Abstract
Elevation of the proinflammatory cytokine Interleukin-1 (IL-1) is an integral part of the local tissue reaction to central nervous system (CNS) insult. The discovery of increased IL-1 levels in patients following acute injury and in chronic neurodegenerative disease laid the foundation for two decades of research that has provided important details regarding IL-1's biology and function in the CNS. IL-1 elevation is now recognized as a critical component of the brain's patterned response to insults, termed neuroinflammation, and of leukocyte recruitment to the CNS. These processes are believed to underlie IL-1's function in the setting of acute brain injury, where it has been ascribed potential roles in repair as well as in exacerbation of damage. Explorations of IL-1's role in chronic neurodegenerative disease have mainly focused on Alzheimer disease (AD), where indirect evidence has implicated it in disease pathogenesis. However, recent observations in animal models challenge earlier assumptions that IL-1 elevation and resulting neuroinflammatory processes play a purely detrimental role in AD, and prompt a need for new characterizations of IL-1 function. Potentially adaptive functions of IL-1 elevation in AD warrant further mechanistic studies, and provide evidence that enhancement of these effects may help to alleviate the pathologic burden of disease.
Similar content being viewed by others
Introduction
Interleukin-1 (IL-1) comprises a pleiotropic cytokine family capable of numerous actions in the central nervous system (CNS). IL-1 classically refers to a 17 kilodalton (kDa) polypeptide existing in two distinct isoforms, IL-1α and IL-1β, although other members of the IL-1 family have recently been proposed [1]. Although IL-1α and IL-1β are encoded by separate genes sharing some sequence homology, they elicit similar biological actions. In addition to these two IL-1 receptor agonists, a native IL-1 receptor antagonist (IL-1ra) also maps to the IL-1 gene cluster on human chromosome two. All three proteins are produced as precursors, of which pro-IL-1α and pro-IL-1ra possess biological activity. Pro-IL-1β, however, requires cleavage by caspase-1 (IL-1β converting enzyme, ICE) to become biologically active. Details about the structure and regulation of these family members, as well as information about many of their actions can be found in recent reviews [2–4].
All known actions of IL-1 are mediated by a single biologically active 80 kDa cell surface receptor, the type I IL-1 receptor (IL-1RI) [5]. IL-1R1 is expressed throughout the rodent brain, with levels generally highest in neuronal rich areas including the dentate gyrus, the pyramidal cell layer of the hippocampus, and the hypothalamus [6, 7]. Binding of IL-1 agonists to IL-1R1 requires association with an accessory protein to elicit downstream signal transduction that includes activation of nuclear factor-kappa B (NFκB) and mitogen-activated protein (MAP) kinase pathways [8, 9]. While all known biological functions of IL-1 are attributable to IL-1 interactions with IL-1R1, some studies suggest that alternate functional IL-1 receptors may exist in the CNS [10, 11].
The evolutionary importance of IL-1 activity within the brain is highlighted by the presence of two distinct endogenous regulatory pathways. IL-1ra is a competitive antagonist of IL-1R1 that selectively binds, but fails to trigger receptor association with the accessory protein resulting in blockade of all known actions of IL-1. A second 68 kDa receptor, the type II IL-1 receptor (IL-1RII), may serve as a decoy as it binds all IL-1 ligands but lacks an intracellular domain and has no demonstrated signaling function [12]. Further description of the IL-1 regulatory pathways can be found in two recent comprehensive reviews [1, 13].
IL-1 actions within the CNS
IL-1 was the first cytokine identified with actions on the brain [14, 15]. Its ability to elicit fever after peripheral administration led to early descriptions of IL-1 as the "endogenous pyrogen". The research that followed has implicated IL-1 in a diverse array of physiologic and pathologic processes within the mammalian CNS, and has earned IL-1 status as a prototypic pro-inflammatory cytokine [13, 16, 17]. Generally speaking, the actions of IL-1 in the CNS are attributed to either responses of the neuroendocrine system or the local tissue microenvironment.
In response to homeostatic threats in mammals, increased IL-1 levels activate the hypothalamo-pituitary-adrenal (HPA) axis and are central to elicitation of sickness behaviors. The downstream effects of this neuroendocrine system stimulation likely underlie the ability of IL-1 to modulate processes such as appetite, body temperature, epilepsy, and sleep/wake cycles in mammals [16, 18–20]. This review will focus on IL-1 as a key regulator of local tissue responses to injury and disease in the CNS, with emphasis on its role in neuroinflammation.
Expression of IL-1 in injury and disease
Initial evidence that IL-1 may play a key role in local brain tissue reactions came from demonstrations of elevated IL-1 expression in a diverse array of CNS diseases. In humans, IL-1 is elevated in brain tissue and cerebrospinal fluid (CSF) from patients who succumbed to brain injury or stroke [21]. This pattern of expression was further extended to animal models of CNS injury where parenchymal IL-1 mRNA and protein levels are elevated in experimental models of ischemia, excitotoxicity, infection and traumatic brain injury in rodents. While IL-1α and IL-1β are barely detectable in either normal human or rodent brain, they are rapidly induced within minutes of acute experimental injuries [reviewed in [1, 3, 22]].
In addition to initial demonstrations of IL-1 elevations following acute injuries, similar observations have been made in a number of chronic neurodegenerative disorders. IL-1 elevations have been reported within brain lesions from patients with Alzheimer's disease (AD), Multiple Sclerosis (MS), Down's Syndrome and HIV-associated dementia [17, 23–25]. Furthermore, increased IL-1 has been detected in CSF samples in MS, Parkinson's and Creutzfeldt-Jakob disease (CJD) [26–28]. These findings have since been reproduced in corresponding animal models of disease for AD, MS and CJD [29–33].
Sources and targets of IL-1 expression
IL-1 is both expressed by and targeted to many different cell types within the CNS. Microglia express ICE, and in response to injury are thought to produce both the initial burst and highest levels of IL-1 production [34]. IL-1 can also be produced by astrocytes, endothelial cells, infiltrating leukocytes, neurons and oligodendrocytes [4, 35, 36]. In turn, IL-1 can feed back on its original cellular sources but is thought to exert its primary actions on microglia, astrocytes and endothelial cells [2].
Neuroglia and endothelial cells produce a myriad of signaling molecules in response to IL-1 stimulation. These include pro-inflammatory cytokines, chemokines, adhesion molecules, prostaglandins, reactive oxygen species, nitric oxide, and matrix metalloproteases. Notably, IL-1 induces expression of the pro-inflammatory cytokines tumor necrosis factor alpha (TNF-α) and Interleukin-6 (IL-6) as well as the enzyme cyclooxygenase-2 (COX-2) in both astrocytes and microglia in culture [4, 37, 38]. These inflammatory mediators have been implicated in the propagation of a number of CNS injuries and diseases [39].
IL-1β and neuroinflammation
Neuroinflammation is traditionally defined as the brain's innate immune response to injury. The hallmarks of a neuroinflammatory response are phenotypic glial activation and de novo production of immune signaling molecules. Both astrocytes and microglia undergo cellular hypertrophy with increased expression of cell-surface immune modulatory proteins, including those of the major histocompatibility complex (MHC). These changes are accompanied by increased synthesis and release of pro-inflammatory cytokines and chemokines.
IL-1β is intimately involved in elaboration of acute neuroinflammatory processes in vivo. Exposure of the rodent brain to IL-1β elicits rapid, robust activation of both astrocytes and microglia. In addition, single bolus injection or parenchymal expression of IL-1β in rodents increases expression of pro-inflammatory cytokines, leukocyte chemotactic chemokines, cell surface adhesion molecules, cyclooxygenases and matrix metalloproteases within the brain parenchyma [40–45]. Importantly, IL-1β is capable of triggering further increases in it's own expression as evidenced by murine IL-1β induction following human IL-1β administration or expression in the brain [45, 46]. By feeding back upon itself, small localized elevations in IL-1 may be sufficient to drive potent neuroinflammatory changes in the brain. Further evidence for a central role of IL-1 in neuroinflammation has been provided in IL-1R1 knockout mice where lack of IL-1 signaling in the setting of penetrating brain injury causes dramatic attenuation in microglial and astrocytic activation as well as IL-6 and COX-2 production [47, 48].
IL-1 and leukocyte recruitment
In addition to elaboration of a robust neuroinflammatory response in the CNS, IL-1 elevations have been implicated in trafficking of peripheral immune cells to the brain. The normal, healthy CNS has relatively few, if any leukocytes [49]. However, cellular populations within the brain can quickly change following injury. The inflammatory response that follows CNS insults such as infection or injuries caused by trauma or ischemia often features rapid infiltration of leukocytes into the brain [50–52].
IL-1β expression is a powerful stimulus for leukocyte recruitment to the CNS. Either single bolus injection or localized expression of IL-1β within the rodent brain is capable of overriding the brain's intrinsic resistance to leukocyte recruitment, resulting in rapid cellular infiltration of the parenchyma. Cell types recruited include neutrophils, CD4+ and CD8+ T-cells, dendritic cells, and cells of the monocyte lineage [40, 43, 44, 46, 53, 54]. This leukocyte infiltration is dependent on IL-1R1, and can be significantly reduced following administration of IL-1ra [44, 53, 55, 56]. The ability of IL-1β to drive enhanced expression of monocyte chemoattractant protein-1 (MCP-1; CCL2) by astrocytes and intercellular adhesion molecule-1 (ICAM-1) on vascular endothelial cells within the brain is thought to facilitate parenchymal cellular recruitment [40, 44]. Indeed, adenoviral overexpression of IL-1ra following experimental ischemia reduces ICAM-1 expression and leukocyte infiltration of the brain [57].
