Abstract
Background
Although tuberculosis (TB) is a minor problem in Denmark, severe and complicated cases occur in HIV positive. Since the new M. tuberculosis specific test for latent TB, the QuantiFERON-TB In-Tube test (QFT-IT) became available the patients in our clinic have been screened for the presence of latent TB using the QFT-IT test. We here report the results from the first patients screened.
Methods
On a routine basis the QFT-IT test was performed and the results from 590 HIV positive individuals consecutively tested are presented here. CD4 cell count and TB risk-factors were recorded from patient files.
Main findings
27/590(4.6%) of the individuals were QFT-IT test positive, indicating the presence of latent TB infection. Among QFT-IT positive patients, 78% had risk factors such as long-term residency in a TB high endemic area (OR:5.7), known TB exposure (OR:4.9) or previous TB disease (OR:4.9). The prevalence of latent TB in these groups were 13%, 16% and 19% respectively. There was a strong correlation between low CD4 T-cell count and a low mitogen response (P < 0.001;Spearman) and more patients with low CD4 cell count had indeterminate results.
Conclusion
We found an overall prevalence of latent TB infection of 4.6% among the HIV positive individuals and a much higher prevalence of latent infection among those with a history of exposure (16%) and long term residency in a high endemic country (13%). The QFT-IT test may indeed be a useful test for HIV positive individuals, but in severely immunocompromised, the test may be impaired by T-cell anergy.
Similar content being viewed by others
Introduction
Tuberculosis (TB) is the most prevalent disease in human immunodeficiency virus (HIV) positive and the majority of the people at risk of HIV and TB are living in Sub Sahara Africa [1]. The risk of developing active TB in HIV positive individuals is increased many fold even when antiretroviral chemotherapy is given [2, 3] and the incidence of TB is increasing in regions where HIV is prevalent [1]. To prevent further spread of TB, intensified efforts are needed such as active case finding, and reducing the risk of reactivating TB in persons with latent tuberculosis infection (LTBI), through prophylactic and antiretroviral treatment.
Diagnosis of early sputum negative tuberculosis and LTBI has been hampered by low performance of the tools currently available. The Tuberculin Skin Test (TST) based on Purified Protein Derivative (PPD) has been the most important tool for the detection of LTBI for almost a century. The main drawback of the TST is the lack of specificity due to cross reactivity with proteins present in other mycobacteria such as the Bacille Calmette Guèrin (BCG) vaccine strain, M. avium complex organisms, and other non tuberculous mycobacteria [4–7]. In addition, the sensitivity of the TST is reduced in HIV positive patients[2, 4, 8].
Identification of 3 M. tuberculosis specific antigens, ESAT-6, CFP-10, and TB 7.7, has led to the development of a whole new generation of M. tuberculosis specific diagnostic tests [6]. ESAT-6, CFP-10, and TB 7.7 are contained within the regions of the mycobacterial genome which are absent from M. bovis BCG, M. avium and most other non-tuberculosis mycobacteria [6, 9–11]. The M. tuberculosis specific tests are based on the stimulation of sensitized T-lymphocytes followed by measurement of interferon-γ (IFN-γ) by either enzyme linked immunoassay (ELISA) or enzyme linked immunospot assay. The latest improvement within this technology is the QuantiFERON® TB-Gold In-Tube test (Cellestis, Australia), in which whole blood is drawn directly into vacutainer tubes precoated with antigens ready for incubation (QFT-IT test).
The sensitivity of the M. tuberculosis specific IFN-γ tests for the diagnosis of active TB has in most studies been >85% [12–15] and specificity in low TB risk populations 97–100% [1, 5, 7, 12–17] with a low number of indeterminate test results. There is high a correlation between a positive antigen specific IFN-γ response and the degree of TB exposure [18–21] indicating that the test detects recent and latent infection. Cross reactivity has not been reported neither in healthy BCG vaccinated individuals [12, 13, 16, 17, 20, 22] nor in patients infected with M. avium[5, 7]. The only other mycobacteria which have been shown to induce T-cell recognition of ESAT-6 and CFP-10 are M. marinum and M. kansasii[23]. Only very limited information is available on the performance of IFN-γ tests in HIV positive and immunocompromised individuals.
