Abstract
The low-grade, chronic, systemic inflammatory state that characterizes the aging process (inflammaging) results from late evolutive-based expression of the innate immune system. Inflammaging is characterized by the complex set of five conditions which can be described as 1. low-grade, 2. controlled, 3. asymptomatic, 4. chronic, 5. systemic, inflammatory state, and fits with the antagonistic pleiotropy theory on the evolution of aging postulating that senescence is the late deleterious effect of genes (pro-inflammatory versus anti-inflammatory)that are beneficial in early life. Evolutionary programming of the innate immune system may act via selection on these genetic traits. Here I propose that the already acquired knowledge in this field may pave the way to a new chapter in the pathophysiology of autoimmunity: the auto-innate-immunity syndromes. Indeed, differently from the well known chapter of conventional autoimmune diseases and syndromes where the main actor is the adaptive immunity, inflammaging may constitute the subclinical paradigm of a new chapter of autoimmunity, namely that arising from an autoimmune inflammatory response of the innate-immune-system, an old actor of immunity and yet a new actor of autoimmunity, also acting as a major determinant of elderly frailty and age-associated diseases.
Similar content being viewed by others
Auto [innate]immunity: a new chapter of autoimmunity
The term "Inflammaging" has been coined by Claudio Franceschi to explain the now widely accepted phenomenon that ageing is accompanied by a low-grade chronic, systemic up-regulation of the inflammatory response and that the underlining inflammatory changes are also common to most age-associated diseases [1–8].
From a review of the literature on Inflammaging [1–8] I suggest that, like acute inflammation is well known to be associated with the five cardinal features 1. rubor (redness), 2. tumor (swelling), 3. dolor (pain), 4. calor (warm), 5. functio lesa (loss of function), on the contrary, inflammaging is characterized by the complex set of five conditions which can be described as 1. low-grade, 2. controlled, 3. asymptomatic, 4. chronic, 5. systemic, inflammatory state.
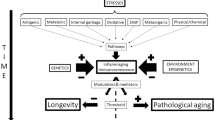
The inflammatory scenario that characterizes inflammaging constitutes a highly complex response to various subtle internal and environmental inflammatory stimuli mediated mainly by the increased circulating levels of pro-inflammatory cytokines. Inflammaging also generates Reactive Oxygen Species (ROS) causing both oxidative damage and eliciting an amplification of the cytokines' release, thus perpetuating a vicious cycle resulting in a chronic systemic pro-inflammatory state where tissue injury and healing mechanisms proceed simultaneously and damage slowly accumulates asymptomatically over decades and is a major determinant both of the ageing process and of the development of age-associated diseases [3, 5–8].
Moreover, Claudio Franceschi, Tom Kirkwood, and Calogero Caruso [1, 8, 9] as well as other authors, postulate that both the ageing process and age-associated diseases are late consequences of evolutionary programming for a pro-inflammatory response mainly selected to resist infections and for a successful response to wound healing in early age, a view that has been discussed in the light of the antagonistic pleiotropy theory [1, 8, 9]. Such a theory on the evolution of aging postulates that senescence is the late deleterious effect of genes that are beneficial in early life. Evolutionary programming of the innate immune system may act via selection on these genetic traits.
Inflammaging is triggered by the first line of biological defense i.e. the innate immunity that operates by detection of a broad range of injuries inducing the activation of inflammatory responses [1, 4, 7]. The mononuclear phagocytes lineage plays a pivotal role in innate immunity that does not require clonal expansion of cell populations [10]. Moreover, several other cell types contribute to innate immunity by expressing pattern recognition receptors, namely various scavenger and Tolllike receptors [11]. These cell encoded proteins recognize ligands from damaged tissues and induce host responses by transmembrane signals that activate NF-kB and mitogen dependent protein kinase pathway [12]. Toll-like receptor activation also induces the expression of a wide variety of number of genes encoding proteins, such as cytokines, with regulatory functions upon cell activations and tissue inflammation [13].
Here I propose that the already acquired knoledge in this field may pave the way to a new chapter in the pathophysiology of autoimmunity: the auto [innate]immunity syndromes, where Inflammaging may constitute the subclinical paradigm of such a new chapter of autoimmunity.
