Abstract
As with other solid tumors, the growth and metastasis of pancreatic cancer is critically dependent on tumor angiogenesis. A major stimulus for a tumor's recruitment of additional blood vessels is cellular hypoxia, a condition which is especially pronounced in this neoplasm. Hypoxia induces transcriptional activation of genes that alter cellular metabolism and promote neoangiogenesis. Pancreatic cancer cells have demonstrated activation of such adaptive pathways even in the absence of hypoxia. A highly-angiogenic response in this neoplasm correlates with increased tumor growth, increased metastasis, and decreased survival. Pancreatic cancers expressing high levels of vascular endothelial growth factor, a potent pro-angiogenic cytokine, also have a higher incidence of metastasis and poorer prognosis. Pancreatic cancer cells uniquely express receptors for vascular endothelial growth factor, indicating a role for an autocrine loop in tumor proliferation and invasion. Multiple experimental anti-angiogenic strategies, many of which target vascular endothelial growth factor, reduce pancreatic cancer growth, spread, and angiogenesis. Anti-angiogenic treatments for pancreatic cancer will likely be most effective when used as an integral part of a combination chemotherapeutic regimen.
Similar content being viewed by others
Introduction
Adenocarcinoma of the pancreas remains a most formidable malignancy. Usually undiagnosed until reaching an advanced stage, pancreatic cancer is characterized by its predisposition to aggressively invade surrounding tissues, to metastasize early and extensively, and to resist conventional chemoradiation treatment strategies. Recent estimates project that over 30,000 new cases of pancreatic cancer will be diagnosed in the United States in 2002, and the annual mortality rate closely approaches that of the number of new cases [1]. Despite diagnostic and therapeutic advances made in other gastrointestinal malignancies, the overall five-year survival for patients with pancreatic cancer remains a dismal 3 to 4% [1]. Improvement in the treatment of this disease must arise from a better understanding of the cellular and molecular mechanisms utilized by the cancer to proliferate, invade surrounding tissues, and elude cytotoxic therapies. As with other solid tumors, there has been a surge in the study of pancreatic tumor neovascularization that is critical to growth and metastasis.
The notion that a growing mass of tumor cells must recruit its own blood supply for the maintenance of oxygen and nutrients, termed tumor angiogenesis, was popularized by Judah Folkman in the early 1970s [2]. Since this first description of angiogenesis as a requisite process for continuous solid tumor growth, many endogenous pro- and anti-angiogenic substances secreted by tumor cells, tissue resident and stromal cells, and infiltrating lymphocytes have been characterized [3–7]. As a solid tumor grows, some cells inevitably become physically separated from the native tissue's nutrient vascular stroma, and delivery of nutrients and oxygen to those cells becomes limited by diffusion [1, 8]. The end result is metabolic stress and cellular hypoxia – conditions thought to be major stimuli underlying the recruitment of additional blood vessels [9]. Hypoxia induces changes in transcriptional regulation that serve to alter cellular metabolism (i.e., shift to glycolytic pathways) and promote the ingrowth of immature, architecturally deranged, and highly permeable blood vessels that facilitate the passage of tumor cells into the circulation [9–12]. Thus, a cancer's response to hypoxia not only sustains tumor growth and survival, but through angiogenesis it fosters invasion and metastasis. Indeed, hypoxic tumors have been reported to have a predilection for tissue invasion and metastasis [13, 14]. Such adaptability has been proposed to be especially relevant in pancreatic cancer, a malignancy that exhibits a profound and characteristic avascular, hypodense appearance on contrast-enhanced computerized tomography of the abdomen [15].
In this article we will review the relevant data characterizing pancreatic cancer as an hypoxic tumor, and discuss the molecular mechanisms by which this neoplasm responds to hypoxia, generates new blood vessel growth, and promotes its own growth and metastasis.
Hypoxia in cancer tumorigenesis and metastasis
Discussion of the role of hypoxia in pancreatic cancer requires some background on the effects of hypoxia on cancer cells in general. A role for an hypoxic microenvironment in the pathogenesis and progression of human cancer was first proposed in 1953, when well-oxygenated tumor cells were found to exhibit 3-fold greater response to radiotherapy when compared to anoxic cells [16]. The reasons why tumors become hypoxic remain unclear, but multiple mechanisms likely contribute to its development. These include unrestrained growth and accelerated oxygen consumption by tumor cells; poor lymphatic drainage of tumors resulting in high interstitial pressures, vascular collapse, and low pH; and intratumoral shunting of oxygen-rich blood through immature vasculature [10]. Furthermore, tumor angiogenesis may not necessarily equate to tumor blood supply, as the discontinuous basement membrane of immature neo-angiogenic vessels allows for the extravasation of plasma and proteins, further increases in intratumoral interstitial pressure, continued vascular collapse, and poor nutrient delivery [10]. Some tumors also demonstrate an inability to preserve blood vessel survival, a condition which accounts for the well-vascularized, invasive periphery and the hypoxic area of central necrosis found in several highly angiogenic tumors [17].
Experimental evidence suggests that tumor cells exist under hypoxic conditions at a distance of 300–400 μm from blood vessels, indicating that hypoxic conditions are generally established in tumors measuring only 0.5 mm in diameter [18]. In order to increase oxygen availability (angiogenesis) or to decrease oxygen consumption (i.e., shift to glycolytic metabolism), tumor cells alter their transcription of a wide range of genes whose protein products serve to stimulate blood vessel growth (pro-angiogenic factors) or to modulate cellular glucose metabolism (glycolytic enzymes) [10]. A large number of genes are now known to be regulated by hypoxia, including those encoding erythropoietin, vascular endothelial growth factor (VEGF), glycolytic enzymes, and inducible nitric oxide synthase (iNOS) [19–22].
Hypoxia-inducible genes contain hypoxia response elements (HREs) – sequences of around 50 base pairs that bind hypoxia-activated transcription factors [23–25]. Several of these transcription factors have been described, and the most important and best understood is the Hypoxia Inducible Factor-1 (HIF-1) [24–29]. HIF-1 was originally identified in 1992 in Hep3B cells as a nuclear protein factor induced by hypoxia with binding activity to an enhancer in the erythropoietin gene [26]. HIF-1 is a heterodimer formed by the association of α – and β-subunits (HIF-1α and HIF-1β), both of which belong to the basic helix-loop-helix (bHLH) – PAS (PER, ARNT, SIM) family of transcription activator proteins (see Figure 1) [29, 30]. HIF-1β is also known as the aryl hydrocarbon receptor nuclear translocator (ARNT) [30–32]. While HIF-1β protein is constitutively expressed in mammalian cells under normoxic conditions, virtually no HIF-1α is found [24]. Under normoxic conditions, the cellular half-life of HIF-1α is around 5 minutes, as the protein is rapidly degraded by the ubiquitin-proteasome system [24, 33, 34]. Under hypoxic conditions, the HIF-1α protein is stabilized by the absence of posttranslational hydroxylation events at PRO 564 of the HIF-1α molecule [24].
