Abstract
Background
The understanding of the epidemiology of severe malaria in African children remains incomplete across the spectrum of Plasmodium falciparum transmission intensities through which communities might expect to transition, as intervention coverage expands.
Methods
Paediatric admission data were assembled from 13 hospitals serving 17 communities between 1990 and 2007. Estimates of Plasmodium falciparum transmission intensity in these communities were assembled to be spatially and temporally congruent to the clinical admission data. The analysis focused on the relationships between community derived parasite prevalence and the age and clinical presentation of paediatric malaria in children aged 0–9 years admitted to hospital.
Results
As transmission intensity declined a greater proportion of malaria admissions were in older children. There was a strong linear relationship between increasing transmission intensity and the proportion of paediatric malaria admissions that were infants (R2 = 0.73, p < 0.001). Cerebral malaria was reported among 4% and severe malaria anaemia among 17% of all malaria admissions. At higher transmission intensity cerebral malaria was a less common presentation compared to lower transmission sites. There was no obvious relationship between the proportions of children with severe malaria anaemia and transmission intensity.
Conclusion
As the intensity of malaria transmission declines in Africa through the scaling up of insecticide-treated nets and other vector control measures a focus of disease prevention among very young children becomes less appropriate. The understanding of the relationship between parasite exposure and patterns of disease risk should be used to adapt malaria control strategies in different epidemiological settings.
Similar content being viewed by others
Background
During the 1980's and 1990's a series of epidemiological observations were reported on the age and clinical patterns of severe malaria in African children across a range of Plasmodium falciparum transmission intensities [1–4]. It appeared from these early observations that the intensity of transmission affected the mean age and clinical features of severe disease and rates of disease showed a nonlinear relationship with transmission intensity, stimulating much heated debate and commentary [5–9].
Subsequent to these earlier studies there has been a renaissance in the clinical epidemiology of severe paediatric malaria across a wide range of different transmission settings, leading to descriptions of severe paediatric malaria from Sudan [10], Mozambique [11], Tanzania [12, 13], Mali [14], Niger [15], Kenya [16], Uganda [17, 18], Yemen [19], Ghana [20, 21] and Zambia [22]. In addition, there have been several further attempts to compare the epidemiological patterns of severe malaria between sites of different transmission intensity in Gabon [23], Burkina Faso [24], Uganda [17], Sudan [25], Tanzania versus Mozambique [26], and one study that compared severe malaria risks at different altitudinal transmission limits in Tanzania [13]. The consensus view of all studies is that as the intensity of P. falciparum transmission increases, the mean age of severe malaria decreases. Less consistent is the reported relationship between clinical syndromes of severe paediatric malaria and transmission intensity.
There are three limitations of many of the reported ecological comparisons. First, they often compare data from very few sites, reducing the contextual ranges of the observations and thus their wider validity. Second, the measures of transmission intensity used in most studies are often imperfect or assumed rather than measured [13, 17, 23, 25]; or not matched to the period of clinical surveillance under review [11, 26]. Finally, despite an increased number of observational studies of severe malaria, they often do not cover the same age range, nor do they use similar diagnosis and surveillance methods.
To circumvent some of these limitations of cross-site comparisons and increase the power to generalize from observations, data from 17 sites across seven countries are presented. The standardization of metrics used to define transmission intensity in each site have significantly improved, have been temporally matched to the clinical surveillance period and attempts have been made to ensure standardization in surveillance and diagnostic methods between survey observations, to examine the relationship between age patterns of hospitalized paediatric malaria and P. falciparum transmission intensity.
Methods
Clinical surveillance
In this review we have assembled clinical admission data from 17 communities served by 13 hospitals. The surveillance sites were selected on the basis of having established clinical and parasitological surveillance, often to specifically study the pathophysiology, management and epidemiology of severe paediatric malaria.