The incidence of TB in Denmark is low <10/105 inhabitants/year [24] and the prevalence of HIV infection is 70/105 inhabitants[25]. Every year 10–12 HIV positive individuals are diagnosed with active TB[24], corresponding to a strikingly high incidence of TB in HIV positive of >300/105 individuals/year. This high incidence suggests a need for greater awareness and improved TB control measures among HIV positive. When the M. tuberculosis specific IFN-γ tests became commercially available in Denmark in 2004, we decided to screen our patients for LTBI using the QFT-IT test. We here report the results of the first 590 HIV positive individuals who were tested with the QFT-IT test.
Materials and methods
Study population
We used the QFT-IT test to screen for LTBI among the HIV positive patients attending the outpatient clinic at the University Hospital Hvidovre, Denmark. The clinic monitors 1300 HIV positive patients out of a total of approximately 3050 known HIV positive persons in Denmark[25]. Patients were screened during their routine quarterly check-up. This check-up comprises clinical evaluation, control of viral load, CD4-cell count, compliance with treatment, and an evaluation of potential side effects. Patients with a positive QFT-IT test were evaluated to rule out active TB. By reviewing the patient files, clinical information was recorded, such as age, sex, ethnicity, year of HIV diagnosis, AIDS defining diagnosis, previous treatment for active TB, and on tuberculosis risk factors such as exposure to an index case with sputum positive TB, history of long term residency in a high endemic country (defined as a country with a TB incidence >25:105), intravenous drug use (IVDU) and factors assumed to influence immune status such as alcohol abuse or diabetes.
QuantiFERON®TB-Gold In-Tube test
The QFT-IT test was performed at the Department for Clinical Microbiology according to the manufacturer's instructions; Briefly, 1 mL of blood was drawn directly into vacutainer tubes coated with saline (negative control), peptides of ESAT-6, CFP-10 and TB-7.7, or PHA (mitogen control). Tubes were incubated for 20 hours at 37°C, and plasma was harvested and frozen until further analysis. The amount of IFN-γ produced was determined using ELISA. IFN-γ release in the saline control tube (Nil) was subtracted from the TB antigen and PHA stimulated tubes. Samples with ≥0.35 IU/mL IFN-γ following stimulation with M. tuberculosis specific antigens were considered positive, while samples with <0.35 IU/mL were considered negative. The QFT-IT test result was considered indeterminate if production of IFN-γ after stimulation with PHA was < 0.5 IU/mL; indeterminate results could be due to technical errors or anergy. Calculations were performed using software provided.
Statistical methods
Median values, 25th and 75th percentiles and mean ± standard deviations are shown. Median values were compared using Mann Whitney ranked sum test. Trend analysis was performed using non-parametric test for trend across ordered groups. Chi-square test and Mc Nemar tests were used to compare proportions. The correlation between CD4-cell count and the level of response to PHA was assessed using Spearman correlation test. Calculations were performed using SAS, Med Calc and the SISA software http://home.clara.net/sisa/.
From the Danish Data Protection Agency, permission to analyze on data from the patient files was obtained (Jr.nr.2005-41-5520).
Results
The screening was initiated October 2004 and by January 2005, 607 patients had been tested. In 17 patients, QFT-IT results were not available due to technical or logistic errors (i.e. samples left for too long before incubation, the patient failed to go to the laboratory for the test) and were not included in the data analysis. Baseline information for 590 HIV patients are shown in Table 1. Based on data from the Danish HIV cohort[25], we believe that the patients included are representative for the entire Danish HIV population.
