V1 to V3 region of bacterial 16S rRNA genes.
The composition and abundance in vaginal bacterial communities was determined using culture-independent methods. The V1 to V3 hypervariable region of 16S rRNA genes was amplified using an optimized barcoded primer set targeting 27f [26] and 533r. Amplifications were performed in 96-well plates using the HotStar HiFidelity DNA Polymerase Kit (QIAGEN). Amplicons were quantified using the Quant-iT PicoGreen kit (Molecular Probes/Invitrogen, Eugene, OR, USA), then equimolar amounts (100 ng) of amplicons were mixed in a single tube prior to purification with the Agencourt AMPure XP PCR Purification System (Beckman Coulter, Brea, CA, USA). Purified amplicon mixtures were sequenced by 454 pyrosequencing (454 Life Sciences, Branford, CT, USA) at the Genomics Resource Center of the Institute for Genome Sciences, University of Maryland School of Medicine.
Quality assurance
Sequence reads quality control, analysis and taxonomic assignments
Individual reads were quality-checked to eliminate short or chimeric reads, reads with ambiguous base pairs and those with low-quality regions using the criteria described in the Supplementary methods section. Taxonomic assignments were performed using a combination of a phylogenetics-based classifier and speciateIT software (http://www.speciateIT.sourceforge.net) (Additional file 3).
Initial findings
A total of 1,657 samples (a mean of 66.3 per woman, and a median of 67 per woman) were successfully sequenced, and 8,757,681 high-quality sequenced reads were generated with a mean of 5,285 and median of 5,093 reads per sample. Lower read counts were obtained for samples from subject 3 and subject 5 (weeks 1 to 3); however, these samples are still comparable to those with higher read counts as demonstrated previously [27] and are included in this data set. The mean read length was 485 bp (median of 515 bp).
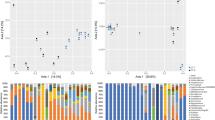
Unexpectedly, the vaginal microbiota prior to SBV mainly comprised strict anaerobes, such as Atopobium, Prevotella, Megasphaera, BV-associated bacterium 2 and the facultative anaerobe G. vaginalis, and the vaginal pH was elevated (>4.5) (Figure 1). During the 2- to 9-week interval prior to the diagnosis of SBV, a few symptoms were reported in daily diaries, but none of these prompted participants to immediately seek medical attention. Women who were diagnosed with ABV harbored vaginal microbiota that lacked significant proportions of Lactobacillus spp. and had symptoms similar to those of patients who ultimately were diagnosed with SBV (Figure 1A and B). Of note, Lactobacillus iners was consistently present in women who had SBV or ABV, albeit in low proportions (Figure 1 and Additional file 4: Figure S1). In most women, the treatment of SBV reduced the proportion of facultative and strict anaerobes and increased the relative proportions of Lactobacillus spp. (mainly L. iners) (Figure 1D to F). This effect was short-lived, however, and, in most individuals, the community returned to its pretreatment state within 2 to 4 weeks. Community dynamics in women who had ABV or SBV appeared to be highly personalized, with some women experiencing rapid shifts in community composition (Figure 1A, F and G) and others harboring stable, but Lactobacillus spp.-depleted, microbiota (Figure 1B to E and H). The vaginal microbiota of women who did not have SBV or ABV were consistently dominated by Lactobacillus spp. or Bifidobacterium, but were not always stable in terms of the dominant species of Lactobacillus present.
Daily temporal dynamics of vaginal bacterial communities. (A) and (B) Women diagnosed with asymptomatic bacterial vaginosis (ABV) at some point during the ten-week period are shown. (C) to (H) women diagnosed with symptomatic bacterial vaginosis (SBV) at some point during the ten-week period are shown. (A) through (H) Color codes for each phylotype represented in the interpolated bar plots are shown next to each panel. Pink open circles indicate symptomology. Red closed circles indicate menstruation days. Large black open circles represent ABV diagnosis. Large black closed circles represent symptomatic BV diagnosis. Small closed circles indicate BV medications used. Daily Nugent scores (range: 0 to 10) and pH (range: 4 to 7) are indicated below the graphs. See Additional file 4: Figure S1 for interpolated bar plots for all subjects.