Neutrophils play a vital role in the innate arm of the immune response that rapidly develops at sites of injury and infection. While primarily recognized for destruction of invading pathogens, neutrophils can also shape immune responses [58]. The chemokines of the ELR+ CXC family are potent stimuli for the recruitment and activation of neutrophils in peripheral and CNS inflammatory responses, and are upregulated by acute IL-1β stimuli [59–63]. In mice, the most potent and well defined members of this family are keratinocyte-derived chemokine (KC, CXCL1) and macrophage inflammatory protein 2 (MIP-2, CXCL2) which are thought to signal exclusively through the CXCR2 receptor [50, 60, 63–65]. Interestingly, chronic IL-1β expression can serve as a long-lasting stimulus for MIP-2 and KC induction as well as neutrophil recruitment to the brain. Using a mouse model of chronic hippocampal human IL-1β overexpression, we observed neutrophil infiltration of the brain parenchyma months after initiation of transgene activation. This neutrophil recruitment appeared to be dependent on signaling through the CXCR2 receptor, as it was absent in CXCR2 knockout mice [44].
Leukocyte recruitment to the CNS is highly restricted by presence of the blood-brain barrier (BBB), which is credited for the virtual absence of leukocytes within the healthy brain parenchyma [66]. Although not thought to be necessary nor sufficient for leukocyte infiltration of the CNS, breakdown of the BBB is believed to potentiate cellular recruitment to the brain [49]. Experimentally induced elevations of IL-1β levels in the brain cause disruptions in the BBB, which may underlie its effectiveness as a leukocyte recruitment stimulus [41, 43, 44, 54]. Neutrophils have been implicated in mediating this effect based on a study in rats where administration of anti-CINC-1 (CXCL1) neutralizing antibodies attenuated neutrophil recruitment and BBB breakdown downstream of intracerebral IL-1β injections [41]. However, recent work in our laboratory indicates that IL-1β can influence BBB integrity even in the relative absence of neutrophil recruitment. More specifically, we observed significant leakage of albumin bound Evan's blue dye into the brain parenchyma of mice engineered to chronically express human IL-1β in a sustained manner, which was not altered in animals lacking the CXCR2 receptor [44]. The precise mechanisms of IL-1β mediated changes in BBB permeability remain unclear. Further studies are needed to elucidate this phenomenon, as it may be important in the pathogenesis of CNS injury and disease.
Learning, memory, and IL-1
In addition to its role in elaboration of neuroinflammation and leukocyte recruitment, local expression of IL-1 has been implicated in impairment of hippocampal dependent memory processing [67]. IL-1β activity is thought to be closely tied to the process of memory consolidation based on demonstrations of increased IL-1β expression in vitro and in vivo during long-term potentiation (LTP), a process that is believed to underlie hippocampal dependent learning and memory processes in mammals [68]. At sufficient concentrations, IL-1β is capable of blocking hippocampal LTP [69]. Also, injection of lipopolysaccharide (LPS), a potent inducer of IL-1β expression by microglia, into the rat hippocampus results in learning and memory deficits [70]. Conversely, blockade of IL-1R1 in rats using adenoviral expressed IL-1ra leads to facilitation of short and long-term memory in an inhibitory avoidance task [71]. Based on these data, it is feasible that IL-1 elevations, as occur following CNS injuries and during neurodegenerative disease, might lead to impairments in learning and memory. This may help explain the prominent memory deficits characteristic of AD and HIV-associated dementia.
The contribution of IL-1 to acute CNS injury
The elevation of IL-1 expression following a diverse array of acute brain injuries coupled with its ability to elicit diverse inflammatory changes as previously discussed, suggests that it may contribute to the pathogenesis of CNS injury. Indeed, data from head injury victims as well as in acute experimental brain injury paradigms has provided strong evidence in support of this [21]. To date most studies have focused on the CNS actions of IL-1β, rather than IL-1α, based on its more rapid induction following injury [16]. A number of studies have demonstrated that administration of IL-1β concurrent with experimental ischemia is capable of exacerbating injury [1, 72]. Conversely, ischemic damage is greatly reduced by knockout of IL-1α and IL-1β, administration of IL-1 blocking antibodies, or disruption of interleukin-1 converting enzyme function [2, 73, 74]. Interestingly, there is some evidence that IL-1 may influence ischemic injury independent of IL-1R1 [11]. In traumatic brain injury, neuronal damage is similarly reduced by administration of IL-1ra [75]. Based on the ability of exogenously administered IL-1ra to attenuate experimental ischemic injury and cross the BBB, therapy with human IL-1ra has been investigated in a Stage II clinical trial of stroke [76–78].
Increased levels of endogenous IL-1ra and IL-1RII are likely to be important mechanisms for regulation of IL-1 activity following brain injury. IL-1ra is rapidly induced following experimental injury, and blockade of endogenous production leads to exacerbation of neurotoxicity following ischemic injury in rodents [74, 79]. Increased expression of IL-1RII, the biologically inactive "decoy" IL-1 receptor, has been demonstrated following injection of IL-1β into the brain parenchyma and may also serve to limit the biological function of IL-1 [12].
In addition to data implicating IL-1 in exacerbation of acute injury, other studies have provided evidence for beneficial effects of IL-1 signaling within the brain. IL-1 has been associated with neuroprotective mechanisms in rodent primary neuron cultures which may be mediated in part by production of survival signals such as nerve growth factor (NGF) [80–82]. IL-1 signaling has also been implicated in re-myelination of the CNS after cuprizone demyelination injury, which may be due in part to IL-1 mediated stimulation of oligodendrocyte proliferation [35, 83]. Finally, absence of IL-1R1 has been associated with deficiencies in hippocampal dependent spatial learning but it is unclear if this is a result of specific beneficial influences of IL-1 on the intact nervous system or represents developmental alterations in the knockout mouse [84].
Mechanisms of IL-1 induced neuronal damage
Due to its pleiotropic actions in the brain it has been difficult to pinpoint the mechanisms by which IL-1 exacerbates acute CNS injuries. In general, it does not appear that IL-1β is capable of triggering direct neurotoxicity when administered to the healthy adult rodent brain [16]. For example, chronic hippocampal overexpression of human IL-1β in mice does not engender overt neurotoxicity or changes in measures of neuronal integrity [44]. In rats, IL-1β induced neurotoxicity has been reported following single bolus injection or adenoviral mediated expression of IL-1β in the substantia nigra or hippocampus, respectively [46, 85, 86]. However, these studies in rats may have been confounded by tissue injury resulting from parenchymal injections, viral induced inflammation, or the use of non-physiologic doses of IL-1β. It is also possible that the capacity of IL-1β to mediate direct neurotoxicity may be a species-specific phenomenon. In vitro, IL-1β exposure does not affect the viability of pure mouse or rat neuronal cultures and can reduce excitotoxin induced neurotoxicity [81, 82]. However, in rat mixed glial/neuronal cultures IL-1β has been reported to cause neurotoxicity through downstream free radical release [87].
Neutrophils have emerged as possible perpetrators of neuronal damage following acute brain insults downstream of IL-1β elevations [40, 41, 43, 53]. Neutrophils are rapidly recruited following CNS injury, present at the time of neuronal death, and can trigger tissue damage through generation of toxic free radicals, proteolytic enzymes and pro-inflammatory cytokines such as IL-1β and TNF-α [52]. In vitro, co-cultures of rat neutrophils and primary hippocampal neurons demonstrate neurotoxicity in the absence of physiologic insults as well as exacerbation of kainic acid excitotoxicity [88]. In vivo, constitutive CNS overexpression of the chemokine KC results in striking recruitment of neutrophils to multiple brain regions and early neurological demise [89]. Depleting neutrophils or limiting their infiltration through ICAM-1 gene ablation attenuates experimental ischemic injury [52, 90]. Despite these observations, recruitment of neutrophils does not appear to be sufficient for neurotoxicity. This point is supported by recent work from our laboratory where no evidence of overt neurotoxicity, synaptic damage, or loss of acetylcholine fibers was observed after 2 weeks or 2 months of sustained IL-1β induced neuroinflammation accompanied by prominent neutrophil infiltrates [44]. However, this study was limited to neuroinflammation in the dentate gyrus in the absence of concomitant injury, and it is possible that neurons in other brain regions may be more susceptible to neutrophil-mediated effects.
Neuroinflammation and AD
Neuroinflammation is now recognized as a fundamental response of the CNS not only to acute injury, but also to chronic neurodegenerative disease. This is perhaps no better demonstrated than in AD, where the severity of the neuroinflammatory response parallels the disease course [91, 92]. Neuroinflammation can be considered part of a characteristic pathologic triad of AD that includes amyloid plaques and neurofibrillary tangles. The neuroinflammatory phenotype in AD is characterized by robust activation of microglia and astrocytes in the vicinity of plaques, endogenous expression of pro-inflammatory cytokines, cell adhesion molecules, and chemokines [17, 93–96]. These changes are thought to result from glial reaction to events related to ongoing deposition of amyloid β (Aβ) [97–99].