Study sites
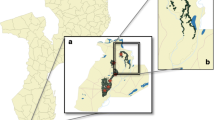
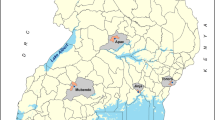
The 17 communities represent a wide range of malaria ecology typical of the P. falciparum endemic world (Figure 1, Table 1). These include six sites where the clinical pattern of severe malaria and its relationship to transmission intensity were described by Snow and colleagues in the early 1990s [2, 3]; three communities in Kenya (Kilifi North, Kilifi South and Siaya), two in The Gambia (Bakau and Sukuta) and one community in Tanzania (Ifakara). The data collected in Ifakara [2] were re-assembled to ensure that only clinical admissions from Namawala and Michenga villages were included to spatially correspond directly to measures of malaria transmission. Three additional temporally discrete surveillance periods have been included among approximately similar communities studied during the 1990's around Kilifi District Hospital, on the Kenyan Coast including Kilifi North, Chonyi and Junju investigated approximately ten years after clinical descriptions in these approximately matched areas. Data from a further six sites in Africa, where identical surveillance methods were reported, were also included: Humera, Ethiopia [27], Foni Kansala, The Gambia (reported in [28]), Mponda, Malawi (reported in [28]), Magunga and Kilimanjaro, Tanzania [13] and Kabale, Uganda [17]. Two additional sites in the Arab peninsular make up the last study sites and are regarded here as sharing a similar malaria and dominant vector species ecology to the horn of Africa; these include clinical admission data from the Yemeni-Swedish Hospital, in Taiz, and Althowra Hospital in Hodeidah City [19].
Hospital sites included in the study of the age and clinical epidemiology of hospitalized paediatric malaria: Kilifi District Hospital (A), Althowra Hospital (B), Royal Victoria Hospital & the Medical Research Council hospital (C), Yemeni Swedish Hospital (D), Kilimanjaro CMC (E), Humera district Hospital (F), Kabale regional refferal Hospital (G), Mangochi district Hospital (H), Sibanor Clinic (I), Korogwe District Hospital (J), Siaya District Hospital (K), St Francis Hospital (L).
Surveillance and diagnosis
At each hospital all paediatric admissions routinely undergo a screening procedure where symptom histories are recorded. the definition of paediatric is restricted to children aged less than ten years. Each child was examined on admission and a blood sample taken for malaria parasitology and haematology. Diagnosis was supported by detailed clinical examination; all clinical and laboratory data are reviewed by investigating physicians who established a primary diagnosis (defined as the principal reason for the child's admission). A primary diagnosis of malaria was made when a child had a positive blood smear and no other detectable cause for the clinical presentation, after a review of all available clinical and haematological data and where indicated, X-ray and microbiological data. Two clinically important complications of severe malaria in African children are cerebral malaria and severe malarial anaemia [29, 30]. Consciousness on admission is recorded at most sites according to the Blantyre Coma Score (BCS) based on verbal, motor, and gaze responses to stimulation [29, 31]. To allow comparison across studies a BCS of 0, 1, or 2 (4 or 5 considered normal depending on age [29]) was used to define coma and cerebral malaria in the presence of malaria infection and absence of other causes for the clinical presentation. In Kabale, a BCS of ≤ 2 was used to describe cerebral malaria in children aged less than 5 years old and a Glasgow Coma score [32] of ≤ 8 for children 5–9 years Severe malaria anaemia was defined as a diagnosis of malaria with an admission haemoglobin level of less than 5.0 g/dl or PCV of less than 15%.
Plasmodium falciparum transmission intensity
Cross-sectional estimates of P. falciparum infection prevalence from the communities served by the study hospital sites were assembled from information available as part of The Malaria Atlas Project [33] database [34, 35]. Infection prevalence estimates were identified where they were spatially congruent, within 20 km of the hospital (Authors, unpublished data), and temporally congruent, during the years of the hospital surveillance. This restriction increases the accuracy of assigning transmission intensity to each of the clinical admission series. For each series of parasite prevalence survey data, the age-ranges reported varied between surveys and these were standardized to a single age range 2–10 years (Pf PR2–10) using algorithms described elsewhere [36].
Results
The study series included a total of 11,446 children admitted to the 13 hospitals with a primary diagnosis of malaria confirmed by microscopy from the 17 communities covering a total of 17 survey years between 1990 and 2007 (Table 1, Figure 1). The communities served by the hospitals represented the entire range of transmission intensity from Pf PR2–10 values of 1% in Kilifi North between 2004–07 to as high as 87% in Namawala/Michenga villages in Tanzania in the early 1990s (Table 1).
To examine the corresponding age-patterns of malaria admission against transmission intensity we computed the proportion of all malaria admissions by single years of age 0 to 9 years at each site, arranged in descending order of Pf PR2–10 in Figure 2. Across the 17 communities the tendency was toward a greater proportion of older children presenting as Pf PR2–10 estimates decreased and a greater proportion of younger children admitted where Pf PR2–10 was higher. It was nevertheless notable, that even at very low estimates of Pf PR2–10, the proportion of cases after the fourth birthday was lower than in early childhood (last five panels in Figure 2).
