Abstract
Background
Human bocavirus (HBoV) is a recently discovered parvovirus associated with mild to severe lower respiratory tract infections in children, the aim of the work was determination of human bocavirus in nasopharyngeal aspirate (NPA) of infants by qualitative PCR and determination of acute human bocavirus infection by estimation of immunoglobulin M (IgM) antibodies in serum by enzyme linked immunosorbent assay.
Results
Twenty two (22%) out of the 100 NPA specimens of the patients with respiratory manifestations were positive for HBoV by qualitative PCR, while ELISA revealed positive HBoV IgM antibodies in 18 (18%) patients who were also positive by PCR. Non of the controls were positive by both techniques. The correlation study between ELISA and PCR revealed high significant association, (p < 0.001, X2 = 36 and agreement = 96%). Also PCR detected 4 (18.1%) NPA samples as HBoV positive cases among the patients that were not identified by ELISA. This could be due to high sensitivity and efficacy of PCR. ELISA being less sensitive than RT-PCR, sensitivity was (81.8% vs 100%), the efficacy was 97.7% in ELISA versus 99.7% for RT-PCR.
Conclusion
HBoV infections could be diagnosed in NPA of children by conventional PCR as a rapid and sensitive technique. While ELISA was a reliable serologic analysis for diagnosis of acute HBoV infection by estimation IgM antibodies in serum.
Similar content being viewed by others
Background
In 2005, Allander et al., [1] reported the discovery of a previously undescribed human parvovirus in respiratory secretions from children with respiratory tract disease in Sweden. Phylogenetic analysis showed that this virus belonged to the genus Bocavirus (subfamily, Parvovirinae; family, Parvoviridae) and was most closely related to bovine parvovirus (BP) and minute virus of canines (MVC). The virus was thus named "human bocavirus" (HBoV).
Human bocaviruses (HBoV) contain 3 open reading frames (ORFs) encoding a nonstructural protein (NS1, NP1) and two capsid proteins VP1 and VP2, respectively [2]. The genomic organization of HBoV closely resembles that of bovine parvovirus type 1 [1].
HBoV has been reported in respiratory samples from children with acute respiratory tract disease in various parts of the world (including Australia, North America, Europe, Asia, and Africa), suggesting that the virus is circulating worldwide [3]. Pneumonia, acute bronchitis, bronchiolitis, are the main manifestations of HBoV infection [4].
HBoV seems to be a new member of the community-acquired respiratory viruses such as respiratory syncytial virus, adenovirus, influenza virus, parainfluenza virus, and rhinovirus, which cause common respiratory tract infections in the community [5]. Because of its very high copy numbers in respiratory tract secretions, aerosol and contact transmission are likely effective, as they are for other respiratory viruses [6].
HBoV has been detected also in nasopharyngeal, serum, fecal and urine samples obtained mainly from young children around the age of 2 years predominantly during the winter season [1]. HBoV was detected in two pediatric patients after organ transplantation [7], in human immunodeficiency virus-infected pediatric patients [8], and immunosuppressed adult patients [9].
Diagnosis of HBoV infection is based on the PCR amplification of viral genome fragments present in human respiratory, serum, stool and urine samples. A great number of different PCR techniques employing varying sets of primers specific for the viral genes NP1[10], NS1 [11], and VP1, VP2 [12, 13] have been described. In addition to the detection of viral genomes by PCR, recent reports describe the detection of HBoV-specific IgG and IgM-antibodies against HBoV VP2 in serum samples using western blot [14] or immunofluorescence assays [2, 15]. Furthermore, a standardized ELISA for the quantitative determination of HBoV-specific antibodies has been established by [16]. The aim of the work was determination of HBoV in respiratory specimens (NPA) of infants by qualitative PCR and determination of acute HBoV infection by estimation of IgM antibodies in serum by ELISA.
Results
Microbiological results
Cultures of nasopharyngeal aspirates from 100 patients were positive in 67% of patients. Cultures yielded growth of one or more pathogen among upper respiratory tract normal flora. Gram positive cocci were isolated from 57/90 (63.3%) of specimens including: Streptococcus pneumoniae 25/90 (27.7%), Staphylococcus aureus 32/90 (35.5%). Gram negative bacilli were detected in 33/90(36.6%) of specimens including, Klebsiella pneumoniae 15/90 (16.6%), Escherichia coli 10/90 (11.1%), Pseudomonas aeruginosa 8/90 (8.8%), while Cultures of the control group showed growth of upper respiratory tract normal flora (table 1).