Baseline IFN-γ responses
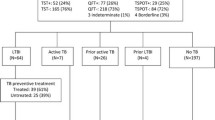
The distribution of IFN-γ released upon stimulation with either PHA or ESAT-6, CFP-10 and TB-7.7 are shown in Figure 1. During the first months, 33 patients had blood drawn twice with an interval of 1–12 weeks. Very low variation was seen between the two time points. The median IFN-γ production were 19.47 IU/mL and 19.74 IU/mL respectively after PHA stimulation and 0.01 IU/mL and 0.01 IU/mL after stimulation with antigen (data not shown). Three individuals changed from an indeterminate PHA response to a positive response or the opposite. Patient 1. changed from 1.72 IU/ml to 0.25 IU/ml, patient 2. from 1.69 IU/ml to 0,16 IU/ml, and patient 3. from 0.07 IU/ml to 6,72. Only patient converted from a negative (0.22 IU/ml) to a positive QFT-IT response (0.42 IU/mL) in the second test 3 month later. This patient had been visiting relatives in a high incidence area between the two tests. The remaining patients were QFT-IT test negative on both tests. For data analysis the first sample was always used. Of the 590 patients screened, 20(3.4%) patients were not able to mount an IFN-γ response above the cut-off (>0.5 IU/mL) in response to PHA and their QFT-IT test results were considered "indeterminate". Of 570 patients with determinate test results, 27 were QFT-IT test positive and 543 were QFT-IT test negative (Figure 2).
IFN-γ release after stimulation of whole blood with either TB antigen (left) or Phytohaematglutinin (PHA)(mitogen) (right). All results are stratified into intervals according to the level of IFN-γ released after stimulation and the number of individuals with IFN-γ release within each interval are shown.
Prevalence latent and incidence of active TB
The overall prevalence of LTBI, determined by a positive QFT-IT test result, was 4.6% (27/590) and 4.7% (27/570) when patients with an indeterminate response were excluded. After excluding all patients with a history of previous TB or indeterminate QFT-IT test result, the prevalence was 4.1% (22/542). One patient was already on chemotherapy when the QFT-IT test was done and all patients with positive QFT-IT tests were screened for active TB. Within A one year period from of the QFT-IT test was performed 2 patients, both QFT-IT positive, were diagnosed with active TB. One of the patients had completed 9 months of treatment 1 year prior, but had a relapse of pulmonary TB. The other patient had been intensively investigated for active TB due to unspecific symptoms and 9 month after the QFT-IT was done active TB was and finally diagnosed in an abdominal lymph gland. Despite the low number of TB cases, the incidence of active TB within the year of the screening was extremely high 7.407:105(2/27).
Identification of risk factors
Risk factor correlation was determined using results from the 570 individuals with a valid QFT-IT test result (PHA response >0.5 IU/mL). Covariates including age, sex, year of HIV diagnosis, AIDS diagnosis, CD4-count, HIV RNA, prior TB diagnosis, factors presumed to influence immune status (alcohol abuse or diabetes) and tuberculosis risk factors (history of TB exposure, long term residency in a high endemic country and IVDU) were analysed (Table 2). The patients with a positive QFT-IT test had significantly more risk factors than the QFT-IT negative patients; 78% (21/27) of the QFT-IT positive patients had one or more TB risk factors in contrast to 34% (184/543) of the patients with negative QFT-IT test (OR 7.2, CI: 2.8–18.2, p= 0.00003). Of those with an indeterminate test, 65%(13/20) had risk factors for TB. Despite the low number of patients with a positive QFT-IT test result, we identified groups of individuals with an increased risk of LTBI: patients with a history of TB exposure (OR 4.9, CI: 2.0–11.8, p= 0.001154) and patients with long term residency in a high endemic country (OR: 5.7, CI: 2.6–12.5, p = 0.00002). Among patients with a history of previously treated TB, there was an increased risk of a positive QFT-IT test(OR: 4.9, CI: 1.7–14.1, p= 0.007). In contrast, age, IVDU, alcohol abuse or diabetes, CD4-cell count or viral load were not associated with positive QFT-IT test results. The calculated odds ratios translated into a prevalence of LTBI among HIV positive patients with a long term residency in a high endemic country of 13% (15/123) among patients with a history of exposure of 16% (8/51), and among patients with previous TB of 19% (5/27).
Nine-teen percent (5/27) of the QFT-IT positive individuals were previously treated for TB. The median interval between TB diagnosis and the present QFT-IT test was 1,5 years (25th–75th quartile 0.5–4.3 years) for the patients with a positive QFT-IT test in contrast to 6.5 years (25th–75th quartile 4.4–9.4 years) for patients with a negative QFT-IT test (p = 0.019, data not shown).