For a number of reasons, that are expanded on in the discussion, the public health and intervention significance of clinical risks in infancy is of programmatic importance. Among the six communities where the Pf PR2–10 estimate was ≥ 40%; approximately 40% of all malaria admissions were in children aged < 1 year. This compared with an average of 20% of all malaria admissions in infancy among the eight sites with a Pf PR2–10 between 5 and 39%, and 10% of all admissions at the three sites where Pf PR2–10 was recorded as < 5%. There is a direct and strong linear relationship between increasing Pf PR2–10 and the proportion of paediatric malaria admissions that are infants (R2 = 0.73, p < 0.001; Figure 3a) and the converse relationship with the proportion of admissions that are aged between 5–9 years (R2 = 0.47, p = 0.002; Figure 3b). A few outliers are worth identifying: first Junju, Kilifi South, Kenya with a Pf PR2–10 estimate of 26% had no admissions above 5 years of age during the observation period; second, at Kilifi North between 2004–07 Pf PR2–10 was recorded as 1% and Kilimanjaro with a Pf PR2–10 estimate of 6%, however, both had considerably more children admitted aged 0–4 years compared to those 5–9 years of age. Finally, the Kilifi South (Chonyi) admission series documented between 1999 and 2001 shows a high proportion of infants while transmission intensity is intermediary between two sites where the infant admissions are much lower.
Age specific proportion of total hospitalized paediatic malaria cases under different transmission intensities (x-axis; Pf PR 2–10 - Plasmodium falciparum parasite prevalence in children 2 to 10 years). The graphs show for each study sites the proportion of total malaria cases in children < 1 year (Figure 3a) and the proportion of total malaria cases in children 5–9 years (Figure 3b).
The observations summarized in Figure 2 include overlapping communities seen at different times with very different estimates of Pf PR2–10 during each observation period: Kilifi North in the 1990s and 2000s and two closely located communities surveyed between 1999 and 2007 south of Kilifi District Hospital and corresponding to Kilifi South surveyed in 1990's. In the same communities over the two time periods transmission had dropped dramatically. In Kilifi North over ten years Pf PR2–10 dropped from 52% to 1% and at Kilifi South (1992–1995) and the nested area of Chonyi (1999–2001) corresponding Pf PR2–10 estimates were 77% and 43% respectively. In both areas the age patterns of malaria admissions had shifted toward older children as Pf PR2–10 declined but the most dramatic age-shift was observed at Kilifi North with the largest decline in Pf PR2–10 over a longer time frame.
The hospitals that routinely recorded unconsciousness using a BCS or anaemia on admission are shown in Table 1. Across this admission series of 10,642 and 10,742 cases of paediatric malaria respectively, cerebral malaria was reported among 4% and severe malaria anaemia among 17% of admissions. The relationship between the proportion of admissions presenting with cerebral malaria (BCS ≤ 2) and Pf PR2–10 is shown in Figure 4a. This suggests that at higher transmission intensity cerebral malaria is a less common presentation compared to lower estimates of Pf PR2–10, however, without the very high proportion of cerebral malaria cases reported at Kilimanjaro this relationship is less convincing. Similarly excluding the community of Nyamawala/Michenga in Tanzania where 50% of all admissions had a PCV <15% there appears to be no direct relationship between increasing transmission intensity and increase in proportion of severe malaria anaemia cases (Figure 4b).
Discussion
There is mounting evidence that the epidemiology of malaria infection and disease risks are in transition is some parts of Africa, in part as a result of scaling of the provision of insecticide treated nets (ITN) and adoption of new effective therapeutics [37–41]. How changing the natural risks of parasite exposure by vector control will alter the clinical epidemiology of severe, complicated disease in young African children was the subject of concern over 50 years ago [42, 43] and interest in this area re-emerged ten years ago following early comparisons of the clinical outcomes of infection in different transmission settings [3, 4, 8, 44].
There are very few serial, long-term clinical observations of severe paediatric malaria in areas where transmission intensity is in transition [41]. Thus to understand the relationships between transmission intensity and disease outcome we must default to cross-sectional estimations of risk and exposure from different settings to infer what might happen if single communities transitioned between exposure states. Ecological comparative observational epidemiology is not without its limitations. An attempt has been made to standardize observations across 17 communities to minimize methodological measurement differences in the study of the clinical epidemiology of hospitalized paediatric malaria and transmission. Here Pf PR2–10 estimates of transmission contemporary with the clinical observations were used to ensure congruence between exposure and outcome.