Structure of the HIF-1 Complex. The hypoxia inducible factor 1 complex (HIF-1) is a dimer composed of two proteins involved in hypoxic gene transactivation, HIF-1α and HIF-1β (ARNT). Dimerization between these two factors is mediated by the helix-loop-helix (HLH) and Per-ARNT-SIM domains, and DNA binding involves the basic (b-) region of the b-HLH domains. HIF-1 modulates transcription through its transactivation domains (TAD). Between amino acids 401 and 603, HIF-1α contains an oxygen-dependent degradation domain (ODD) which controls its degradation under normoxia [24]. Fig. 1
Stable HIF-1α translocates to the nucleus in a process mediated by specific nuclear localization signals and dimerizes with HIF-1β [24]. To activate transcription of hypoxia-regulated genes, the intact heterodimeric HIF-1 complex binds DNA at specific HREs characterized by the consensus sequence 5'-RCGTG-3' [23]. Within the HIF-1 complex, the HLH and PAS-domains mediate factor dimerization, whereas the basic domain binds directly to DNA HREs [24]. Once nuclear translocation and dimerization are complete, activation of transcription occurs through interactions between co-activator proteins and two transactivation domains (TADs), both of which are located in the C-terminal half of HIF-1α (N-TAD, C-TAD) [23]. In summary, hypoxic conditions lead to HIF-1α stabilization and translocation to the cell nucleus, dimerization with HIF-1β to form the HIF-1 complex, and activation of transcription through HIF-1's binding to specific HREs in target sequences (see Figure 2).
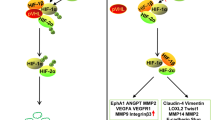
Molecular mechanisms of hypoxia-induced angiogenesis. Under normoxic conditions (panel A), HIF-1α is hydroxylated by the active prolyl-4-hydroxylase enzyme, which facilitates the binding of VHL protein and leads to rapid HIF-1α degradation by the ubiquitin proteasome system. In the face of hypoxia (panel B), the hydroxylase enzyme is inactive and HIF-1α is stabilized in its de-hydroxylated state. The stable HIF-1α translocates to the nucleus, where it accumulates and dimerizes with the constitutively expressed HIF-1β, forming the intact HIF-1 complex. This complex binds hypoxia response elements (HREs) in selective genes to alter transcriptional activity. A notable hypoxia-induced gene is that coding for vascular endothelial growth factor (VEGF), a cytokine which potently stimulates neoangiogenesis [24].
While hypoxia is the major stimulus for HIF-1α stabilization and activation, some evidence indicates that cellular constituents participate in the regulation of HIF-1α activity as well. The von Hippel-Lindau protein (pVHL) is the product of the VHL gene, a tumor-suppressor gene known to be inactivated in renal clear-cell carcinomas as well as other markedly vascular tumors such as central nervous system hemangioblastoma [24]. The VHL protein contains a binding site in the oxygen-dependent degradation domain (ODD) of HIF-1α between amino acids 401–603 [35–37]. As the VHL protein is a subunit in the multimeric E3 ubiquitin ligase complex, its binding to the ODD regions of HIF-1α leads to ubiquitin conjugation and degradation of the factors by the ubiquitin proteasome system. Thus, loss of the VHL protein results in constitutive stabilization of HIF-1α and transactivation of genes promoting vasculogenesis (i.e., VEGF) [24, 35–37]. In addition, phosphorylation of HIF-1α by the p44/42 mitogen activated protein kinases (MAPK) results in enhanced transcriptional activation independent of cellular hypoxia [38]. Experimental evidence suggests that p44/42 MAPK phosphorylation events are required for transcriptional activation mediated by HIF-2α, a related hypoxia-induced factor also known as endothelial PAS-protein-1 (EPAS-1) [39].
Compared to normal tissue controls, HIF-1 protein has been shown through immunohistochemical studies to be overexpressed in several human cancers, including colon, breast, gastric, lung, skin, ovarian, prostate, renal, and pancreatic carcinomas [40]. Interestingly, in these studies, HIF-1α positive cells were noted to be crowded most densely at a tumor's infiltrating margin, around the periphery of necrotic areas, and surrounding regions of high microvessel density [40]. HIF-1α expression was also more pronounced in nodal and bone metastases than in primary tumor specimens [40]. Premalignant lesions such as breast comedo-type ductal carcinoma in situ, prostatic intraepithelial neoplasia, and colonic adenoma showed HIF-1α positivity, whereas benign lesions (mammary fibroadenoma and uterine leiomyoma) did not [40]. These results emphasize that HIF-1α plays an important role in cancer growth and metastasis. Its overexpression may represent an early event in carcinogenesis and may eventually serve as a possible biomarker for precancerous disease.
Hypoxia in pancreatic cancer pathogenesis and progression
The presence of significant hypoxia in pancreatic cancers has been long suspected, especially given these lesions' characteristic avascular appearance on contrast-enhanced CT scan [15]. Hypoxia in pancreatic cancer was first documented by Koong and colleagues in 2000, when they reported results from direct intratumoral needle O2 measurements at the time of resection in seven patients with operable pancreatic cancers [41]. Areas of pancreatic carcinoma exhibited median pO2 levels of 0–5.3 mmHg with 24–94% of samplings having pO2 levels less than 2.5 mmHg [41]. In contrast, adjacent areas of normal pancreatic tissue had median tissue pO2 levels of 24–92.7 mmHg, and no more than 9% of any samplings had measurements less than 2.5 mmHg (seven patients had no levels < 2.5 mmHg) [41]. In our own unpublished experience we have found similar levels of hypoxia measured by intraoperative needle measurement. Earlier we demonstrated profound pancreatic tissue hypoxia in chronic pancreatitis, a condition that usually co-exists in pancreatic cancer patients [42].
Our laboratory has confirmed that HIF-1 is activated in pancreatic cancer in response to low oxygen levels in vitro and in vivo [43]. Studies in human specimens of pancreatic cancer showed co-localization of VEGF mRNA, which is produced in ductal cancer cells, and HIF-1α protein, which was detectable in the cell nuclei of cancer cells [43]. HIF-1α mRNA expression was dramatically upregulated in human pancreatic cancer specimens [43]. In vitro all pancreatic cancer cell lines increased VEGF production under low oxygen levels by highly specific activation of HIF-1 DNA binding activity to the VEGF promotor [43]. Cell lines with high constitutive levels of HIF-1α protein were found to produce higher basal levels of VEGF [43]. Thus it appears that HIF-1 is the link between tumor hypoxia and VEGF production in pancreatic cancer.
The effects of an hypoxic environment on pancreatic cancer cells are beginning to be understood on a molecular level. Our laboratory has recently collaborated in the identification of three genes induced by hypoxia in vitro in the well-differentiated human pancreatic cancer cell line Capan-2 [44]. The genes are GPI/NLK/AMF (glucose phosphate isomerase/neuroleukin/autocrine motility factor), DEC1, and hexokinase II [44]. These results marked the first evidence that DEC1 and hexokinase II were hypoxia-induced in human pancreatic cancer and represented the initial report of hypoxic-regulation of GPI/NLK/AMF in any human system [44]. Additional studies are under way to further elucidate the roles of these genes in the development and progression of pancreatic cancer.