Influence of low CD4 cell count on the outcome of the QFT-IT test
We analyzed the possible effect of a low CD4 count on the test performance and found a strong correlation (p < 0.001 Spearman) between the CD4-cell count and the level of PHA stimulated IFN-γ production (data not shown). The level of IFN-γ produced in response to PHA by each individual has been stratified according to the level of CD-4 cell count and is shown in Fig. 3. The median IFN-γ levels as well as the proportion of patients with indeterminate results is shown in Table 3. The median IFN-γ release in the group with a CD4-cell count <100 cells/μL was significantly lower than any of the three other groups (Mann-Whitney ranked sum test: p < 0.0001) and there was a trend for increasing INF-γ release for increasing CD4 group (non-parametric test for trend across ordered groups (p < 0.0001). In addition, 24% (4/17) of the patients with a CD4-cell count <100 cells/μL had an indeterminate test result due to low INF-γ production following PHA stimulation compared to only 2.8%(16/573) of the patients with a CD4 cell count >100 cells/μL (p < 0.0005).
IFN-γ release (IU/mL) after stimulation of whole blood with PHA (mitogen). Results are stratified into intervals according to the CD4-cell count for each individual. The median IFN-γ values within each CD4-cell count interval are indicated with horizontal lines. Cut off for PHA response of 0.5 IU/ml is shown by a dotted line.
Discussion
We found that the overall prevalence of LTBI (defined by a positive QFT-IT test) of 4.6% among HIV positive in Denmark was relatively low, but the prevalence of LTBI was much higher among those with a history of residence in a TB high endemic country (13%) or with known TB exposure (16%). In low endemic countries very low prevalence of LTBI (0–3%) has been found independently of BCG vaccination status [12, 13, 15–17, 20]. In an intermediate endemic burden country, the prevalence of LTBI in the general population was low 4%, increasing to 21% in contacts of sputum positive TB patients[18]. In TB high endemic regions, the prevalence of LTBI in the population was 30%[19] increasing to 60–70% in household contacts of TB patients[16, 19] and to 40% in a group of Indian health care workers[26]. Together, the QFT-IT test appears to be very efficient in specific identification of individuals at risk of LTBI. We did not find an association between IVDU or alcohol abuse and being QFT-IT test positive. This was unexpected since the impression is that there is an increased risk of TB among patients with IVDU and alcoholics in Denmark due to increased risk of exposure[24, 27].
Patients with a history of previously treated TB had a high rate of positive QFT-IT test results(19%). The rate was highest in patients with recent TB compared to patients with TB many years ago suggesting that the QFT-IT test response may diminish over time. There is an ongoing debate whether it is possible to monitor the effect of chemotherapy treatment using INF-γ based tests[28, 29], but the present study and previous reports[13, 30], indicate M. tuberculosis-specific responses can be retained for many years after treatment. Whether this reflects differences in long term memory immunity or insufficient treatment leading to persistent or latent infection is unknown.
There is a relevant concern that the performance of the QFT-IT test, in line with the TST, could be impaired by low sensitivity in patients with advanced immunodeficiency. The PHA control serves as a surrogate marker for anergy as well as a quality control of the assay. In patients with a CD4-cell count <100 cells/μL, we found a higher proportion of indeterminate test results (24% vs 2.8%) due to low PHA response and there was a significant correlation between CD4-cell count and PHA induced IFN-γ release. These findings support the hypothesis that the performance of the IFN-γ based tests is impaired in patients with advanced immunosuppression. In vivo and in vitro anergy in HIV positive individuals is well recognized [2–4, 8, 31, 32] and the reduced antigen response correlates proportionally with CD4-cell count and is reversible during antiretroviral treatment[3, 32]. Fisk and colleagues found that a CD4-cell count <100 cells/μL, was the critical level associated with skin test anergy[32]. Limited data are available on the performance of the IFN-γ test in HIV positive individuals. Converse and colleagues found, using the 1st generation QuantiFERON® test based on tuberculin PPD, a reduced rate of responders and a lower mean IFN-γ response in HIV positive individuals with a low CD4-cell count (<200 cells/μL)[8]. Other studies [15, 33] have used the ELISPOT test based on ESAT-6 and CFP-10 and found that the number of responders as well as the mean IFN-γ response was reduced in HIV positive individuals. However neither CD4-cell count or AIDS diagnosis, were available in either study. A small study including 29 HIV positive patients surprisingly concluded that there was no impact of a low CD4-cell count on the performance of the IFN-γ response in an ELISPOT assay[34]. However, based on our findings and the numerous reports demonstrating reduced T-cell function in HIV patients it is most likely that the M. tuberculosis specific IFN-γ responses are impaired in patients with advanced immunosuppression in both ELISPOT and whole blood assays.