One of the most striking observations was the relationship between increasing transmission intensity and the predominant age of paediatric malaria admissions (Figures 2, 3a and 3b). Among communities where Pf PR2–10 is ≥ 40% more than 40% of malaria admissions to paediatric wards were infants, compared to only 10% in areas where Pf PR2–10 is < 5%. These observations are consistent with the view that the speed of acquired clinical immunity scales with the frequency of parasite exposure since birth [3, 4, 45]. Interestingly from the sites where the intensity of transmission was very low (Figure 2), there remains evidence of some acquired functional immunity as expressed by the continued decline after the fourth birthday in the proportion of overall malaria admissions. This was most notable at Taiz (Pf PR2–10 6%) and Bakau (Pf PR2–10 2%). These declining risks with age under very low parasite exposure from birth suggest that only a few parasite exposures might confer a degree of clinical immunity [46] or age itself modifies risks of hospitalized malaria [47].
Despite the overall linear pattern of proportions of admissions aged less than one year (Figure 3a) or greater than five years (Figure 3b) with increasing transmission intensity there were some interesting exceptions to this general pattern. At two coincidentally matched sites investigated between ten years apart (Kilifi North) and five years apart (Kilifi South versus Chonyi) on the Kenyan coast the age-patterns were not as one might have anticipated based on the age patterns of disease seen in areas with very similar Pf PR2–10 (Figure 2). Both sites did show a changing age pattern of disease presentation with decreasing transmission intensity but had not resulted in an age pattern similar to those of historically similar transmission intensity in their second observation period. What these data might suggest is that the cross-sectional investigation of the clinical epidemiology of hospitalized malaria during a period of transmission transition, inevitably results in the study of older children exposed to different transmission intensity risks at different times in their young lives with a cohort effect of accumulated acquired immunity. Thus the "true" age pattern in a community would take some time to stabilize. This phenomenon might also explain the slightly divergent patterns seen at the two South Eastern sites in Tanzania (Magunga and Kilimanjaro) where scaled ITN coverage may also have resulted in a difference between "historical" estimations of Pf PR2–10 and the current values used to match the clinical surveillance period [48].
More importantly the differences in peak age of hospitalized malaria disease presentation and transmission intensity have implications for the design of suites of prevention strategies planned for the control of malaria in Africa. The benefit of targeted intervention in the use of bed nets for malaria control as currently recommended by the WHO is based on the reasoning that targeting bed nets to the highest risk groups; infants and pregnant women, achieves the highest public health impact. Following the same reasoning it is clear that the likely public health impact of intermittent presumptive treatment of infants (IPTi) coincidental with vaccine schedules [49], is likely to be greatest in areas of the transmission axis where the disease burden in concentrated in infancy (Figure 3a). As the estimate of Pf PR2–10 declines IPTi must adapt to include increasingly older age risk groups [50] until one considers adoption of IPT in school-aged children [51] (Figure 3b). It seems entirely plausible that with adequate scaling of ITN coverage in most areas of Africa where Pf PR2–10 starts at values <40% a dramatic reduction in transmission intensity is likely within 3–5 years [52], as this happens the age-patterns of severe malaria presenting to hospital will change and increasingly become less dominated by infants, making the adaptation of the IPTi rationale an immediate priority. Following the same reasoning, outpatient screening tools such as the WHO recommended IMCI guidelines currently in use across many African countries will need to be modified to accommodate expected changes in disease presentation. The current dogma is that across Africa hospitalized malaria is a young paediatric problem, however recent assemblies of Pf PR2–10 information from across the continent [34], suggest that the predominant transmission pattern is one approximating to areas closer to the left hand side of the X-axis of Figures 3a and 3b. Areas of exceptionally high transmission are likely to be less common than previously thought and yet are often the choices of location for most clinical studies of hospitalized malaria in childhood.