Interestingly, recent studies are beginning to define a role for HIF-1α in pancreatic cancer independent of an hypoxic environment. Akakura et al have reported expression of HIF-1α protein in several human pancreatic cancer cell lines in normoxic conditions [45]. This constitutive HIF-1α expression improved pancreatic cancer cell proliferation and survival under hypoxic and glucose-deprived conditions in vitro, results that were associated with increased mRNA expression of Glut1 and aldolase A, both glycolytic enzymes [45]. These studies demonstrate that pancreatic cancer cells can survive and proliferate despite hypoxia and glucose deprivation, and HIF-1α likely mediates their adaptive cellular responses [45]. However, they also emphasize that in human pancreatic cancer cells, HIF-1α stabilization and activity may be promoted through primary intracellular alterations not induced by hypoxia.
Recent evidence indicates that the hypoxic adaptive response in pancreatic cancer cells may also involve upregulation of pro-inflammatory cytokines. Shi et al demonstrated that pancreatic cancer cells which constitutively expressed high levels of interleukin-8 (IL-8), a pro-angiogenic ELR+ member of the -CXC- chemokine family, formed larger tumors with more extensive metastases in an orthotopic mouse model [46]. Immunohistochemical analyses of tumors revealed that IL-8 upregulation was clustered primarily near areas of tumor necrosis, sites likely to have the most acidic interstitial pH and the lowest levels of diffusible oxygen and nutrients [46]. In vitro exposure to hypoxia increased expression of IL-8 in all cell lines examined [46]. Treatment with IL-8 antisense oligonucleotides resulted in decreased tumor growth and angiogenesis in vivo [46]. Unpublished results from our laboratory have demonstrated constitutive secretion of additional pro-angiogenic CXC chemokines by multiple cell lines of human pancreatic cancer. Further studies will continue to unravel the mechanisms by which pro-and anti-angiogenic inflammatory cytokines modulate angiogenesis and growth of pancreatic adenocarcinoma.
Neoangiogenesis in pancreatic cancer
Interest in tumor angiogenesis in pancreatic cancer stems not only from this tumor's remarkable tendency toward early local tissue invasion and metastasis, but also from its characteristic hypodense, hypovascular appearance on contrast-enhanced computerized tomographic scans. While investigation into angiogenesis in pancreatic cancer may appear contradictory at first, it is important to keep in perspective that CT-enhancement reflects intra-and peritumoral macro-vessels, not micro-vessels. Furthermore, several lines of evidence indicate that neoangiogenesis is an important component in pancreatic cancer growth and metastasis [47, 48].
Pancreatic adenocarcinomas exhibit high levels of intratumoral microvessel density
Several studies have evaluated pancreatic adenocarcinomas for intratumoral microvessel density (IMD) profiles suggestive of significant tumor-induced angiogenesis. Through immunohistochemistry, Kuehn et al found IMD to be increased in pancreatic cancer specimens over that of normal pancreas and chronic pancreatitis specimens [49]. Other researchers have found high IMD in pancreatic cancer to correlate with poor patient survival [50–54]. In an immunohistochemical analysis of 22 pancreatic adenocarcinoma specimens, Karademir and colleagues found that a tumor's vascular surface density and number of microvessels per mm2 of stroma correlated with increased tumor proliferation, poor differentiation, larger tumor size (>3 cm), and decreased patient survival [54]. Further support has come from Fujioka et al who found that high IMD in pancreatic tumors correlated with significantly reduced overall and disease free survival rates [55]. In addition, those tumors with high IMD had significantly-increased incidence of hepatic metastasis compared to low-IMD tumors [55]. Conversely, an immunohistochemical study by Ellis and colleagues of 22 pancreatic adenocarcinoma specimens demonstrated no significant correlation between IMD/VEGF expression and patient survival or time to recurrence [56]. Despite these findings, the vast majority of data at this point indicate that pancreatic adenocarcinomas exhibit a high degree of angiogenesis; and, as has been demonstrated in other solid tumors such as breast, lung, prostate, cervix, and colon cancer, high IMD correlates with poorer prognosis and greater risk for metastasis [50–55, 57–61].
Angiogenic factors and their receptors are expressed by pancreatic adenocarcinomas
The process of angiogenesis reflects a balance between pro- and anti-angiogenic factors in the peri-tumoral milieu [12]. Although several pro- and anti-angiogenic factors are expressed by pancreatic adenocarcinomas [62–65], much of the research in pancreatic cancer thus far has centered on vascular endothelial growth factor (VEGF). First described in 1979 as a tumor-secreted protein that profoundly increased microvascular permeability in subcutaneous tumors in guinea pigs (originally termed vascular permeability factor) [66], VEGF subsequently has been noted to stimulate endothelial cell proliferation and migration, to influence endothelial cell gene activation, and to act on endothelial cells as an anti-apoptotic agent [67–69]. It should be noted that VEGF's initial function, rendering tumor microvessels markedly permeable to plasma and proteins, is paramount to tumor growth and progression through angiogenesis: the resultant extravascular fibin-rich stroma provides a nutrient scaffold upon which activated endothelial cells can migrate and form vascular tubes [70].
VEGF represents the original dimeric cytokine belonging to the platelet-derived growth factor (PDGF) family of growth factors, with members including VEGF-A (vascular permeability factor), VEGF-B, VEGF-C, VEGF-D, VEGF-E, and placenta growth factor (PlGF) [70]. Investigation in pancreatic cancer has focused thus far on VEGF-A, a disulfide-bonded dimeric glycoprotein of 34–45 kDa encoded on chromosome 6p and existing as several isoforms secondary to differential splicing (VEGF-A165 is the most commonly found isoform) [70]. VEGF-A exerts its effects on target endothelial cells through interactions with its two specific transmembrane tyrosine kinase receptors, VEGFR-1 (Flt-1) and VEGFR-2 (KDR, flk-1) [70]. These receptors are selectively expressed on endothelial cells, but rarely they may also be expressed on some tumor cells.
Upon binding VEGF-A, the VEGF receptors dimerize, undergo autophosphorylation, and propagate signals through multiple intracellular pathways, including the MAPK, PI3-kinase, Ras, and phospholipase C cascades [70]. VEGFR-2 appears to modulate endothelial cell proliferation and migration, and increases microvessel permeability, whereas the actions of VEGFR-1 are not yet fully described [70]. Mice null (-/-) for either VEGFR have abnormal vasculogenesis and die during embryogenesis [70].
Recently, the neuropilins 1 and 2, known to be receptors for axonal guidance factors of the semaphorin family, have been identified as additional receptors for some VEGF-A isoforms [71–73]. Existing evidence indicates that neuropilin-1 acts as a coreceptor which enhances the activity of VEGFR-2 upon binding to VEGF-A165, leading to increased endothelial cell migration [73]. Neuropilin-2 is also able to bind VEGF-A165, but unlike neuropilin-1, it also interacts with VEGF-A145 [70, 72, 73]. The roles of the non-kinase neuropilins in tumor-induced angiogenesis are now beginning to be examined [70].