Qualitative PCR results
Twenty two (22%) out of the 100 NPA specimens of the patients were positive for HBoV and 78 (78%) specimens were negative by qualitative PCR. While all the 50 NPA of the control group were negative for HBoV. Also there was a high significant difference between the patient and the control groups since p < 0.001 (table 2).
ELISA results
Eighteen (18%) out of the 100 serum samples of the patients with respiratory tract manifestations were positive for HBoV IgM antibodies by ELISA such patients are also positive by PCR, and 82 (82%) specimens were HBoV negative by ELISA. While all 50 serum samples of the controls were negative (table 3). Serum concentration of IgM antibodies against HBoV were detected significantly in patients (0.28 ± 0.06 vs 0.07 ± 0.01 controls), p < 0.001. Table 4 showed the number of positive cases by the different diagnostic methods. Table 5 showed that there was a highly significant association between the PCR and ELISA techniques.
Diagnostic validity tests
Diagnostic validity test including sensitivity, specificity, predictive values and efficacy of both HBoV ELISA and PCR were calculated (table 6 and 7) considering PCR as a reference method. In our work we found ELISA to be less sensitive than PCR, it was (81.8% vs 100%), but the specificity of ELISA is higher than PCR, it was (100% vs 78%) (table 6 and 7).
Discussion
In recent years, several novel viruses have been discovered in patients with respiratory infections using molecular biology methods. These novel viruses include the human metapneumovirus and several coronaviruses (SARS, NL63, and HKU1) [17, 18] the latest addition to this list was the human bocavirus (HBoV).
Attempts to culture this virus on conventional cell lines had failed but, Dijkman et al., [19] had investigated whether the virus can replicate on pseudostratified human airway epithelium. The cells were inoculated with human bocavirus-positive nasopharyngeal washes from children, and virus replication was monitored by measuring apical release of the virus via real-time PCR.
Electron Microscopy supported the ultrastructure analysis of the HBoV virus like particles (VLP) using a transmission electron microscope equipped with digital camera [20].
In our work 22 (22%) out of the 100 NPA specimens of the patients were positive for HBoV, There was a high significant difference between the patient and the control groups (p < 0.001). PCR detected four HBoV positive cases that were negative by ELISA, this could be explained by the high sensitivity of PCR over ELISA since it was (100% vs 81.1%) respectively. Weissbrich et al., [21] had found HBoV DNA in (10.3%) of NPA samples obtained from 786 hospitalized infants and children with febrile respiratory tract diseases during the years 2002 to 2005 in the region of northern Bavaria in Germany. While Neske et al., [22] had studied 834 nasopharyngeal aspirates (NPA), 10 serum samples, and 31 stool samples of children with acute respiratory diseases. For phylogenetic analysis, the VP2 genes were sequenced from 69 HBoV-positive NPA samples. The qualitative results of the real-time HBoV PCR were in good agreement with a conventional HBoV PCR. They found that 12% of the NPA were positive for HBoV DNA by both techniques.
Söderlund-Venermo et al., [23] reported that the unique region in VP1 is less immunogenic than the major virus capsid protein VP2, Also he expressed HBoV VP2 viral like particles (VLPs) in insect cells for use in IgM and IgG ELISA that are superior to immunoblots in diagnostic performance.
In the present study 18 (18%) out of the 100 serum samples of the patients with respiratory tract manifestations were positive for HBoV IgM antibodies by ELISA. There was a significant difference between the patient and the control group (p < 0.001). The mean serum concentration of IgM antibodies against HBoV, in the two groups was (0.28 ± 0.06 vs 0.07 ± 0.01). There was also a highly significant association between PCR and ELISA techniques (p < 0.001 and agreement = 96%). Söderlund-Venermo et al., [23] diagnosed acute primary HBoV infections in 49 (19%) of 258 children with expiratory wheezing, and Lindner et al., [24] detected IgM against HBoV by ELISA in 10/24 (42%) of sera samples obtained from HBoV DNA-positive children and infants with infections of the respiratory tract.