In this study series, cerebral malaria appeared to be a more common presentation among children hospitalized with malaria from lower intensity transmission settings compared to areas of high transmission (Figure 4a). This observation has been made in other between site comparative studies [2, 3, 13, 17, 24, 53]. The proportion of malaria admissions regarded as having a BCS ≤ 2 varied considerably under a wide range of transmission conditions from Pf PR2–10 1% to 33%, however, and may also reflect the difficulties in measuring cerebral malaria in very young children [54]. The proportion of children presenting with severe malaria anaemia showed little variation across the range of transmission conditions from 1–80% Pf PR2–10 (Figure 4b) with the exception of the highest recorded proportion of anemic children (50%) from Nyamawala/Michenga villages where Pf PR2–10 was 87%. The epidemiology of severe malaria anaemia may be more complex than previously thought [12, 55] and while is a common feature in young hospitalized infants remains a clinical predictor in older children [30]. A recent study looking at severe anaemia in children indicates that the occurrence of SMA is more likely to be multi-factorial than is CM and importantly is also more likely to be context specific relating to nutrition, prevalence of HIV and prevalence of other diseases which are associated with severe anaemia [56], thus complicating direct comparisons between sites.
The incidence of hospitalization has not been examined, largely because the precise calculation of the paediatric populations at risk was not possible across most of the sites studied after the 1990's. Therefore, no specific comments on the overall changing risks of hospitalization as Pf PR2–10 declines can be made. Nevertheless, it is interesting to note that the one long-term serial study of severe clinical malaria in Africa has investigated the rate of hospitalization during a time of major transmission reduction at Kilifi North [41]. O'Meara et al. (2008) showed that in this community, that began with a Pf PR2–10 of approximately 50% and declined to 1% over ten years, resulted in a ten-fold decline in the risks of hospitalization with malaria in childhood. The focus here has been on better descriptions, across more sites of the age and clinical presentation of hospitalized malaria in childhood likely to be observed with reductions in transmission intensity across Africa as prevention strategies go to scale over the next ten years. Perhaps not surprisingly these results confirm many other observations, using less rigorous inclusion criteria [11, 23, 25], that declining transmission intensity will result in fewer infants and proportionately more children of older age groups as representing the clinical burdens facing hospitals in Africa. It is less certain whether the case-mix of cerebral malaria and severe malaria anaemia will change coincidental with declining transmission intensity.
References
Trape JF, Quinet MC, Nzingoula S, Senga P, Tchichelle F, Carme B, Candito D, Mayanda H, Zoulani A: Malaria and urbanization in central Africa: the example of Brazzaville. Part V: Pernicious attacks and mortality. Trans R Soc Trop Med Hyg. 1987, 81 (Suppl 2): 34-42.
Snow RW, Bastos de Azevedo I, Lowe BS, Kabiru EW, Nevill CG, Mwankusye S, Kassiga G, Marsh K, Teuscher T: Sever e childhood malaria in two areas of markedly different falciparum transmission in east Africa. Acta Trop. 1994, 57: 289-300.
Snow RW, Omumbo JA, Lowe B, Molyneux CS, Obiero JO, Palmer A, Weber MW, Pinder M, Nahlen B, Obonyo C, Newbold C, Gupta S, Marsh K: Relation between severe malaria morbidity in children and level of Plasmodium falciparum transmission in Africa. Lancet. 1997, 349: 1650-1654.
Marsh K, Snow RW: Malaria transmission and morbidity. Parassitologia. 1999, 41: 241-246.
D'Alessandro U: Severity of malaria and level of Plasmodium falciparum transmission. Lancet. 1997, 350: 362-
Molineaux L: Nature's experiment: what implications for malaria prevention?. Lancet. 1997, 349: 1636-1637.
Lengeler C, Smith TA, Armstrong Schellenberg J: Focus on the effect of bednets on malaria morbidity and mortality. Parasitol Today. 1997, 13: 123-124.
Trape JF, Rogier C: Combating malaria morbidity and mortality by reducing transmission. Parasitol Today. 1996, 12: 236-240.
Smith TA, Leuenberger R, Lengeler C: Child mortality and malaria transmission intensity in Africa. Trends Parasitol. 2001, 17: 145-149.
Giha HA, Elghazali G, A-Elgadir TM, A-Elbasit IE, Eltahir EM, Baraka OZ, Khier MM, Adam I, Troye-Blomberg M, Theander TG, Elbashir MI: Clinical pattern of severe Plasmodium falciparum malaria in Sudan in an area characterized by seasonal and unstable malaria transmission. Trans R Soc Trop Med Hyg. 2005, 99: 243-251.