Several studies have examined VEGF-A expression and function in pancreatic cancer. The first evidence for VEGF-A expression was immunopositive staining of a single pancreatic cancer specimen [74]. Multiple subsequent studies have confirmed VEGF expression by pancreatic cancer and have demonstrated correlation between high tumoral expression and poor prognosis [75–80]. VEGF-A overexpression has been detected in the ascites induced by pancreatic cancer metastases [81]. Seo et al demonstrated VEGF-A protein in 132/142 (93%) human pancreatic cancer specimens using immunohistochemistry, and high VEGF positivity correlated directly with increased IMD and presence of hepatic metastasis [75]. Also, patients with high VEGF tumor expression had significantly shorter survival than did those with low to absent expression [75]. However, in this study, VEGF expression by pancreatic cancers failed to correlate with tumor size, lymph node metastasis, vascular invasion, perineural invasion, peritoneal carcinomatous implants, or local recurrence [75]. Itakura et al examined VEGF expression in both human pancreatic cancer cell lines and histologic specimens [76]. They demonstrated VEGF mRNA and protein expression in all cultured cell lines and specimens examined, and they noted that pancreatic cancer tissue had a greater than 5-fold increase in VEGF mRNA versus normal pancreatic control tissue [76].
Furthermore, immunohistochemical analysis of 75 pancreatic cancer tissues showed specific VEGF positivity in the cancerous cells in 64% of all tissues examined [76]. High VEGF expression in pancreatic cancer tissue on immunohistochemistry directly correlated with increased IMD, larger tumor size, and enhanced local spread, but not with decreased patient survival [76]. Additional studies by this group have confirmed overexpression of VEGF mRNA and protein compared to normal pancreas, and interestingly, have demonstrated the presence of VEGF receptors, VEGFR-1 and VEGFR-2, on both cultured human pancreatic cancer cells (AsPC-1, Capan-1, and MIA PaCa-2) and tissue specimens [82]. Functional receptor binding studies by this group confirmed high levels of VEGF-VEGFR interaction only in Capan-1 cells; VEGF dose-dependently enhanced proliferation, promoted MAPK phosphorylation, and induced c-fos activity only in these Capan-1 cells [82]. These results were later reinforced by von Marschall et al, who demonstrated overexpression of VEGF and VEGF receptors in cancerous ductal epithelial cells versus normal pancreas and chronic pancreatitis specimens using immunohistochemistry and in-situ hybridization [83]. VEGF and VEGFR were also demonstrated in human pancreatic cancer cell lines, although, in contrast to the Itakura et al study, no VEGFR mRNA was detected in cultured Capan-1 cells (VEGFR-1 mRNA-positive cells were AsPC-1, Dan-G, and PANC-1; VEGFR-2 mRNA-positive cells were AsPC-1 and Dan-G) [83]. In this study, multiple cell lines of human pancreatic cancer actively secreted VEGF, and treatment of VEGFR-positive cells with VEGF produced significant enhancement of pancreatic cancer cell growth [83]. Therefore, in contrast to other malignancies, in pancreatic cancer VEGF not only influences endothelial cells and tumor angiogenesis, but it appears to be a unique autocrine mitogen for the malignant ductal epithelial cells themselves.
Our laboratory has continued the investigation into the roles of VEGF and its receptors in pancreatic cancer. Our results confirmed the presence of VEGF, VEGFR-1, and VEGFR-2 mRNA and reinforced VEGF's mitogenic effect in multiple human pancreatic cancer cell lines [84]. Immunohistochemistry of human pancreatic cancer specimens demonstrated positive VEGFR-1 and VEGFR-2 staining, and VEGFR-2 positivity correlated significantly with shorter survival [84]. In vitro, VEGF stimulation significantly increased pancreatic cancer cell proliferation, an effect that was abrogated by treatment with antisense oligonucleotides for VEGFR-2, but not for VEGFR-1 [84]. Finally, in an orthotopic nude mouse model of human pancreatic cancer, VEGFR-2 antisense oligonucleotide treatment significantly decreased tumor growth, tumor IMD, peripancreatic tumor infiltration, and intra-abdominal tumor dissemination, but not extra-abdominal metastases [84]. Thus, multiple studies demonstrate the presence of VEGF-A and VEGFRs in malignant pancreatic ductal cells, and VEGF-VEGFR interactions appear to be mitogenic for pancreatic cancer cells. VEGF-A, then, represents a potential single therapeutic target whose inhibition can have important and far-reaching ramifications on both pancreatic cancer angiogenesis and tumorigenesis. Further studies will continue to elucidate the role of VEGF-A and its receptors, along with other pro-and anti-angiogenic cytokines, in pancreatic cancer.
Angiogenesis inhibitors regulate pancreatic cancer growth and metastasis
Additional evidence supporting a crucial role for angiogenesis in pancreatic cancer growth and metastasis comes from the effects of anti-angiogenic compounds on tumor growth, spread, and vascularity in vitro and in vivo. Several studies have demonstrated decreased growth and metastasis of pancreatic cancer using the fumagillin analog TNP-470 with or without cytotoxic agents in vivo [85–87]. In our orthotopic model of human pancreatic cancer, Hotz et al showed that TNP-470 alone decreased tumor growth, IMD, and metastatic spread by anti-angiogenic mechanisms versus antitumor effects [87]. The endogenous anti-angiogenic compound angiostatin, a fragment of plasminogen, has been shown to inhibit growth and neovascularization of hepatic metastases in a hamster model of metastatic pancreatic cancer [88].
While the aforementioned studies utilized general angiogenesis inhibitors, other experiments have targeted specific pro-angiogenic cytokines, including VEGF-A, to inhibit tumor growth. In our laboratory, use of a diphtheria toxin-VEGF fusion protein significantly decreased tumor volume, IMD, and metastasis, and increased animal survival in vivo [89]. Interestingly, despite evidence for the presence of VEGF receptor expression in one of the cell lines used (AsPC-1), the inhibitory effects of the fusion protein were isolated anti-angiogenic phenomena, as the doses of the protein showed no effect on cell growth in vitro [89]. These results underscore the findings of Itakura et al that some pancreatic cancer cells express such low VEGFR levels that they do not exhibit significant ligand-receptor interactions [82]. Further examination of VEGF-A inhibition was carried out by Bruns et al, who used an anti-VEGFR-2 antibody (DC101) with and without gemcitabine in an orthotopic nude mouse model [90]. Treatment with DC101 alone and gemcitabine alone both inhibited tumor growth, but combination therapy inhibited growth to a greater degree and produced demonstrable endothelial cell apoptosis [90]. These results suggest that VEGF-targeted therapies may potentiate the effects of cytotoxic treatments in pancreatic cancer.