In the present study sensitivity, specificity, positive predictive value and efficacy of ELISA were 81.8%,100%,100% and 97.7% respectively Lindner et al., [16] had reported diagnostic sensitivity and specificity of their antibody ELISA were as high as 97% and 99.5%, respectively; positive predictive value was 97% by using ELISA among wheezing children.
Conclusion
HBoV infections could be diagnosed in NPA by conventional PCR as a rapid and sensitive technique. ELISA was a reliable serologic analysis for diagnosis of acute HBoV infection by estimation IgM antibodies in serum.
Methods
The present case - control study was conducted on 100 patients aged from 1 to 5 years (61 males and 39 females) with a mean ± SD age of (2.7 ± 1.1) attending the Pediatric outpatient clinic, Ain Shams University Hospitals, Cairo, Egypt in the period from September 2009 to May 2010. Patients were suffering from lower respiratory tract infection together with upper respiratory tract manifestations such as cough, running nose and fever. In addition to 50 apparently healthy children (32 males and 18 females) matched in age with the patients as a control group.
All patients were subjected to the following after their written consent, full history taking and thorough clinical examination, complete blood picture, chest plain X-ray. Nasopharyngeal aspirate (NPA) samples collected from both patient and control groups were subjected to microbiological examination and qualitative polymerase chain reaction (PCR) for detection HBoV. Serum samples were collected from both patient and control groups for detection of HBoV- IgM antibodies by ELISA.
Sample collection
Nasopharyngeal aspirates were collected from patients and control group according to Svensson et al., [25]. Sterile normal saline solution was instilled in one nostril while occluding the other nostril, using a sterile blunt-tipped disposable syringe. Then the patient was instructed to forcibly exhale through the lavaged side into a sterile specimen cup. The sequence was then repeated in the other side of the nose. NPA specimens were examined microbiologically immediately and part of the specimens was stored in aliquots at -70°C for PCR. Two ml blood samples from both patients and control were collected into vacutainer, centrifuged and serum was separated and stored at - 20°C for HBoV-IgM antibodies by ELISA.
Microbiological examination
It was done by Gram stained smear for detection of pus cells and microorganisms. Quantitative culture of NPA specimens of patients and control was done. Undiluted and tenfold serial dilutions were inoculated with a calibrated loop on chocolate agar, blood agar and MacConkey agar plates, after over night incubation in appropriate conditions, Quantitative NPA cultures were considered positive when the growth of 106 (cfu/ml) or more was observed [26].
Qualitative polymerase chain reaction (PCR)
DNA was extracted from 200 μl of the NPA samples using the High Pure Viral Nucleic Acid Kit (Roche, Mannheim, Germany) according to the instructions of the manufacturer.
Amplification of hBoV DNA was performed using 50 μl elution volume with the NP-1 primers BoV188F and BoV542R described by Allander et al., [1] (table 8) using the HotStarTaq DNA Polymerase (Qiagen, Hilden, Germany). PCR reactions were carried out in a 50 μl volume consisting of 5 μl extracted DNA, 1× Qiagen HotStar buffer, dNTPs at a final concentration of 200 μM each, 200 pmol of each primer, and 1.5 U of Taq Polymerase. The cycling conditions were 50 cycles (94°C 30 s, 53°C 40 s and 1 min at 72°C) after a preheating step of 10 min at 95°C.
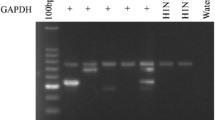
After amplification, PCR products were visualized by staining with ethidium bromide on agarose gels. A PCR reaction was considered as positive when a band of the expected size (354 base pairs) was visible.
A plasmid containing the PCR product cloned in the vector PCR 2.1-TOPO (Invitrogen) was used as positive control.
Enzyme linked immunosorbent assay (ELISA)
HBoV-IgM antibodies were determined by a commercially available immunoglobulin M (IgM) enzyme-linked immunosorbent assay supplied by (Dako, Glostrup, Denmark) for the quantitative determination of IgM antibodies to HBoV in serum. Briefly: serum samples diluted 1:200 in phosphate buffer saline (PBS) and 0.05% Tween (PBST) were applied in duplicate into wells of plates coated with goat anti-human IgM for 60 min at room temperature. After being rinsed 5 times with PBST, biotinylated HBoV viral like particles (VLPs) were applied at a concentration of 25 ng/well and incubated for 45 min at 37°C. Bound antigen was visualized by using horseradish peroxidase-conjugated streptavidin at 1:12,000 in PBST plus 0.5% bovine serum albumin for 45 min at 37°C, followed by o-phenylenediamine dihydrochloride and H2O2 for 15 min at 37°C. The reaction was stopped after 10 min with 0.5 M H2SO4, and the absorbance at 492 nm were recorded. Cut off absorbance for negative and positive IgM ELISA results were 0.136 and 0.167, respectively.