Bassat Q, Guinovart C, Sigauque B, Aide P, Sacarlal J, Nhampossa T, Bardaji A, Nhacolo A, Macete E, Mandomando I, Aponte JJ, Menendez C, Alonso PL: Malaria in rural Mozambique. Part II: children admitted to hospital. Malar J. 2008, 7: 37-
Schellenberg D, Menendez C, Kahigwa E, Font F, Galindo C, Acosta C, Schellenberg JA, Aponte JJ, Kimario J, Urassa H, Mshinda H, Tanner M, Alonso P: African children with malaria in an area of intense Plasmodium falciparum transmission: features on admission to the hospital and risk factors for death. Am J Trop Med Hyg. 1999, 61: 431-438.
Reyburn H, Mbatia R, Drakeley C, Bruce J, Carneiro I, Olomi R, Cox J, Nkya WM, Lemnge M, Greenwood BM, Riley EM: Association of transmission intensity and age with clinical manifestations and case fatality of severe Plasmodium falciparum malaria. JAMA. 2005, 293: 1461-1470.
Ranque S, Poudiougou B, Traore A, Keita M, Oumar AA, Safeukui I, Marquet S, Cabantous S, Diakite M, Mintha D, Cisse MB, Keita MM, Dessein AJ, Doumbo OK: Life-threatening malaria in African children: a prospective study in a mesoendemic urban setting. Pediatr Infect Dis J. 2008, 27: 130-135.
Gay-Andrieu F, Adehossi E, Lacroix V, Gagara M, Ibrahim ML, Kourna H, Boureima H: Epidemiological, clinical and biological features of malaria among children in Niamey, Niger. Malar J. 2005, 4: 10-
Obonyo CO, Vulule J, Akhwale WS, Grobbee DE: In-hospital morbidity and mortality due to severe malarial anemia in western Kenya. Am J Trop Med Hyg. 2007, 77: 23-28.
Idro R, Aloyo J, Mayende L, Bitarakwate E, John CC, Kivumbi GW: Severe malaria in children in areas with low, moderate and high transmission intensity in Uganda. Trop Med Int Health. 2006, 11: 115-124.
Opoka RO, Xia Z, Bangirana P, John CC: Inpatient mortality in children with clinically diagnosed malaria as compared with microscopically confirmed malaria. Pediatr Infect Dis J. 2008, 27: 319-324.
Al-Taiar A, Jaffar S, Assabri A, Al-Habori M, Azazy A, Al-Mahdi N, Ameen K, Greenwood BM, Whitty CJ: Severe malaria in children in Yemen: two site observational study. BMJ. 2006, 333: 827-
Mockenhaupt FP, Ehrhardt S, Burkhardt J, Bosomtwe SY, Laryea S, Anemana SD, Otchwemah RN, Cramer JP, Dietz E, Gellert S, Bienzle U: Manifestation and outcome of severe malaria in children in northern Ghana. Am J Trop Med Hyg. 2004, 71: 167-172.
Oduro AR, Koram KA, Rogers W, Atuguba F, Ansah P, Anyorigiya T, Ansah A, Anto F, Mensah N, Hodgson A, Nkrumah F: Severe falciparum malaria in young children of the Kassena-Nankana district of northern Ghana. Malar J. 2007, 6: 96-
Biemba G, Dolmans D, Thuma PE, Weiss G, Gordeuk VR: Severe anaemia in Zambian children with Plasmodium falciparum malaria. Trop Med Int Health. 2000, 5: 9-16.
Issifou S, Kendjo E, Missinou MA, Matsiegui PB, Dzeing-Ella A, Dissanami FA, Kombila M, Krishna S, Kremsner PG: Differences in presentation of severe malaria in urban and rural Gabon. Am J Trop Med Hyg. 2007, 77: 1015-1019.
Modiano D, Sirima BS, Sawadogo A, Sanou I, Pare J, Konate A, Pagnoni F: Severe malaria in Burkina Faso: influence of age and transmission level on clinical presentation. Am J Trop Med Hyg. 1998, 59: 539-542.
Zeidan Z, Kojal H, Habour A, Nowary K, Hashim F, Awadelkarim M: Clinical and epidemiological features of severe malaria in children in four hospitals in Sudan. East Mediterr Health J. 2006, 12: 783-791.