There is not yet consensus on how to determine the critical level of immunosuppression which may impair the performance of the tests. Reducing the cut off level is a possibility, but may result in the loss of specificity. An alternative is to define a cut-off level of CD4-cells at which the sensitivity of the IFN-γ is impaired. Until further information has been obtained, we argue that PHA is used as the currently best described control and emphasize the need for careful interpretation of an indeterminate or negative test result in HIV positive with low a CD4 cell count (i.e. <100–200 cells/μL). Despite these considerations it is worth noticing that 76% of the patients with a low CD4-cell count did respond to stimulation with PHA.
TST was not performed in parallel with the QFT-IT screening, which is of course a constrain to the overall evaluation of the results. TST however, is not routinely performed in our patients because most of the HIV positive patients were born before 1975 and thus BCG vaccinated and a poor specificity of the TST is expected. Despite this, a TST would have contributed to understanding of the differences between the TST and QFT-IT in HIV positive.
Perspectives
The M. tuberculosis specific QFT-IT test offers methodological and logistic advantages over the TST. It requires only one patient visit and plasma can be frozen for later analysis. It does not induce a boosting phenomenon that is seen with the TST due to repeated injections of mycobaterial antigens. Once established in the laboratory, reproducibility is high as shown herein. The number of steps resulting in direct contact with potentially contagious blood from HIV positive individuals is minimal with the In-Tube test system, thus reducing the occupational hazards of performing TB testing. By introducing the M. tuberculosis specific tests, we may be able to improve TB control by specific identification of those HIV positive individuals with LTBI. A positive QFT-IT test is strongly suggestive of LTBI whereas an indeterminate test result or a negative QFT-IT test result in the severely immunocompromised hosts should always be interpreted with caution
Conclusion
Using the QFT-IT test, we found an overall prevalence of LTBI of 4.6% in HIV positive individuals and a much higher prevalence of LTBI among patients with known exposure(16%) and residency in a high endemic country(13%). Two cases of active TB was found among 27 QFT-IT positive patients resulting in an extremely high incidence of TB (7.4%). The QFT-IT test may be a useful new test for detecting LTBI in immunocompetent HIV positive individuals and future studies should be designed to determine the critical lower level of CD4-cells and to determine the role of these tests in high endemic regions.
References
WHO: Global tuberculosis control- surveillance, planning, financing. WHO report 2005. [http://www.who.int/tb/publications/global_report/2005/en/] WHO/HTM/TB/2005 2005.
Horsburgh CR Jr: Priorities for the treatment of latent tuberculosis infection in the United States. N Engl J Med 350(20):2060–7. 2004; May 13
Lawn SD, Bekker LG, Wood R: How effectively does HAART restore immune responses to Mycobacterium tuberculosis? Implications for tuberculosis control. AIDS 2005,19(11):1113–1124. July 22
American Thoracic Society: Targeted tuberculin testing and treatment of latent tuberculosis infection. American Thoracic Society. MMWR Recomm Rep 2000,49(RR-6):1–51.
Lein AD, von-Reyn CF, Ravn P, Horsburg CR, Alexander LN, Andersen P: Cellular immune responses to ESAT-6 discriminate between patients with pulmonary disease due to Mycobacterium tuberculosis. Clin Diagn Lab 1999, 6:606–609.
Andersen P, Munk ME, Pollock JM, Doherty TM: Specific immune-based diagnosis of tuberculosis. Lancet 2000,356(9235):1099–1104.