Future directions
We will use these data to examine shifts in vaginal microbial community composition in conjunction with epidemiological and behavioral data to better define BV and identify patterns that predict an increased risk for the disease. This study will be done using model-based statistical clustering and classification approaches to associate microbial community composition and dynamics with metadata and clinical diagnoses of health or BV. The large body of information generated will facilitate understanding vaginal microbial community dynamics and the etiology of BV, and it will drive the development of better diagnostic tools for use in the differential diagnosis of BV. Furthermore, we anticipate that the information will enable a more personalized, more effective treatment of BV and ultimately help to prevent adverse sequelae associated with this highly prevalent disruption of the vaginal microbiome.
Supporting data
All sequence data and metadata were deposited in the Sequence Read Archive (SRA; http://www.ncbi.nlm.nih.gov/Traces/sra/) under BioProject PRJNA208535 (“The daily dynamics of the vaginal microbiota before and after bacterial vaginosis”; http://www.ncbi.nlm.nih.gov/bioproject/?term=PRJNA208535) ([SRP026107] and [SRA091234]). Quantitative Insights Into Microbial Ecology (QIIME software) mapping files are provided in Additional file 5. Because of the sensitivity of the metadata and Institutional Review Board restrictions, additional metadata can be requested only directly from the principal investigators.
Abbreviations
- PCR:
-
Polymerase chain reaction.
References
Martin DH: The microbiota of the vagina and its influence on women’s health and disease. Am J Med Sci. 2012, 343: 2-9. 10.1097/MAJ.0b013e31823ea228.
Workowski KA, Berman SM, Centers for Disease Control and Prevention: Sexually transmitted diseases treatment guidelines, 2006. MMWR Recomm Rep. 2006, 55 (RR-11): 1-94.
Klebanoff MA, Schwebke JR, Zhang J, Nansel TR, Yu KF, Andrews WW: Vulvovaginal symptoms in women with bacterial vaginosis. Obstet Gynecol. 2004, 104: 267-272. 10.1097/01.AOG.0000134783.98382.b0.
Fredricks DN, Fiedler TL, Marrazzo JM: Molecular identification of bacteria associated with bacterial vaginosis. N Engl J Med. 2005, 353: 1899-1911. 10.1056/NEJMoa043802.
Srinivasan S, Hoffman NG, Morgan MT, Matsen FA, Fiedler TL, Hall RW, Ross FJ, McCoy CO, Bumgarner R, Marrazzo JM, Fredricks DN: Bacterial communities in women with bacterial vaginosis: high resolution phylogenetic analyses reveal relationships of microbiota to clinical criteria. PLoS One. 2012, 7: e37818-10.1371/journal.pone.0037818.
Ness RB, Kip KE, Hillier SL, Soper DE, Stamm CA, Sweet RL, Rice P, Richter HE: A cluster analysis of bacterial vaginosis-associated microflora and pelvic inflammatory disease. Am J Epidemiol. 2005, 162: 585-590. 10.1093/aje/kwi243.
Wiesenfeld HC, Hillier SL, Krohn MA, Landers DV, Sweet RL: Bacterial vaginosis is a strong predictor of Neisseria gonorrhoeae and Chlamydia trachomatis infection. Clin Infect Dis. 2003, 36: 663-668. 10.1086/367658.
Cherpes TL, Meyn LA, Krohn MA, Lurie JG, Hillier SL: Association between acquisition of herpes simplex virus type 2 in women and bacterial vaginosis. Clin Infect Dis. 2003, 37: 319-325. 10.1086/375819.