Statistical analysis
Association between PCR and ELISA for diagnosis of HBoV infection was evaluated using CHI square test. Significance (p < 0.05). Diagnostic validity test including sensitivity, specificity, positive and negative predictive values were calculated considering the PCR a reference method for diagnosis of HBoV infection. The diagnostic power of both ELISA and PCR was estimated using the efficacy rate.
References
Allander T, Tammi MT, Eriksson M, Bjerkner A, Tiveljung-Lindell A, Andersson B: Cloning of a human parvovirus by molecular screening of respiratory tract samples. Proc Natl Acad Sci USA 2005,102(36):12891-6. 10.1073/pnas.0504666102
Endo R, Ishiguro N, Kikuta H, et al.: Seroepidemiology of human bocavirus in Hokkaido prefecture, Japan. J Clin Microbiol 2007, 45: 3218-23. 10.1128/JCM.02140-06
Sloots TP, McErlean P, Speicher DJ, Arden KE, Nissen MD, Mackay IM: Evidence of human coronavirus HKU1 and human bocavirus in Australian children. J Clin Virol 2006, 35: 99-102. 10.1016/j.jcv.2005.09.008
Lau SK, Yip CC, Que TL, Lee RA, Au-Yeung RK, Zhou B, So LY, Lau YL, Chan KH, Woo PC, Yuen KY: Clinical and molecular epidemiology of human bocavirus in respiratory and fecal samples from children in Hong Kong. J Infect Dis 2007, 196: 986-993. 10.1086/521310
Arden KE, McErlean P, Nissen MD, Sloots TP, Mackay IM: Frequent detection of human rhinoviruses, paramyxoviruses, coronaviruses, and bocavirus during acute respiratory tract infections. J Med Virol 2006, 78: 1232-1240. 10.1002/jmv.20689
Schildgen O, Müller A, Allander T, Mackay IM, Völz S, Kupfer B, Simon A: Human bocavirus: passenger or pathogen in acute respiratory tract infections? Clin Microbiol Rev 2008,21(2):291-304. 10.1128/CMR.00030-07
Arnold JC, Singh KK, Spector SA, Sawyer MH: Human bocavirus: prevalence and clinical spectrum at a children's hospital. Clin Infect Dis 2006, 43: 283-288. 10.1086/505399
Smuts H, Hardie D: Human bocavirus in hospitalized children, South Africa. Emerg Infect Dis 2006, 12: 1457-1458.
Manning A, Russell V, Eastick E, Leadbetter GH, Hallam N, Templeton K, Simmonds P: Epidemiological profile and clinical associations of human bocavirus and other human parvoviruses. J Infect 2006, 12: 56-60.