Therapeutic implications
Hypoxia is clearly a driving force in pancreatic cancer growth and metastasis. The major effect of hypoxia currently appears to be that of induction of angiogenesis. Numerous anti-angiogenic treatment strategies have shown early promise for therapy of pancreatic cancer. However, because tumor angiogenesis is regulated on multiple complex levels, involves multiple pro- and anti-angiogenic cytokines, and depends upon critical interactions between tumor cells, endothelial cells, tissue resident cells, infiltrating lymphocytes, and the extracellular matrix, single agent approaches are unlikely to produce significant clinical effects. Combination therapies targeting multiple points along the angiogenic pathway will likely be more effective in the treatment of pancreatic cancer. Such therapies may combine VEGF-targeted molecules with matrix metalloproteinase inhibitors, agents that incapacitate enzymes used by migrating endothelial and tumor cells to degrade extracellular matrix and promote tissue invasion [91]. While these agents showed great promise in preclinical studies, initial results in clinical trials comparing MMP-inhibition with gemcitabine have been disappointing [92]. Nevertheless, tumor angiogenesis and its endless array of regulatory factors provides nearly limitless opportunity for the development of new therapeutic agents and/or methods. In fact, recent studies have demonstrated favorable anti-tumor and anti-angiogenic effects using soluble VEGFR products that can be delivered via viral-encoded gene therapy [93, 94]. Further intensive study of human pancreatic adenocarcinoma pathologic specimens may soon identify which patients stand to benefit most from anti-angiogenic treatments. In reality, at this time research exploring hypoxia and angiogenesis in pancreatic cancer remains in its infancy. The implications of hypoxia on cellular metabolism have not been well defined in these tumors. As knowledge in these important areas continues to expand, new approaches to impeding tumor neovascularization will be discovered and implemented.
References
Jemal A, Thomas A, Murray T, Thun M: Cancer statistics, 2002. CA Cancer J Clin. 2002, 52: 23-47.
Folkman J: Tumor angiogenesis: therapeutic implications. N Engl J Med. 1971, 285: 1182-1186.
Connolly DT, Heuvelman DM, Nelson R, Olander JV, Eppley BL, Delfino JJ, Siegel NR, Leimgruber RM, Feder J: Tumor vascular permeability factor stimulates endothelial cell growth and angiogenesis. J Clin Invest. 1989, 84: 1470-1478.
O'Reilly MS, Boehm T, Shing Y, Fukai N, Vasios G, Lane WS, Flynn E, Birkhead JR, Olsen BR, Folkman J: Endostatin: an endogenous inhibitor of angiogenesis and tumor growth. Cell. 1997, 88: 277-285.
Moscatelli D, Presta M, Joseph-Silverstein J, Rifkin DB: Both normal and tumor cells produce basic fibroblast growth factor. J Cell Physiol. 1986, 129: 273-276.
Fett JW, Strydom DJ, Lobb RR, Alderman EM, Bethune JL, Riordan JF, Vallee BL: Isolation and characterization of angiogenin, an angiogenic protein from human carcinoma cells. Biochemistry. 1985, 24: 5480-5486.
Folkman J, Klagsbrun M: Angiogenic factors. Science. 1987, 235: 442-447.
Kerbel RS: Tumor angiogenesis: past, present, and the near future. Carcinogenesis. 2000, 21: 505-515. 10.1093/carcin/21.3.505.
Richard DE, Berra E, Pouysségur J: Angiogenesis: How a tumor adapts to hypoxia. Biochem Biophys Res Commun. 1999, 266: 718-722. 10.1006/bbrc.1999.1889.
Giatromanolaki A, Harris AL: Tumour hypoxia, hypoxia signaling pathways and hypoxia inducible factor expression in human cancer. Anticancer Res. 2001, 21: 4317-4324.
Liotta LA, Steeg PS, Stetler-Stevenson WG: Cancer metastasis and angiogenesis: an imbalance of positive and negative regulation. Cell. 1991, 64: 327-336.
Hanahan D, Folkman J: Patterns and emerging mechanisms of the angiogenic switch during tumorigenesis. Cell. 1996, 86: 353-364.
Brizel DM, Scully SP, Harrelson JM, Layfield LJ, Bean JM, Prosnitz LR, Dewhirst MW: Tumor oxygenation predicts for the likelihood of distant metastases in human soft tissue sarcoma. Cancer Res. 1996, 56: 941-943.
Hockel M, Schlenger K, Aral B, Mitze M, Schaffer U, Vaupel P: Association between tumor hypoxia and malignant progression in advanced cancer of the uterine cervix. Cancer Res. 1996, 56: 4509-4515.
Megibow AJ: Pancreatic adenocarcinoma: designing the examinaton to evaluate the clinical questions. Radiology. 1992, 183: 297-303.
Gray LH, Conger AD, Ebert M: The concentration of oxygen dissolved in tissues at the time of irradiation as a factor in radiotherapy. Br J Radiol. 1953, 26: 683-
Giatromanolaki A, Koukourakis MI, O'Byrne K, Gatter KC, Harris AL: Invading edge vs. inner' (edvin) patterns of vascularization: an interplay between angiogenic and vascular survival factors defines clinical behaviour of non-small cell lung cancer. J Pathol. 2000, 192: 140-149. 10.1002/1096-9896(2000)9999:9999<::AID-PATH693>3.0.CO;2-R.
Gatenby RA, Kessler HB, Rosenblum JS, Coia LR, Moldofsky PJ, Hartz WH, Broder GJ: Oxygen distribution in squamous cell carcinoma metastases and its relationship in outcome of radiation therapy. Int J Radiat Oncol Biol Phys. 1988, 48: 831-838.
Ebert BL, Gleadle JM, O'Rourke JF, Bartlett SM, Poulton J, Ratliffe PJ: Iso-enzyme specific regulation of genes involved in energy metabolism by hypoxia: similarities with the regulation of erythropoietin. Biochem J. 1996, 313: 809-814.
Forsythe JA, Jiang BH, Iyer NV, Agani F, Leung SW, Koos RD, Semenza GL: Activation of vascular endothelial growth factor gene transcription by hypoxia-inducible factor 1. Mol Cell Biol. 1996, 16: 4604-4613.
Semenza GL: Signal transduction to hypoxia-inducible factor 1. Biochem Pharmacol. 2002, 64: 993-998. 10.1016/S0006-2952(02)01168-1.
Melillo G, Musso T, Sica A, Taylor LS, Cox GW, Versio L: A hypoxia-responsive element mediates a novel pathway of activation of the inducible nitric oxide synthase promoter. J Exp Med. 1995, 182: 1683-1693.
Semenza GL, Jiang BH, Leung SW, Passantino R, Concordet JP, Maire P, Giallongo A: Hypoxia response elements in the aldolase A, enolase 1, and lactate dehydrogenase A gene promoters contain essential binding sites for hypoxia-inducible factor 1. J Biol Chem. 1996, 271: 32529-32537. 10.1074/jbc.271.51.32529.