Rolinck-Werninghaus C, Magdorf K, Stark K, et al.: The potential of recombinant antigens ESAT-6 and MPT63 for specific discrimination of Mycobacterium tuberculosis and M. avium infection . Eur J Pediatr 2003,162(7–8):534–536.
Converse PJ, Jones LJ, Astemborski J, Vlahov D, Graham NMH: Comparison of a tuberculin Interferon-g assay with the tuberculin skin test in high risk adults: effect of human immunodeficiency virus infection. The Journal of Infectious Diseases 1997, 176:144–150.
Behr MA, Wilson MA, Gill WP, et al.: Comparative genomics of BCG vaccines by whole-genome DNA microarray. Science 1999,284(5419):1520–1533.
Harboe M, Oettinger T, Wiker HG, Wiker I, Rosenkrands I, Andersen P: Evidence for occurrence of the ESAT-6 protein in Mycobacterium tuberculosis and virulent Mycobacterium bovis and for its absence in Mycobacterium bovis BCG. Infect Immun 1996,64(1):16–22.
Aagaard C, Brock I, Olsen A, Ottenhoff TH, Weldingh K, Andersen P: Mapping Immune Reactivity toward Rv2653 and Rv2654: Two Novel Low-Molecular-Mass Antigens Found Specifically in the Mycobacterium tuberculosis Complex. The Journal of Infectious Diseases 2004, 189:812–819.
Mori T, Sakatani M, Yamagishi F: Specific Detection of Tuberculosis Infection with an Interferon-gamma Based Assay Using New Antigens. Am J Respir Crit Care Med 2004,170(1):65–69.
Ravn P, Munk ME, Andersen AB, et al.: Prospective evaluation of a whole blood test using mycobacterium tuberculosis specific antigen ESAT-6 and CFP10 for diagnosis of active tuberculosis. Clinical Diagnostic Laboratory Immunology 2005,12(4):491–496.
Lalvani A, Pathan AA, McShane H, et al.: Rapid detection of Mycobacterium tuberculosis infection by enumeration of antigen-specific T-cells. Am J Respir Crit Care Med 2001,163(4):824–828.
Chapman AL, Munkanta M, Wilkinson KA, et al.: Rapid detection of active and latent tuberculosis infection in HIV-positive individuals by enumeration of Mycobacterium tuberculosis-specific T-cells. Aids 2002,16(17):2285–2293.
Ravn P, Demissie A, Eguale T, et al.: Human T-cell responses to the ESAT-6 antigen from Mycobacterium tuberculosis. J Infect Dis 1999,179(3):637–645.
Johnson PD, Stuart RL, Grayson ML, et al.: Tuberculin-purified protein derivative-, MPT-64-, and ESAT-6-stimulated gamma interferon responses in medical students before and after mycobacterium bovis BCG vaccination and in patients with tuberculosis. Clin Diagn Lab Immunol 1999,6(6):934–937.
Kang YA, Lee HW, Yoon HI, et al.: Discrepancy between the tuberculin skin test and the whole-blood interferon g assay for the diagnosis of latent tuberculosis infection in an intermediate tuberculosis burden country. JAMA 2005,293(22):2756–2771.
Vekemans J, Lienhardt C, Sillah JS, et al.: Tuberculosis contacts but not patients have higher gamma interferon responses to ESAT-6 than do community controls in The Gambia. Infect Immun 2001,69(10):6554–6557.
Brock I, Weldingh K, Lillebaek T, Follmann F, Andersen P: Comparison of a New Specific Blood Test and the Skin Test in Tuberculosis Contacts. Am J Respir Crit Care Med 170(1):65–69. 2004; Jul 1
Ewer K, Deeks J, Alvarez L, et al.: Comparison of T-cell-based assay with tuberculin skin test for diagnosis of Mycobacterium tuberculosis infection in a school tuberculosis outbreak. Lancet 2003,361(9364):1168–1173.
Brock I, Munk ME, Kok-Jensen A, Andersen P: Performance of whole blood IFN-gamma test for tuberculosis diagnosis based on PPD or the specific antigens ESAT-6 and CFP-10. Int J Tuberc Lung Dis 2001,5(5):462–467.