Moreover, while the innate immunity induced Inflammaging may remain sub-clinical as a determinant of the ageing process, however, upon the presence of high responder inflammatory genotypes (pro-inflammatory cytokines versus anti-inflammatory cytokines), this auto [innate]immunity syndrome may determine or at least contribute to age-associated frailty and chronic diseases including cardiovascular diseases, Alzheimer's disease, insulin-resistance and diabetes, osteoarthritis, osteoporosis, sarcopenia. Therefore, differently from the well known chapter of conventional autoimmune diseases and syndromes where the main actor is the adaptive immunity, Inflammaging may constitute the subclinical paradigm of a new chapter of autoimmunity, namely that arising from an auto-immune inflammatory response of the innate-immune-system an old actor of immunity and yet a new actor of autoimmunity.
References
Franceschi C, Bonafe M, Valensin S, Olivieri F, De Luca M, Ottaviani E, De Benedictis G: Inflammaging. An evolutionary perspective on immunosenescence. Ann N Y Acad Sci. 2000, 908: 244-54.
Salvioli S, Capri M, Valensin S, Tieri P, Monti D, Ottaviani E, Franceschi C: Inflamm-Aging, Cytokines and Aging: State of the Art, New Hypotheses on the Role of Mitochondria and New Perspectives from Systems Biology. Current Pharmaceutical Design. 2006, 12 (24): 3161-3171.
De Martinis M, Franceschi C, Monti D, Ginaldi L: Inflamm-ageing and lifelong antigenic load as major determinants of ageing rate and longevity. FEBS Lett. 2005, 11;579 (10): 2035-9. 10.1016/j.febslet.2005.02.055.
Fagiola U, Cossarizza A, Scala E, Fanales-Belasio E, Ortolani C, Cozzi E, Monti D, Franceschi C, Paganelli R: Increased cytokine production in mononuclear cells of healthy elderly people. Eur J Immunol. 1993, 23: 2375-237.
Franceschi C, Monti D, Sansoni P, Cossarizza A: The immunology of exceptional individuals:the lesson of centenarians. Immunol Today. 1995, 16: 12-16. 10.1016/0167-5699(95)80064-6.
Lio D, Scola L, Crivello A, Colonna-Romano G, Candore G, Bonafe M, Cavallone L, Marchegiani F, Olivieri F, Franceschi C, Caruso C: Inflammation, genetics, and longevity: further studies on the protective effects in men of IL-10 -1082 promoter SNP and its interaction with TNF- -308 promoter SNP. J Med Genet. 2003, 40: 296-299. 10.1136/jmg.40.4.296.
Candore G, Colonna-Romano G, Balestrieri CR, Di Carlo D, Grimaldi MP, Listi F, Nuzzo D, Vasto S, Lio D, Caruso C: Biology of longevity: role of the innate immune system. Rejuvenation Res. 2006, 9 (1): 143-148. 10.1089/rej.2006.9.143.
Vasto S, Candore G, Balestrieri CR, Caruso M, Colonna-Romano G, Grimaldi MP, Listi F, Nuzzo D, Lio D, Caruso C: Inflammatory networks in ageing, age-related diseases and longevity. Mech Aging Dev. 2006,
Van Den Biggelaar AHJ, De Craen AJM, Gussekloo J, Huizinga J, Heijmans BT, Frölich M, Kirkwood TBL, Westendorp RGJ: Inflammation underlying cardiovascular mortality is a late consequence of evolutionary programming. The FASEB Journal. 2004, 18: 1022-1024. E. pub
Medzhitov R, Janeway C: Innate Immunity. N Engl J Med. 2000, 343: 338-344. 10.1056/NEJM200008033430506.
Krieger M: The other side of scavenger receptors pattern recognition for host defense. Curr Opin Lipidol. 1997, 8: 275-280.
Muzio M, Natoli G, Saccani S, Levrero M, Mantovani A: The human Toll signaling pathway; divergence of nuclear factor kappaB and JNK/SAPK activation upstream of tumor necrosis factor receptor-associated factor 6 (TRAF6). J Exp Med. 1998, 187: 2097-2101. 10.1084/jem.187.12.2097.
Guha M, Mackman N: LPS induction of gene expression in human monocytes. Cell Signal. 2001, 13: 85-94. 10.1016/S0898-6568(00)00149-2.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
This article is published under license to BioMed Central Ltd. This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/2.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
About this article
Cite this article
Giunta, S. Is inflammaging an auto[innate]immunity subclinical syndrome?. Immun Ageing 3, 12 (2006). https://doi.org/10.1186/1742-4933-3-12
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/1742-4933-3-12