Brahimi-Horn C, Berra E, Pouyssegur J: Hypoxia: the tumor's gateway to progression along the angiogenic pathway. Trends Cell Biol. 2001, 11: S32-S36. 10.1016/S0962-8924(01)02126-2.
Semenza GL: HIF-1 and tumor progression: pathophysiology and therapeutics. Trends Mol Med. 2002, 8: S62-S67. 10.1016/S1471-4914(02)02317-1.
Semenza GL, Wang GL: A nuclear factor induced by hypoxia via de novo protein syntesis binds to the human erythropoietin gene enhancer at a site required for transcriptional activation. Mol Cell Biol. 1992, 12: 5447-5454.
Wang GL, Semenza GL: General involvement of hypoxia-inducible factor 1 in transcriptional response to hypoxia. Proc Natl Acad Sci U S A. 1993, 90: 4304-4308.
Wang GL, Semenza GL: Characterization of hypoxia-inducible factor 1 and regulation of DNA binding activity by hypoxia. J Biol Chem. 1993, 268: 21513-21518.
Wang GL, Semenza GL: Purification and characterization of hypoxia-inducible factor 1. J Biol Chem. 1995, 270: 1230-1237. 10.1074/jbc.270.3.1230.
Wang GL, Jiang BH, Rue EA, Semenza GL: Hypoxia-inducible factor 1 is a basic-helix-loop-helix-PAS heterodimer regulated by cellular O2 tension. Proc Natl Acad Sci U S A. 1995, 92: 5510-5514.
Hoffman EC, Reyes H, Chu FF, Sander F, Conley LH, Brooks BA, Hankinson O: Cloning of a factor required for activity of the Ah (dioxin) receptor. Science. 1991, 252: 954-958.
Reyes H, Reisz-Porszasz S, Hankinson O: Identification of the Ah receptor nuclear translocator protein (Arnt) as a component of the DNA binding form of the Ah receptor. Science. 1992, 256: 1193-1195.
Huang LE, Gu J, Schau M, Bunn HF: Regulation of hypoxia-inducible factor 1α is mediated by an O2-dependent degradation domain via the ubiquitin-proteasome pathway. Poc Natl Acad Sci USA. 1998, 95: 7987-7992. 10.1073/pnas.95.14.7987.
Salceda S, Caro J: Hypoxia-inducible factor 1α (HIF-1α) protein is rapidly degraded by the ubiquitin-proteasome system under normoxic conditions: its stabilization by hypoxic depends upon redox-induced changes. J Biol Chem. 1997, 272: 22642-22647. 10.1074/jbc.272.36.22642.
Maxwell PH, Wiesener MS, Chang GW, Clifford SC, Vaux EC, Cockman ME, Wykoff CC, Pugh CW, Maher ER, Ratcliffe PJ: The tumour suppressor protein VHL targets hypoxia-inducible factors for oxygen-dependent proteolysis. Nature. 1999, 399: 271-275. 10.1038/20459.
Cockman ME, Masson N, Mole DR, Jaakkola P, Chang GW, Clifford SC, Maher ER, Pugh CW, Ratcliffe PJ, Maxwell PH: Hypoxia inducible factor-alpha binding and ubiquitylation by the von Hippel-Lindau tumor suppressor protein. J Biol Chem. 2000, 275: 25733-25741. 10.1074/jbc.M002740200.
Ohh M, Park CW, Ivan M, Hoffman MA, Kim TY, Huang LE, Pavletich N, Chau V, Kaelin WG: Ubiquitination of hypoxia-inducible factor requires direct binding to the beta-domain of the von Hippel-Lindau protein. Nat Cell Biol. 2000, 2: 423-427. 10.1038/35017054.
Richard DE, Berra E, Gothie E, Roux D, Pouyssegur J: p42/p44 mitogen-activated protein kinases phosphorylate hypoxia-inducible factor 1alpha (HIF-1alpha) and enhance the transcriptional activity of HIF-1. J Biol Chem. 1999, 274: 32631-32637. 10.1074/jbc.274.46.32631.
Conrad PW, Freeman TL, Beitner-Johnson D, Millhorn DE: EPAS1 trans-activation during hypoxia requires p42/p44 MAPK. J Biol Chem. 1999, 274: 33709-33713. 10.1074/jbc.274.47.33709.
Zhong H, DeMarzo AM, Laughner E, Lim M, Hilton DA, Zagzag D, Buechler P, Isaacs WB, Semenza GL, Simons JW: Overexpression of Hpoxia-inducible Factor 1 in common human cancers and their metastases. Cancer Res. 1999, 59: 5830-5835.
Koong AC, Mehta VK, Le QT, Fisher GA, Terris DJ, Brown JM, Bastidas AJ, Vierra M: Pancreatic tumors show high levels of hypoxia. Int J Radiat Oncol Biol Phys. 2000, 48: 919-22. 10.1016/S0360-3016(00)00803-8.
Patel A, Toyama MT, Reber P, Alvarez C, Nguyen TN, Ashley SW, Reber HA: Pancreatic interstitial pH in human and feline chronic pancreatitis. Gastroenterology. 1995, 109: 1639-1645.
Buchler P, Hines OJ, Reber HA: HIF-1α and VEGf in pancreatic cancer. Pancreas. 2003, 26: 1-5. 10.1097/00006676-200301000-00010.
Yoon DY, Buchler P, Saarikoski ST, Hines OJ, Reber HA, Hankinson O: Identification of genes differentially induced by hypoxia in pancreatic cancer cells. Biochem Biophys Res Commun. 2001, 288: 882-886. 10.1006/bbrc.2001.5867.
Akakura N, Kobayashi M, Horiuchi I, Suzuki A, Wang J, Cen J, Nizeki H, Kawamura K, hosokawa M, Asaka M: Constitutive expression of Hypoxia-inducible Factor-1α renders pancreatic cancer cells resistant to apoptosis induced by hypoxia and nutrient deprivation. Cancer Res. 2001, 61: 6548-6554.
Shi Q, Abruzzese JL, Huang S, Fidler IJ, Xiong Q, Xie K: Constitutive and inducible Interleukin 8 expression by hypoxia and acidosis renders human pancreatic cells more tumorigenic and metastatic. Clin Cancer Res. 1999, 5: 3711-3721.
Ellenrieder V, Adler G, Gress TM: Invasion and metastasis in pancreatic cancer. Ann Oncol. 1999, 10 (Suppl 4): 46-50. 10.1023/A:1008380501633.
Schwarte-Waldhoff I, Volpert OV, Bouck NP, Sipos B, Hahn SA, Klein-Scory S, Luttges J, Kloppel G, Graeven U, Eilert-Micus C, Hintelmann A, Schmiegel W: Smad4/DPC4-mediated tumor suppression through suppression of angiogenesis. Proc Natl Acad Sci U S A. 2000, 97: 9624-9629. 10.1073/pnas.97.17.9624.
Kuehn R, Lelkes PI, bloechle C, Niendorf A, Izbicki JR: Angiogenesis, angiogenic growth factors, and cell adhesion molecules are upregulated in chronic pancreatic diseases: angiogenesis in chronic pancreatitis and pancreatic cancer. Pancreas. 1999, 18: 96-103.