Peters SE, Beck-Sagué CM, Farshy CE, Gibson I, Kubota KA, Solomon F, Morse SA, Sievert AJ, Black CM: Behaviors associated with Neisseria gonorrhoeae and Chlamydia trachomatis: cervical infection among young women attending adolescent clinics. Clin Pediatr (Phila). 2000, 39: 173-177. 10.1177/000992280003900307.
Martin HL, Richardson BA, Nyange PM, Lavreys L, Hillier SL, Chohan B, Mandaliya K, Ndinya-Achola JO, Bwayo J, Kreiss J: Vaginal lactobacilli, microbial flora, and risk of human immunodeficiency virus type 1 and sexually transmitted disease acquisition. J Infect Dis. 1999, 180: 1863-1868. 10.1086/315127.
Koumans EH, Sternberg M, Bruce C, McQuillan G, Kendrick J, Sutton M, Markowitz LE: The prevalence of bacterial vaginosis in the United States, 2001–2004: associations with symptoms, sexual behaviors, and reproductive health. Sex Transm Dis. 2007, 34: 864-869. 10.1097/OLQ.0b013e318074e565.
Sobel JD, Ferris D, Schwebke J, Nyirjesy P, Wiesenfeld HC, Peipert J, Soper D, Ohmit SE, Hillier SL: Suppressive antibacterial therapy with 0.75% metronidazole vaginal gel to prevent recurrent bacterial vaginosis. Am J Obstet Gynecol. 2006, 194: 1283-1289. 10.1016/j.ajog.2005.11.041.
Amsel R, Totten PA, Spiegel CA, Chen KC, Eschenbach D, Holmes KK: Nonspecific vaginitis: diagnostic criteria and microbial and epidemiologic associations. Am J Med. 1983, 74: 14-22. 10.1016/0002-9343(83)91112-9.
Nugent RP, Krohn MA, Hillier SL: Reliability of diagnosing bacterial vaginosis is improved by a standardized method of Gram stain interpretation. J Clin Microbiol. 1991, 29: 297-301.
Ison CA, Hay PE: Validation of a simplified grading of Gram stained vaginal smears for use in genitourinary medicine clinics. Sex Transm Infect. 2002, 78: 413-415. 10.1136/sti.78.6.413.
Spiegel CA, Amsel R, Holmes KK: Diagnosis of bacterial vaginosis by direct Gram stain of vaginal fluid. J Clin Microbiol. 1983, 18: 170-177.
Joesoef MR, Hillier SL, Josodiwondo S, Linnan M: Reproducibility of a scoring system for Gram stain diagnosis of bacterial vaginosis. J Clin Microbiol. 1991, 29: 1730-1731.
Morgan DJ, Aboud CJ, McCaffrey IM, Bhide SA, Lamont RF, Taylor-Robinson D: Comparison of Gram-stained smears prepared from blind vaginal swabs with those obtained at speculum examination for the assessment of vaginal flora. Brit J Obstet Gynaecol. 1996, 103: 1105-1108. 10.1111/j.1471-0528.1996.tb09591.x.
Brotman RM, Ghanem KG, Klebanoff MA, Taha TE, Scharfstein DO, Zenilman JM: The effect of vaginal douching cessation on bacterial vaginosis: a pilot study. Am J Obstet Gynecol. 2008, 198: 628.e1-629.e7.
Schwebke JR, Morgan SC, Weiss HL: The use of sequential self-obtained vaginal smears for detecting changes in the vaginal flora. Sex Transm Dis. 1997, 24: 236-239. 10.1097/00007435-199704000-00009.
Srinivasan S, Liu C, Mitchell CM, Fiedler TL, Thomas KK, Agnew KJ, Marrazzo JM, Fredricks DN: Temporal variability of human vaginal bacteria and relationship with bacterial vaginosis. PLoS One. 2010, 5: e10197-10.1371/journal.pone.0010197.