Epidemiological studies of nonsteroidal anti-inflammatory drug (NSAID) users lent credence to initial hypotheses as to the role of neuroinflammation in AD. Early observations among identical twins discordant for AD onset showing that those receiving anti-inflammatory therapy had delays in disease onset provided strong evidence for a detrimental role of neuroinflammation in AD pathogenesis [100]. Soon thereafter, additional case-based and longitudinal epidemiologic studies confirmed these findings, and demonstrated substantial reductions in disease incidence among patients on long-term regimens of NSAIDs [101–103]. In fact, recent meta-analysis has revealed as much as a 50% reduction in the risk of acquiring disease among chronic NSAID users [104]. This data led to a surge of research activity directed at elucidating the role of inflammation in AD and other chronic neurodegenerative disorders in hopes of designing new effective anti-inflammatory therapies for disease.
Unfortunately, clinical trials of traditional anti-inflammatory agents for treatment of patients with AD have failed to demonstrate efficacy [105–110]. Also, the only trial designed to directly address the hypothesis that chronic NSAID use can prevent AD in cognitively normal subjects failed to demonstrate a protective effect [111]. Drawing conclusions from these studies is complicated by the selection and dose of NSAIDs used, length of trials and overall designs [112]. Furthermore, the patient populations in these trials differ from their epidemiologic counterparts as patients in the latter were being treated with NSAIDs for inflammatory disorders which may have modified their risk of acquiring AD. Overall, the stark contrast between these results and the early epidemiological studies of chronic NSAID users suggests a complex role for neuroinflammation in AD.
Transgenic mouse models of AD harboring familial amyloid precursor protein (APP) mutations have recapitulated in part the intimate relationships between neuroinflammation and disease pathogenesis. In APPV717F mice astrocyte activation was evident before plaques were detected, and in the Tg2576 mouse model increased microglial density was observed in regions of Aβ deposits [113, 114]. Similar neuroinflammatory changes have been observed in other murine models of AD, including the APP/PS1 double transgenic and APP/PS1/Tau triple transgenic (3xTg-AD) mice [115–117]. Finally, NSAID administration reduced both plaque pathology and neuroinflammatory measures in the Tg2576 mice [32].
Possible roles for IL-1 in AD
IL-1 elevations became closely tied to AD pathogenesis soon after the discovery of prominent neuroinflammation in AD brain. Increased IL-1 expression in reactive microglia surrounding amyloid plaques provided the initial indication that IL-1 may be associated with AD pathogenesis [17]. Since that time, IL-1β elevations have been detected in the brains of aged AD mouse models and plaque associated microglia [31, 32]. Microglial IL-1 activity was later tied to the evolution of plaques in AD [118]. In Down's syndrome, where patients are predisposed to AD neuropathological changes, IL-1 elevation and neuroinflammation precede by years the formation of plaques [119]. Additionally, specific polymorphisms in the IL-1α and IL-1β genetic loci were shown to be associated with increased disease risk in certain patient populations [reviewed in [120, 121]]. These associations, in addition to observations of IL-1 elevations in AD patients, provided the key evidence for a central role of IL-1 in disease pathogenesis. However, recent meta-analysis has not supported a clear association between IL-1 genetic loci and AD when the data is examined as a whole [122].
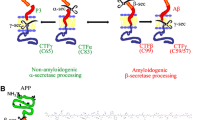
IL-1 has been implicated in both the initiation and propagation of neuroinflammatory changes seen in AD through several lines of indirect evidence [reviewed in [39, 123]]. Obviously, the known ability of IL-1 to drive robust neuroinflammatory changes in the acute setting adds to its attractiveness as a prime candidate for these actions. In AD, neuronal injury or insults including amyloid deposition may trigger a self-propagating cytokine cycle, which when chronically induced initiates a vicious feedback loop of continuing IL-1β elevation promoting further neuronal and synaptic dysfunction and Aβ plaque accumulation [99]. In support of this idea, cultured human monocytes and mouse microglia produce IL-1β in response to Aβ exposure or, to a greater extent, to secreted fragments of β-APP [124, 125]. In other tissue culture studies IL-1 has been shown to increase β-APP mRNA expression, translation, and processing perhaps through enhanced gamma secretase activity [126–130]. In addition, IL-1β injection into rat brain results in elevation of β-APP [131]. Furthermore, IL-1ra knockout mice demonstrate enhanced human amyloid-beta induced neuropathology, suggesting the unopposed action of IL-1 as a likely culprit [132]. Although these findings are largely in vitro based, correlations in Alzheimer and control patients support the idea that these basic mechanisms occur in the disease itself.
In addition to association with modulation of β-APP processing, IL-1 activity has been tied to exacerbation of neurofibrillary tangles. Implantation of slow release IL-1β pellets in rats led to microglial activation and MAPK-p38-mediated hyperphosphorylation of tau protein, which is thought to contribute to microtubule destabilization and ultimately to formation of neurofibrillary tangles [133, 134]. Analogous studies have been reported in cortical neuron cultures [135]. Microglial activation may be responsible for these effects as suggested by a recent study of synapse loss in a mouse tauopathy model [136]. Further support for IL-1β mediated activation of microglia and resultant tau hyperphosphorylation has been indirectly provided in the 3xTg-AD mouse model which expresses human mutated forms of tau, presenilin-1 and APP, and is characterized by both Aβ and tau pathology. Intraperitoneal LPS injections elicited significant IL-1β induction, microglial activation and accelerated the time course of tau hyperphosphorylation. Interestingly, LPS activity did not affect APP processing or Aβ deposition [137].
A beneficial role for neuroinflammation in AD
While epidemiologic and experimental studies lend strong support for neuroinflammatory responses as drivers of AD pathogenesis, recent work also supports a beneficial role for such reactions [reviewed in [98]]. A number of reports have provided evidence that activation of microglia and their subsequent degradation of amyloid plaques may underlie this phenomenon. Direct injection of LPS into the CNS, which drives IL-1β synthesis and robust microglial activation, yields reductions of Aβ levels and plaque load [138–140]. Microglial activation has also been suggested to underlie enhanced plaque clearance in other transgenic AD models following treatment with either a modified nitric oxide-releasing NSAID (NCX-2216) or transforming growth factor beta overexpression (TGF-β) [141, 142]. Conversely, inhibition of microglial activation with minocycline can increase Aβ deposition [143]. Although these reports and others suggest a beneficial role of microglial activation in mouse models of AD, it is worth noting that LPS stimulated neuroinflammation has also been associated with increased Aβ deposition [144, 145].
Microglial activation is thought to reduce plaque burden through phagocytosis of Aβ peptides. There is substantial evidence for plaque associated microglia as phagocytosing scavengers of amyloid in vivo [146]. Indeed, the efficacy of antibody-mediated plaque clearance in AD mouse models appears in part to be mediated by enhanced phagocytosis by microglia [147, 148]. In support of this, interference with microglial activation during Aβ immunotherapy reduced clearance of fibrillar deposits [149].
Infiltration of peripheral immune cells into sites of pathology, though not reported in AD itself, may enhance the beneficial effects of microglial mediated plaque clearance. It has been convincingly demonstrated, using green fluorescent protein (GFP) expressing bone marrow transplants in AD mouse models, that a proportion of activated microglia adjacent to amyloid plaques are in fact recruited from bone marrow-derived myeloid populations [150, 151]. LPS administration enhances the seeding of bone marrow-derived myeloid cells in the brain which may in part explain its ability to enhance amyloid plaque clearance [150]. Selective elimination of bone marrow-derived myeloid cells exacerbates plaque pathology in AD models, and providing strong evidence that this microglial sub-population is efficient at degrading plaque [151, 152]. Interestingly, an infiltrative cell type with dendritic cell-like characteristics appears to be particularly important in this process [153]. Taken altogether, these results suggest that the beneficial effects of neuroinflammation may in part result from increased recruitment of bone marrow-derived cells to the brain.
A new view of IL-1's role in AD?
Since the original observations of IL-1 elevation in AD two decades ago, a body of evidence has implicated this proinflammatory cytokine as contributing to the pathogenic processes characteristic of disease. Much of this data has relied on indirect evidence and extrapolation from studies in tissue culture and acute injury paradigms. As is the case for neuroinflammation, contemporary studies in animal models of AD are challenging our original assumptions as to the role of IL-1 in AD.
Substantial support for an adaptive role of IL-1 elevation comes from a model developed in our laboratory to specifically address the function of chronic IL-1 driven neuroinflammation in AD pathology. When IL-1β was chronically overexpressed in the hippocampus of APP/PS1 transgenic animals, we witnessed a surprising reduction in both plaque pathology and insoluble amyloid peptide without evidence of effects on Aβ processing or APP expression. There was also a striking increase in numbers of plaque associated myeloid cells, suggesting enhanced phagocytosis of Aβ by microglia or infiltrating myeloid cells [45]. A limitation of this study is the use of a heterologous APP promoter, as this does not allow for interplay between inflammation and the APP promoter as discussed earlier. However, IL-1β overexpression was not associated with increased levels of murine APP mRNA [45].
The initial stimulus for elevation of IL-1 in AD is likely the result of exposure of microglia to injured neurons, β-APP, and its cleavage product Aβ as has been demonstrated both in vitro and in vivo [125, 151]. Microglia chronically exposed to these stimuli during the course of disease likely mount sustained elevations in IL-1 and drive a self-perpetuating cycle of IL-1 overexpression in the brain parenchyma leading to chronic neuroinflammation [45]. As highlighted above, IL-1 elevation may potentiate plaque degradation by enhancing microglial activation and phagocytic activity, as well as seeding of peripheral phagocytic cells to areas of plaque deposition [44]. Despite this evidence pointing toward an important function of IL-1 in AD pathogenesis, a recent study in the Tg2576 AD mouse model failed to detect any influence of IL-1R1 knockout on either Aβ deposition or the efficacy of passive immunotherapy [154]. However, these results must be interpreted with caution as IL-1R1 knockout animals may be affected by compensatory changes during development.