Niedergethmann M, hildenbrand R, Wolf G, Verbeke CS, Richter A, Post S: Angiogenesis and cathepsin expression are prognostic factors in pancreatic adenocarcinoma after curative resection. Int J Pancreatol. 2000, 28: 31-39. 10.1385/IJGC:28:1:31.
Ikeda N, Adachi M, Taki T, Huang C, Hashida H, Takabayashi A, Sho M, Nakajima Y, Kanehiro H, Hisanaga M, Nakano H, Miyake M: Prognostic significance of angiogenesis in human pancreatic cancer. Br J Cancer. 1999, 79: 1553-1563. 10.1038/sj.bjc.6690248.
Khan AW, Dhillon AP, Hutchins R, Abraham A, Shah SR, Snooks S, Davidson BR: Prognostic significance of intratumoural microvessel density (IMD) in resected pancreatic and ampullary cancers to standard histopathological variables and survival. Eur Surg J Oncol. 2002, 28: 637-644. 10.1053/ejso.2002.1307.
Linder S, Blasjo M, von Rosen A, Parrado C, Falkmer UG, Falkmer S: Pattern of distribution and prognostic value of angiogenesis in pancreatic duct carcinoma: a semiquantitative immunohistochemical study of 45 patients. Pancreas. 2001, 22: 240-247. 10.1097/00006676-200104000-00003.
Karademir S, Sokmen S, Terzi C, Sagol O, Ozer E, Astarcioglu H, Coker A, Astarcioglu I: Tumor angiogenesis as a prognostic predictor in pancreatic cancer. J Hepatobiliary Pancreat Surg. 2000, 7: 489-495. 10.1007/s005340070020.
Fujioka S, Yoshida K, Yanagisawa S, Kawakami M, Aoki T, Yamazaki Y: Angiogenesis in pancreatic carcinoma: thymidine phosphorylase expression in stromal cells and intratumoral microvessel density as independent predictors of overall and relapse-free survival. Cancer. 2001, 92: 1788-1797. 10.1002/1097-0142(20011001)92:7<1788::AID-CNCR1695>3.0.CO;2-Z.
Ellis LM, Takahashi Y, Fenoglio CJ, cleary KR, Bucana CD, Evans DB: Vessel counts and vascular endothelial growth factor expression in pancreatic adenocarcinoma. Eur J Cancer. 1998, 34: 337-340. 10.1016/S0959-8049(97)10068-5.
Wiedner N, Semple JP, Welch WR, Folkman J: Tumor angiogenesis and metastasis – correlation in invasive breast cancer. N Engl J Med. 1991, 324: 1-8.
Macchiarini P, Fontanini G, Hardin M, Squartini F, Angeletti C: Relation of neovascularization to metastasis of non-small cell lung cancer. Lancet. 1992, 340: 145-146. 10.1016/0140-6736(92)93217-B.
Wiedner N, Carroll PR, Flax J, Blumenfield W, Folkman J: Tumor angiogenesis correlates with metastasis in invasive prostate carcinoma. Am J Pathol. 1993, 143: 401-409.
Smith-McCune KK, Wiedner N: Demonstration and characterization of the angiogenic properties of cervical dysplasia. Cancer Res. 1994, 54: 800-804.
Takahashi Y, Kitadai Y, Bucana CD, Cleary KR, Ellis LM: Expression of vascular endothelial growth factor and its receptor, KDR, correlated with vascularity metastasis, and proliferation of human colon cancer. Cancer Res. 1995, 55: 3964-3968.
Shimoyama S, Gansauge F, Gansauge S, Negri G, Oohara T, Beger HG: Increased angiogenin expression in pancreatic cancer is related to cancer aggressiveness. Cancer Res. 1996, 56: 2703-2706.
O'Mahony CA, Seidel A, Albo D, Chang H, Tuszynski GP, Berger DH: Angiostatin generation by human pancreatic cancer. J Surg Res. 1998, 77: 55-58. 10.1006/jsre.1998.5334.
Kisker O, Onizuka S, Banyard J, Komiyama T, Becker CM, Achilles EG, Barnes CM, O'Reilly MS, Folkman J, Pirie-Shepherd SR: Generation of multiple angiogenesis inhibitors by human pancreatic cancer. Cancer Res. 2001, 61: 7298-7304.
Yamazaki K, Nagao T, Yamaguchi T, Saisho H, Kondo Y: Expression of basic fibroblast growth factor (FGF-2)-associated with tumour proliferation in human pancreatic carcinoma. Virchows Arch. 1997, 431: 95-101. 10.1007/s004280050074.
Dvorak HF, Orenstein NS, Carvalho AC, Churchill WH, Dvorak AM, Galli SJ, Feder J, Bitzer AM, Rypysc J, Giovinco P: Induction of a fibrin-gel investment: an early event in line 10 hepatocarcinoma growth mediated by tumor-secreted products. J Immunol. 1979, 122: 166-174.
Dvorak HF, Brown LF, Detmar M, Dvorak AM: Vascular permeability factor/vascular endothelial growth factor, microvascular hyperpermeability, and angiogenesis. Am J Pathol. 1995, 146: 1029-1039.
Brown LF, Detmar M, Claffey K, Nagy JA, Feng D, Dvorak AM, Dvorak HF: Vascular permeability factor/vascular endothelial growth factor: a multifunctional angiogenic cytokine. EXS. 1997, 79: 233-269.
Ferrara N: Molecular and biological properties of vascular endothelial growth factor. J Mol Med. 1999, 77: 527-543. 10.1007/s001099900019.
Dvorak HF: Vascular permeability factor/vascular endothelial growth factor: a critical cytokine in tumor angiogenesis and a potential target for diagnosis and therapy. J Clin Oncol. 2002, 20: 4368-4380. 10.1200/JCO.2002.10.088.
Soker S, Takashima S, Miao HQ, Neufeld G, Klagsbrun M: Neuropilin-1 is expressed by endothelial and tumor cells as an isoform-specific receptor for vascular endothelial growth factor. Cell. 1998, 92: 735-745.
Gluzman-Poltorak Z, Cohen T, Herzog Y, Neufeld G: Neuropilin-2 is a receptor for the vascular endothelial growth factor (VEGF) forms VEGF-145 and VEGF-165. J Biol Chem. 2000, 275: 18040-18045. 10.1074/jbc.M909259199.
Neufeld G, Cohen T, Shraga N, Lange T, Kessler O, Herzog Y: The neuropilins: multifunctional semaphorin and VEGF receptors that modulate axon guidance and angiogenesis. Trends Cardiovasc Med. 2002, 12: 13-19. 10.1016/S1050-1738(01)00140-2.
Brown LF, Berse B, Jackman RW, Tognazzi K, Manseau EJ, Senger DR, Dvorak HF: Expression of vascular permeability factor (vascular endothelial growth factor) and its receptors in adenocarcinomas of the gastrointestinal tract. Cancer Res. 1993, 53: 4727-4735.