Arend SM, van Meijgaarden KE, de Boer K, et al.: Tuberculin skin testing and in vitro T cell responses to ESAT-6 and culture filtrate protein 10 after infection with Mycobacterium marinum or M. kansasii. J Infect Dis 186(12):1797–1807. 2002 Dec 15
Kjelsø C, Andersen PH: Tuberculosis. [http://www.ssi.dk] Epi-news week 2004, 47–48.
Lohse N, Hansen AB, Jensen-Fangel S, et al.: Demographics of HIV-1 infection in Denmark: results from the Danish HIV Cohort Study. Scand J Infect Dis 2005,37(5):338–343.
Pai M, Gokhale K, Joshi R, et al.: Mycobacterium tuberculosis infection in health care workers in rural India. Comparison of a whole blood interferon g assay with tuberculin skin testing. JAMA 2005,293(22):27546–27555.
Dragsted UB, Bauer J, Poulsen S, Askgaard D, Andersen AB, Lundgren JD: Epidemiology of tuberculosis in HIV-infected patients in Denmark. Scand J Infect Dis 1999,31(1):57–61.
Carrara S, Vincenti D, Petrosillo N, Petrosillo N, Amicosante M, Giardi E, Goletti D: Use of a T cell-based assay for monitoring efficacy of antituberculosis therapy. Clin Infect Dis 38(5):754–756. 2004; Mar 1
Nicol MP, Pienar D, Wood K, et al.: Enzyme-Linked Immunospot assay responses to early secretory antigen target 6, Culture filtrate protein 19, and purified protein derivate among children with tuberculosis: Implications for diagnosis and monitoring of therapy. CID 2005, 40:1301–1308.
Wu-Hsieh BA, Chen CK, Chang JH, et al.: Long-lived immune response to early secretory antigenic target 6 in individuals who had recovered from tuberculosis. Clin Infect Dis 33(8):1336–1340. 2001; Oct 15
Garcia-Garcia ML, Valdespino-Gomez JL, Garcia-Sancho C, et al.: Underestimating mycobacterium tuberculosis infection in HIV infected subjects using reactivity to tuberculin and anergy panel. International Journal of Epidemiolgy 2000, 29:369–375.
Fisk TL, Hon H, Lennox JL, von Reyn CF, Horsburgh CR Jr: Detection of latent tuberculosis among HIV-infected patients after initiation of highly active antiretroviral therapy. AIDS 2003,17(7):1102–1104.
Scarpellini P, Tasca S, Galli L, Beretta A, Lazzarin A, Fortis C: Selected pool of peptides from ESAT_6 and CFP-10 proteins for detection of Mycobacterium tuberculosis infection. JCM 2004, 42:3469–3474.
Dheda K, Lalvani A, Miller RF, et al.: Performance of a T-cell-based diagnostic test for tuberculosis infection in HIV-infected individuals is independent of CD4 cell count. AIDS 19(17):2038–2041. 2005 Nov 18
Acknowledgements
We thank technician Solveigh Kreisby, Simab Gol Lodhi, Helle Nørreskov (Department for Clinical Microbiology, Hvidovre) for coordinating the blood samples and setting up the ELISA, and Klaus Larsen and Janne Petersen (University Hospital Hvidovre) for statistical counselling.
Author information
Authors and Affiliations
Corresponding author
Additional information
Competing interests
The author(s) declare that they have no competing interests.
Authors' contributions
Inger Brock and Morten Ruhwald have contributed equally to the study.
Financial support
has been obtained by Danish AIDS foundation
Hvidovre Hospital Research Foundation.
Reagents have been supplied at reduced price by Cellestis Ltd. Australia and Statens Serum Institute, Denmark.
Rights and permissions
Open Access This article is published under license to BioMed Central Ltd. This is an Open Access article is distributed under the terms of the Creative Commons Attribution License ( https://creativecommons.org/licenses/by/2.0 ), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
About this article
Cite this article
Brock, I., Ruhwald, M., Lundgren, B. et al. Latent Tuberculosis in HIV positive, diagnosed by the M. Tuberculosis Specific Interferon-γ test. Respir Res 7, 56 (2006). https://doi.org/10.1186/1465-9921-7-56
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/1465-9921-7-56