At the present time our understanding of the relationship between neuroinflammation, IL-1, and AD is evolving. The downstream consequences of IL-1 elevation in AD likely involve a balance between the beneficial and detrimental functions highlighted in this review (Figure 1). Failures of recent anti-inflammatory trials in the treatment of AD may be in part explained by blockade of both beneficial and detrimental neuroinflammatory processes in the course of disease. Current findings are consistent with the idea that strategies aimed at enhancing beneficial components of neuroinflammatory pathways in chronic neurodegenerative disease may hold promise in the development of new therapies.
Conclusion
This review highlights recent scientific studies of IL-1 activity in neuroinflammation and AD, and paints a complex picture of IL-1 function in the local tissue response of the brain to injury and disease. A clearer understanding of IL-1's role is unfolding, yielding observations of both helpful and harmful effects in experimental paradigms. This is particularly true in regard to the pathogenesis of AD, where recent observations urge a reexamination of original assumptions as to the role of IL-1 in disease. This emerging understanding of IL-1's contribution to the pathogenesis of CNS insults has identified possible roles in triggering adaptive innate immune processes during the course of chronic neurodegenerative disease. IL-1 can no longer be regarded as simply the villain in the setting of brain injury and disease, but instead might be understood as a factor that can influence the balance between beneficial and detrimental outcomes. Potentiation of such adaptive IL-1 driven responses in chronic neurodegenerative disease may provide new avenues for therapeutic intervention.
References
Allan SM, Tyrrell PJ, Rothwell NJ: Interleukin-1 and neuronal injury. Nature reviews. 2005, 5 (8): 629-640. 10.1038/nri1664.
Gibson RM, Rothwell NJ, Le Feuvre RA: CNS injury: the role of the cytokine IL-1. Vet J. 2004, 168 (3): 230-237. 10.1016/j.tvjl.2003.10.016.
Patel HC, Boutin H, Allan SM: Interleukin-1 in the brain: mechanisms of action in acute neurodegeneration. Ann N Y Acad Sci. 2003, 992: 39-47.
Basu A, Krady JK, Levison SW: Interleukin-1: a master regulator of neuroinflammation. J Neurosci Res. 2004, 78 (2): 151-156. 10.1002/jnr.20266.
Glaccum MB, Stocking KL, Charrier K, Smith JL, Willis CR, Maliszewski C, Livingston DJ, Peschon JJ, Morrissey PJ: Phenotypic and functional characterization of mice that lack the type I receptor for IL-1. J Immunol. 1997, 159 (7): 3364-3371.
Farrar W, Kilian P, Ruff M, Hill J, Pert C: Visualization and characterization of interleukin-1 receptors in brain. J Immunol. 1987, 139: 459-463.
Cunningham ET, Wada E, Carter DB, Tracey DE, Battey JF, De Souza EB: In situ histochemical localization of type 1 interleukin-1 receptor messenger RNA in the central nervous system, pituitary, and adrenal gland of the mouse. J Neurosci. 1993, 12 (3): 1101-1114.
Muzio M, Ni J, Feng P, Dixit VM: IRAK (Pelle) family member IRAK-2 and MyD88 as proximal mediators of IL-1 signaling. Science. 1997, 278 (Nov 28, 1997): 1612-1615. 10.1126/science.278.5343.1612.
Malinin NL, Boldin MP, Kovalendo AV, Wallach D: MAP3K-related kinase involved in NF-kB induction by TNF, CD95 and IL-1. Nature. 1997, 385 (Feb 06, 1997): 540-544. 10.1038/385540a0.
Andre R, Moggs JG, Kimber I, Rothwell NJ, Pinteaux E: Gene regulation by IL-1beta independent of IL-1R1 in the mouse brain. Glia. 2006, 53 (5): 477-483. 10.1002/glia.20302.
Touzani O, Boutin H, LeFeuvre R, Parker L, Miller A, Luheshi G, Rothwell N: Interleukin-1 influences ischemic brain damage in the mouse independently of the interleukin-1 type I receptor. J Neurosci. 2002, 22 (1): 38-43.
Docagne F, Campbell SJ, Bristow AF, Poole S, Vigues S, Guaza C, Perry VH, Anthony DC: Differential regulation of type I and type II interleukin-1 receptors in focal brain inflammation. Eur J Neurosci. 2005, 21 (5): 1205-1214. 10.1111/j.1460-9568.2005.03965.x.
Gosselin D, Rivest S: Role of IL-1 and TNF in the brain: twenty years of progress on a Dr. Jekyll/Mr. Hyde duality of the innate immune system. Brain Behav Immun. 2007, 21 (3): 281-289. 10.1016/j.bbi.2006.12.004.
Berkenbosch F, van Oers J, del Rey A, Tilders F, Besedovsky H: Corticotropin-releasing factor-producing neurons in the rat activated by interleukin-1. Science. 1987, 238 (4826): 524-526. 10.1126/science.2443979.
Besedovsky H, del Rey A, Sorkin E, Dinarello CA: Immunoregulatory feedback between interleukin-1 and glucocorticoid hormones. Science. 1986, 233 (4764): 652-654. 10.1126/science.3014662.
Rothwell N: Interleukin-1 and neuronal injury: mechanisms, modification, and therapeutic potential. Brain Behav Immun. 2003, 17 (3): 152-157. 10.1016/S0889-1591(02)00098-3.
Griffin WS, Stanley LC, Ling C, White L, MacLeod V, Perrot LJ, White CL, Araoz C: Brain interleukin 1 and S-100 immunoreactivity are elevated in Down syndrome and Alzheimer disease. Proc Natl Acad Sci USA. 1989, 86 (19): 7611-7615. 10.1073/pnas.86.19.7611.
Dunn AJ: Cytokine activation of the HPA axis. Ann N Y Acad Sci. 2000, 917 (1): 608-617.
Dube C, Vezzani A, Behrens M, Bartfai T, Baram TZ: Interleukin-1beta contributes to the generation of experimental febrile seizures. Ann Neurol. 2005, 57 (1): 152-155. 10.1002/ana.20358.
Sheng JG, Boop FA, Mrak RE, Griffin WS: Increased neuronal beta-amyloid precursor protein expression in human temporal lobe epilepsy: association with interleukin-1 alpha immunoreactivity. J Neurochem. 1994, 63 (5): 1872-1879.
Griffin WS, Sheng JG, Gentleman SM, Graham DI, Mrak RE, Roberts GW: Microglial interleukin-1 alpha expression in human head injury: correlations with neuronal and neuritic beta-amyloid precursor protein expression. Neurosci Lett. 1994, 176 (2): 133-136. 10.1016/0304-3940(94)90066-3.
Sheng JG, Griffin WS, Royston MC, Mrak RE: Distribution of interleukin-1-immunoreactive microglia in cerebral cortical layers: implications for neuritic plaque formation in Alzheimer's disease. Neuropathol Appl Neurobiol. 1998, 24 (4): 278-283. 10.1046/j.1365-2990.1998.00122.x.
McGuinness MC, Powers JM, Bias WB, Schmeckpeper BJ, Segal AH, Gowda VC, Wesselingh SL, Berger J, Griffin DE, Smith KD: Human leukocyte antigens and cytokine expression in cerebral inflammatory demyelinative lesions of X-linked adrenoleukodystrophy and multiple sclerosis. J Neuroimmunol. 1997, 75 (1-2): 174-182. 10.1016/S0165-5728(97)00020-9.
Zhao ML, Kim MO, Morgello S, Lee SC: Expression of inducible nitric oxide synthase, interleukin-1 and caspase-1 in HIV-1 encephalitis. J Neuroimmunol. 2001, 115 (1-2): 182-191. 10.1016/S0165-5728(00)00463-X.
Stanley LC, Mrak RE, Woody RC, Perrot LJ, Zhang S, Marshak DR, Nelson SJ, Griffin WS: Glial cytokines as neuropathogenic factors in HIV infection: pathogenic similarities to Alzheimer's disease. J Neuropathol Exp Neurol. 1994, 53 (3): 231-238.
Van Everbroeck B, Dewulf E, Pals P, Lubke U, Martin JJ, Cras P: The role of cytokines, astrocytes, microglia and apoptosis in Creutzfeldt-Jakob disease. Neurobiol Aging. 2002, 23 (1): 59-64. 10.1016/S0197-4580(01)00236-6.
Mogi M, Harada M, Narabayashi H, Inagaki H, Minami M, Nagatsu T: Interleukin (IL)-1 beta, IL-2, IL-4, IL-6 and transforming growth factor-alpha levels are elevated in ventricular cerebrospinal fluid in juvenile parkinsonism and Parkinson's disease. Neurosci Lett. 1996, 211 (1): 13-16. 10.1016/0304-3940(96)12706-3.
Hauser SL, Doolittle TH, Lincoln R, Brown RH, Dinarello CA: Cytokine accumulations in CSF of multiple sclerosis patients: frequent detection of interleukin-1 and tumor necrosis factor but not interleukin-6. Neurology. 1990, 40 (11): 1735-1739.
Kennedy MK, Torrance DS, Picha KS, Mohler KM: Analysis of cytokine mRNA expression in the central nervous system of mice with experimental autoimmune encephalomyelitis reveals that IL-10 mRNA expression correlates with recovery. J Immunol. 1992, 149 (7): 2496-2505.