Menendez C, Schellenberg D, Macete E, Aide P, Kahigwa E, Sanz S, Aponte JJ, Sacarlal J, Mshinda H, Tanner M, Alonso PL: Varying efficacy of intermittent preventive treatment for malaria in infants in two similar trials: public health implications. Malar J. 2007, 6: 132-
Seboxa T, Snow RW: Epidemiological features of severe paediatric malaria in north western Ethiopia. East Afr Med J. 1997, 74: 780-783.
Aguas R, White LJ, Snow RW, Gomes MG: Prospects for malaria eradication in sub-Saharan Africa. PLoS One. 2008, 3: e1767-
Marsh K, Forster D, Waruiru C, Mwangi I, Winstanley M, Marsh V, Newton C, Winstanley P, Warn P, Peshu N: Indicators of life-threatening malaria in African children. N Engl J Med. 1995, 332: 1399-1404.
Severe falciparum malaria. World Health Organization, Communicable Diseases Cluster. Trans R Soc Trop Med Hyg. 2000, 94 (Suppl 1): S1-90.
Molyneux ME, Taylor TE, Wirima JJ, Borgstein A: Clinical features and prognostic indicators in paediatric cerebral malaria: a study of 131 comatose Malawian children. Q J Med. 1989, 71: 441-459.
Teasdale G, Jennett B: Assessment of coma and impaired consciousness. A practical scale. Lancet. 1974, 2: 81-84.
Malaria Atlas Project. [http://www.map.ox.ac.uk]
Guerra CA, Gikandi PW, Tatem AJ, Noor AM, Smith DL, Hay SI, Snow RW: The limits and intensity of Plasmodium falciparum transmission: implications for malaria control and elimination worldwide. PLoS Med. 2008, 5: e38-
Guerra CA, Hay SI, Lucioparedes LS, Gikandi PW, Tatem AJ, Noor AM, Snow RW: Assembling a global database of malaria parasite prevalence for the Malaria Atlas Project. Malar J. 2007, 6: 17-
Smith DL, Guerra CA, Snow RW, Hay SI: Standardizing estimates of the Plasmodium falciparum parasite rate. Malar J. 2007, 6: 131-
Ndugwa RP, Ramroth H, Mueller O, Jasseh M, Sie A, Kouyate B, Greenwood B, Becher H: Comparison of all-cause and malaria-specific mortality from two West African countries with different malaria transmission patterns. Malar J. 2008, 7: 15-
Fegan GW, Noor AM, Akhwale WS, Cousens S, Snow RW: Effect of expanded insecticide-treated bednet coverage on child survival in rural Kenya: a longitudinal study. Lancet. 2007, 370: 1035-1039.
Okiro EA, Hay SI, Gikandi PW, Sharif SK, Noor AM, Peshu N, Marsh K, Snow RW: The decline in paediatric malaria admissions on the coast of Kenya. Malar J. 2007, 6: 151-
Bhattarai A, Ali AS, Kachur SP, Martensson A, Abbas AK, Khatib R, Al-Mafazy AW, Ramsan M, Rotllant G, Gerstenmaier JF, Molteni F, Abdulla S, Montgomery SM, Kaneko A, Bjorkman A: Impact of artemisinin-based combination therapy and insecticide-treated nets on malaria burden in Zanzibar. PLoS Med. 2007, 4: e309-
O'Meara WP, Mwangi TW, Williams TN, McKenzie FE, Snow RW, Marsh K: Relationship between exposure, clinical malaria, and age in an area of changing transmission intensity. Am J Trop Med Hyg. 2008, 79: 185-191.
Garnham PC: Malarial immunity in Africans; effects in infancy and early childhood. Ann Trop Med Parasitol. 1949, 43: 47-61.
Wilson DB, Garnham PC, Swellengrebel NH: A review of hyperendemic malaria. Trop Dis Bull. 1950, 47: 677-698.
Snow RW, Marsh K: Will reducing Plasmodium falciparum transmission alter mortality among African children?. Parasitol Today. 1995, 11 (11): 188-190.
Snow RW, Marsh K: The consequences of reducing transmission of Plasmodium falciparum in Africa. Adv Parasitol. 2002, 52: 235-264.
Gupta S, Snow RW, Donnelly CA, Marsh K, Newbold C: Immunity to non-cerebral severe malaria is acquired after one or two infections. Nat Med. 1999, 5: 340-343.
Baird JK, Masbar S, Basri H, Tirtokusumo S, Subianto B, Hoffman SL: Age-dependent susceptibility to severe disease with primary exposure to Plasmodium falciparum. J Infect Dis. 1998, 178: 592-595.