Seo Y, Baba H, Fukuda T, Takashima M, Sugimachi K: High expression of vascular endothelial growth factor is associated with liver metastasis and a poor prognosis for patients with ductal pancreatic adenocarcinoma. Cancer. 2000, 88: 2239-2245. 10.1002/(SICI)1097-0142(20000515)88:10<2239::AID-CNCR6>3.0.CO;2-V.
Itakura J, Ishiwata T, Friess H, Fujii H, Matsumoto Y, Buchler MW, Korc M: Enhanced expression of vascular endothelial growth factor in human pancreatic cancer correlates with local disease progression. Clin Cancer Res. 1997, 3: 1309-1316.
Fujimoto K, Hosotani R, Wada M, Lee J-U, Koshiba T, Miyamoto Y, Tsuji S, Nakajima S, Doi R, Imamura M: Expression of two angiogenic factors, vascular endothelial growth factor and platelet-derived endothelial cell growth factor in human pancreatic cancer, and its relationship to angiogenesis. Eur J Cancer. 1998, 34: 1439-1447. 10.1016/S0959-8049(98)00069-0.
Liu N, Furukawa T, Kobari M, Tsao MS: Comparative phenotypic studies of duct epithelial cell lines derived from normal human pancreas and pancreatic carcinoma. Am J Pathol. 1998, 153: 263-269.
Knoll MR, Rudnitzki D, Sturm J, Manegold BC, Post S, Jaeger TM: Correlation of postoperative survival and angiogenic growth factors in pancreatic carcinoma. Hepatogastroenterology. 2001, 48: 1162-1165.
Niedergethmann M, Hildenbrand R, Wostbrock B, Hartel M, Sturm JW, Richter A, Post S: High expression of vascular endothelial growth factor predicts early recurrence and poor prognosis after curative resection for ductal adenocarcinoma of the pancreas. Pancreas. 2002, 25: 122-129. 10.1097/00006676-200208000-00002.
Liu CD, Tilch L, Kwan D, McFadden DW: Vascular endothelial growth factor is increased in ascites from metastatic pancreatic cancer. J Surg Res. 2002, 102: 31-34. 10.1006/jsre.2001.6307.
Itakura J, Ishiwata T, Shen B, Kornmann M, Korc M: Concomitant over-expression of vascular endothelial growth factor and its receptors in pancreatic cancer. Int J Cancer. 2000, 85: 27-34. 10.1002/(SICI)1097-0215(20000101)85:1<27::AID-IJC5>3.0.CO;2-8.
von Marschall Z, Cramer T, Höcker M, Burde R, Plath T, Schirner M, Heidenreich R, Breier G, Riecken E, Wiedenmann B, Rosewicz S: De novo expression of vascular endothelial growth factor in human pancreatic cancer: evidence for an autocrine mitogenic loop. Gastroenterology. 2000, 119: 1358-1372.
Buchler P, Reber HA, Buchler MW, Friess H, Hines OJ: VEGF-RII Influences the Prognosis of Pancreatic Cancer. Ann Surg. 2002, 236: 738-749. 10.1097/00000658-200212000-00006.
Shishido T, Yasoshima T, Denno R, Mukaiya M, Sato N, Hirata K: Inhibition of liver metastasis of human pancreatic carcinoma by angiogenesis inhibitor TNP-470 in combination with cisplatin. Jpn J Cancer Res. 1998, 89: 963-969.
Kato H, Ishikura H, Kawarada Y, Furuya M, Kondo S, Kato H, Yoshiki T: Anti-angiogenic treatment for peritoneal dissemination of pancreas adenocarcinoma: a study using TNP-470. Jpn J Cancer Res. 2001, 92: 67-73.
Hotz H, Reber HA, Hotz B, Sanghavi PC, Yu T, Foitzik T, Buhr HJ, Hines OJ: Angiogenesis inhibitor TNP-470 reduces pancreatic cancer growth. J Gastrointest Surg. 2001, 5: 131-138. 10.1016/S1091-255X(01)80024-X.
Yanagi K, Onda M, Uchida E: Effect of angiostatin on liver metastasis of pancreatic cancer in hamsters. Jpn J Cancer Res. 2000, 91: 723-730.
Hotz H, Gill PS, Masood R, Hotz B, Buhr HJ, Foitzik T, Hines OJ, Reber HA: Specific targeting of tumor vasculature by diphtheria toxin-vascular endothelial growth factor fusion protein reduces angiogenesis and growth of pancreatic cancer. J Gastrointest Surg. 2002, 6: 159-166. 10.1016/S1091-255X(01)00040-3.
Bruns CJ, Shrader M, Harbison MT, Portera C, Solorzano CC, Jauch KW, Hicklin DJ, Radinsky R, Ellis LM: Effect of the vascular endothelial growth factor receptor-2 antibody DC101 plus gemcitabine on growth, metastasis and angiogenesis of human pancreatic cancer growing orthotopically in nude mice. Int J Cancer. 2002, 102: 101-108. 10.1002/ijc.10681.
Matsushita A, Onda M, Uchida E, Maekawa R, Yoshioka T: Antitumor effect of a new selective matrix metalloproteinase inhibitor, MMI-166, on experimental pancreatic cancer. Int J Cancer. 2001, 92: 434-440. 10.1002/ijc.1199.
Bloomston M, Zervos EE, Rosemurgy AS: Matrix metalloproteinases and their role in pancreatic cancer: a review of preclinical studies and clinical trials. Ann Surg Oncol. 2002, 9: 668-674. 10.1245/aso.2002.9.7.668.
Ogawa T, Takayama K, Takakura N, Kitano S, Ueno H: Anti-tumor angiogenesis therapy using soluble receptors: enhanced inhibition of tumor growth when soluble fibroblast growth factor receptor-1 is used with soluble vascular endothelial growth factor receptor. Cancer Gene Ther. 2002, 9: 633-640. 10.1038/sj.cgt.7700478.
Hoshida T, Sunamura M, Duda DG, Egawa S, Miyazaki S, Shineha R, Hamada H, Ohtani H, Satomi S, Matsuno S: Gene therapy for pancreatic cancer using an adenovirus vector encoding soluble flt-1 vascular endothelial growth factor receptor. Pancreas. 2002, 25: 111-121. 10.1097/00006676-200208000-00001.
Author information
Authors and Affiliations
Corresponding author
Authors’ original submitted files for images
Below are the links to the authors’ original submitted files for images.
Rights and permissions
This article is published under an open access license. Please check the 'Copyright Information' section either on this page or in the PDF for details of this license and what re-use is permitted. If your intended use exceeds what is permitted by the license or if you are unable to locate the licence and re-use information, please contact the Rights and Permissions team.
About this article
Cite this article
Duffy, J.P., Eibl, G., Reber, H.A. et al. Influence of hypoxia and neoangiogenesis on the growth of pancreatic cancer. Mol Cancer 2, 12 (2003). https://doi.org/10.1186/1476-4598-2-12
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/1476-4598-2-12