Kordek R, Liberski PP, Yanagihara R, Isaacson S, Gajdusek DC: Molecular analysis of prion protein (PrP) and glial fibrillary acidic protein (GFAP) transcripts in experimental Creutzfeldt-Jakob disease in mice. Acta Neurobiol Exp (Wars). 1997, 57 (2): 85-90.
Benzing WC, Wujek JR, Ward EK, Shaffer D, Ashe KH, Younkin SG, Brunden KR: Evidence for glial-mediated inflammation in aged APP(SW) transgenic mice. Neurobiol Aging. 1999, 20 (6): 581-589. 10.1016/S0197-4580(99)00065-2.
Lim GP, Yang F, Chu T, Chen P, Beech W, Teter B, Tran T, Ubeda O, Ashe KH, Frautschy SA, Cole GM: Ibuprofen suppresses plaque pathology and inflammation in a mouse model for Alzheimer's disease. J Neurosci. 2000, 20 (15): 5709-5714.
Bauer J, Berkenbosch F, Van Dam AM, Dijkstra CD: Demonstration of interleukin-1 beta in Lewis rat brain during experimental allergic encephalomyelitis by immunocytochemistry at the light and ultrastructural level. J Neuroimmunol. 1993, 48 (1): 13-21. 10.1016/0165-5728(93)90053-2.
Eriksson C, Van Dam AM, Lucassen PJ, Bol JG, Winblad B, Schultzberg M: Immunohistochemical localization of interleukin-1beta, interleukin-1 receptor antagonist and interleukin-1beta converting enzyme/caspase-1 in the rat brain after peripheral administration of kainic acid. Neuroscience. 1999, 93 (3): 915-930. 10.1016/S0306-4522(99)00178-5.
Vela JM, Molina-Holgado E, Arevalo-Martin A, Almazan G, Guaza C: Interleukin-1 regulates proliferation and differentiation of oligodendrocyte progenitor cells. Mol Cell Neurosci. 2002, 20 (3): 489-502. 10.1006/mcne.2002.1127.
Higgins GA, Olschowka JA: Induction of interleukin-1 beta mRNA in adult rat brain. Brain Res Mol Brain Res. 1991, 9 (1-2): 143-148. 10.1016/0169-328X(91)90139-O.
O'Banion MK, Miller JC, Chang JW, Kaplan MD, Coleman PD: Interleukin-1 beta induces prostaglandin G/H synthase-2 (cyclooxygenase-2) in primary murine astrocyte cultures. J Neurochem. 1996, 66 (6): 2532-2540.
Chao CC, Hu S, Sheng WS, Bu D, Bukrinsky MI, Peterson PK: Cytokine-stimulated astrocytes damage human neurons via a nitric oxide mechanism. Glia. 1996, 16 (3): 276-284. 10.1002/(SICI)1098-1136(199603)16:3<276::AID-GLIA10>3.0.CO;2-X.
Mrak RE, Griffin WS: Glia and their cytokines in progression of neurodegeneration. Neurobiol Aging. 2005, 26 (3): 349-354. 10.1016/j.neurobiolaging.2004.05.010.
Proescholdt MG, Chakravarty S, Foster JA, Foti SB, Briley EM, Herkenham M: Intracerebroventricular but not intravenous interleukin-1beta induces widespread vascular-mediated leukocyte infiltration and immune signal mRNA expression followed by brain-wide glial activation. Neuroscience. 2002, 112 (3): 731-749. 10.1016/S0306-4522(02)00048-9.
Anthony D, Dempster R, Fearn S, Clements J, Wells G, Perry VH, Walker K: CXC chemokines generate age-related increases in neutrophil-mediated brain inflammation and blood-brain barrier breakdown. Curr Biol. 1998, 8 (16): 923-926. 10.1016/S0960-9822(07)00373-9.
Moore AH, Olschowka JA, O'Banion MK: Intraparenchymal administration of interleukin-1beta induces cyclooxygenase-2-mediated expression of membrane- and cytosolic-associated prostaglandin E synthases in mouse brain. J Neuroimmunol. 2004, 148 (1-2): 32-40. 10.1016/j.jneuroim.2003.11.001.
Ferrari CC, Depino AM, Prada F, Muraro N, Campbell S, Podhajcer O, Perry VH, Anthony DC, Pitossi FJ: Reversible demyelination, blood-brain barrier breakdown, and pronounced neutrophil recruitment induced by chronic IL-1 expression in the brain. Am J Pathol. 2004, 165 (5): 1827-1837.
Shaftel SS, Carlson TJ, Olschowka JA, Kyrkanides S, Matousek SB, O'Banion MK: Chronic interleukin-1beta expression in mouse brain leads to leukocyte infiltration and neutrophil-independent blood brain barrier permeability without overt neurodegeneration. J Neurosci. 2007, 27 (35): 9301-9309. 10.1523/JNEUROSCI.1418-07.2007.
Shaftel SS, Kyrkanides S, Olschowka JA, Miller JN, Johnson RE, O'Banion MK: Sustained hippocampal IL-1 beta overexpression mediates chronic neuroinflammation and ameliorates Alzheimer plaque pathology. J Clin Invest. 2007, 117 (6): 1595-1604. 10.1172/JCI31450.
Depino A, Ferrari C, Pott Godoy MC, Tarelli R, Pitossi FJ: Differential effects of interleukin-1beta on neurotoxicity, cytokine induction and glial reaction in specific brain regions. J Neuroimmunol. 2005, 168 (1-2): 96-110. 10.1016/j.jneuroim.2005.07.009.
Basu A, Krady JK, O'Malley M, Styren SD, DeKosky ST, Levison SW: The type 1 interleukin-1 receptor is essential for the efficient activation of microglia and the induction of multiple proinflammatory mediators in response to brain Injury. J Neurosci. 2002, 22 (14): 6071-6082.
Lin HW, Basu A, Druckman C, Cicchese M, Krady JK, Levison SW: Astrogliosis is delayed in type 1 interleukin-1 receptor-null mice following a penetrating brain injury. J Neuroinflammation. 2006, 3: 15-10.1186/1742-2094-3-15.
Ransohoff RM, Kivisakk P, Kidd G: Three or more routes for leukocyte migration into the central nervous system. Nat Rev Immunol. 2003, 3 (7): 569-581. 10.1038/nri1130.
Del Rio L, Bennouna S, Salinas J, Denkers EY: CXCR2 deficiency confers impaired neutrophil recruitment and increased susceptibility during Toxoplasma gondii infection. J Immunol. 2001, 167 (11): 6503-6509.
Morganti-Kossmann MC, Rancan M, Stahel PF, Kossmann T: Inflammatory response in acute traumatic brain injury: a double-edged sword. Current opinion in critical care. 2002, 8 (2): 101-105. 10.1097/00075198-200204000-00002.
Emerich DF, Dean RL, Bartus RT: The role of leukocytes following cerebral ischemia: pathogenic variable or bystander reaction to emerging infarct?. Exp Neurol. 2002, 173 (1): 168-181. 10.1006/exnr.2001.7835.
Ching S, He L, Lai W, Quan N: IL-1 type I receptor plays a key role in mediating the recruitment of leukocytes into the central nervous system. Brain Behav Immun. 2005, 19 (2): 127-137. 10.1016/j.bbi.2004.06.001.
Anthony DC, Bolton SJ, Fearn S, Perry VH: Age-related effects of interleukin-1 beta on polymorphonuclear neutrophil-dependent increases in blood-brain barrier permeability in rats. Brain. 1997, 120: 435-444. 10.1093/brain/120.3.435.
Yang GY, Liu XH, Kadoya C, Zhao YJ, Mao Y, Davidson BL, Betz AL: Attenuation of ischemic inflammatory response in mouse brain using an adenoviral vector to induce overexpression of interleukin-1 receptor antagonist. J Cereb Blood Flow Metab. 1998, 18 (8): 840-847. 10.1097/00004647-199808000-00004.
Garcia JH, Liu KF, Relton JK: Interleukin-1 receptor antagonist decreases the number of necrotic neurons in rats with middle cerebral artery occlusion. The American journal of pathology. 1995, 147 (5): 1477-1486.
Yang GY, Mao Y, Zhou LF, Gong C, Ge HL, Betz AL: Expression of intercellular adhesion molecule 1 (ICAM-1) is reduced in permanent focal cerebral ischemic mouse brain using an adenoviral vector to induce overexpression of interleukin-1 receptor antagonist. Brain research. 1999, 65 (2): 143-150. 10.1016/S0169-328X(98)00335-0.
Nathan C: Neutrophils and immunity: challenges and opportunities. Nature reviews. 2006, 6 (3): 173-182. 10.1038/nri1785.
Lee J, Cacalano G, Camerato T, Toy K, Moore MW, Wood WI: Chemokine binding and activities mediated by the mouse IL-8 receptor. J Immunol. 1995, 155 (4): 2158-2164.
Tateda K, Moore TA, Newstead MW, Tsai WC, Zeng X, Deng JC, Chen G, Reddy R, Yamaguchi K, Standiford TJ: Chemokine-dependent neutrophil recruitment in a murine model of Legionella pneumonia: potential role of neutrophils as immunoregulatory cells. Infect Immun. 2001, 69 (4): 2017-2024. 10.1128/IAI.69.4.2017-2024.2001.
Bell MD, Taub DD, Perry VH: Overriding the brain's intrinsic resistance to leukocyte recruitment with intraparenchymal injections of recombinant chemokines. Neuroscience. 1996, 74 (1): 283-292. 10.1016/0306-4522(96)00083-8.