Workowski KA, Berman S, Centers for Disease Control and Prevention (CDC): Sexually transmitted diseases treatment guidelines, 2010. MMWR Recomm Rep. 2010, 59 (RR-12): 1-110. A published erratum appears in MMWR Recomm Rep 2011, 60(1):18 [dosage error in article text]
Forney LJ, Gajer P, Williams CJ, Schneider GM, Koenig SS, McCulle SL, Karlebach S, Brotman RM, Davis CC, Ault K, Ravel J: Comparison of self-collected and physician-collected vaginal swabs for microbiome analysis. J Clin Microbiol. 2010, 48: 1741-1748. 10.1128/JCM.01710-09.
Ravel J, Gajer P, Abdo Z, Schneider GM, Koenig SS, McCulle SL, Karlebach S, Gorle R, Russell J, Tacket CO, Brotman RM, Davis CC, Ault K, Peralta L, Forney LJ: Vaginal microbiome of reproductive-age women. Proc Natl Acad Sci USA. 2011, 108 (Suppl 1): 4680-4687.
Yuan S, Cohen DB, Ravel J, Abdo Z, Forney LJ: Evaluation of methods for the extraction and purification of DNA from the human microbiome. PLoS One. 2012, 7: e33865-10.1371/journal.pone.0033865.
Frank JA, Reich CI, Sharma S, Weisbaum JS, Wilson BA, Olsen GJ: Critical evaluation of two primers commonly used for amplification of bacterial 16S rRNA genes. Appl Environ Microbiol. 2008, 74: 2461-2470. 10.1128/AEM.02272-07.
Caporaso JG, Lauber CL, Walters WA, Berg-Lyons D, Huntley J, Fierer N, Owens SM, Betley J, Fraser L, Bauer M, Gormley N, Gilbert JA, Smith G, Knight R: Ultra-high-throughput microbial community analysis on the Illumina HiSeq and MiSeq platforms. ISME J. 2012, 6: 1621-1624. 10.1038/ismej.2012.8.
Acknowledgements
The research reported in this publication was supported by National Institute of Allergy and Infectious Diseases grants from the National Institutes of Health (NIH) under award numbers UH2AI083264 and K01 AI080974. The content is solely the responsibility of the authors and does not necessarily represent the official views of the NIH.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Competing interests
The authors declare that they have no competing interests.
Authors’ contributions
JR, RMB, PG and LJF designed the study. JRS lead the clinical study and sample collection. MN, DWF, JS, SSKK, LF and XZ processed the samples and generated the sequence data. PG, BM, JR, XZ, RJH and LJF analyzed and interpreted the data. JR, PG, RMB and LJF wrote the manuscript. All authors read and approved the final manuscript.
Electronic supplementary material
40168_2013_28_MOESM4_ESM.pdf
Additional file 4: Figure S1: Daily temporal dynamics of vaginal bacterial communities in 15 women who experienced symptomatic BV diagnosis (A to O), asymptomatic BV only (P to U) at some point during a 10-week period or no BV (V to Y). Color codes for each phylotype represented in the interpolated bar plots are shown next to each panel. Pink open circles: symptomology; red closed circles: menstruation days (small circles indicate low bleeding, medium circles, medium bleeding and large circles heavy bleeding); large black open circles: asymptomatic BV diagnosis; large black closed circles: symptomatic BV diagnosis; small closed circles: BV medication used. Daily Nugent scores (range 0–10) and pH (range 4–7) are indicated below the graph. (PDF 3 MB)
Rights and permissions
This article is published under an open access license. Please check the 'Copyright Information' section either on this page or in the PDF for details of this license and what re-use is permitted. If your intended use exceeds what is permitted by the license or if you are unable to locate the licence and re-use information, please contact the Rights and Permissions team.
About this article
Cite this article
Ravel, J., Brotman, R.M., Gajer, P. et al. Daily temporal dynamics of vaginal microbiota before, during and after episodes of bacterial vaginosis. Microbiome 1, 29 (2013). https://doi.org/10.1186/2049-2618-1-29
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/2049-2618-1-29