Simon A, Groneck P, Kupfer B, Kaiser R, Plum G, Tillmann RL, Muller A, Schildgen O: Detection of bocavirus DNA in nasopharyngeal aspirates of a child with bronchiolitis. J Infect 2007, 54: e125-e127. 10.1016/j.jinf.2006.08.001
Regamey N, Frey U, Deffernez C, Latzin PK, Aiser L: Isolation of human bocavirus from Swiss infants with respiratory infections. Pediatr Infect Dis J 2007, 26: 177-179. 10.1097/01.inf.0000250623.43107.bc
Bastien N, Chui N, Robinson JL, Lee BE, Dust K, Hart L, Li Y: Detection of human bocavirus in Canadian children in a 1-year study. J Clin Microbiol 2007, 45: 610-613. 10.1128/JCM.01044-06
Lee JI, Chung JY, Han TH, Song MO, Hwang ES: Detection of human bocavirus in children hospitalized because of acute gastroenteritis. J Infect Dis 2007, 196: 994-997. 10.1086/521366
Kantola K, Hedman L, Allander T, Jartti T, Lehtinen P, Ruuskanen O, Hedman K, Soderlund-Venermo M: Serdiagnosis of human bocavirus infections. J Infect Dis 2008, 46: 540-546. 10.1086/526532
Neske F, Prifert C, Scheiner B, Ewald M, Schubert J, Opitz A, Weissbrich B: High prevalence of antibodies against polyomavirus WU, polyomavirus KI, and human bocavirus in German blood donors. BMC Infect Dis 2010, 10: 215. 10.1186/1471-2334-10-215
Lindner J, Modrow S: Human bocavirus: a novel parvovirus to infect humans. Intervirology 2008,51(2):116-22. 10.1159/000137411
Fouchier RA, Rimmelzwaan GF, Kuiken T, Osterhaus AD: Newer respiratory virus infections: human metapneumovirus, avian influenza virus, and human coronaviruses. Curr Opin Infect Dis 2005, 18: 141-146. 10.1097/01.qco.0000160903.56566.84
Woo PC, Lau SK, Chu CM, Chan KH, Tsoi HW, Huang Y, Wong BH, Poon RW, Cai JJ, Luk WK, Poon LL, Wong SS, Guan Y, Peiris JS, Yuen KY: Characterization and complete genome sequence of a novel coronavirus, coronavirus HKU1, from patients with pneumonia. J Virol 2005, 79: 884-895. 10.1128/JVI.79.2.884-895.2005
Dijkman R, Koekkoek SM, Molenkamp R, Schildgen O, van der Hoek L: Human bocavirus can be cultured in differentiated human airway epithelial cells. J Virol 2009,83(15):7739-48. 10.1128/JVI.00614-09
Cecchini S, Negrete A, Virag T, Graham BS, Cohen JI, Kotin RM: Evidence of prior exposure to human bocavirus as determined by a retrospective serological study of 404 serum samples from adults in the United States. Clin Vaccine Immunol 2009,16(5):597-604. 10.1128/CVI.00470-08
Weissbrich B, Neske F, Schubert J, Tollmann F, Blath K, Blessing K, Kreth HW: Frequent detection of Bocavirus DNA in German children with respiratory tract infections. BMC Infect Dis 2006, 6: 109. 10.1186/1471-2334-6-109
Neske F, Blessing K, Tollmann F, Schubert J, Rethwilm A, Kreth HW, Weissbrich B: Real-time PCR for diagnosis of human bocavirus infections and phylogenetic analysis. J Clin Microbiol 2007,45(7):2116-22. 10.1128/JCM.00027-07
Söderlund-Venermo M, Lahtinen A, Jartti T, Hedman L, Kemppainen K, Lehtinen P, Allander T, Ruuskanen O, Hedman K: Clinical assessment and improved diagnosis of bocavirus-induced wheezing in children, Finland. Emerg Infect Dis 2009,15(9):1423-30.
Lindner J, Karalar L, Zehentmeier S, Plentz AS, Pfister H, Struff W, et al.: Humoral immune response against human bocavirus VP2 virus-like particles. Viral Immunol 2008, 21: 443-9. 10.1089/vim.2008.0045
Svensson C, Andersson M, Persson CG, Venge P: Albumin bradykinin, and eosinophil cationic protein on the nasal mucosal surface in patients with hay fever during natural allergen exposure. J Allergy Clin Immunol 1990, 85: 828-33. 10.1016/0091-6749(90)90064-B
Barrow GI, Feltham RK: Cowman and Steel's manual for the identification of medical bacteria. 3rd edition. Cambridge: Cambridge University Press; 1993.
Author information
Authors and Affiliations
Corresponding author
Additional information
Competing interests
The author declares that she has no competing interests.
Authors' contributions
MZ carried out the enzyme linked immunosorbent assay, qualitative polymerase chain reaction, drafted the manuscript, designed the study and performed the statistical analysis. The author read and approved the final manuscript.
Rights and permissions
This article is published under license to BioMed Central Ltd. This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/2.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
About this article
Cite this article
Zaghloul, M.Z. Human bocavirus (HBoV) in children with respiratory tract infection by enzyme linked immunosorbent assay (ELISA) and qualitative polymerase chain reaction (PCR). Virol J 8, 239 (2011). https://doi.org/10.1186/1743-422X-8-239
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/1743-422X-8-239