Lappalainen U, Whitsett JA, Wert SE, Tichelaar JW, Bry K: Interleukin-1beta causes pulmonary inflammation, emphysema, and airway remodeling in the adult murine lung. Am J Respir Cell Mol Biol. 2005, 32 (4): 311-318. 10.1165/rcmb.2004-0309OC.
Mehrad B, Strieter RM, Moore TA, Tsai WC, Lira SA, Standiford TJ: CXC chemokine receptor-2 ligands are necessary components of neutrophil-mediated host defense in invasive pulmonary aspergillosis. J Immunol. 1999, 163 (11): 6086-6094.
Tessier PA, Naccache PH, Clark-Lewis I, Gladue RP, Neote KS, McColl SR: Chemokine networks in vivo: involvement of C-X-C and C-C chemokines in neutrophil extravasation in vivo in response to TNF-alpha. J Immunol. 1997, 159 (7): 3595-3602.
Kielian T, Barry B, Hickey WF: CXC chemokine receptor-2 ligands are required for neutrophil-mediated host defense in experimental brain abscesses. J Immunol. 2001, 166 (7): 4634-4643.
Carson MJ, Doose JM, Melchior B, Schmid CD, Ploix CC: CNS immune privilege: hiding in plain sight. Immunol Rev. 2006, 213: 48-65. 10.1111/j.1600-065X.2006.00441.x.
Pugh RC, Fleshner M, Watkins LR, Maier SF, Rudy JW: The immune system and memory consolidation: a role for the cytokine IL-1beta. Neurosci Biobehav Rev. 2001, 25 (1): 29-41. 10.1016/S0149-7634(00)00048-8.
Schneider H, Pitossi F, Balschun D, Wagner A, del Rey A, Besedovsky HO: A neuromodulatory role of interleukin-1beta in the hippocampus. Proc Natl Acad Sci USA. 1998, 95 (13): 7778-7783. 10.1073/pnas.95.13.7778.
O'Connor JJ, Coogan AN: Actions of the pro-inflammatory cytokine IL-1 beta on central synaptic transmission. Exp Physiol. 1999, 84 (4): 601-614. 10.1017/S0958067099018928.
Tanaka S, Ide M, Shibutani T, Ohtaki H, Numazawa S, Shioda S, Yoshida T: Lipopolysaccharide-induced microglial activation induces learning and memory deficits without neuronal cell death in rats. J Neurosci Res. 2006, 83 (4): 557-566. 10.1002/jnr.20752.
Depino AM, Alonso M, Ferrari C, del Rey A, Anthony D, Besedovsky H, Medina JH, Pitossi F: Learning modulation by endogenous hippocampal IL-1: blockade of endogenous IL-1 facilitates memory formation. Hippocampus. 2004, 14 (4): 526-535. 10.1002/hipo.10164.
Stroemer RP, Rothwell NJ: Exacerbation of ischemic brain damage by localized striatal injection of interleukin-1ß in the rat. J Cereb Blood Flow Metab. 1998, 18 (8): 833-839. 10.1097/00004647-199808000-00003.
Boutin H, LeFeuvre RA, Horai R, Asano M, Iwakura Y, Rothwell NJ: Role of IL-1alpha and IL-1beta in ischemic brain damage. J Neurosci. 2001, 21 (15): 5528-5534.
Loddick SA, Wong ML, Bongiorno PB, Gold PW, Licinio J, Rothwell NJ: Endogenous interleukin-1 receptor antagonist is neuroprotective. Biochem Biophys Res Commun. 1997, 234 (1): 211-215. 10.1006/bbrc.1997.6436.
Toulmond S, Rothwell NJ: Interleukin-1 receptor antagonist inhibits neuronal damage caused by fluid percussion injury in the rat. Brain Res. 1995, 671: 261-266. 10.1016/0006-8993(94)01343-G.
Clark SR, McMahon CJ, Gueorguieva I, Rowland M, Scarth S, Georgiou R, Tyrrell PJ, Hopkins SJ, Rothwell NJ: Interleukin-1 receptor antagonist penetrates human brain at experimentally therapeutic concentrations. J Cereb Blood Flow Metab. 2007
Emsley HC, Smith CJ, Georgiou RF, Vail A, Hopkins SJ, Rothwell NJ, Tyrrell PJ: A randomised phase II study of interleukin-1 receptor antagonist in acute stroke patients. J Neurol Neurosurg Psychiatry. 2005, 76 (10): 1366-1372. 10.1136/jnnp.2004.054882.
Gueorguieva I, Clark SR, McMahon CJ, Scarth S, Rothwell NJ, Tyrell PJ, Hopkins SJ, Rowland M: Pharmacokinetic modelling of interleukin-1 receptor antagonist in plasma and cerebrospinal fluid of patients following subarachnoid haemorrhage. Br J Clin Pharmacol. 2008, 65 (3): 317-325. 10.1111/j.1365-2125.2007.03026.x. Epub 2007 Sep 13.
Pinteaux E, Rothwell NJ, Boutin H: Neuroprotective actions of endogenous interleukin-1 receptor antagonist (IL-1ra) are mediated by glia. Glia. 2006, 53 (5): 551-556. 10.1002/glia.20308.
Juric DM, Carman-Krzan M: Interleukin-1 beta, but not IL-1 alpha, mediates nerve growth factor secretion from rat astrocytes via type I IL-1 receptor. Int J Dev Neurosci. 2001, 19 (7): 675-683. 10.1016/S0736-5748(01)00044-2.
Strijbos PJ, Rothwell NJ: Interleukin-1 beta attenuates excitatory amino acid-induced neurodegeneration in vitro: involvement of nerve growth factor. J Neurosci. 1995, 15 (5): 3468-3474.
Carlson NG, Wieggel WA, Chen J, Bacchi A, Rogers SW, Gahring LC: Inflammatory cytokines IL-1 alpha, IL-1 beta, IL-6, and TNF-alpha impart neuroprotection to an excitotoxin through distinct pathways. J Immunol. 1999, 163 (7): 3963-3968.
Mason JL, Suzuki K, Chaplin DD, Matsushima GK: Interleukin-1beta promotes repair of the CNS. J Neurosci. 2001, 21 (18): 7046-7052.
Avital A, Goshen I, Kamsler A, Segal M, Iverfeldt K, Richter-Levin G, Yirmiya R: Impaired interleukin-1 signaling is associated with deficits in hippocampal memory processes and neural plasticity. Hippocampus. 2003, 13 (7): 826-834. 10.1002/hipo.10135.
Ferrari CC, Pott Godoy MC, Tarelli R, Chertoff M, Depino AM, Pitossi FJ: Progressive neurodegeneration and motor disabilities induced by chronic expression of IL-1beta in the substantia nigra. Neurobiol Dis. 2006, 24 (1): 183-193. 10.1016/j.nbd.2006.06.013.
Carvey PM, Chen EY, Lipton JW, Tong CW, Chang QA, Ling ZD: Intra-parenchymal injection of tumor necrosis factor-alpha and interleukin 1-beta produces dopamine neuron loss in the rat. J Neural Transm. 2005, 112 (5): 601-612. 10.1007/s00702-004-0222-z.
Thornton P, Pinteaux E, Gibson RM, Allan SM, Rothwell NJ: Interleukin-1-induced neurotoxicity is mediated by glia and requires caspase activation and free radical release. J Neurochem. 2006, 98 (1): 258-266. 10.1111/j.1471-4159.2006.03872.x.
Dinkel K, Dhabhar FS, Sapolsky RM: Neurotoxic effects of polymorphonuclear granulocytes on hippocampal primary cultures. Proc Natl Acad Sci USA. 2004, 101 (1): 331-336. 10.1073/pnas.0303510101.
Tani M, Fuentes ME, Peterson JW, Trapp BD, Durham SK, Loy JK, Bravo R, Ransohoff RM, Lira SA: Neutrophil infiltration, glial reaction, and neurological disease in transgenic mice expressing the chemokine N51/KC in oligodendrocytes. J Clin Invest. 1996, 98 (2): 529-539. 10.1172/JCI118821.
Connolly ES, Winfree CJ, Springer TA, Naka Y, Liao H, Yan SD, Stern DM, Solomon RA, Gutierrez-Ramos JC, Pinsky DJ: Cerebral protection in homozygous null ICAM-1 mice after middle cerebral artery occlusion. Role of neutrophil adhesion in the pathogenesis of stroke. J Clin Invest. 1996, 97 (1): 209-216. 10.1172/JCI118392.
Sheng JG, Mrak RE, Griffin WS: Glial-neuronal interactions in Alzheimer disease: progressive association of IL-1alpha+ microglia and S100beta+ astrocytes with neurofibrillary tangle stages. J Neuropathol Exp Neurol. 1997, 56 (3): 285-290.
Sheng JG, Mrak RE, Griffin WS: Neuritic plaque evolution in Alzheimer's disease is accompanied by transition of activated microglia from primed to enlarged to phagocytic forms. Acta Neuropathol (Berl). 1997, 94 (1): 1-5. 10.1007/s004010050664.
McGeer PL, Itagaki S, Tago H, McGeer EG: Reactive microglia in patients with senile dementia of the Alzheimer type are positive for the histocompatibility glycoprotein HLA-DR. Neurosci Lett. 1987, 79 (1-2): 195-200. 10.1016/0304-3940(87)90696-3.