Drakeley CJ, Corran PH, Coleman PG, Tongren JE, McDonald SL, Carneiro I, Malima R, Lusingu J, Manjurano A, Nkya WM, Lemnge MM, Cox J, Reyburn H, Riley EM: Estimating medium- and long-term trends in malaria transmission by using serological markers of malaria exposure. Proc Natl Acad Sci USA. 2005, 102: 5108-5113.
Schellenberg D, Cisse B, Menendez C: The IPTi Consortium: research for policy and action. Trends Parasitol. 2006, 22: 296-300.
Dicko A, Sagara I, Sissoko MS, Guindo O, Diallo AI, Kone M, Toure OB, Sacko M, Doumbo OK: Impact of intermittent preventive treatment with sulphadoxine-pyrimethamine targeting the transmission season on the incidence of clinical malaria in children in Mali. Malar J. 2008, 7: 123-
Brooker S, Clarke S, Snow RW, Bundy DA: Malaria in African schoolchildren: options for control. Trans R Soc Trop Med Hyg. 2008, 102: 304-305.
Hay SI, Smith DL, Snow RW: Measuring malaria endemicity from intense to interrupted transmission. Lancet Infect Dis. 2008, 8: 369-378.
Slutsker L, Taylor TE, Wirima JJ, Steketee RW: In-hospital morbidity and mortality due to malaria-associated severe anaemia in two areas of Malawi with different patterns of malaria infection. Trans R Soc Trop Med Hyg. 1994, 88: 548-551.
Kahigwa E, Schellenberg D, Schellenberg JA, Aponte JJ, Alonso PL, Menendez C: Inter-observer variation in the assessment of clinical signs in sick Tanzanian children. Trans R Soc Trop Med Hyg. 2002, 96: 162-166.
Imbert P, Sartelet I, Rogier C, Ka S, Baujat G, Candito D: Severe malaria among children in a low seasonal transmission area, Dakar, Senegal: influence of age on clinical presentation. Trans R Soc Trop Med Hyg. 1997, 91: 22-24.
Calis JC, Phiri KS, Faragher EB, Brabin BJ, Bates I, Cuevas LE, de Haan RJ, Phiri AI, Malange P, Khoka M, Hulshof PJ, van Lieshout L, Beld MG, Teo YY, Rockett KA, Richardson A, Kwiatkowski DP, Molyneux ME, van Hensbroek MB: Severe anemia in Malawian children. N Engl J Med. 2008, 358: 888-899.
Acknowledgements
The following people generously helped with the provision of clinical and parasitological data presented in this paper and their interpretation: James Nokes, Geisler Snieder, Terrie Taylor and Edna Ogada. We thank Quique Bassat and Robert Opoka who provided comparative data which for various inclusion criteria reasons we were unable to include in this paper. We thank Simon Hay and Wendy O' Meara for helpful comments on earlier versions of the manuscript. RWS is supported by the Wellcome Trust as Principal Research Fellow (#079081). AAT was funded by UNICEF-UNDP-World Bank-WHO Special Programme for Research and Training in Tropical Diseases (TDR) (project ID: A30333 linked to project ID: A10491). HR was funded by Medical Research Council, UK (grant no. 9901439). JAB is supported by the Wellcome Trust as a Research Fellow (#083579). There are no competing interests. This work also forms an output of the Malaria Atlas Project (MAP, http://www.map.ox.ac.uk) and is published with the permission of the director of KEMRI.
Author information
Authors and Affiliations
Corresponding author
Additional information
Competing interests
The authors declare that they have no competing interests.
Authors' contributions
EA assembled all the hospital data, restructured the data and wrote the manuscript; AAT, HR, RI and JAB were responsible for the assembly of hospital data from Yemen, Tanzania, Uganda and Kilifi, Kenya respectively and contributed to the final manuscript. RWS was responsible for the project and its overall scientific management, interpretation and preparation of the final manuscript.
Authors’ original submitted files for images
Below are the links to the authors’ original submitted files for images.
Rights and permissions
This article is published under license to BioMed Central Ltd. This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/2.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
About this article
Cite this article
Okiro, E.A., Al-Taiar, A., Reyburn, H. et al. Age patterns of severe paediatric malaria and their relationship to Plasmodium falciparum transmission intensity. Malar J 8, 4 (2009). https://doi.org/10.1186/1475-2875-8-4
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/1475-2875-8-4