Tuppo EE, Arias HR: The role of inflammation in Alzheimer's disease. Int J Biochem Cell Biol. 2005, 37 (2): 289-305. 10.1016/j.biocel.2004.07.009.
Akiyama H, Barger S, Barnum S, Bradt B, Bauer J, Cole GM, Cooper NR, Eikelenboom P, Emmerling M, Fiebich BL, Finch CE, Frautschy S, Griffin WS, Hampel H, Hull M, Landreth G, Lue L, Mrak R, Mackenzie IR, McGeer PL, O'Banion MK, Pachter J, Pasinetti G, Plata-Salaman C, Rogers J, Rydel R, Shen Y, Streit W, Strohmeyer R, Tooyoma I, Van Muiswinkel FL, Veerhuis R, Walker D, Webster S, Wegrzyniak B, Wenk G, Wyss-Coray T: Inflammation and Alzheimer's disease. Neurobiol Aging. 2000, 21 (3): 383-421. 10.1016/S0197-4580(00)00124-X.
Rogers J, Luber-Narod J, Styren SD, Civin WH: Expression of immune system-associated antigens by cells of the human central nervous system: relationship to the pathology of Alzheimer's disease. Neurobiol Aging. 1988, 9 (4): 339-349. 10.1016/S0197-4580(88)80079-4.
Heneka MT, O'Banion MK: Inflammatory processes in Alzheimer's disease. J Neuroimmunol. 2007, 184 (1-2): 69-91. 10.1016/j.jneuroim.2006.11.017.
Wyss-Coray T: Inflammation in Alzheimer disease: driving force, bystander or beneficial response?. Nat Med. 2006, 12 (9): 1005-1015.
Griffin WS, Sheng JG, Royston MC, Gentleman SM, McKenzie JE, Graham DI, Roberts GW, Mrak RE: Glial-neuronal interactions in Alzheimer's disease: the potential role of a 'cytokine cycle' in disease progression. Brain Pathol. 1998, 8 (1): 65-72.
Breitner JC, Gau BA, Welsh KA, Plassman BL, McDonald WM, Helms MJ, Anthony JC: Inverse association of anti-inflammatory treatments and Alzheimer's disease: initial results of a co-twin control study. Neurology. 1994, 44 (2): 227-232.
McGeer PL, Rogers J, McGeer EG: Inflammation, anti-inflammatory agents and Alzheimer disease: the last 12 years. J Alzheimers Dis. 2006, 9 (3 Suppl): 271-276.
in t' Veld BA, Ruitenberg A, Hofman A, Launer LJ, van Duijn CM, Stijnen T, Breteler MM, Stricker BH: Nonsteroidal antiinflammatory drugs and the risk of Alzheimer's disease. N Engl J Med. 2001, 345 (21): 1515-1521. 10.1056/NEJMoa010178.
Stewart WF, Kawas C, Corrada M, Metter EJ: Risk of Alzheimer's disease and duration of NSAID use. Neurology. 1997, 48 (3): 626-632.
Szekely CA, Thorne JE, Zandi PP, Ek M, Messias E, Breitner JC, Goodman SN: Nonsteroidal anti-inflammatory drugs for the prevention of Alzheimer's disease: a systematic review. Neuroepidemiology. 2004, 23 (4): 159-169. 10.1159/000078501.
Rogers J, Kirby LC, Hempelman SR, Berry DL, McGeer PL, Kaszniak AW, Zalinski J, Cofield M, Mansukhani L, Willson P, et al: Clinical trial of indomethacin in Alzheimer's disease. Neurology. 1993, 43 (8): 1609-1611.
Scharf S, Mander A, Ugoni A, Vajda F, Christophidis N: A double-blind, placebo-controlled trial of diclofenac/misoprostol in Alzheimer's disease. Neurology. 1999, 53 (1): 197-201.
Aisen PS, Schmeidler J, Pasinetti GM: Randomized pilot study of nimesulide treatment in Alzheimer's disease. Neurology. 2002, 58 (7): 1050-1054.
Aisen PS, Schafer KA, Grundman M, Pfeiffer E, Sano M, Davis KL, Farlow MR, Jin S, Thomas RG, Thal LJ: Effects of rofecoxib or naproxen vs placebo on Alzheimer disease progression: a randomized controlled trial. Jama. 2003, 289 (21): 2819-2826. 10.1001/jama.289.21.2819.
Reines SA, Block GA, Morris JC, Liu G, Nessly ML, Lines CR, Norman BA, Baranak CC: Rofecoxib: no effect on Alzheimer's disease in a 1-year, randomized, blinded, controlled study. Neurology. 2004, 62 (1): 66-71. 10.1159/000080761.
Soininen H, West C, Robbins J, Niculescu L: Long-term efficacy and safety of celecoxib in Alzheimer's disease. Dement Geriatr Cogn Disord. 2007, 23 (1): 8-21. 10.1159/000096588.
Group AR, Lyketsos CG, Breitner JC, Green RC, Martin BK, Meinert C, Piantadosi S, Sabbagh M: Naproxen and celecoxib do not prevent AD in early results from a randomized controlled trial. Neurology. 2007, 68 (21): 1800-1808. 10.1212/01.wnl.0000260269.93245.d2.
McGeer PL, McGeer EG: NSAIDs and Alzheimer disease: epidemiological, animal model and clinical studies. Neurobiol Aging. 2007, 28 (5): 639-647. 10.1016/j.neurobiolaging.2006.03.013.
Frautschy SA, Yang F, Irrizarry M, Hyman B, Saido TC, Hsiao K, Cole GM: Microglial response to amyloid plaques in APPsw transgenic mice. Am J Pathol. 1998, 152 (1): 307-317.
Sheng JG, Mrak RE, Bales KR, Cordell B, Paul SM, Jones RA, Woodward S, Zhou XQ, McGinness JM, Griffin WS: Overexpression of the neuritotrophic cytokine S100beta precedes the appearance of neuritic beta-amyloid plaques in APPV717F mice. J Neurochem. 2000, 74 (1): 295-301. 10.1046/j.1471-4159.2000.0740295.x.
Janelsins MC, Mastrangelo MA, Oddo S, LaFerla FM, Federoff HJ, Bowers WJ: Early correlation of microglial activation with enhanced tumor necrosis factor-alpha and monocyte chemoattractant protein-1 expression specifically within the entorhinal cortex of triple transgenic Alzheimer's disease mice. J Neuroinflammation. 2005, 2: 23-10.1186/1742-2094-2-23.
Matsuoka Y, Picciano M, Malester B, LaFrancois J, Zehr C, Daeschner JM, Olschowka JA, Fonseca MI, O'Banion MK, Tenner AJ, Lemere CA, Duff K: Inflammatory responses to amyloidosis in a transgenic mouse model of Alzheimer's disease. Am J Pathol. 2001, 158 (4): 1345-1354.
Liang X, Wang Q, Hand T, Wu L, Breyer RM, Montine TJ, Andreasson K: Deletion of the prostaglandin E2 EP2 receptor reduces oxidative damage and amyloid burden in a model of Alzheimer's disease. J Neurosci. 2005, 25 (44): 10180-10187. 10.1523/JNEUROSCI.3591-05.2005.
Griffin WS, Sheng JG, Roberts GW, Mrak RE: Interleukin-1 expression in different plaque types in Alzheimer's disease: significance in plaque evolution. J Neuropathol Exp Neurol. 1995, 54 (2): 276-281.
Mrak RE, Griffin WS: Trisomy 21 and the brain. J Neuropathol Exp Neurol. 2004, 63 (7): 679-685.
McGeer PL, McGeer EG: Polymorphisms in inflammatory genes and the risk of Alzheimer disease. Arch Neurol. 2001, 58 (11): 1790-1792. 10.1001/archneur.58.11.1790.
Griffin WS, Nicoll JA, Grimaldi LM, Sheng JG, Mrak RE: The pervasiveness of interleukin-1 in alzheimer pathogenesis: a role for specific polymorphisms in disease risk. Exp Gerontol. 2000, 35 (4): 481-487. 10.1016/S0531-5565(00)00110-8.
Bertram L, McQueen MB, Mullin K, Blacker D, Tanzi RE: Systematic meta-analyses of Alzheimer disease genetic association studies: the AlzGene database. Nat Genet. 2007, 39 (1): 17-23. 10.1038/ng1934.
Mrak RE, Griffin WS: The role of chronic self-propagating glial responses in neurodegeneration: implications for long-lived survivors of human immunodeficiency virus. J Neurovirol. 1997, 3 (4): 241-246.
Meda L, Baron P, Prat E, Scarpini E, Scarlato G, Cassatella MA, Rossi F: Proinflammatory profile of cytokine production by human monocytes and murine microglia stimulated with beta-amyloid[25-35]. J Neuroimmunol. 1999, 93 (1-2): 45-52. 10.1016/S0165-5728(98)00188-X.
Barger SW, Harmon AD: Microglial activation by Alzheimer amyloid precursor protein and modulation by apolipoprotein E. Nature. 1997, 388 (6645): 878-881. 10.1038/42257.
Brugg B, Dubreuil YL, Huber G, Wollman EE, Delhaye-Bouchard N, Mariana J: Inflammatory processes induce ß-amyloid precursor protein changes in mouse brain. Proc Natl Acad Sci USA. 1995, 92: 3032-3035. 10.1073/pnas.92.7.3032.
Goldgaber D, Harris HH, Hla T, Maciag T, Donnelly RJ, Jacobsen JS, Vitek MP, Gajdusek DC: Interleukin 1 regulates synthesis of amyloid ß-protein precursor mRNA in human endothelial cells. Proc Natl Acad Sci USA. 1989, 86: 7606-7610. 10.1073/pnas.86.19.7606.
Gray CW, Patel AJ: Regulation of ß-amyloid precursor protein isoform mRNAs by transforming growth factor-ß1 and interleukin-1ß in astroctyes. Mol Brain Res. 1993, 19: 251-256. 10.1016/0169-328X(93)90037-P.
Rogers JT, Leiter LM, McPhee J, Cahill CM, Zhan SS, Potter H, Nilsson LN: Translation of the Alzheimer amyloid precursor protein mRNA is up-regulated by interleukin-1 through 5'-untranslated region sequences. J Biol Chem. 1999, 274 (10): 6421-6431. 10.1074/jbc.274.10.6421.
Liao YF, Wang BJ, Cheng HT, Kuo LH, Wolfe MS: Tumor necrosis factor-alpha, interleukin-1beta, and interferon-gamma stimulate gamma-secretase-mediated cleavage of amyloid precursor protein through a JNK-dependent MAPK pathway. J Biol Chem. 2004, 279 (47): 49523-49532. 10.1074/jbc.M402034200.
Sheng JG, Ito K, Skinner RD, Mrak RE, Rovnaghi CR, Van Eldik LJ, Griffin WS: In vivo and in vitro evidence supporting a role for the inflammatory cytokine interleukin-1 as a driving force in Alzheimer pathogenesis. Neurobiol Aging. 1996, 17 (5): 761-766. 10.1016/0197-4580(96)00104-2.
Craft JM, Watterson DM, Hirsch E, Van Eldik LJ: Interleukin 1 receptor antagonist knockout mice show enhanced microglial activation and neuronal damage induced by intracerebroventricular infusion of human beta-amyloid. J Neuroinflammation. 2005, 2 (1): 15-10.1186/1742-2094-2-15.
Griffin WS, Liu L, Li Y, Mrak RE, Barger SW: Interleukin-1 mediates Alzheimer and Lewy body pathologies. J Neuroinflammation. 2006, 3: 5-10.1186/1742-2094-3-5.
Sheng JG, Zhu SG, Jones RA, Griffin WS, Mrak RE: Interleukin-1 promotes expression and phosphorylation of neurofilament and tau proteins in vivo. Exp Neurol. 2000, 163 (2): 388-391. 10.1006/exnr.2000.7393.
Li Y, Liu L, Barger SW, Griffin WS: Interleukin-1 mediates pathological effects of microglia on tau phosphorylation and on synaptophysin synthesis in cortical neurons through a p38-MAPK pathway. J Neurosci. 2003, 23: 1605-1611.
Yoshiyama Y, Higuchi M, Zhang B, Huang SM, Iwata N, Saido TC, Maeda J, Suhara T, Trojanowski JQ, Lee VM: Synapse loss and microglial activation precede tangles in a P301S tauopathy mouse model. Neuron. 2007, 53 (3): 337-351. 10.1016/j.neuron.2007.01.010.
Kitazawa M, Oddo S, Yamasaki TR, Green KN, LaFerla FM: Lipopolysaccharide-induced inflammation exacerbates tau pathology by a cyclin-dependent kinase 5-mediated pathway in a transgenic model of Alzheimer's disease. J Neurosci. 2005, 25 (39): 8843-8853. 10.1523/JNEUROSCI.2868-05.2005.
DiCarlo G, Wilcock D, Henderson D, Gordon M, Morgan D: Intrahippocampal LPS injections reduce Abeta load in APP+PS1 transgenic mice. Neurobiol Aging. 2001, 22 (6): 1007-1012. 10.1016/S0197-4580(01)00292-5.
Quinn J, Montine T, Morrow J, Woodward WR, Kulhanek D, Eckenstein F: Inflammation and cerebral amyloidosis are disconnected in an animal model of Alzheimer's disease. J Neuroimmunol. 2003, 137 (1-2): 32-41. 10.1016/S0165-5728(03)00037-7.
Herber DL, Roth LM, Wilson D, Wilson N, Mason JE, Morgan D, Gordon MN: Time-dependent reduction in Abeta levels after intracranial LPS administration in APP transgenic mice. Exp Neurol. 2004, 190 (1): 245-253. 10.1016/j.expneurol.2004.07.007.
Wyss-Coray T, Lin C, Yan F, Yu GQ, Rohde M, McConlogue L, Masliah E, Mucke L: TGF-beta1 promotes microglial amyloid-beta clearance and reduces plaque burden in transgenic mice. Nature medicine. 2001, 7 (5): 612-618. 10.1038/87945.
Jantzen PT, Connor KE, DiCarlo G, Wenk GL, Wallace JL, Rojiani AM, Coppola D, Morgan D, Gordon MN: Microglial activation and beta -amyloid deposit reduction caused by a nitric oxide-releasing nonsteroidal anti-inflammatory drug in amyloid precursor protein plus presenilin-1 transgenic mice. J Neurosci. 2002, 22 (6): 2246-2254.
Seabrook TJ, Jiang L, Maier M, Lemere CA: Minocycline affects microglia activation, Abeta deposition, and behavior in APP-tg mice. Glia. 2006, 53 (7): 776-782. 10.1002/glia.20338.
Qiao X, Cummins DJ, Paul SM: Neuroinflammation-induced acceleration of amyloid deposition in the APPV717F transgenic mouse. Eur J Neurosci. 2001, 14 (3): 474-482. 10.1046/j.0953-816x.2001.01666.x.
Sheng JG, Bora SH, Xu G, Borchelt DR, Price DL, Koliatsos VE: Lipopolysaccharide-induced-neuroinflammation increases intracellular accumulation of amyloid precursor protein and amyloid beta peptide in APPswe transgenic mice. Neurobiol Dis. 2003, 14 (1): 133-145. 10.1016/S0969-9961(03)00069-X.
D'Andrea MR, Cole GM, Ard MD: The microglial phagocytic role with specific plaque types in the Alzheimer disease brain. Neurobiol Aging. 2004, 25 (5): 675-683. 10.1016/j.neurobiolaging.2003.12.026.
Bacskai BJ, Kajdasz ST, Christie RH, Carter C, Games D, Seubert P, Schenk D, Hyman BT: Imaging of amyloid-beta deposits in brains of living mice permits direct observation of clearance of plaques with immunotherapy. Nat Med. 2001, 7 (3): 369-372. 10.1038/85525.
Bard F, Cannon C, Barbour R, Burke RL, Games D, Grajeda H, Guido T, Hu K, Huang J, Johnson-Wood K: Peripherally administered antibodies against amyloid bold beta-peptide enter the central nervous system and reduce pathology in a mouse model of Alzheimer disease. Nat Med. 2000, 6: 916-919. 10.1038/78682.
Wilcock DM, Munireddy SK, Rosenthal A, Ugen KE, Gordon MN, Morgan D: Microglial activation facilitates Abeta plaque removal following intracranial anti-Abeta antibody administration. Neurobiol Dis. 2004, 15 (1): 11-20. 10.1016/j.nbd.2003.09.015.
Malm TM, Koistinaho M, Parepalo M, Vatanen T, Ooka A, Karlsson S, Koistinaho J: Bone-marrow-derived cells contribute to the recruitment of microglial cells in response to beta-amyloid deposition in APP/PS1 double transgenic Alzheimer mice. Neurobiol Dis. 2005, 18 (1): 134-142. 10.1016/j.nbd.2004.09.009.
Simard AR, Soulet D, Gowing G, Julien JP, Rivest S: Bone marrow-derived microglia play a critical role in restricting senile plaque formation in Alzheimer's disease. Neuron. 2006, 49 (4): 489-502. 10.1016/j.neuron.2006.01.022.
Simard AR, Rivest S: Neuroprotective properties of the innate immune system and bone marrow stem cells in Alzheimer's disease. Mol Psychiatry. 2006, 11 (4): 327-335. 10.1038/sj.mp.4001809.
Butovsky O, Kunis G, Koronyo-Hamaoui M, Schwartz M: Selective ablation of bone marrow-derived dendritic cells increases amyloid plaques in a mouse Alzheimer's disease model. Eur J Neurosci. 2007, 26 (2): 413-416. 10.1111/j.1460-9568.2007.05652.x.
Das P, Smithson LA, Price RW, Holloway VM, Levites Y, Chakrabarty P, Golde TE: Interleukin-1 receptor 1 knockout has no effect on amyloid deposition in Tg2576 mice and does not alter efficacy following Abeta immunotherapy. J Neuroinflammation. 2006, 3: 17-10.1186/1742-2094-3-17.
Author information
Authors and Affiliations
Corresponding author
Additional information
Competing interests
The author(s) declare that they have no competing interests.
Authors' contributions
The manuscript was written by SS as part of his doctoral thesis. MKO'B and WSTG provided historical perspectives and editorial assistance.
Authors’ original submitted files for images
Below are the links to the authors’ original submitted files for images.
Rights and permissions
Open Access This article is published under license to BioMed Central Ltd. This is an Open Access article is distributed under the terms of the Creative Commons Attribution License ( https://creativecommons.org/licenses/by/2.0 ), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
About this article
Cite this article
Shaftel, S.S., Griffin, W.S.T. & O'Banion, M.K. The role of interleukin-1 in neuroinflammation and Alzheimer disease: an evolving perspective. J Neuroinflammation 5, 7 (2008). https://doi.org/10.1186/1742-2094-5-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/1742-2094-5-7